Abstract
We provide a comprehensive overview of the typical decisions to be made in resource capacity planning and control in health care, and a structured review of relevant articles from the field of Operations Research and Management Sciences (OR/MS) for each planning decision. The contribution of this paper is twofold. First, to position the planning decisions, a taxonomy is presented. This taxonomy provides health care managers and OR/MS researchers with a method to identify, break down and classify planning and control decisions. Second, following the taxonomy, for six health care services, we provide an exhaustive specification of planning and control decisions in resource capacity planning and control. For each planning and control decision, we structurally review the key OR/MS articles and the OR/MS methods and techniques that are applied in the literature to support decision making.
Similar content being viewed by others
1. Introduction
Health care professionals face the challenging task to organize their processes more effectively and efficiently. The pressure on health care systems rises as both demand for health care and expenditures are increasing steadily [329]. Within a health care organization, professionals of different functions jointly organize health care delivery with the objective to provide high-quality care using the limited resources that are available [56]. Designing and organizing processes is known as planning and control, which involves setting goals and deciding in advance what to do, how to do it, when to do it and who should do it. Health care planning and control comprises multiple managerial functions, making medical, financial and resource decisions. In this paper we address the managerial function of resource capacity planning and control as defined in [200]: ‘Resource capacity planning and control addresses the dimensioning, planning, scheduling, monitoring, and control of renewable resources’.
Operations Research and Management Sciences (OR/MS) is an interdisciplinary branch of applied mathematics, engineering and sciences that uses various scientific research-based principles, strategies, and analytical methods including mathematical modeling, statistics and algorithms to improve an organization's ability to enact rational and meaningful management decisions [228]. OR/MS has been applied widely to resource capacity planning and control in manufacturing. Since the 1950s, the application of OR/MS to health care also yields significant contributions in accomplishing essential efficiency gains in health care delivery. Many different topics have been addressed, such as operating room planning, nurse staffing and appointment scheduling. Owing to the interdisciplinary nature of OR/MS applied to health care, there is an extensive base of literature published across various academic fields. Tailored reference databases prove to be valuable in retrieving references from this broad availability. For example, Dexter provides a comprehensive bibliography on operating room management [111]. The Center for Healthcare Operations Improvement and Research (CHOIR) of the University of Twente has introduced and maintains the online literature database ‘ORchestra’ [ 226, 328], in which references in the field of OR/MS in health care are categorized by medical and mathematical subject. All the articles mentioned in this review are included and categorized in ORchestra.
Contribution
We aim to guide health care professionals and OR/MS researchers through the broad field of OR/MS in health care. We provide a structured overview of the typical decisions to be made in resource capacity planning and control in health care, and provide a review of relevant OR/MS articles for each planning decision.
The contribution of this paper is twofold. First, to position the planning decisions, we present a taxonomy. This taxonomy provides health care managers and OR/MS researchers with a method to identify, break down and classify planning and control decisions. The taxonomy contains two axes. The vertical axis reflects the hierarchical nature of decision making in resource capacity planning and control, and the horizontal axis the various health care services. The vertical axis is strongly connected, because higher-level decisions demarcate the scope of and impose restrictions on lower-level decisions. Although health care delivery is generally organized in autonomous organizations and departments, the horizontal axis is also strongly interrelated as a patient pathway often consists of several health care services from multiple organizations or departments.
Second, following the vertical axis of the taxonomy, and for each health care service on the horizontal axis, we provide a comprehensive specification of planning and control decisions in resource capacity planning and control. For each planning and control decision, we structurally review the key OR/MS articles and the OR/MS methods and techniques that are applied in the literature to support decision making. No structured review exists of this nature, as existing reviews are typically exhaustive within a confined scope, such as simulation modeling in health care [240] or outpatient appointment scheduling [76], or are more general to the extent that they do not focus on the concrete specific decisions.
This paper is organized as follows. Section 2 presents our taxonomy, Section 3 identifies, classifies and discusses the planning and control decisions. Section 4 concludes this paper with a discussion of our findings.
2. Taxonomy
Taxonomy is the practice and science of classification. It originates from biology where it refers to a hierarchical classification of organisms. The National Biological Information Infrastructure [318] provides the following definition of taxonomy: “Taxonomy is the science of classification according to a pre-determined system, with the resulting catalog used to provide a conceptual framework for discussion, analysis, or information retrieval; … a good taxonomy should be simple, easy to remember, and easy to use”. With exactly these objectives, we present a taxonomy for resource capacity planning and control in health care.
Planning and control decisions are made by health care organizations to design and operate the health care delivery process. It requires coordinated long-term, medium-term and short-term decision making in multiple managerial areas. In Hans et al [200], a framework is presented to subdivide these decisions in four hierarchical, or temporal, levels and four managerial areas. These hierarchical levels and the managerial area of resource capacity planning and control form the basis for our taxonomy. For the hierarchical levels, [200] applies the well-known breakdown of strategic, tactical and operational [9]. In addition, the operational level is subdivided in offline and online decision making, where offline reflects the in advance decision making and online the real-time reactive decision making in response to events that cannot be planned in advance. The four managerial areas are: medical planning, financial planning, materials planning and resource capacity planning. These are defined as follows. Medical planning comprises decision making by clinicians regarding medical protocols, treatments, diagnoses and triage. Financial planning addresses how an organization should manage its costs and revenues to achieve its objectives under current and future organizational and economic circumstances. Materials planning addresses the acquisition, storage, distribution and retrieval of all consumable resources/materials, such as suture materials, blood, bandages, food, etc. Resource capacity planning addresses the dimensioning, planning, scheduling, monitoring and control of renewable resources. Our taxonomy is a refinement of the health care planning and control framework of [200] in the resource capacity planning area.
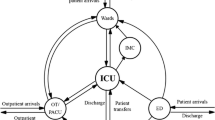
The taxonomy contains two axes. The vertical axis reflects the hierarchical nature of decision making in resource capacity planning and control, and is derived from [200]. On the horizontal axis of our taxonomy we position different services in health care. We identify ambulatory care services, emergency care services, surgical care services, inpatient care services, home care services and residential care services. The taxonomy is displayed in Figure 1. We elaborate on both axes in more detail below.
Vertical axis
Our taxonomy is intended for planning and control decisions within the boundaries of a health care delivery organization. Every health care organization operates in a particular external environment. Therefore, all planning and control decisions are made in the context of this external environment. The external environment is characterized by factors such as legislation, technology and social factors.
The nature of planning and control decision making is such that decisions disaggregate as time progresses and more information becomes available [460]. Aggregate decisions are made in an early stage, while more detailed information supports decision making with a finer granularity in later stages. Because of this disaggregating nature, most well-known taxonomies and frameworks for planning and control are organized hierarchically [ 200, 460]. As the impact of decisions decreases when the level of detail increases, such a hierarchy also reflects the top-down management structure of most organizations [39].
