Abstract
Background
Delayed antibiotic prescribing reduces antibiotic use for acute respiratory infections in trials in general practice, but the uptake in clinical practice is low. The aim of the study was to identify facilitators and barriers to general practitioners’ (GPs’) use of delayed prescribing and to gain pharmacists’ and the public’s views about delayed prescribing in Australia.
Methods
This study used the Theoretical Domains Framework and the Behaviour Change Wheel to explore facilitators and barriers to delayed prescribing in Australia. Forty-three semi-structured, face-to-face interviews with general practitioners, pharmacists and patients were conducted. Responses were coded into domains of the Theoretical Domains Framework, and specific criteria from the Behaviour Change Wheel were used to identify which domains were relevant to increasing the use of delayed prescribing by GPs.
Results
The interviews revealed nine key domains that influence GPs’ use of delayed prescribing: knowledge; cognitive and interpersonal skills; memory, attention and decision-making processes; optimism; beliefs about consequences; intentions; goals; emotion; and social influences: GPs knew about delayed prescribing; however, they did not use it consistently, preferring to bring patients back for review and only using it with patients in a highly selective way. Pharmacists would support GPs and the public in delayed prescribing but would fill the prescription if people insisted. The public said they would delay taking their antibiotics if asked by their GP and given the right information on managing symptoms and when to take antibiotics.
Conclusions
Using a theory-driven approach, we identified nine key domains that influence GPs’ willingness to provide a delayed prescription to patients with an acute respiratory infection presenting to general practice. These data can be used to develop a structured intervention to change this behaviour and thus reduce antibiotic use for acute respiratory infections in general practice.
Similar content being viewed by others
Background
Antibiotic use contributes to the development of bacterial resistance, [1, 2] which is a significant threat to public health [3]. Acute respiratory infections (ARIs) constitute more than half of all problems treated with antibiotics in general practice [4], but many will resolve without the need for antibiotics [5–7]. Antibiotic resistance appears to be reversible if the selection pressure from antibiotic use is removed [8].
“Delayed prescribing” (also known as “wait-and-see” or “back-up prescription” [9, 10]) is one approach that reduces antibiotic use – 93% of those given an immediate prescription will fill it compared to 32% of those given a delayed script [11]. For patients suffering from cough or common cold, there are no significant differences in duration and severity measures for pain, malaise, fever, cough and rhinorrhoea between patients given a delayed, immediate or no antibiotic prescription. For patients suffering acute otitis media and sore throat, immediate antibiotics do provide slightly quicker relief than those given a delayed prescription but there is an increase in adverse reactions (including nausea, vomiting and diarrhoea) [12, 13]. Patients asked to delay antibiotics were only slightly less satisfied (87%) with care received than those given an immediate antibiotic prescription (92%) [11]. Providing a delayed prescription does not impact re-consultation rates [11] or increase emergency department presentations, [13] is associated with better outcomes [14] and is popular with patients [15].
Delayed prescribing can be used for acute otitis media, acute sore throat/pharyngitis/tonsillitis, the common cold, acute rhinosinusitis and acute cough/bronchitis. Delayed prescribing is the process of a general practitioner (GP) making available an antibiotic prescription during the consultation, but asking patients to delay its use, to see if symptoms will resolve first. Patient concerns and expectations should be addressed when GPs and patients agree to using delayed prescribing. Advice should be given about using the delayed antibiotic if symptoms do not stabilise in accordance with the expected course of the illness or symptoms worsen significantly. Prescriptions can be made available in different ways: patient recontacting the practice subsequently to request it by phone; patients collecting their pre-written prescriptions from the practice after the consultation if their condition worsens; post-dating the prescription; and giving prescriptions to patients while asking them to wait some days before having it dispensed. This last method seems most suitable for the Australian fee-for-service health system. Delayed prescribing has not been implemented in Australian general practice, and local facilitators and barriers to the uptake of this intervention have not been explored. It is the authors belief that delayed prescribing could be one successful strategy Australian GPs could utilise to reduce the overuse of antibiotics.
