Abstract
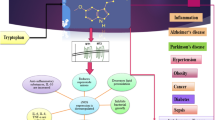
Sleep is an essential ubiquitous biological process, a periodical state of quiescence in which there is minimal processing of sensory information and no interaction with conspecifics or the environment. Despite relevant research on sleep structure and testing of numerous endogenous sleep-affecting chemicals, questions as to the precise mechanisms and functions of sleep remain without satisfactory responses. The purpose of this review is to report on current evidence as regards the effect of several endogenous and exogenous hormones, hormonal agents, and neuropeptides on sleep onset or wake process, when administered in humans in specific doses and via different routes. The actions of several peptides are presented in detail. Some of them (growth hormone releasing hormone, ghrelin, galanin, neuropeptide Y) seem to promote sleep, whereas others (corticotropin, somatostatin) impair its continuity.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Greenspan RJ, Tononi G, Cirelli C, Shaw PJ, 2001 Sleep and the fruit fly. Trends Neurosci 24: 142–145.
“The Regulation of Sleep”, 2000 Borbély AA, Hayaishi O, Sejnowski TJ, Altman JS (eds). HFSP, Strasbourg, France.
Porkka-Heiskanen T, Alanko L, Kalinchuk A, Stenberg D, 2002 Adenosine and Sleep. Sleep Med Rev 6: 321–332.
Krueger JM, Majde JA, Obál F Jr, 2003 Sleep in host defense. Brain Behav Immun 17: S41–S47.
Akerstedt T, Nilsson PM, 2003 Sleep as restitution: an introduction. J Intern Med 254: 6–12.
Sateia MJ, Santulli RB, 1998 Sleep in palliative care. In: Doyle O, Hanks GWC, MacDonald N (eds). Oxford Textbook of Palliative Medicine (2nd Ed). New York: Oxford University Press; Chapter 8, pp, 731–746.
Buckley TM, Schatzberg AF, 2005 On the interactions of the HPA axis and sleep: Normal HPA axis and rhythm, exemplary sleep disorders. J Clin Endocrinol Metab 90: 3106–3114.
Borbély AA, 1982 A two process model of sleep regulation [Abstract]. Hum Neurobiol 1: 195–204.
Borbély AA, Achermann P, 1999 Sleep homeostasis and models of sleep regulation. J Biol Rhythms 14: 557–568.
Steiger A, 2003 Sleep and endocrinology. J Intern Med 254: 13–22.
Steiger A, 2007 Neurochemical regulation of sleep. J Psychiatr Res 41: 537–552.
Antonijevic IA, Murck H, Frieboes RM, et al, 1999 On the gender differences in sleep-endocrine regulation in young normal humans. Neuroendocrinol 70: 280–287.
Obál F Jr, Krueger JM, 2004 GHRH and sleep. Sleep Med Rev 8: 367–377.
Steiger A, Guldner J, Hemmeter U, et al, 1992 Effects of growth hormone-releasing hormone and somatostatin on sleep EEG and nocturnal hormone secretion in male controls. Neuroendocrinol 56: 566–573.
Marshall L, Mölle M, Böschen G, et al, 1996 Greater efficacy of episodic than continuous growth hormone-releasing hormone (GHRH) administration in promting slow-wave sleep (SWS). J Clin Endocrinol Metab 81: 1009–1013.
Obál F Jr, Krueger JM, 2003 Biochemical regulation of non-rapideye-movement sleep. Front Biosci 8: d520–550.
Kupfer DJ, Jarrett DB, Ehlers CL, 1991 The effect of GRF on the EEG sleep of normal males. Sleep 14: 87–88.
Mathias S, Held K, Ising M, et al, 2007 Systemic growth hormone-releasing hormone (GHRH) impairs sleep in healthy young women. Psychoneuroendocrinol 32: 1021–1027.
Kerkhofs M, Van Cauter E, Van Onderbergen A, et al, 1993 Sleep-promoting effects of growth hormone-releasing hormone in normal men. Am J Physiol 264: E594–E598.
Schier T, Guldner J, Colla M, Holsboer F, Steiger A, 1997 Changes in sleep-endocrine activity after growth hormone-releasing hormone depend on time of administration. J Neuroendocrinol 9: 201–205.
Steiger A, 2003 Sleep and endocrine regulation. Front Biosci 8: s358–s376.
