Abstract
Hydroxyapatite modified with methacrylate groups-bearing polyhedral oligomeric silsesquioxane was for the first time applied as a filler in the experimental composite for dental applications. As the modifier changed the hydroxyapatite surface from hydrophilic to hydrophobic, it was predicted that the stability of the obtained composites would be improved in comparison with raw hydroxyapatite-filled composites. The stability in the oral imitating environment, basic physicochemical properties, and remineralizing potential understood as the ability to release calcium ions, were examined. The distribution of the fillers in the organic matrix, composites’ degree of conversion, depth of cure, flexural and compressive strengths, sorption, and solubility after 2 and 12 weeks of incubation, and the concentrations of calcium released were examined. The results were subjected to statistical analysis. The filler modification resulted in the improvement of the composites’ mass stability during long-term incubation with simultaneous beneficial more balanced calcium release profiles and comparable physicochemical properties.
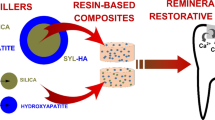
Graphical abstract

Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Avoid common mistakes on your manuscript.
Introduction
Calcium phosphates (CPs) arouse an increasing interest as potential fillers for dental resin-based composites (RBCs). It is due to their chemical formula, similar to the inorganic components of teeth and bones [1,2,3]. Representatives of this group differ mainly in the ratio of Ca to P and, consequently, in solubility [2]. Their capacity to release calcium and phosphate ions results in the remineralizing potential [3]. These ions are able to reverse the destructive demineralization process of teeth in the remineralization process [4]. The remineralizing potential of CPs has been used in toothpaste, mouth rinses, chewing gums, etc. [3]. Concerning the application of CPs as fillers in RBCs, the most examined is amorphous calcium phosphate (ACP) [5]. Its highly soluble form is beneficial in some applications, e.g. in bleaching agents or dentifrices. However, in dental composites, its application results in weak mechanical properties and limited ability to release remineralizing ions, as large quantities of ions are leached at the beginning, causing the rapid exhaustion of this reservoir [5]. Another representative from the CPs group, i.e. hydroxyapatite (HA) seems to be more attractive, as it is the main component of teeth and bones [6,7,8]. Our previous research has shown that HA-filled composites are homogeneous, able to release calcium ions, show a high degree of conversion [9], high depth of cure [10], and have good mechanical properties [11].
Another interesting group of compounds for dental composites is polyhedral oligomeric silsesquioxanes (POSS). These high molecular weight compounds with the general formula RSiO1.5 (R is the organic group) are characterized by different spatial structures and hybrid organic–inorganic structure [12,13,14]. The addition of a few percent of POSS to RBC resulted in improved mechanical properties and lowered polymerization shrinkage [15, 16]. Moreover, these odorless and environment-friendly compounds are known for their good miscibility with other organic compounds enabling the preparation of homogeneous composites, which is an undoubtful advantage of this group of materials [13].
Our previous research concerned the modification of hydroxyapatite particles with methacrylic groups-bearing POSS, namely heptaisobutyltri((methacryloxypropyl) dimethylsiloxy) heptasilsesquioxane (HIB-Met) [17]. HIB-Met was synthesized and after confirmation of its structure, it was used as an HA modifier in eight different modification procedures. Their effectiveness was verified and the structure of modified powders was characterized. The most important observation was that in all cases highly hydrophilic HA changed to more, or even completely hydrophobic. It was predicted that this wettability change will influence the stability of the composites with such fillers during the incubation in the aqueous solutions imitating the oral environment [17].
Therefore, the aim of this study is to verify this finding, with the research hypothesis being that the HIB-Met-modified fillers enhance the stability of the composites in aqueous solutions. The further questions are how the application of such fillers impacts the composites’ physicochemical properties, as well as their remineralizing potential. For this purpose, four composites: with HA, silanized HA, and two with HIB-Met-modified HA were prepared and examined. Their basic properties, including the degree of conversion (DC), depth of cure (DOC), sorption (SP), and solubility (SL) after 2 and 12 weeks of incubation, compressive (R) and flexural (σ) strength, and the ability to release calcium ions, were examined. Also, the fillers’ distribution in the organic matrix was examined.
Results and discussion
To facilitate the reading of the results, the names of the composites come from the type of filler used.
