Abstract
Background
There is extensive evidence for the cost-effectiveness of programmatic and additional tuberculosis (TB) interventions, but no studies have employed the social return on investment (SROI) methodology. We conducted a SROI analysis to measure the benefits of a community health worker (CHW) model for active TB case finding and patient-centered care.
Methods
This mixed-method study took place alongside a TB intervention implemented in Ho Chi Minh City, Viet Nam, between October-2017 – September-2019. The valuation encompassed beneficiary, health system and societal perspectives over a 5-year time-horizon. We conducted a rapid literature review, two focus group discussions and 14 in-depth interviews to identify and validate pertinent stakeholders and material value drivers. We compiled quantitative data from the TB program’s and the intervention’s surveillance systems, ecological databases, scientific publications, project accounts and 11 beneficiary surveys. We mapped, quantified and monetized value drivers to derive a crude financial benefit, which was adjusted for four counterfactuals. We calculated a SROI based on the net present value (NPV) of benefits and investments using a discounted cash flow model with a discount rate of 3.5%. A scenario analysis assessed SROI at varying discount rates of 0-10%.
Results
The mathematical model yielded NPVs of US$235,511 in investments and US$8,497,183 in benefits. This suggested a return of US$36.08 for each dollar invested, ranging from US$31.66-US39.00 for varying discount rate scenarios.
Conclusions
The evaluated CHW-based TB intervention generated substantial individual and societal benefits. The SROI methodology may be an alternative for the economic evaluation of healthcare interventions.
Similar content being viewed by others
Background
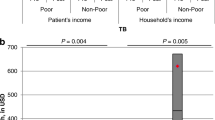
Tuberculosis (TB) remains a global public health challenge [1]. About 10 million people worldwide contracted TB in 2019 and almost half a million individuals developed multidrug-resistant TB (MDR-TB) [2]. Individuals with TB often face barriers to accessing and completing treatment throughout the cascade of care [3]. Pre-treatment barriers can be logistical, socioeconomic or sociocultural in nature, often working in unison to cause patients to delay or forego health-seeking [4, 5]. After enrollment, the direct and economic costs of productivity loss from TB treatment constitute major burdens [5]. Drug resistance severely exacerbates burdens related to disease and treatment, and associated risk of unfavorable outcomes [6]. TB survivors often carry long-term medical and social sequelae and elevated risk of chronic recurrence [7, 8]. The impoverishing effects of TB on affected households have been widely documented [9]. The average cost of TB care was equivalent to 58% of reported annual individual income and 39% of reported household income. These costs as a proportion of income were higher for people with low income and for those with MDR-TB [10]. These economic disincentives throughout the care cascade contribute to loss to follow-up (LTFU), chronic morbidity, development of drug resistance and continued community transmission [11, 12]. Realizing that progress in fighting TB needs to be measured by more than clinical outcomes, the WHO included the elimination of catastrophic cost, defined as incurring TB-related costs over 20% of annual household income, as one of three core performance indicators in its End TB Strategy [13,14,15].
Global societal costs attributable to TB were estimated to be US$4 billion each year in direct healthcare and US$12 billion in lost productivity [16]. Across 135 low- and middle-income countries (LMIC), total spending on TB increased 3.9% per year between 2000 and 2017, with overall government spending for detected and missed cases reaching US$6.9 billion in 2017 [17]. From the health system perspective, the average treatment cost was US$6,667 per case of drug-susceptible TB (DS-TB) and US$46,219 per case of MDR-TB [18].
Given these costs, many studies have documented the cost-effectiveness of TB interventions [19,20,21,22,23]. Targeted TB interventions were cited to produce a return of US$56 per dollar spent with benefit-cost ratios (BCR) ranging from 11–192:1 [24]. A modelling study found active case finding (ACF) to be a cost-effective tool in India, China, and South Africa as the cost per disability-adjusted life year (DALY) averted was lower than the per capita gross domestic product [25]. Besides ACF, engagement of all stakeholders in the community [22, 26, 27] or private sector [28,29,30], is another strategy commonly identified as cost-effective. Regarding MDR-TB, the BCR for ACF as well as diagnosis and treatment of MDR-TB were cited to be US$32 (6–47:1) and US$2 (0–23:1), respectively [24]. Concordantly, a systematic review found MDR-TB treatment to be a highly cost-effective intervention in LMICs [31].
Despite much evidence, there is large heterogeneity in TB intervention valuations, including methodology, design and perspective [32]. Health economic analyses use basic methods including reporting of costs, [33] and cost minimization [34, 35] expressed as lowest cost to achieve one empirical effect, e.g., TB case detection, and BCRs. More sophisticated procedures employed cost-utility analyses, [23] defined as costs to achieve unified effects expressed as Quality-adjusted life-year (QALY) or DALY, and cost-effectiveness analyses [36, 37] estimating the incremental costs to achieve an incremental empirical effect, e.g., additional costs per additional successful TB treatment. Designs can be empirical (retrospective case analyses, randomized trials) or mathematical (decision-tree and Markov simulation models) [38]. These analyses can assume patient [39], health system [40], and sometimes, societal perspectives [41].
An alternative economic evaluation method to achieve this comprehensive perspective involves estimating social return on investment (SROI), [42] defined as the monetary value generated for society for every unit of money invested. An SROI is a simultaneous valuation of personal, social and community outcomes [43]. By capturing the benefit and costs from multiple stakeholder perspectives, SROI offers a more comprehensive assessment of an intervention’s net benefit for society as a whole and thus a more compelling analysis for policy-makers. There is a growing body of evidence employing the SROI methodology in various settings and for diverse development and healthcare interventions with demonstrated value in program evaluation [44,45,46,47]. However, evaluations employing SROI for TB interventions remain scarce as our literature review found no such published studies. A systematic review in 2019, found only eight peer-reviewed SROI studies for health, only one of which was conducted in a LMIC [48].
In 2020, there were 172,000 persons with incident TB, including 8,400 persons with MDR-TB, and 10,400 TB-related deaths in Viet Nam [49]. Nevertheless, the government remains committed to ending TB by 2030 [50]. The National TB Control Programme (NTP) identified a greater engagement of community health workers (CHW) as a key strategy to achieve this goal [51]. Between 2017 and 2019, Friends for International TB Relief piloted a TB intervention in Ho Chi Minh City (HCMC), Viet Nam, called Proper Care. The project employed CHW to systematically screen vulnerable populations and provide support to patients on treatment. Prior evaluations reported this intervention model increased case detection [52] as well as reduced LTFU [53] and catastrophic cost incurrence [54]. The current study evaluated the economic impact of Proper Care via the SROI method to offer further evidence to national stakeholders for intensified intervention towards ending TB.