Perras B, Marshall L, Köhler G, Born J, Fehm HL, 1999 Sleep and endocrine changes after intranasal administration of growth hormone-releasing hormone in young and aged humans. PNEC 24: 743–757.
Schiissler P, Yassouridis A, Uhr M, et al, 2006 Growth hormone-releasing hormone and corticotropin-releasing hormone enhance non-rapid-eye-movement sleep after sleep deprivation. Am J Physiol Endocrinol Metab 291: E549–556.
Guldner J, Schier T, Friess E, et al, 1997 Reduced efficacy of growth hormone-releasing hormone in modulating sleep endocrine activity in the elderly. Neurobiol Aging 18: 491–495.
Antonijevic IA, Murck H, Frieboes RM, Barthelmes J, Steiger A, 2000 Sexually dimorphic effects of GHRH on sleep endocrine activity in patients with depression and normal controls — part I: the sleep EEG. Sleep Research Online 3: 5–13.
Obál Jr F, Payne L, Kapas L, et al, 1991 Inhibition of growth hormone-releasing factor suppresses both sleep and growth hormone secretion in the rat. Brain Res 557: 149–153.
Zhang J, Obál F Jr, Zheng T, et al, 1999 Intrapreoptic microinjection of GHRH or its antagonist alters sleep in rats. J Neurosci 19: 2187–2194.
Obál F Jr, Payne L, Opp M, et al, 1992 Growth hormone-releasing hormone antibodies suppress sleep and prevent enhancement of sleep after sleep deprivation. Am J Physiol 263: R1078–R1085.
Merriam GR, Schwartz RS, Vitiello MV, 2003 Growth hormone-releasing hormone and growth hormone secretagogues in normal aging. Endocrine 22: 41–48.
Doga M, Bonadonna S, Burattin A, Giustina A, 2001 Ectopic secretion of growth hormone-releasing hormone (GHRH) in neuroendocrine tumors: relevant clinical aspects. Ann Oncol 12: Suppl 2: S89–S94.
Kojima M, Hosoda H, Date Y, et al, 1999 Ghrelin is a growth hormone-releasing acylated peptide from stomach. Nature 402: 656–660.
Ghigo E, Broglio F, Arvat E, et al, 2005 Ghrelin: more than a natural GH secretagogue and/or an orexigenic factor. Clin Endocrinol 62: 1–17.
Korbonits M, Goldstone AP, Gueorguiev M, Grossman AB, 2004 Ghrelin — a hormone with multiple functions. Front Neuroendocrinol 25: 27–68.
van der Lely AJ, Tschop M, Heiman ML, Ghigo E, 2004 Biological, physiological, pathophysiological, and pharmacological aspects of ghrelin. Endocrin Rev 25: 426–457.
Arvat E, Maccario M, Di Vito L, et al, 2001 Endocrine activities of ghrelin, a natural growth hormone secretagogue (GHS), in humans: comparison and interactions with hexarelin, a nonnatural peptidyl GHS, and GH-releasing hormone. J Clin Endocrinol Metab 86: 1169–1174.
Weikel JC, Wichniak A, Ising M, et al, 2003 Ghrelin promotes slow-wave sleep in humans. Am J Physiol Endocrinol Metab 284: E407–E415.
Schuessler P, Uhr M, Ising M, et al, 2005 Nocturnal ghrelin levels — relationship to sleep EEG, the levels of growth hormone, ACTH and cortisol — and gender differences. J Sleep Res 14: 329–336.
Kluge M, Schüssler P, Zuber V, Yassouridis A, Steiger A, 2007 Ghrelin administered in the early morning increases secretion of cortisol and growth hormone without affecting sleep. Psychoneuroendocrinol 32: 287–292.
Copinschi G, Leproult R, Van Onderbergen A, et al, 1997 Prolonged oral treatment with MK-677, a novel growth hormone secretagogue, improves sleep quality in man. Neuroendocrinol 66: 278–286.
Frieboes RM, Murck H, Antonijevic IA, Steiger A, 1999 Effects of growth hormone-releasing peptide-6 on the nocturnal secretion of GH, ACTH and cortisol and on the sleep EEG in man: role of routes of administration. J Neuroendocrinol 11: 473–478.
Moreno-Reyes R, Kerkhofs M, L’Hermite-Baleriaux M, et al, 1998 Evidence against a role for the growth hormone-releasing peptide axis in human slow-wave sleep regulation. Am J Physiol 274: E779–E784.