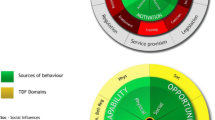
A growing body of research [17–19] supports the use of psychological theories to identify local facilitators and barriers to changing clinicians’ behaviour [20, 21]. The Behaviour Change Wheel (BCW) is an eight-step guide to designing interventions using a theoretical approach [22]. The first four steps help researchers understand the target behaviour: (1) define the problem in behavioural terms, being specific about the target population and the behaviour itself; (2) select the target behaviour from a list of potential competing behaviours; (3) specify the target behaviour in terms of who needs to do what, when, where, how often and with whom; (4) identify what needs to change in the person or environment in order to achieve the desired behaviour by analysing interview data using the Theoretical Domains Framework (TDF) [23]. The TDF comprises 14 theoretical ‘domains’ representing a range of possible theory-based facilitators and barriers to behaviour change [24].
The primary aim of this study was to use the BCW and the TDF to define delayed prescribing by GPs in behavioural terms, and to identify GPs’ facilitators and barriers to changing this behaviour. The secondary aim was to explore pharmacists’ and the public’s views on delayed prescribing, using the TDF as a framework for analysis.
Methods
GPs, pharmacists and members of the public completed a single face-to-face, one-on-one, semi-structured interview (February 2014 to July 2015) with the principal researcher (LS, who had previous interviewing experience and no prior relationships with any participant).
Inclusion and exclusion criteria
Eligible GPs were practising and regularly seeing patients with ARIs. Eligible pharmacists were practising in community pharmacy, and eligible members of the public were those between 18 and 65 years whom accepted the invitation to participate in the research.
Recruitment strategy
We recruited participants from the Gold Coast and the Sunshine Coast, Queensland, and continued until data saturation was reached. LS transcribed the interviews. Recruitment ceased when all domains had been populated and no new themes within each domain emerged [25].
We recruited GPs practising on the Gold Coast by telephone using snowball sampling. One researcher (CDM) provided a list of 8 GPs to approach for interview. LS telephoned them directly (two agreed). After each interview was completed, the researcher requested a name of another GP to contact. This continued until 5 GPs had been interviewed and no new contacts occurred. GPs on the Sunshine Coast were recruited in person using convenience sampling. Medical practices were identified using an internet search. LS walked into medical practices and requested to see the practice manager. LS extended an invitation to participate which the practice manager distributed via email to all GPs in that practice. GPs contacted the researcher directly by telephone or email. Thirteen GPs agreed to be interviewed. Due to difficulties in recruiting GPs, GPs recruited later in the study (mainly the Sunshine Coast) were offered compensation for the time taken for interview (between $70 and $100 depending on length of interview; figures derived from 2015 Royal Australian College of General Practitioners Medicare Benefits Schedule fee summary) [26]. Only half of the GPs interviewed took the offer of compensation. The researcher arranged an appointment with GPs, who were aware that the consultation was for research, not medical purposes.
We recruited community pharmacists on the Sunshine Coast using convenience sampling and face-to-face discussion with pharmacy managers, who either agreed to be interviewed or allocated a member of staff for interview.
We recruited members of the public (in person) in shopping malls, schools (parents only), universities and coffee shops, and some sitting on park benches, using maximum variation sampling (across gender, age and educational status). LS kept a table to document age, gender and educational status of the public interviewed. Gaps in the table identified the ideal demographic of next participant.
Setting
Interviews took place in locations convenient for participants: (1) GPs – at home, in general practices and coffee shops; (2) pharmacists – in their pharmacies; (3) the public – at home, outside school gates and in coffee shops. No others were present during interviews.
Data collection and analysis
Figure 1 shows the process of data collection and analysis.
-
Step 1 (Define the problem in behaviour terms): We (LS and AMcC) used three questions to define the problem [22]: (1) What behaviour?; (2) Where does the behaviour occur; (3) Who is involved in the behaviour?
-
Step 2 (Select the target behaviour): We (LS and AMcC) generated a list of all potential GP behaviours relevant to the target behaviour, including influences out of scope (see Additional file 1). To identify the most important target behaviour, we used four criteria [22] and generated a rating system for each criteria: (1) How much of an impact will changing this target behaviour/issue have on outcome? (1 = highly unlikely, 2 = likely and 3 = very likely); (2) How likely it is that the behaviour can be changed? (1 = yes, 0 = no); (3) How likely it is that the behaviour (or group of behaviours) will have a positive or negative impact on other related behaviours? (1 = negative or no impact, 2 = potential impact, 3 = positive impact); (4) How easy will it be to measure the behaviour? (1 = difficult, 2 = possible, 3 = easy). A total score for each behaviour on the list was generated. LS and AMcC used this score along with discussion to reach consensus about which behaviour to target.
