Abstract
Background
Selection of colorectal cancer patients with concomitant peritoneal (PM) and liver metastases (LM) for radical treatment with cytoreductive surgery (CRS), including liver resection and hyperthermic intraperitoneal chemotherapy (HIPEC), needs improvement. This retrospective, monocentric study was designed to evaluate the predictive factors for early recurrence, disease-free survival (DFS), and overall survival (OS) in such patients treated in a referral center.
Methods
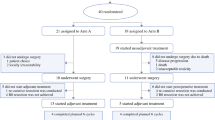
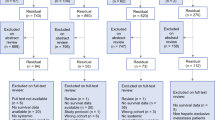
Consecutive colorectal cancer patients with concomitant LM and PM treated with curative intent with perioperative systemic chemotherapy, simultaneous complete CRS, liver resection, and HIPEC in 2011–2022 were included. Clinical, radiological (before and after preoperative chemotherapy), surgical, and pathological data were investigated, along with long-term oncologic outcomes. A multivariate analysis was performed to identify predictive factors associated with early recurrence (diagnosed <6 months after surgery), DFS, and OS.
Results
Of more than 61 patients included, 31 (47.1%) had pT4 and 27 (40.9%) had pN2 primary tumors. Before preoperative chemotherapy, the median number of LM was 2 (1–4). The median surgical PCI (peritoneal carcinomatosis index) was 3 (5–8.5). The median DFS and OS were 8.15 (95% confidence interval [CI] 5.5–10.1) and 34.1 months (95% CI 28.1–53.5), respectively. In multivariate analysis, pT4 (odds ratio [OR] = 4.14 [1.2–16.78], p = 0.032]) and pN2 (OR = 3.7 [1.08–13.86], p = 0.042) status were independently associated with an early recurrence, whereas retroperitoneal lymph node metastasis (hazard ratio [HR] = 39 [8.67–175.44], p < 0.001) was independently associated with poor OS.
Conclusions
In colorectal cancer patients with concomitant PM and LM, an advanced primary tumor (pT4 and/or pN2) was associated with a higher risk of early recurrence following a radical multimodal treatment, whereas RLN metastases was strongly detrimental for OS.



Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71(3):209–49.
Manfredi S, Lepage C, Hatem C, Coatmeur O, Faivre J, Bouvier A-M. Epidemiology and management of liver metastases from colorectal cancer. Ann Surg. 2006;244(2):254–9.
Koppe MJ, Boerman OC, Oyen WJG, Bleichrodt RP. Peritoneal carcinomatosis of colorectal origin: Incidence and current treatment strategies. Ann Surg. 2006;243(2):212–22.
Franko J, Shi Q, Meyers JP, et al. Prognosis of patients with peritoneal metastatic colorectal cancer given systemic therapy: an analysis of individual patient data from prospective randomised trials from the Analysis and Research in Cancers of the Digestive System (ARCAD) database. Lancet Oncol. 2016;17(12):1709–19.
Cremolini C, Antoniotti C, Stein A, et al. Individual patient data meta-analysis of FOLFOXIRI plus bevacizumab versus doublets plus bevacizumab as initial therapy of unresectable metastatic colorectal cancer. J Clin Oncol. 2020;38(28):3314–24.
Molla M, Fernandez-Plana J, Albiol S, et al. Limited liver or lung colorectal cancer metastases. Systemic treatment, surgery, ablation or SBRT. J Clin Med. 2021;10(10):2131.
Rijsemus CJV, Kok NFM, Aalbers AGJ, et al. Diagnostic performance of MRI for staging peritoneal metastases in patients with colorectal cancer after neoadjuvant chemotherapy. Eur J Radiol. 2022;149:110225.
Kambakamba P, Hoti E, Cremen S, Braun F, Becker T, Linecker M. The evolution of surgery for colorectal liver metastases: A persistent challenge to improve survival. Surgery. 2021;170(6):1732–40.
