Abstract
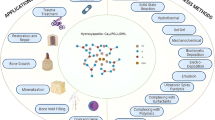
Despite having excellent osteoconductivity and biocompatibility, hydroxyapatite (HA) exhibits inadequate mechanical properties and bacterial susceptibility, which limits its medical applications. The present study aims to fabricate 3-aminopropyltrimethoxysilane (3-APTMS) functionalized gold (Au)-silver (Ag) nanoparticles incorporated in hydroxyapatite bioceramics to overcome this limitation. Thermogravimetric analysis (TGA), X-Ray diffraction, and scanning electron microscopy were carried out to understand the physical and chemical characteristics of the material. The maximum values of fracture toughness, hardness, compressive and flexural strength were measured for HA-10 Au/Ag NPs. Both quantitative and qualitative analyses of antibacterial behavior revealed that the adhesion of gram-positive (Staphylococcu aureus) and gram-negative (Eschericia coli) bacterial cells were reduced significantly after the incorporation of Au/Ag NPs as compared with the HA control. In addition, the effect of Au/Ag NPs incorporation on the cellular response was observed for the MG63 cell line. Both the quantitative and qualitative results indicate significantly enhanced cell proliferation with the incorporation of Au/Ag NPs as compared to HA. The addition of Au/Ag NPs in HA provides a material with appropriate mechanical, antibacterial, and cellular responses for further consideration.
Graphical abstract











Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in the article.
References
T. Kokubo, H.M. Kim, M. Kawashita, Novel bioactive materials with different mechanical properties. Biomaterials 24, 2161–2175 (2003). https://doi.org/10.1016/S0142-9612(03)00044-9
N. Miyata, K.I. Fuke, Q. Chen, M. Kawashita, T. Kokubo, T. Nakamura, Apatite-forming ability and mechanical properties of PTMO-modified CaO-SiO2 hybrids prepared by sol-gel processing effect of CaO and PTMO contents. Biomaterials 23, 3033–3040 (2002). https://doi.org/10.1016/S0142-9612(02)00065-0
H.M. Kim, H. Takadama, T. Kokubo, S. Nishiguchi, T. Nakamura, Formation of a bioactive graded bioactive surface structure on Ti-15Mo-5Zr-3Al alloy by chemical treatment. Biomaterials 21, 353–358 (2000). https://doi.org/10.1016/S0142-9612(99)00190-8
P. Feng, M. Niu, C. Gao, S. Peng, C. Shuai, A novel two-step sintering for nano-hydroxyapatite scaffolds for bone tissue engineering. Sci. Rep. 4, 5599 (2014). https://doi.org/10.1038/srep05599
A. Haider, S. Haider, S.S. Han, I.K. Kang, Recent advances in the synthesis, functionalization and biomedical applications of hydroxyapatite: a review. RSC Adv. 7, 7442–7458 (2017). https://doi.org/10.1039/C6RA26124H
D.K. Khajuria, R. Razdan, D.R. Mahapatra, Development, in vitro and in vivo characterization of zoledronic acid functionalized hydroxyapatite nanoparticle based formulation for treatment of osteoporosis in animal model. Eur. J. Pharm. Sci. 66, 173–183 (2015). https://doi.org/10.1016/j.ejps.2014.10.015
M. Okada, T. Matsumoto, Synthesis and modification of apatite nanoparticles for use in dental and medical applications. Jpn. Dent. Sci. Rev. 51, 85–95 (2015). https://doi.org/10.1016/j.jdsr.2015.03.004
G. Radha, N. Manjubaashini, S. Balakumar, Nano-hydroxyapatite/natural polymer composite scaffolds for bone tissue engineering: a brief review of recent trend. In vitro models 13, 1–27 (2023). https://doi.org/10.1007/s44164-023-00049-w