For completeness we explicitly state the definitions of the four hierarchical levels [200], which we position on the vertical axis of our taxonomy. The definitions are adapted to specifically fit the managerial area of resource capacity planning and control.
-
Strategic planning addresses structural decision making. It involves defining the organization's mission (i.e., ‘strategy’ or ‘direction’), and the decision making to translate this mission into the design, dimensioning and development of the health care delivery process. Inherently, strategic planning has a long planning horizon and is based on highly aggregated information and forecasts. Examples of strategic planning are determining the facility's location, dimensioning resource capacities (e.g., acquisition of an MRI scanner, staffing) and deciding on the service and case mix.
-
Tactical planning translates strategic planning decisions to guidelines that facilitate operational planning decisions. While strategic planning addresses structural decision making, tactical planning addresses the organization of the operations/execution of the health care delivery process (i.e., the ‘what, where, how, when and who’). As a first step in tactical planning, patient groups are characterized based on disease type/diagnose, urgency and resource requirements. As a second step, the available resource capacities, settled at the strategic level, are divided among these patient groups. In addition to the allocation in time quantities, more specific timing information can already be added, such as dates or time slots. In this way, blueprints for the operational planning are created that allocate resources to different tasks, specialties and patient groups. Temporary capacity expansions like overtime or hiring staff are also part of tactical planning. Demand has to be (partly) forecasted, based on (seasonal) demand, waiting list information, and the ‘downstream’ demand in care pathways of patients currently under treatment. Examples of tactical planning are staff-shift scheduling and the (cyclic) surgical block schedule that allocates operating time capacity to patient groups.
-
Operational planning (both ‘offline’ and ‘online’) involves the short-term decision making related to the execution of the health care delivery process. Following the tactical blueprints, execution plans are designed at the individual patient level and the individual resource level. In operational planning, elective demand is entirely known and only emergency demand has to be forecasted. In general, the capacity planning flexibility is low on this level, since decisions on higher levels have demarcated the scope for the operational level decision making.
-
Offline operational planning reflects the in advance planning of operations. It comprises the detailed coordination of the activities regarding current (elective) demand. Examples of offline operational planning are patient-to-appointment assignment, staff-to-shift assignment and surgical case scheduling.
-
Online operational planning reflects the control mechanisms that deal with monitoring the process and reacting to unplanned events. This is required due to the inherent uncertain nature of health care processes. An example of online operational planning is the real-time dynamic (re)scheduling of elective patients when an emergency patient requires immediate attention.
Note that the decision horizon lengths are not explicitly given for any of the hierarchical planning levels, since these depend on the specific characteristics of the application. For example, an emergency department inherently has shorter planning horizons than a long-stay ward in a nursing home. Furthermore, there is a strong interrelation between hierarchical levels. Top-down interaction exists as higher-level decisions demarcate the scope of and impose restrictions on lower-level decisions. Conversely, bottom-up interaction exists as feedback about the health care delivery realization supports decision making in higher levels.
Horizontal axis
On the horizontal axis of our taxonomy we position the different services in health care. The complete spectrum of health care delivery is a composition of many different services provided by many different organizations. From the perspective of resource capacity planning and control, different services may face similar questions. To capture this similarity, we distinguish six clusters of health-care services. The definitions of the six care services are obtained from the corresponding MeSH terms provided by PubMed [310]. For each care service we offer several examples of facilities that provide this service.
-
Ambulatory care services provide care to patients without offering a room, a bed and board, and they may be free-standing or part of a hospital. In ambulatory care services, we position primary care services and community services as well as hospital-based services such as the outpatient clinic, since these services face similar questions from a resource capacity planning perspective. Examples of ambulatory care facilities are outpatient clinics, primary care services and the hospital departments of endoscopy, radiology and radiotherapy.
-
Emergency care services are concerned with the evaluation and initial treatment of urgent and emergent medical problems, such as those caused by accidents, trauma, sudden illness, poisoning or disasters. Emergency medical care can be provided at the hospital or at sites outside the medical facility. Examples of emergency care facilities are hospital emergency departments, ambulances and trauma centers.
-
Surgical care services provide operative procedures (surgeries) for the correction of deformities and defects, repair of injuries, and diagnosis and cure of certain diseases. Examples of surgical care facilities are the hospital's operating theater, surgical daycare centers and anesthesia facilities.
-
Inpatient care services provide care to hospitalized patients by offering a room, a bed and board. Examples are intensive care units, general nursing wards and neonatal care units.
-
Home care services are community health and nursing services that provide multiple, coordinated services to a patient at the patient's home. Home care services are provided by a visiting nurse, home health agencies, hospitals or organized community groups using professional staff for health care delivery. Examples are medical care at home, housekeeping support and personal hygiene assistance.
-
Residential care services provide supervision and assistance in activities of daily living with medical and nursing services when required. Examples are nursing homes, psychiatric hospitals, rehabilitation clinics with overnight stay, homes for the aged, and hospices.
Note that the horizontal subdivision is not based on health care organizations, but on the provided care services. Therefore, it is possible that a single health care organization offers services in multiple clusters. It may be that a particular facility is used by multiple care services, for example a diagnostics department that is used in both ambulatory and emergency care services. In addition, a patient's treatment often comprises of consecutive care stages offered by multiple care services. The health care delivery realization within one care service is impacted by decisions in other services, as inflow and throughput strongly depend on these other services. Therefore, resource capacity planning and control decisions are always made in the context of decisions made for other care services. Hence, like the interrelation in the vertical levels, a strong interrelation exists between the horizontal clusters.
This taxonomy provides a method to identify, break down and classify planning and control decisions in health care. This is a starting point for a complete specification of planning decisions and helps to gain understanding of the interrelations between various planning decisions. Hence, health care professionals can identify lacking, insufficiently defined and incoherent planning decisions within their department or organization. It also gives the opportunity to identify planning decisions that are not yet addressed often in the OR/MS literature. Therefore, in the next section, with our taxonomy as the foundation, we provide an exhaustive specification of planning decisions for each care service, combined with a review of key OR/MS literature.
3. Identification and classification of planning and control decisions
In this section, we identify the resource capacity planning and control decisions for each of the six care services in our taxonomy. The decisions are classified according to the vertical hierarchical structure of our taxonomy. For each identified planning decision, we will discuss the following in our overview:
-
What is the concrete decision?
-
Which performance measures are considered?
-
What are the key trade-offs?
-
What are main insights and results from the literature?
-
What are general conclusions?
-
Which OR/MS methods are applied to support decision making?
The identified planning decisions are in the first place obtained from available books and articles on health care planning and control. Our literature search method will be explained in more detail below. In addition, to be as complete as possible, expert opinions from health care professionals and OR/MS specialists are obtained to identify decisions that are not yet well-addressed in the literature and for this reason cannot be obtained from the literature. In this introduction, we first discuss the scope of the identified planning decisions and the applied OR/MS methods, and next we present the applied literature search method.
