Abstract
According to WHO, cancer is the cause of ~5 million deaths annually. To date, there is no universal solution to fight cancer despite outstanding achievements of radiotherapy, chemotherapy, and immunotherapy. In this regard, there is a need to develop new approaches to antitumor therapy, in particular based on the search and use of targeted molecules that allow killing tumor cells of various types with high efficiency without significant toxic effects on healthy organs and tissues. This review presents the characteristics of the main proteins of the heat shock proteins (HSP) family, the features of their expression in tumor cells, and the possibility of using monoclonal antibodies against these proteins as a guiding vector for antitumor immunotherapy.
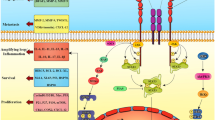
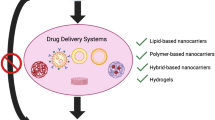
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1. INTRODUCTION
7. CONCLUSIONS
1. INTRODUCTION
Targeted cancer therapy based on antibodies to the markers exposed predominantly on the surface of cancer cells has a number of advantages compared to chemotherapy. Such antibodies can have a direct cytotoxic effect, but the most promising approach is the development of an antibody–drug conjugate or complex. The structure of the antibody ensures long-term circulation of such a pair in the blood, delivering the cytotoxic drug into the tumor. Several such conjugates are already approved in the USA. The examples of target molecules for the treatment of solid tumors include the epidermal growth factor receptor HER2, the trophoblast receptor Trop2, the cellular adhesion molecule nectin-4, and others [1]. For the treatment of lymphomas, receptors expressed on lymphoid and other hematological cells (CD19, CD22, CD33, CD30, BCMA, CD79b) are used [2].
Heat shock proteins (HSP) exposed on the plasma membrane can be one of the target markers of solid tumors. The presence of these marker proteins on the surface of cancer cells allows the delivery of various antitumor drugs. Delivery of antitumor drugs to these targets is universal for many solid tumors, including metastatic ones, and demonstrates promising results in combinational therapy.
The aim of this work was to summarize the data on HSPs as a promising target for research and for targeted drug delivery in antitumor therapy.
2. FUNCTIONS OF HEAT SHOCK PROTEINS
HSPs function as molecular chaperons, participating in the conformationally correct folding of de novo synthesized proteins, their transportation, as well as in the control of the formation of protein complexes, which allows maintaining cellular proteostasis [3]. Exposure to various stress factors (hypoxia, sudden temperature changes, the influence of reactive oxygen species, etc.) leads to the denaturation of some intracellular proteins and to the formation of toxic protein aggregates [3–5]. These processes are counteracted by a system of intracellular molecular chaperons, consisting mainly of HSPs, which are involved in the refolding of denatured proteins and in the ubiquitin-dependent proteasomal degradation of the damaged proteins. In normal cells, HSPs are typically located intracellularly. In cancer cells, HSPs can be translocated to the cell surface, however the reasons and the mechanisms of this process are not well understood yet. The unusual surface localization of HSPs has been found in a wide range of cancer cells of different types, which allows the classification of membrane-associated HSPs as tumor-specific markers [6]. Along with this, the extracellular form of HSPs has also been registered. These proteins and antibodies recognizing them can be detected in blood serum, urine, and other body fluids. The role of membrane-associated and extracellular HSPs, as well as the mechanisms of their translocation to the cell surface and their secretion into the extracellular fluid, are not clear enough yet. However, the tumor-specificity of this phenomenon has attracted the attention of the researchers due to the possibility to use HSPs for targeted delivery of chemotherapeutic drugs to cancer cells and for antitumor immunotherapy [7, 8].
HSPs are usually classified according to their molecular mass. The main groups are HSPs with a mass of 110, 100, 90, 70, 60, 40 kDa, as well as small HSPs. The mechanisms of HSP functioning have been studied for a long time, but many aspects of these processes remain incompletely understood [9–12].
The group of small HSPs includes the proteins with a mass of 12–43 kDa, which do not require ATP to carry out their intracellular functions. To perform their chaperone functions, these proteins form multimeric complexes. Along with this, HSP27 is involved in the organization of the cytoskeleton and implementation of apoptosis [12]. HSP40 is a cochaperone that plays an important role in the transport of proteins to HSP70 and regulation of its ATPase activity. HSP60 is a conserved protein that performs protein folding and controls the transport of proteins into mitochondria. The presence of HSP60 in the extracellular space can trigger autoimmune reactions and antitumor adaptive immune response [10]. HSP70 promotes the synthesis and refolding of proteins, assembly of polypeptide chains; it also prevents protein aggregation and participates in the transport and degradation of proteins [13]. HSP70 is associated with the mitochondrial apoptosis and receptor-dependent apoptosis signaling pathways [14]. Like HSP27 and HSP70, the HSP90 family inhibits cell apoptosis and plays an important role in the folding, stabilization, activation, and proteolytic degradation of proteins [9]. Typically, HSPs perform chaperone functions together. In particular, the functions of HSP70 are carried out with the participation of HSP40 and HSP10 (Fig. 1) [15].
Mechanism of protein refolding by HSP70. HSP40 (DnaJ), containing a J domain, transports misfolded proteins (substrate) to HSP70 (1); HSP40 triggers ATP hydrolysis and conformational changes in the structure of HSP70, stabilizing the bonds between the substrate and HSP70 (2); the nucleotide exchange factor GrpE (HSP10) participates in the nucleotide exchange in the HSP70 molecule (3); the released substrate either returns to its native conformation (solved conformation) (4), or its structure remains unresolved, thus the substrate binds to HSP70 again and undergoes refolding [15].
