Abstract
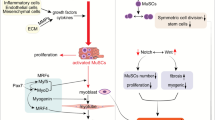
Skeletal muscle structure and function are dependent on the presence or absence of mechanical cues in the tissue microenvironment. High intensity or sustained contractions can build muscle mass with exercise training, whereas bedrest or limb immobilization result in loss of muscle mass. Molecular signaling pathways, such as mTORC1 and induction of activating transcription factor 4 (ATF4), regulate intrinsic myofiber growth and atrophy respectively, yet the extent to which mononuclear cells outside the fiber contribute to muscle structure remodeling remains unclear. The skeletal muscle microenvironment is enriched with mononuclear cells, including progenitor and stem cells, fibroblasts, immune cells, and vascular stromal cells. All possess the potential to sense mechanical cues and contribute to structural remodeling, but the intricate positioning of vascular stromal cells around vessels make these cells particularly receptive to changes in mechanical stimuli due to alterations in both blood perfusion and contraction. Recent studies suggest that pericytes, a population of vascular stromal cells supporting capillaries and venules, are highly responsive to conditions of use and disuse. This chapter discusses the characteristics and behavior of skeletal muscle-derived pericytes as well as the specific responses to physiological stimuli with which muscle can be subjected. Determining how pericytes behave in situations of muscle activation and immobilization is important for the development of cell-based therapies for the treatment of skeletal muscle disorders.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Arentson-Lantz EJ, English KL, Paddon-Jones D, Fry CS (2016) Fourteen days of bed rest induces a decline in satellite cell content and robust atrophy of skeletal muscle fibers in middle-aged adults. J Appl Physiol 120:965–975
Armulik A, Abramsson A, Betsholtz C (2005) Endothelial/pericyte interactions. Circ Res 97:512–523
Armulik A, Genové G, Betsholtz C (2011) Pericytes: developmental, physiological, and pathological perspectives, problems, and promises. Dev Cell 21:193–215
Atherton PJ, Greenhaff PL, Phillips SM et al (2016) Control of skeletal muscle atrophy in response to disuse: clinical/preclinical contentions and fallacies of evidence. Am J Physiol Endocrinol Metab 311:594–604
Biferali B, Proietti D, Mozzetta C, Madaro L (2019) Fibro–adipogenic progenitors cross-talk in skeletal muscle: the social network. Front Physiol 10:1074
Birbrair A, Zhang T, Wang ZM et al (2013) Role of pericytes in skeletal muscle regeneration and fat accumulation. Stem Cells Dev 22:2298–2314
Birbrair A, Zhang T, Files DC et al (2014) Type-1 pericytes accumulate after tissue injury and produce collagen in an organ-dependent manner. Stem Cell Res Ther 5:122
Bodine SC (2013) Disuse-induced muscle wasting. Int J Biochem Cell Biol 45:2200–2208
Boppart MD, De Lisio M, Zou K, Huntsman HD (2013) Defining a role for non-satellite stem cells in the regulation of muscle repair following exercise. Front Physiol 4:310
Brooks NE, Myburgh KH (2014) Skeletal muscle wasting with disuse atrophy is multi-dimensional: the response and interaction of myonuclei, satellite cells and signaling pathways. Front Physiol 5:99
Brooks MJ, Hajira A, Mohamed JS, Alway SE (2018) Voluntary wheel running increases satellite cell abundance and improves recovery from disuse in gastrocnemius muscles from mice. J Appl Physiol 124:1616–1628
Caplan AI (2010) What’s in a name? Tissue Eng Part A 16:2415–2417
Caplan AI, Correa D (2011) The MSC: an injury drugstore. Cell Stem Cell 9:11–15
Cappellari O, Cossu G (2013) Pericytes in development and pathology of skeletal muscle. Circ Res 113:341–347
Chal J, Pourquié O (2017) Making muscle: Skeletal myogenesis in vivo and in vitro. Development 144:2104–2122
Charville GW, Cheung TH, Yoo B et al (2015) Ex vivo expansion and in vivo self-renewal of human muscle stem cells. Stem Cell Rep 5:621–632