Raman spectra of the examined composites, as well as Raman maps showing the distribution of the fillers in the composites’ organic matrix with corresponding histograms, are presented in Fig. 1. The ratio of the bands’ intensities at 960 cm−1 to 1608 cm−1 was used to determine the distribution of fillers in composites. 960 cm−1 band is assigned to the phosphate groups of HA, while 1608 cm−1 band is connected with the presence of aromatic double C=C bonds in the organic matrix [18]. Similar values of their ratio throughout the examined area indicate low variability of the filler content in the material, i.e. its homogeneous distribution. The fillers (unmodified and modified HA) were present over the entire study area. 960/1608 values differed among the study materials. Composites with modified HA showed lower values of this parameter in comparison with raw HA composites. This is because the modification resulted in the coverage of the HA surface by other groups originating from modifiers. Basic statistics for the Raman maps are presented in Fig. 2. Most importantly, based on the histograms, as well as basic statistics, it can be concluded that all fillers were distributed homogeneously. There are no gaps or clusters of fillers. Standard deviations are very low, so the observed values are well concentrated around the mean value. Moreover, in all cases, about 99% of observations are within the narrow ranges of 960/1608. These ranges are 2.2–2.8 for HA, 2.0–2.8 for HA-sil, 1.9–2.4 for HA-HIB-Met, and 1.7–2.3 for HA-sil-HIB-Met.
Mean values (± standard deviation, SD) of DC, DOC, CS, and FS are presented in Table 1. The table contains also the results of the statistical analysis.
Most of the Bis-GMA-based composites showed typical DC values in the range of 52–75%, while the contractual lower level of this parameter is set as 55% [19]. The meaning of this parameter is crucial as it correlated with the mechanical properties, as well as health effects, as the unreacted monomers can be leached from the restoration causing irritation and other adverse consequences [20]. Examined composites showed DC values higher than 70%, which makes them highly polymerized. The highest DC values showed composites with HA and HA-HIB-Met fillers. There are no statistically significant differences in DC values between these two composites. Lower values of this parameter were observed if the filler was silanized (HA-sil and HA-sil-HIB-Met). It is somehow surprising as the prediction is that methacrylic groups from MPS take part in the polymerization process [21]. However, the silanization may result in the increased viscosity of the composite which in turn causes reduced mobility of molecules during polymerization and low conversion [22, 23]. In consequence, despite the MPS reaction with monomers, DCs are lower as less mobile monomer molecules cannot reach each other and react together. Moreover, the initial methacrylic bond number is higher as it is a sum of all CH2=CH2 bonds: from Bis-GMA, TEGDMA, and additionally MPS.
DOC is the parameter that describes the thickness of the composite, on which it is properly cured. It is quite an inaccurate definition and our previous research has proved that the scratching method is rather subjective and is burdened with error [10]. But the procedure is easy to handle and no-time consuming, and most important, it is officially recommended by ISO 4049 [24]. The value of this parameter defines how thick layer of the restorative material can be applied, therefore, it is crucial in clinical practice. According to ISO 4049, the minimal DOC for restorative materials is 1.0 mm for opaque shades and 1.5 mm for others [24]. Examined composites met both criteria, as their DOC was above 2.8 mm. No effect of silanization was observed, which is in accordance with other research [21]. The significantly higher DOC was however observed in the case of the HA-HIB-Met composite. This suggests that the modifier likely participates in the cross-linking of the organic matrix, enabling the cured composite to polymerize to a greater depth than others.
The compressive strength (CS) of restoration seems to reflect how it counteracts masticatory forces. However, there are no strict requirements in terms of the critical values of this parameter. It is however quite intuitive that CS values should be close to CS values of dental hard tissues, i.e. dentin and enamel. Unfortunately, at that point, there is also some vagueness as different sources claim different compressive strengths of these tissues. Sakaguchi and Powers [25] give the CS values of 384 and 297 MPa for enamel and dentin, respectively, whereas, the compressive strength of these tissues determined in [26] are 62.2 (± 23.8) and 193.7 (± 30.6) MPa, respectively. Literature reported also some theoretical values of compressive strength of photocurable resin composites being within the range of 246–448 MPa [27], and typical values for RBCs of 225 MPa [25]. CS values can be also related to the masticatory forces, which are 100–150 N during biting [28]. Concerning the above, it is hard to clearly define whether the measured compressive strengths were sufficient to ensure the durability of the composites during masticatory. However, it can be noted that they surpassed the masticatory forces and were within the typical range of RBCs, as they were between 246.7 (SD 23.0) and 289.9 (SD 19.6) MPa. Moreover, the values of this parameter can be easily increased by the addition of some amount of another filler, e.g. silica [29]. A slight effect of silanization can be observed, as HA-sil composite showed the highest CS values with no further statistically significant increase after HIB-Met modification. Material strength, including compressive strength, depends on various factors such as composition, including both the organic matrix and filler, filler amount and shape, as well as its distribution within the organic matrix [30]. Since the morphology of the fillers remained unchanged after silanization and HIB-Met modification [17], their fraction also remained constant, and their comparable homogeneous distribution was confirmed by Raman mapping (Figs. 1, 2). Therefore, it appears that the slightly higher compressive strength value observed in the HA-sil composite was a result of the formation of a slightly stronger interfacial bond between silanized HA and the organic matrix.
