Abstract
Background
Ghana has reached an advanced stage of nutrition transition, contributing to an increase in nutrition-related non-communicable diseases, particularly amongst urban women. Community involvement is an important factor in the success of efforts to promote healthy eating. The readiness of populations to accept a range of interventions needs to be understood before appropriate interventions can be implemented. Therefore, this study assessed how ready urban communities are to improve diets of women of reproductive age in Ghana.
Methods
Using the Community Readiness Model (CRM), in-depth interviews were conducted with 24 key informants from various sectors in low income communities across two cities in Ghana: Accra and Ho. The CRM consists of 36 open questions addressing five readiness dimensions (community knowledge of efforts, leadership, community climate, knowledge of the issue and resources). Interviews were scored using the CRM protocol with a maximum of 9 points per dimension (from 1 = no awareness to 9 = high level of community ownership). Thematic analysis was undertaken to gain insights of community factors that could affect the implementation of interventions to improve diets.
Results
The mean community readiness scores indicated that both communities were in the “vague awareness stage” (3.35 ± 0.54 (Accra) and 3.94 ± 0.41 (Ho)). CRM scores across the five dimensions ranged from 2.65–4.38/9, ranging from denial/resistance to pre-planning. In both communities, the mean readiness score for ‘knowledge of the issue’ was the highest of all dimensions (4.10 ± 1.61 (Accra); 4.38 ± 1.81 (Ho)), but was still only at the pre-planning phase. The lowest scores were found for community knowledge of efforts (denial/resistance; 2.65 ± 2.49 (Accra)) and resources (vague awareness; 3.35 ± 1.03 (Ho)). The lack of knowledge of the consequences of unhealthy diets, misconceptions of the issue partly from low education, as well as challenges faced from a lack of resources to initiate/sustain programmes explained the low readiness.
Conclusions
Despite recognising that unhealthy diets are a public health issue in these urban Ghanaian communities, it is not seen as a priority. The low community readiness ratings highlight the need to increase awareness of the issue prior to intervening to improve diets.
Similar content being viewed by others
Background
Ghana, a lower-middle income country [1], is in the latter stages of the nutrition transition [2, 3]. Although the overall prevalence of overweight and obesity in adults in Ghana is 43%, the prevalence is significantly higher in women than in men (49.7% vs 27.8%), and in urban than rural dwellers (47.8% vs 24.7%) [4]. As women play a key role in society by contributing to the health-care workforce, nutritional adequacy of households, education, and to the care of families and communities [5], promoting healthy eating in women could benefit immediate family members as well as others within the wider community [5]. There is therefore an urgent need for interventions to promote healthier diets to prevent obesity and other forms of malnutrition that reach urban females in Ghana.
Community involvement has been recognised as an important factor in the success and sustainability of efforts to promote healthy eating and prevent obesity [6]. Within a community, the success of an intervention is dependent upon the community’s readiness for change [7]; according to behaviour change theory, strategies should be matched to the stage of readiness [8]. An initial assessment of community readiness should therefore be conducted prior to implementing a community-based intervention.
The CRM provides a theoretical framework for understanding and improving community readiness [7, 9]. Based on the Transtheoretical Model of Behaviour Change for individual readiness [10], the CRM approaches problems that exist in a community by integrating a community’s culture, resources and level of readiness to assess the degree to which a community is prepared to take action on an issue [11]. The CRM provides quantitative scores of readiness level via assessment of in-depth individual interviews conducted with key informants in the community [12]. A qualitative analysis of responses is also recommended to support the quantitative scoring [13].
The CRM has most frequently been used within the U.S.A, for alcohol and drug use [14]. However, the tool has also been used to assess readiness for overweight and obesity prevention in high-income countries (HICs) including the U.S.A [15, 16], Australia [17, 18] and the UK [19] and applied to ethnic minority [20] or disadvantaged communities [21]. Limited research has been conducted in low- and middle-income countries (LMICs) using the CRM. For example, it has been applied to preventing communicable diseases in Bangladesh [22] and Mali [23], and mental health stigma in Vietnam [24]. Only one study (from South Africa) has assessed community readiness for overweight/obesity prevention in Africa [25].
This current study investigated how ready urban communities are to improve the diets of women of reproductive age in Ghana. The specific objectives were: (i) to determine the stage of readiness of communities to address the consumption of unhealthy foods and beverages in adolescent girls and women of reproductive age in two deprived communities at different stages of the nutrition transition in urban Ghana, and (ii) to gain qualitative insights of community factors that could affect the implementation of interventions targeting unhealthy food and beverage consumption.