HSP70 has two functional domains: a nucleotidebinding domain (NDB) at the N-terminus and a substratebinding domain (SBD) located closer to the C-terminus [16]. The TKDNNLLGRFELSG (TKD) sequence, containing 450–461 a.a., is localized at the C-terminus [17]. The immunization of mice with the TKD peptide induced the formation of HSP70.1 antibodies, which were able to bind to HSP70 on the cell membrane due to the rather exposed position of the C-terminus of the chaperone on the plasma membrane surface. Thus, the tumor cell membrane carrying HSP70 can serve as a target structure for specific antibodies that can deliver therapeutic drugs precisely to cancer cells or that can stimulate antitumor activity of the immune system.
3. HEAT SHOCK PROTEINS AS TUMOR MARKERS
The level of HSP expression can reflect the dynamics of tumor development and has characteristic features for each specific type of cancer (Table 1). Overexpression of HSP40 was found in many types of cancer, including colorectal, gastric, and lung cancer [18]. Overexpression of HSP60 can both stimulate tumor development (ovarian cancer, glioblastoma, etc.) and suppress it (hepatocellular carcinoma), which suggests the possibility of using this protein for oncological diagnostics and therapy [12]. Overexpression of HSP70 is often associated with metastasis and invasiveness in head and neck squamous cell carcinoma, childhood acute myeloid leukemia, breast cancer, and colorectal cancer. High level of HSP70 expression can serve as a tumor-specific marker of a highly aggressive tumor [9, 10, 12]. Increased expression of HSP90 can indicate an unfavorable prognosis in various tumors, including cholangiocarcinoma, glioblastoma, lung, stomach, breast, and prostate cancer [9].
4. TRANSLOCATION OF HSP70 TO CELL SURFACE
Translocation of HSPs to the cancer cell surface has been registered in many types of cancer [19–22]. Translocation of HSPs, in particular of HSP70, to the surface of the plasma membrane and secretion into the extracellular space is carried out through alternative vesicular transport without the participation of the Golgi complex [23], because the addition of general secretory pathway inhibitors such as monensin or colchicine, to heat-shocked cells does not inhibit chaperone release [22]. In the classical protein secretion pathway, a specific peptide signal should be present, lacking in most HSPs. The inhibitor of this pathway, brefeldin A, also did not affect the secretion of HSP70 from the cells. Apparently, apart from the release of HSP70 in vesicles, other ways of alternative protein secretion can be involved, for example, with the use of ABC transporters or indirectly through pores [24]. However, protein release is affected by methyl-β-cyclodextrin, a drug that destroys lipid microdomains [24]. Globotriaosylceramide (Gb3), a component of cholesterol-enriched lipid rafts in the plasma membrane, is rarely found in normal cells, but is often present in tumor cells. A significantly higher amount of Gb3 on the surfaces of HSP70-positive cancer cell lines in comparison to HSP70-negative ones reflects the fact that this protein interacts with Gb3 on the membrane surface [26]. Moreover, the membrane form of HSP70 bound to phosphatidylserine (PS) [27] has been found on the external side of the plasma membrane of hypoxic cancer cells. Normally, PS is located on the internal side of the membrane, which is supported by a group of enzymes such as ATP-dependent flippases [28], as well as by floppases and calcium-dependent scramblases. However, under stress conditions, PS together with HSP70 is translocated to the outer surface of the cell [29]. Interestingly, in addition to the exposure to classical stress factors, the introduction of exogenous recombinant HSP70 into culture medium also facilitated the appearance of endogenous HSP70 on the outer side of the plasma membrane [30]. It is possible that membrane-associated and exogenous HSP70 can bind to each other through protein-protein interactions [31].
HSP70 is capable of activating innate and adaptive immunity cells [6], both by being in the extracellular space and associated with tumor cell membranes [32]. It has been shown that HSP70 induces the maturation of dendritic cells, expression of costimulatory molecules CD40, CD86, CD80 by these cells, and synthesis of pro-inflammatory cytokines IL-6, TNF- α, and IL-12p40. HSP70 also increases the ability of dendritic cells to present antigens to T cells by cross-presentation [33]. Extracellular HSP70 significantly increases the level of expression of pro-inflammatory cytokines in monocytes and macrophages by activating the Toll-like receptors 2 and 4 signaling pathway. It also activates neutrophiles and promotes the secretion of reactive oxygen species [34]. However, a significant number of published studies indicates the opposite: the anti-inflammatory effect of extracellular HSP70 on immune cells. In particular, a decrease in the synthesis of TNF-α and reactive oxygen specie production has been shown using a monocytic cell line and human neutrophiles when these cells were exposed to lipopolysaccharide [35, 36]. Therefore, literature data suggest that extracellular form of HSP70 can have a multidirectional effect on immune cells.
A number of authors have found that HSP70 is involved in tumorigenesis. In particular, it has been shown that the extracellular pool of these proteins, released by tumor cells, is capable of suppressing the adaptive immune response by inhibiting macrophages [37]. On the other hand, there is information in the literature showing the suppression of glioblastoma growth in rats upon the injection of exogenous recombinant HSP70 [38]. It has also been demonstrated that exogenous HSP70 and HSP70 exposed on cell membrane stimulate the antitumor activity of NK cells, enhancing their migration, proliferation, and cytolytic activity [39]. Ex vivo administration of HSP70 in combination with IL-2 resulted in a significant activation of NK cells [40]. CD4+ and CD8+ T cells, in turn, are also capable of forming an antitumor response in the presence of HSP70. Transfection of cancer cells with a transgene encoding HSP70 led to the activation of T cell immunity and suppression of tumor growth [33]. On the other hand, HSP70 can induce the polarization of tumor-associated macrophages from M2 to M1, thus stimulating the antitumor immunity [41]. Moreover, the HSP70 exposed on cell membrane activates the formation of regulatory T cells (Tregs) that suppress inflammation [42, 43].