R. Kumar, S. Mohanty, Hydroxyapatite: a versatile bioceramic for tissue engineering application. J. Inorg. Organomet. Polym. 32, 4461–4477 (2022). https://doi.org/10.1007/s10904-022-02454-2
H. Zhou, J. Lee, Nanoscale hydroxyapatite particles for bone tissue engineering. Acta Biomater. 7, 2769–2781 (2011). https://doi.org/10.1016/j.actbio.2011.03.019
X. Zhang, C. Zhang, Y. Lin, P. Hu, Y. Shen, K. Wang, S. Meng, Y. Chai, X. Dai, X. Liu, Y. Liu, X. Mo, C. Cao, S. Li, X. Deng, L. Chen, Nanocomposite membranes enhance bone regeneration through restoring physiological electric microenvironment. ACS Nano 10, 7279–7286 (2016). https://doi.org/10.1021/acsnano.6b02247
T. Gong, J. Xie, J. Liao, T. Zhang, S. Lin, Y. Lin, Nanomaterials and bone regeneration. Bone Res. 3, 1–7 (2015). https://doi.org/10.1038/boneres.2015.29
Y. Chen, C. Gan, T. Zhang, G. Yu, P. Bai, A. Kaplan, Lasersurface-alloyed carbon nanotubes reinforced hydroxyapatite composite coatings. Appl. Phys. Lett. 86, 251905 (2005). https://doi.org/10.1063/1.1951054
Y.C. Tsui, C. Doyle, T.W. Clyne, Plasma sprayed hydroxyapatite coatings on titanium substrates Part 1: Mechanical properties and residual stress levels. Biomaterials 19, 2015–2029 (1998). https://doi.org/10.1016/S0142-9612(98)00103-3
H. Li, K.A. Khor, P. Cheang, Young’s modulus and fracture toughness determination of high velocity oxy-fuel-sprayed bioceramic coatings. Surf. Coat. Technol. 155, 21–32 (2002). https://doi.org/10.1016/S0257-8972(02)00026-9
X. Zhang, W. Chaimayo, C. Yang, J. Yao, B.L. Miller, M.Z. Yates, Silver-hydroxyapatite composite coatings with enhanced antimicrobial activities through heat treatment. Surf. Coat. Technol. 325, 39–45 (2017). https://doi.org/10.1016/j.surfcoat.2017.06.013
S.U. Victor, V.B.J. Roberto, Gold and silver nanotechnology on medicine. J. Chem. Biochem. 3, 21–33 (2015)
M. Ribeiro, M.P. Ferraz, F.J. Monteiro, M.H. Fernandes, M.M. Beppu, D. Mantione, H. Sardon, Antibacterial silk fibroin/nanohydroxyapatite hydrogels with silver and gold nanoparticles for bone regeneration. Nanomed. Nanotechnol. Biol. Med. 13, 231–239 (2017). https://doi.org/10.1016/j.nano.2016.08.026
D.N. Heo, W.K. Ko, M.S. Bae, J.B. Lee, D.W. Lee, W. Byun, C.H. Lee, E.C. Kim, B.Y. Jung, I.K. Kwon, Enhanced bone regeneration with a gold nanoparticle–hydrogel complex. J. Mater. Chem. B 2, 1584–1593 (2014). https://doi.org/10.1039/C3TB21246G
H. Geng, G. Poologasundarampillai, N. Todd, A. Devlin-Mullin, K.L. Moore, Z. Golrokhi, J.B. Gilchrist, E. Jones, R.J. Potter, C. Sutcliffe, M. O’Brien, D.W.L. Hukins, S. Cartmell, C.A. Mitchell, P.D. Lee, Biotransformation of Silver Released from Nanoparticle Coated Titanium Implants Revealed in Regenerating Bone. ACS Appl. Mater. Interfaces 9, 21169–21180 (2017). https://doi.org/10.1021/acsami.7b05150
K. Glenske, P. Donkiewicz, A. Köwitsch, N. Milosevic-Oljaca, P. Rider, S. Rofall, J. Franke, O. Jung, R. Smeets, R. Schnettler, S. Wenisch, M. Barbeck, Applications of metals for bone regeneration Int. J. Mol. Sci 19, 826 (2018). https://doi.org/10.3390/ijms19030826
H. Qin, C. Zhu, Z. An, Y. Jiang, Y. Zhao, J. Wang, X. Liu, B. Hui, X. Zhang, Y. Wang, Silver nanoparticles promote osteogenic differentiation of human urine-derived stem cells at noncytotoxic concentrations. Int. J. Nanomed. 9, 2469–2478 (2014). https://doi.org/10.2147/IJN.S59753