Hübner M, Kusamura S, Villeneuve L, et al. Guidelines for perioperative care in cytoreductive surgery (CRS) with or without hyperthermic IntraPEritoneal chemotherapy (HIPEC): Enhanced Recovery After Surgery (ERAS®) Society Recommendations — Part II: Postoperative management and special considerations. Eur J Surg Oncol. 2020;46(12):2311–23.
Kotani D, Oki E, Nakamura Y, et al. Molecular residual disease and efficacy of adjuvant chemotherapy in patients with colorectal cancer. Nat Med. 2023;29(1):127–34.
Buisman FE, Filipe WF, Galjart B, et al. Adjuvant intra-arterial chemotherapy for patients with resected colorectal liver metastases: a systematic review and meta-analysis. HPB. 2022;24(3):299–308.
Arjona-Sánchez A, Espinosa-Redondo E, Gutiérrez-Calvo A, et al. Efficacy and safety of intraoperative hyperthermic intraperitoneal chemotherapy for locally advanced colon cancer: A phase 3 randomized clinical trial. JAMA Surg [Internet] 2023 [cited 2023 May 16];Available from: https://jamanetwork.com/journals/jamasurgery/fullarticle/2804110
Van Cutsem E, Cervantes A, Adam R, et al. ESMO consensus guidelines for the management of patients with metastatic colorectal cancer. Ann Oncol. 2016;27(8):1386–422.
Di Carlo S, Cavallaro G, La Rovere F, et al. Synchronous liver and peritoneal metastases from colorectal cancer: Is cytoreductive surgery and hyperthermic intraperitoneal chemotherapy combined with liver resection a feasible option? Front Surg. 2022;9:1006591.
Jayne DG, Fook S, Loi C, Seow-Choen F. Peritoneal carcinomatosis from colorectal cancer. Br J Surg. 2002;89(12):1545–50.
Glehen O, Kwiatkowski F, Sugarbaker PH, et al. Cytoreductive surgery combined with perioperative intraperitoneal chemotherapy for the management of peritoneal carcinomatosis from colorectal cancer: A Multi-Institutional Study. J Clin Oncol. 2004;22(16):3284–92.
Kianmanesh R, Scaringi S, Sabate J-M, et al. Iterative cytoreductive surgery associated with hyperthermic intraperitoneal chemotherapy for treatment of peritoneal carcinomatosis of colorectal origin with or without liver metastases. Ann Surg. 2007;245(4):597–603.
Alzahrani N, Ung L, Valle SJ, Liauw W, Morris DL. Synchronous liver resection with cytoreductive surgery for the treatment of liver and peritoneal metastases from colon cancer: results from an Australian centre: Synchronous liver resection with CRS. ANZ J Surg. 2017;87(11):E167–72.
Pinto A, Hobeika C, Philis A, Kirzin S, Carrère N, Ghouti L. Synchronous liver metastases and peritoneal carcinomatosis from colorectal cancer: different strategies for curative treatment? Langenbecks Arch Surg. 2019;404(4):477–88.
de Cuba EMV, Kwakman R, Knol DL, Bonjer HJ, Meijer GA, te Velde EA. Cytoreductive surgery and HIPEC for peritoneal metastases combined with curative treatment of colorectal liver metastases. Cancer Treat Rev. 2013;39(4):321–7.
Flood MP, Das AA, Soucisse ML, et al. Synchronous liver resection, cytoreductive surgery, and hyperthermic intraperitoneal chemotherapy for colorectal liver and peritoneal metastases: A systematic review and meta-analysis. Dis Colon Rectum. 2021;64(6):754–64.
Zou Y, Chen X, Zhang X, et al. Clinical outcomes of curative treatment for colorectal liver metastases combined with cytoreductive surgery and intraperitoneal chemotherapy for peritoneal metastases: a systematic review and meta-analysis of current evidence. Int J Hyperthermia. 2020;37(1):944–54.