5. TARGETED DRUG DELIVERY TO TUMORS USING ANTIBODIES AGAINST HEAT SHOCK PROTEINS
Currently, antitumor drugs based on monoclonal antibodies (mAb) against specific epitopes, such as ipilimumab (mAb against CTLA-4), trastuzumab (mAb against HER2), and rituximab (mAb against CD20), have been proven to be highly effective. There are several commercially available mAbs against different epitopes of HSP70, predominantly against the C-terminus [44], that can be used for targeted drug delivery to cancer cells displaying this protein on their surface.
Nanoparticles (NPs) are widely used as drug carriers. In particular, of great interest are magnetic NPs based on iron, nickel, cobalt or their oxides (magnetite Fe3O4, hematite α-Fe2O3, maghemite g-Fe2O3 and B-Fe2O3) that are characterized by high sensitivity to external magnetic field. Superparamagnetic NPs, especially those based on iron oxide, SPIONs, are most effective. Due to their characteristics, they make it possible to deliver drugs into cancer cells, as well as to visualize the tumor and metastases [45]. Coating these NPs with monoclonal antibodies against HSP70 enhanced the antitumor effect in a rat glioma model [46]. The content of the SPIONs–mHSP70.1 complex inside C6 rat glioma cells was 7 times higher than the accumulation of uncoated NPs. Cellular uptake of NPs bound to antibodies against HSP70 was further enhanced after exposure to a single dose of ionizing radiation [47].
The antitumor effect of magnetic NPs can be enhanced by combination therapy using an alternative magnetic field (AMF). AMF promotes heating of NPs through mechanisms of relaxation or hysteresis, which depends on the size of the nanostructure [48]. This type of therapy is called AMF-induced hyperthermia. It allows killing of cancer cells by heating them with reduced side effects. Combination therapy using magnetic NPs and their further heating due to AMF in tandem with radiotherapy has been demonstrated to be effective for the treatment of patients with glioblastoma and prostate cancer, which indicates that this approach is promising for further development [49, 50].
Gold NPs (AuNPs) are characterized by improved biocompatibility and widely used for drug delivery into tumors, diagnostics, visualization, as well as for photothermic and photodynamic therapy [46, 51, 52]. In the same way as iron-based NPs, coating of AuNPs with antibodies against HSP70 (HSP70.1) increased their uptake by cancer cells in comparison to uncoated NPs or NPs coated with isotypic IgG1 antibodies, which was shown both in vitro and in vivo in the rat model of glioma. These NPs were localized in the perinuclear region after 24 h [53].
While the use of AMF was justified for magnetic NPs, administration of AuNPs is combined with the use of X-ray radiation or plasmonic photothermal therapy (PPTT). It has been shown that exposure of cancer cells with absorbed AuNPs to X-ray radiation leads to an increase in the number of double-stranded DNA breaks due to the formation of low-energy secondary electrons and to oxidative stress [54, 55]. In the case of PPTT, a laser with a wavelength close to a plasmonic one heats the AuNPs, which damages cancer cells without harming surrounding tissue. However, experiments with epithelial cancer cell lines (oral cavity, breast, liver) have shown that only cells with a reduced amount of HSP70 were susceptible to apoptosis [56]. When using HSP70 inhibitor, apoptosis was observed in all three cell lines, which was due to the suppression of the protective effect of the chaperone. Therefore, the combination of targeting HSP70 on the surface of cancer cells with inhibition of the chaperone function of this protein has shown promise.
Apart from the use of full-sized mAb against HSP70, smaller molecules, such as mini-antibodies and peptides, are widely used in the field of cancer theranostics. These molecules are characterized by a shorter circulation period in blood, rapid clearance from the organism, favorable biodistribution, and an improved penetration into cancer cells in comparison to antibodies. The use of a synthetic 14-mer TKD-peptide, which is part of the C-terminus of HSP70 is functionally justified [57]. It ensures the effective binding of the peptide with a membrane form of HSP70. Membrane chaperone, in turn, is rapidly metabolized within the endosome, allowing TKD to localize within the tumor cells. TKD does not induce an immune response because it is a sequence of endogenous HSP70. Therefore, TKD can be safely administered multiple times. However, there is data showing that immunization of mice with TKD leads to the development of the antibody-dependent cellular cytotoxicity [17, 19].
Certain antitumor drugs can be delivered by mAbs not only as part of NPs, but also as a drug–antibody conjugate. For instance, anti-HSP65 mouse mAb ML30 conjugated to saporin-6 (ribosome-inactivating protein) almost fully inhibited cell proliferation of cell lines U937 and Daudi that express HSP65 on their surfaces [58].
Targeted drug delivery systems are summarized in Table 2 [59–73]. Liposomes, various biopolymer-based carriers, NPs of different compositions can be decorated with antibodies. They can also be used in combination with chemotherapy drugs.