M. Mahmood, Z. Li, D. Casciano, M.V. Khodakovskaya, T. Chen, A. Karmakar, E. Dervishi, Y. Xu, T. Mustafa, F. Watanabe, A. Fejleh, M. Whitlow, M. Al-Adami, A. Ghosh, A.S. Biris, Nanostructural materials increase mineralization in bone cells and affect gene expression through miRNA regulation. J. Cell. Mol. Med. 15, 2297–2306 (2011). https://doi.org/10.1111/j.1582-4934.2010.01234.x
T. Qing, M. Mahmood, Y. Zheng, A.S. Biris, L. Shi, D.A. Casciano, A genomic characterization of the influence of silver nanoparticles on bone differentiation in MC3T3-E1 cells. J. Appl. Toxicol. 38(2), 172–179 (2018). https://doi.org/10.1002/jat.3528
S.H. Hsu, H.J. Yen, C.L. Tsai, The response of articular chondrocytes to type II collagen- Au nanocomposites. Artif. Organs 31, 854–868 (2007). https://doi.org/10.1111/j.1525-1594.2007.00482.x
D. Liu, J. Zhang, C. Yi, M. Yang, The effects of gold nanoparticles on the proliferation, differentiation, and mineralization function of MC3T3-E1 cells in vitro. Chinese Sci. Bull. 55, 1013–1019 (2010). https://doi.org/10.1007/s11434-010-0046-1
P. Gao, H. Zhang, Y. Liu, B. Fan, X. Li, X. Xiao, P. Lan, M. Li, L. Geng, D. Liu, Y. Yuan, Q. Lian, J. Lu, Z. Guo, Z. Wang, Beta-tricalcium phosphate granules improve osteogenesis in vitro and establish innovative osteo-regenerators for bone tissue engineering in vivo Sci. Rep. 6, 1–14 (2016). https://doi.org/10.1038/srep23367
M. Alvarez, N. Davidenko, R. García, A. Alonso, R. Rodríguez, R.M. Guerra, R. Sastre, Kinetic study of the photopolymerization of a bisphenol-A-bis(glycidylmethacrylate)/ triethyleneglycol dimethacrylate system in hydroxyapatite-filled composites. Polym. Int. 48, 699–704 (1999). https://doi.org/10.1002/(SICI)1097-0126(199908)48:8%3c699::AID-PI204%3e3.0.CO;2-Z
H. Bala, W. Fu, Y. Guo, J. Zhao, Y. Jiang, X. Ding, K. Yu, M. Li, Z. Wang, In situ preparation and surface modification of barium sulfate nanoparticles. Colloids Surf. A Physicochem. Eng. Asp. 274, 71–76 (2006). https://doi.org/10.1016/j.colsurfa.2005.08.050
C.M. Vaz, R.L. Reis, A.M. Cunha, Use of coupling agents to enhance the interfacial interactions in starch–EVOH/hydroxyapatite composites. Biomaterials 23, 629–635 (2002). https://doi.org/10.1016/S0142-9612(01)00150-8
W.L. Tham, W.S. Chow, Z.A.M. Ishak, The effect of 3-(trimethosilyl) propylmethacrylate on the mechanical, thermal, and morphological properties of poly(methyl methacrylate)/hydroxyapatite composites. J. Appl. Polym. Sci. 118, 218–228 (2010). https://doi.org/10.1002/app.32111
A.M.P. Dupraz, J.R. de Wijn, V.D. Meer, K. de Groot, Characterization of silane treated hydroxyapatite powders for use as filler in biodegradable composites. J. Biomed. Mater. Res. 30, 231–238 (1996)
C.L.E. Domingo, J. Fraile, Grafting of trialkoxysilane on the surface of nanoparticles by conventional wet alcoholic and supercritical carbon dioxide deposition methods. J. Supercrit. Fluids 37, 72–86 (2006). https://doi.org/10.1016/j.supflu.2005.06.013
O.G. Cisneros-Pineda, W.H. Kao, M.I. Loría-Bastarrachea, Y. Veranes-Pantoja, J.V. Cauich-Rodríguez, J.M. Cervantes-Uc, Towards optimization of the silanization process of hydroxyapatite for its use in bone cement formulations. J. Mater. Sci. Eng. C 40, 157–163 (2014). https://doi.org/10.1016/j.msec.2014.03.064
P.C. Pandey, R. Singh, Y. Pandey, Controlled synthesis of functional Ag, Ag–Au/Au–Ag nanoparticles and their Prussian blue nanocomposites for bioanalytical applications. RSC Adv. 5, 49671–49679 (2015). https://doi.org/10.1039/C5RA06251A