Methods
Study setting
This study was conducted in two Ghanaian cities; the densely populated city of Accra (estimated population of 1.85 million) and Ho (estimated population of 120,349) [26]. These two cities were chosen as they are at different stages of the nutrition transition, as evidenced by differences in the regional prevalence of overweight/obesity; 57.3% in Greater Accra (Accra) and 31.1% in the Volta region (Ho) [27].
Communities within these two cities were selected to represent the lower quintile wealth populations, as the study was most interested in understanding the potential for intervention in the very poorest urban communities in Ghana. A list of all deprived communities in Accra and Ho was produced. In Accra, the selection of a study community was informed by findings of the Accra Poverty Mapping Exercise [28]. The Ga Mashie community in Accra was chosen purposively as it was classified as a high poverty zone. In Ho, the selection of a study community was informed by using the 2009 United Nations Human Settlements Programme urban profiling report [29]. The Ho Central area was purposely chosen for convenience of location and meeting the economic inclusion criteria.
Data collection
A geographical definition was used to define our communities of interest (Ga Mashie and Ho Central areas in Accra and Ho, as defined by the respective local authorities – Accra Metropolitan Assembly and Ho Municipal Assembly respectively). Key informants with a leadership role within the selected communities were interviewed (n = 12 in each community) between February and May 2018 [30]. To ensure a range of views within the communities, key informants were recruited purposively to represent a wide range of sectors (schools, commerce, health, religious institutions, development agencies, traditional authorities and youth clubs). If leaders agreed to participate, they were given a participant information letter and written informed consent was taken on the day of the interview.
The CRM tool [30] was administered via individual face to face interviews with key informants. The CRM tool consists of 36 open questions addressing five readiness dimensions: community knowledge of efforts, leadership, community climate, community knowledge of the issue, and resources (Fig. 1). The issue was defined as the “consumption of unhealthy foods and drinks in adolescent girls and women aged 13-49 years”. This referred to the consumption of products such as processed meats; sugar and sweet spreads; cakes and sweets; sodas and sweetened drinks; fried potatoes, yam or plantain; oils; spreading fats; cooking fats; and condiments (such as ketchup, mayonnaise).
The dimensions of the Community Readiness Model. Source: Adapted from the Tri Ethnic Center Community Readiness Handbook 2nd Edition, page 1 [30]
Interviews were administered in English. The CRM interview guide was piloted with the local teams and two community key informants. As a result of this, the tool was amended and adapted to the urban Ghanaian context (i.e. re-phrasing of sentences and altering terminology) (Additional file 1). The Likert scales to measure opinions were culturally adapted to facilitate the understanding of the scale system. To keep the interview time relatively short (approximately 30–45 min), the number of questions included in the interview guide was also limited to only those required for scoring readiness as specified by the CRM authors [30].
Data analysis
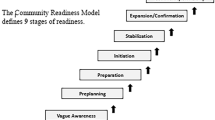
Key informant interviews were transcribed verbatim, reviewed for accuracy and scored by two independent scorers (RP/CM or RP/KB) [25, 30]. Each interview was first read through in full to gain a general idea of the content. Scorers then compared each response given by community key informants to the nine anchored rating statements for each dimension and matched it to the most appropriate anchored rating statements [30] (see pages 49–53). After scoring, the average score for each dimension was generated and a score for each key informant was then calculated as the sum of average scores for each dimension divided by the number of dimensions. Finally, an overall stage of community readiness to address consumption of unhealthy foods and beverages in women and adolescent girls was calculated for all key informants. This was obtained by summing the scores for each key informant, divided by the number of key informants included in the study (range 1–9). Scores were generated separately for Ga Mashie and Ho Central to allow comparisons between the two communities. The overall mean score was then compared to the nine stages of community readiness defined in the CRM (Fig. 2) to evaluate the level of readiness, and efforts needed.
The nine stages of Community Readiness. Source: Adapted from the Tri Ethnic Center Community Readiness Handbook, 2nd Edition, page 6 [30]
Transcripts were also analysed using thematic analysis to allow an in-depth interpretation of the scores obtained [31]. Pattern themes, defined as concepts that occurred frequently across interviews, were identified from the analysis of the coded text. Themes were identified from initial codes if the topic was raised in more than one interview, meaning that an inductive approach was taken. The coders (RP/CM) then agreed on the final codebook to use to code all transcripts (Additional file 2). Coding was undertaken using NVivo version 11. Six of the 24 transcripts (25%) were independently coded by a second coder and final codes were agreed upon discussion.
