Abstract
Given rising healthcare costs and a growing population of patients with chronic kidney disease (CKD), there is an urgent need to identify health interventions that provide good value for money.
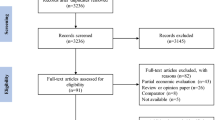
For this review, the English-language literature was searched for studies of interventions in CKD reporting an original incremental cost-utility (cost per QALY) or cost-effectiveness (cost per life-year) ratio. Published cost studies that did not report cost-effectiveness or cost-utility ratios were also reviewed. League tables were then created for both cost-utility and cost-effectiveness ratios to assess interventions in patients with stage 1–4 CKD, waitlist and transplant patients and those with end-stage renal disease (ESRD). In addition, the percentage of cost-saving or dominant interventions (those that save money and improve health) was compared across these three disease categories.
A total of 84 studies were included, contributing 72 cost-utility ratios, 20 cost-effectiveness ratios and 42 other cost measures. Many of the interventions were dominant over the comparator, indicating better health outcomes and lower costs. For the three disease categories, the greatest number of dominant or cost-saving interventions was reported for stage 14 CKD patients, followed by waitlist and transplant recipients and those with ESRD (91%, 87% and 55% of studies reporting a dominant or cost-saving intervention, respectively).
There is evidence of opportunities to lower costs in the treatment of patients with CKD, while either improving or maintaining the quality of care. In order to realize these cost savings, efforts will be required to promote and effectively implement changes in treatment practices.






Similar content being viewed by others
References
Coresh J, Selvin E, Stevens LA, et al. Prevalence of chronic kidney disease in the United States. JAMA 2007 Nov 7; 298 (17): 2038–47
Eknoyan G, Levin NW. K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Am J Kidney Dis 2002 Feb; 39 (2 Suppl. 1): S1–266
S Renal Data System 2008 annual data report: atlas of chronic kidney disease and end-stage renal disease in the United States. USRDS 2008 [online]. Available from URL: http://www.usrds.org/atlas.htm [Accessed 2009 Aug 14]
Grassmann A, Gioberge S, Moeller S, et al. ESRD patients in 2004: global overview of patient numbers, treatment modalities and associated trends. Nephrol Dial Transplant 2005; 20 (12): 2587–93
Hoerger TJ, Wittenborn JS, Segel JE, et al. A health policy model of CKD: 1. Model construction, assumptions, and validation of health consequences. Am J Kidney Dis 2010 Mar; 55 (3): 452–62
Hoerger TJ, Wittenborn JS, Segel JE, et al. A health policy model of CKD: 2. The cost-effectiveness of microalbuminuria screening. Am J Kidney Dis 2010 Mar; 55 (3): 463–73
Centers for Medicare and Medicaid Services. End stage renal disease (ESRD) payment. Baltimore (MD): CMS, 2010 [online]. Available from URL: http://www.cms.gov/ESRDPayment/ [Accessed 2011 Apr 25]
Sullivan SD, Watkins J, Sweet B, et al. Health technology assessment in health-care decisions in the United States. Value Health 2009 Jun; 12 Suppl. 2: S39–44
Federal Coordinating Council for Comparative Effectiveness Research. Federal Coordinating Council for Comparative Effectiveness Research, report to the President and Congress. Washington, DC: US Department of Health and Human Services, 2009 Jun 30 [online]. Available from URL: http://www.hhs.gov/recovery/programs/cer/cerannualrpt.pdf [Accessed 2010 Mar 31]