Scope
Numerous processes are involved in health care delivery. We focus on the resource capacity planning and control decisions to be made regarding the primary process of health care delivery. In the management literature, the primary process is defined as the set of activities that are directly concerned with the creation or delivery of a product or service [343]. Thus, we do not focus on supporting activities, such as procurement, information technology, human resource management, laboratory services, blood services and instrument sterilization.
We focus on OR/MS methods that quantitatively support and rationalize decision making in resource capacity planning and control. Based on forecasting of demand for care (see [330] for forecasting techniques), these methods provide optimization techniques for the design of the health care delivery process. Outside our scope is statistical comparison of performance of health care organizations, so-called benchmarking, of which Data Envelopment Analysis (DEA) and Stochastic Frontier Analysis (SFA) are well-known examples [91]. Quantitative decision making requires measurable performance indicators by which the quality of health care delivery can be expressed. A comprehensive survey of applied performance measures in health care organizations is provided in [277]. Next, practical implementation of OR/MS methods may require the development of Information Communications Technology (ICT) solutions (that are possibly integrated in health care organizations’ database systems); this is also outside the scope of this paper.
The spectrum of different OR/MS methods is wide (see for example [ 218, 394, 406, 448] for introductory books). In this review, we distinguish the following OR/MS methods: computer simulation [272], heuristics [1], Markov processes (which includes Markov reward and decision processes) [406], mathematical programming [ 331, 371], queueing theory [363]. For a short description of each of these OR/MS methods, the reader is referred to Appendix A.
Literature search method
As the body of literature on resource capacity planning and control in health care is extensive, we used a structured search method and we restricted to articles published in ISI-listed journals to ensure that we found and filter key and state-of-the-art contributions. Table 1 displays our search method. To identify the search terms as listed in Appendix B and to create the basic structure of the planning decision hierarchy for each care service, we consulted available literature reviews [ 45, 53, 55, 65, 72, 76, 84, 141, 156, 157, 192, 196, 197, 233, 240, 244, 246, 259, 287, 301, 311, 316, 336, 342, 345, 350, 353, 385, 386, 411, 422] and books [ 56, 199, 267, 309, 330, 433]. Additional search terms were obtained from the index of Medical Subject Headings (MeSH) [310] and available synonyms. With these search terms, we performed a search on the database of Web of Science (WoS) [440]. WoS was chosen as it contains articles from all ISI-listed journals. It is particularly useful as it provides the possibility to select Operations Research and Management Science as a specific subject category and to sort references on the number of citations.
We identify a base set containing the 10 most-cited articles in the predefined subject category of Operations Research and Management Science. Starting from this base set, we include all articles from ISI-listed journals that are referred by or refer to one of the articles in the base set and deal with resource capacity planning and control decisions. As such, we ensure that we also review recent work that may not have been cited often yet. In addition, we include articles published in Health Care Management Science (HCMS), which is particularly relevant for OR/MS in health care and obtained an ISI listing in 2010. To be sure that by restricting to WoS and HCMS, we do not neglect essential references, we also performed a search with our search terms on the databases of Business Source Elite [135], PubMed [346] and Scopus [372]. This search did not result in significant additions to the already found set of papers. The literature search was updated up to 10 May 2012.
The review is organized as follows. Section 3.1 is devoted to ambulatory care services, the Section 3.2 to emergency care services, Section 3.3 to surgical care services, Section 3.4 to inpatient care services, Section 3.5 to home care services and Section 3.6 to residential care services. For each care service, the review is subdivided in strategic, tactical, offline operational and online operational planning. In Appendix C, tables are included in which the identified planning decisions are listed for each care service, together with applied OR/MS methods and literature references per planning decision. When for different care services a similar planning decision is involved, we use the same term. Our intention is that all the following sub-sections are self-contained, so that they can be read in isolation. Therefore, minor passages are overlapping. When in the description of a planning decision a paper is cited, while it does not appear in the ‘methods’-list, it means that this paper contains a relevant statement about this planning decision, but the particular planning decision is not the main focus of the paper.
3.1. Ambulatory care services
Ambulatory care services provide medical interventions without overnight stay, that is, the patient arrives at the facility and leaves the facility on the same day. These medical interventions comprise for example diagnostic services (e.g., CT scan, MRI scan), doctor consultations (e.g., general practitioner, hospital specialist), radiotherapy treatments or minor surgical interventions. Demand for ambulatory care services is growing in most western countries since 2000 [324]. The existing literature has mainly focused on the offline operational planning decision of appointment scheduling.
Strategic planning
Regional coverage
Ambulatory care planning on a regional level aims to create the infrastructure to provide health care to the population in its catchment area. This regional coverage decision involves determining the number, size and location of facilities in a certain region to find a balanced distribution of facilities with respect to the geographical location of demand [130]. The main trade-off in this decision is between patient accessibility and efficiency. Patient accessibility is represented by access time and travel distance indicators. Efficiency is represented by utilization and productivity indicators [ 130, 385]. Common regional planning models incorporate the dependency of demand on the regional demographic and socioeconomic characteristics [2].
Methods: computer simulation [ 298, 359, 388, 404], heuristics [ 2, 130], literature review [385].
Service mix
An organization decides the particular services that the ambulatory care facility provides. The service mix stipulates which patient types can be consulted. In general, the service mix decision is not made at an ambulatory care service level, but at the regional or hospital level, as it integrally impacts the ambulatory, emergency, surgical and inpatient care services. This is also expressed in the literature, in which for example inpatient resources, such as beds and nursing staff, are indicated as ‘following’ resources [431]. This may be the reason that we have not found any references focusing on service mix decisions for ambulatory care services in specific.
Methods: no papers found.
Case mix
Every ambulatory care facility decides on a particular case mix, which is the volume and composition of patient groups that the facility serves. The settled service mix restricts the decisions to serve particular patient groups. Patient groups can be classified based on disease type, age, acuteness, home address, etc. The case mix influences almost all other planning decisions, such as a facility's location, capacity dimensions and layout. Also, demand for different patient groups in the case mix may vary, which influences required staffing levels significantly [ 384, 392]. However, case mix decision making has not received much attention in the OR/MS literature. In the literature, the case mix is often treated as given.
Methods: computer simulation [392], mathematical programming [384].
Panel size
The panel size is the number of potential patients of an ambulatory care facility [187]. Since only a fraction of these potential patients, also called calling population, actually demands health care, the panel size can be larger than the number of patients a facility can serve. The panel size is particularly important for general practitioners, as they need an accurate approximation of how many patients they can subscribe or admit to their practice. A panel size should be large enough to have enough demand to be profitable and to benefit from economies of scale, as a facility's costs per patient decrease when the panel size increases [388]. On the other hand, when the panel size is too large, access times may grow exponentially [187].