Methods
Study design
This was a mixed-methods study to construct an evaluative SROI analysis with a 5-year time-horizon on the economic benefit of a CHW-based TB intervention.
The planning and design of this mixed-method study was developed based on the strategies and procedures outlined by Creswell [55]. Accordingly, the transformative mixed-method strategy was selected whereby a theoretical lens was applied based on a rapid literature review followed by the qualitative research to apply an inductive approach and quantitative methods to expand findings from the prior two strategies.
The literature review framed the health economic evaluation and qualitative research identified and synthesized pertinent stakeholders and material value drivers. Our quantitative methods encompassed the development of the model components and calculation of the discounted cash flow (DCF) to arrive at the SROI estimate.
This study was conducted according to the guidelines and principles of the Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement [56].
Intervention
The intervention was additional to routine TB program activities and took place from Oct-2017 to Sep-2019 in three districts of HCMC, Viet Nam, with a population of 1,465,819. CHWs systematically screened household and first-degree contacts of active TB patients and key vulnerable populations, and then referred persons with symptoms suggestive of TB or collected and transported sputum to the District TB Unit (DTU) for further evaluation. Health-seeking persons received a study-subsidized chest X-ray and free sputum testing as per national treatment guidelines [57]. Individuals diagnosed with TB were initiated on appropriate treatment according to NTP guidelines. CHWs provided adherence counseling and psychosocial support to all patients treated at the DTU. For destitute families, CHWs sometimes provided self-financed nutrition support and transport to the DTU for follow-up consultations. CHWs were supported by a site coordinator responsible for supervision and coordination. The intervention was previously described [53, 58]. In total, the intervention involved approximately 20 public health staff at the DTUs and provincial lung hospital and 151 CHWs and coordinators in the community. The total number of persons with TB engaged before and during the intervention was 7,776 and the number of family members and other vulnerable persons screened for TB by the intervention was 38,130 (Supplementary information – TB-SROI Model).
Model development procedures
The SROI analysis contained five stages based on the guidelines and principles developed by Social Value UK [59]: (1) identifying stakeholders and value drivers, (2) calculating inputs and outputs, (3) calculating crude social returns on investment, (4) incorporating counterfactuals, and (5) calculating net present value (NPV) and SROI (Fig. 1). Value drivers are defined as sources of value creation or destruction. Net present value is defined as the current discounted value of future cash flows after subtracting any investments.
Stage 1: We identified hypothetical stakeholders and value drivers based on a rapid literature review [60, 61]. In summary, this rapid review aimed to assess existing knowledge on the application of SROIs for valuation of interventions in health and TB using systematic review methods, but conceding breadth or depth by limiting aspects of the process to compensate for time limitations [62]. The detailed search methodology is provided in the Supplementary information – Rapid literature review. To validate the stakeholders and value drivers, we conducted two focus group discussions (FGD, n = 15) and 14 in-depth interviews (IDI). Participants were purposively sampled to achieve information power [63]. Interviews were conducted using a topic guide about the benefits of the intervention, challenges faced, and potential negative impacts of the intervention on individuals and society. Audio recordings were collected and transcribed in the language of the interview (Vietnamese or English). The audio and transcriptions were compared to ensure accuracy. Interviews in Vietnamese were professionally translated and independently verified. Inconsistencies in the translation were discussed among a group of translators until consensus was reached. Qualitative data were coded and analyzed in Dedoose v8.3.17 (SocioCultural Research Consultants; Los Angeles, CA). We used content framework analysis for qualitative research [64, 65] to validate the stakeholders and value drivers.
Stage 2: After identification of pertinent stakeholders and material value drivers, we calculated the associated inputs and outputs. Inputs were financial and non-monetary stakeholder resources to enable interventions such as activity implementation budgets and self-financed payments by CHWs and site coordinators for patient support. All costs were converted to US$ at an average rate of US$1 = VNĐ22,921 (2017–2018, oanda.com). Outputs were a quantitative summary of each of the value drivers by stakeholder. Sample outputs included the additional TB patients detected and linked to treatment through ACF, number of project staff hired and compensated for their efforts, and amount of additional funding obtained throughout the intervention period. The number of additional persons with TB detected (additionality) was determined based on a comparison with operational and clinical data from the baseline period (2016) [66]. Quantitative inputs and outputs for each value driver were derived from primary and secondary data sources. One primary data source entailed a quantitative survey informed by the qualitative research activities (provided in the supplemental information). This survey included 13 questions and was fielded by study staff among 11 project beneficiaries through in-person/phone conversations. The survey collected data on previous and current monthly income, average length of routine and after-hour work, and material out-of-pocket costs for the intervention. Additional primary sources included the intervention’s operational data repository, routine surveillance data from the NTP, human resource and payroll registers, and project accounting records. Secondary data sources included published scientific literature and ecological databases.
Stage 3: The operational outputs of each value driver were monetized to obtain a crude financial return. The monetization process used financial proxies to arrive at price assumptions obtained from primary and secondary sources as described above. Financial proxies assign a monetary value to an operational indicator or activity. An example of a financial proxy is the minimum wage as a proxy for average income per patient per year to estimate the value of individual benefit for persons detected and cured of TB. Monetary benefits were positive and negative, and encompassed beneficiary, health system and societal perspectives. Monetization procedures were tailored to previously identified relevant stakeholders: (1) TB-affected patients and households; (2) site coordinators and CHWs; (3) NTP; (4) municipal government; and (5) Viet Nam TB ecosystem. In this case, ecosystem is defined as the overall amount of available funds for TB care and prevention in Viet Nam.
For TB-affected patients and households, we calculated the additional income earned after being cured of TB for persons who were detected and linked to treatment through ACF. We further quantified the reduction of mortality rates in the ACF and Passive Case Finding (PCF) cohorts in monetary terms. The price assumption for the additional income generated was based on the minimum wage legislation for the intervention area [67]. Lastly, we also included pre-treatment cost avoidance through early detection via ACF using values reported by the Viet Nam national patient cost survey [39].