Results
Sample characteristics
Across the two communities, informants interviewed (n = 24) had similar roles and were representing similar sectors. In Ga Mashie, the majority of respondents were male (66.7%), whilst in Ho Central there was an equal proportion of male and female respondents. Across both communities, most key informants were above the age of 35 years (Table 1).
Community readiness scores
Mean (standard deviation) community readiness scores were 3.35 ± 0.54 (Ga Mashie) and 3.94 ± 0.41 (Ho Central) which correspond to the “vague awareness stage” (Table 2). This corresponds to the third lowest (of nine) stage of community readiness. This stage is reached when: (i) a few community members have at least heard about local efforts, but know little about them, (ii) the leadership and community members believe that the consumption of unhealthy foods and beverages is a concern in the community but they show no immediate motivation to act, (iii) community members have only vague knowledge about the issue and (iv) there are limited resources within the community to mobilise towards the issue [30].
In the Ga Mashie community, the mean readiness score for knowledge of the issue was the highest of all the dimensions (4.10 ± 1.61), followed by leadership (3.50 ± 1.34). In Ho Central, the highest scores were displayed for knowledge of the issue (4.38 ± 1.81) and community climate (4.29 ± 1.32). The lowest scores were found for knowledge of efforts (2.65 ± 2.49) and resources (3.35 ± 1.03) in Ga Mashie and Ho Central, respectively.
Community knowledge of efforts
The scores for community knowledge of efforts were low in both communities. Ga Mashie had the lowest score for this dimension (2.6), which revealed that the Ga Mashie community is in the ‘denial resistance stage’, whereby community members have misconceptions or incorrect knowledge about current efforts. In contrast, scores for Ho Central suggested that they are in a slightly higher readiness stage (3.8) referred to as the ‘vague awareness stage’, reflecting that a few community members have heard about local efforts but know little about them (Table 2).
The low scores across both communities can be attributed to the many (Ga Mashie) or some (Ho Central) key informants who were unaware of any efforts to address the consumption of unhealthy food and drinks in women of reproductive age (Table 3). In both communities, existing programmes were often only one-off events and conducted in health care facilities, or schools. Consequently, only specific groups were targeted, e.g. pregnant women, patients with non-communicable diseases, or school pupils. The content of such efforts ranged from basic food hygiene to targeting nutrient balance.
The difference in scores between the two communities can be explained by a number of factors. In Ga Mashie, some community members held misconceptions around who efforts are for; assuming that efforts were only for the old and sick, rather than recognising the need for prevention efforts. In contrast, no misconceptions concerning efforts were identified in Ho Central. Additionally, engagement of community members was stronger within Ho Central; key community members act as community champions to engage others. Messages conveyed through the radio were also considered successful in Ho Central.
In both communities, key informants suggested that once programmes are established, community members would engage and assist with them to ensure their success, particularly if it is community led.
Leadership
The level of readiness of the community ‘leadership’ was low in both Ga Mashie (3.50) and Ho Central (3.85), which places the communities at a “vague awareness stage”. This means that the leadership recognises the issue may be a concern but there is no immediate motivation to act (Table 2).
There was no general consensus amongst key informants about the concern/priority level that community leadership assigned to the consumption of unhealthy foods and beverages (Table 4). Others recognised that this was an issue of interest but no active efforts are made towards implementation, which implies that the level of concern is not high enough to translate into action. Another explanation for not engaging actively with this issue is that the community leadership prioritises other efforts (e.g. allocating funds for obtaining more classrooms or for celebrations), or other health issues such as anaemia and undernutrition in women of reproductive age.
Furthermore, key informants acknowledged that there was a lack of resources to support them in engaging in such programmes; they suggested that engagement would be increased if they received financial gains to start initiatives and support efforts to tackle the issue of consumption of unhealthy foods and drinks.
Influential leaders in both communities that could help gather and influence the community included members of the municipal assembly, traditional leaders (e.g. community chiefs, church leaders, opinion leaders, elders), health workers, youth leaders and teachers.
Community climate
The scores for community climate were low across both communities. Ga Mashie was at the ‘vague awareness’ stage (score of 3.4), whereby community members believed that the consumption of unhealthy food and drinks in adolescent girls and women may be a concern but they showed no immediate motivation to act. Ho Central was slightly higher, ranked in the ‘pre-planning’ stage (score of 4.3), i.e. community members acknowledged that this issue was a concern in the community and that something needed to be done to address it (Table 2).