Costamagna D, Berardi E, Ceccarelli G, Sampaolesi M (2015) Adult stem cells and skeletal muscle regeneration. Curr Gene Ther 15:348–363
Crisan M, Yap S, Casteilla L et al (2008) A perivascular origin for mesenchymal stem cells in multiple human organs. Cell Stem Cell 3:301–313
De Lisio M, Farup J, Sukiennik RA et al (2015) The acute response of pericytes to muscle-damaging eccentric contraction and protein supplementation in human skeletal muscle. J Appl Physiol 119:900–907
De Souza J, Gottfried C (2013) Muscle injury: review of experimental models. J Electromyogr Kinesiol 23:1253–1260
Dellavalle A, Sampaolesi M, Tonlorenzi R et al (2007) Pericytes of human skeletal muscle are myogenic precursors distinct from satellite cells. Nat Cell Biol 9:255–267
Dellavalle A, Maroli G, Covarello D et al (2011) Pericytes resident in postnatal skeletal muscle differentiate into muscle fibres and generate satellite cells. Nat Commun 2:499
Díaz-Flores L, Gutiérrez R, Varela H (1992) Behavior of postcapillary venule pericytes during postnatal angiogenesis. J Morphol 213:33–45
Díaz-Flores L, Gutiérrez R, Madrid JF et al (2009) Pericytes. Morphofunction, interactions and pathology in a quiescent and activated mesenchymal cell niche. Hist Histopathol 24:909–969
Dumont NA, Bentzinger CF, Sincennes MC, Rudnicki MA (2015) Satellite cells and skeletal muscle regeneration. Compr Physiol 5:1027–1059
Dvoretskiy S, Garg K, Munroe M et al (2019) The impact of skeletal muscle contraction on CD146+Lin− pericytes. Am J Physiol Cell Physiol 317:1011–1024
Egner IM, Bruusgaard JC, Gundersen K (2016) Satellite cell depletion prevents fiber hypertrophy in skeletal muscle. Development 143:2898–2906
Endo T (2015) Molecular mechanisms of skeletal muscle development, regeneration, and osteogenic conversion. Bone 80:2–13
English KL, Paddon-Jones D (2010) Protecting muscle mass and function in older adults during bed rest. Curr Opin Clin Nutr Metab Care 13:34–39
Farup J, De Lisio M, Klejs Rahbek S et al (2015) Pericyte response to contraction mode-specific resistance exercise training in human skeletal muscle. J Appl Physiol 119:1053–1063
Finnerty CC, McKenna CF, Cambias LA et al (2017) Inducible satellite cell depletion attenuates skeletal muscle regrowth following a scald-burn injury. J Physiol 595:6687–6701
Forcina L, Miano C, Pelosi L, Musarò A (2019) An overview about the biology of skeletal muscle satellite cells. Curr Genomics 20:24–37
Frontera WR, Ochala J (2015) Skeletal muscle: a brief review of structure and function. Behav Genet 45:183–195
Fry CS, Lee JD, Jackson JR et al (2014) Regulation of the muscle fiber microenvironment by activated satellite cells during hypertrophy. FASEB J 28:1654–1665
Gautam J, Nirwane A, Yao Y (2017) Laminin differentially regulates the stemness of type I and type II pericytes. Stem Cell Res Ther 8:1–16
Gerhardt H, Betsholtz C (2003) Endothelial-pericyte interactions in angiogenesis. Cell Tissue Res 314:15–23
Giannelli G, de Marzo A, Marinosci F, Antonaci S (2005) Matrix metalloproteinase imbalance in muscle disuse atrophy. Hist Histopathol 20:99–106
Gillies AR, Lieber RL (2011) Structure and function of the skeletal muscle extracellular matrix. Muscle Nerve 44:318–331
Goh Q, Millay DP (2017) Requirement of myomaker-mediated stem cell fusion for skeletal muscle hypertrophy. Elife 6
Guimarães-Camboa N, Cattaneo P, Sun Y et al (2017) Pericytes of multiple organs do not behave as mesenchymal stem cells in vivo. Cell Stem Cell 20:345–359
Günther S, Kim J, Kostin S et al (2013) Myf5-positive satellite cells contribute to Pax7-dependent long-term maintenance of adult muscle stem cells. Cell Stem Cell 13:590–601
Hammers DW, Merscham-Banda M, Hsiao JY et al (2017) Supraphysiological levels of GDF11 induce striated muscle atrophy. EMBO Mol Med 9:531–544
Harrell CR, Simovic Markovic B, Fellabaum C et al (2018) Molecular mechanisms underlying therapeutic potential of pericytes. J Biomed Sci 25:21