Concerning the mechanical properties, it has to be noted that even if intuitive, testing the compressive strength is not as realistic as it may look. Research has shown that RBCs wear as a result of tension forces rather than compression [31, 32]. However, the tensile strength is very difficult to measure for such materials, therefore, flexural strength (FS) testing is recommended, also by ISO 4049 [24], as some kind of approximation of tensile strength [31] [32]. According to ISO 4049, the flexural strength of restoration should be at least 50 MPa for non-occlusal surfaces and at least 80 MPa for occlusal surfaces [24]. Examined composites met the first criteria while failing in terms of the second. To improve their resistance to flexural forces, the addition of fiber-shaped fillers is advised [33], but this is out of the scope of this paper. There was no effect of silanization or HIB-Met modification on the values of FS.
Elastic modulus is a measure of the material's rigidity. The values of both elastic moduli, CM and FM, did not differ statistically significantly between the tested materials, indicating that their elastic properties should be considered the same. Additionally, the obtained values of CM and FM fall within the typical range for microfilled composites, i.e., CM between 2.6 and 4.8 GPa, and FM between 4.0 and 6.9 GPa [25].
Mean values (± standard deviation) of SP, SP12, SL, and SL12 are presented in Fig. 3. The figure contains also the results of the statistical analysis.
Basic statistics for SP, SP12, SL, and SL12 values; materials showing no statistical differences (p > 0.05) were connected with a clamp (one-way variance analysis with post-hoc Tukey's multiple comparison tests); no statistical differences (p > 0.05) in the values of each parameter according to the incubation time (2 vs 12 weeks) are marked with the same capital letters (Student's t-tests).
Sorption and solubility are very important factors affecting the stability of the restoration. Concerning dental materials, mainly the sorption of and the solubility in water or other aqueous solutions is considered, as the oral cavity is a highly aqueous environment. Water sorption results in dimensional changes of restoration by swelling, which in turn may cause deterioration of the bonding with the tooth cavity. Plasticization may also occur, deteriorating the mechanical properties of a filling. Whereas, solubility is connected with the leaching of compounds showing potential negative health effects. The aqueous environment of the oral cavity is also conducive to hydrolytic degradation [34, 35]. In general, both sorption and solubility affect the biocompatibility, susceptibility to staining, and deterioration of restorative materials properties [32]. According to ISO 4049, after seven days of incubation in water, sorption should be not higher than 40 μg mL−1, while the solubility cannot exceed 7.5 μg mL−1 [24]. In this research, the incubation time was longer, so the obtained results cannot be interpreted literally in terms of ISO requirements. However, they can be used to assess differences in composite stability in aqueous environments, depending on the type of filler used.
It can be observed that composites showed no statistical differences in SP values after 2 weeks of incubation (above 66 μg mL−1). However, materials differed in their solubility after this incubation period. HA composite showed the highest SL value (21 ± 3.6 μg mL−1), while the SL of HA-HIB-Met and HA-sil-HIB-Met composites was 5 to 10 times lower (4 ± 1.4 μg mL−1 and 2 ± 0.5 μg mL−1, respectively). These two composites met the ISO 4049 criterion in terms of SL values, even with the longer than 7 days incubation time. The solubility of HA-sil composite after 14 days of incubation was higher than the ISO criterion specifies, i.e. 12 ± 3.7 μg mL−1. The hydrophilic character of HA explains the obtained results. Also, the silanization effect could not be different as MPS is also hydrophilic [36]. However, the lack of differences in SP when using HIB-Met modified fillers is surprising. According to the significant differences in wettability of raw and HIB-Met-modified HA, it was predicted that both SP and SL will differ significantly [17]. Meanwhile, this beneficial effect is observed only in the case of SL. However, it can be explained by the fact that SP reflects the amount of water that penetrates the voids in the structure of the composite, while SL is the amount of substances leached from their structure [37]. Probably the modification of HA by HIB-Met did not change the HA structure to the extent, which would provide the difference in the structure of the obtained composites. Therefore, despite the filler's wettability changes, a similar composite structure is obtained so the water is absorbed in the same quantity. However, the modified HA surface contains also the HIB-Met molecules, which provide an additional boundary for the leached compounds, making their diffusion more difficult. An additional organic layer protects the filler particles from the environment, decreasing their solubility [34]. After a long time of incubation (12 weeks) still no clear effect of the silanization and modification of filler on SP12 was observed. However, it seems that HA-sil and HA-HIB-Met composites reached the water saturation very fast, as their SP12 values (70 ± 5.5 μg mL−1 and 77 ± 7.2 μg mL−1, respectively) did not differ significantly from SP. A significant increase was however observed in the case of HA- and HA-sil-HIB-Met-composites (85 ± 1.8 μg mL−1 and 79 ± 5.5 μg mL−1, respectively). In all cases, SL12 values (SL12 for HA, HA-sil, HA-HIB-Met, and HA-sil-HIB-Met composites: 31 ± 1 μg mL−1, 22 ± 0.6 μg mL−1, 19 ± 0.5 μg mL−1, 13 ± 1.7 μg mL−1) were higher than SL. Still, silanization and modification of fillers resulted in less soluble composites making them beneficial over raw HA-filled composite.