Crude financial returns on investment for site coordinators and CHWs were calculated by summation of the salaries (fixed compensation) and incentives (variable compensation) paid over the course of the project. The model incorporated a negative impact from one of the field staff contracting TB. To quantify this return in monetary terms, we used household costs and health care system costs for DS-TB treatment from published scientific literature [39].
First, returns generated for the NTP included the fixed and variable stipends paid to district and provincial staff to compensate for time and effort dedicated to the study that were incremental to their routine responsibilities. Other positive returns such as increased capacity building and awareness about TB and their role as well as improved performance and ranking within the government’s performance appraisal system were excluded according to the SROI principles of materiality and not over-claiming. Based on the same principle, we did not incorporate negative returns such as detraction from the daily responsibilities resulting from participation in the study. Second, the impact of the NTP included MDR-TB treatment cost avoidance calculated based on the difference in treatment outcomes of LTFU, treatment failure and transfer out measured during the intervention in comparison to the pre-intervention baseline period. Clinical assumptions and financial proxies for the monetization of the MDR-TB cost avoidance were obtained from published literature [33, 68].
The municipal government benefitted from the macroeconomic value of TB-related mortalities averted. We employed the Value of Statistical Life (VSL) method to calculate the VSL-Year (VSLY) based on average life expectancy in Viet Nam. To localize the US-based VSLY results, we employed the benefits-transfer method at unit elasticity to obtain VSLYs for Viet Nam [69]. The benefits-transfer method relies on the GDP ratio of two countries and has been used to translate VSL between high-income countries with reliable data from hedonic wage studies to low- and middle-income countries that tend to lack these data [70]. Macroeconomic productivity loss was estimated for persons with TB detected through ACF or PCF, who completed treatment during the study period.
To assess the benefits to the Viet Nam TB ecosystem, we counted all additional resources mobilized during the study period that were based on the Proper Care model. These resources represent the leverage gained from the initial investment in the Proper Care project that resulted in the co-financing from two additional funding mechanisms.
Stage 4: The SROI method integrates four counterfactuals to adjust crude financial returns from the previous stage. These adjustment parameters include: (1) deadweight; (2) displacement; (3) attribution; and (4) drop-off [71]. Deadweight represents the benefits that would have arisen irrespective of the intervention. Displacement represents any activity and associated economic gains the intervention displaced through its activities. Attribution represents the amount of impact that can be attributed to project activities and contributions. Drop-off represents a decline in recurring value generated from the project over time [59].
Stage 5: A DCF model was used to calculate the NPV of the monetary benefits and costs over a 5-year time-horizon to appropriately measure the impact of mortality avoidance. Thus, even though several value drivers would generate impact beyond the evaluation horizon, this impact was truncated after a 5-year projection to avoid overestimation of the impact. The discount rate to estimate the NPV was 3.5% based on the 2017 reported inflation rate in Viet Nam [72]. A sensitivity analysis tested the effect of applying a discount rate ranging from 0 to 10% on NPV and SROI.
Ethical considerations
The study was conducted in accordance with the Helsinki Declaration (7th Revision) as well as the guidelines and principles of the Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement. We obtained ethical approval for the study from the Institutional Review Board of the Pham Ngoc Thach Hospital in Ho Chi Minh City (129/HDDD-PNT). All participants provided informed, written consent and all data were anonymized prior to analysis.
Results
Stakeholders and value drivers
Our rapid literature review resulted in 65 search results of which all titles were reviewed. We excluded 12 studies not relevant to our study or that were published prior to the year 2000, and read the abstracts of the remaining 53 studies. Based on these abstracts, we reviewed 12 manuscripts in detail. This yielded eight stakeholders and 25 positive and negative value drivers of the intervention (Fig. 2). Based on data gathered through the FGDs and IDIs, we narrowed the scope to five relevant stakeholders and 14 material value drivers. Table 1 presents a summary and representative quotations of the qualitative data for the validation of the hypothesized value drivers by individual stakeholder groups, while Table 2 presents a summary of the perceived benefits and costs by stakeholder groups.
Across stakeholder groups, participants identified the clinical, economic and epidemiological benefits provided to individuals and society as the intervention’s main value driver. Patients appreciated the socioeconomic and psychosocial support from site coordinators and CHWs to help them recover from the illness.
“I tried to follow the treatment. Luckily, I had the help from my healthcare worker. She encouraged me and helped me receive my medicine. Overall, I was very happy and even went to hug her and said thank you. Without her, I don’t know what I would have done.” – Male, TB Patient, Painter.
Site coordinators and CHWs expressed a strong personal satisfaction about simultaneously earning an income, expanding their knowledge, and contributing to society. These stakeholders also frequently mentioned earlier disease detection and increased access to healthcare services for their patients as one of the project’s key value propositions.
“When participating in the project, I have a job to do, and have income for myself as well as more knowledge.” – Male, Site coordinator 1.
TB program staff and municipal government representatives emphasized the benefit for citizens in their municipality and for society in general. They also highlighted their improved performance on public health indicators. Furthermore, they identified the strengthened collaboration between TB programs and local governments as a key benefit.
“In terms of benefits, it is huge. If [the intervention] reduces the number of patients of this communicable disease, the transmission rate will decline. When the transmission rate decreases, the number of TB patients will decrease. The number of TB patients decreasing means the economic burden on a locality or district or city will decline. It’s one of the most important benefits of this program, because the lower the number of TB patients, the more healthy people can work and produce for society.” – Male, DTU Officer 1.
Key benefits included increased funding for the Viet Nam TB ecosystem, greater value perception of the intervention and its investment, and gains in sponsor reputation. Moreover, the intervention facilitated a strong partnership between all relevant groups and elucidated grassroots realities to national actors.
“It really helped us to inform national policy. Back in the day, we didn’t really know what it’s like on the ground. Now, we have someone who really understands the details to help us make an impact. – Male, NGO Country Director.
A notable challenge was trepidation and experience of isolation and stigma as part of the disease as well as a lack of trust in the health care system. This lack of trust was underlined by the need for CHWs and study staff to dedicate additional time and resources to travel to patient homes and provide counseling to promote enrollment onto the government TB treatment program.
“The most difficult thing is trust. There was a drug-resistant TB patient with a positive result, but he did not believe that he suffered from TB. He did not agree to treatment even though the TB counselor visited his house and a public health officer talked with him.” – Female, CHW.
Another key concern among CHWs and patients was contracting the disease when fulfilling their responsibilities.