M. Rai, S.D. Deshmukh, A.P. Ingle, I.R. Gupta, M. Galdiero, S. Galdiero, Metal nanoparticles: The protective nanoshield against virus infection. Crit. Rev. Microbiol. 42(1), 46–56 (2016). https://doi.org/10.3109/1040841X.2013.879849
V. Gopinath, S. Priyadarshini, M.F. Loke, J. Arunkumar, E. Marsili, D. MubarakAli, P. Velusamy, J. Vadivelu, Biogenic synthesis, characterization of antibacterial silver nanoparticles and its cell cytotoxicity. Arab. J. Chem. 10(8), 1107–1117 (2017). https://doi.org/10.1016/j.arabjc.2015.11.011
M. Kobayashi, S. Nihonmatsu, T. Okawara, H. Onuki, H. Sakagami, H. Nakajima, H. Takeishi, J. Shimada, Adhesion and Proliferation of Osteoblastic Cells on Hydroxyapatite-dispersed Ti-based Composite Plate. In Vivo 33(4), 1067–1079 (2019). https://doi.org/10.21873/invivo.11575.PMID:31280194;PMCID:PMC6689340
S. Wang, S. Wen, M. Shen, R. Guo, X. Cao, J. Wang, X. Shi, Aminopropyltriethoxysilane-mediated surface functionalization of hydroxyapatite nanoparticles: synthesis, characterization, and in vitro toxicity assay. Int. J. Nanomed. 6, 3449–3459 (2011). https://doi.org/10.2147/IJN.S27166
S. Rehman, K. Khan, M. Mujahid, S. Nosheen, Synthesis of nano-hydroxyapatite and its rapid mediated surface functionalization by silane coupling agent. Mater. Sci. Eng., C 58, 675–681 (2016). https://doi.org/10.1016/j.msec.2015.09.014
E. Ji, Y.H. Song, J.H. Seo, K.I. Joo, Utilization of functionalized silane coatings for enhanced mechanical properties of hydroxyapatite filler. Korean J. Chem. Eng. (2023). https://doi.org/10.1007/s11814-023-1396-0
J. Jiao, S. Zhang, X. Qu, B. Yue, Recent Advances in Research on Antibacterial Metals and Alloys as Implant Materials. Front. Cell Infect. Microbiol. 11, 693939 (2021). https://doi.org/10.3389/fcimb.2021.693939
N.A. Abdul Halim, M.Z. Hussein, M.K. Kandar, Nanomaterials-upconverted hydroxyapatite for bone tissue engineering and a platform for drug delivery. Int. J. Nanomed. 16, 6477–6496 (2021). https://doi.org/10.2147/IJN.S298936
C.C.V. Cintra, D.A. Ferreira-Ermita, F.H. Loures, P.M. Araújo, I.M. Ribeiro, F.R. Araújo, F.L. Valente, E.C.C. Reis, A.C.F. Costa, S.M. Bicalho, A.P. Borges, In vitro characterization of hydroxyapatite and cobalt ferrite nanoparticles compounds and their biocompatibility in vivo. J. Mater. Sci. Mater. Med. 33(2), 21 (2022). https://doi.org/10.1007/s10856-022-06640-z
C. Wang, J. Feng, J. Zhou, X. Huang, L. Wang, G. Liu, J. Cheng, Microstructure, mechanical properties and in vitro biocompatibilities of a novel bionic hydroxyapatite bone scaffold prepared by the addition of boron nitride. J. Mater. Sci. 55, 14501–14515 (2020). https://doi.org/10.1007/s10853-020-05015-5
S. Mondal, G. Hoang, P. Manivasagan, M.S. Moorthy, T.T.V. Phan, H.H. Kim, T.P. Nguyen, J. Oh, Rapid microwave-assisted synthesis of gold loaded hydroxyapatite collagen nano-bio materials for drug delivery and tissue engineering application. Ceram. Int. 45(3), 2977–2988 (2019). https://doi.org/10.1016/j.ceramint.2018.10.016
A.A. Yetisgin, S. Cetinel, M. Zuvin, A. Kosar, O. Kutlu, Therapeutic Nanoparticles and Their Targeted Delivery Applications. Molecules 25(9), 2193 (2020). https://doi.org/10.3390/molecules25092193.PMID:32397080;PMCID:PMC7248934