Among community members, the issue often only became a priority when individuals were diagnosed with an illness, because community members placed a low priority on prevention (Table 5). When programmes were available, community members tend to passively engage with efforts, but often require incentives to do so. Furthermore, low levels of literacy and high poverty rates act as barriers to behaviour change and some community members were concerned about the impact of efforts on their business.
Within Ho Central, although there was a low concern towards the consumption of unhealthy foods and drinks in general, community members were concerned about the consumption of alcoholic beverages in adolescent girls and women. There were also greater variations in the views of key informants regarding community concern and priority levels and these differences explained the slightly higher readiness scores in Ho Central.
In both communities, influential community members and groups were highlighted that could boost the success of future efforts, e.g. youth groups, school clubs, church groups and women’s groups.
Knowledge about the issue
Both communities were at the “pre-planning” stage for their level of knowledge about the issue (i.e. occurrence, causes, consequences and misconceptions) (4.10 for Ga Mashie and 4.38 for Ho Central) (Table 2).
Community members were aware that the consumption of unhealthy foods and drinks in the community was occurring (Table 6). They mentioned a shift in consumption practices from home cooked meals to ‘fast food’, from eating in the home to eating late at the market and they highlighted a marked increase in alcohol consumption. As a result, the community was perceived as facing increased risks of diet-related illnesses.
Key informants disagreed about the level of community knowledge of causes of consumption of unhealthy foods and beverages, ranging from knowing nothing to knowing a lot. Causes discussed were: availability of unhealthy foods and drinks, advertisement of unhealthy products, cost of food, poverty, level of education, peer influences and social and environmental influences.
Key informants also disagreed on the level of community knowledge of the consequences of consuming unhealthy foods and beverages, ranging from knowing nothing to knowing a lot. Some community members may know that unhealthy food and drink consumption impacts upon health but may not know the specific consequences, although those who are educated may have a greater understanding. Some community members only learn about the consequences once they are affected with diet-related diseases. However, key informants mentioned that knowledge of the consequences may be growing due to information being provided in the media and via health workers.
Key informants described misconceptions that existed within both communities around the consumption of unhealthy foods and drinks. These included whether specific food and drink items were harmful (e.g. all foreign imported foods were viewed as healthy); to whom the items were harmful (e.g. items that harm only the old, items that should or should not be consumed during pregnancy/lactation); consequences of unhealthy food and drink consumption; causes of illness (e.g. spiritual or supernatural powers) and social connotations associated with particular food items (e.g. wealth associated with consumption of certain foods/beverages). It is believed that misconceptions originated from older family members or from people who have consumed unhealthy products for a long period of time, but have not developed any illness.
Resources
Both communities were at the ‘vague awareness stage’ for resources, (3.08 for Ga Mashie and 3.35 for Ho Central), which means that overall there were limited resources identified that could be leveraged for further efforts to tackle the issue (Table 2). Some resources were identified as clear barriers to leaders engaging with or implementing actions to address the issue (i.e. money, time, and experts or volunteers in the community) (Table 7). In terms of funding, informants reported that there were zero to limited funds available (e.g. money from individual donors, community contributions and local levies) and the funding from ministries was deemed inconsistent. The community key informants also mentioned that they would expect subsistence allowances to support various programmes but this was not currently in place and therefore hindered leadership engagement. Key informants reported that businesses and organisations in the area would not financially support such efforts and that donor support is overall reducing.
Several key informants discussed time as a barrier to engaging in programmes. For example, health visits were deemed too short to allow women to ask questions. Community leaders reported that they may prioritise their time for other matters. When volunteers are recruited to help, they often refuse on the basis of not having enough time. It is also believed that some community members may not make time to attend programmes around healthy eating as they would rather spend their time working or looking for work. A few key informants mentioned that radio messages were perceived as more successful because community members could listen whilst doing other activities.
Other resources such as information, organisations, space and experts/volunteers currently exist and could be further leveraged to address the issue of consumption of unhealthy foods and beverages in the communities. Some key informants mentioned that there may be some posters addressing the consumption of unhealthy foods and beverages displayed in the communities but only in certain places (e.g. health care facilities and schools). Additional information on the topic was shared via radio programmes but reach may be limited as not all community members own a radio. Information vans are also a way of sharing information within the community. Nurses and health workers have booklets for mothers and carers but it is unclear if these address the issue of consumption of unhealthy foods and drinks specifically.
