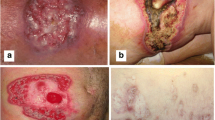
Abstract
This chapter reviews noninfectious inflammatory dermatoses with mainly neutrophilic infiltrates and the formation of pustules. The infiltrate containing neutrophils may be either mild as in urticaria or very dense, even with leukocytoclasia as in Sweet syndrome or pyoderma gangrenosum. Neutrophilic infiltrates and pustular eruptions are caused by different noninfectious immunomechanisms. For some of them, mutations have been found (e.g., NLRC4 mutation in cryopyrin-associated periodic syndromes (CAPS) leading to activation of the inflammasome; IL36RN mutation in pustular psoriasis resulting in uncontrolled IL36-signaling). Neutrophilic dermatoses are of high interest, as they may present dermatological reaction patterns of underlying benign or malignant conditions.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Kasha EE Jr, Epinette WW. Subcorneal pustular dermatosis (Sneddon-Wilkinson disease) in association with a monoclonal IgA gammopathy: a report and review of the literature. J Am Acad Dermatol. 1988;19(5 Pt 1):854–8.
Kretschmer L, Maul J-T, Hofer T, Navarini AA. Interruption of Sneddon-Wilkinson subcorneal pustulation with infliximab. Case Rep Dermatol. 2017;9(1):140–4.
Patel R, Cafardi JM, Patel N, et al. Tumor necrosis factor biologics beyond psoriasis in dermatology. Expert Opin Biol Ther. 2011;11(10):1341–59.
Grob JJ, Mege JL, Capo C, et al. Role of tumor necrosis factor-alpha in Sneddon-Wilkinson subcorneal pustular dermatosis. A model of neutrophil priming in vivo. J Am Acad Dermatol. 1991;25(5 Pt 2):944–7.
Pinkus H. Is subcorneal pustular dermatosis of Sneddon and Wilkinson and entity sui generis? Am J Dermatopathol. 1981;3(4):379–80.
Letter LBL. Subcorneal pustular dermatosis vs pustular psoriasis. Arch Dermatol. 1974;110(1):131.
Navarini AA, Satoh TK, French LE. Neutrophilic dermatoses and autoinflammatory diseases with skin involvement-innate immune disorders. Semin Immunopathol. 2016;38(1):45–56.
Sneddon IB, Wilkinson DS. Subcorneal pustular dermatosis. Br J Dermatol. 1956;68(12):385–94.
Reed J, Wilkinson J. Subcorneal pustular dermatosis. Clin Dermatol. 2000;18(3):301–13.
Patton D, Lynch PJ, Fung MA, Fazel N. Chronic atrophic erosive dermatosis of the scalp and extremities: a recharacterization of erosive pustular dermatosis. J Am Acad Dermatol. 2007;57(3):421–7.
Feramisco JD, Goerge T, Schulz SE, et al. Disseminated erosive pustular dermatosis also involving the mucosa: successful treatment with oral dapsone. Acta Derm Venereol. 2012;92(1):91–2.
Wilk M, Zelger BG, Hauser U, et al. Erosive pustular dermatosis of the scalp: reappraisal of an underrecognized entity. J Dtsch Dermatol Ges. 2018;16(1):15–9.
Marchini G, Ståbi B, Kankes K, et al. AQP1 and AQP3, psoriasin, and nitric oxide synthases 1–3 are inflammatory mediators in erythema toxicum neonatorum. Pediatr Dermatol. 2003;20(5):377–84.
Marchini G, Ulfgren A-K, Loré K, et al. Erythema toxicum neonatorum: an immunohistochemical analysis. Pediatr Dermatol. 2001;18(3):177–87.
Reginatto FP, Muller FM, Peruzzo J, Cestari TF. Epidemiology and predisposing factors for erythema toxicum neonatorum and transient neonatal pustular: a multicenter study. Pediatr Dermatol. 2017;34(4):422–6.
Van Praag MCG, Van Rooij RWG, Folkers E, et al. Diagnosis and treatment of pustular disorders in the neonate. Pediatr Dermatol. 1997;14(2):131–45.
Freeman RG, Spiller R, Knox JM. Histopathology of erythema toxicum neonatorum. Arch Dermatol. 1960;82:586–9.
Lucky AW, Esterly NB, Heskel N, et al. Eosinophilic pustular folliculitis in infancy. Pediatr Dermatol. 1984;1(3):202–6.