“We talk so much about our job, our children said that you go to work for the community and take the disease home.” – Female, Site coordinator 2.
Social return on investment
The total crude impact was $34,608,108 (Fig. 3). A large portion of the value ($9,516,225) was among treated TB patients, driven by the additional income generated from mortality avoidance ($8,971,527). The crude impact among site coordinators and CHWs overall was positive and estimated to be $61,996, primarily consisting of salaries and stipends. The crude impact for the overall TB program was negative, $-671,190, which was mainly driven by a net increase in LTFU (-$696,344) and higher estimated costs associated with drug-resistant TB management. The largest driver of crude impact with $22,675,830 was the macroeconomic benefit for municipal governments from the economic output generated by additional TB survivors. For the Viet Nam TB ecosystem, the crude impact was $3,025,247 from the additional resources mobilized with leverage from the initial investment. For a full breakdown of the crude returns on investment, please refer to the impact map provided in the supplementary information – TB-SROI Model.
After factoring in the counterfactuals, the adjusted impact was $4,368,850 (Fig. 3). This represents an 87% reduction from the initially-calculated crude impact. The largest adjustment ($-29,768,772) to our crude impact arose from deadweight, i.e., the benefit that would have been generated even in the absence of the investment represented by costs paid by the government for operating the NTP.
Projecting this adjusted impact over the 5-year valuation window shows that the present value of returns from the intervention was $8,497,183 (Fig. 4). The largest benefits were gained in the first year with a return of $4,220,295. Returns diminished in subsequent years. Factoring in the initial investment of $-235,511 resulted in a NPV of $8,261,672, suggesting the SROI of the project was 3,608%. The sensitivity analysis showed the SROI ranged from 3,166%–3,900% for discount rates of 10% and 0%, respectively (supplemental information).
Discussion
Our SROI analysis found that the investment in the Proper Care project created $36.08 in societal returns for every dollar spent. This result is concordant with existing evidence that ACF TB interventions using CHWs generate positive value for individual patients, local communities, and society [20, 73]. Furthermore, our SROI aligns with a study on TB in the Western Pacific Region that used a Solow model to estimate the return on investment for TB care in Vietnam and Laos, which ranged between $4-$49 per dollar spent [74].
The SROI measured on this project tended to be higher than results from other SROI analyses of general public health interventions. A systematic review of 26 evaluative analyses reported a median SROI of 509% (IQR: 253-729%).75 However, comparability with these studies is limited. Most had a time-horizon of one year and only six studies were from LMICs with none originating from Viet Nam or evaluating a TB-related intervention [75]. One key driver for the high SROI on this study may have been the inclusion of resources mobilized by leveraging this initial investment. This value driver was not included in any other studies and contributed to one-third of the value generated. Excluding this value driver would have lowered the estimated SROI of this intervention to 2,367%, which was in line with an analysis of a stigma reduction intervention among people living with HIV in Zambia (SROI = 2,120%) [76].
The highest value creation arose from additional income and economic output due to avoidance of TB-related mortality. This applies particularly to individuals with TB detected and successfully treated through ACF, as past studies have shown that many of these persons remain unreached by NTPs [77, 78]. These unreached persons also comprise the bulk of the estimated mortalities in the WHO’s annual global TB reports [2]. When combining the individual and economic gains from this intervention, the adjusted impact over the 5-year horizon constituted two-thirds of the returns. While this high proportion is clearly a function of the long time-horizon, it is concordant with prior modeling studies, which suggest that TB ACF can be highly cost-effective, especially when appropriately targeted, [36] but that short-term evaluations (1–2-year evaluation horizon) tend to underestimate its economic returns [25]. Benefits for individuals cured of TB include prolonged life, while and economic activity over the time-horizon evaluated represents a value to society.
A critical success factor of this project was the involvement of CHWs [79]. There is extensive evidence for the effectiveness of CHW-based models for TB ACF [80,81,82]. Similarly, studies in various settings reported CHWs were a critical component of patient- and person-centered care [83, 84]. Thus, CHW models were cited as a cost-effective way to provide healthcare services [20, 85]. By this intervention, these CHWs fulfilled the dual purpose of raising case detection and successfully supporting those patients to complete treatment. Therefore, the CHW model may have helped catalyze the high value creation from mortality avoidance.
This SROI evaluation had several limitations. First, given the operational research nature of the intervention and this study, we were unable to capture the effect of externalities such as a parallel private sector engagement project implemented in one of the intervention districts. Additionally, the limited geographic scope and distinct package of interventions limited the generalizability of the quantified benefits and SROI. Nevertheless, using SROI to evaluate the impact of our intervention was an effective way of measuring individual, health system and societal returns. This model also accounted for negative value drivers and placed a strong emphasis on adjusting for counterfactuals and discounting. Adjusting crude impact for counterfactuals was a particularly critical step of the analysis to avoid overestimation of the SROI. Specifically, these adjustments reduced the final impact to one-eighth of the crude value. This was mainly driven by deadweight among passively-detected cases that would have been successfully treated by the NTP irrespective of the intervention. The existing government structure contributed to most of the deadweight.
Another strength of this study was the combination of data sources and use of quantitative and qualitative methods. Particularly the latter enabled the discussion and refinement of value drivers with stakeholders, which were concordant with later studies analyzing the facilitators and barriers of ACF and patient support interventions [86]. Lastly, our methodology also generated information on the personal resources consumed by the intervention, which is uncommon in program evaluations [87]. The combination of these efforts yielded a deeper analysis to raise confidence in the positive, negative, and incremental value of an intervention.
Conclusions
The SROI analysis shows that investment in CHW-supported ACF and TB patient support interventions generated substantial returns for a wide range of stakeholders. With its comprehensive perspective and conservative valuation, the SROI methodology may offer a viable alternative for economic evaluation of public health intervention that warrants further investigation. However, as with other benefit-cost analyses, the associated shortcomings should also be well considered prior to its application.
Data availability
The data that support the findings of this study are available from the Viet Nam National TB Control Program and Pham Ngoc Thach Hospital upon reasonable request to the corresponding author LNQV, but restrictions apply to the availability of these data.