V. Chandrakala, V. Aruna, G. Angajala, Review on metal nanoparticles as nanocarriers: current challenges and perspectives in drug delivery systems. Emergent Materials 5, 1593–1615 (2022). https://doi.org/10.1007/s42247-021-00335-x
A.S. Verma, D. Kumar, A.K. Dubey, Dielectric and electrical response of hydroxyapatite-Na0.5K0.5NbO3 bioceramic composite. Ceram. Int. 45, 329–3305 (2019). https://doi.org/10.1016/j.ceramint.2018.10.240
S.K. Arumugam, A.M. Rajam, N. Natarajan, U. Rao, C. Rose, T.P. Sastry, Formation of gold nanoparticles on hydroxyapatite surface for enhancement of blood compatibility via a negative cilia concept. J. Biomed. Nanotechnol. 2(1), 46–52 (2006). https://doi.org/10.1166/jbn.2006.009
H. Furedi-Milhofer, V. Hlady, F.S. Baker, R.A. Beebe, N.W. Wikholm, J.S. Kittelberger, Temperature-programmed dehydration of hydroxyapatite. J. Colloid Interf. Sci. 70(1), 1–9 (1979). https://doi.org/10.1016/0021-9797(79)90002-X
B. Sreedhar, D. Keerthi Devi, A. Sai Neetha, V. Pavan Kumar, K.V.R. Chary, Green synthesis of gum-acacia assisted gold-hydroxyapatite nanostructures e Characterization and catalytic activity. Mater. Chem. Phys. 153, 23–31 (2015). https://doi.org/10.1016/j.matchemphys.2014.12.031
P.K. Zysset, X.E. Guo, C.E. Hoffler, K.E. Moore, S.A. Goldstein, Elastic modulus and hardness of cortical and trabecular bone lamellae measured by nanoindentation in the human femur. J. Biomech. 32, 1005–1012 (1999). https://doi.org/10.1016/S0021-9290(99)00111-6
D.T. Reilly, A.H. Burstein, The mechanical properties of corticalbone. J. Bone Joint Sur. 57A, 1001–1022 (1974)
E.D. Sedlin, A rheological model for cortical bone: a study of thephysical properties of human femoral samples, Acta Orthop. Scan. 36, 1–77 (1965). https://doi.org/10.3109/ort.1965.36.suppl-83.01
S. Sahmani, S. Saber-Samandari, A. Khandan, M.M. Aghdam, Influence of MgO nanoparticles on the mechanical properties of coated hydroxyapatite nanocomposite scaffolds produced via space holder technique: Fabrication, characterization and simulation. J. Mech. Behav. Biomed. Mater. 95, 76–88 (2019). https://doi.org/10.1016/j.jmbbm.2019.03.014
G.R. Irwin, D.C. Washington, Analysis of Stresses and Strains near the End of a Crack Traversing a Plate. J. Appl. Mech. 24, 361–364 (1957)
W.J. Sun, S. Kothari, C.C. Sun, The relationship among tensile strength, Young’s modulus, and indentation hardness of pharmaceutical compacts. Powder Technol. 331, 1–6 (2018). https://doi.org/10.1016/j.powtec.2018.02.051
A.S. Verma, D. Kumar, A.K. Dubey, A review of an innovative concept to increase the toughness of the ceramics by piezoelectric secondary phases. Ceram. Int. 44, 16119–16127 (2018). https://doi.org/10.1016/j.ceramint.2018.06.063
A.M. Fayaz, K. Balaji, M. Girilal, R. Yadav, P.T. Kalaichelvan, R. Venketesan, Biogenic synthesis of silver nanoparticles and their synergistic effect with antibiotics: a study against gram-positive and gramnegative bacteria. Nanomed. Nanotechnol. Biol. Med. 6, 103–109 (2010). https://doi.org/10.1016/j.nano.2009.04.006
G. Tan, S. Wang, Y. Zhu, L. Zhou, P. Yu, X. Wang, T. He, J. Chen, C. Mao, C. Ning, Surface-selective preferential production of reactive oxygen species on piezoelectric ceramics for bacterial killing. ACS Appl. Mater. Interfaces 8, 24306–24309 (2016). https://doi.org/10.1021/acsami.6b07440
K.S. Ong, Y.L. Cheow, S.M. Lee, The role of reactive oxygen species in the antimicrobial activity of Pyochelin. J. Adv. Res. 8, 393–398 (2017). https://doi.org/10.1016/j.jare.2017.05.007
