Summary
Synopsis
Cefixime is an orally active third generation cephalosporin with in vitro antibacterial activity against most important lower respiratory pathogens. The drug is active against Haemophilus influenzae, Moraxella catarrhalis and penicillin-susceptible Streptococcus pneumoniae but not Staphylococcus aureus.
Cefixime has a long elimination half-life (3 hours compared with 0.5 hours for cefaclor and 1.5 hours for cefalexin), which allows once daily administration. Several trials have established the clinical efficacy of the drug in patients with lower respiratory tract infection (LRTI). In comparative studies cefixime had similar efficacy to amoxicillin ± clavulanic acid, cefaclor, cefalexin, cefuroxime axetil and clarithromycin.
Trials evaluating the efficacy of cefixime as the oral component of intravenous to oral switch therapy have produced promising preliminary results although further carefully designed trials are needed in this area.
As with certain other drugs of its class, gastrointestinal disturbances are the most frequently reported adverse events in patients taking cefixime and cases of pseudomembranous colitis have been reported.
Thus, cefixime is an effective treatment for mild to moderate LRTI and may have a role as the oral component of intravenous to oral switch therapy although further well designed studies are needed to confirm initial favourable results in this important emerging area of antibacterial therapy.
Overview of In Vitro Antibacterial Activity
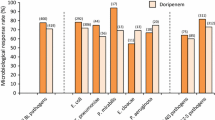
Cefixime has good (MIC ≤0.75 mg/L) in vitro activity against Haemophilus influenzae, Moraxella catarrhalis and penicillin-susceptible (but not penicillin-resistant) Streptococcus pneumoniae, the most common lower respiratory pathogens. Certain acute pneumonia pathogens are susceptible to cefixime including Escherichia coli and Klebsiella pneumoniae, while others, including Bacteroides spp., Peptostreptococcus spp., Enterobacter spp., Pseudomonas aeruginosa, Legionella spp. and Staphylococcus aureus are not.
Pharmacokinetic Properties
Oral administration of cefixime 200mg produces peak plasma concentrations of approximately 2.0 to 2.6 mg/L after 3 to 4 hours. Time to maximal plasma concentrations is lengthened slightly when the drug is given with food. Accumulation did not occur after administration of cefixime 400 mg/day for 15 days to volunteers. Cefixime does not appear to penetrate well into sputum but reaches useful levels in bronchial mucosa (up to 2.4 mg/L). Total systemic clearance was 4.4 L/hour (73 ml/min) after administration of a single 200mg intravenous dose of cefixime to volunteers; renal clearance accounted for 40% of this. Clearance was 9.7 L/h (162 ml/min) after oral administration of a single 200mg dose and 11.4 L/h (190 ml/min) after oral administration of a single 400mg dose. Up to 20% of a 200mg dose is recovered unchanged from the urine over a 24-hour period.
Although maximum plasma concentrations and the area under the plasma concentration versus time curve may be greater in older versus younger patients, the dosage of cefixime does not need to be adjusted according to age. However, elimination half-life and clearance are prolonged in patients with severe renal function impairment and in patients on haemodialysis or continuous ambulatory peritoneal dialysis.
Therapeutic Use in Lower Respiratory Tract Infections
Numerous noncomparative and comparative trials have evaluated the efficacy of cefixime as treatment for lower respiratory tract infection (LRTI). In a large noncomparative multicentre trial in patients with acute bronchitis or acute exacerbations of chronic bronchitis, cefixime produced a clinical cure/improvement rate of 96%. The drug has also shown similar efficacy to amoxicillin/clavulanic acid, cefaclor, cefalexin and cefuroxime axetil in patients with various LRTIs.
Studies conducted solely in patients with community-acquired LRTI have also shown cefixime to be clinically efficacious. Comparative studies in this indication have shown the drug to be as effective as clarithromycin in adults and amoxicillin/clavulanic acid in children. Comparative studies in hospitalised patients with LRTI reported cefixime was as effective as intravenous ceftriaxone or oral cefalexin or amoxicillin.