Key informants also identified organisations (e.g. Non-Governmental Organisations (NGOs), youth groups, women’s group, food vendors’ association and other community groups), currently not mobilised to address the consumption of unhealthy foods and drinks in the communities, that could help support such efforts. Some of these organisations may already be involved in one-off efforts, but there was no sustainable involvement due to a lack of financial resources.
There were a number of experts identified in the community that could be engaged to support programmes around healthy eating and drinking, e.g. public health and community nurses trained in basic nutrition, dietitians, health promotion officers, School Health Education Programme coordinators, Food and Drug Administration workers, nutrition officers, sanitary inspectors, NGOs and University researchers. However, not all experts will be willing to support such efforts. Space is not a limiting factor, as a lot of space was available in both communities to implement efforts to address the consumption of unhealthy foods and drinks. Churches, parks, municipal buildings, stadium, community centres and schools could be utilised for a given intervention.
Discussion
This study investigated how ready urban communities are to improve the diets of women of reproductive age in Ghana. The specific objectives were: (i) to determine the stage of readiness of community key informants to address the consumption of unhealthy foods and beverages in adolescent girls and women of reproductive age in two deprived communities at different stages of the nutrition transition in urban Ghana, and (ii) to gain qualitative insights of community factors that could affect the implementation of interventions targeting unhealthy food and beverage consumption.
Whilst consumption of unhealthy foods and beverages was defined as the consumption of energy-dense, nutrient-poor products, key informants referred to unhealthy diets in terms of both nutritional balance and food safety. Actions discussed in the interviews therefore referred to unhealthy in a holistic sense and demonstrate that food hygiene is a concern in the target communities. Despite their different stages of nutrition transition, the mean community readiness scores were similar between the two communities. These indicated that both communities were at a “vague awareness stage”, highlighting that they are not yet ready to address the issue of unhealthy food and beverage consumption in women of reproductive age. This level of readiness reflects the fact that “most key informants feel there is a local concern about the issue under investigation, but there is no immediate motivation to do anything about it” [11]. This result also suggests that a higher prevalence of overweight/obesity in Ga Mashie, compared to Ho Central, has not yet translated into accelerated readiness for intervention.
Within each community, the scores observed across dimensions were quite similar, indicating a relatively low level of readiness for all dimensions of the model. Plested et al. [11] state that for an intervention to be effective, each dimension should be at an equal stage of readiness. Therefore, based on our findings, an initial focus should be on increasing the community knowledge of efforts (Ga Mashie) and the resources available (Ho Central).
Our study is the first to assess the stage of community readiness to address unhealthy diets in Sub-Saharan Africa or other LMICs, making relevant comparisons difficult. However, studies utilising the CRM for obesity prevention interventions have been conducted in South Africa [25] and in several HICs [15, 16, 18, 19, 32, 33], with some studies focusing specifically on deprived communities [20, 21, 34]. The overall readiness stage (i.e. “vague awareness”) found in the current study is higher than the one reported in South Africa (i.e. “denial/resistance stage”) [25]. In both studies, community knowledge of efforts was one of the lowest scoring dimensions. In the South African study, the highest scores were seen for resources (3.75), followed by knowledge of the issue (3.18) [25] whereas in the present study, the highest readiness scores were seen for knowledge of the issue (4.10) and leadership (3.50) (Ga Mashie) and for knowledge of the issue (4.38) and community climate (4.29) (Ho Central).
Findings from our study were also comparable to those found in deprived communities in HICs [20, 21, 34]. As in the current study, the readiness score for the prevention of adolescent obesity in a Latino community in Nebraska was 3, corresponding to the “vague awareness” stage [34]. However, in contrast to the present study, the highest scores were observed for community knowledge of efforts and resources [34], which were the lowest dimensions in our study. In comparison to studies conducted in non-deprived communities in HICs, the stage of community readiness in our study was either similar [16, 18] or consistently lower [15, 19]. For example, a UK study aimed at tackling obesity amongst pre-adolescent girls found much higher readiness scores for implementing both physical activity (6.08; “initiation stage”) and dietary interventions (5.74; “preparation stage”) [19].
Strengths and limitations
This study is novel as it is one of the first studies to assess community readiness in the African context prior to designing and implementing interventions to reduce consumption of unhealthy foods and beverages. A further strength of this study is the thematic qualitative analysis that complemented the quantitative scoring, which provided crucial information that can be leveraged to design and implement effective interventions on healthy eating in the two target communities, which showed a similar level of community readiness.