Frieboes RM, Antonijevic IA, Held K, et al, 2004 Hex-arelin decreases slow-wave sleep and stimulates the secretion of GH, ACTH, cortisol and prolactin during sleep in healthy volunteers. Psychoneuroendocrinol 29: 851–860.
Simi L, Pinzani P, Raggi CC, et al, 2007 Influence of 17q gain and promoter polymorphisms on mRNA expression of somatostatin receptor type 2 in neuroblastoma. Clin Chim Acta 384: 149–154.
Frieboes RM, Murck H, Schier T, Holsboer F, Steiger A, 1997 Somatostatin impairs sleep in elderly human subjects [Abstract]. Neuropsychopharmacol 16: 339–345.
Steiger A, Weikel J, Held K, Schmid D, Ziegenbein M, 2002 Arginine improves sleep in elderly men [Abstract]. Sleep 25: A203.
Ziegenbein M, Murck H, Künzel H, Held K, Steiger A, 1999 Sleep-endocrine effects of growth hormone-releasing hormone (GHRH) in patients with obsessive-compulsive disorder (OCD). Pharmacopsychiatry 32: 220.
de Lecea L, Bourgin P, 2008 Neuropeptide interactions and REM sleep: a role for Urotensin II? Peptides 29: 845–851.
de Lecea L, 2005 Cortistatin: a natural somatostatin analog. J Endocrinol Invest 28: 10–14.
van der Klaauw AA, Pereira AM, van Kralingen KW, Rabe KF, Romijn JA, 2008 Somatostatin analog treatment is associated with an increased sleep latency in patients with long-term biochemical remission of acromegaly. Growth Horm IGF Res 18: 446–453.
Holsboer F, von Bardeleben U, Steiger A, 1988 Effects of intravenous corticotropin-releasing hormone upon sleep-related growth hormone surge and sleep EEG in man. Neuroendocrinol 48: 32–38.
Steiger A, Holsboer F, 1997. Neuropeptides and human sleep. Sleep 20: 1038–1052.
Antonijevic IA, Murck H, Frieboes RM, et al, 1999 Hyporesponsiveness of the pituitary to CRH during slow wave sleep is not mimicked by systemic GHRH. Neuroendocrinol 69: 88–96.
Vgontzas AN, Bixler EO, Wittman AM, et al, 2001 Middle-aged men show higher sensitivity of sleep to the arousing effects of corticotropin-releasing hormone than young men: clinical implications. J Clin Endocrinol Metab 86: 1489–1495.
Chang FC, Opp MR, 2001 Corticotropin-releasing hormone (CRH) as a regulator of waking. Neurosci Biobehav Rev 25: 445–453.
Held K, Kunzel H, Ising M, et al, 2004 Treatment with the CRH1-receptorantagonist R121919 improves sleep-EEG in patients with depression. J Psychiatr Res 38: 129–136.
Antonijevic I, 2007. HPA axis and sleep: identifying subtypes of major depression. Stress 11: 15–27.
Liu Z, Zhu F, Wang G, et al, 2007 Association study of corticotropin-releasing hormone receptor1 gene polymorphisms and antidepressant response in major depressive disorders. Neurosci Lett 414: 155–158.
Fehm HL, Späth-Schwalbe E, Pietrowsky R, et al, 1993 Entrainment of nocturnal pituitary-adrenocortical activity to sleep processes in man — a hypothesis. Exp Clin Endocrinol 101: 267–276.
Born J, Hansen K, Marshall L, et al, 1999 Timing the end of nocturnal sleep. Nature 397: 29–30.
Steiger A, 2002. Sleep and the hypothalamo-pituitary-adrenocortical system. Sleep Med Rev 6: 125–138.
Alexis MN, Stylianopoulou F, Kitraki E, Sekeris CE, 1983 The distribution and properties of the glucocorticoid receptor from rat brain and pituitary. J Biol Chem 258: 4710–4714.
Friess E, Wiedemann K, Steiger A, et al, 1995 The hypothalamic-pituitary-adrenocortical system and sleep in man. Adv Neuroimmunol 5: 111–125.
Bohlhalter S, Murck H, Holsboer F, Steiger A, 1997 Cortisol enhances non-REM sleep and growth hormone secretion in elderly subjects. Neurobiol Aging 18: 423–429.
Born J, DeKloet ER, Wenz H, Kern W, Fehm HL, 1991 Gluco- and antimineralocorticoid effects on human sleep: a role of central corticosteroid receptors. Am J Physiol 260: E183–188.