Abbreviations
- ACF:
-
Active Case Finding
- AFB:
-
Acid-fast Bacilli
- CHW:
-
Community Health Worker
- CI:
-
Confidence Interval
- CXR:
-
Chest X-ray
- DTU:
-
District TB Unit
- EP:
-
Extra-pulmonary
- GEE:
-
Generalized Estimating Equation
- HCMC:
-
Ho Chi Minh City
- IRR:
-
Incidence Rate Ratio
- ITS:
-
Interrupted Time Series
- NNS:
-
Number Needed to Screen
- NTP:
-
National TB Control Program
- PBI:
-
Performance-based Incentive
- PNTH:
-
Pham Ngoc Thach Provincial TB Hospital
- TB:
-
Tuberculosis
- WHO:
-
World Health Organization
References
Daniel TM. The history of tuberculosis. Respir Med. 2006;100(11):1862–70.
World Health Organization. Global tuberculosis report 2020. Switzerland: Geneva; 2020.
MacPherson P, Houben RM, Glynn JR, Corbett EL, Kranzer K. Pre-treatment loss to follow-up in tuberculosis patients in low- and lower-middle-income countries and high-burden countries: a systematic review and meta-analysis. Bull World Health Organ. 2014;92(2):126–38.
Vo LNQ, Vu TN, Nguyen HT, Truong T, Khuu CM, Pham PQ, et al. Optimizing community screening for tuberculosis: spatial analysis of localized case finding from door-to-door screening for TB in an urban district of Ho Chi Minh City, Viet Nam. PLoS ONE. 2018;13(12):e0209290.
Mauch V, Woods N, Kirubi B, Kipruto H, Sitienei J, Klinkenberg E. Assessing access barriers to tuberculosis care with the tool to Estimate Patients’ costs: pilot results from two districts in Kenya. BMC Public Health. 2011;11:18–21.
Dheda K, Gumbo T, Maartens G, Dooley KE, McNerney R, Murray M, et al. The epidemiology, pathogenesis, transmission, diagnosis, and management of multidrug-resistant, extensively drug-resistant, and incurable tuberculosis. Lancet Respir Med. 2017;5(4):291–360.
Rachow A, Ivanova O, Wallis R, Charalambous S, Jani I, Bhatt N, et al. TB sequel: incidence, pathogenesis and risk factors of long-term medical and social sequelae of pulmonary TB - A study protocol 11 Medical and Health Sciences 1117 Public Health and Health Services. BMC Pulm Med. 2019;19(1):1–9.
Naidoo K, Dookie N. Insights into Recurrent Tuberculosis: Relapse Versus Reinfection and Related Risk Factors. In: Kayembe JMN, editor. Tuberculosis [Internet]. IntechOpen; 2018. Available from: http://www.intechopen.com/books/tuberculosis/insights-into-recurrent-tuberculosis-relapse-versus-reinfection-and-related-risk-factors.
Siroka A, Law I, Macinko J, Floyd K, Banda RP, Hoa NB, et al. The effect of household poverty on tuberculosis HHS Public Access. Int J Tuberc Lung Dis. 2016;20(12):1603–8.
Tanimura T, Jaramillo E, Weil D, Raviglione M, Lönnroth K. Financial burden for tuberculosis patients in low- and middle-income countries: a systematic review. Eur Respir J. 2014;43(6):1763–75.
Nissen TN, Rose MV, Kimaro G, Bygbjerg IC, Mfinanga SG, Ravn P. Challenges of loss to follow-up in tuberculosis research. PLoS ONE. 2012;7(7):1–8.
Tupasi TE, Garfin AMCG, Kurbatova EV, Mangan JM, Orillaza-Chi R, Naval LC, et al. Factors associated with loss to follow-up during treatment for multidrug-resistant tuberculosis, the Philippines, 2012–2014. Emerg Infect Dis. 2016;22(3):491–502.
Wingfield T, Boccia D, Tovar M, Gavino A, Zevallos K, Montoya R et al. Defining Catastrophic Costs and Comparing Their Importance for Adverse Tuberculosis Outcome with Multi-Drug Resistance: A Prospective Cohort Study, Peru. PLoS Med. 2014;11(7).
World Health Organization. The end TB strategy. Switzerland: Geneva; 2015.
Pedrazzoli D, Borghi J, Viney K, Houben RMGJ, Lönnroth K. Measuring the economic burden for TB patients in the end TB strategy and universal health coverage frameworks. Int J Tuberc Lung Dis. 2019;23(1):5–11.
KPMG. Global Economic Impact of Tuberculosis: A report for the Global TB Caucus [Internet]. 2017. Available from: https://docs.wixstatic.com/ugd/309c93_bf9baa1398334a8aa1ff19cb083b129e.pdf?index=true.
Su Y, Garcia Baena I, Harle AC, Crosby SW, Micah AE, Siroka A et al. Tracking total spending on tuberculosis by source and function in 135 low-income and middle-income countries, 2000–17: a financial modelling study. Lancet Infect Dis [Internet]. 2020;20(8):929–42. Available from: https://doi.org/10.1016/S1473-3099(20)30124-9.
Laurence YV, Griffiths UK, Vassall A. Costs to Health Services and the patient of treating tuberculosis: a systematic literature review. PharmacoEconomics. 2015;33(9):939–55.
Floyd K, Skeva J, Nyirenda T, Gausi F, Salaniponi F. Cost and cost-effectiveness of increased community and primary care facility involvement in tuberculosis care in Lilongwe District, Malawi. Int J Tuberc Lung Dis. 2003 Sep;7(9 Suppl 1):29–37.
Vaughan K, Kok MC, Witter S, Dieleman M. Costs and cost-effectiveness of community health workers: evidence from a literature review. Hum Resour Health [Internet]. 2015 Dec 1;13(1):71. Available from: https://doi.org/10.1186/s12960-015-0070-y.
Datiko DG, Lindtjørn B. Cost and cost-effectiveness of treating smear-positive tuberculosis by health extension workers in Ethiopia: an ancillary cost-effectiveness analysis of community randomized trial. PLoS ONE. 2010;5(2):1–7.
Okello D, Floyd K, Adatu F, Odeke R, Gargioni G. Cost and cost-effectiveness of community-based care for tuberculosis patients in rural Uganda. Int J Tuberc Lung Dis. 2003 Sep;7(9 Suppl 1):72–9.
Lung T, Marks GB, Nhung NV, Anh NT, Le N, Hoa P et al. Household contact investigation for the detection of tuberculosis in Vietnam: economic evaluation of a cluster-randomised trial. Lancet Glob Heal [Internet]. 2019;7(3):e376–84. Available from: https://doi.org/10.1016/S2214-109X(18)30520-5.