Andersen BL, Shapiro CL, Farrar WB, Crespin T, Wells-DiGregorio S. Psychological responses to cancer recurrence: A controlled prospective study. Cancer. 2005;104(7):1540–7.
Navez J, Remue C, Leonard D, et al. Surgical treatment of colorectal cancer with peritoneal and liver metastases using combined liver and cytoreductive surgery and hyperthermic intraperitoneal chemotherapy: Report from a single-centre experience. Ann Surg Oncol. 2016;23(S5):666–73.
Bacalbasa N, Balescu I, Cretoiu D, et al. Determination of whether HIPEC is beneficial in patients with synchronous peritoneal and liver metastases from colorectal cancer (review). Exp Ther Med. 2021;22(5):1267.
Lo Dico R, Faron M, Yonemura Y, et al. Combined liver resection and cytoreductive surgery with HIPEC for metastatic colorectal cancer: Results of a worldwide analysis of 565 patients from the Peritoneal Surface Oncology Group International (PSOGI). Eur J Surg Oncol. 2021;47(1):89–100.
Schwartz LH, Litière S, deVries E, et al. RECIST 1.1—Update and clarification: From the RECIST committee. Eur J Cancer. 2016;62:132–7.
Sasaki K, Morioka D, Conci S, et al. The tumor burden score: A new, “metro-ticket” prognostic tool for colorectal liver metastases based on tumor size and number of tumors. Ann Surg. 2018;267(1):132–41.
Villeneuve L, Thivolet A, Bakrin N, et al. A new internet tool to report peritoneal malignancy extent. PeRitOneal malignancy stage evaluation (PROMISE) application. Eur J Surg Oncol (EJSO). 2016;42(6):877–82.
Jacquet P, Sugarbaker PH. Clinical research methodologies in diagnosis and staging of patients with peritoneal carcinomatosis [Internet]. In: Sugarbaker PH, editor. Peritoneal Carcinomatosis: Principles of Management. Boston, MA: Springer US; 1996 [cited 2023 Apr 16]. pp. 359–74. https://doi.org/10.1007/978-1-4613-1247-5_23
Sugarbaker PH. Peritonectomy procedures [Internet]. In: Ceelen WP (ed). Peritoneal carcinomatosis. Boston, MA: Springer US; 2007 [cited 2023 May 23]. pp. 247–64. https://doi.org/10.1007/978-0-387-48993-3_15
Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250(2):187–96.
Baratti D, Kusamura S, Iusco D, et al. Postoperative complications after cytoreductive surgery and hyperthermic intraperitoneal chemotherapy affect long-term outcome of patients with peritoneal metastases from colorectal cancer: a two-center study of 101 patients. Dis Colon Rectum. 2014;57(7):858–68.
Maggiori L, Goéré D, Viana B, et al. Should patients with peritoneal carcinomatosis of colorectal origin with synchronous liver metastases be treated with a curative intent? A case-control study. Ann Surg. 2013;258(1):116–21.
Cavaliere F, DeSimone M, Virzì S, et al. Prognostic factors and oncologic outcome in 146 patients with colorectal peritoneal carcinomatosis treated with cytoreductive surgery combined with hyperthermic intraperitoneal chemotherapy: Italian multicenter study S.I.T.I.L.O. Eur J Surg Oncol (EJSO). 2011;37(2):148–54.
Lorimier G, Linot B, Paillocher N, et al. Curative cytoreductive surgery followed by hyperthermic intraperitoneal chemotherapy in patients with peritoneal carcinomatosis and synchronous resectable liver metastases arising from colorectal cancer. Eur J Surg Oncol. 2017;43(1):150–8.
Duraj FF, Cashin PH. Cytoreductive surgery and intraperitoneal chemotherapy for colorectal peritoneal and hepatic metastases: a case-control study. J Gastrointest Oncol. 2013;4(4):388–96.