Three studies have evaluated the use of cefixime as the oral component of cephalosporin-based intravenous to oral switch regimens (a relatively new cost saving strategy) in hospitalised patients with LRTI. Cefixime 400mg once daily administered after a 2- to 3-day course of intravenous ceftizoxime (2 g/day) was clinically effective in 9 patients with severe acute pneumonia. A larger study in this indication also found cefixime to be clinically effective; in this trial cefixime 400mg once daily was given after intravenous ceftizoxime or ceftriaxone. In this study, clear criteria had to be met before the change to oral therapy was made but such criteria were absent in other studies that changed treatment from a parenteral cephalosporin to oral cefixime. 120 patients were enrolled; of these, 45 were withdrawn (many with infections caused by pathogens not susceptible to cefixime). 74 of 75 evaluated patients experienced clinical cure; bacteriological data for these patients were not presented. The sole comparative trial in this indication found cefixime administered after intravenous cefotaxime to be as effective as a full course of intravenous cefotaxime in patients with LRTI of unspecified severity.
Tolerability
Analysis of individual comparative studies reveals that the rate of adverse events in cefixime recipients was generally similar to that in patients who received the comparative drug. However, the overall rate of adverse events in these premarketing studies was generally higher than that obtained in postmarketing trials; this variation is probably largely attributable to methodological differences. Gastrointestinal symptoms, especially diarrhoea, are the most frequent adverse events in patients treated with cefixime. Other adverse events associated with cefixime therapy include skin and appendage symptoms, headache and dizziness. Cases of pseudomembranous colitis associated with administration of the drug have also been reported.
Dosage and Administration
The recommended adult (including children >12 years of age or weighing >50kg) dosage of cefixime is 400 mg/day which may be given as a single daily dose or 200mg every 12 hours. The recommended dosage for children ≤12 years of age or weighing ≤50kg is 8 mg/kg/day (oral suspension). This may be administered as a single daily dose or 4 mg/kg every 12 hours.
The dosage of cefixime should be reduced by 25% (to 300 mg/day) in patients with moderate renal impairment (creatinine clearance 21 to 60 ml/min) or patients undergoing haemodialysis and by 50% (to 200 mg/day) in patients with severe renal impairment (creatinine clearance ≤20 ml/min) or undergoing continuous ambulatory peritoneal dialysis.
Similar content being viewed by others
References
Brogden RN, Campoli-Richards DM. Cefixime: a review of its antibacterial activity, pharmacokinetic properties and therapeutic potential. Drugs 1989; 38: 524–50.
Barry AL, Jones RN. Cefixime: spectrum of antibacterial activity against 16 016 clinical isolates. Pediatr Infect Dis J 1987; 6: 954–7.
Sader HS, Jones RN, Washington JA, et al. In vitro activity of cefpodoxime compared with other oral cephalosporins tested against 5556 recent clinical isolates from five medical centers. Diagn Microbiol Infect Dis 1993; 17: 143–50.
Neu HC, Chick TW. Efficacy and safety of clarithromycin compared to cefixime as outpatient treatment of lower respiratory tract infections. Chest 1993; 104: 1393–9.
Linares J, Alonso T, Pérez JL, et al. Decreased susceptibility of penicillin-resistant pneumococci to twenty-four α-lactam antibiotics. J Antimicrob Chemother 1992; 30: 279–88.
Yokota Y, Teratani N, Ikemoto A, et al. Antibacterial activity of cefixime, cefpodoxime, and cefuroxime against penicillin-G-resistant Streptococcus pneumoniae. J Drug Dev 1993 Nov; 6 Suppl. 1: 1–4.
Spangler SK, Jacobs MR, Pankuch GA, et al. Susceptibility of 170 penicillin-susceptible and penicillin-resistant pneumococci to six oral cephalosporins, four quinolones, desacetylcefotaxime, Ro 23-9424 and RP 67829. J Antimicrob Chemother 1993; 31: 273–80.