Vogel S. Benefits of early utilization of intravenous iron. Nephrol Nurs J 2000 Feb; 27 (1): 61–5
Duh MS, Weiner JR, White LA, et al. Management of anaemia: a critical and systematic review of the cost effectiveness of erythropoiesis-stimulating agents. Pharmacoeconomics 2008; 26 (2): 99–120
Garside R, Pitt M, Anderson R, et al. The effectiveness and cost-effectiveness of cinacalcet for secondary hyperparathyroidism in end-stage renal disease patients on dialysis: a systematic review and economic evaluation. Health Technol Assess 2007 May; 11 (18): iii, xi-iii, 167
Manns B, Stevens L, Miskulin D, et al. A systematic review of sevelamer in ESRD and an analysis of its potential economic impact in Canada and theUnited States. Kidney Int 2004 Sep; 66 (3): 1239–47
Komenda P, Levin A, Manns B. The economics of home nocturnal hemodialysis: how should we cost the benefits? Clin Nephrol 2007 Sep; 68 (3): 151–8
Tufts Medical Center, Institute for Clinical Research and Health Policy Studies. The cost-effectiveness analysis registry. Tufts Medical Center, Institute for Clinical Research and Health Policy Studies, 2009 [online]. Available from URL: https://research.tufts-nemc.org/cear/default.aspx [Accessed 2009 Sep 1]
UK NHS, National Institute for Health Research. Centre for Reviews and Dissemination economic evaluations database [online]. Available from URL: http://www.crd.york.ac.uk/crdweb/ [Accessed 2009 Jan 2]
Boulware LE, Jaar BG, Tarver-Carr ME, et al. Screening for proteinuria in US adults: a cost-effectiveness analysis. JAMA 2003 Dec 17; 290 (23): 3101–14
Clark WF, Churchill DN, Forwell L, et al. To pay or not to pay? A decision and cost-utility analysis of angiotensinconverting-enzyme inhibitor therapy for diabetic nephropathy. CMAJ 2000 Jan 25; 162 (2): 195–8
Cleemput I, Kesteloot K, Vanrenterghem Y, et al. The economic implications of non-adherence after renal transplantation. Pharmacoeconomics 2004; 22 (18): 1217–34
Douzdjian V, Ferrara D, Silvestri G. Treatment strategies for insulin-dependent diabetics with ESRD: a cost-effectiveness decision analysis model. Am J Kidney Dis 1998 May; 31 (5): 794–802
Gonzalez-Perez JG, Vale L, Stearns SC, et al. Hemodialysis for end-stage renal disease: a cost-effectiveness analysis of treatment-options. Int J Technol Assess Health Care 2005; 21 (1): 32–9
Hogan TJ, Elliott WJ, Seto AH, et al. Antihypertensive treatment with and without benazepril in patients with chronic renal insufficiency: a US economic evaluation. Pharmacoeconomics 2002; 20 (1): 37–47
Kontodimopoulos N, Niakas D. An estimate of lifelong costs and QALYs in renal replacement therapy based on patients’ life expectancy. Health Policy 2008 Apr; 86 (1): 85–96
Lindsay RM. The London, Ontario, daily/nocturnal hemodialysis study. Semin Dial 2004 Mar; 17 (2): 85–91
Matas AJ, Schnitzler M. Payment for living donor (vendor) kidneys: a cost-effectiveness analysis. Am J Transplant 2003; 4 (2): 216–21
McEwan P, Baboolal K, Conway P, et al. Evaluation of the cost-effectiveness of sirolimus versus cyclosporin for immunosuppression after renal transplantation in the United Kingdom. Clin Ther 2005 Nov; 27 (11): 1834–46
McEwan P, Dixon S, Baboolal K, et al. Evaluation of the cost effectiveness of sirolimus versus tacrolimus for immunosuppression following renal transplantation in the UK. Pharmacoeconomics 2006; 24 (1): 67–79