The presence of HSP70 on the cell membrane has been registered in oral cancer [74], colorectal cancer [75], and several others. Targeting membrane-associated HSP70 may provide a new strategy in cancer immunotherapy. It is known that the amount of membrane HSP70 can be up to 10% of the intracellular pool of a tumor cell [40]. The appearance of HSPs on the cell membranes means that the intracellular pool of these proteins has also been increased, which is directly related to the effective functioning of chaperones in cells. Suppression of the chaperone function of HSPs leads to the suppression of tumor cells growth and, in some cases, to their death. In this regard, one of the directions of antitumor therapy is the use of different molecules that suppress the protective activity of HSPs. In particular, it has been demonstrated that the neutralizing peptide ADD70, containing an apoptosis-inducing factor domain and able to interact with HSP70, increases the sensitivity of rat colorectal cancer cells and of mouse melanoma cells to apoptosis induced by cisplatin [76]. Pifithrin-μ blocks the association of HSP70 with its co-chaperone HSP40. Combination therapy using pifithrin-μ and oxaliplatin significantly enhanced the cytotoxic effect of oxaliplatin against human colorectal and prostate cancer cells in vitro [77]. MAL3101, allosteric HSP70 inhibitor that blocks the ATPase activity of the nucleotide-binding domain, efficiently suppressed the cell proliferation of breast cancer, multiple myeloma, Merkel cell carcinoma, colorectal cancer, and others [78, 79]. Other HSP70 inhibitors (tanespimycin, MKT-077) also efficiently enhance the antitumor activity of chemotherapy drugs [80–83].
Apart from targeted delivery of NPs and different therapeutic drugs into cancer cells, another advantage of mAbs against HSP70 is their ability to activate antitumor antibody-dependent cellular cytotoxicity (ADCC).
6. POSSIBLE MECHANISMS OF ANTITUMOR ACTIVITY OF ANTIBODIES AGAINST HEAT SHOCK PROTEINS
Administration of TKD-specific cmHSP70.1 antibodies to mice with CT26 colon cancer promoted the destruction of cancer cells expressing HSP70 on their membranes and the inhibition of tumor growth due to the activation of ADCC, accompanied by infiltration of granulocytes, NK cells and macrophages, as well as by the increase in their migratory and cytolytic activity [17, 72]. According to the authors, other antibodies against HSP70, such as SPA810, Ox7.11 or the Fab fragment of HSP70.1, did not demonstrate a similar antitumor effect. The use of combination therapy based on, for instance, radiochemotherapy that leads to an increase in the surface concentration of HSP70 on cancer cells, and on immunotherapy with cmHSP70.1 mAb can be a promising area for future clinical research.
However, a number of studies on mAbs against HSP70 demonstrated the inhibition of the antitumor activity of NK cells, provided that these antibodies bind the extracellular C-terminus of the chaperone that is necessary for the recognition of HSP70 by NK cells [44, 73]. In this case, immunization by, for example, TKD-peptide seems sensible, as this peptide is able to stimulate the proliferative and cytolytic activity of NK cells. To study the effect of pre-activation of spleen cells for the destruction of mHSP70-positive mouse CT26 carcinoma cells in vitro, a combination of TKD/IL-2 was used, which led to a significant increase in the amount of CD49b+ NK cells and CD25+ cells and promoted tumor cell lysis [72].
Data on the ability of some mAbs against HSP70 to activate cellular cytotoxicity raises the question of the possibility of inducing the complement system for tumor suppression. It is known that extracellular HSP70, being a stress signal, can independently activate the complement system [84]. The same applies to autoantibodies against HSPs in atherosclerosis [85]. BD091 antibodies that recognize the C-terminus of surface HSP70, similar to antibodies formed in atherosclerosis, activated the complement system and cellular toxicity in the presence of low-density lipoproteins, which led to the development of an autoimmune disease and lysis of HSP70-positive rat cells. At the same time, SPA-810 mAbs that recognize a different epitope of HSP70 did not demonstrate a similar effect [85].
7. CONCLUSIONS
Heat shock proteins, which are presented on the surface of tumor cells in some types of cancer, can be a target for the delivery of antitumor drugs. Various carriers, such as nanoparticles and liposomes, can be decorated with antibodies to the membrane-associated HSPs. Small molecule inhibitors that suppress the functional activities of HSPs can be used in combination with cytotoxic drugs, which enhances the action of therapeutic molecules due to the suppression of the chaperone function of HSPs in cancer cells. The use of full-length antibodies against HSPs (including HSP70) or of their fragments is a promising approach for the targeted drug delivery to solid tumors.
Currently, only a limited number of markers for tumors of different localization is used in the clinic. Expanding the range of tumor markers and their combination can be an effective approach for cancer therapy.
DATA AVAILABILITY
The data that support the findings of this study are available from the corresponding author upon reasonable request.