Calcium release profiles are presented in Fig. 4.
The role of calcium in the remineralization process is undoubtedly crucial. Some amount of this element is available from the saliva. However, saturated solutions are required to induce remineralization [38]. Therefore, delivering Ca from additional sources is always beneficial. Using calcium-releasing restorations enables the delivery of Ca2+ to places directly exposed to secondary caries, i.e. at the tooth-filling interface. Besides the evident role of calcium, phosphate, and fluorine ions in the remineralization process, calcium ions are of particular importance as their release precedes the release of phosphate ions in the demineralization process. Therefore, delivering Ca2+ is considered more effective at the early stages of demineralization [39]. Calcium release proceeds in a diffusion-controlled mechanism, so initially, high Ca2+ concentrations are observed, with the subsequent slowdown of the process [5]. All examined composites retained the ability to release calcium ions under the experiment conditions. The obtained calcium release profiles are in accordance with this finding, as well as they correspond to the solubility of composites. The initial phase of high Ca2+ concentrations decreased gradually to obtain some kind of stable plateau after five weeks of incubation, which is in accordance with the previous research [5]. In this first incubation period, i.e. between one and five weeks of incubation, the highest Ca2+ concentrations were observed for HA and HA-sil composites. Since MPS is hydrophilic, HA-sil composite mass stability was similar to HA composite, as well as the release of calcium [40]. In that incubation period, composites filled with HIB-Met-modified HA showed lower Ca2+ concentration, which probably resulted from the decreased accessibility of HA particles that were surrounded by the molecules of the modifier. The lower initial calcium release may be beneficial as it may result in a prolongation of calcium release. It can also be observed that after reaching the plateau (five weeks), Ca2+ concentrations were at a similar level for all examined composites. Therefore, it can be stated that modification of the HA surface with HIB-Met resulted not only in reducing the solubility but also slowing down the process of Ca2+ release, preventing the rapid exhaustion of this calcium reservoir. As far as the long-lasting remineralizing potential and mass stability are concerned, the application of HIB-Met-modified HA in resin-based composites can be considered advantageous.
Conclusions
The hydrophobization of the HA surface through HIB-Met modification resulted in enhanced mass stability of the obtained composites during incubation in aqueous environments, thereby supporting our research hypothesis. Additionally, a more balanced remineralizing potential was observed in the composites filled with HIB-Met modified HA. Furthermore, the remaining physicochemical properties studied, including the degree of conversion, depth of cure, compressive and flexural strengths, and filler distribution, were comparable or exhibited only slight differences regardless of the filler used. Despite the limitations of this study, i.e. incubation time longer than specified in ISO 4049 and no aging before mechanical testing, the obtained results are promising. Therefore, further experiments to assess the application potential of the tested materials are recommended. These experiments may include attempts to enhance the flexural strength, examination of the properties of the composites after aging, biological tests, and testing properties according to the applicable standards, including ISO 4049.
Methods
Reagents
Hydroxyapatite (≥ 90%; mean particle size 10 μm; HA), bisphenol A glycerolate dimethacrylate (Bis-GMA), triethylene glycol dimethacrylate (95%; TEGDMA), camphorquinone (97%; CQ), and ethyl 4-(dimethylamino)benzoate (≥ 99%; EDMAB) were supplied by Merck (Germany).