McFarlane PA, Bayoumi AM, Pierratos A, et al. The quality of life and cost utility of home nocturnal and conventional incenter hemodialysis. Kidney Int 2003 Sep; 64 (3): 1004–11
McFarlane PA, Bayoumi AM, Pierratos A, et al. The impact of home nocturnal hemodialysis on end-stage renal disease therapies: a decision analysis. Kidney Int 2006 Mar; 69 (5): 798–805
McLaughlin K, Manns B, Nickerson P. The routine use of high-resolution immunological screening of recipients of primary deceased donor kidney allografts is cost-effective. Transplantation 2006 May 15; 81 (9): 1278–84
Mendeloff J, Ko K, Roberts MS, et al. Procuring organ donors as a health investment: how much should we be willing to spend? Transplantation 2004 Dec 27; 78 (12): 1704–10
Mutinga N, Brennan DC, Schnitzler MA. Consequences of eliminating HLA-B in deceased donor kidney allocation to increase minority transplantation. Am J Transplant 2005 May; 5 (5): 1090–8
Palmer AJ, Chen R, Valentine WJ, et al. Cost-consequence analysis in a French setting of screening and optimal treatment of nephropathy in hypertensive patients with type 2 diabetes. Diabetes Metab 2006 Feb; 32 (1): 69–76
Roels L, Kalo Z, Boesebeck D, et al. Cost-benefit approach in evaluating investment into donor action: the German case. Transpl Int 2003 May; 16 (5): 321–6
Rosen AB, Hamel MB, Weinstein MC, et al. Cost-effectiveness of full Medicare coverage of angiotensin-converting enzyme inhibitors for beneficiaries with diabetes. Ann Intern Med 2005 Jul 19; 143 (2): 89–99
Schweitzer EJ, Perencevich EN, Philosophe B, et al. Estimated benefits of transplantation of kidneys from donors at increased risk for HIV or hepatitis C infection. Am J Transplant 2007 Jun; 7 (6): 1515–25
Sennfalt K, Magnusson M, Carlsson P. Comparison of hemodialysis and peritoneal dialysis: a cost-utility analysis. Perit Dial Int 2002 Jan; 22 (1): 39–47
Takahashi T, Reed SD, Schulman KA. Cost-effectiveness of the oral adsorbent AST-120 versus placebo for chronic kidney disease. Nephrology (Carlton) 2008 Oct; 13 (5): 419–27
Whiting JF, Kiberd B, Kalo Z, et al. Cost-effectiveness of organ donation: evaluating investment into donor action and other donor initiatives. Am J Transplant 2004 Apr; 4 (4): 569–73
Klarenbach SW, Pannu N, Tonelli MA, et al. Cost-effectiveness of hemofiltration to prevent contrast nephropathy in patients with chronic kidney disease. Crit Care Med 2006 Apr; 34 (4): 1044–51
Manns B, Meltzer D, Taub K, et al. Illustrating the impact of including future costs in economic evaluations: an application to end-stage renal disease care. Health Econ 2003 Nov; 12 (11): 949–58
Jassal SV, Krahn MD, Naglie G, et al. Kidney transplantation in the elderly: a decision analysis. J Am Soc Nephrol 2003 Jan; 14 (1): 187–96
Palmer AJ, Valentine WJ, Chen R, et al. A health economic analysis of screening and optimal treatment of nephropathy in patients with type 2 diabetes and hypertension in the USA. Nephrol Dial Transplant 2008 Apr; 23 (4): 1216–23
Glenngard AH, Persson U, Schon S. Cost-effectiveness analysis of treatment with epoietin-alpha for patients with anaemia due to renal failure: the case of Sweden. Scand J Urol Nephrol 2008; 42 (1): 66–73
Lee CP. An empirical estimate of the value of life: updating the renal dialysis cost-effectiveness standard. Value Health 2009; 12 (1): 80–7
Brennan A, Akehurst R, Davis S, et al. The cost-effectiveness of lanthanum carbonate in the treatment of hyperphosphatemia in patients with end-stage renal disease. Value Health 2007 Jan; 10 (1): 32–41
