Abstract
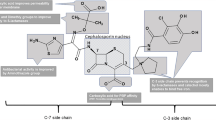
Ceftobiprole, a β-lactam, is the first of a new generation of broad-spectrum cephalosporins in late-stage development with activity against methicillin-resistant Staphylococcus aureus (MRSA) in addition to broad-spectrum bactericidal activity against other Gram-positive and Gram-negative pathogens. The prodrug, ceftobiprole medocaril, is converted rapidly and almost completely to the active drug, ceftobiprole, upon infusion by type A esterases. In humans, ceftobiprole binds minimally (16%) to plasma proteins, and binding is independent of the drug and protein concentrations. Its steady-state volume of distribution (18.4 L) approximates the extracellular fluid volume in humans. Ceftobiprole undergoes minimal hepatic metabolism, and the primary metabolite is the β-lactam ring-opened hydrolysis product (open-ring metabolite). Systemic exposure of the open-ring metabolite accounts for 4% of ceftobiprole exposure following single-dose administration; approximately 5% of the dose is excreted in the urine as the metabolite. Ceftobiprole does not significantly induce or inhibit relevant cytochrome P450 enzymes and is neither a substrate nor an inhibitor of P-glycoprotein. Ceftobiprole is rapidly eliminated, primarily unchanged, by renal excretion, with a terminal elimination half-life of 3 hours; the predominant mechanism responsible for elimination is glomerular filtration, with approximately 89% of the dose being excreted as the prodrug, active drug (ceftobiprole) and open-ring metabolite. The pharmacokinetics of ceftobiprole are linear following single and multiple infusions of 125–1000 mg. Steady-state drug concentrations are attained on the first day of dosing, with no appreciable accumulation when administered three times daily (every 8 hours) and twice daily (every 12 hours) in subjects with normal renal function. Low intersubject variability has been seen across studies. Ceftobiprole exposure is slightly higher (∼15%) in females than in males; this difference has been attributed to bodyweight. However, the pharmacodynamics of ceftobiprole are similar in males and females, and dosing adjustments are not required based on gender. In patients with moderate to severe renal impairment, systemic clearance of ceftobiprole correlated well with creatinine clearance. For these patients, dose adjustments for the treatment of infections caused by target pathogens, including MRSA, should be based on creatinine clearance. Ceftobiprole is undergoing clinical evaluation in phase III trials in patients with complicated skin and skin structure infections, patients with nosocomial pneumonia, and community-acquired pneumonia in hospitalized patients.














Similar content being viewed by others
References
Hebeisen P, Heinze-Krauss I, Angehrn P, et al. In vitro and in vivo properties of Ro 63–9141, a novel broad-spectrum cephalosporin with activity against methicillin-resistant staphylococci. Antimicrob Agents Chemother 2001 Mar; 45(3): 825–36
Schmitt-Hoffmann A, Roos B, Schleimer M, et al. Single-dose pharmacokinetics and safety of a novel broad-spectrum cephalosporin (BAL5788) in healthy volunteers. Antimicrob Agents Chemother 2004 Jul; 48(7): 2570–5
Bogdanovich T, Ednie LM, Shapiro S, et al. Antistaphylococcal activity of ceftobiprole, a new broad-spectrum cephalosporin. Antimicrob Agents Chemother 2005 Oct; 49(10): 4210–9
Jones RN, Deshpande LM, Mutnick AH, et al. In vitro evaluation of BAL9141, a novel parenteral cephalosporin active against oxacillin-resistant staphylococci. J Antimicrob Chemother 2002 Dec; 50(6): 915–32
Deshpande LM, Jones RN. Bactericidal activity and synergy studies of BAL9141, a novel pyrrolidinone-3-ylidenemethyl cephem, tested against streptococci, enterococci and methicillin-resistant staphylococci. Clin Microbiol Infect 2003 Nov; 9(11): 1120–4
von Eiff C, Friedrich AW, Becker K, et al. Comparative in vitro activity of ceftobiprole against staphylococci displaying normal and small-colony variant phenotypes. Antimicrob Agents Chemother 2005 Oct; 49(10): 4372–4