The preparation procedure of silanized HA (HA-sil) and HA modified with HIB-Met (HA-HIB-Met and HA-sil-HIB-Met) was described in [17]. Briefly, HA was silanized with methacryloxypropyltrimethoxysilane (MPS) in ethanol/deionized water solution with pH adjusted to 4.0 with 3 M acetic acid for 24 h (300 rpm). Then, HA-sil was separated from the solution and dried for 24 h at 100 °C. The excess of MPS was removed by concentrated ethanol (5 mL of ethanol to 0.5 g of HA-sil, 350 rpm, 10 min). Then, HA-sil was separated from the solution and dried again for 24 h at 100 °C. HA and HA-sil were modified by HIB-Met chloroform solution for 24 h (300 rpm). Then, HA-HIB-Met and HA-sil-HIB-Met were separated from the solution and dried for 24 h at 70 °C. The excess of HIB-Met was removed by concentrated chloroform (5 mL of chloroform to 0.5 g of HA or HA-sil, 350 rpm, 10 min). Then, HA-HIB-Met and HA-sil-HIB-Met were separated from the solution and dried again for 24 h at 70 °C [17]. The synthesis and structures of HIB-Met and the obtained fillers were characterized in detail in the previous article using Fourier-Transform Infrared Spectroscopy, Nuclear Magnetic Resonance Spectroscopy (1H, 13C, 29Si), Mass Spectrometry, Energy Dispersive Spectrometry, Thermogravimetric Analysis, Elemental Analysis, and Scanning Electron Microscopy; therefore, this section was not duplicated here. Moreover, contact angle measurements were carried out to observe the wettability changes on the surface of modified HA [17]. Only the main modification steps were cited, as the article refers to the application of the fillers.
A schematic representation of the applied fillers is presented in Fig. 5.
Preparation of composites
Composites were prepared by mixing filler and organic matrix 1:1 (wt.). Therefore, the mass content of a filler was 50%, which was equivalent to 73% vol. Organic matrix was composed of Bis-GMA and TEGDMA 3:2 (wt.). CQ and EDMAB were added as polymerization initiator and accelerator in the amount of 0.5% (wt.). To obtain a homogeneous paste, components of each composite were mixed together in an automatic mortar grinder for five minutes (Pulverisette 2, Fritsch, Germany). Subsequently, mixtures were placed in PTFE forms, which dimensions depended on the tested parameter (see description below), protected on both sides with PET foil, and cured for 20 s both sides (except samples for depth of cure) with LED lamp (DB-685, Coxo, China, wavelength of the emitted light: 420–480 nm, emitted power > 1100 mW cm−2, diode power: max 5 W). Then, samples were removed from the forms and subjected to further tests.
Characterization of composites
Fillers’ distribution in the organic matrix of composites
The distribution of the fillers (HA, HA-sil, HA-HIB-Met, and HA-sil-HIB-Met) in the organic matrix of composites was examined with the use of Raman mapping (inVia Renishaw, United Kingdom). Raman maps were acquired in the areas of 100 × 100 μm2 with 5 μm step using a 785 nm laser.
Degree of conversion
The degree of conversion (DC) of composites was examined according to the well-developed procedure described in [18] using Fourier-transform infrared spectroscopy (FT-IR Spectroscope Vertex70, Bruker Optics, USA) in ATR (Attenuated Total Reflectance) mode on the diamond crystal. For this purpose, at least three samples of uncured paste and at least five samples of cured composites (φ 4 mm, 4 mm thick) were prepared and examined within the spectral range of 4000–600 cm−1 with 4 cm−1 resolution (32 scans). DC [%] was calculated from the following equation:
where Rcured and Runcured are the ratios of integral intensities of 1638 and 1608 cm−1 bands of cured and uncured samples, respectively. 1638 cm−1 is the band of double methacrylic bonds that reacts during polymerization, while 1608 cm−1 is the reference band of C=C aromatic bonds, which quantity remains constant during polymerization.
Depth of cure
Depth of cure (DOC) was examined according to ISO 4049 procedure [24]. Briefly, three samples of each material were cured for 20 s from one side (φ 4 mm, multiplicated 4 mm thick). Immediately after curing, the opposite side of the samples was scratched with the spatula to remove the uncured part of the composite. Subsequently, the thickness of the remaining cured sample was measured in four points with the digital caliper (± 0.02 mm) and each value was divided by two to obtain the DOC.
Mechanical properties
Compressive and flexural strength were examined for at least ten samples of each composite using a universal testing machine (Zwick Z010 TN ProLine, Zwick Roell, Germany). Cylindrical (φ 4 mm, 4 mm thick) and rectangular (25 × 2x2 mm) samples were prepared for compressive and flexural strength, respectively. A 3-point bend test was carried out according to ISO 4049 [24], i.e. the applied crosshead speed was 0.75 mm min−1, the initial force was 1 kgF, and the distance between the supports was 20 mm. Compressive strength test parameters were selected according to the previous experiments [11], i.e. crosshead speed of 1 mm·min−1, initial force 1KgF. Compressive, CS [Pa] and flexural, FS [Pa] strengths were calculated from the following equations:
where F is maximum load recorded during the test [N], A is an initial cross-section area of the sample [mm2], l is the distance between the supports [mm], b is the center width of the sample [mm], and h is the center height of the sample [mm]. The elastic modulus in compression (CM) and flexural (FM) tests were obtained automatically from the slope of the stress/strain curve with the initial deformation set at 0.05%.