Vassall A. Benefits and costs of the tuberculosis targets for the Post-2015 Development Agenda. Copenhagen Consensus. Copenhagen Consensus Center; 2014 Dec.
Azman AS, Golub JE, Dowdy DW. How much is tuberculosis screening worth? Estimating the value of active case finding for tuberculosis in South Africa, China, and India. BMC Med. 2014 Oct;12(1):1–9.
Moalosi G, Floyd K, Phatshwane J, Moeti T, Binkin N, Kenyon T. Cost-effectiveness of home-based care versus hospital care for chronically ill tuberculosis patients, Francistown, Botswana. Int J Tuberc Lung Dis. 2003 Sep;7(9 Suppl 1):80–5.
Nganda B, Wang’ombe J, Floyd K, Kangangi J. Cost and cost-effectiveness of increased community and primary care facility involvement in tuberculosis care in Machakos District, Kenya. 2International J Tuberc Lung Dis. 2003 Sep;7(9 Suppl 1):S14–20.
Floyd K, Arora VK, Murthy KJR, Lonnroth K, Singla N, Akbar Y, et al. Cost and cost-effectiveness of PPM-DOTS for tuberculosis control: evidence from India. Bull World Health Organ. 2006 Jun;84(6):437–45.
Pantoja A, Floyd K, Unnikrishnan KP, Jitendra R, Padma MR, Lal SS, et al. Economic evaluation of public-private mix for tuberculosis care and control, India. Part I. Socio-economic profile and costs among tuberculosis patients. Int J Tuberc Lung Dis. 2009;13(6):698–704.
Pantoja A, Lönnroth K, Lal SS, Chauhan LS, Uplekar M, Padma MR, et al. Economic evaluation of public-private mix for tuberculosis care and control, India. Part II. Cost and cost-effectiveness. Int J Tuberc Lung Dis. 2009;13(6):705–12.
Fitzpatrick C, Floyd K. C. F, K. F. A systematic review of the cost and cost effectiveness of treatment for multidrug-resistant tuberculosis. Pharmacoeconomics [Internet]. 2012 Jan;30(1):63–80. Available from: http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=emed10&NEWS=N&AN=2011684675.
Verdier JE, De Vlas SJ, Baltussen R, Richardus JH. A systematic review of economic evaluation studies of tuberculosis control in high-income countries. Int J Tuberc Lung Dis. 2011;15(12):1587–97.
Minh HV, Mai VQ, Nhung NV, Hoi LV, Giang KB, Chung LH et al. Costs of providing tuberculosis diagnosis and treatment services in Viet Nam. Int J Tuberc Lung Dis [Internet]. 2017;21(9):1035–40. Available from: http://www.ingentaconnect.com/content/https://doi.org/10.5588/ijtld.16.0778.
Bogdanova EN, Mariandyshev AO, Balantcev GA, Eliseev PI, Nikishova EI, Gaida AI, et al. Cost minimization analysis of line probe assay for detection of multidrug-resistant tuberculosis in Arkhangelsk region of Russian Federation. PLoS ONE. 2019;14(1):1–15.
Nguyen LH, Codlin AJ, Vo LNQ, Dao T, Tran D, Forse RJ, et al. An evaluation of Programmatic Community-Based chest X-ray screening for tuberculosis in Ho Chi Minh City, Vietnam. Trop Med Infect Dis. 2020 Dec;10(4):185.
Dobler CC. Screening strategies for active tuberculosis: focus on cost-effectiveness. Clin Outcomes Res [Internet]. 2016 Jun;8:335–47. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L612341993%0Ahttp://dx.doi.org/10.2147/CEOR.S92244
Quang TN. Cost-effectiveness of public-private mixed models in National Tuberculosis Program in Ho Chi Minh City. Vietnam PSAKU Int J Interdiscip Res. 2018;1(1):44–69.
Gomez GB, Dowdy DW, Bastos ML, Zwerling A, Sweeney S, Foster N et al. Cost and cost-effectiveness of tuberculosis treatment shortening: a model-based analysis. BMC Infect Dis [Internet]. 2016;16(1):1–13. Available from: https://doi.org/10.1186/s12879-016-2064-3.
Nhung NV, Hoa NB, Anh NT, Anh LTN, Siroka A, Lönnroth K et al. Measuring catastrophic costs due to tuberculosis in Viet Nam. Int J Tuberc Lung Dis [Internet]. 2018 Sep 1;22(9):983–90. Available from: http://www.ingentaconnect.com/content/https://doi.org/10.5588/ijtld.17.0859.
Cunnama L, Gomez GB, Siapka M, Herzel B, Hill J, Kairu A et al. A Systematic Review of Methodological Variation in Healthcare Provider Perspective Tuberculosis Costing Papers Conducted in Low- and Middle-Income Settings, Using An Intervention-Standardised Unit Cost Typology. Pharmacoeconomics [Internet]. 2020;38(8):819–37. Available from: https://doi.org/10.1007/s40273-020-00910-w.
Nam VX, Nhung NV, Hoa NB, Thuy HTT, Phuong NTM, Anh NT, et al. Economic burden of multidrug-resistant tuberculosis: a multicenter study across vietnamese regions. Int J Tuberc Lung Dis. 2018;22(8):912–7.
Nicholls J. Social return on investment—Development and convergence. Eval Program Plann [Internet]. 2017;64:127–35. Available from: https://doi.org/10.1016/j.evalprogplan.2016.11.011.
Dyakova M, Hamelmann C, Bellis MA, Besnier E, Grey CNB, Ashton K et al. Investment for health and well-being: a review of the social return on investment from public health policies to support implementing the Sustainable Development Goals by building on Health 2020 [Internet]. Health Evidence Network Synthesis Report 51. Copenhagen; 2017. Available from: http://www.euro.who.int/__data/assets/pdf_file/0008/345797/HEN51.pdf.
Laing CM, Moules NJ. Social return on investment: a new approach to understanding and advocating for value in healthcare. J Nurs Adm. 2017;47(12):623–8.
Philipson TJ, Snider JT, Chit A, Green S, Hosbach P, Schwartz TT, et al. The social value of childhood vaccination in the United States. Am J Manag Care. 2017;23(1):41–7.