Friess E, von Bardeleben U, Wiedemann K, Lauer C, Holsboer F, 1994 Effects of pulsatile cortisol infusion on sleep-EEG and nocturnal growth hormone release in healthy men. J Sleep Res 3: 73–79.
Friess E, Tagaya H, Grethe C, Trachsel L, Holsboer F, 2004 Acute cortisol administration promotes sleep intensity in man. Neuropsychopharmacol 29: 598–604.
Schmid DA, Brunner H, Lauer CJ, et al, 2008 Acute cortisol administration increases sleep depth and growth hormone release in patients with major depression. J Psychiatr Res 42: 991–999.
Gillin JC, Jacobs LS, Fram DH, Snyder F, 1972 Acute effect of a glucocorticoid on normal human sleep [Abstract]. Nature 237: 398–399.
Gillin JC, Jacobs LS, Snyder F, et al, 1974 Effects of ACTH on the sleep of normal subjects and patients with Addison’s disease. Neuroendocrinology 15: 21–31.
Krieger DT, Glick SM, 1974 Sleep EEG stages and plasma growth hormone concentration in states of endogenous and exogenous hypercortisolemia or ACTH elevation. J Clin Endocrinol Metab 39: 986–1000.
Shipley JE, Schteingart DE, Tandon R, et al, 1992 Sleep architecture and sleep apnea in patients with Cushing’s disease. Sleep 15: 514–518.
Steiger A 2007 Neuroendocrinology of Sleep. In: Lajtha A, Blaustein JD (Eds). Handbook of Neurochemistry and Molecular Neurobiology, Plenum Press, New York, pp, 897–926.
Antonijevic IA, Steiger A, 2003 Depression-like changes of the sleep-EEG during high dose corticosteroid treatment in patients with multiple sclerosis. PNEC 28: 780–795.
Buckley T, Duggal V, Schatzberg AF, 2008 The acute and post-discontinuation effects of a glucocorticoid receptor (GR) antagonist probe on sleep and the HPA axis in chronic insomnia: a pilot study. J Clin Sleep Med 4: 235–241.
Murck H, Held K, Ziegenbein M, et al, 2004 Intravenous administration of the neuropeptide galanin has fast antidepressant efficacy and affects the sleep EEG. PNEC 29: 1205–1211.
Murck H, Antonijevic IA, Frieboes RM, et al, 1999 Galanin has REM-sleep deprivation-like effects on the sleep EEG in healthy young men. J Psychiatr Res 33: 225–232.
Unschuld PG, Ising M, Erhardt A, et al, 2008 Polymorphisms in the galanin gene are associated with symptom-severity in female patients suffering from panic disorder. J Affect Disord 105: 177–184.
Gallopin T, Luppi PH, Cauli B, et al, 2005 The endogenous somnogen adenosine excites a subset of sleep-promoting neurons via A2A receptors in the ventrolateral preoptic nucleus. Neuroscience 134: 1377–1390.
Rétey JV, Adam M, Honegger E, et al, 2005 A functional genetic variation of adenosine deaminase affects the duration and intensity of deep sleep in humans. Proc Natl Acad Sci U S A 102: 15676–15681.
Perras B, Pannenborg H, Marshall L, et al, 1999 Beneficial treatment of age-related sleep disturbances with prolonged intranasal vasopressin. J Clin Psychopharmacol 19: 28–36.
van West D, Del-Favero J, Aulchenko Y, et al, 2004 A major SNP haplotype of the arginine vasopressin 1B receptor protects against recurrent major depression. Mol Psychiatry 9: 287–292.
Abdelfatah D, Shaker H, Ismail M, et al, 2009 Nocturnal polyuria and nocturnal arginine vasopressin (AVP): A key factor in the pathophysiology of monosymptomatic nocturnal enuresis. Neurourol Urodyn 28: 506–509.
Gozmen S, Keskin S, Akil I, 2008 Enuresis nocturna and sleep quality. Pediatr Nephrol 23: 1293–1296.
Schneider T, de la Rosette JJ, Michel MC, 2009 Nocturia: a non-specific but important symptom of urological disease. Int J Urol 16: 249–256.
Antonijevic IA, Murck H, Bohlhalter S, et al, 2000 NPY promotes sleep and inhibits ACTH and cortisol release in young men. Neuropharmacol 39: 1474–1481.