-
Step 3 (Specify the target behaviour): We defined the target GP behaviour from Step 2 using the following questions [22]: (1) Who needs to perform the behaviour? (2) What does the person need to do differently? (3) When will they do it? (4) Where will they do it? (5) How often will they do it? (6) With whom will they do it?
-
Step 4 (Identify what needs to change to achieve target behaviour):
We collected two rounds of interview data for this step (Fig. 1). Round 1 interview questions explored broad factors influencing GPs’, pharmacists’ and the public’s beliefs on delayed prescribing (see Additional file 2). We did not design this topic guide using the TDF and had not defined the problem in behavioural terms when these interviews were conducted, but did complete steps 1–3 before analysis of Round 1 data took place, allowing us to identify domains not explored that may have been important. We piloted interview questions with one GP, 3 pharmacists and 3 members of the public. No pilot interviews were used in the final data set. No repeat interviews were required. Two GPs requested a copy of the transcripts before analysis. Transcribed interviews were sent via secure email, with a request to reply within 2 weeks if issues were identified; no replies were received. Field notes were made after each interview for use during analysis.
LS recorded and transcribed verbatim all Round 1 interviews. Two researchers (LS and AMcC) coded each transcript independently by assigning each relevant piece of data to one or more TDF domains using NVivo (10 QSR International). All coding was discussed and agreed by the two researchers, one of whom (AMcC) had previous experience using the TDF [27]. From this process, we identified that some domains had not been fully explored (skills, beliefs about capability, optimism, intentions, goals, reinforcement and emotion). We then modified the topic guide (interview questions) to target the domains that required further exploration (see Additional file 3). Two researchers (LS and AMcC) analysed the interviews as previously described for Round 1. In addition, within each category, the researchers (LS and AMcC) identified facilitators and barriers to the target behaviour. The process was iterative and, as new data were added to TDF domains, facilitators and barriers were modified, expanded or re-categorised.
We (all authors) agreed relevant domains (i.e. those directly influencing the target behaviour) by consensus using three questions: (1) What needs to happen for the target behaviour to occur? (2) Is there need for change? (3) Is it relevant?
Table 1 outlines the domains identified as important: Knowledge; Physical, cognitive and interpersonal skills; Memory, attention and decision processes; Optimism; Beliefs about consequences; Intentions; Goals; Emotion and Social influences.
Results
Eighteen GPs (8 females, mean age 43 years [range 29–61 years], mean 13 years in practice [range 1–33 years]) with 7 GPs using delayed prescribing, 2 regularly. Two GPs interviewed were married to each other and worked at the same practice but had opposing views on delayed prescribing. Nine pharmacists and three pharmacy assistants (11 female, mean age 36 years [range 24–56 years], mean 10 years in practice [range 1–34 years]) participated. Approximately 35 members of the public were approached for interviews. Fourteen agreed to be interviewed (9 female, mean age 40 years [range 20–61 years], educational status ranged from completion of secondary school to completion of tertiary degrees). One pharmacist withdrew due to time constraints; no GPs or members of the public withdrew. Mean interview time was 29 min (range 13–45 min).
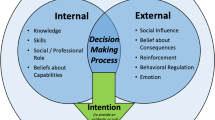
Figure 2 illustrates the key results from steps 1 to 4. We defined the problem as the need for GPs to change from prescribing immediate antibiotics to delayed prescription, and specified when and how this should happen. We identified nine relevant domains that influence this behaviour, briefly discussed below. Table 2 provides example quotations from participants that pertain to facilitators and barriers within these domains. The 5 domains identified as irrelevant were behavioural regulation, professional/social role and identity, beliefs about capabilities, reinforcement, and environmental context and resources (Table 1). GPs believed prescribing is part of their role, with delayed prescribing an extension of this role (professional/social role), and that they have the capability to do it (beliefs about capabilities). GPs did not believe systems aimed at monitoring (behavioural regulation), or punishments and rewards (reinforcement), would be appropriate. GPs believed resources (environmental context and resources) are important to help patients manage their symptoms and follow instructions for delayed prescribing; however, they also believed these resources are not relevant to their adopting delayed prescribing.