Methods: computer simulation [388], queueing theory [187].
Capacity dimensioning
Ambulatory care facilities dimension their resources, such as staff, equipment and space, with the objective to (simultaneously) maximize clinic profit, patient satisfaction and staff satisfaction [392]. To this end, provider capacity must be matched with patient demand, such that performance measures such as costs, access time and waiting time are controlled. Capacity is dimensioned for the following resource types:
-
Consultation rooms. The number of consultation rooms that balances patient waiting times and doctor idle time with costs for consultation rooms [ 227, 385, 391, 392].
-
Staff. Staff in the ambulatory care services concern for example doctors, nurses and assistants [ 32, 240, 298, 360, 384, 385, 388, 391, 392, 438, 444].
-
Consultation time capacity. The total consultation time that is available, for example for an MRI scanner or a doctor [ 98, 136, 138].
-
Equipment. Some ambulatory care services require equipment for particular consultations, for example MRI scanners, CT scanners and radiotherapy machines [ 161, 298, 404].
-
Waiting room. The waiting room is dimensioned such that patients and their companions waiting for consultation can be accommodated [392].
When capacity is dimensioned to cover average demand, variations in demand may cause long access and waiting times [404]. Basic rules from queueing theory demonstrate the necessity of excess capacity to cope with uncertain demand [182]. Capacity dimensioning is a key decision, as it influences how well a facility can meet demand and manage access and waiting times.
Methods: computer simulation [ 136, 138, 161, 227, 298, 360, 388, 391, 392, 404, 444], Markov processes [438], mathematical programming [384], queueing theory [ 32, 98, 138, 227], literature review [ 240, 385].
Facility layout
The facility layout concerns the positioning and organization of various physical areas in a facility. A typical ambulatory care facility consists of a reception area, a waiting area and consultation rooms [164]. The facility layout is a potentially cost-saving decision in ambulatory care facilities [ 164, 330], but we found no papers that used an OR/MS approach to study the layout of an ambulatory care facility. Yet, the handbook [330] discusses heuristics for facility layout problems in health care.
Methods: heuristics [330].
Tactical planning
Patient routing
Ambulatory care typically consists of multiple stages. We denote the composition and sequence of these stages as the route of a patient. An effective and efficient patient route should match medical requirements, capacity requirements and restrictions, and the facility's layout. For a single facility, identifying different patient types and designing customized patient routes for each type prevents superfluous stages and delays [298]. For example, instead of two visits to a doctor and a medical test in between, some patient types may undergo a medical test before visiting the doctor, which saves valuable doctor time. Parallel processing of patients may increase utilization of scarce resources (e.g., a doctor or a CT scanner) [ 161, 227]. When parallel processing is applied, idle time of the scarce resource is reduced by preparing patients for consultation during the consultation time of other patients. Performance is typically measured by total visit time, waiting time and queue length.
Methods: computer simulation [ 82, 161, 227, 298, 388], queueing theory [ 227, 461].
Capacity allocation
On the tactical level, resource capacities settled on the strategic level are subdivided over all patient groups. To do so, patient groups are first assigned to resource types:
-
Assign patient groups to resource types. The assignment of patient groups to available resources requires knowledge about the capabilities of for example clinical staff, support staff or medical equipment, and the medical characteristics of patients. The objective is to maximize the number of patients served, by calculating the optimal assignment of patient groups to appropriately skilled members of clinical staff [384]. Efficiency gains are possible when certain tasks can be substituted between clinical staff, either horizontally (equally skilled staff) or vertically (lower skilled staff) [385].
-
Time subdivision. The available resource capacities, such as staff and equipment, are subdivided over patient groups. For example, general practitioners divide their time between consulting patients and performing prevention activities for patients [195]. When patient demand changes over time (e.g., seasonality), a dynamic subdivision of capacity, updated based on current waiting lists, already planned appointments and expected requests for appointments, performs better than a long-term, static subdivision of resource capacity [429].
Methods: computer simulation [429], mathematical programming [ 195, 384], literature review [433].
Temporary capacity change
The balance between access times and resource utilization may be improved when resource capacities can temporarily be increased or decreased, to cope with fluctuations in patient demand [429]. For example, changing a CT scanner's opening hours [429] or changing doctor consultation time [138].
Methods: computer simulation [ 138, 429].
Access policy
In appointment-driven facilities, the access policy concerns the waiting list management that deals with prioritizing waiting lists so that access time is equitably distributed over patient groups. In the traditional approach, there is one queue for each doctor, but when patient queues are pooled into one joint queue, patients can be treated by the first available doctor, which reduces access times [427]. Another policy is to treat patients without a scheduled appointment, also called ‘walk-in’ service. In between scheduled and walk-in service is ‘advanced access’ (also called ‘open access’, or ‘same-day scheduling’). With advanced access, a facility leaves a fraction of the appointment slots vacant for patients that request an appointment on the same day or within a couple of days. The logistical difficulty of both walk-in service and advanced access is a greater risk of resource idle time, since patient arrivals are more uncertain. However, implementation of walk-in/advanced access can provide significant benefits to patient access time, doctor idle time and doctor overtime, when the probability of patients not showing up is relatively large [ 334, 358]. A proper balance between traditional appointment planning and walk-in/advanced access further decreases access times and increases utilization [ 356, 461]. The specification of such a balanced design will be discussed below.
Methods: computer simulation [ 12, 152, 284, 334, 356, 427], heuristics [284], Markov processes [334], queueing theory [ 358, 461].
Admission control
Given the access policy decisions, admission control involves the rules according to which patients are selected to be admitted from the waiting lists. Factors that are taken into account are for example resource availability, current waiting lists and expected demand. Clearly, this makes admission control and capacity allocation mutually dependent. This is for example the case in [429], where the capacity subdivision for a CT scanner is settled by determining the number of patients to admit of each patient group. Access times can be controlled by adequate admission control [ 168, 173, 238, 429]. Admission control plays a significant role in advanced access or walk-in policies. Successful implementation of these policies requires a balance between the reserved and demanded number of slots for advanced access or walk-in patients. Too many reserved slots results in resource idle time, and too little reserved slots results in increased access time [ 348, 349].
Methods: computer simulation [429], heuristics [173], Markov processes [ 168, 173], mathematical programming [ 238, 348, 349].