Tanaree A, Assanangkornchai S, Isaranuwatchai W, Thavorn K, Coyte PC. Integrated treatment program for alcohol related problems in community hospitals, Songkhla province of Thailand: A social return on investment analysis. Seedat S, editor. PLoS One [Internet]. 2019 Jan 2;14(1):e0209210. Available from: https://doi.org/10.1371/journal.pone.0209210.
Banke-Thomas A, Madaj B, Van Den Broek N. Social return on investment of emergency obstetric care training in Kenya. BMJ Glob Heal. 2019;4(1):1–11.
Hutchinson CL, Berndt A, Forsythe D, Gilbert-Hunt S, George S, Ratcliffe J. Valuing the impact of health and social care programs using social return on investment analysis: how have academics advanced the methodology? A systematic review. BMJ Open. 2019;9(8):1–6.
World Health Organization. Global Tuberculosis Report 2021.Geneva, Switzerland.
Office of the Prime Minister. Approval of the National Strategy for TB prevention and control until 2020 with vision to 2030 [vietnamese]. 374/QĐ-TTg Viet Nam. Viet Nam; 2014.
Viet Nam National TB Control Programme. Viet Nam National Strategic Plan for TB 2021–2025. Ha Noi, Viet Nam;; 2020.
Vo LNQ, Forse RJ, Codlin AJ, Vu TN, Le GT, Do GC, et al. A comparative impact evaluation of two human resource models for community-based active tuberculosis case finding in Ho Chi Minh City, Viet Nam. BMC Public Health. 2020 Dec;15(1):934.
Vo LNQ, Codlin AJ, Forse RJ, Nguyen HT, Vu TN, Van Truong V et al. Tuberculosis among economic migrants: a cross-sectional study of the risk of poor treatment outcomes and impact of a treatment adherence intervention among temporary residents in an urban district in Ho Chi Minh City, Viet Nam. BMC Infect Dis [Internet]. 2020 Dec 12;20(1):134. Available from: https://bmcinfectdis.biomedcentral.com/articles/https://doi.org/10.1186/s12879-020-4865-7.
Vo LNQ, Forse RJ, Codlin AJ, Dang HM, Van Truong V, Nguyen LH et al. Socio-protective effects of active case finding on catastrophic costs from tuberculosis in Ho Chi Minh City, Viet Nam: a longitudinal patient cost survey. BMC Health Serv Res [Internet]. 2021 Dec 5;21(1):1051. Available from: https://bmchealthservres.biomedcentral.com/articles/https://doi.org/10.1186/s12913-021-06984-2.
Creswell JW. Research Design: qualitative, quantitative, and mixed methods approaches. Third ed. Thousand Oaks, CA, USA: SAGE Publications; 2009.
Husereau D, Drummond M, Petrou S, Carswell C, Moher D, Greenberg D et al. Consolidated health economic evaluation reporting standards (CHEERS)-explanation and elaboration: A report of the ISPOR health economic evaluation publication guidelines good reporting practices task force. Value Heal [Internet]. 2013;16(2):1–6. Available from: https://doi.org/10.1016/j.jval.2013.02.010.
Viet Nam Ministry of Health. Decision on the promulgation of the Guidelines on the diagnosis, treatment and prevention of tuberculosis [vietnamese]. 1314/QD-BYT Viet Nam; 2020.
Vo LNQ, Codlin AJ, Forse RJ, Nguyen NT, Vu TN, Le GT, et al. Evaluating the yield of systematic screening for tuberculosis among three priority groups in Ho Chi Minh City, Viet Nam. Infect Dis Poverty. 2020;9(1):1–13.
Nicholls J, Lawlor E, Neitzert E, Goodspeed T, Jeremy Nicholls, Lawlor E et al. A guide to Social Return on Investment [Internet]. 2012. Available from: http://www.thesroinetwork.org/publications/doc_details/241-a-guide-to-social-return-on-investment-2012.
Grant MJ, Booth A. A typology of reviews: an analysis of 14 review types and associated methodologies. Health Info Libr J. 2009;26(2):91–108.
Sagliocca L, De Masi S, Ferrigno L, Mele A, Traversa G. A pragmatic strategy for the review of clinical evidence. J Eval Clin Pract. 2013;19(4):689–96.
Ganann R, Ciliska D, Thomas H. Expediting systematic reviews: methods and implications of rapid reviews. Implement Sci. 2010;5(1):1–10.
Malterud K, Siersma VD, Guassora AD. Sample size in qualitative interview studies: guided by Information Power. Qual Health Res. 2016;26(13):1753–60.
Ritchie J, Lewis J. In: Ritchie J, Lewis J, editors. Qualitative Research Practice A Guide for Social Science Students and Researchers. First edit. London, England: SAGE Publications; 2003. p. 349.
Green J, Thorogood N. Qualitative methods in Health Research. Fourth edi. London, UK: SAGE Publications Ltd; 2018. p. 440.
Blok L, Creswell J, Stevens R, Brouwer M, Ramis O, Weil O, et al. A pragmatic approach to measuring monitoring and evaluating interventions for improved tuberculosis case detection. Int Health. 2014;6(3):181–8.
Government of Viet Nam. Stipulating region-based minimum wages applied to employees working under labour contracts. 90/2019/ND-CP Viet Nam; 2019.
Gao J, Ma Y, Du J, Zhu G, Tan S, Fu Y, et al. Later emergence of acquired drug resistance and its effect on treatment outcome in patients treated with Standard Short-Course Chemotherapy for tuberculosis. BMC Pulm Med. 2016;16(1):1–9.
Viscusi WK, Aldy JE. The Value of a Statistical Life: Throughout the World. Cambridge, MA; 2003. (NBER Working Paper Series). Report No.: 9487.
Laxminarayan R, Klein E, Dye C, Floyd K, Darley S, Adeyi O. Economic benefit of tuberculosis control. The World Bank; 2007. p. WPS4295. Aug. Report No.
Cooney K, Lynch-Cerullo K. Measuring the social returns of nonprofits and Social Enterprises: the Promise and Perils of the SROI. Nonprofit Policy Forum. 2014;5(2):367–93.
The World Bank. Inflation, consumer prices (annual %) - Vietnam [Internet]. Washington, D.C., United States of America; 2021 [cited 2021 Dec 22]. Available from: https://data.worldbank.org/indicator/FP.CPI.TOTL.ZG?end=2017&locations=VN&start=2013.
