Abstract
Background
Standardization of surgical and pathologic techniques is crucial to the interpretation of studies evaluating adjuvant therapies for pancreatic cancer (PC).
Methods
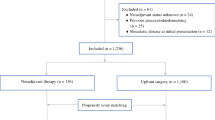
To assess the degree to which treatment administered prior to enrollment of patients in trials of adjuvant therapy is quality controlled, the operative and pathology reports of patients in American College of Surgeons Oncology Group (ACOSOG) Z5031—a national trial of chemoradiation following pancreaticoduodenectomy (PD)—were rigorously evaluated. We analyzed variables with the potential to influence staging or outcome.
Results
80 patients reported to have undergone R0 (75%) or R1 (25%) pylorus-preserving (38%) or standard (62%) PD were evaluated. A search for metastases was documented in 96% of cases. The proximity of the tumor to the superior mesenteric vein was reported in 69%; vein resection was required in 9% and lateral venorrhaphy in 14%. The method of dissection along the superior mesenteric artery (SMA) was described in 68%, being ultrasonic dissection (17%), stapler (24%), and clamp and cut (59%). SMA skeletonization was described in 25%, and absence of disease following resection was documented in 24%. The surgeon reported marking the critical SMA margin in 25%; inking was documented in 65% of cases and evaluation of the SMA margin was reported in 47%. A range of 1–49 lymph nodes was evaluated. Only 34% of pathology reports met College of American Pathologists criteria.
Conclusions
Trials of adjuvant therapy following PD suffer from a lack of standardization and quality control prior to patient enrollment. These data suggest areas for improvement in the design of multidisciplinary treatment protocols.

Similar content being viewed by others
References
Howard TJ, Krug JE, Yu J, Zyromski NJ, Schmidt CM, Jacobson LE, et al. A margin-negative R0 resection accomplished with minimal postoperative complications is the surgeon’s contribution to long-term survival in pancreatic cancer. J Gastrointest Surg. 2006;10:1338–45 (discussion 1345–6).
Katz MH, Wang H, Fleming JB, Sun CC, Hwang RF, Wolff RA, et al. Long-term survival after multidisciplinary management of resected pancreatic adenocarcinoma. Ann Surg Oncol. 2009;16:836–47.
Pancreatic adenocarcinoma V.2.2010. NCCN Clinical Practice Guidelines in Oncology. 2009. Available at: http://www.nccn.org/professionals/physicians_gls/PDF/pancreatic.pdf. Accessed 16 August 2010.
Kalser MH, Ellenberg SS. Pancreatic cancer. Adjuvant combined radiation and chemotherapy following curative resection. Arch Surg. 1985;120:899–903.
Neoptolemos JP, Dunn JA, Stocken DD, Almond J, Link K, Beger H, et al. Adjuvant chemoradiotherapy and chemotherapy in resectable pancreatic cancer: a randomised controlled trial. Lancet. 2001;358:1576–85.
Neoptolemos JP, Stocken DD, Dunn JA, Almond J, Beger HG, Pederzoli P, et al. Influence of resection margins on survival for patients with pancreatic cancer treated by adjuvant chemoradiation and/or chemotherapy in the ESPAC-1 randomized controlled trial. Ann Surg. 2001;234:758–68.
Neoptolemos JP, Stocken DD, Friess H, Bassi C, Dunn JA, Hickey H, et al. A randomized trial of chemoradiotherapy and chemotherapy after resection of pancreatic cancer. N Engl J Med. 2004;350:1200–10.
Oettle H, Post S, Neuhaus P, Gellert K, Langrehr J, Ridwelski K, et al. Adjuvant chemotherapy with gemcitabine vs. observation in patients undergoing curative-intent resection of pancreatic cancer: a randomized controlled trial. JAMA. 2007;297:267–77.
Nelson H, Petrelli N, Carlin A, Couture J, Fleshman J, Guillem J, et al. Guidelines 2000 for colon and rectal cancer surgery. J Natl Cancer Inst. 2001;93:583–96.
Vauthey JN, Dixon E. AHPBA/SSO/SSAT consensus conference on resectable and borderline resectable pancreatic cancer: rationale and overview of the conference. Ann Surg Oncol. 2009;16:1725–6.
American Joint Committee on Cancer. Exocrine pancreas. In: Greene FL, Page DL, Fleming ID, et al., editors. AJCC cancer staging manual. 6th ed. Chicago: Springer; 2002. pp 157–64.
College of American Pathologists Cancer Protocols. Pancreas (exocrine); 2009. Available at: http://www.cap.org/apps/docs/committees/cancer/cancer_protocols/2009/PancreasExo_09protocol.pdf. Accessed 16 August 2010.
American Joint Committee on Cancer. Exocrine pancreas. In: Edge SB, Byrd DR, Compton CC, et al., editors. AJCC cancer staging manual. 7th ed. Chicago: Springer; 2009. pp 241–9.