Appointment scheduling
Appointment schedules are blueprints that can be used to provide a specific time and date for patient consultation (e.g., an MRI scan or a doctor visit). Appointment scheduling comprises the design of such appointment schedules. Typical objectives of this design are to minimize patient waiting time, maximize resource utilization or minimize resource overtime. A key trade-off in appointment scheduling is the balance between patient waiting time and resource idle time [ 76, 219, 245]. Appointment scheduling is comprehensively reviewed in [ 76, 197]. In an early paper [443], the Bailey-Welch appointment scheduling rule is presented, which is a robust and well-performing rule in many settings [ 219, 241, 253]. References differ in the extent in which various aspects are incorporated in the applied models. Frequently modeled aspects that influence the performance of an appointment schedule are patient punctuality [ 152, 276, 446], patients not showing up (‘no-shows’) [ 152, 153, 220, 241], walk-in patients or urgent patients [ 12, 152, 356, 461], doctor lateness at the start of a consultation session [ 152, 153, 283, 360], doctor interruptions (e.g., by comfort breaks or administration) [ 153, 276] and the variance of consultation duration [219]. These factors can be taken into account when modeling the following key decisions that together design an appointment schedule:
-
Number of patients per consultation session. The number of patients per consultation session is chosen to control patient access times and patient waiting times. When the number of patients is increased, access times may decrease, but patient waiting times and provider overtime tend to increase [ 73, 152, 219].
-
Patient overbooking. Patients not showing up, also called ‘no-shows’, cause unexpected gaps, and thus increase resource idleness [219]. Overbooking of patients, that is, booking more patients into a consultation session than the number of planned slots is suggested to compensate no-shows in [ 254, 258, 273, 317, 387]. Overbooking can significantly improve patient access times and provider productivity, but it may also increase patient waiting time and staff overtime [ 254, 258]. Overbooking particularly provides benefits for large facilities with high no-show rates [254].
-
Length of the appointment interval. The decision for the length of the planned appointment interval or slot affects resource utilization and patient waiting times. When the slot length is decreased, resource idle time decreases, but patient waiting time increases [153]. For some distributions of consultation time, patient waiting times and resource idle time are balanced when the slot length equals the expected length of a consultation [76]. The slot length can be chosen equal for all patients [ 153, 219, 443], but using different, appropriate slot lengths for each patient group may decrease patient waiting time and resource idle time when expected consultation times differ between patient groups [136].
-
Number of patients per appointment slot. Around 1960, it was common to schedule all patients in the first appointment slot of a consultation session [158]. This minimizes resource idle time, but has a negative effect on patient waiting times [ 342, 360]. Later, it became common to distribute patients evenly over the consultation session to balance resource idle time and patient waiting time. In [158], various approaches in between these two extremes are evaluated, such as two patients in one time slot and zero in the next.
-
Sequence of appointments. When different patient groups are involved, the sequence of appointments influences waiting times and resource utilization. Appointments can be sequenced based on patient group or expected variance of the appointment duration. In [253], various rules for patient sequencing are compared. Alternatively, when differences between patients exist with respect to the variation of consultation duration, sequencing patients by increasing variance (i.e., lowest variance first) may minimize patient waiting time and resource idle time [76].
-
Queue discipline in the waiting room. The queue discipline in the waiting room affects patient waiting time, and the higher a patient's priority, the lower the patient's waiting time. The queue discipline in the waiting room is often assumed to be first-come-first-serve (FCFS), but when emergency patients and walk-in patients are involved, the highest priority is typically given to emergency patients and the lowest priority to walk-in patients [76]. Priority can also be given to the patient that has to visit the most facilities on the same day [298].
-
Anticipation for unscheduled patients. Facilities that also serve unscheduled patients, such as walk-in and urgent patients, require an appointment scheduling approach that anticipates these unscheduled patients by reserving slack capacity. This can be achieved by leaving certain appointment slots vacant [128], or by increasing the length of the appointment interval [76]. Reserving too little capacity for unscheduled patients results in an overcrowded facility, while reserving too many may result in resource idle time. Often, unscheduled patients arrive in varying volumes during the day and during the week. When an appropriate number of slots is reserved for unscheduled patients, and appointments are scheduled at moments that the expected unscheduled demand is low, patient waiting times decrease and resource utilization increases [ 326, 356, 461]. In the online operational level of this section, we discuss referring unscheduled patients to a future appointment slot when the facility is overcrowded.
Methods: computer simulation [ 14, 73, 77, 110, 136, 152, 153, 205, 219, 220, 245, 258, 276, 283, 284, 298, 326, 356, 392, 433, 434, 443, 446], heuristics [ 73, 241, 284], Markov processes [ 158, 188, 241, 253, 280, 317, 387], mathematical programming [ 25, 73, 106, 357], queueing theory [ 52, 98, 128, 254, 273, 357, 433, 461], literature review [ 76, 197, 240, 385].
Staff-shift scheduling
Shifts are duties with a start and end time [65]. Shift scheduling deals with the problem of selecting what shifts are to be worked and how many employees should be assigned to each shift to meet patient demand [141]. More attractive schedules promote job satisfaction, increase productivity and reduce turnover. While staff dimensioning on the strategic level has received much attention, shift scheduling in ambulatory care facilities seems underexposed in the literature. In [63], shift schedules are developed for physicians, who often have disproportionate leverage to negotiate employment terms, because of their specialized skills. Hence, physicians often have individual arrangements that vary by region, governing authority, seniority, specialty and training. Although these individual arrangements impose requirements to the shift schedules, there is often flexibility for shifts of different lengths and different starting times to cope with varying demand during the day or during a week. In this context, the handbook by [330] discusses staggered shift scheduling and flexible shift scheduling. In the first alternative, employees have varying start and end times of a shift, but always work a fixed number of hours per week. In the latter, cheaper alternative, a core level of staff is augmented with daily adjustments to meet patient demand.
Methods: computer simulation [338], mathematical programming [63], literature review [ 65, 141, 199, 330].
Offline operational planning
Patient-to-appointment assignment
Based on the appointment scheduling blueprint developed on the tactical level, patient scheduling comprises scheduling of an appointment in a particular time slot for a particular patient. A patient may require multiple appointments on one or more days. Therefore, we distinguish scheduling a single appointment, combination appointments and appointment series:
-
Single appointment. Patients requiring an appointment often have a preference for certain slots. When information is known about expected future appointment requests and the expected preferences of these requests, a slot can be planned for this patient to accommodate the current patient, but also to have sufficient slots available for future requests from other patients. This can for example be necessary to ensure that a sufficient number of slots is available for advanced access patients [ 198, 439], or to achieve equitable access for all patient groups to a diagnostic facility [335].
-
Combination appointments. Combination appointments imply that multiple appointments for a single patient are planned on the same day, so that a patient requires fewer hospital visits. This is the case when a patient has to undergo various radiotherapy operations on different machines within one day [340].
-
Appointment series. For some patients, a treatment consisting of multiple (recurring) appointments may span a period of several weeks or months. The treatment is planned in an appointment series, in which appointments may have precedence relations and certain requirements for the time intervals in between. In addition, the involvement of multiple resources may further complicate the planning of the appointment series. The appointment series have to fit in the existing appointment schedules, which are partly filled with already scheduled appointments. Examples of patients that require appointment series are radiotherapy patients [ 93, 94, 95] and rehabilitation patients [85].