Locher R, Strässle A, Kayser FH. In vitro activity of oral cephalosporin BAY v 3522 compared with other oral cephalosporins. Drugs Exp Clin Res 1990; 16: 515–25.
Hodges TL, Eliopoulos GM, Klimm K, et al. In vitro activity of BAY v 3522, a new cephalosporin for oral administration [published erratum appears in Antimicrob Agents Chemother 1990 Nov; 34 (11):2289]. Antimicrob Agents Chemother 1990; 34: 1849–54.
Sultan T, Baltcn AL, Smith RP, et al. In vitro activity of cefdinir (FK482) and ten other antibiotics against gram-positive and gram-negative bacteria isolated from adult and pediatric patients. Chemotherapy Basel 1994; 40: 80–91.
Stefani S, Pellegrino MB, D’Amico G, et al. In vitro activity of a new broad-spectrum, beta-lactamase-stable oral cephalosporin, cefixime, in comparison with other drugs, against Haemophilus influenzae, Haemophilus parainfluenzae, Moraxella catarrhalis and Streptococcus pneumoniae. Chemotherapy Basel 1992; 38: 36–45.
Scriver SR, Willey BM, Low DE, et al. Comparative in vitro activity of cefdinir (CI-983; FK-482) against staphylococci, gram-negative bacilli and respiratory tract pathogens. Eur J Clin Microbiol Infect Dis 1992; 11: 646–52.
Nash DR, Flanagan C, Steele LC, et al. Comparison of the activity of cefixime and activities of other oral antibiotics against adult clinical isolates of Moraxella (Branhamella) catarrhalis containing BRO-1 and BRO-2 and Haemophilus influenzae. Antimicrob Agents Chemother 1991; 35: 192–4.
Thomson KS, Sanders CC, Sanders Jr WE. In vitro studies with Bay v 3522, a new oral cephalosporin. Drugs Exp Clin Res 1991; 17: 165–73.
Lehtonen L, Huovinen P. Susceptibility of respiratory tract pathogens in Finland to cefixime and nine other antimicrobial agents. Scand J Infect Dis 1993; 25 (3): 373–8.
Konno M, Yoshida S, Inoue M, et al. An epidemiological study of penicillin-resistant Streptococcus pneumoniae in Japan [in Japanese]. Kansenshogaku Zasshi 1994; 68: 1338–51.
Barry AL, Pfaller MA, Fuchs PC, et al. In vitro activities of 12 orally administered antimicrobial agents against four species of bacterial respiratory pathogens from U.S. medical centers in 1992 and 1993. Antimicrob Agents Chemother 1994; 38: 2419–25.
Loo VG, Lavellée J, McAlear D, et al. The in-vitro susceptibilities of 326 Streptococcus pneumoniae isolates to nine antimicrobial agents including penicillin and newer quinolones. J Antimicrob Chemother 1994; 33: 641–45.
Donowitz GR, Mandell GL. Acute pneumonia. In: Mandell GL, Douglas Jr RG, Bennett JE, editors. Principles and practice of infectious diseases. 3rd ed. New York: Churchill Livingstone, 1990: 540–55.
Cullmann W, Dick W. Cefpodoxime: comparable evaluation with other orally available cephalosporins. With a note on the role of beta-lactamases. Int J Med Microbiol 1990; 273: 501–17.
Jones RN, Erwin ME, Barrett MS. Antimicrobial activity of three investigational oral cephalosporins (BK-218, cefdinir, and RU29246) against Legionella. Diagn Microbiol Infect Dis 1991; 14: 519–21.
Focht J, Kraus H, Nösner K. In vitro activity of clarithromycin. Efficacy against pathogenic agents of chronic bronchitis and chronic tonsillitis in comparison with other oral antibiotics [in German]. Munch Med Wochenschr 1993; 135: 642–6.