Knowledge
All GPs had heard of delayed prescribing but did not use it correctly or only used it selectively. GPs knew that delayed prescribing involves giving an antibiotic prescription to the patient with instructions on how long to wait and when to take the antibiotics if symptoms worsen.
“…if you are no better in a couple of days, fill the script. Um, so I am thinking how often I do it, um, I do do that occasionally, especially if it is near the weekend or something and they can’t come back to see me.” (GP16)
All pharmacists were knowledgeable about management of ARI symptoms. The public reported needing to know when to start antibiotics (if given a delayed prescription) and how to treat their symptoms.
“So I would need to know when to take the antibiotic, so when is the cold getting worse, how long this takes, the expected length of time for the cough and how it would impact my breathing.” (Pt15)
All participants knew antibiotic use caused antibiotic resistance.
Skills
GPs considered they did not need any additional physical skills to conduct delayed prescribing. GPs reported using interpersonal skills to explore patient expectations regarding antibiotic prescription, although they seldom explicitly ask patients about their expectations.
“[I do not ask them about their expectations]… in such a straight forward way – like, I normally ask them what they have been doing to cope before they come to me for help.” (GP19)
All pharmacists reported using interpersonal skills in their interactions with the public to identify customers’ needs. Pharmacists did not believe they need additional skills to conduct delayed prescribing because talking to the public about prescriptions is a skill they use frequently.
“…we are really big on coming down and talking to everyone about their medication, this would be another thing that we already do.” (Ph10)
The public didn’t think they need any skills for delaying taking an antibiotic.
Memory, attention and decision-making
GPs who said they use delayed prescribing use it in highly specific situations: for patients whom they believe are well educated and sensible, and whom they trust will delay filling the prescription. Further, they identified that the only reasons they would use delayed prescribing are if patients have difficulties accessing a GP, are going on holiday, are suffering from otitis media, or demand antibiotics. Some GPs stated they would never use delayed prescribing because they prefer to bring patients back for review.
“…if they perceive the condition isn’t resolving and to come back if they want.” (GP10)
Pharmacists had no comment on this domain. The public stated they would wait for worsening symptoms before taking antibiotics but, if a previous infection had progressed to a severe one or they were in pain, they would be more likely to want to take antibiotics immediately.
Optimism (and pessimism)
The minority of GPs who said they already use delayed prescribing regularly were optimistic about using this strategy. Most GPs believed that it would be difficult to implement delayed prescribing: they do not trust patients to delay and do not believe there is enough evidence to refute this perception. Pharmacists and the public were optimistic about using delayed prescribing.
“Some people are just going to go out and fill the prescription anyway.” (GP19)
“I like the idea that I might be able to make my own decision about when to take antibiotics, this doesn’t frighten me at all” (Pt13)
Beliefs about consequences
Participants (GPs, pharmacists and the public) believed antibiotic resistance is a serious issue influenced by antibiotic use. They identified advantages of delayed prescribing as reduced antibiotic use and resistance, providing an opportunity for patient education, and giving professional satisfaction.
“I think it would be good – it would work, education would be for the people using it” (GP16)
“Um, I use it as it means less reviews, less people coming in, I guess giving patients control over their condition.” (GP09)
“Um, I guess it makes me feel I am just playing a small part in reducing antibiotic resistance.” (GP15)
But they were also concerned that the public would misuse the delayed prescription by either using it immediately or keeping it for a subsequent infection. GPs were specifically concerned about missing serious infections, that delayed prescribing could be more time-consuming and that it could potentially lose them business.
“…but it is easier to give the script because the patient leaves the room immediately. So most of that is time pressure.” (GP06)
Intentions
GPs who regularly use delayed prescribing said they do not have to consciously think about it – they believe it is an effective strategy and intend to use it as often as they can. GPs who use delayed prescribing selectively said they need to think carefully if patients fit certain criteria. Most GPs stated they have no intention of using delayed prescribing because they can bring patients back for review. All pharmacists stated that, if they have the time, they intend to talk to patients who request an antibiotic prescription be filled. The public said they intend to do what the GP asks of them.