Methods: heuristics [ 85, 340, 439], Markov processes [ 198, 335, 439], mathematical programming [ 93, 94, 95].
Staff-to-shift assignment
On the tactical level, staff-shift scheduling results in shifts that have to be worked. In staff-to-shift assignment on the offline operational level, a date and time are given to staff members to perform particular shifts. For example, a consultation session is scheduled for a doctor on a particular day and time, and with a certain duration. For an endoscopy unit, in [238] a model is presented to schedule available doctors to endoscopy unit shifts.
Methods: mathematical programming [238], literature review [199].
Online operational planning
Dynamic patient (re)assignment
After patients are assigned to slots in the appointment schedule, the appointments are carried out on their planned day. During such a day, unplanned events, such as emergency or walk-in patients, extended consultation times, and equipment breakdown, may disturb the planned appointment schedule. In such cases, real-time dynamic (re)scheduling of patients is required to improve patient waiting times and resource utilization in response to acute events. For example, to cope with an overcrowded facility walk-in patients can be rescheduled to a future appointment slot to improve the balance of resource utilization over time [351]. Dynamic patient (re)assignment can also be used to decide which patient group to serve in the next time slot in the appointment schedule [188], for example based on the patient groups’ queue lengths. When inpatients are involved in such decisions, they are often subject to rescheduling [76], since it is assumed that they are less harmed by a rescheduled appointment as they are already in the hospital. However, longer waiting times of inpatients may be more costly, since it may mean they have to be hospitalized longer [100].
Methods: computer simulation [351], Markov processes [ 100, 188, 280], mathematical programming [100].
Staff rescheduling
At the start of a shift, the staff schedule is reconsidered. Before and during the shift, the staff capacities may be adjusted to unpredicted demand fluctuations and staff absenteeism by using part-time, on-call nurses, staff overtime and voluntary absenteeism [ 191, 342].
Methods: no papers found.
3.2. Emergency care services
Emergency care services have the goal to reduce morbidity and mortality resulting from acute illness and trauma [ 352, 454]. To attain this goal, rapid response of an ambulance and transportation to an emergency care center (e.g., an emergency department in a hospital, or an emergency location near a disaster) is required [ 37, 352]. Patients arrive to the emergency department (ED) of a hospital as a self-referral, through ambulatory care services or by ambulance [54]. A frequently reported and studied problem in emergency care is that of long ED waiting times. One of the causes of long ED waiting time is treatment of a high number of self-referrals that could also be treated in ambulatory care services (e.g., by general practitioners). To cope with this problem, EDs increasingly cooperate with ambulatory care services, for example by combining the ED with a service that provides primary care outside office hours, or by opening an ambulatory walk-in center to which these patients can be referred [270]. The body of OR/MS literature directed to emergency care services is large. The existing literature mainly focuses on the strategic decisions regional coverage and capacity dimensioning for ambulances, and the tactical decision staff-shift scheduling.
Strategic planning
Regional coverage
To be able to provide rapid response to an acute illness or trauma, emergency care services need to be geographically close to their customer base, where emergencies can potentially occur [342]. Given a geographical region with a certain spatial distribution of service requests (i.e. emergency demand), the locations, types and number of emergency care facilities have to be decided. The objective is to find a balanced distribution of facilities to guarantee a desired level of service [ 36, 279]. This level of service can for example be measured by the maximum time it takes for a patient to travel to the closest ED, or the maximum response time that an ambulance requires to reach a specified region. The main trade-off in the decision where to locate emergency care centers and ambulances is between the level of service for emergency patients and costs [ 36, 41, 68, 203, 237]. Below, we will elaborate on this trade-off for both emergency care centers and ambulances.
-
Emergency care centers. The decision where to locate emergency care centers, such as an ED in a hospital, is determined such that locations where emergencies may occur have at least one emergency care center within a target travel time or distance [353]. When a large-scale emergency or disaster occurs, an emergency care center may be unable to provide emergency care services (e.g., the facility is destroyed). In [222], this possibility is incorporated in regional coverage models that can be used to determine good locations for (temporary) emergency care centers after a disaster.
-
Ambulances (e.g., vans, motorcycles, helicopters, airplanes). The decision where to locate ambulances is determined such that a specified region can be reached within a target response time by one or more ambulances, or that the average or maximum response time to a potential emergency is minimized [ 41, 68, 134, 140, 237]. The response time of an ambulance concerns the time elapsed from notification of an emergency until an ambulance arrives at the emergency location [154]. Other factors to take into account in planning the locations of ambulances are the likelihood of timing and location of an emergency, staff availability, location constraints (e.g., a place where staff can rest), and the emergency care center where patients are potentially transported to [ 33, 56, 68, 134, 154, 175, 230, 237, 342, 352, 454].
Methods: computer simulation [ 56, 140, 154, 160, 174, 203, 230, 352, 366, 393, 454], heuristics [ 20, 33, 35, 139, 170, 229], Markov processes [ 19, 222], mathematical programming [ 16, 33, 35, 36, 37, 41, 68, 99, 134, 140, 160, 175, 177, 203, 222, 237, 352, 353, 380, 393, 407], queueing theory [ 33, 170, 229, 269, 290, 380], literature review [ 61, 183, 237, 279, 342, 353].
Service mix
An organization decides the particular services that the emergency care facility provides. Facilities may provide services for particular types of emergency patients, which are possibly classified by severity of trauma. For example, a first-aid center may provide services that are adequate for minor emergencies, while an academic medical center is equipped to treat the most complex and severe traumas. In this case, treating minor emergencies at the first-aid center may alleviate the use of expensive resources in the academic medical center, and may be more cost-effective from a societal viewpoint. In order to balance provided emergency care and the cost of emergency care resources within a region or country, the service mix decision may be governed by societal influences and governmental regulations.
In general, the service mix decision is not made at an emergency care service level, but at the hospital level, as it integrally impacts the ambulatory, emergency, surgical and inpatient care services. The decided service mix dictates the case mix of emergency patients that can be served by the emergency care facility. Emergency care facilities in general do not decide a particular case mix, as they are often obliged to serve arriving emergency patients with any type of injury or disease [ 78, 336].
Methods: no papers found.
Ambulance districting
A covered region may be subdivided into several districts to which available ambulances are assigned. In subdividing a region and assigning ambulances to districts, it is the objective to minimize response times, while balancing the workload [ 33, 74, 269]. When an emergency occurs in a district, one of the available ambulances within that district is dispatched to the emergency [ 33, 269]. When none are available (e.g., when all ambulances are responding to a call), an ambulance from a different district may be dispatched to the emergency [269]. Such interdistrict dispatching decreases average response times, especially for relatively smaller districts. This is the effect of so-called pooling of resources [366]. Owing to this possibility of interdistrict dispatching, only predicting the workload generated within the assigned district may not lead to a well-balanced ambulance districting decision. In the analysis of the districting problem, overlapping districts, mobile locations and interdistrict dispatching should be included for an accurate prediction of workload balance [269].