Kroeker A, Clark WF, Heidenheim AP, et al. An operating cost comparison between conventional and home quotidian hemodialysis. Am J Kidney Dis 2003 Jul; 42 (1 Suppl.): 49–55
Tonelli M, Winkelmayer WC, Jindal KK, et al. The costeffectiveness of maintaining higher hemoglobin targets with erythropoietin in hemodialysis patients. Kidney Int 2003 Jul; 64 (1): 295–304
de Wit GA, Ramsteijn PG, de Charro FT. Economic evaluation of end stage renal disease treatment. Health Policy 1998 Jun; 44 (3): 215–32
Quinn RR, Naimark DM, Oliver MJ, et al. Should hemodialysis patients with atrial fibrillation undergo systemic anticoagulation? A cost-utility analysis. Am J Kidney Dis 2007 Sep; 50 (3): 421–32
Lee CP, Zenios SA, Chertow GM. Cost-effectiveness of frequent in-center hemodialysis. J Am Soc Nephrol 2008 Sep; 19 (9): 1792–7
Lee CP, Chertow GM, Zenios SA. A simulation model to estimate the cost and effectiveness of alternative dialysis initiation strategies. Med Decis Making 2006 Sep; 26 (5): 535–49
Manns B, Klarenbach S, Lee H, et al. Economic evaluation of sevelamer in patients with end-stage renal disease. Nephrol Dial Transplant 2007 Oct; 22 (10): 2867–78
Manns B, Tonelli M, Shrive F, et al. Sevelamer in patients with end-stage renal disease: a systematic review and economic evaluation. Ottawa (ON): Canadian Agency for Drugs and Technologies in Health, 2006. Technology report no. 71
Carides GW, Shahinfar S, Dasbach EJ, et al. The impact of losartan on the lifetime incidence of end-stage renal disease and costs in patients with type 2 diabetes and nephropathy. Pharmacoeconomics 2006; 24 (6): 549–58
Costa-Scharplatz M, van Asselt AD, Bachmann LM, et al. Cost-effectiveness of pharmacogenetic testing to predict treatment response to angiotensin-converting enzyme inhibitor. Pharmacogenet Genomics 2007 May; 17 (5): 359–68
Coyle D, Rodby R, Soroka S, et al. Cost-effectiveness of irbesartan 300 mg given early versus late in patients with hypertension and a history of type 2 diabetes and renal disease: a Canadian perspective. Clin Ther 2007 Jul; 29 (7): 1508–23
Littlewood KJ, Greiner W, Baum D, et al. Adjunctive treatment with moxonidine versus nitrendipine for hypertensive patients with advanced renal failure: a cost-effectiveness analysis. BMC Nephrol 2007 Jul 24; 8: 9
McLaughlin K, Manns B, Culleton B, et al. An economic evaluation of early versus late referral of patients with progressive renal insufficiency. Am J Kidney Dis 2001 Nov; 38 (5): 1122–8
Palmer AJ, Annemans L, Roze S, et al. Cost-effectiveness of early irbesartan treatment versus control (standard antihypertensive medications excluding ACE inhibitors, other angiotensin-2 receptor antagonists, and dihydropyridine calcium channel blockers) or late irbesartan treatment in patients with type 2 diabetes, hypertension, and renal disease. Diabetes Care 2004 Aug; 27 (8): 1897–903
Palmer AJ, Valentine WJ, Ray JA, et al. Health economic implications of irbesartan treatment versus standard blood pressure control in patients with type 2 diabetes, hypertension and renal disease: a Hungarian analysis. Eur J Health Econ 2007 Jun; 8 (2): 161–8
Rodby RA, Chiou CF, Borenstein J, et al. The cost-effectiveness of irbesartan in the treatment of hypertensive patients with type 2 diabetic nephropathy. Clin Ther 2003 Jul; 25 (7): 2102–19