Boone M, Dangoisse C, Andre J, et al. Eosinophilic pustular folliculitis in three atopic children with hypersensitivity to Dermatophagoides pteronyssinus. Dermatology. 1995;190(2):164–8.
Hernández-Martín Á, Nuño-González A, Colmenero I, Torrelo A. Eosinophilic pustular folliculitis of infancy: a series of 15 cases and review of the literature. J Am Acad Dermatol. 2013;68(1):150–5.
Ziemer M, Böer A. Eosinophilic pustular folliculitis in infancy: not a distinctive inflammatory disease of the skin. Am J Dermatopathol. 2005;27(5):443–55.
Nervi SJ, Schwartz RA, Dmochowski M. Eosinophilic pustular folliculitis: a 40 year retrospect. J Am Acad Dermatol. 2006;55(2):285–9.
Ishiguro N, Shishido E, Okamoto R, et al. Ofuji’s disease: a report on 20 patients with clinical and histopathologic analysis. J Am Acad Dermatol. 2002;46(6):827–33.
Falanga V. Infantile acropustulosis with eosinophilia. J Am Acad Dermatol. 1985;13(5 Pt 1):826–8.
Mancini AJ, Frieden IJ, Paller AS. Infantile acropustulosis revisited: history of scabies and response to topical corticosteroids. Pediatr Dermatol. 1998;15(5):337–41.
Bundino S, Zina AM, Ubertalli S. Infantile acropustulosis. Dermatologica. 1982;165(6):615–9.
Roujeau JC, Bioulac-Sage P, Bourseau C, et al. Acute generalized exanthematous pustulosis. Analysis of 63 cases. Arch Dermatol. 1991;127(9):1333–8.
Zelickson BD, Muller SA. Generalized pustular psoriasis: a review of 63 cases. Arch Dermatol. 1991;127(9):1339–45.
Navarini AA, Burden AD, Capon F, et al., ERASPEN Network. European consensus statement on phenotypes of pustular psoriasis. J Eur Acad Dermatol Venereol. 2017;31(11):1792–9.
Christophers E, Metzler G, Röcken M. Bimodal immune activation in psoriasis. Br J Dermatol. 2014;170(1):59–65.
Gibson LE, el-Azhari RA. Erythema elevatum diutinum. Clin Dermatol. 2000;18(3):295–9.
Wahl CE, Bouldin MB, Gibson LE. Erythema elevatum diutinum: clinical, histopathologic, and immunohistochemical characteristics of six patients. Am J Dermatopathol. 2005;27(5):397–400.
Llamas-Velasco M, Stengel B, Pérez-González YC, Mentzel T. Late-stage erythema elevatum diutinum mimicking a fibroblastic tumor: a potential pitfall. Am J Dermatopathol. 2018;40(6):442–4.
Cardis MA, Sowash MG, Mosojane KI, et al. HIV-associated erythema elevatum diutinum: a case report and review of a clinically distinct variant. Dermatol Online J. 2018;24(5):15.
Creus L, Salleras M, Sola MA, et al. Erythema elevatum diutinum associated with pulmonary infiltrates. Br J Dermatol. 1997;137(4):652–3.
Ackerman AB, Chongchitnant N, Sanchez J, Guo J. Histologic diagnosis of inflammatory skin diseases: an algorithmic method based on pattern analysis. 2nd ed. Williams and Wilkins; Philadelphia. 1997. p. 488.
Ziemer M, Koehler MJ, Weyers W. Erythema elevatum diutinum – a chronic leukocytoclastic vasculitis microscopically indistinguishable from granuloma faciale? J Cutan Pathol. 2011;38(11):876–83.
Dicken C, Seehafer J. Bowel bypass syndrome. Arch Dermatol. 1979;115(7):837–9.
Kemp DR, Gin D. Bowel-associated dermatosis-arthritis syndrome. Med J Aust. 1990;152:43–5.
Ashchyan HJ, Nelson CA, Stephen S, et al. Neutrophilic dermatoses. Part II. Pyoderma gangrenosum and other bowel- and arthritis-associated neutrophilic dermatoses. J Am Acad Dermatol. 2018;79(6):1009–22.
Marzano AV, Ishak RS, Saibeni S, et al. Autoinflammatory skin disorders in inflammatory bowel diseases, pyoderma gangrenosum and Sweet’s syndrome: a com- prehensive review and disease classification criteria. Clin Rev Allergy Immunol. 2013;45(2):202–10.