Methods: computer simulation [ 174, 366], heuristics [33], mathematical programming [33], queueing theory [ 33, 74, 269].
Capacity dimensioning
Emergency care facilities dimension their resources with the objective to attain a reliable level of service while minimizing costs [ 36, 37, 323]. Often, this level of service is represented by a response target, for example x% of the emergency patients should be reached (ambulance) or seen (ED) within y minutes. An imbalance in supply and demand can lead to congestion or overcrowding in the ED [56]. ED overcrowding results in long waiting times, patients who leave the ED without being seen, and ambulance diversions [ 78, 189, 336]. This leads to patient dissatisfaction, medical errors and decreased staff satisfaction [336]. A typical cause of congestion in the ED is the delay in admitting emergency patients to an inpatient bed due to congested medical care units and ICUs [ 15, 78, 90, 322, 323, 422]. Congestion may also be caused by insufficient available resources in the surgical care services (e.g., operating time capacity) and ambulatory care services (e.g., diagnostic equipment). Moreover, coordinated decision making for resource capacity dimensioning both within, and in services relating to emergency care services, reduces delays for emergency patients [ 15, 54, 78, 90, 266, 422]. The following resources are dimensioned:
-
Ambulances. Ambulances exist in different transport modalities (helicopters, vans, cars) carrying different types of equipment and staff [ 35, 36, 37, 140, 160, 230, 352, 366, 380, 401, 454]. Ambulances collect emergency patients, but also perform less urgent transfers of patients between care facilities [401]. The number of ambulances should be chosen to include buffer capacity, to cope with fluctuations in demand and ambulance availability. Fluctuations in demand may be caused by expected demand peaks, such as large events, or unexpected demand peaks, such as large-scale accidents [454].
-
Waiting room. The waiting rooms is possibly separated for patients awaiting results and patients awaiting initiation of service [ 90, 336].
-
Treatment rooms. Treatment rooms comprise treatment beds or treatment chairs [ 78, 90, 266, 336]. Occupation of treatment rooms can be alleviated by letting patients await their lab test results in the waiting room and not in the treatment room [ 78, 90].
-
Emergency wards. These are observation wards for a temporary stay, possibly before admission to the general wards [ 15, 90, 322, 323], also called Acute Admission Unit (AAU). Capacity is generally given in the number of beds.
-
Equipment. Equipment may be required for emergency procedures, including treatment beds, treatment chairs and diagnostic equipment [ 78, 90, 336]. In general, diagnostic testing is considered outside the control of the emergency care services [155]. Emergency patients may require an X-ray or other diagnostic testing, and may have to compete with inpatients and outpatients for diagnostic resource capacity. Ineffective management of the diagnostic department causes delays in the emergency care services [155]. Installing diagnostic equipment in the ED may decrease the waiting time for diagnostic results, and therewith the overall length of stay of a patient in the ED [336].
-
Staff. Staff in emergency care services is composed of different skill and responsibility levels, for example doctors, emergency nurses and support staff [ 54, 155, 189, 240, 266, 322, 323, 336, 458]. Required staffing dimensions, and thereby staff costs, may be reduced by passing on non-critical patients from doctors to lower-qualified, less-costly staff, releasing doctors to work on the critical cases [54]. Moreover, flexibility in staffing can be used to cost-effectively match uncertain emergency demand with resource capacity. For example, staff members may be ‘on call’ while working elsewhere or being off-duty, and they are called upon when additional staff is required in the ED to cope with unexpected demand peaks [323].
Methods: computer simulation [ 15, 37, 54, 78, 140, 155, 160, 230, 266, 270, 322, 352, 366, 454, 458], heuristics [35], mathematical programming [ 35, 36, 140, 322, 323, 352], queueing theory [ 90, 189, 380, 401], literature review [ 56, 240, 336].
Facility layout
The facility layout concerns the positioning and organization of different physical areas in a facility. Hospital managers aim to find the layout of the emergency care facility that maximizes the number of emergency patients that can be examined, given the budgetary and building constraints. Letting patients wait for their lab results in a waiting area instead of the treatment room enables the treatment rooms to be used more effectively, which can decrease patient waiting time [90]. Moreover, integration of the facility layout decision and the patient routing decision may decrease costs.
Methods: computer simulation [458], heuristics [330], literature review [336].
Tactical planning
Patient routing
An emergency patient process consists of multiple stages. We denote the composition and sequence of these stages as the route of a patient. Patient routes are designed to minimize patient waiting time, maximize patient throughput and increase staff utilization [ 54, 240]. A typical patient process is as follows. Patients arrive to the hospital as a self-referral, through ambulatory care services or by ambulance [54]. Generally, upon arrival at the ED, patients see a ‘triage-nurse’, who prioritizes these patients into urgency categories [78]. After triage and possibly a wait in the waiting room, patients see a medical staff member that aims to establish a diagnosis of the patient's condition timely and cost-effectively. In this phase, diagnostic tests (e.g., laboratory, X-ray) are typically required. Although more expensive, it may be decided to directly administer multiple diagnostic tests, to reduce the time to establish a diagnosis and patient waiting time [240]. When a diagnosis is determined, possibly a treatment is carried out at the ED. This treatment may be continued in the operating room or a medical care unit in the hospital. If (further) treatment is not required, the patient is discharged, possibly with a referral to an ambulatory care clinic [265].
To minimize patient waiting time, maximize patient throughput and increase staff utilization, alternative patient routing systems within the emergency care services may be developed. For example, a ‘fast-track system’ in the ED separates the patients with minor injuries and illnesses from the more severe traumas [ 90, 240, 299]. It reduces waiting time for patients with minor injuries and illnesses [299], but may lead to increased waiting time for the other patient groups, since less resources are available for these groups [155]. This may be acceptable, when the effect is not too large [299] and the increased waiting times are still within the set targets for each patient group [ 54, 240]. As relatively many steps in the emergency care process depend on effective and efficient processing in other care services (e.g., diagnostic services, surgical care services, and inpatient care services), coordinated decision making between the services involved in the emergency care process reduces delays for emergency patients [ 54, 78, 90, 155].
Methods: computer simulation [ 54, 78, 155, 265, 299, 425], queueing theory [ 90, 302], literature review [ 240, 336].