Held K, Antonijevic I, Murck H, Kuenzel H, Steiger A, 2006 Neuropeptide Y (NPY) shortens sleep latency but does not suppress ACTH and cortisol in depressed patients and normal controls. Psychoneuroendocrinol 31: 100–107.
Drucker-Colin R, Bernal-Pedraza J, Fernandez-Cancino F, et al, 1984 Is vasoactive intestinal polypeptide (VIP) a sleep factor? [Abstract]. Peptid 5: 837–840.
Murck H, Guldner J, Colla-Miiller M, et al, 1996 VIP decelerates non-REM-REM cycles and modulates hormone secretion during sleep in men. Am J Physiol 271: R905–R911.
Roky R, Obál F Jr, Valatx JL, et al, 1995 Prolactin and rapid eye movement sleep regulation. Sleep 18: 536–542.
Frieboes RM, Murck H, Stalla GK, Antonijevic IA, Steiger A, 1998 Enhanced slow wave sleep in patients with prolactinoma. J Clin Endocrinol Metab 83: 2706–2710.
Antonijevic IA, Murck H, Frieboes RM, Uhr M, Steiger A, 2003 On the role of menopause for sleep-endocrine alterations associated with major depression. PNEC 28: 401–418.
Wiklund I, Karlberg J, Mattsson L-A, 1993 Quality of life of post-menopausal women on a regimen of transdermal estradiol therapy: a double-blind placebo-controlled study [Abstract]. Am J Obstet Gynecol 168: 824–830.
Polo-Kantola P, Erkkola R, Helenius H, Irjala K, Polo O, 1998 When does estrogen replacement therapy improve sleep quality? Am J Obstet Gynecol 178: 1002–1009.
Shin K, Shapiro C, 2003 Menopause, sex hormones, and sleep. Bibolar Disord 5: 106–109.
Antonijevic IA, Stalla GK, Steiger A, 2000 Modulation of the sleep electroencephalogram by estrogen replacement in postmenopausal women. Am J Obstet Gynecol 182: 277–282.
Malacara JM, Pérez-Luque EL, Martínez-Garza S, et al, 2004 The relationship of estrogen receptor-alpha polymorphism with symptoms and other characteristics in post-menopausal women. Maturitas 49:163–169.
Viswanathan AN, Schernhammer ES, 2009 Circulating melatonin and the risk of breast and endometrial cancer in women. Cancer Lett 281: 1–7.
Natale V, Albertazzi P, Zini M, Di Marco R, 2001 Exploration of cyclical changes in memory and mood in postmenopausal women taking sequential combined oestrogen and progestogen preparations. Br J Obstet Gynaecol 108: 286–290.
Montplaisir J, Lorrain J, Denesle R, Petit D, 2001 Sleep in menopause. differential effects of two forms of hormone replacement therapy. Menopause 8: 10–16.
Kalleinen N, Polo O, Himanen SL, Joutsen A, Polo-Kantola P, 2008 The effect of estrogen plus progestin treatment on sleep: a randomized, placebo-controlled, double-blind trial in premenopausal and late postmenopausal women. Climacteric 11: 233–243.
Friess E, Trachsel L, Guldner J, et al, 1995 DHEA administration increases rapid eye movement sleep and EEG power in the sigma frequency range. Am J Physiol 268: E107–E113.
Schiffelholz T, Holsboer F, Lancel M, 2000 High doses of systemic DHEA-sulfate do not affect sleep structure and elicit moderate changes in non-REM sleep. Physiol Behav 69: 399–404.
Dayal M, Sammel MD, Zhao J, et al, 2005 Supplementation with DHEA: effect on muscle size, strength, quality of life, and lipids [Abstract]. J Womens Health (Larchmt) 14: 391–400.
Nikolakopoulou D, Stamatakis A, 2009 The Role of Melatonin in the Pathology of the Cardiovascular System. Nosileftiki, 48: 143–149.
Cajochen C, Kräuchi K, Wirz-Justice A, 2003 Role of melatonin in the regulation of human circadian rhythms and sleep. J Neuroendocrinol 15: 432–437.
Zeitzer JM, Ayas NT, Shea SA, Brown R, Czeisler CA, 2000 Absence of detectable melatonin and preservation of cortisol and thyrotropin rhythms in tetraplegia. J Clin Endocrinol Metab 85: 2189–2196.