Sorption, solubility, and calcium release
To determine sorption and solubility, a modified ISO 4049 procedure was employed. The modification involved extending the incubation time from 7 to 14 days and 12 weeks. This decision was driven by the assumption that, given the application of the same organic matrix and filler fraction, differences between the materials would only become apparent with a longer duration of experimentation. Six cylindrical samples (φ 15 mm, 1 mm thick) of each composite were incubated in deionized water at 36.6 °C to imitate the aqueous environment of the oral cavity. Samples were first incubated dry at 36.6 °C and weighed every 24 h to obtain their stabilized mass (± 0.1 mg in 24 h, m1). Samples’ diameter and thickness were measured in four places with the use of the digital caliper (± 0.02 mm) to calculate their volume (V). Subsequently, samples were placed in 20 mL of deionized water and incubated at 36.6 °C. Incubation time for three samples of each composite was 2 weeks for sorption (SP) and solubility (SL). The remaining three samples of each composite were incubated for a total of 12 weeks for Ca release and extended-time SP (SP12) and SL (SL12) determination. After the total time of incubation, samples were weighed (m2) and stored dry at 36.6 °C for mass stabilization (± 0.1 mg in 24 h). Then, their stabilized masses were recorded (m3). SP/SP12 [μg·mm−3] and SL/SL12 [μg·mm−3] were calculated from the equations:
For Ca release and extended-time SP12 and SL12 determination, every week the solution was replaced with fresh deionized water and subjected to the combined ion-selective electrode (ISE) measurement. Three blank samples of deionized water were also every time prepared, incubated at 36.6 °C, and measured by ISE. Before ISE measurement, 0.4 mL of ionic-strength adjuster (ISA) was added to each sample. To compare the results the amounts of calcium released were re-calculated on 100 mg of composites.
A schematic diagram of the conducted research is presented in Fig. 6.
Statistical analysis
The obtained results were subjected to statistical analysis at α = 0.05 significance level. The normal distribution and the variance homogeneity of the data were confirmed by the Shapiro–Wilks tests and the Levene test. One-way variance analysis with post-hoc Tukey’s multiple comparison tests for DC, DOC, CS, CM, FS, FM, SP, SP12, SL, SL12 values between four examined composites, as well as Student's t-tests for SP and SP12, SL and SL12 for each composite, were applied to determine the statistically significant differences in the values of examined parameters. The calculations were performed with the use of Statistica 13.1 software (TIBCO Software).
Data availability
Data supporting the findings of this study are available in the open RepOD repository with the identifier https://doi.org/10.18150/MY7WZS.
References
S.V. Dorozhkin, Bioceramics of calcium orthophosphates. Biomaterials 31, 1465–1485 (2010). https://doi.org/10.1016/j.biomaterials.2009.11.050
S.V. Dorozhkin, M. Epple, Biological and medical significance of calcium phosphates. Angew. Chem. Int. Ed. 41, 3130–3146 (2002). https://doi.org/10.1002/1521-3773(20020902)41:17%3c3130::AID-ANIE3130%3e3.0.CO;2-1
S.V. Dorozhkin, Calcium orthophosphates in dentistry. J. Mater. Sci. Mater. Med. 24, 1335–1363 (2013). https://doi.org/10.1007/s10856-013-4898-1
H. Ehrlich, P.G. Koutsoukos, K.D. Demadis, O.S. Pokrovsky, Principles of demineralization: Modern strategies for the isolation of organic frameworks. Micron 39, 1062–1091 (2008). https://doi.org/10.1016/j.micron.2008.02.004
R.R. Braga, Calcium phosphates as ion-releasing fillers in restorative resin-based materials. Dent. Mater. 35, 3–14 (2019). https://doi.org/10.1016/j.dental.2018.08.288