Picozzi VJ, Abrams RA, Decker PA, Traverso LW, O’Reilly EM, Greeno E, et al. Multicenter, phase II trial of adjuvant therapy for resected pancreatic cancer using cisplatin, 5-fluorouracil, and interferon-alfa-2b-based chemoradiation: ACOSOG Trial Z05031. Ann Oncol. 2010 [Epub ahead of print].
Raut CP, Tseng JF, Sun CC, Wang H, Wolff RA, Crane CH, et al. Impact of resection status on pattern of failure and survival after pancreaticoduodenectomy for pancreatic adenocarcinoma. Ann Surg. 2007;246:52–60.
Phillips RK, Hittinger R, Blesovsky L, Fry JS, Fielding LP. Local recurrence following ‘curative’ surgery for large bowel cancer: I. The overall picture. Br J Surg. 1984;71:12–6.
Holm T, Johansson H, Cedermark B, Ekelund G, Rutqvist LE. Influence of hospital- and surgeon-related factors on outcome after treatment of rectal cancer with or without preoperative radiotherapy. Br J Surg. 1997;84:657–63.
Kockerling F, Reymond MA, Altendorf-Hofmann A, Dworak O, Hohenberger W. Influence of surgery on metachronous distant metastases and survival in rectal cancer. J Clin Oncol. 1998;16:324–9.
Stocchi L, Nelson H, Sargent DJ, O’Connell MJ, Tepper JE, Krook JE, et al. Impact of surgical and pathologic variables in rectal cancer: a United States community and cooperative group report. J Clin Oncol. 2001;19:3895–902.
Gruen RL, Pitt V, Green S, Parkhill A, Campbell D, Jolley D. The effect of provider case volume on cancer mortality: systematic review and meta-analysis. CA Cancer J Clin. 2009;59:192–211.
Kuhlmann KF, de Castro SM, Wesseling JG, ten Kate FJ, Offerhaus GJ, Busch OR, et al. Surgical treatment of pancreatic adenocarcinoma; actual survival and prognostic factors in 343 patients. Eur J Cancer. 2004;40:549–58.
Winter JM, Cameron JL, Campbell KA, Arnold MA, Chang DC, Coleman J, et al. 1423 pancreaticoduodenectomies for pancreatic cancer: a single-institution experience. J Gastrointest Surg. 2006;10:1199–210 (discussion 1210–1).
Menon KV, Gomez D, Smith AM, Anthoney A, Verbeke CS. Impact of margin status on survival following pancreatoduodenectomy for cancer: the Leeds Pathology Protocol (LEEPP). HPB (Oxford). 2009;11:18–24.
Katz MH, Hwang R, Fleming JB, Evans DB. Tumor-node-metastasis staging of pancreatic adenocarcinoma. CA Cancer J Clin. 2008;58:111–25.
Evans DB, Hess KR, Pisters PW. ESPAC-1 trial of adjuvant therapy for resectable adenocarcinoma of the pancreas. Ann Surg. 2002;236:694 (author reply 694–6).
Baque P, Iannelli A, Delotte J, de Peretti F, Bourgeon A. Division of the right posterior attachments of the head of the pancreas with a linear stapler during pancreaticoduodenectomy: vascular and oncological considerations based on an anatomical cadaver-based study. Surg Radiol Anat. 2009;31:13–7.
Evans DB, Pisters PW. Novel applications of endo GIA linear staplers during pancreaticoduodenectomy and total pancreatectomy. Am J Surg. 2003;185:606–7.
Staley CA, Cleary KR, Abbruzzese JL, Lee JE, Ames FC, Fenoglio CJ, et al. The need for standardized pathologic staging of pancreaticoduodenectomy specimens. Pancreas. 1996;12:373–80.
Chatelain D, Flejou JF. [Pancreatectomy for adenocarcinoma: prognostic factors, recommendations for pathological reports]. Ann Pathol. 2002;22:422–31.
Luttges J, Zamboni G, Kloppel G. Recommendation for the examination of pancreaticoduodenectomy specimens removed from patients with carcinoma of the exocrine pancreas. A proposal for a standardized pathological staging of pancreaticoduodenectomy specimens including a checklist. Dig Surg. 1999;16:291–6.
Khalifa MA, Maksymov V, Rowsell C. Retroperitoneal margin of the pancreaticoduodenectomy specimen: anatomic mapping for the surgical pathologist. Virchows Arch. 2009;454:125–31.
Verbeke CS, Leitch D, Menon KV, McMahon MJ, Guillou PJ, Anthoney A. Redefining the R1 resection in pancreatic cancer. Br J Surg. 2006;93:1232–7.
Acknowledgment
Supported by funding from the US National Institutes of Health to the American College of Surgeons Oncology Group, grant U10 CA 76001.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
This study was conducted for the American College of Surgeons Oncology Group.
Rights and permissions
About this article
Cite this article
Katz, M.H.G., Merchant, N.B., Brower, S. et al. Standardization of Surgical and Pathologic Variables is Needed in Multicenter Trials of Adjuvant Therapy for Pancreatic Cancer: Results from the ACOSOG Z5031 Trial. Ann Surg Oncol 18, 337–344 (2011). https://doi.org/10.1245/s10434-010-1282-y
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-010-1282-y