Jolley A, Andrews JM, Brenwald N, et al. The in-vitro activity of a new highly active quinolone, DU-6859a. J Antimicrob Chemother 1993; 32: 757–63.
Chin NX, Yu KW, Neu HC. Antimicrobial activity and beta-lactamase stability of BMY-28232, parent compound of an oral cephalosporin. Eur J Clin Microbiol Infect Dis 1990; 9: 841–6.
Dance DAB, Wuthiekanun V, Chaowagul W, et al. The antimicrobial susceptibility of Pseudomonas pseudomallei. Emergence of resistance in vitro and during treatment. J Antimicrob Chemother 1989; 24: 295–309.
Dhib M, Moulin B, Leroy A, et al. Relationship between renal function and disposition of oral cefixime. Eur J Clin Pharmacol 1991; 41: 579–83.
Faulkner RD, Bohaychuck W, Haynes JD, et al. The pharmacokinetics of cefixime in the fasted and fed state. Eur J Clin Pharmacol 1988; 34: 525–8.
Hayashi I. Serum and. sputum concentration and clinical results of cefixime on respiratory tract infection. Chemotherapy 1985; 33 Suppl. 6: 253–67.
Maesen FPV, Costongs R, Davies BI. Concentrations of cefixime in bronchial mucosa and sputum. Thorax 1990; 45: 982.
Baldwin DR, Andrews JM, Ashby JP, et al. Concentrations of cefixime in bronchial mucosa and sputum after three oral multiple dose regimens. Thorax 1990; 45: 401–2.
Faulkner RD, Fernandez P, Lawrence G, et al. Absolute bioavailability of cefixime in man. J Clin Pharmacol 1988; 28: 700–6.
Faulkner RD, Bohaychuck W, Desjardins RE, et al. Pharmacokinetics of cefixime after once-a-day and twice-a-day dosing to steady state. J Clin Pharmacol 1987; 27: 807–12.
Silber DM, Bohaychuk W, Stout M, et al. Pharmacokinetics of cefixime in young and elderly volunteers. Workshop. 15th International Congress of Chemotherapy, Jul 87. Advances in Experimental and Clinical Chemotherapy 1988; 1: 18–20.
Guay DRP, Meatherall RC, Harding GK, et al. Pharmacokinetics of cefixime (CL 284,635; FK 027) in healty subjects and patients with renal insufficiency. Antimicrob Agents Chemother 1986; 30: 485–90.
Stratton CW. Efficacy and safety of cefixime for the empiric therapy of acute bronchitis and AECB. Infect Med 1993; 10 Suppl. D: 11–5.
Beumer HM. Cefixime versus amoxicillin/clavulanic acid in lower respiratory tract infections. Int J Clin Pharmacol Ther Toxicol 1989; 27: 30–3.
Dorow P. Safety and efficacy of cefixime versus cefaclor in respiratory tract infections. J Chemother 1989; 1: 257–60.
Verghese A, Roberson D, Kalbfleisch JH, et al. Randomized comparative study of cefixime versus cephalexin in acute bacterial exacerbations of chronic bronchitis. Antimicrob Agents Chemother 1990; 34: 1041–4.
Drehobl M, Sahn S, Puopolo A, et al. A multicenter trial of cefixime and cefuroxime axetil in the treatment of acute LRTI. Infect Med 1993; 10 Suppl. D: 22–8.
Heinz G, Greene S, Haddow A, et al. Comparison of cefixime and cefaclor in acute LRTI: two randomized studies. Infect Med 1993; 10 Suppl. D: 29–35.
Kiani R, Coulson L, Johnson D, et al. Comparison of once-daily and twice-daily cefixime regimens with amoxicillin in the treatment of acute lower respiratory tract infections. Curr Ther Res 1990; 48: 841–52.
Wallace Jr RJ, Brown BA, Stocks JM, et al. Comparison of cefixime and amoxicillin/clavulanic acid in LRTI. Infect Med 1993; 10 Suppl. D: 16–21.