REFERENCES
Fu, Z., Li, S., Han, S., Shi, C., and Zhang, Y., Signal Trans.Target Ther., 2022, vol. 7, p. 93. https://doi.org/10.1038/s41392-022-00947-7
Beck, A., Goetsch, L., Dumontet, C., and Corvaïa, N.,Nat. Rev. Drug. Discov., 2017, vol. 16, pp. 315–337. https://doi.org/10.1038/nrd.2016.268
Richter, K., Haslbeck, M., and Buchner, J., Mol. Cell.,2010, vol. 40, pp. 253–266. https://doi.org/10.1016/j.molcel.2010.10.006
Mertz-Henning, L.M., Pegoraro, C., Maia, L.C.,Venske, E., Rombaldi, C.V., and Costa de Oliveira, A.,Genet. Mol. Res., 2016, vol. 15, Article ID: gmr.15027954. https://doi.org/10.4238/gmr.15027954
Cedraz, H., Gromboni, J.G.G., Garcia, A.A.P. Jr., FariasFilho, R.V., Souza, T.M., Oliveira, E.R., Oliveira, E.B.,Nascimento, C.S.D., Meneghetti, C., and Wenceslau, A.A., PLoS One, 2017, vol. 12, Article ID: e0186083. https://doi.org/10.1371/journal.pone.0186083
Taha, E.A., Ono, K., and Eguchi, T., Int. J. Mol. Sci.,2019, vol. 20, Article ID: 4588. https://doi.org/10.3390/ijms20184588
García Lorenzo, J., León Vintró, X., and Camacho Pérezde Madrid, M., Acta Otorrinolaringol. Esp., 2016, vol. 67,pp. 130–134. https://doi.org/10.1016/j.otorri.2015.03.002
Minnaar, C.A. and Szasz, A., Cells, 2022, vol. 11,Article ID: 1838. https://doi.org/10.3390/cells11111838
Youness, R.A., Gohar, A., Kiriacos, C.J., and El-Shazly, M.,Adv. Exp. Med. Biol., 2023, vol. 1409, pp. 193–203. https://doi.org/10.1007/5584_2022_736
Lianos, G.D., Alexiou, G.A., Mangano, A., Manganho, A.,Rausei, S., Boni, L., Dionigi, G., and Roukos, D.H., Cancer Lett., 2015, vol. 360, pp. 114–118. https://doi.org/10.1016/j.canlet.2015.02.026
Wu, J., Liu, T., Rios, Z., Mei, Q., Lin, X., and Cao, S., Trends Pharmacol. Sci., 2017, vol. 38, pp. 226–256. https://doi.org/10.1016/j.tips.2016.11.009
Yun, C.W., Kim, H.J., Lim, J.H., and Lee, S.H., Cells,2019, vol. 9, Article ID: 60. https://doi.org/10.3390/cells9010060
Fernández-Fernández, M.R., Gragera, M., Ochoa-Ibarrola, L., Quintana-Gallardo, L., and Valpuesta, J.M., FEBS Lett., 2017, vol. 591, pp. 2648–2660. https://doi.org/10.1002/1873-3468.12751
Havalová, H., Ondrovičová, G., Keresztesová, B., Bauer, J.A., Pevala, V., Kutejová, E., and Kunová, N., Int. J. Mol. Sci., 2021, vol. 22, Article ID: 8077. https://doi.org/10.3390/ijms22158077
Stangl, S., Gehrmann, M., Riegger, J., Kuhs, K., Riederer, I., Sievert, W., Hube, K., Mocikat, R., Dressel, R.,Kremmer, E., Pockley, A.G., Friedrich, L., Vigh, L.,Skerra, A., and Multhoff, G., Proc. Natl. Acad. Sci. USA,2011, vol. 108, pp. 733–738. https://doi.org/10.1073/pnas.1016065108
Liu, Q., Liang, C., and Zhou, L., Protein Sci., 2020, vol. 29,pp. 378–390. https://doi.org/10.1002/pro.3725
Fan, W., Fan, S.S., Feng, J., Xiao, D., Fan, S., and Luo, J.,PLoS One, 2017, vol. 12, Article ID: e0185563. https://doi.org/10.1371/journal.pone.0185563
Shiber, A. and Ravid, T., Biomolecules, 2014, vol. 4,pp. 704–724. https://doi.org/10.3390/biom4030704
Werner, C., Stangl, S., Salvermoser, L., Schwab, M., Shevtsov, M., Xanthopoulos, A., Wang, F., Dezfouli, A.B.,Thölke, D., Ostheimer, C., Medenwald, D., Windberg, M.,Bache, M., Schlapschy, M., Skerra, A., and Multhoff, G.,Cancers, 2021, vol. 13, Article ID: 3706. https://doi.org/10.3390/cancers13153706
Zolkiewski, M., Zhang, T., and Nagy, M., Arch. Biochem.Biophys., 2012, vol. 520, pp. 1–6. https://doi.org/10.1016/j.abb.2012.01.012
Wang, X.Y. and Subjeck, J.R., Int. J. Hyperthermia.,2013, vol. 29, pp. 364–375. https://doi.org/10.3109/02656736.2013.803607
Hightower, L.E. and Guidon, P.T. Jr., J. Cell Physiol.,1989, vol. 138, pp. 257–266. https://doi.org/10.1002/jcp.1041380206
Mambula, S.S. and Calderwood, S.K., J. Immunol.,2006, vol. 177, pp. 7849–7857. https://doi.org/10.4049/jimmunol.177.11.7849
Li, D.Y., Liang, S., Wen, J.H., Tang, J.X., Deng, S.L.,and Liu, Y.X., Molecules, 2022, vol. 27, Article ID: 2361. https://doi.org/10.3390/molecules27072361
Broquet, A.H., Thomas, G., Masliah, J., Trugnan, G.,and Bachelet, M., J. Biol. Chem., 2003, vol. 278,pp. 21601–21606. https://doi.org/10.1074/jbc.M302326200
