Abstract
Background: The dosing of opioid receptor agonist medications adequately and on an individual basis is crucial in the pharmacotherapy of opioid dependence. Clinical tools that are able to measure dose appropriateness are sorely needed. The recently developed and validated Opiate Dosage Adequacy Scale (ODAS) comprehensively evaluates the main outcomes relevant for methadone dose optimization, namely relapse, cross-tolerance, objective and subjective withdrawal symptoms, craving and overdose. Based on the ODAS, we developed a new assessment tool (BUprenorphine-naloxone Dosage Adequacy eVAluation [BUDAVA]) for evaluating dosage adequacy in patients in treatment with buprenorphine-naloxone.
Objective: The main goal of this observational study was to explore whether the BUDAVA questionnaire could be used to assess buprenorphine-based, long-term substitution therapy for heroin addiction.
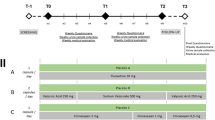
Methods: The study included heroin-dependent patients who had been in treatment with buprenorphine-naloxone for at least 3 months. Patients (n = 196) were recruited from 11 drug abuse treatment centres in Italy. Dosage adequacy was assessed with the BUDAVA questionnaire. Patients classified as inadequately treated had their dosage modified. After 1 week, they were again administered the questionnaire to assess the adequacy of the new dosage.
Results: The buprenorphine-naloxone dosage was found to be inadequate in 61 of the 196 patients. In 13 patients, the treatment scored as inadequate only in the subjective withdrawal symptoms item of the questionnaire and therefore no dosage adjustment was made in the 2 weeks that have characterized this work. The remaining 48 inadequately treated patients had their dosage modified (42 dose increases and six dose decreases). After 1 week on the modified dosage, in 24 of these patients the new regimen was found by the assessment with the questionnaire to be adequate.
Conclusion: These preliminary results suggest that the BUDAVA questionnaire may be useful for guiding buprenorphine-naloxone maintenance dose adjustments in heroin-dependent patients.
Similar content being viewed by others
References
Nicholls L, Bragaw L, Ruetsch C. Opioid dependence treatment and guidelines. J Manag Care Pharm 2010; 16 (1 Suppl. B): S14–21
Donny EC, Brasser SM, Bigelow GE, et al. Methadone doses of 100 mg or greater are more effective than lower doses at suppressing heroin self-administration in opioid-dependent volunteers. Addiction 2005; 100 (10): 1496–509
Donny EC, Walsh SL, Bigelow GE, et al. High-dose methadone produces superior opioid blockade and comparable withdrawal suppression to lower doses in opioid-dependent humans. Psychopharmacology (Berl) 2002; 161 (2): 202–12
Gonzáles-Saiz F. Opiate Dosage Adequacy Scale (ODAS): a clinical diagnostic tool as a guide to dosing decisions. Heroin Addict Relat Clin Probl 2004; 6 (3): 41–50
Gonzáles-Saiz F, Rojas O, Gómez B, et al. Evidence of reliability and validity of the Opiate Dosage Adequacy Scale (ODAS) in a sample of methadone maintenance patients. Heroin Addict Relat Clin Probl 2008; 10 (1): 25–38
Bignamini E, Carboni G, D’Egidio P, et al. Validazione culturale e linguistica del questionario EADO (ODAS) utilizzato per definire l’adeguatezza del dosaggio giornaliero di metadone nel contesto di un programma di mantenimento per il trattamento della dipendenza da oppiacei. Mission 2008; 26 (6): 18
Gardini A, Pöhlke T, Reimer J, et al. Kulturelle und sprachliche Validierung des ODAS (EADO) Fragebogens —eines Instrumentes zur Beurteilung der Angemessenheit der Methadondosierung im Rahmen der Substitutionstherapie Opiatabhängiger. Suchttherapie 2010; 11 (3): 138–40
Lucchini A, D’Egidio P, Bignamini E, et al. Studio METO-DO (Methadone Efficacy Therapy Optimization Dosage Ongoing): i risultati preliminari. Mission 2010; 32: 4–13
Lucchini A, D’Egidio P, Bignamini E, et al. La scala ODAS in un campione di eroinomani in trattamento con buprenorfina nei Ser. T. italiani: uno studio di validazione ed affidabilità. Mission 2010; 32: 15–26
Johnson RE, Strain EC, Amass L. Buprenorphine: how to use it right. Drug Alcohol Depend 2003; 70 (2 Suppl.): S59–77
Stotts AL, Dodrill CL, Kosten TR. Opioid dependence treatment: options in pharmacotherapy. Expert Opin Pharmacother 2009; 10 (11): 1727–40
Amato P. Clinical experience with fortnightly buprenorphine/naloxone versus buprenorphine in Italy: preliminary observational data in an office-based setting. Clin Drug Investig 2010; 30 Suppl. 1: 33–9
Reckitt Benkiser Pharmaceuticals. Buprenorphine-naloxone: summary of product characteristics [online]. Available from URL: http://www.ema.europa.eu [Accessed 2011 Sep 15]
Diagnostic and statistical manual of mental disorders, 4th edition, text revision (DSM-IV-TR)200). Washing, DC: American Psychiatry Association (APA), 2000
Leri F, Bruneau J, Stewart J. Understanding polydrug use: review of heroin and cocaine co-use. Addiction 2003; 98 (1): 7–22
McCance-Katz EF, Rainey PM, Moody DE. Effect of cocaine use on buprenorphine pharmacokinetics in humans. Am J Addict 2009; 19: 38–46
Handelsman L, Cochrane KJ, Aronson MJ, et al. Two new rating scales for opiate withdrawal. Am J Drug Alcohol Abuse 1987; 13 (3): 293–308
Wesson DR, Ling W. The Clinical Opiate Withdrawal Scale (COWS). J Psychoactive Drugs 2003; 35 (2): 253–9
Acknowledgements
We thank Jane Caple of inScience Communications, Springer Healthcare, who provided medical writing assistance and English language editing. This assistance was funded by Reckitt Benkiser.
The authors have no conflicts of interest that are directly relevant to the content of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
D’Amore, A., Romano, F., Biancolillo, V. et al. Evaluation of Buprenorphine Dosage Adequacy in Opioid Receptor Agonist Substitution Therapy for Heroin Dependence. Clin Drug Investig 32, 427–432 (2012). https://doi.org/10.2165/11633230-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11633230-000000000-00000