This study also has some limitations. Including views from only two deprived communities (Ga Mashie and Ho Central) may not be representative of the whole of Accra and Ho. Scoring CRM interviews using pre-defined anchored rating statements has been criticised [35, 36] for permitting too much researcher subjectivity. In order to reduce this potential bias and ensure inter-rater reliability, the CRM interviews were scored independently by two reviewers and then combined. If discrepancies arose between reviewers, these were discussed until consensus was reached. By only focusing on key informants in the community, the CRM places responsibility for health-related issues on the shoulders of communities, and therefore does not engage with other key decision-makers in government.
Implications for future interventions
This study has identified avenues for potential implementation of future interventions. Our findings suggest that community members are relatively knowledgeable about this issue. It was acknowledged that there are some unhealthy food practices occurring within the communities, including increased consumption of ‘fast foods’, eating out, and excessive alcohol consumption. However, there was less knowledge about the specific health consequences of these behaviours. There was recognition from the communities that the consumption of unhealthy foods and beverages is an issue that needs to be tackled (particularly in Ho Central), but this concern does not necessarily translate into prioritisation and action. Key informants interviewed were also concerned that any programmes focusing on improving food hygiene practices and reducing the consumption of unhealthy food and beverages would impact negatively on local businesses and consequently, on community members’ livelihoods. This suggests a need to increase awareness of the issue to ensure it is prioritised and resources are mobilised sensitively to address the issue, whilst including local businesses to ensure that they can continue to trade using healthier food options. This would minimise negative economic consequences of any intervention on the communities concerned. Additionally, it may be necessary to target community members’ understanding of non-communicable disease prevention, emphasising that prevention strategies are preferable to treatment, and a worthwhile investment.
The low scores for community knowledge of efforts implies that there is a need to develop initiatives further, ensuring that these are scaled-up and actively shared within the communities. Any actions that do exist to reduce unhealthy eating are currently targeted at specific population groups and there is a need for interventions that support healthy eating specifically in women of reproductive age.
The relatively low scores for resources suggest that they may act as barriers to implementing interventions. However, it is important to note that there is potential for some existing resources to be leveraged further to support efforts, e.g. information, expert/volunteers, organisations and space. There is a need to consider low-cost strategies and potential support from existing NGOs to administer programmes. Coordinating existing experts and NGO activity and utilising widely available community spaces for information sharing would maximise efforts. Other potential people who might be mobilised to support interventions are members of the municipal assembly, health workers, youth leaders, teachers and traditional leaders, e.g. community chiefs, church leaders, opinion leaders, elders and women’s groups. Information sharing could take place through the radio, as this is seen as a potentially positive delivery route because people can listen to it whilst working. Information contained in booklets or posters, currently displayed in health facilities and schools, could be placed more strategically to ensure a broader community outreach than is currently being achieved.
Conclusions
Despite some awareness that the consumption of unhealthy foods and beverages is an issue amongst women of reproductive age in urban Ghana, tackling unhealthy diets is not yet a priority for intervention, except on a small scale to specific target groups. For both communities, the community readiness assessment suggests that there is a need to raise further awareness regarding the issue prior to implementing initiatives to improve diets. Key stakeholders and groups have been identified, who could be engaged to develop low-cost strategies for raising awareness through channels suggested by the communities. Examples of such channels include community nurses, radios, information buses and posters. The focus should be on raising the awareness that non-communicable diseases are preventable with lifestyle changes and that making these changes will benefit the whole community. Simultaneously, efforts should be made to tackle the issue of food hygiene, which was recognised as both a high concern and priority. If not addressed, this could be a potentially limiting factor in making healthy food choices, e.g. sliced fruits and vegetables that are promoted as part of a healthy diet can become unhygienic and potentially unhealthy if washed in unclean water. This last factor emphasises a unique additional challenge in designing interventions to reduce the rise of diet-related non-communicable diseases in communities undergoing nutrition transition in LMICs. There is a need to ensure such communities are ready for interventions to improve their diets prior to implementation. These communities need to be serviced with interventions that are sensitive to, and include members of the local trading environment and that also incorporate food safety and hygiene, if they are to be successful at reducing diet- related non-communicable diseases.
Abbreviations
- CRM:
-
Community Readiness Model
- HICs:
-
High income countries
- LMICs:
-
Low- and middle-income countries
- NGOs:
-
Non-Governmental Organisations
References
The World Bank Group. Data for Ghana, lower middle income. 2018. https://data.worldbank.org/?locations=GH-XN. Accessed 19 Sept 2018.
Abrahams Z, Mchiza Z, Steyn NP. Diet and mortality rates in sub-Saharan Africa: stages in the nutrition transition. BMC Public Health. 2011;11:801.