Youngstedt SD, Kripke DF, Elliott JA, 1998 Melatonin excretion is not related to sleep in the elderly. J Pineal Res 24: 142–145.
Hughes RJ, Sack RL, Lewy AJ, 1998 The role of melatonin and circadian phase in age-related sleep-maintenance insomnia: assessment in a clinical trial of melatonin replacement. Sleep 21: 52–68.
Zhdanova IV, Wurtman RJ, Morabito C, Piotrovska VR, Lynch HJ, 1996 Effects of low oral doses of melatonin, given 2-4 hours before habitual bedtime, on sleep in normal young humans. Sleep 19: 423–431.
Zhdanova IV, 2005. Melatonin as a hypnotic: Pro. Sleep Med Rev 9: 51–65.
Van den Heuvel CJ, Ferguson SA, Mila Macchi M, Dawson D, 2005 Melatonin as a hypnotic: Con. Sleep Med Rev 9: 71–80.
Gehrman PR, Connor DJ, Martin JL, et al, 2009 Mela-tonin fails to improve sleep or agitation in double-blind randomized placebo-controlled trial of institutionalized patients with Alzheimer disease. Am J Geriatr Psychiatry 17: 166–169.
Srinivasan V, Pandi-Perumal SR, Cardinali DP, et al, 2006 Melatonin in Alzheimer’s disease and other neu-rodegenerative disorders. Behav Brain Funct 2: 15.
Gehrman PR, Connor DJ, Martin JL, et al, 2009 Melatonin fails to improve sleep or agitation in double-blind randomized placebo-controlled trial of institutionalized patients with Alzheimer disease. Am J Geriatr Psychiatry 17: 166–169.
Braam W, Smits MG, Didden R, et al, 2009 Exogenous melatonin for sleep problems in individuals with intellectual disability: a meta-analysis. Dev Med Child Neurol 51: 340–349.
Srinivasan V, Spence DW, Pandi-Perumal SR, et al, 2008 Therapeutic actions of melatonin in cancer: possible mechanisms. Integr Cancer Ther 7: 189–203.
Lyssenko V, Nagorny CL, Erdos MR, et al, 2009 Common variant in MTNR1B associated with increased risk of type 2 diabetes and impaired early insulin secretion. Nat Genet 41: 82–88.
Bouatia-Naji N, Bonnefond A, Cavalcanti-Proença C, et al, 2009 A variant near MTNR1B is associated with increased fasting plasma glucose levels and type 2 diabetes risk. Nat Genet 41: 89–94.
Prokopenko I, Langenberg C, Florez JC, et al, 2009 Variants in MTNR1B influence fasting glucose levels. Nat Genet 41: 77–81.
Wade A, Downie S, 2008 Prolonged-release melatonin for the treatment of insomnia in patients over 55 years. Expert Opin Investig Drugs 17: 1567–1572.
Rivara S, Mor M, Bedini A, Spadoni G, Tarzia G, 2008 Melatonin receptor agonists: SAR and applications to the treatment of sleep-wake disorders. Curr Top Med Chem 8: 954–968.
Simpson D, Curran MP, 2008 Ramelteon: a review of its use in insomnia. Drugs 68: 1901–1919.
Gross PK, Nourse R, Wasser TE, 2009 Ramelteon for insomnia symptoms in a community sample of adults with generalized anxiety disorder: an open label study. J Clin Sleep Med 5: 28–33.
Dobkin RD, Menza M, Bienfait KL, et al, 2009 Ramelteon for the treatment of insomnia in menopausal women. Menopause Int 15: 13–18.
Srinivasan V, Pandi-Perumal SR, Trakht I, et al, 2009 Pathophysiology of depression: role of sleep and the melatonergic system. Psychiatry Res 165: 201–214.
Nishino S, Arrigoni J, Shelton J, et al, 1997 Effects of thyrotropin-releasing hormone and its analogs on daytime sleepiness and cataplexy in canine narcolepsy. J Neurosci 17: 6401–6408.
Hemmeter U, Rothe B, Guldner J, Holsboer F, Steiger A, 1998 Effects of thyrotropin-releasing hormone on the sleep EEG and nocturnal hormone secretion in male volunteers. Neuropsychobiol 38: 25–31.
Staner L, Duval F, Haba J, et al, 2003 Disturbances in hypothalamo pituitary adrenal and thyroid axis identify different sleep EEG patterns in major depressed patients. J Psychiatr Res 37: 1–8.