Huybrechts KF, Caro JJ, Wilson DA, et al. Health and economic consequences of sevelamer use for hyperphosphatemia in patients on hemodialysis. Value Health 2005 Sep; 8 (5): 549–61
Schon D, Blume SW, Niebauer K, et al. Increasing the use of arteriovenous fistula in hemodialysis: economic benefits and economic barriers. Clin J Am Soc Nephrol 2007 Mar; 2 (2): 268–76
Lefebvre P, Duh MS, Mody SH, et al. The economic impact of epoetin alfa therapy on delaying time to dialysis in elderly patients with chronic kidney disease. Dis Manag 2007 Feb; 10 (1): 37–45
Loubeau PR, Loubeau JM, Jantzen R. The economics of kidney transplantation versus hemodialysis. Prog Transplant 2001 Dec; 11 (4): 291–7
Schnitzler MA, Woodward RS, Lowell JA, et al. Economics of the antithymocyte globulins thymoglobulin and atgam in the treatment of acute renal transplant rejection. Pharmacoeconomics 2000 Mar; 17 (3): 287–93
Lee H, Manns B, Taub K, et al. Cost analysis of ongoing care of patients with end-stage renal disease: the impact of dialysis modality and dialysis access. Am J Kidney Dis 2002 Sep; 40 (3): 611–22
Shih YC, Guo A, Just PM, et al. Impact of initial dialysis modality and modality switches on Medicare expenditures of end-stage renal disease patients. Kidney Int 2005 Jul; 68 (1): 319–29
Mohr PE, Neumann PJ, Franco SJ, et al. The case for daily dialysis: its impact on costs and quality of life. Am J Kidney Dis 2001 Apr; 37 (4): 777–89
McFarlane PA, Pierratos A, Redelmeier DA. Cost savings of home nocturnal versus conventional in-center hemodialysis. Kidney Int 2002 Dec; 62 (6): 2216–22
Emparan C, Wolters H, Laukotte M, et al. The cost-effectiveness of basiliximab induction in old-to-old kidney transplant programs: Bayesian estimation, simulation, and uncertainty analysis. Transplant Proc 2005 Jun; 37 (5): 2069–71
Ruggenenti P, Pagano E, Tammuzzo L, et al. Ramipril prolongs life and is cost effective in chronic proteinuric nephropathies. Kidney Int 2001 Jan; 59 (1): 286–94
Herman WH, Shahinfar S, Carides GW, et al. Losartan reduces the costs associated with diabetic end-stage renal disease: the RENAAL study economic evaluation. Diabetes Care 2003 Mar; 26 (3): 683–7
Plantinga LC, Fink NE, Jaar BG, et al. Attainment of clinical performance targets and improvement in clinical outcomes and resource use in hemodialysis care: a prospective cohort study. BMC Health Serv Res 2007 Jan 9; 7 (5): 5–18
Manns B, Tonelli M, Yilmaz S, et al. Establishment and maintenance of vascular access in incident hemodialysis patients: a prospective cost analysis. J Am Soc Nephrol 2005 Jan; 16 (1): 201–9
Brophy DF, Wallace JF, Kennedy DT, et al. Cost-effectiveness of sevelamer versus calcium carbonate plus atorvastatin to reduce LDL in patients with chronic renal insufficiency with dyslipidemia and hyperphosphatemia. Pharmacotherapy 2000 Aug; 20 (8): 950–7
Besarab A, Reyes CM, Hornberger J. Meta-analysis of subcutaneous versus intravenous epoetin in maintenance treatment of anemia in hemodialysis patients. Am J Kidney Dis 2002 Sep; 40 (3): 439–46
Hardinger KL, Schnitzler MA, Koch MJ, et al. Cyclosporine minimization and cost reduction in renal transplant recipients receiving a C2-monitored, cyclosporine-based quadruple immunosuppressive regimen. Transplantation 2004 Oct 27; 78 (8): 1198–203
Taal MW, van Zyl-Smit R. Cost-effectiveness of hepatitis B vaccination in haemodialysis patients. S Afr Med J 2001 Apr; 91 (4): 340–4