Hawke TJ, Garry DJ (2001) Myogenic satellite cells: physiology to molecular biology. J Appl Physiol 91:534–551
Huard J, Li Y, Fu FH (2002) Muscle injuries and repair: current trends in research. J Bone Joint Surg 84-A:822–832
Huntsman HD, Zachwieja N, Zou K et al (2013) Mesenchymal stem cells contribute to vascular growth in skeletal muscle in response to eccentric exercise. Am J Physiol Heart Circ Physiol 304:H72–H81
Huntsman HD, Rendeiro C, Merritt JR et al (2018) The impact of mechanically stimulated muscle-derived stromal cells on aged skeletal muscle. Exp Gerontol 103:35–46
Hyldahl RD, Xin L, Hubal MJ et al (2011) Activation of nuclear factor-κB following muscle eccentric contractions in humans is localized primarily to skeletal muscle-residing pericytes. FASEB J 25:2956–2966
Itoh Y, Hayakawa K, Mori T et al (2014) Stand-up exercise training facilitates muscle recovery from disuse atrophy by stimulating myogenic satellite cell proliferation in mice. Physiol Rep 2
Jackson JR, Mula J, Kirby TJ et al (2012) Satellite cell depletion does not inhibit adult skeletal muscle regrowth following unloading-induced atrophy. Am J Physiol Cell Physiol 303:854–861
Jankowski RJ, Deasy BM, Huard J (2002) Muscle-derived stem cells. Gene Ther 9:642–647
Joe AWB, Yi L, Natarajan A et al (2010) Muscle injury activates resident fibro/adipogenic progenitors that facilitate myogenesis. Nat Cell Biol 12:153–163
Karstoft K, Pedersen BK (2016) Skeletal muscle as a gene regulatory endocrine organ. Curr Opin Clin Nutr Metab Care 19:270–275
Kim JH, Jin P, Duan R, Chen EH (2015) Mechanisms of myoblast fusion during muscle development. Curr Opin Genet Dev 32:162–170
Kirby TJ, Patel RM, McClintock TS et al (2016) Myonuclear transcription is responsive to mechanical load and DNA content but uncoupled from cell size during hypertrophy. Mol Biol Cell 27:788–798
Kostallari E, Baba-Amer Y, Alonso-Martin S et al (2015) Pericytes in the myovascular niche promote post-natal myofiber growth and satellite cell quiescence. Development 142:1242–1253
Kutcher ME, Herman IM (2009) The pericyte: cellular regulator of microvascular blood flow. Microvasc Res 77:235–246
Lepper C, Partridge TA, Fan CM (2011) An absolute requirement for Pax7-positive satellite cells in acute injury-induced skeletal muscle regeneration. Development 138:3639–3646
Li S, Hu GF (2012) Emerging role of angiogenin in stress response and cell survival under adverse conditions. J Cell Physiol 227:2822–2826
Mann CJ, Perdiguero E, Kharraz Y et al (2011) Aberrant repair and fibrosis development in skeletal muscle. Skelet Muscle 1:21
Marg A, Escobar H, Karaiskos N et al (2019) Human muscle-derived CLEC14A-positive cells regenerate muscle independent of PAX7. Nat Commun 10:5776
Mccarthy JJ, Mula J, Miyazaki M et al (2011) Effective fiber hypertrophy in satellite cell-depleted skeletal muscle. Development 138:3657–3666
Mitchell PO, Pavlath GK (2004) Skeletal muscle atrophy leads to loss and dysfunction of muscle precursor cells. Am J Physiol Cell Physiol 287:1753–1762
Montarras D, Morgan J, Collins C et al (2005) Direct isolation of satellite cells for skeletal muscle regeneration. Science 309:2064–2067
Motohashi N, Asakura Y, Asakura A (2014) Isolation, culture, and transplantation of muscle satellite cells. J Vis Exp 86
Munroe M, Dvoretskiy S, Lopez A et al (2019) Pericyte transplantation improves skeletal muscle recovery following hindlimb immobilization. FASEB J 33:7694–7706
Murach KA, White SH, Wen Y et al (2017) Differential requirement for satellite cells during overload-induced muscle hypertrophy in growing versus mature mice. Skelet Muscle 7:14
Murach KA, Fry CS, Kirby TJ et al (2018) Starring or supporting role? Satellite cells and skeletal muscle fiber size regulation. Physiology 33:26–38
Murphy MM, Lawson JA, Mathew SJ et al (2011) Satellite cells, connective tissue fibroblasts and their interactions are crucial for muscle regeneration. Development 138:3625–3637