P. Laurance-Young, L. Bozec, L. Gracia, G. Rees, F. Lippert, R.J.M. Lynch, J.C. Knowles, A review of the structure of human and bovine dental hard tissues and their physicochemical behaviour in relation to erosive challenge and remineralisation. J. Dent. 39, 266–272 (2011). https://doi.org/10.1016/j.jdent.2011.01.008
M.A. Meyers, P.-Y. Chen, A.Y.-M. Lin, Y. Seki, Biological materials: Structure and mechanical properties. Prog. Mater. Sci. 53, 1–206 (2008). https://doi.org/10.1016/j.pmatsci.2007.05.002
I.M. Low, N. Duraman, U. Mahmood, Mapping the structure, composition and mechanical properties of human teeth. Mater. Sci. Eng. C 28, 243–247 (2008). https://doi.org/10.1016/j.msec.2006.12.013
Z. Okulus, T. Buchwald, A. Voelkel, Calcium release from experimental dental materials. Mater. Sci. Eng. C 68, 213–220 (2016). https://doi.org/10.1016/j.msec.2016.05.116
Z. Okulus, T. Buchwald, A. Voelkel, Characterization of light-cured, dental-resin-based biocomposites. J. Appl. Polym. Sci. (2015). https://doi.org/10.1002/app.42812
Z. Okulus, A. Voelkel, Mechanical properties of experimental composites with different calcium phosphates fillers. Mater. Sci. Eng. C 78, 1101–1108 (2017). https://doi.org/10.1016/j.msec.2017.04.158
H. Ghanbari, B.G. Cousins, A.M. Seifalian, A nanocage for nanomedicine: polyhedral oligomeric silsesquioxane (POSS): a nanocage for nanomedicine …. Macromol. Rapid Commun. 32, 1032–1046 (2011). https://doi.org/10.1002/marc.201100126
G. Li, L. Wang, H. Ni, Polyhedral oligomeric silsesquioxane (POSS) polymers and copolymers: a review. J. Inorg. Organomet. Polym. 11, 123–154 (2001)
R.Y. Kannan, H.J. Salacinski, P.E. Butler, A.M. Seifalian, Polyhedral oligomeric silsesquioxane nanocomposites: the next generation material for biomedical applications. Acc. Chem. Res. 38, 879–884 (2005). https://doi.org/10.1021/ar050055b
X. Wu, Y. Sun, W. Xie, Y. Liu, X. Song, Development of novel dental nanocomposites reinforced with polyhedral oligomeric silsesquioxane (POSS). Dent. Mater. 26, 456–462 (2010). https://doi.org/10.1016/j.dental.2009.11.161
W. Wang, X. Sun, L. Huang, Y. Gao, J. Ban, L. Shen, J. Chen, Structure–property relationships in hybrid dental nanocomposite resins containing monofunctional and multifunctional polyhedral oligomeric silsesquioxanes. Int. J. Nanomed. 84, 1 (2014). https://doi.org/10.2147/IJN.S56062
Z. Buchwald, M. Szołyga, J. Zwolińska, B. Marciniec, A. Voelkel, Surface modification of hydroxyapatite with polyhedral oligomeric silsesquioxane. React. Funct. Polym. 170, 105131 (2022). https://doi.org/10.1016/j.reactfunctpolym.2021.105131
Z. Okulus, T. Buchwald, M. Szybowicz, A. Voelkel, Study of a new resin-based composites containing hydroxyapatite filler using Raman and infrared spectroscopy. Mater. Chem. Phys. 145, 304–312 (2014). https://doi.org/10.1016/j.matchemphys.2014.02.012
R.Z. Alshali, N. Silikas, J.D. Satterthwaite, Degree of conversion of bulk-fill compared to conventional resin-composites at two time intervals. Dent. Mater. 29, e213–e217 (2013). https://doi.org/10.1016/j.dental.2013.05.011
M.J. German, Developments in resin-based composites. Br. Dent. J. 232, 638–643 (2022). https://doi.org/10.1038/s41415-022-4240-8
A. Aydınoğlu, A.B.H. Yoruç, Effects of silane-modified fillers on properties of dental composite resin. Mater. Sci. Eng. C 79, 382–389 (2017). https://doi.org/10.1016/j.msec.2017.04.151
I.D. Sideridou, M.M. Karabela, Effect of the amount of 3-methacyloxypropyltrimethoxysilane coupling agent on physical properties of dental resin nanocomposites. Dent. Mater. 25, 1315–1324 (2009). https://doi.org/10.1016/j.dental.2009.03.016
L.M. Cavalcante, L.G. Ferraz, K.B. Antunes, I.M. Garcia, L.F.J. Schneider, F.M. Collares, Silane content influences physicochemical properties in nanostructured model composites. Dent. Mater. 37, e85–e93 (2021). https://doi.org/10.1016/j.dental.2020.10.022
ISO_4049_2019_EN, (n.d.).