Alexander CM, Lyle PA, Keane WF, et al. Losartan and the United States costs of end-stage renal disease by baseline albuminuria in patients with type 2 diabetes and nephropathy. Kidney Int Suppl. 2004 Nov; (92): S115–7
Soroka SD, Kiberd BA, Jacobs P. The marginal cost of satellite versus in-center hemodialysis. Hemodial Int 2005 Apr; 9 (2): 196–201
Saab S, Weston SR, Ly D, et al. Comparison of the cost and effectiveness of two strategies for maintaining hepatitis B immunity in hemodialysis patients. Vaccine 2002 Aug 19; 20 (25-26): 3230–5
Dominguez J, Fuenzalida D, Norambuena R, et al. C2 monitoring of cyclosporine in stable renal transplant patients results in lower costs and improved renal function. Transplant Proc 2005 Apr; 37 (3): 1583–5
Yen EF, Hardinger K, Brennan DC, et al. Cost-effectiveness of extending Medicare coverage of immunosuppressive medications to the life of a kidney transplant. Am J Transplant 2004 Oct; 4 (10): 1703–8
Chuang FR, Lee CH, Chang HW, et al. A quality and costbenefit analysis of dialyzer reuse in hemodialysis patients. Ren Fail 2008; 30 (5): 521–6
Churchill DN, Macarios D, Attard C, et al. Costs associated with erythropoiesis-stimulating agent administration to hemodialysis patients. Nephron Clin Pract 2007; 106 (4): c193–8
Orme ME, Jurewicz WA, Kumar N, et al. The cost effectiveness of tacrolimus versus microemulsified cyclosporin: a 10-year model of renal transplantation outcomes. Pharmacoeconomics 2003; 21 (17): 1263–76
Roderick P, Armitage A, Nicholson T, et al. A clinical and cost evaluation of hemodialysis in renal satellite units in England and Wales. Am J Kidney Dis 2004 Jul; 44 (1): 121–31
White CA, Jaffey J, Magner P. Cost of applying the K/DOQI guidelines for bone metabolism and disease to a cohort of chronic hemodialysis patients. Kidney Int 2007 Feb; 71 (4): 312–7
Dykstra DM, Beronja N, Menges J, et al. ESRD managed care demonstration: financial implications. Health Care Financ Rev 2003; 24 (4): 59–75
Tonelli M, Klarenbach S, Jindal K, et al. Economic implications of screening strategies in arteriovenous fistulae. Kidney Int 2006 Jun; 69 (12): 2219–26
Chang CF, Winsett RP, Gaber AO, et al. Cost-effectiveness of post-transplantation quality of life intervention among kidney recipients. Clin Transplant 2004 Aug; 18 (4): 407–14
Lacson Jr E, Ikizler TA, Lazarus JM, et al. Potential impact of nutritional intervention on end-stage renal disease hospitalization, death, and treatment costs. J Ren Nutr 2007 Nov; 17 (6): 363–71
Trivedi HS, Pang MM, Campbell A, et al. Slowing the progression of chronic renal failure: economic benefits and patients’ perspectives. Am J Kidney Dis 2002 Apr; 39 (4): 721–9
Hynes DM, Stroupe KT, Greer JW, et al. Potential cost savings of erythropoietin administration in end-stage renal disease. Am J Med 2002 Feb 15; 112 (3): 169–75
Gerth WC, Remuzzi G, Viberti G, et al. Losartan reduces the burden and cost of ESRD: public health implications from the RENAAL study for the European Union. Kidney Int Suppl. 2002 Dec; (82): S68–72
Ortega T, Ortega F, Diaz-Corte C, et al. The timely construction of arteriovenous fistulae: a key to reducing morbidity and mortality and to improving cost management. Nephrol Dial Transplant 2005 Mar; 20 (3): 598–603
Narayan R, Perkins RM, Berbano EP, et al. Parathyroidectomy versus cinacalcet hydrochloride-based medical therapy in the management of hyperparathyroidism in ESRD: a cost utility analysis. Am J Kidney Dis 2007 Jun; 49 (6): 801–13