Gehrmann, M., Liebisch, G., Schmitz, G., Anderson, R., Steinem, C., De Maio, A., Pockley, G., and Multhoff, G.,PLoS One, 2008, vol. 3, Article ID: e1925. https://doi.org/10.1371/journal.pone.0001925
Bilog, A.D., Smulders, L., Oliverio, R., Labanieh, C., Zapanta, J., Stahelin, R.V., and Nikolaidis, N., Biomolecules,2019, vol. 9, Article ID: 152. https://doi.org/10.3390/biom9040152
Pomorski, T., Holthuis, J.C., Herrmann, A., and vanMeer, G., J. Cell Sci., 2004, vol. 117, pp. 805–813. https://doi.org/10.1242/jcs.01055
Schilling, D., Gehrmann, M., Steinem, C., De Maio, A., Pockley, A.G., Abend, M., Molls, M., and Multhoff, G., FASEB J., 2009, vol. 23, pp. 2467–2477. https://doi.org/10.1096/fj.08-125229
Shevtsov, M.A., Komarova, E.Y., Meshalkina, D.A.,Bychkova, N.V., Aksenov, N.D., Abkin, S.V., Margulis, B.A., and Guzhova, I.V., Oncotarget., 2014, vol. 5,pp. 3101–3114. https://doi.org/10.18632/oncotarget.1820
Benaroudj, N., Ebel, C., and Ladjimi, M.M., Eur. J. Biochem., 1999, vol. 259, pp. 379–384. https://doi.org/10.1046/j.1432-1327.1999.00053.x
Rafiee, M., Kanwar, J.R., Berg, R.W., Lehnert, K.,Lisowska, K., Krissansen, G.W., Cancer Gene Ther.,2001, vol. 8, pp. 974–981. https://doi.org/10.1038/sj.cgt.7700395
Bethke, K., Staib, F., Distler, M., Schmitt, U., Jonuleit, H.,Enk, A.H., Galle, P.R., and Heike, M., J. Immunol., 2002,vol. 169, pp. 6141–6148. https://doi.org/10.4049/jimmunol.169.11.6141
Luo, H., Yang, H., Lin, Y., Zhang, Y., Pan, C., Feng, P.,Yu, Y., and Chen, X., Oncotarget., 2017, vol. 8, pp. 98455–98470. https://doi.org/10.18632/oncotarget.21427
Yurinskaya, M.M., Kochetkova, O.Y., Shabarchina, L.I., Antonova, O.Y., Suslikov, A.V., Evgen’ev, M.B., and Vinokurov, M.G., Cell Stress Chaperones, 2017, vol. 22,pp. 163–171. https://doi.org/10.1007/s12192-016-0743-z
Evgen’ev, M.B., Cell Stress Chaperones, 2021, vol. 26,pp. 617–627. https://doi.org/10.1007/s12192-021-01219-z
Komarova, E.Y., Marchenko, L.V., Zhakhov, A.V., Nikotina, A.D., Aksenov, N.D., Suezov, R.V., Ischenko, A.M., Margulis, B.A., and Guzhova, I.V., Int. J. Mol. Sci., 2019, vol. 21, pp. 59–77. https://doi.org/10.3390/ijms21010059
Shevtsov, M.A., Pozdnyakov, A.V., Mikhrina, A.L.,Yakovleva, L.Y., Nikolaev, B.P., Dobrodumov, A.V.,Meshalkina, D.A., Ischenko, A.M., Pitkin, E., Guzhova, I.V., and Margulis, B.A., Int. J. Cancer, 2014,vol. 135, pp. 2118–2128. https://doi.org/10.1002/ijc.28858
Lobinger, D., Gempt, J., Sievert, W., Barz, M., Schmitt, S.,Nguyen, H.T., Stangl, S., Werner, C., Wang, F., Wu, Z., Fan, H., Zanth, H., Shevtsov, M., Pilz, M., Riederer, I., Schwab, M., Schlegel, J., and Multhoff, G., Front. Mol.Biosci., 2021, vol. 8, Article ID: 669366. https://doi.org/10.3389/fmolb.2021.669366
Krause, S.W., Gastpar, R., Andreesen, R., Gross, C., Ullrich, H., Thonigs, G., Pfister, K., and Multhoff, G.,Clin. Cancer Res., 2004, vol. 10, pp. 3699–3707. https://doi.org/10.1158/1078-0432.CCR-03-0683
Kaczmarek, M., Lagiedo, M., Masztalerz, A., Kozlowska, M., Nowicka, A., Brajer, B., Batura-Gabryel, H., andSikora, J., Immunobiology, 2018, vol. 223, pp. 200–209. https://doi.org/10.1016/j.imbio.2017.10.025
Tukaj, S. and Sitko, K., Biomolecules, 2022, vol. 12,Article ID: 1153. https://doi.org/10.3390/biom12081153
Wachstein, J., Tischer, S., Figueiredo, C., Limbourg, A.,Falk, C., Immenschuh, S., Blasczyk, R., and Eiz-Vesper, B., PLoS One, 2012, vol. 7, Article ID: e51747. https://doi.org/10.1371/journal.pone.0051747
Botzler, C., Li, G., Issels, R.D., and Multhoff, G., Cell StressChaperones, 1998, vol. 3, pp. 6–11. https://doi.org/10.1379/1466-1268(1998)003<0006:doeleo>2.3.co;2
Affatigato, L., Licciardi, M., Bonamore, A., Martorana, A.,Incocciati, A., Boffi, A., and Militello, V., Molecules, 2023,vol. 28, Article ID: 1163. https://doi.org/10.3390/molecules28031163
Shevtsov, M., Huile, G., and Multhoff, G., Philos. Trans. R Soc. Lond. B Biol. Sci., 2018, vol. 373, Article ID:20160526. https://doi.org/10.1098/rstb.2016.0526
Shevtsov, M.A., Nikolaev, B.P., Ryzhov, V.A., Yakovleva, L.Y., Marchenko, Y.Y., Parr, M.A., Rolich, V.I.,Mikhrina, A.L., Dobrodumov, A.V., Pitkin, E., andMulthoff, G., Nanoscale, 2015, vol. 7, pp. 20652–20664. https://doi.org/10.1039/c5nr06521f