Goals
Most GPs did not mention that they had a goal of using delayed prescribing. One GP expressed a strong goal of using delayed prescribing if patients were able to make an informed decision on their care. All groups identified the main goal of sick patients is to feel better.
“If I was bedridden then I would take anything to get better.” (Pt08)
Emotion
This domain overlaps with the ‘beliefs about consequences’ domain – GPs and the public expressed a fear of missing a serious diagnosis - one GP stated he is a regular prescriber of antibiotics because he had had some patients experience severe complications from not starting antibiotics sooner. GPs believe delayed prescribing reduces patient anxiety about disease progression because they have a management plan in place.
Social influences
Several conflicting social influences were evident. These influences centre on perceived expectations of antibiotic treatment and on trust between clinicians and patients. All GPs said they do not feel pressured when patients demand antibiotics, but they reported mixed views on whether patients expect antibiotics. The time and day of the week, patients’ social situation (e.g. getting back to work, financial status, age and comorbidities) and an existing relationship with a patient influence their antibiotic prescribing. GPs who use delayed prescribing reported the practice encourages trust between GPs and patients. Other GPs reported they don’t trust their patients; however, they contradicted this statement by saying they believe that their patients listen to them.
“A position of trust I think. Being a doctor. Patients listen to you.” (GP15)
“Oh – you see – look, I don’t trust my patients enough for delayed prescribing.” (GP17)
“… if we take the time to educate patients here, when they are sitting in the chair, they go home, they don’t use the antibiotic and then they get better, if we are talking about the best case scenario, then they learn for the rest of their lives – they will get better without antibiotics but not just that – they also learn that we have trusted them and it all worked out well.” (GP19)
Pharmacists acknowledged many people do not want antibiotics to treat their illness and would rather have natural remedies; however, pharmacists also believe some people go to the GP expecting antibiotics. Many members of the public stated they do not want antibiotics if they don’t need them; all identified good relationships with both GPs and pharmacists as important because they often want reassurance they are doing the right thing. The public reported trusting GPs, saying they would do what the GP asks of them and that delayed prescribing indicates that the GP trusts them to make decisions about their own health.
“Even if it was also just re-assurance that I knew what I was talking about – and then he wouldn’t need to hand over that antibiotic prescription straight over, and then I wouldn’t need to start them on it straight away.” (Pt04)
Discussion
Main findings
To implement delayed prescribing in Australian general practice, GPs need to change from immediate antibiotic prescribing to delayed prescribing and educate patients about how to manage ARI symptoms and when to start antibiotics. This education can take place during any consultation with a person presenting with an ARI in a general practice setting. Nine TDF domains influence this behaviour: knowledge; skills; memory, attention and decision-making; optimism; beliefs about consequences; intentions; goals; emotion; and social influences. Pharmacists and members of the public are broadly supportive of using delayed prescribing; whilst most had not heard of delayed prescribing, they were optimistic that it could be a useful strategy to reduce antibiotic use.
Although effective, uptake of delayed prescribing by general practitioners (GPs) appears to be low: one study found that 15% of patients prescribed antibiotics in the past year had been given the option of a delayed prescription [16]. These findings may be helpful to researchers trying to implement an intervention to support delayed prescribing in other fee-for-service environments.
Strengths and limitations
The main strengths of this study are the systematic and structured approach to defining and specifying, in behavioral terms, the problem of implementing delayed prescribing, and the use of a theory-driven approach to identify facilitators and barriers to changing this behaviour. Interviewing pharmacists and members of the public ensured that views from these two key groups of stakeholder can be used to inform the development of a future intervention.