Nakano M, Atobe Y, Goris RC et al (2000) Ultrastructure of the capillary pericytes and the expression of smooth muscle α-actin and desmin in the snake infrared sensory organs. Anat Rec 260:299–307
Narici MV, de Boer MD (2011) Disuse of the musculo-skeletal system in space and on earth. Euro J Appl Physiol 111:403–420
Newlands S, Levitt LK, Robinson CS et al (1998) Transcription occurs in pulses in muscle fibers. Genes Dev 12:2748–2758
Nirwane A, Gautam J, Yao Y (2017) Isolation of type I and type II pericytes from mouse skeletal muscles. J Vis Exp 123
Otto A, Collins-Hooper H, Patel K (2009) The origin, molecular regulation and therapeutic potential of myogenic stem cell populations. J Anat 215:477–497
Pavlath GK, Rich K, Webster SG, Blau HM (1989) Localization of muscle gene products in nuclear domains. Nature 337:570–573
Petrany MJ, Millay DP (2019) Cell fusion: merging membranes and making muscle. Trends Cell Biol 29:964–973
Relaix F, Zammit PS (2012) Satellite cells are essential for skeletal muscle regeneration: the cell on the edge returns Centre stage. Development 139:2845–2856
Sacchetti B, Funari A, Remoli C et al (2016) No identical “mesenchymal stem cells” at different times and sites: human committed progenitors of distinct origin and differentiation potential are incorporated as adventitial cells in microvessels. Stem Cell Rep 6:897–913
Sambasivan R, Yao R, Kissenpfennig A et al (2011) Pax7-expressing satellite cells are indispensable for adult skeletal muscle regeneration. Development 138:3647–3656
Sampaolesi M, Torrente Y, Innocenzi A et al (2003) Cell therapy of alpha-sarcoglycan null dystrophic mice through intra-arterial delivery of mesoangioblasts. Science 301:487–492
Schwartz LM (2019) Skeletal muscles do not undergo apoptosis during either atrophy or programmed cell death-revisiting the myonuclear domain hypothesis. Front Physiol 9:1887
Snijders T, Wall BT, Dirks ML et al (2014) Muscle disuse atrophy is not accompanied by changes in skeletal muscle satellite cell content. Clin Sci 126:557–566
Suetta C, Frandsen U, Mackey AL et al (2013) Ageing is associated with diminished muscle re-growth and myogenic precursor cell expansion early after immobility-induced atrophy in human skeletal muscle. J Physiol 591:3789–3804
Tidball JG (2005) Inflammatory processes in muscle injury and repair. Am J Physiol Regul Integr Comp Physiol 288:345–353
Uezumi A, Ito T, Morikawa D et al (2011) Fibrosis and adipogenesis originate from a common mesenchymal progenitor in skeletal muscle. J Cell Sci 124:3654–3664
Valero MC, Huntsman HD, Liu J et al (2012) Eccentric exercise facilitates mesenchymal stem cell appearance in skeletal muscle. PLoS One 7:e29760
Wall BT, Dirks ML, van Loon LJC (2013) Skeletal muscle atrophy during short-term disuse: implications for age-related sarcopenia. Ageing Res Rev 12:898–906
Wosczyna MN, Konishi CT, Perez Carbajal EE et al (2019) Mesenchymal stromal cells are required for regeneration and homeostatic maintenance of skeletal muscle. Cell Rep 27:2029–2035
Xu X, Wilschut KJ, Kouklis G et al (2015) Human satellite cell transplantation and regeneration from diverse skeletal muscles. Stem Cell Reports 5:419–434
Yin H, Price F, Rudnicki MA (2013) Satellite cells and the muscle stem cell niche. Physiol Rev 93:23–67
Zou K, Huntsman HD, Carmen Valero M et al (2015) Mesenchymal stem cells augment the adaptive response to eccentric exercise. Med Sci Sports Exerc 47:315–325
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Munroe, M., Dvoretskiy, S., Boppart, M.D. (2021). Skeletal Muscle-Resident Pericyte Responses to Conditions of Use and Disuse. In: Birbrair, A. (eds) Biology of Pericytes – Recent Advances. Stem Cell Biology and Regenerative Medicine, vol 68. Humana, Cham. https://doi.org/10.1007/978-3-030-62129-2_9
Download citation
DOI: https://doi.org/10.1007/978-3-030-62129-2_9
Published:
Publisher Name: Humana, Cham
Print ISBN: 978-3-030-62128-5
Online ISBN: 978-3-030-62129-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)