Sack K. US cost-saving policy forces new kidney transplant. New York Times 2009 Sep 13 [online]. Available from URL: http://www.nytimes.com/2009/09/14/health/policy/14kidney.html [Accessed 2009 Sep 13]
Lacson Jr E, Wang W, Lazarus JM, et al. Hemodialysis facility-based quality-of-care indicators and facility-specific patient outcomes. Am J Kidney Dis 2009 Sep; 54 (3): 490–7
Rocco MV, Frankenfield DL, Hopson SD, et al. Relationship between clinical performance measures and outcomes among patients receiving long-term hemodialysis. Ann Intern Med 2006 Oct 3; 145 (7): 512–9
Tentori F, Hunt WC, Rohrscheib M, et al. Which targets in clinical practice guidelines are associated with improved survival in a large dialysis organization? J Am Soc Nephrol 2007 Aug; 18 (8): 2377–84
Leikis MJ, Kent AB, Becker GJ, et al. Haemoglobin response to subcutaneous versus intravenous epoetin alfa administration in iron-replete haemodialysis patients. Nephrology (Carlton) 2004 Jun; 9 (3): 153–60
Pizzarelli F, David S, Sala P, et al. Iron-replete hemodialysis patients do not require higher EPO dosages when converting from subcutaneous to intravenous administration: results of the Italian Study on Erythropoietin Converting (ISEC). Am J Kidney Dis 2006 Jun; 47 (6): 1027–35
Collins AJ. Cardiovascular mortality in end-stage renal disease. Am J Med Sci 2003 Apr; 325 (4): 163–7
Curtis BM, Levin A, Parfrey PS. Multiple risk factor intervention in chronic kidney disease: management of cardiac disease in chronic kidney disease patients. Med Clin North Am 2005 May; 89 (3): 511–23
Charytan D, Kuntz RE. The exclusion of patients with chronic kidney disease from clinical trials in coronary artery disease. Kidney Int 2006 Dec; 70 (11): 2021–30
Kalantar-Zadeh K, Block G, Humphreys MH, et al. Reverse epidemiology of cardiovascular risk factors in maintenance dialysis patients. Kidney Int 2003 Mar; 63 (3): 793–808
Wanner C, Krane V, Marz W, et al. Atorvastatin in patients with type 2 diabetes mellitus undergoing hemodialysis. N Engl J Med 2005 Jul 21; 353 (3): 238–48
Fellstrom BC, Jardine AG, Schmieder RE, et al. Rosuvastatin and cardiovascular events in patients undergoing hemodialysis. N Engl J Med 2009 Apr 2; 360 (14): 1395–407
Kausz AT, Guo H, Pereira BJ, et al. General medical care among patients with chronic kidney disease: opportunities for improving outcomes. J Am Soc Nephrol 2005 Oct; 16 (10): 3092–101
Chow I, Lemos EV, Einarson TR. Management and prevention of diabetic foot ulcers and infections: a health economic review. Pharmacoeconomics 2008; 26 (12): 1019–35
Javitt JC, Aiello LP, Chiang Y, et al. Preventive eye care in people with diabetes is cost-saving to the federal government: implications for health-care reform. Diabetes Care 1994 Aug; 17 (8): 909–17
Zoungas S, Kerr PG, Lui M, et al. The impact of glycaemic control on outcomes in patients with end-stage renal disease and type 2 diabetes. Nephrology (Carlton) 2008 Apr; 13 (2): 124–7
McMurray SD, Johnson G, Davis S, et al. Diabetes education and care management significantly improve patient outcomes in the dialysis unit. Am J Kidney Dis 2002 Sep; 40 (3): 566–75
Philipneri MD, Rocca Rey LA, Schnitzler MA, et al. Delivery patterns of recommended chronic kidney disease care in clinical practice: administrative claims-based analysis and systematic literature review. Clin Exp Nephrol 2008 Feb; 12 (1): 41–52