Maesen FPV, Davies BI, Path FRC, et al. Cefixime in acute exacerbations of bronchitis — a new disappointment [abstract]. Chest 1991 Aug; 100 Suppl.: 146S.
Lemos L, Barroso A, Coelho A, et al. Cefixime in respiratory infections resistant to previous antibiotic therapy. J Drug Dev 1993 Nov; 6 Suppl. 1: 57–8.
Carrière JP, Trinh A, Darchy L, et al. Effectiveness and safety of cefixime compared with amoxicillin-clavulanate in the treatment of acute bronchopneumonia in paediatrics: results of a multicentre controlled trial. J Drug Dev 1993 Nov; 6 Suppl. 1: 41–3.
Catena E, Mistretta A, Micillo E, et al. Cefixime: comparative clinical trial on the treatment of lower respiratory tract infection in adults. 6th Mediterranean Congress of Chemotherapy 1988; 1 Suppl. 4: 786–8.
Cogo R, Monzani GP, Caiazzo G. Safety and efficacy of cefixime vs ceftriaxone in the treatment of infectious exacerbations of chronic bronchitis. J Drug Dev 1993 Nov; 6 Suppl. 1: 55–6.
Hugues FC, Le Jeunne CL, Benard Y, et al. A controlled, multicentre study of cefixime versus amoxicillin in the treatment of lower respiratory tract infections in adults [in French]. Presse Med 1989; 18: 1600–4.
Matsumoto F, Imai T, Saito A, et al. Double blind comparative study on cefetamet pivoxil vs cefixime in bacterial pneumonia [in Japanese]. Chemotherapy Tokyo 1991; 39: 864–82.
McVey D, Tolcher L, Piper D, et al. An open general practice assessment of cefixime in the treatment of otitis media and acute lower respiratory tract infection in adults and children. Br J Clin Res 1991; 2 (2): 211–21.
Wang F-D, Liu C-Y, Wong W-W, et al. Cefixime in the treatment of acute lower respiratory tract and urinary tract infections. Drug Invest 1992; 4 (1): 34–9.
Donowitz GR, Mandell GL. Cephalosporins. In: Mandell GL, Douglas RG, Bennett JE, editors. Principles and practice of infectious diseases. 3rd ed. New York: Churchill Livingstone, 1990: 246–56.
Neu HC. Do we need the third-generation cephalosporins? J Antimicrob Chemother 1984 Sep 14 Suppl. B: 1–12.
Jewesson P. Cost-effectiveness and value of an IV switch. PharmacoEconomics 1994; 5 Suppl. 2: 20–6.
McCracken Jr GH. New era for orally administered antibiotics: use of sequential parenteral-oral antibiotic therapy for serious infectious diseases of infants and children. Pediatr Infect Dis J 1987; 6: 951–3.
Janknegt R, van der Meer JWM. Antimicrobial practice. Sequential therapy with intravenous and oral cefalosporins. J Antimicrob Chemother 1994; 33: 169–77.
Rimmer D. Third generation cefalosporins in the parenteral to oral switch. PharmacoEconomics 1994; 5 Suppl. 2: 27–33.
Quintiliani R, Cooper BW, Briceland LL, et al. Economic impact of streamlining antibiotic administration. Am J Med 1987; 82 Suppl. 4A: 391–4.
Ramirez JA. Advances in antibiotic therapy: parenteral to oral switch. Clinician 1993; 11: 38–40.
Cahn P, Grinberg N, Kauffman S, et al. Cefixime therapy for the treatment of severe acute pneumonias. J Drug Dev 1993 Nov; 6 Suppl. 1: 59–60.
Ramirez JA, Srinath L, Akee S, et al. Early switch from intravenous to oral cephalosporins in the treatment of hospitalized patients with community-aquired pneumonia. Arch Intern Med 1995; In press.
Vogel F, Bodem G, Kunze M, et al. Efficacy and tolerance of cefotaxime followed by oral cefixime versus cefotaxime alone in patients with lower respiratory tract infections. Curr Ther Res 1994; 55 Suppl. A: 42–8.