The main limitation of this study is that the TDF was not used to design the topic guide for Round 1 interviews as the BCW work book was not published and the TDF was not identified as a method for analysis until after the interviews had commenced. However, the TDF was used for the interim analysis and to identify gaps in the emerging data that were subsequently addressed by modifying the interview questions. More than one-third of GPs in this sample reported using delayed prescribing – higher than the uptake rates estimated earlier, [16] which could indicate selection bias, in that GPs who were supportive of delayed prescribing were more likely to agree to be interviewed. There could also have been social desirability bias in all interviews where participants answered the questions in a manner that would be viewed as favourable by the researcher. Snowball sampling of GPs on the Gold Coast and convenience sampling of participants on the Sunshine Coast may also have introduced selection bias. Further, most of the pharmacists interviewed were female. Participants were encouraged to arrange interviews at a time and place most convenient to them, with most interviews of GPs and pharmacists occurring at workplaces. This factor may have affected participants’ responses due to time pressure, and may have led to participants’ feeling less able to disclose certain information. The decision about whether to prescribe antibiotics for patients with ARIs is potentially a sensitive issue. Hence, GPs may be reticent to divulge overprescribing – only one GP admitted to being a high prescriber. We did not collect data on GPs’ current rate of antibiotic prescription.
Comparison with existing literature
Similar to findings in other qualitative studies of delayed prescribing, [28–33], we found that Australian GPs were concerned about the misuse of prescriptions by patients, diagnostic uncertainty and patient hoarding of medication. We also found that Australian GPs were often highly selective regarding the patients for which they used delayed prescribing. Some of these concerns are not consistent with the evidence: 32% of patients fill a delayed prescription whilst 93% fill an immediate prescription [11, 20, 34, 35]. Hoarding could be a valid concern. When asked about repeat prescriptions (for any indication), one-third of Australian respondents stated they would keep prescriptions for future use [36]. To our knowledge, this study is the first to explore facilitators and barriers to delayed prescribing using the TDF and the BCW. However, this approach has been used successfully for developing other interventions [27, 37–39].
Implications for clinicians and policy makers
There is adequate evidence that delayed prescribing reduces antibiotic use, [11] and the concept has been previously introduced into the Australian GP environment [40]. However, our interviews indicate the practice is not consistently used, with many GPs expressing concerns about its implementation. GPs can use the results of this study to identify their individual facilitators and barriers to using this strategy in their own practice. Policymakers and researchers will need to consider the facilitators and barriers to delayed prescribing identified in this study before designing an acceptable implementation intervention.
Unanswered questions and future research
We have identified theory-derived facilitators and barriers to the implementation of delayed prescribing in Australian general practice. The next step is to use the BCW to identify which behaviour-change techniques could be used to target the TDF domains that influence the use of delayed prescribing by Australian GPs, and then to test the feasibility of this theory-based intervention in Australian general practice.
Conclusion
Using a theory-driven approach, we have identified nine key domains that influence Australian GPs’ willingness to provide a delayed prescription to patients with an ARI presenting to general practice. These data can be used to develop a structured intervention to change GPs’ behaviour and thus reduce antibiotic use in Australian general practice.
Abbreviations
- ARI:
-
Acute respiratory infection
- BCW:
-
Behaviour Change Wheel
- GP:
-
General practitioner
- TDF:
-
Theoretical Domains Framework
References
Costelloe C, Lovering A, Montgomery A, Lewis D, McNulty C, Hay AD. Effect of antibiotic prescribing in primary care on meticillin-resistant Staphylococcus aureus carriage in community-resident adults: a controlled observational study. Int J Antimicrob Agents. 2012;39(2):135–41.
Goossens G, Ferech M, Vander Stichele R, Elseviers M. Outpatients antibiotic use in Europe and association with resistance: a cross national database study. Lancet. 2005;365(9459):579.
World Health Organization. Global Action Plan on Antimicrobial Resistance. Geneva: World Health Organization; 2015.
Pan Y, Henderson J, Britt H. Antibiotic prescribing in Australian general practice: How has it changed from 1990–91 to 2002-03? Respir Med. 2006;100(11):2004–11.
National Institute for Health and Clinical Excellence. Respiratory tract infections - antibiotic prescribing. In: Prescribing of antibiotics for self-limiting respiratory infections in adults and children in primary care. London: National Institute for Health and Clinical Excellence; 2008.
Arroll B. Antibiotics for upper respiratory tract infections: an overview of Cochrane reviews. Respir Med. 2005;99(3):255–61.
Smith SM, Fahey T, Smucny J, Becker LA. Antibiotics for acute bronchitis. Cochrane Database Syst Rev. 2004;(4):CD000245. doi:10.1002/14651858.CD000245.pub2.