Staner L, Duval F, Calvi-Gries F, et al, 2001 Morning and evening TSH response to TRH and sleep EEG disturbances in major depressive disorder. Prog Neuropsychopharmacol Biol Psychiatry 25: 535–547.
Nishino S, Ripley B, Overeem S, et al, 2000 Hypocretin (orexin) deficiency in human narcolepsy. Lancet 355: 39–40.
Taylor MM, Samson WK, 2003 The other side of the orexins: endocrine and metabolic actions. Am J Physiol Endocrinol Metab 284: E13–E17.
Nishino S, 2003 The Hypocretin/Orexin System in Health and Disease. Biol Psychiatry 54: 87–95.
Nishino S, Yoshida Y, 2003 History and perspectives of hypocretin/orexin research in sleep medicine. Sleep Biol Rhyth 1: 43–54.
Watson CJ, Soto-Calderon H, Lydic R, Baghdoyan HA, 2008 Pontine reticular formation (PnO) administration of hypocretin-1 increases PnO GABA levels and wake-fulness. Sleep 31: 453–464.
Nishino S, 2007. The hypocretin/orexin receptor: therapeutic prospective in sleep disorders. Expert Opin Investig Drugs 16: 1785–1797.
Saper CB, Chou TC, Scammell TE, 2001 The sleep switch: hypothalamic control of sleep and wakefulness. Trends Neurosci 24: 726–731.
Klein J, Sato A, 2000 The HLA system. Second of two parts. N Engl J Med 343: 782–786.
Hallmayer J, Faraco J, Lin L, et al, 2009 Narcolepsy is strongly associated with the T-cell receptor alpha locus. Nat Genet 41: 708–711.
“Narcolepsy is an autoimmune disorder, Stanford researcher says”. EurekAlert. American Association for the Advancement of Science. 2009-05-03. http://www.eurekalert.org/pub_releases/2009-05/sumc-nia042809.php. Retrieved on 2009-07-12.
Nishino S, Sakurai E, Nevsimalova S, et al, 2009 Decreased CSF histamine in narcolepsy with and without low CSF hypocretin-1 in comparison to healthy controls. Sleep 32: 175–180.
Nishino S, Okuro M, Kotorii N, et al, 2009 Hypocretin/orexin and narcolepsy new basic and clinical insights. Acta Physiol (Oxf) Jun 25. [Epub ahead of print]
Knudsen S, Jennum PJ, Korsholm K, et al, 2008 Normal levels of cerebrospinal fluid hypocretin-1 and daytime sleepiness during attacks of relapsing-remitting multiple sclerosis and monosymptomatic optic neuritis. Mult Scler 14: 734–738.
Aksu K, Firat Güven S, Aksu F, et al, 2009 Obstructive sleep apnoea, cigarette smoking and plasma orexin—A in a sleep clinic cohort. J Int Med Res 37: 331–340.
Asai H, Hirano M, Furiya Y, et al, 2009 Cerebrospinal fluid-orexin levels and sleep attacks in four patients with Parkinson’s disease. Clin Neurol Neurosurg 111: 341–344.
Poceta JS, Parsons L, Engelland S, et al, 2009 Circadian rhythm of CSF monoamines and hypocretin-1 in restless legs syndrome and Parkinson’s disease. Sleep Med 10: 129–133.
Rissling I, Körner Y, Geller F, et al, 2005 Preprohypocretin polymorphisms in Parkinson disease patients reporting “sleep attacks”. Sleep 28: 871–875.
Cortese S, Konofal E, Lecendreux M, 2008 Alertness and feeding behaviors in ADHD: does the hypocretin/orexin system play a role? Med Hypotheses 71: 770–775.
Baranowska B, Baranowska-Bik A, Bik W, et al, 2008 The role of leptin and orexins in the dysfunction of hypothalamo-pituitary-gonadal regulation and in the mechanism of hyperactivity in patients with anorexia nervosa. Neuro Endocrinol Lett 29: 37–40.
Knutson KL, Van Cauter E, 2008 Associations between sleep loss and increased risk of obesity and diabetes. Ann N Y Acad Sci 1129: 287–304.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kotronoulas, G., Stamatakis, A. & Stylianopoulou, F. Hormones, hormonal agents, and neuropeptides involved in the neuroendocrine regulation of sleep in humans. Hormones 8, 232–248 (2009). https://doi.org/10.14310/horm.2002.1239
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.14310/horm.2002.1239