Shaterabadi, Z., Nabiyouni, G., and Soleymani, M.,Prog. Biophys. Mol. Biol., 2018, vol. 133, pp. 9–19. https://doi.org/10.1016/j.pbiomolbio.2017.10.001
Johannsen, M., Thiesen, B., Wust, P., and Jordan, A.,Int. J. Hyperthermia, 2010, vol. 26, pp. 790–795. https://doi.org/10.3109/02656731003745740
Maier-Hauff, K., Ulrich, F., Nestler, D., Niehoff, H.,Wust, P., Thiesen, B., Orawa, H., Budach, V., and Jordan, A., J. Neurooncol., 2011, vol. 103, pp. 317–324. https://doi.org/10.1007/s11060-010-0389-0
Ruan, S., Yuan, M., Zhang, L., Hu, G., Chen, J., Cun, X.,Zhang, Q., Yang, Y., He, Q., and Gao, H., Biomaterials,2015, vol. 37, pp. 425–435. https://doi.org/10.1016/j.biomaterials.2014.10.007
Ruan, S., He, Q., and Gao, H., Nanoscale, 2015, vol. 7,pp. 9487–9496. https://doi.org/10.1039/c5nr01408e
Gehrmann, M.K., Kimm, M.A., Stangl, S., Schmid, T.E., Noël, P.B., Rummeny, E.J., and Multhoff, G., Int. J. Nanomedicine, 2015, vol. 10, pp. 5687–5700. https://doi.org/10.2147/IJN.S87174
Zheng, Y., Hunting, D.J., Ayotte, P., and Sanche, L., Radiat. Res., 2008, vol. 169, pp. 19–27. https://doi.org/10.1667/RR1080.1
Schuemann, J., Berbeco, R.I., Chithrani, D.B., Cho, S.H.,Kumar, R.R., McMahon, S.J., Sridhar, S., and Krishnan, S., Int. J. Radiat. Oncol. Biol. Phys., 2016, vol. 94,pp. 189–205. https://doi.org/10.1016/j.ijrobp.2015.09.032
Ali, M.R., Ali, H.R., Rankin, C.R., and El-Sayed, M.A.,Biomaterials, 2016, vol. 102, pp. 1–8. https://doi.org/10.1016/j.biomaterials.2016.06.017
Gehrmann, M., Stangl, S., Foulds, G.A., Oellinger, R., Breuninger, S., Rad, R., Pockley, A.G., and Multhoff, G., PLoS One, 2014, vol. 9, Article ID: 105344. https://doi.org/10.1371/journal.pone.0105344
Poccia, F., Piselli, P., Di Cesare, S., Bach, S., Colizzi, V.,Mattei, M., Bolognesi, A., and Stirpe, F., Br. J. Cancer,1992, vol. 66, pp. 427–432. https://doi.org/10.1038/bjc.1992.291
Dezfouli, A.B., Stangl, S., Foulds, G.A., Lennartz, P., Pilkington, G.J., Pockley, A.G., and Multhoff, G., MethodsMol. Biol., 2023, vol. 2693, pp. 307–324. https://doi.org/10.1007/978-1-0716-3342-7_23
Madamsetty, V.S., Mukherjee, A., and Mukherjee, S., Front. Pharmacol., 2019, vol. 10, Article ID: 1264. https://doi.org/10.3389/fphar.2019.01264
Slingerland, M., Guchelaar, H.J., and Gelderblom, H.,Drug Discov. Today, 2012, vol. 17, pp. 160–166. https://doi.org/10.1016/j.drudis.2011.09.015f
Lu, R.M., Chen, M.S., Chang, D.K., Chiu, C.Y.,Lin, W.C., Yan, S.L., Wang, Y.P., Kuo, Y.S., Yeh, C.Y.,Lo, A., and Wu, H.C., PLoS One, 2013, vol. 8, Article ID:e66128. https://doi.org/10.1371/journal.pone.0066128
Wilhelm, S., Tavares, A.J., Dai, Q., Ohta, S., Audet, J.,Dvorak, H.F., Chan, C.W., Nat. Rev. Mater., 2016, vol. 1,Article ID: e16014. https://doi.org/10.1038/natrevmats.2016.14
Alswieleh, A.M., J. Chem., 2020, vol. 2020, Article ID:e9176257. https://doi.org/10.1155/2020/9176257
Hassanpour, A., Irandoust, M., Soleimani, E., and Zhaleh, H., Mat. Sci. Eng. C Mater. Biol. Appl., 2019,vol. 103, Article ID: 109771. https://doi.org/10.1016/j.msec.2019.109771
Lu, S., Neoh, K.G., Huang, C., Shi, Z., and Kang, E.T.,J. Colloid Interface Sci., 2013, vol. 412, pp. 46–55. https://doi.org/10.1016/j.jcis.2013.09.011
Shevtsov, M., Zhou, Y., Khachatryan, W., Multhoff, G.,and Gao, H., Curr. Drug Metab., 2018, vol. 19, pp. 768–780. https://doi.org/10.2174/1389200219666180611080736
Genc, S., Taghizadehghalehjoughi, A., Yeni, Y., Jafarizad, A., Hacimuftuoglu, A., Nikitovic, D., Docea, A.O.,Mezhuev, Y., and Tsatsakis, A., Pharmaceutics, 2023,vol. 15, Article ID: 245. https://doi.org/10.3390/pharmaceutics15010245
Sparreboom, A., Scripture, C.D., Trieu, V., Williams, P.J.,De, T., Yang, A., Beals, B., Figg, W.D., Hawkins, M.,and Desai, N., Clin. Cancer Res., 2005, vol. 11, pp. 4136–4143. https://doi.org/10.1158/1078-0432.CCR-04-2291
Svenson, S., Chem. Soc. Rev., 2015, vol. 44, pp. 4131–4144. https://doi.org/10.1039/c5cs00288e
Caminade, A.M., J. Pers. Med., 2022, vol. 12, Article ID:1334. https://doi.org/10.3390/jpm12081334