Bosu WK. An overview of the nutrition transition in West Africa: implications for non-communicable diseases. Proc Nutr Soc. 2015;74:466–77.
Ofori-Asenso R, Agyeman AA, Laar A, Boateng D. Overweight and obesity epidemic in Ghana-a systematic review and meta-analysis. BMC Public Health. 2016;16:1239.
Langer A, Meleis A, Knaul FM, Atun R, Aran M, Arreola-Ornelas H, et al. Women and health: the key for sustainable development. Lancet. 2015;386:1165–210.
Institute of Medicine (U.S.). Preventing childhood obesity: health in the balance. Washington, D.C.: National Academies Press; 2005.
Edwards RW, Jumper-Thurman P, Plested BA, Oetting ER, Swanson L. Community readiness: research to practice. J Community Psychol. 2000;28:291–307.
Prochaska JO, Velicer WF. The Transtheoretical model of health behavior change. Am J Health Promot. 1997;12:38–48.
Oetting ER, Donnermeyer JF, Plested BA, Edwards RW, Kelly K, Beauvais F. Assessing community readiness for prevention. Int J Addict. 1995;30:659–83.
Prochaska JO, DiClemente CC. Stages of change in the modification of problem behaviors. Progr Behav Modif. 1992;28:183–218.
Plested B, Edwards R, Jumper-Thurman P. Community readiness: a handbook for successful change. 2006. http://www.ndhealth.gov/injury/ND_Prevention_Tool_Kit/docs/Community_Readiness_Handbook.pdf. Accessed 10 Sept 2018.
Plested BA, Jumper-Thurman P, Edwards R, Oetting E. Community readiness: a tool for effective community-based prevention. Prev Res. 1998;5:5–7.
Kesten JM, Griffiths PL, Cameron N. A critical discussion of the community readiness model using a case study of childhood obesity prevention in England. Health Soc Care Community. 2015;23:262–71.
Kostadinov I, Daniel M, Stanley L, Gancia A, Cargo M. A systematic review of community readiness tool applications: implications for reporting. Int J Environ Res Public Health. 2015;12:3453–68.
Sheldon E, Lyn R, Bracci L, Ann Phillips M. Community readiness for childhood obesity prevention. Environ Behav. 2016;48:78–88.
Hildebrand DA, Blevins P, Carl L, Brown B, Betts NM, Poe T. Use of community readiness model to develop and evaluate a pilot culinary training program for school nutrition staff. J Nutr Educ Behav. 2018;50:118–124.e1.
Kostadinov I, Daniel M, Stanley L, Cargo M. Assessing community readiness online: a concurrent validation study. BMC Public Health. 2015;15:598.
Millar L, Robertson N, Allender S, Nichols M, Bennett C, Swinburn B. Increasing community capacity and decreasing prevalence of overweight and obesity in a community based intervention among Australian adolescents. Prev Med (Baltim). 2013;56:379–84. https://doi.org/10.1016/j.ypmed.2013.02.020.
Kesten JM, Cameron N, Griffiths PL. Assessing community readiness for overweight and obesity prevention in pre-adolescent girls: a case study. BMC Public Health. 2013;13:1205.
Jernigan VBB, Boe G, Noonan C, Carroll L, Buchwald D. Assessing feasibility and readiness to address obesity through policy in American Indian reservations. J Health Dispar Res Pract. 2016;9:168–80.
Cyril S, Polonsky M, Green J, Agho K, Renzaho A. Readiness of communities to engage with childhood obesity prevention initiatives in disadvantaged areas of Victoria, Australia. Aust Health Rev. 2017;41:297.
Aboud F, Huq NL, Larson CP, Ottisova L. An assessment of community readiness for HIV/AIDS preventive interventions in rural Bangladesh. Soc Sci Med. 2010;70:360–7.
Borresen E, Stone C, Boré A, Cissoko A, Maiga A, Koita O, et al. Assessing community readiness to reduce childhood diarrheal disease and improve food security in Dioro, Mali. Int J Environ Res Public Health. 2016;13:571.
Han M, Cao L, Anton K. Exploring the role of ethnic media and the community readiness to combat stigma attached to mental illness among Vietnamese immigrants: the pilot project tam an (inner peace in Vietnamese). Community Ment Health J. 2015;51:63–70.
Pradeilles R, Rousham EK, Norris SA, Kesten JM, Griffiths PL. Community readiness for adolescents’ overweight and obesity prevention is low in urban South Africa: a case study. BMC Public Health. 2016;16:763.