Ely PH. The bowel bypass syndrome: a response to bacterial peptidoglycans. J Am Acad Dermatol. 1980;2(6):473–87.
Delaney TA, Clay CD, Randell PL. The bowel-associated dermatosis—arthritis syndrome. Australas J Dermatol. 1989;30(1):23–7.
Cugno M, Gualtierotti R, Meroni PL, Marzano AV. Inflammatory joint disorders and neutrophilic dermatoses: a comprehensive review. Clin Rev Allerg Immunol. 2018;54(2):269–81.
Andre M, Aumaitre O, Papo T, et al. Disseminated aseptic abscesses associated with Crohn’s disease: a new entity. Dig Dis Sci. 1998;43(2):420–8.
Kennedy C. The spectrum of inflammatory skin disease following jejuno-ileal bypass for morbid obesity. Br J Dermatol. 1981;105(4):425–35.
Harrist TJ, Fine JD, Berman RS, et al. Neutrophilic eccrine hidradenitis. A distinctive type of neutrophilic dermatosis associated with myelogenous leukemia and chemotherapy. Arch Dermatol. 1982;118(4):263–6.
Marini M, Wright D, Ropolo M. Neutrophilic eccrine hidradenitis secondary to topotecan. J Dermatolog Treat. 2002;13(1):35–7.
Turan H, Kaya E, Gurlevik Z, et al. Neutrophilic eccrine hidradenitis induced by cetuximab. Cutan Ocul Toxicol. 2012;31(2):148–50.
Dib EG, Ifthikharuddin JJ, Scott GA, et al. Neutrophilic eccrine hidradenitis induced by imatinib mesylate (Gleevec) therapy. Leuk Res. 2005;29(2):233–4.
Herms F, Franck N, Kramkimel N, et al. Neutrophilic eccrine hidradenitis in two patients treated with BRAF inhibitors: a new cutaneous adverse event. Br J Dermatol. 2017;176(6):1645–8.
Bachmeyer C, Reygagne P, Aractingi S. Recurrent neutrophilic eccrine hidradenitis in an HIV-1-infected patient. Dermatology. 2000;200(4):328–30.
Nijsten TE, Meuleman L, Lambert J. Chronic pruritic neutrophilic eccrine hidradenitis in a patient with Behçet’s disease. Br J Dermatol. 2002;147(4):797–800.
Brehler R, Reimann S, Bonsmann G, Metze D. Neutrophilic hidradenitis induced by chemotherapy involves eccrine and apocrine glands. Am J Dermatopathol. 1997;19(1):73–8.
Bailey DL, Barron D, Lucky AW. Neutrophilic eccrine hidradenitis: a case report and review of the literature. Pediatr Dermatol. 1989;6(1):33–8.
Stahr BJ, Cooper PH, Caputo RV. Idiopathic plantar hidradenitis: a neutrophilic eccrine hidradenitis occurring primarily in children. J Cutan Pathol. 1994;21(4):289–96.
Sweet RD. An acute febrile neutrophilic dermatosis. Br J Dermatol. 1964;76:349–56.
Rochet NM, Chavan RN, Cappel MA, et al. Sweet syndrome: clinical presentation, associations, and response to treatment in 77 patients. J Am Acad Dermatol. 2013;69(4):557–64.
Satra K, Zalka A, Cohen PR, Grossman ME. Sweet’s syndrome and pregnancy. J Am Acad Dermatol. 1994;30(2 Pt 2):297–300.
Amouri M, Masmoudi A, Ammar M, et al. Sweet’s syndrome: a retrospective study of 90 cases from a tertiary care center. Int J Dermatol. 2016;55(9):1033–9.
Cohen PR, Kurzrock R. Sweet’s syndrome: a review of current treatment options. Am J Clin Dermatol. 2002;3(2):117–31.
Marcoval J, Martín-Callizo C, Valentí-Medina F, et al. Sweet syndrome: long-term follow-up of 138 patients. Clin Exp Dermatol. 2016;41(7):741–6.
Bidyasar S, Montoya M, Suleman K, Markowitz AB. Sweet syndrome associated with granulocyte colony-stimulating factor. J Clin Oncol. 2008;26(26):4355–6.
Giasuddin AS, El-Orfi AH, Ziu MM, El-Barnawi NY. Sweet’s syndrome: is the pathogenesis mediated by helper T cell type 1 cytokines? J Am Acad Dermatol. 1998;39(6):940–3.