Wu DH. A review of the safety profile of cefixime. J Drug Dev 1993 Nov; 6 Suppl. 1: 81–3.
Spilker B. Collecting adverse event and adverse reaction data in clinical trials. In: Spilker B, editor. Guide to clinical trials. New York: Raven Press, 1991: 196–201.
Wilson WR. Tolerance and safety of orally administered antimicrobial agents: an important factor in the selection of drug therapy. Curr Ther Res 1994; 55 Suppl. A: 49–56.
Tröster K, Kraus E, Hostalek U, et al. Post-marketing experiences with cefixime, J Drug Dev 1993 Nov; 6 Suppl. 1: 69–71.
Pimentel FL. Efficacy and safety of cefixime in 1,891 patients with otorhinolaryngologic and paediatric infections. J Drug Dev 1993 Nov; 6 Suppl. 1: 77–9.
Fekety R. Antibiotic-associated colitis. In: Mandell GL, Douglas RG, Bennett JE, editors. Principles and practice of infectious diseases. 3rd ed. New York: Churchill Livingstone, 1990: 863–9.
Wu DH. A review of the safety profile of cefixime. Clin Ther 1993; 15: 1108–19.
Gales MA, Gales BJ. Recognition of severe cefixime-induced diarrhea. Clin Pharm 1993; 12: 881.
Gremse DA, Dean PC, Farquhar DS. Cefixime and antibiotic-associated colitis. Pediatr Infect Dis J 1994; 13: 331–3.
Carbon C, Richard A, Bons B. Antibiotic associated pseudomembranous colitis. Results of a study done with 900 gastroenterologists [in French]. Therapie 1994; 49: 325–31.
American Cyanamid Company. Cefixime prescribing information. Pearl River, New York, USA.
Finch RG. Epidemiological features and chemotherapy of community-acquired respiratory tract infections. J Antimicrob Chemother 1990; 26 Suppl. E: 53–61.
Woodhead M. Pneumonia in the elderly. J Antimicrob Chemother 1994; 34 Suppl. A: 85–92.
Low DE, Scriver SR. Evaluation of the in vitro activity of cefixime for its use in switch therapy. Curr Ther Res 1994; 55 Suppl. A: 35–41.
Author information
Authors and Affiliations
Additional information
Various sections of the manuscript reviewed by: C. Carbon, Service de Medecine Interne, C.H.U. Bichat Claude Bernard, Paris, France; R. Cogo, Department of Pneumology, Ornago Hospital, Milan, Italy; B.I. Davies, Department of Medical Microbiology, De Wever Ziekenhuis, Heerlen, The Netherlands; R.G. Finch, Department of Microbial Diseases, Nottingham City Hospital, Nottingham, England; R.F. Grossman, Division of Respiratory Medicine, Mount Sinai Hospital, Toronto, Ontario, Canada; J.M.T. Hamilton-Miller, Department of Medical Microbiology, Royal Free Hospital, London, England; F.V.P. Maesen, Department of Medical Microbiology, De Wever Ziekenhuis, Heerlen, The Netherlands; Y. Ohsaki, First Department of Internal Medicine, Asahikawa Medical College, Nishikagura, Asahikawa, Japan; J.A. Ramirez, Division of Infectious Diseases, School of Medicine, University of Louisville, Louisville, Kentucky, USA; F. Vögel, Medizinische Klinik III, Kliniken des Main-Taunus-Kreises, Hofheim am Taunus, Germany; R. Wise, Department of Medical Microbiology, City Hospital NHS Trust, Birmingham, England; S.F. Yeo, Department of Medical Microbiology, The London Hospital Medical College, University of London, London, England.
Rights and permissions
About this article
Cite this article
Markham, A., Brogden, R.N. Cefixime. Drugs 49, 1007–1022 (1995). https://doi.org/10.2165/00003495-199549060-00010
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199549060-00010