Medicare Improvements for Patients and Providers Act of 2008. Medicare, provisions to relating to part B, other payment and coverage improvements. US Congress 2010 [online]. Available from URL: http://frwebgate.access.gpo.gov/cgi-bin/getdoc.cgi?dbname=110_cong_bills&docid=f:h6331enr.txt.pdf [Accessed 2010 Feb 9]
Weiner DE, Watnick SG. The 2009 proposed rule for prospective ESRD payment: historical perspectives and public policies. Bundle up! Am J Kidney Dis 2010 Feb; 55 (2): 217–22
Desai AA, Bolus R, Nissenson A, et al. Is there ‘cherry picking’ in the ESRD Program? Perceptions from a dialysis provider survey. Clin J Am Soc Nephrol 2009 Apr; 4 (4): 772–7
Dubose Jr TD, Behrens MT, Berns A, et al. The patientcentered medical home and nephrology. J Am Soc Nephrol 2009 Apr; 20 (4): 681–2
Gilbody S, Bower P, Sutton AJ. Randomized trials with concurrent economic evaluations reported unrepresentatively large clinical effect sizes. J Clin Epidemiol 2007 Aug; 60 (8): 781–6
Bell CM, Urbach DR, Ray JG, et al. Bias in published cost effectiveness studies: systematic review. BMJ 2006 Mar 25; 332 (7543): 699–703
Fleurence RL, Spackman DE, Hollenbeak C. Does the funding source influence the results in economic evaluations? A case study in bisphosphonates for the treatment of osteoporosis. Pharmacoeconomics 2010 Apr 1; 28 (4): 295–306
Ligthart S, Vlemmix F, Dendukuri N, et al. The cost-effectiveness of drug-eluting stents: a systematic review. CMAJ 2007 Jan 16; 176 (2): 199–205
Neumann PJ. Using cost-effectiveness analysis to improve health care: opportunities and barriers. Oxford: Oxford University Press, Inc., 2005
US Department of Health and Human Services. Draft definition, prioritization criteria, and strategic framework for public comment: draft definition of comparative effectiveness research for the Federal Coordinating Council [online]. Available from URL: http://www.hhs.gov/recovery/programs/cer/draftdefinition.html [Accessed 2009 Jun 22]
Neumann PJ. Costing and perspective in published costeffectiveness analysis. Med Care 2009 Jul; 47 (7 Suppl. 1): S28–32
Neumann PJ, Fang CH, Cohen JT. 30 years of pharmaceutical cost-utility analyses: growth, diversity and methodological improvement. Pharmacoeconomics 2009; 27 (10): 861–72
Acknowledgements
Funding for this study was provided by Amgen. Aside from the participation of Dr Agodoa, the sponsor had no role in study design and concept or manuscript preparation. The publication of this study was not contingent on sponsor approval of the manuscript. Dr Menzin and Ms Lines, Nichols and Rodriguez received funding from the sponsor. Dr Weiner receives research funding from the American Society of Nephrology, Dialysis Clinic, Inc., and Covidien; he previously received funding from Amgen. Dr Neumann received honoraria for his participation in advisory boards sponsored by Amgen and Genzyme. Dr Agodoa is an employee and stockholder of the sponsor. Dr Mayne is an employee of Davita Clinical Research, and was previously an employee and stockholder of Amgen.
Portions of this analysis were presented in preliminary form at the 42nd Annual Meeting and Scientific Exposition of the American Society of Nephrology in San Diego, CA, USA, 29 October 2009.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Menzin, J., Lines, L.M., Weiner, D.E. et al. A Review of the Costs and Cost Effectiveness of Interventions in Chronic Kidney Disease. Pharmacoeconomics 29, 839–861 (2011). https://doi.org/10.2165/11588390-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11588390-000000000-00000