Imhof L, Meier B, Frei P, et al. Severe Sweet’s syndrome with elevated cutaneous interleukin-1β after azathioprine exposure: case report and review of the literature. Dermatology. 2015;230(4):293–8.
Miyoshi T, Yamashita K, Ohno T, et al. Familial Mediterranean fever gene as a possible modifier of Sweet syndrome with chronic myelogenous leukemia. Acta Haematol. 2008;120(1):57–62.
Torrelo A, Patel S, Colmenero I, et al. Chronic atypical neutrophilic dermatosis with lipodystrophy and elevated temperature (CANDLE) syndrome. J Am Acad Dermatol. 2010;62(3):489–95.
Baartman B, Kosari P, Warren CC, et al. Sight-threatening ocular manifestations of acute febrile neutrophilic dermatosis (Sweet’s syndrome). Dermatology. 2014;228(3):193–7.
Su WP, Liu HN. Diagnostic criteria for Sweet’s syndrome. Cutis. 1986;37(3):167–74.
Magro CM, Momtahen S, Nguyen GH, Wang X. Histiocytoid Sweet’s syndrome: a localized cutaneous proliferation of macrophages frequently associated with chronic myeloproliferative disease. Eur J Dermatol. 2015;25(4):335–41.
Rahier JF, Lion L, Dewit O, Lambert M. Regression of Sweet’s syndrome associated with Crohn’s disease after anti-tumor necrosis factor therapy. Acta Gastroenterol Belg. 2005;68(3):376–9.
Cohen PR. Neutrophilic dermatoses: a review of current treatment options. Am J Clin Dermatol. 2009;10(5):301–12.
Requena L, Kutzner H, Palmedo G, et al. Histiocytoid Sweet syndrome. A dermal infiltration of immature neutrophilic granulocytes. Arch Dermatol. 2005;141(7):834–42.
Strutton G, Weedon D, Robertson I. Pustular vasculitis of the hands. J Am Acad Dermatol. 1995;32(2Pt1):192–8.
Galaria NA, Junkins-Hopkins JM, Kligman D, James WD. Neutrophilic dermatosis of the dorsal hands: pustular vasculitis revisited. J Am Acad Dermatol. 2000;43(5Pt1):870–4.
Weenig RH, Bruce AJ, McEvoy MT, et al. Neutrophilic dermatosis of the hands: for new cases and review of the literature. Int J Dermatol. 2004;43(2):95–102.
Stransky L, Broshtilova V. Neutrophilic dermatosis of the dorsal hands elicited by thermal injury. Contact Dermatitis. 2003;49(1):42.
Duquia RP, Almeida HL Jr, Vettorato G, et al. Neutrophilic dermatosis of the dorsal hands: acral Sweet syndrome? Int J Dermatol. 2006;45(1):51–2.
Walling HW, Snipes CJ, Gerami P, Piette WW. The relationship between neutrophilic dermatosis of the dorsal hands and Sweet syndrome: report of 9 cases and comparison to atypical pyoderma gangrenosum. Arch Dermatol. 2006;142(1):57–63.
Cravo M, Cardoso JC, Tellechea O, et al. Neutrophilic dermatosis of the dorsal hands associated with hypopharyngeal carcinoma. Dermatol Online J. 2008;14(7):5.
Cohen PR. Skin lesions of Sweet syndrome and its dorsal hand variant contain vasculitis: an oxymoron or an epiphenomenon? Arch Dermatol. 2002;138(3):400–3.
Jaimes-Lopez N, Molina V, Arroyave JE, et al. Development of pyoderma gangrenosum during therapy with infliximab. J Dermatol Case Rep. 2009;3(2):20–3.
Marzano AV, Cugno M, Trevisan V, et al. Role of inflammatory cells, cytokines and matrix metalloproteinases in neutrophil-mediated skin diseases. Clin Exp Immunol. 2010;162(1):100–7.
Marzano AV, Borghi A, Meroni PL, Cugno M. Pyoderma gangrenosum and its syndromic forms: evidence for a link with autoinflammation. Br J Dermatol. 2016;175(5):882–91.
Powell FC, Su WPD, Perry HO. Pyoderma gangrenosum: classification and management. J Am Acad Dermatol. 1996;34(3):395–409.