Delhorme J-B, Dupont-Kazma L, Addeo P, et al. Peritoneal carcinomatosis with synchronous liver metastases from colorectal cancer: Who will benefit from complete cytoreductive surgery? Int J Surg. 2016;25:98–105.
Franco F, Monaco D, Volpi A, Marcato C, Larini P, Rossi C. The role of arterial embolization in blunt splenic injury. Radiol Med. 2011;116(3):454–65.
Schell F, Kefleyesus A, Benzerdjeb N, et al. Influence of extraperitoneal metastases on the curative-intent management of colorectal peritoneal metastases. Ann Surg Oncol. 2023. https://doi.org/10.1245/s10434-023-13279-9.
Japanese Society for Cancer of the Colon and Rectum, Watanabe T, Itabashi M, et al. Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol. 2012;17(1):1–29.
Zizzo M, Dorma MPF, Zanelli M, et al. Long-term outcomes of surgical resection of pathologically confirmed isolated para-aortic lymph node metastases in colorectal cancer: A systematic review. Cancers. 2022;14(3):661.
Aylward C, Noori J, Tyrrell J, et al. Survival outcomes after synchronous para-aortic lymph node metastasis in colorectal cancer: A systematic review. J Surg Oncol. 2023;127(4):645–56.
Fadel MG, Ahmed M, Pellino G, et al. Retroperitoneal lymph node dissection in colorectal cancer with lymph node metastasis: A systematic review. Cancers. 2023;15(2):455.
Bae SU, Hur H, Min BS, Baik SH, Lee KY, Kim NK. Which patients with isolated para-aortic lymph node metastasis will truly benefit from extended lymph node dissection for colon cancer? Cancer Res Treat. 2018;50(3):712–9.
Gagnière J, Dupré A, Chabaud S, Peyrat P, Meeus P, Rivoire M. Retroperitoneal nodal metastases from colorectal cancer: Curable metastases with radical retroperitoneal lymphadenectomy in selected patients. Eur J Surg Oncol (EJSO). 2015;41(6):731–7.
Lee J, Chang JS, Shin SJ, et al. Incorporation of radiotherapy in the multidisciplinary treatment of isolated retroperitoneal lymph node recurrence from colorectal cancer. Ann Surg Oncol. 2015;22(5):1520–6.
Shu P, Ouyang G, Wang F, et al. The role of radiotherapy in the treatment of retroperitoneal lymph node metastases from colorectal cancer. CMAR. 2020;12:8913–21.
Nakai N, Yamaguchi T, Kinugasa Y, et al. Diagnostic value of computed tomography (CT) and positron emission tomography (PET) for paraaortic lymph node metastasis from left-sided colon and rectal cancer. Asian J Surg. 2020;43(6):676–82.
Rosenthal MH, Kim KW, Fuchs CS, Meyerhardt JA, Ramaiya NH. CT predictors of overall survival at initial diagnosis in patients with stage IV colorectal cancer. Abdom Imaging. 2015;40(5):1170–6.
Hale GR, Teplitsky S, Truong H, Gold SA, Bloom JB, Agarwal PK. Lymph node imaging in testicular cancer. Transl Androl Urol. 2018;7(5):864–74.
Kwak JY, Kim JS, Kim HJ, Ha HK, Yu CS, Kim JC. Diagnostic value of FDG-PET/CT for lymph node metastasis of colorectal cancer. World J Surg. 2012;36(8):1898–905.
Klaver CEL, Wasmann KATGM, Verstegen M, et al. Postoperative abdominal infections after resection of T4 colon cancer increase the risk of intra-abdominal recurrence. Eur J Surg Oncol. 2018;44(12):1880–8.
Zhang Y, Qin X, Chen W, et al. Risk factors for developing peritoneal metastases after curative surgery for colorectal cancer: A systematic review and meta-analysis. Colorectal Dis. 2021;23(11):2846–58.