B. Blanc, C. Gerez, S.O. de Choudens, Assembly of Fe/S proteins in bacterial systems. Biochim. Biophys. Acta Mol. Cell Res. 1853, 1436–1447 (2015). https://doi.org/10.1016/j.bbamcr.2014.12.009
A.S. Verma, A. Sharma, A. Kumar, A. Mukhopadhyay, D. Kumar, A.K. Dubey, Multifunctional response of piezoelectric sodium potassium niobate (NKN)-toughened hydroxyapatite-based biocomposites. ACS Appl. Biomater. 3(8), 5287–5299 (2020). https://doi.org/10.1021/acsabm.0c00642
D. Grotto, L.S. Maria, J. Valentini, C. Paniz, G. Schmitt, S.C. Garcia, V.J. Pomblum, J.B.T. Rocha, M. Farina, Importance of the lipid peroxidation biomarkers and methodological aspects for malondialdehyde quantification. Quim. Nova 32, 169–174 (2009). https://doi.org/10.1590/S0100-40422009000100032
M.H. Hadwan, Simple spectrophotometric assay for measuring catalase activity in biological tissues. BMC Biochem. 19, 7 (2018). https://doi.org/10.1186/s12858-018-0097-5
K.M. Schaich, 2016 Analysis of Lipid and Protein Oxidation in Fats Oils and Foods. Chapter 1, AOCS Press, Champaign
M.P. Murphy, A. Holmgren, N.G. Larsson, B. Halliwell, C.J. Chang, B. Kalyanaraman, S.G. Rhee, P.J. Thornalley, L. Partridge, D. Gems, T. Nyström, Unraveling the biological roles of reactive oxygen species. Cell Metab. 13, 361–366 (2011). https://doi.org/10.1016/j.cmet.2011.03.010
X.Q. Chen, X.Z. Tian, I. Shin, J. Yoon, Fluorescent and luminescent probes for detection of reactive oxygen and nitrogen species. Chem. Soc. Rev. 40, 4783–4804 (2011). https://doi.org/10.1039/C1CS15037E
M. Solioz, A. Odermatt, Copper and silver transport by CopB-ATPase in membrane vesicles of Enterococcus hirae. J. Biol. Chem. 270, 9217–9221 (1995). https://doi.org/10.1074/jbc.270.16.9217
U. Klueh, V. Wagner, S. Kelly, A. Johnson, J.D. Bryers, Efficacy of silver-coated fabric to prevent bacterial colonization and subsequent device-based biofilm formation. J. Biomed. Mater. Res. 53, 621–631 (2000). https://doi.org/10.1002/1097-4636(2000)53:6%3c621::AID-JBM2%3e3.0.CO;2-Q
R.L. Davies, S.F. Etris, The development and functions of silver in water purification and disease control. Catal. Today 36, 107–114 (1997). https://doi.org/10.1016/S0920-5861(96)00203-9
H.Y. Song, K.K. Ko, I.H. Oh, B.T. Lee, Fabrication of silver nanoparticles and their antimicrobial mechanisms. Eur. Cells Mater. 11, 58 (2006)
S. Egger, R.P. Lehmann, M.J. Height, M.J. Loessner, M. Schuppler, Antimicrobial properties of a novel silver-silica nanocomposite material. Appl. Environ. Microbiol. 75, 2973–2976 (2009). https://doi.org/10.1128/AEM.01658-08
P.D. Bragg, D.J. Rannie, The effect of silver ios on the respiratory chain of E coli. Can. J. Microbiol. 20, 883–889 (1974). https://doi.org/10.1139/m74-135
T. Emami, R. Madani, F. Golchinfar, A. Shoushtary, S.M. Amini, Comparison of gold nanoparticle conjugated secondary antibody with non-gold secondary antibody in an ELISA kit model. Monocl. Antibodies Immunodiagn. Immunother. 34, 366–370 (2015). https://doi.org/10.1089/mab.2015.0021
A.A.K. Zarchi, S.M. Amini, A. Salimi, S. Kharazi, Synthesis and characterisation of liposomal doxorubicin with loaded gold nanoparticles. IET Nanobiotechnol. 12, 846–849 (2018). https://doi.org/10.1049/iet-nbt.2017.0321