Denis O, Deplano A, Nonhoff C, et al. In vitro activities of ceftobiprole, tige-cycline, daptomycin, and 19 other antimicrobials against methicillin-resistant Staphyiococcus aureus strains from a national survey of Belgian hospitals. Antimicrob Agents Chemother 2006 Aug; 50(8): 2680–5
Kosowska K, Hoellman DB, Lin G, et al. Antipneumococcal activity of ceftobiprole, a novel broad-spectrum cephalosporin. Antimicrob Agents Chemother 2005 May; 49(5): 1932–42
Zbinden R, Punter V, von Graevenitz A. In vitro activities of BAL9141, a novel broad-spectrum pyrrolidinone cephalosporin, against gram-negative nonfer-menters. Antimicrob Agents Chemother 2002 Mar; 46(3): 871–4
Issa NC, Rouse MS, Piper KE, et al. In vitro activity of BAL9141 against clinical isolates of gram-negative bacteria. Diagn Microbiol Infect Dis 2004 Jan; 48(1): 73–5
Arias CA, Singh KV, Panesso D, et al. Time-kill and synergism studies of ceftobiprole against Enterococcus faecalis, including beta-lactamase-producing and vancomycin-resistant isolates. Antimicrob Agents Chemother 2007 Jun; 51(6): 2043–7
Arias CA, Singh KV, Panesso D, et al. Evaluation of ceftobiprole medocaril against Enterococcus faecalis in a mouse peritonitis model. J Antimicrob Chemother 2007 Sep; 60(3): 594–8
Data on file, Johnson & Johnson Pharmaceutical Research & Development, LLC, 2005
Craig WA. Pharmacokinetic/pharmacodynamic parameters: rationale for antibacterial dosing of mice and men. Clin Infect Dis 1998 Jan; 26(1): 1–10; quiz 11–2
Schmitt-Hoffmann A, Nyman L, Roos B, et al. Multiple-dose pharmacokinetics and safety of a novel broad-spectrum cephalosporin (BAL5788) in healthy volunteers. Antimicrob Agents Chemother 2004 Jul; 48(7): 2576–80
Schmitt-Hoffmann A, Murthy B, Strauss RS, et al. Pharmacokinetics (PK) of multiple infusions of ceftobiprole (1000 mg every 8 hours) in healthy volunteers [abstract no. A-1943]. 46th Annual Interscience Conference on Antimicrobial Agents and Chemotherapy, American Society for Microbiology; 2006 Sep 27–30; San Francisco (CA)
Murthy B, Skee D, Wexler D, et al. Pharmacokinetics of ceftobiprole following single and multiple intravenous infusions administered to healthy subjects [abstract/poster no. P779]. 17th European Congress of Clinical Microbiology and Infectious Diseases; 2007 Mar 31–Apr 3; Munich
Roos B, Schmitt-Hoffmann A, Schleimer M, et al. Safety and pharmacokinetics of BAL5788 in healthy subjects with normal or impaired renal function [abstract A-23]. 43rd Annual Interscience Conference on Antimicrobial Agents and Chemotherapy, American Society for Microbiology; 2003 Sep 14–17; Chicago (IL)
Schmitt-Hoffmann A, Harsch M, Heep M, et al. BAL5788 in patients with complicated skin and skin structure infections caused by Gram-positive pathogens including methicillin-resistant Staphylococcus species (MRSS) [abstract/poster no. P-1031]. 14th European Congress of Clinical Microbiology and Infectious Diseases; 2004 May 1–4; Prague
Andes D, Craig W. In-vivo pharmacodynamics of RO 63-9141 against multiple bacterial pathogens [abstract no. 1079]. 40th Interscience Conference on Antimicrobial Agents and Chemotherapy; 2000 Sep 17–20; Toronto
Mouton JW, Schmitt-Hoffmann A, Shapiro S, et al. Use of Monte Carlo simulations to select therapeutic doses and provisional breakpoints of BAL9141. Antimicrob Agents Chemother 2004 May; 48(5): 1713–8
Lodise TP, Drusano GL, Ma L, et al. Probability of target attainment for ceftobiprole as derived from a population pharmacokinetic analysis of 150 subjects. Antimicrob Agents Chemother 2007 Jul; 51(7): 2378–87
Acknowledgements
Bindu Murthy is an employee of Johnson & Johnson. Anne Schmitt-Hoffmann is an employee of Basilea Pharmaceutica Ltd. No sources of funding were used to assist in the preparation of this review. The authors have no other conflicts of interest that are directly relevant to the content of this review.
The authors would like to thank Karen Bush, PhD, for her contributions to the microbiology sections.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Murthy, B., Schmitt-Hoffmann, A. Pharmacokinetics and Pharmacodynamics of Ceftobiprole, an Anti-MRSA Cephalosporin with Broad-Spectrum Activity. Clin Pharmacokinet 47, 21–33 (2008). https://doi.org/10.2165/00003088-200847010-00003
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003088-200847010-00003