Costelloe C, Metcalfe C, Lovering A, Mant D, Hay AD. Effect of antibiotic prescribing in primary care on antimicrobial resistance in individual patients: systematic review and meta-analysis. BMJ. 2010;340:c2096.
McNulty C, et al. Have the public's expectations for antibiotics for acute uncomplicated respiratory tract infections changed since the H1N1 influenza pandemic? A qualitative interview and quantitative questionnaire study. BMJ Open. 2012;2(2):e000674.
Sprio D, Arnold H. The concpet and practice of a wait-and-see approach to acute otitis media. Curr Opin Pediatr. 2008;20(1):72–78.
Spurling GKP, Del Mar CB, Dooley L, Foxlee R, Farley R. Delayed antibiotics for respiratory infections. Cochrane Database Syst Rev. 2013;(4):CD004417. doi:10.1002/14651858.CD004417.pub4.
Little P, et al. Antibiotic prescription strategies for acute sore throat: a prospective observational cohort study. Lancet Infect Dis. 2014;14(3):213–9.
Spiro D, Tay K, Arnold D, Dziura JD, Baker MD, Shapiro ED. Wait and see prescription for the treatment of acute otitis media - a randomized control trial. Am Med Assoc. 2006;296(10):123.
Little P, et al. Observational study of effect of patient centredness and positive approach on outcomes of general practice consultations. BMJ. 2001;323:908.
Smith SM, Fahey T, Smucny J, Becker LA. Antibiotics for acute bronchitis. Cochrane Database Syst Rev. 2014;(3):CD000245. doi:10.1002/14651858.CD000245.pub3.
McNulty CAM, Lecky DM, Hawking MKD, Quigley A, Butler CC. Delayed/back up antibiotic prescriptions: what do the public think? BMJ Open. 2015;5:e009748. doi:10.1136/bmjopen-2015-009748.
Craig P, Dieppe P, Macintyre S, Michie S, Nazareth I, Petticrew M. Developing and evaluating complex interventions: new guidance. Med Res Counc. 2008.
Francis JJ, et al. Evidence-based selection of theories for designing behaviour change interventions: using methods based on theoretical construct domains to understand clinicians' blood transfusion behaviour. Br J Health Psychol. 2009;14(Pt 4):625–46.
Michie S, Prestwich A. Are interventions theory-based? Development of a theory coding scheme. Health Psychol. 2010;29(1):1–8.
Arnold S, Strauss R. Interventions to improve prescribing practices in ambulatory care. Cochrane Database Syst Rev. 2005;(4):CD003539. doi:10.1002/14651858.CD003539.pub2.
McCullough AR, Glasziou PP. Delayed antibiotic prescribing strategies-time to implement? JAMA Intern Med. 2016;176(1):29–30.
Michie S, Atkins L, West R. The behaviour change wheel: a guide to designing interventions. Great Britian: Silverback Publishing; 2014.
Francis JJ, O'Connor D, Durran J. Theories of behaviour change synthesised into a set of theoretical groupings: introducing a thematic series on the theoretical domains framework. Implement Sci. 2012;7(35). doi:10.1186/1748-5908-7-35.
Cane J, O'Connor D, Mickie S. Validation of TDF in behaviour change and implementation research. Implementation Sci. 2012;7(37). doi:10.1186/1748-5908-7-37.
Creswell JW. Research design. 3rd ed. California: Sage Publications, Inc.; 2009.
Australian Government Department of Health. Medicare Benefits Schedule Book. Canberra: Commonwealth of Australia; 2014.
McCullough AR, Ryan C, O'Neill B, Bradley JM, Elborn JS, Hughes CM. Defining the content and delivery of an intervention to Change AdhereNce to treatment in BonchiEctasis (CAN-BE): a qualitative approach incorporating the Theoretical Domains Framework, behavioural change techniques and stakeholder expert panels. BMC Health Serv Res. 2015;15:342.
Hoye S, Gjelstad S, Lindboek M. Effects on antibiotic dispensing rates of interventions to promote delayed prescribing for respiratory tract infections in primary care. Br J Gen Pract. 2013;63(616):E777–86.
Hoye S, Frich J, Lindbaek M. Delayed prescribing for upper respiratory tract infections: a qualitative study of GPs' views and experiences. Br J Gen Pract. 2010;60(581):907–12.