Y. Zhang, P. Wang, Y. Wang, J. Li, D. Qiao, R. Chen, W. Yang, F. Yan, Gold nanoparticles promote the bone regeneration of periodontal ligament stem cell sheets through activation of autophagy. Int. J. Nanomed. 16, 61 (2021). https://doi.org/10.2147/IJN.S282246
H. Samadian, H. Khastar, A. Ehterami, M. Salehi, Bioengineered 3D nanocomposite based on gold nanoparticles and gelatin nanofibers for bone regeneration: In vitro and in vivo study. Sci. Rep. 11, 1–11 (2021). https://doi.org/10.1038/s41598-021-93367-6
C. Yi, D. Liu, C.C. Fong, J. Zhang, M. Yang, Gold nanoparticles promote osteogenic differentiation of mesenchymal stem cells through p38 MAPK pathway. ACS Nano 4, 6439–6448 (2010). https://doi.org/10.1021/nn101373r
H. Liang, X. Xu, X. Feng, L. Ma, X. Deng, S. Wu, X. Liu, C. Yang, Gold nanoparticles-loaded hydroxyapatite composites guide osteogenic differentiation of human mesenchymal stem cells through Wnt/β-catenin signaling pathway. Int. J. Nanomed. (2019). https://doi.org/10.2147/IJN.S213889
Y. Zhang, P. Wang, H. Mao, Y. Zhang, L. Zheng, P. Yu, Z. Guo, L. Li, Q. Jiang, PEGylated gold nanoparticles promote osteogenic differentiation in in vitro and in vivo systems. Mater. Design 197, 109231 (2021). https://doi.org/10.1016/j.matdes.2020.109231
J. Ge, K. Liu, W. Niu, M. Chen, M. Wang, Y. Xue, C. Gao, P.X. Ma, B. Lei, Gold and gold-silver alloy nanoparticles enhance the myogenic differentiation of myoblasts through p38 MAPK signaling pathway and promote in vivo skeletal muscle regeneration. Biomaterials 175, 19–29 (2018). https://doi.org/10.1016/j.biomaterials.2018.05.027
N.H. Daraghmeh, B.Z. Chowdhry, S.A. Leharne, M.M. Al Omari, A.A. Badwan, Profiles of drug substances. Excip. Relat. Methodol 36, 35–102 (2011). https://doi.org/10.1016/B978-0-12-387667-6.00002-6
ASTM E3484–99 A. Standard test method for micro indentation hardness of materials. 1984.
A.G. Evans, E.A. Charles, Fracture toughness determinations by indentation. J. Am. Ceram. Soc. 59, 371–372 (2006)
Y.J. Garcia, A.J. Rodríguez-Malaver, N. Peñaloza, Lipid peroxidation measurement by thiobarbituric acid assay in rat cerebellar slices. J. Neurosci. Methods 144, 127–135 (2005). https://doi.org/10.1016/j.jneumeth.2004.10.018
E.D. Wills, Lipid peroxide formation in microsomes. Biochem. J. 113, 315–324 (1969). https://doi.org/10.1042/bj1130315
B. Chance, A.C. Maehly, Assay of catalases and peroxidise. Methods Enzymol. 2, 764–775 (1955). https://doi.org/10.1016/S0076-6879(55)02300-8
Acknowledgments
The financial support from IIT (BHU) is gratefully acknowledged.
Author information
Authors and Affiliations
Contributions
MP: conceptualization, investigation, methodology, validation, writing—original draft. ASV: investigation, methodology. PCP: supervisor. RN: writing—original draft.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Roger Narayan was an editor of this journal during the review and decision stage. For the JMR policy on review and publication of manuscripts authored by editors, please refer to http://www.mrs.org/editor-manuscripts/.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pandey, M., Verma, A.S., Pandey, P.C. et al. Bone tissue engineering application of 3-aminopropyltrimethoxysilane functionalized Au/Ag bimetallic nanoparticles incorporated hydroxyapatite bioceramic. Journal of Materials Research 38, 4157–4174 (2023). https://doi.org/10.1557/s43578-023-01132-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1557/s43578-023-01132-4