Ghana Statistical Service. 2010 Population and Housing Census. Summary report of final results. http://www.statsghana.gov.gh/gssmain/storage/img/marqueeupdater/Census2010_Summary_report_of_final_results.pdf. Accessed 19 Aug 2018.
Ghana Statistical Service (GSS), Ghana Health Service (GHS), ICF International. Ghana demographic and health survey 2014. 2015. https://dhsprogram.com/publications/publication-FR307-DHS-Final-Reports.cfm. Accessed 19 Aug 2018.
CHF International. Accra poverty map. A guide to urban poverty reduction in Accra. 2010. https://www.globalcommunities.org/publications/2010-accra-poverty-map.pdf. Accessed 24 Jan 2017.
Abankwa V, El-Sioufi M, Grimard A, Sommer K, Kuria F. Ghana: Ho city profile. 2009. https://unhabitat.org/wp-content/uploads/2014/07/Ghana-Ho-City-Profile.pdf. Accessed 24 Jan 2017.
Stanley LR. Tri ethnic center community readiness handbook 2nd edition. Model originally developed by Oetting ER, Plested BA, Edwards RW, Thurman PJ, Kelly KJ and Beauvais F. 2014. http://www.triethniccenter.colostate.edu/wp-content/uploads/sites/24/2018/04/CR_Handbook_8-3-15.pdf. Accessed 1 May 2018.
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3:77–101.
Findholt N. Application of the community readiness model for childhood obesity prevention. Public Health Nurs. 2007;24:565–70.
Sliwa S, Goldberg JP, Clark V, Collins J, Edwards R, Hyatt RR, et al. Using the community readiness model to select communities for a community-wide obesity prevention intervention. Prev Chronic Dis. 2011;8:A150.
Frerichs L, Brittin J, Robbins R, Steenson S, Stewart C, Fisher C, et al. SaludABLEOmaha: improving readiness to address obesity through healthy lifestyle in a Midwestern Latino community, 2011–2013. Prev Chronic Dis. 2015;12:140328.
Beebe TJ, Harrison PA, Sharma A, Hedger S. The community readiness survey. Eval Rev. 2001;25:55–71.
Mayer K. In response to the published article “application of the community readiness model for childhood obesity prevention (Findholt, 2007)”. Public Health Nurs. 2008;25:389.
Acknowledgements
We acknowledge the leadership and political support of the Ghana Health Service (national and regional levels), as well as Ga Mashie Development Agency (GAMADA) for their support during the community entry phase of the study. We would like to thank all key informants from Ga Mashie and Ho Central that have taken part in this “Dietary transitions in Ghanaian cities” project.
Funding
The ‘Dietary transitions in Ghana’ project was funded by a grant from the Drivers of Food Choice (DFC) Competitive Grants Programme which is funded by the Bill & Melinda Gates Foundation and the Department for International Development (DFID), and managed by the University of South Carolina Arnold School of Public Health, USA. DFC supports new research on understanding food choice among the poor in low and middle-income countries, strengthening country-level leadership in nutrition and fostering a global community of food-choice researchers.
Availability of data and materials
The data generated during the current study are not publicly available as the project is ongoing and data are not ready for archiving. We will consider requests for access to the data 12 months after the grant funding period (so from May 2020). Requests can be made to Professor Michelle Holdsworth (michelle.holdsworth@sheffield.ac.uk).
Author information
Authors and Affiliations
Contributions
RP, PG, MH, AL, FZ, and MG were involved in the design of this study and in seeking funding for it. AT, SK and NC conducted the research. The paper was conceived by RP, PG and MH. RP and CM performed all analyses with the help of KB. RP and CM wrote the first draft of the paper and RP coordinated contributions from other authors. All authors made critical comments on drafts of the paper. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the Ghana Health Service Ethics Review Committee (Protocol number GHS-ERC:07/09/2016), for primary data collection and an ethics checklist was approved by the University of Sheffield. All interviews were conducted after written informed consent.
Consent for publication
As part of the informed consent process, key informants provided written consent for publication.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Additional files
Additional file 1:
CRM Interview Guide. (DOCX 36 kb)
Additional file 2:
CRM Codebook for analysis. (DOCX 23 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Pradeilles, R., Marr, C., Laar, A. et al. How ready are communities to implement actions to improve diets of adolescent girls and women in urban Ghana?. BMC Public Health 19, 646 (2019). https://doi.org/10.1186/s12889-019-6989-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12889-019-6989-5