Arroll B, Goodyear-smith F, Thomas DR, Kerse N. Delayed antibiotic prescriptions: what are the experiences and attitudes of physicians and patients? J Fam Pract. 2002;51(11):954–59.
Francis NA, et al. Delayed antibiotic prescribing and associated antibiotic consumption in adults with acute cough. Br J Gen Pract. 2012;62(602):e639–46.
Peters S, et al. Managing self-limiting respiratory tract infections: a qualitative study of the usefulness of the delayed prescribing strategy. Br J Gen Pract. 2011;61(590):e579–e589. https://doi.org/10.3399/bjgp11X593866.
Hoye S, Frich JC, Lindbaek M. Use and feasibility of delayed prescribing for respiratory tract infections: a questionnaire survey. BMC Fam Pract. 2011;12:34.
Arroll B, Kenealy T, Kerse N. Do delayed prescriptions reduce antibiotic use in respiratory tract infections? A systematic review. Br J Gen Pract. 2003;53(496):871–7.
Little P, et al. Delayed antibiotic prescribing strategies for respiratory tract infections in primary care: pragmatic, factorial, randomised controlled trial. BMJ. 2014;348:g1606.
Thompson A, Copping S, Stafford A, Peterson G. Repeatable antibiotic prescriptions: an assessment of patient attitudes, knowledge and advice from health professionals. Australas Med J. 2014;7(1):1–5.
Webb J, Foster J, Poulter E. Increasing the frequency of physical activity very brief advice for cancer patients. Development of an intervention using the behaviour change wheel. Public Health. 2016;133:45–56.
Newlands R, et al. Barriers and facilitators of evidence-based management of patients with bacterial infections among general dental practitioners: a theory-informed interview study. Implemen Sci. 2016;11(1):1–12.
O'Connell SE, et al. Providing NHS staff with height-adjustable workstations and behaviour change strategies to reduce workplace sitting time: protocol for the Stand More AT (SMArT) Work cluster randomised controlled trial. BMC Public Health. 2015;15:1219.
Del Mar C, Galsziou P, Lowe JB, van driel ML, Hoffman T, Beller E. Addressing antibiotic resistance: focusing on acute respiratory infections in primary care. Aust Fam Physician. 2012;41(11):839–40.
Acknowledgements
We wish to thank all the participants in the study and Dr Leigh Findlay for editing services.
Funding
This project was funded by the National Health and Medical Research Council (GNT1044904).
Availability of data and materials
All data generated or analysed during this study are included in this published article [and its Additional files].
Authors’ contributions
LS conducted all the interviews and led the writing of the manuscript. AMcC contributed to the analysis of the data and drafting of the manuscript. LS, AMcC, CDM and JL contributed to the conceptual and theoretical development of the study, critically reviewed and contributed to draft revisions, and read and approved the final version of the paper.
Authors’ information
LS, JL: University of the Sunshine Coast, Faculty of Science, Health and Engineering, Maroochydore, Queensland, 4558, Australia. LS, AMcC, CDM: Bond University, Centre for Research in Evidence-Based Practice, Faculty of Health Sciences and Medicine, Gold Coast, Queensland, 4229, Australia.
Competing interests
The authors declare they have no competing interests.
Consent for publication
Not applicable.
Ethics approval and consent to participate
The University of the Sunshine Coast Human Research Ethics Committee considered the ethics application for face-to-face interviews and confirmed it was low risk (Ethics Approval Number S/13/556). Consent was given by each participant prior to interview.
Author information
Authors and Affiliations
Corresponding author
Additional files
Additional file 1:
Step 2 in Behaviour Change Wheel. (DOCX 15 kb)
Additional file 2:
Topic Guide for Round 1 interview questions. (DOCX 14 kb)
Additional file 3:
Topic guide for Round 2 interview questions (modified: Step 4a in Behaviour Change Wheel). (DOCX 20 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Sargent, L., McCullough, A., Del Mar, C. et al. Using theory to explore facilitators and barriers to delayed prescribing in Australia: a qualitative study using the Theoretical Domains Framework and the Behaviour Change Wheel. BMC Fam Pract 18, 20 (2017). https://doi.org/10.1186/s12875-017-0589-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12875-017-0589-1