Kieffer C, Cribier B, Lipsker D. Neutrophilic urticarial dermatosis: a variant of neutrophilic urticaria strongly associated with systemic disease. Report of 9 new cases and review of the literature. Medicine. 2009;88(1):23–31.
Broekaert SM, Böer-Auer A, Kerl K, et al. Neutrophilic epitheliotropism is a histopathological clue to neutrophilic urticarial dermatosis. Am J Dermatopathol. 2016;38(1):39–49.
McGonagle D, McDermott MF. A proposed classification of the immunological diseases. PLoS Med. 2006;3(8):e297.
Willis WF. The gyrate erythemas. Int J Dermatol. 1978;17(9):698–702.
Rasmussen ER, de Freitas PV, Bygum A. Urticaria and prodromal symptoms including erythema marginatum in danish patients with hereditary angioedema. Acta Derm Venereol. 2016;96(3):373–6.
Farkas H, Harmat G, Fáy A, et al. Erythema marginatum preceding an acute oedematous attack of hereditary angioneurotic oedema. Acta Derm Venereol. 2001;81(5):376–7.
Stollerman GH. Changing streptococci and prospects for the global eradication of rheumatic fever. Perspect Biol Med. 1997;40(2):165–89.
Soria C, Allegue F, España A, et al. Vegetating iododerma with underlying systemic diseases: report of three cases. J Am Acad Dermatol. 1990;22(3):418–42.
Sterling JB, Heymann WR. Potassium iodide in dermatology: a 19th century drug for the 21st century – uses, pharmacology, adverse effects, and contraindications. J Am Acad Dermatol. 2000;43(4):691–7.
Wells GC, Smith N. Eosinophilic cellulitis. Br J Dermatol. 1979;199(1):101–9.
Ackerman AB. Eosinophilic cellulitis (Wells’ Syndrome)? From: http://www.derm101.com/quandaries/eosinophilic-cellulitis-wells-syndrome/. Accessed 25 Nov 2018.
Melski JW. Wells’ syndrome, insect bites, and eosinophils. Dermatol Clin. 1990;8(2):287–93.
Schorr WF, Tauscheck AL, Dickson KB, Melski JW. Eosinophilic cellulitis (Wells’ syndrome): histologic and clinical features in arthropod bite reactions. J Am Acad Dermatol. 1984;11(6):1043–9.
Weedon D. Skin pathology. 3rd ed. Churchill-Livingstone Elsevier; London. 2010. p. 940–41.
Spigel GT, Winkelmann RK. Wells’ syndrome: recurrent granulomatous dermatitis with eosinophilia. Arch Dermatol. 1979;115(5):611–3.
Prakash Babu S, Chen YK, Bonne-Annee S, et al. Dysregulation of interleukin 5 expression in familial eosinophilia. Allergy. 2017;72(9):1338–45.
Dispenza MC, Bochner BS. Diagnosis and novel approaches to the treatment of hypereosinophilic syndromes. Curr Hematol Malig Rep. 2018;13(3):191–201.
Gotlib J. World Health Organization-defined eosinophilic disorders: 2017 update on diagnosis, risk stratification, and management. Am J Hematol. 2017;92(11):1243–59.
Fitzpatrick JE, Johnson C, Simon P, et al. Cutaneous microthrombi: a histologic clue to the diagnosis of hypereosinophilic syndrome. Am J Dermatopathol. 1987;9(5):419–22.
Rueda RA, Valencia IC, Covelli C, et al. Eosinophilic, polymorphic, and pruritic eruption associated with radiotherapy. Arch Dermatol. 1999;135(7):804–10.
van Kester MS, Quint KD. Eosinophilic, polymorphic, and pruritic eruption associated with radiotherapy on the skin of the right breast. JAMA Oncol. 2016;2(5):677–8.
Gallego H, Crutchfield CE 3rd, Wilke MS, Lewis EJ. Delayed EPPER syndrome. Arch Dermatol. 2001;137(6):821–2.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Möckel, S.M.C., Metze, D. (2020). Neutrophilic and Pustular Eruptions. In: Hoang, M., Selim, M. (eds) Hospital-Based Dermatopathology. Springer, Cham. https://doi.org/10.1007/978-3-030-35820-4_4
Download citation
DOI: https://doi.org/10.1007/978-3-030-35820-4_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-35819-8
Online ISBN: 978-3-030-35820-4
eBook Packages: MedicineMedicine (R0)