R.L. Sakaguchi, J.M. Powers, Craig’s Restorative Dental Materials, Thirteen. (Elsevier, New York, 2012). https://doi.org/10.1016/B978-0-323-08108-5.10001-5
K. Chun, H. Choi, J. Lee, Comparison of mechanical property and role between enamel and dentin in the human teeth. J. Dent. Biomech. 5, 1 (2014). https://doi.org/10.1177/1758736014520809
X. Zhang, Q. Zhang, X. Meng, Y. Ye, D. Feng, J. Xue, H. Wang, H. Huang, M. Wang, J. Wang, Rheological and mechanical properties of resin-based materials applied in dental restorations. Polymers 13, 2975 (2021). https://doi.org/10.3390/polym13172975
S. Şahin, M.C. Çehreli, E. Yalçın, The influence of functional forces on the biomechanics of implant-supported prostheses—a review. J. Dent. 30, 271–282 (2002). https://doi.org/10.1016/S0300-5712(02)00065-9
M. Sandomierski, Z. Buchwald, T. Buchwald, A. Voelkel, Silica-filled methacrylic composites with extremely high compressive strength. J. Mech. Behav. Biomed. Mater. 116, 104319 (2021). https://doi.org/10.1016/j.jmbbm.2021.104319
K. Cho, G. Rajan, P. Farrar, L. Prentice, B.G. Prusty, Dental resin composites: a review on materials to product realizations. Compos. Part B 230, 109495 (2022). https://doi.org/10.1016/j.compositesb.2021.109495
N. Ilie, T.J. Hilton, S.D. Heintze, R. Hickel, D.C. Watts, N. Silikas, J.W. Stansbury, M. Cadenaro, J.L. Ferracane, Academy of dental materials guidance—resin composites: part i—mechanical properties. Dent. Mater. 33, 880–894 (2017). https://doi.org/10.1016/j.dental.2017.04.013
J.L. Ferracane, Resin-based composite performance: are there some things we can’t predict? Dent. Mater. 29, 51–58 (2013). https://doi.org/10.1016/j.dental.2012.06.013
G. Guo, Y. Fan, J.-F. Zhang, J.L. Hagan, X. Xu, Novel dental composites reinforced with zirconia–silica ceramic nanofibers. Dent. Mater. 28, 360–368 (2012). https://doi.org/10.1016/j.dental.2011.11.006
J.L. Ferracane, Hygroscopic and hydrolytic effects in dental polymer networks. Dent. Mater. 22, 211–222 (2006). https://doi.org/10.1016/j.dental.2005.05.005
R. Bagheri, M.J. Tyas, M.F. Burrow, Subsurface degradation of resin-based composites. Dent. Mater. 23, 944–951 (2007). https://doi.org/10.1016/j.dental.2006.06.035
B.R.C. De Menezes, A.D.G. Sampaio, D.M. Da Silva, L.S. Montagna, T.L.D.A. Montanheiro, C.Y. KogaIto, G.P. Thim, Nanocomposites obtained by incorporation of silanized silver nanowires to improve mechanical properties and prevent fungal adhesion. Nano Sel. 2, 2358–2372 (2021). https://doi.org/10.1002/nano.202100095
H.Y. Marghalani, Sorption and solubility characteristics of self-adhesive resin cements. Dent. Mater. 28, e187–e198 (2012). https://doi.org/10.1016/j.dental.2012.04.037
L.J. Walsh, Contemporary technologies for remineralization therapies: a review, 11 (n.d.).
E. AbouNeel, A. Aljabo, A. Strange, S. Ibrahim, M. Coathup, A. Young, L. Bozec, V. Mudera, Demineralization & remineralization dynamics in teeth and bone. Int. J. Nanomed. 11, 4743–4763 (2016). https://doi.org/10.2147/IJN.S107624
T.O. Rifane, K.E.M. Cordeiro, F.A. Silvestre, M.T. Souza, E.D. Zanotto, V.G. Araújo-Neto, M. Giannini, S. Sauro, D.M. De Paula, V.P. Feitosa, Impact of silanization of different bioactive glasses in simplified adhesives on degree of conversion, dentin bonding and collagen remineralization. Dent. Mater. 39, 217–226 (2023). https://doi.org/10.1016/j.dental.2023.01.005
Funding
This work was produced with financial support from the National Science Centre, Poland (Grant No. 2021/43/D/ST5/00888). This research was funded in whole or in part by National Science Centre, Poland (Grant No. 2021/43/D/ST5/00888). For the purpose of Open Access, the author has applied a CC-BY public copyright licence to any Author Accepted Manuscript (AAM) version arising from this submission.
Author information
Authors and Affiliations
Contributions
Conceptualization: Zuzanna Buchwald; Methodology: Zuzanna Buchwald; Formal analysis and investigation: Zuzanna Buchwald, Tomasz Buchwald (Raman spectroscopy measurement, Raman maps figure preparation); Writing—original draft preparation: Zuzanna Buchwald; Writing—review and editing: Zuzanna Buchwald, Tomasz Buchwald, Adam Voelkel; Funding acquisition: Zuzanna Buchwald; Resources: Zuzanna Buchwald.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare no conflict of interest or competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Buchwald, Z., Buchwald, T. & Voelkel, A. Hydroxyapatite modified with polyhedral oligomeric silsesquioxane as a filler for dental resin-based composites. Journal of Materials Research (2024). https://doi.org/10.1557/s43578-024-01385-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1557/s43578-024-01385-7