Scott K, Beckham SW, Gross M, Pariyo G, Rao KD, Cometto G, et al. What do we know about community-based health worker programs? A systematic review of existing reviews on community health workers. Hum Resour Health. 2018;16(1):1–17.
Estill J, Islam T, Houben RMGJ, Rudman J, Ragonnet R, McBryde ES et al. Tuberculosis in the Western Pacific Region: Estimating the burden of disease and return on investment 2020–2030 in four countries. Lancet Reg Heal - West Pacific [Internet]. 2021;11:100147. Available from: https://doi.org/10.1016/j.lanwpc.2021.100147.
Banke-Thomas AO, Madaj B, Charles A, Van Den Broek N. Social Return on Investment (SROI) methodology to account for value for money of public health interventions: A systematic review. BMC Public Health [Internet]. 2015;15(1):1–14. Available from: https://doi.org/10.1186/s12889-015-1935-7.
Brady R. The True Cost of Stigma: Evaluating the Social Return on Investment of the stigma and discrimination component of the Alliance’s Africa Regional Programme II [Internet]. 2011. 1–36 p. Available from: http://www.aidsalliance.org/assets/000/002/381/SROI_Zambia_original.pdf?1453739463.
Golub JE, Mohan CI, Comstock GW, Chaisson RE. Active case finding of tuberculosis: historical perspective and future prospects. Int J Tuberc Lung Dis. 2005;9(11):1183–203.
Ho J, Fox GJ, Marais BJ. Passive case finding for tuberculosis is not enough. Int J Mycobacteriology. 2016;5(4):374–8.
Dam TA, Forse R, Creswell J. What Makes Community Health Worker Models for Tuberculosis Active Case Finding Work ? A Cross- Sectional Study of TB REACH Projects to Identify Success Factors for Increasing Case Notifications [pre-print]. Hum Resour Health. 2022.
Siahaan ES, Bakker MI, Pasaribu R, Khan A, Pande T, Hasibuan AM, et al. Islands of tuberculosis elimination: an evaluation of community-based active case finding in North Sumatra, Indonesia. Trop Med Infect Dis. 2020;5(4):163.
Vyas A, Creswell J, Codlin AJ, Stevens R, Rao VG, Kumar B et al. Community-based active case-finding to reach the most vulnerable: tuberculosis in tribal areas of India. Int J Tuberc Lung Dis [Internet]. 2019 Jun 1;23(6):750–5. Available from: https://www.ingentaconnect.com/content/https://doi.org/10.5588/ijtld.18.0741.
Datiko DG, Yassin MA, Theobald SJ, Blok L, Suvanand S, Creswell J, et al. Health extension workers improve tuberculosis case finding and treatment outcome in Ethiopia: a large-scale implementation study. BMJ Glob Heal. 2017;2(4):1–8.
Dorman SE, Schumacher SG, Alland D, Nabeta P, Armstrong DT, King B, et al. Xpert MTB/RIF Ultra for detection of Mycobacterium tuberculosis and rifampicin resistance: a prospective multicentre diagnostic accuracy study. Lancet Infect Dis. 2018;18(1):76–84.
Biermann O, Lönnroth K, Caws M, Viney K. Factors influencing active tuberculosis case-finding policy development and implementation: a scoping review. BMJ Open. 2019;9(12):1–12.
Clarke M, Dick J, Bogg L. Cost-effectiveness analysis of an alternative tuberculosis management strategy for permanent farm dwellers in South Africa amidst health service contraction. Scand J Public Health. 2006;34(1):83–91.
Biermann O, Tran PB, Forse RJ, Vo LNQ, Codlin AJ, Viney K et al. Capitalizing on facilitators and addressing barriers when implementing active tuberculosis case-finding in six districts of Ho Chi Minh City, Vietnam: a qualitative study with key stakeholders. Implement Sci [Internet]. 2021 Dec 19;16(1):54. Available from: https://implementationscience.biomedcentral.com/articles/https://doi.org/10.1186/s13012-021-01124-0.
Yates BT, Marra M. Social Return On Investment (SROI): Problems, solutions ? and is SROI a good investment? Eval Program Plann [Internet]. 2017 Oct;64:136–44. http://dx.doi.org/10.1016/j.evalprogplan.2016.11.009
Acknowledgements
We would like to acknowledge the Ho Chi Minh City Public Health Association, Viet Nam’s National TB Control Program, and Pham Ngoc Thach Hospital for their support. We would also like to thank our interviewers and translators and our patients for their work and participation. We would like to especially thank the site coordinators and CHWs for their tireless efforts to care for their patients and contribute towards ending TB in Viet Nam.
Funding
This research and LNQV, AJC, RJF were supported by the European Commission Horizon 2020 programme grant number 733174 (analysis) as well as Janssen Global Services contract reference number C2016010337 (intervention & analysis). These funding bodies had no role in the design of the study, in collection, analysis, and interpretation of data, or in writing the manuscript.
Author information
Authors and Affiliations
Contributions
LNQV, RJF, JD, VVT contributed to conceptualization of the study. LNQV, RJF, JT developed the methodology. LNQV, RFJ, JT, TD conducted the formal analysis. The investigation was conducted by LNQV, RJF, JT, TD, VVT. Resources were provided by HDTM, LNH, HBN, NVN. LNQV, RJF, JT, TD, AJC contributed to data curation for the study. LNQV, RJF, JT, TD wrote the original draft, while review and editing was done by LNQV, RJF, AJC, JD, JC, KSA. LNQV, RJF, JT, TD contributed to the visualization of the data. Supervision was provided by JC, VVT, HDTM, LNH, HBN, NVN. RJF, JT, TD, AJC, VVT were responsible for project administration, while LNQV led funding acquisition. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests with regard to this work.
Ethics approval and consent to participate
We obtained ethical approval for the study from the Institutional Review Board of the Pham Ngoc Thach Hospital in Ho Chi Minh City (129/HDDD-PNT). All participants provided informed, written consent and all data were anonymized prior to analysis.
Consent for publication
Not applicable.
Authors’ information (optional)
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Quang Vo, L., Forse, R.J., Tran, J. et al. Economic evaluation of a community health worker model for tuberculosis care in Ho Chi Minh City, Viet Nam: a mixed-methods Social Return on Investment Analysis. BMC Public Health 23, 945 (2023). https://doi.org/10.1186/s12889-023-15841-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12889-023-15841-2