Simkens GA, Van Oudheusden TR, Nieboer D, et al. Development of a prognostic nomogram for patients with peritoneally metastasized colorectal cancer treated with cytoreductive surgery and HIPEC. Ann Surg Oncol. 2016;23(13):4214–21.
Vassos N, Förtsch T, Aladashvili A, Hohenberger W, Croner RS. Repeated cytoreductive surgery (CRS) with hyperthermic intraperitoneal chemotherapy (HIPEC) in patients with recurrent peritoneal carcinomatosis. World J Surg Oncol. 2016;14(1):42.
Elias D, De Baere T, Smayra T, Ouellet JF, Roche A, Lasser P. Percutaneous radiofrequency thermoablation as an alternative to surgery for treatment of liver tumour recurrence after hepatectomy. Br J Surg. 2002;89(6):752–6.
Malla M, Loree JM, Kasi PM, Parikh AR. Using circulating tumor DNA in colorectal cancer: Current and evolving practices. J Clin Oncol. 2022;40(24):2846–57.
Engstrand J, Nilsson H, Strömberg C, Jonas E, Freedman J. Colorectal cancer liver metastases – a population-based study on incidence, management and survival. BMC Cancer. 2018;18(1):78.
Downs-Canner S, Shuai Y, Ramalingam L, et al. Safety and efficacy of combined resection of colorectal peritoneal and liver metastases. J Surg Res. 2017;219:194–201.
Elias D, Faron M, Goéré D, et al. A simple tumor load-based nomogram for surgery in patients with colorectal liver and peritoneal metastases. Ann Surg Oncol. 2014;21(6):2052–8.
Esquivel J, Sticca R, Sugarbaker P, et al. Cytoreductive surgery and hyperthermic intraperitoneal chemotherapy in the management of peritoneal surface malignancies of colonic origin: a consensus statement. Society of Surgical Oncology. Ann Surg Oncol. 2007;14(1):128–33.
Bhatt A, Rousset P, Benzerdjeb N, et al. Prospective correlation of the radiological, surgical and pathological findings in patients undergoing cytoreductive surgery for colorectal peritoneal metastases: implications for the preoperative estimation of the peritoneal cancer index. Colorectal Dis. 2020;22(12):2123–32.
Faron M, Macovei R, Goéré D, Honoré C, Benhaim L, Elias D. Linear relationship of peritoneal cancer index and survival in patients with peritoneal metastases from colorectal cancer. Ann Surg Oncol. 2016;23(1):114–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
OG is consultant for GAMIDA.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplemental Fig. 1
A 69-year-old female was referred for synchronous PM and LM from sigmoid pT4N2 adenocarcinoma. Initial CT scan at portal phase revealed 9 LM, the largest of which measured 35 mm (arrow) (A). Initial PCI score was 4, including a 10-mm peritoneal nodule of the left pre-renal fascia (dotted arrow) (B). Preoperative CT scan after 12 cycles of Folfirinox-Cetuximab showed a significant reduction in size of the nine LM (partial response according RECIST 1.1 classification), the largest measuring 25 mm with necrotic modification (arrow) (C). Peritoneal analysis assessed the PCI score at 3, with reduction in size of the nodule, and a thickening of the left pre-renal fascia (dotted arrow) (D). PCI score was assessed at 5 intraoperatively. The patient had a complete resection of the PM (completeness of cytoreduction score at 0) with four hepatic wedge resections combined with five radiofrequency ablations. The patient had a postoperative ileus. The patient presented an early recurrence at 2 months, treated with chemotherapy. The patient was still alive 14 months after surgery (JPG 69 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Grange, R., Rousset, P., Williet, N. et al. Metastatic Colorectal Cancer Treated with Combined Liver Resection, Cytoreductive Surgery, and Hyperthermic Intraperitoneal Chemotherapy (HIPEC): Predictive Factors for Early Recurrence. Ann Surg Oncol 31, 2378–2390 (2024). https://doi.org/10.1245/s10434-023-14840-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-14840-2