Stangl, S., Gehrmann, M., Dressel, R., Alves, F., Dullin, C., Themelis, G., Ntziachristos, V., Staeblein, E., Walch, A., Winkelmann, I., and Multhoff, G., J. Cell Mol. Med., 2011, vol. 15, pp. 874–887. https://doi.org/10.1111/j.1582-4934.2010.01067.x
Multhoff, G., Pfister, K., Gehrmann, M., Hantschel, M., Gross, C., Hafner, M., and Hiddemann, W.A., Cell Stress Chaperones, 2001, vol. 6, pp. 337–344. https://doi.org/10.1379/1466-1268(2001)006<0337:AMHPSN>2.0.CO;2
Taglia, L., Matusiak, D., and Benya, R.V., Clin. Exp. Metastasis., 2008, vol. 25, pp. 451–463. https://doi.org/10.1007/s10585-008-9151-9
Gobbo, J., Marcion, G., Cordonnier, M., Dias, A.M.M., Pernet, N., Hammann, A., Richaud, S., Mjahed, H., Isambert, N., Clausse, V., Rébé, C., Bertaut, A., Goussot, V.,Lirussi, F., Ghiringhelli, F., de Thonel, A., Fumoleau, P.,Seigneuric, R., and Garrido, C., J. Natl. Cancer Inst.,2015, vol. 108. Article ID: djv330. https://doi.org/10.1093/jnci/djv330
Schmitt, E., Maingret, L., Puig, P.E., Rerole, A.L.,Ghiringhelli, F., Hammann, A., Solary, E., Kroemer, G.,and Garrido, C., Cancer Res., 2006, vol. 66, pp. 4191–4197. https://doi.org/10.1158/0008-5472.CAN-05-3778
McKeon, A.M., Egan, A., Chandanshive, J., McMahon, H., and Griffith, D.M., Molecules, 2016, vol. 21,Article ID: 949. https://doi.org/10.3390/molecules21070949
Adam, C., Baeurle, A., Brodsky, J.L., Wipf, P., Schrama, D., Becker, J.C., and Houben, R., PLoS One, 2014,vol. 9, Article ID: e92041. https://doi.org/10.1371/journal.pone.0092041
Prince, T., Ackerman, A., Cavanaugh, A., Schreiter, B.,Juengst, B., Andolino, C., Danella, J., Chernin, M., andWilliams, H., Oncotarget., 2018, vol. 9, pp. 32702–32717. https://doi.org/10.18632/oncotarget.26021
Li, X., Srinivasan, S.R., Connarn, J., Ahmad, A., Young, Z.T., Kabza, A.M., Zuiderweg, E.R.P., Sun, D., and Gestwicki, J.E., ACS Med. Chem. Lett., 2013, vol. 4,pp. 1042–1047. https://doi.org/10.1021/ml400204n
Wadhwa, R., Sugihara, T., Yoshida, A., Nomura, H., Reddel, R.R., Simpson, R., Maruta, H., and Kaul, S.C., Cancer Res., 2000, vol. 60, pp. 6818–6821.
Koya, K., Li, Y., Wang, H., Ukai, T., Tatsuda, N., Kawakami, M., Shishido, T., and Chen, L.B., Cancer Res.,1996,vol. 56, pp. 538–543.
Modica-Napolitano, J.S., Koya, K., Weisberg, E., Brunelli, B.T., Li, Y., and Chen, L.B., Cancer Res., 1996, vol. 56,pp. 544–550.
Schett, G., Xu, Q., Amberger, A., Van der Zee, R., Recheis, H., Willeit, J., and Wick, G., J. Clin. Invest., 1995,vol. 96, pp. 2569–2577. https://doi.org/10.1172/JCI118320
Leng, X., Wang, X., Pang, W., Zhan, R., Zhang, Z.,Wang, L., Gao, X., and Qian, L., Cell Stress Chaperones,2013, vol. 18, pp. 483–493. https://doi.org/10.1007/s12192-013-0404-4
Funding
This work supported by the Russian Scientific Foundation (project no. 23-15-00472).
Author information
Authors and Affiliations
Contributions
All authors made an equal contribution to the writing of this article.
Corresponding author
Ethics declarations
This article does not contain any studies involving patients or animals as test objects.
Informed consent was not required for this article. No conflict of interest was declared by the authors.
Additional information
Publisher's Note. Pleiades Publishing remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Abbreviations: HSP, heat shock protein; NK, natural killers; Treg, regulatory T-cells; IL, interleukin; mAb, monoclonal antibodies; CD, cluster of differentiation; CTLA4, cytotoxic T-lymphocyte-associated protein 4; HER2, human epidermal growth factor receptor 2; PS, phosphatidylserine; BCMA, B-cell maturation antigen; NPs, nanoparticles; AuNPs, gold nanoparticles; AMF, alternating magnetic field; PPTT, plasmonic photothermal therapy; AIF, apoptosis-inducing factor; ADD70 (150–228), AIF peptide that recognizes HSP70; ADCC, antibody-dependent cellular cytotoxicity.
Rights and permissions
Open Access. This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Makarova, A.O., Kostenko, V.V., Ovsyanikova, O.V. et al. Heat Shock Proteins on Tumor Cell Surface as Target for Anti-Tumor Therapy (A Review). Russ J Bioorg Chem 50, 644–656 (2024). https://doi.org/10.1134/S1068162024030038
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S1068162024030038