Admission control
Admission control involves the rules according to which patients are selected to be served. The admission control rules first prescribe that the highest priority (life-threatened) patients are seen immediately, and that other patients can be deferred to the waiting room until they can be seen by a clinician [54]. Secondly, they define the order in which waiting patients are selected to be served. In the triage process, mentioned earlier in the patient routing decision, emergency patients are classified into ‘triage categories’ (often five) during an assessment by a qualified medical practitioner [78]. Typically, waiting time targets are set for each triage category, as a particular waiting time has a different impact on the health status of two patients in different urgency groups [302]. In general, patients are served in the order of triage category of decreasing urgency. However, applying more dynamic rules that take into account the number of waiting patients per triage category can enhance the compliance to the waiting time targets per category [54].
Methods: computer simulation [ 54, 78], queueing theory [302].
Staff-shift scheduling
Shifts are hospital duties with a start and end time [65]. Shift scheduling deals with the problem of selecting what shifts are to be worked and how many employees should be assigned to each shift to meet patient demand [141]. The objective of shift scheduling is to generate shifts that minimize the number of staff hours required to cover the desired staffing levels [345]. The required staffing levels are determined by calculating how much staff is required to reach a given service level target, for example x% of the patients should be seen in y minutes.
For an ED, patient demand varies significantly throughout the week and throughout the day. Therefore, identical staffing schedules each day and each hour may seem convenient and practical, but they are likely suboptimal [185]. Implementing different staffing levels based on patient arrival rates for different moments within the day and week may decrease patient waiting times and reduce the number of patients that leave an ED without being seen [189]. To calculate the required staffing levels on each moment of the day, the working day is typically divided into planning intervals [184]. The required staffing level in each interval is dependent on the patient arrivals in that interval, but also by delayed congestion effects from prior intervals [ 184, 189]. Therefore, it can be beneficial to let a change in staffing level follow a change in patient arrival rate after a certain delay in time [184].
When staffing levels are determined, a set of shifts can be developed to meet those staffing levels as close as possible. Staggered shift scheduling is when shifts do not have to start and finish at the same time. This results in more flexibility to accommodate shifts to the required staffing levels at specific intervals, leading to improved utilization of resources [381]. Shift schedules are impacted by the preferences of staff and by laws prescribing emergency staff is only available for a limited number of hours [ 139, 189].
Methods: computer simulation [ 230, 381, 382, 458], heuristics [ 381, 382], queueing theory [ 184, 185, 189], literature review [ 199, 240, 336].
Offline operational planning
Staff-to-shift assignment
In staff-to-shift assignment, a date and time are given to a staff member to perform a particular shift. The objective is to attain the tactically settled staffing levels for each shift while minimizing costs, such as overtime by regular staff or staff hired temporarily from an agency [18]. Staff-to-shift assignments can be noncyclic and cyclic, where in the latter a staff member constantly repeats the same shift pattern [75]. In staff-to-shift assignment, labor laws, staff availability and staff satisfaction have to be taken into account [ 18, 23, 103]. In [139], the staff-to-shift assignment for ambulance staff is coordinated with the regional coverage decision for ambulances, to maximize the provided service level for patients in a region.
Methods: heuristics [75], mathematical programming [ 18, 23, 75, 103, 139].
Online operational planning
Ambulance dispatching
Ambulance dispatching concerns deciding which ambulance to send to an emergency patient [8]. When calls to report an emergency event come in, a physician, nurse or paramedic assesses whether the reported emergency requires an ambulance. If so, the call is transferred to the dispatcher, who decides which ambulance will respond [380]. Many dispatching rules exist, and a commonly used rule is to send the ambulance closest to the emergency [281]. However, when predictions on future emergency calls are incorporated, sending the closest ambulance is not always optimal, as dispatching an ambulance makes it temporarily unavailable to respond to other calls. Shorter overall response times can be achieved when future demand is also incorporated in the dispatching decision [274]. When multiple calls come in, prioritizing calls and dispatching accordingly may balance ambulance workload [174]. Prioritizing and dispatching based on urgency improves response rates for the high-urgent calls [281]. After the dispatching decision has been made and an ambulance is traveling to the emergency, a request for emergency care may be canceled, leading to resource idle time [203].
Methods: computer simulation [ 8, 274, 281, 454], heuristics [274], mathematical programming [281], queueing theory [401].
Facility selection
When an ambulance has collected a patient, the emergency facility to which to bring a collected emergency patient has to be decided [454]. It is the aim to select the facility that minimizes the patient's travel time and is ‘adequate’ to serve the patient. The prospective emergency facility may for example be a local health clinic, a first-aid center or a hospital ED, and its appropriateness depends on the match between the facility's services, resources and bed availability, and the services required for the medical condition of the patient [366]. Delivering the emergency patient to the closest appropriate ED also leads to higher ambulance availability, as ambulance travel time is minimized [366].
Methods: computer simulation [366].
Ambulance routing
When an ambulance is dispatched to a particular emergency, the fastest route between an ambulance's location and the emergency location needs to be determined with the aim to minimize ambulance response times. Information with respect to distance, traffic, road work, accessibility can be taken into account. No specific contributions have been found for ambulance routing with our search method, but note that a wide range of contributions in the general problem of vehicle routing exists [408].
Methods: no papers found.
Ambulance relocation
When ambulances are unavailable, for example because they are dispatched to emergency cases or they are in repair, they may leave a significant fraction of population without ambulance coverage [167]. In this case, to maximize regional coverage and to decrease response times, ambulances may be relocated [ 8, 61, 167, 300]. Relocation improves flexibility to respond to fluctuating patient demand [454] and dynamic traffic conditions [368]. When relocating ambulances dynamically, one aims to control the number of relocations to avoid successively relocating the same set of ambulances, long travel times between the initial and final location, and repeated round trips between the same two locations [ 61, 167]. However, the increased movements of ambulances caused by dynamic relocation may also pose advantages. There is a higher chance of receiving a call while on the road, which may result in a decrease in response times caused by shorter turn-out times, that is, the time for a crew to get ready before they can drive to an emergency when they are dispatched [300]. Real-time dynamic relocation is increasingly implementable, due to the increased availability of location information and the decreasing price of computing power [300].
Methods: computer simulation [ 8, 167, 454], Markov processes [ 300, 368], mathematical programming [167], literature review [61].
Treatment planning and prioritization
Each patient may follow a tailored set of stages through the ED, for example patients may receive different diagnostic tests and visit different types of doctors [78]. It is the objective to dynamically plan these stages, such that resource utilization is maximized and waiting time between stages is minimized. Planning the sequence of these stages and the selection of which task for which patient is performed at each point in time includes various factors, such as urgency, medical requirements, resource availability and patient waiting time. This planning decision is highly interrelated with the strategic and tactical level decisions facility layout, patient routing and admission control. As these decisions shape the process flow for a particular patient and set the priority rules applying to the patient. Furthermore, there is a significant interdependence between medical decision making and resource capacity planning in this planning decision.
Methods: computer simulation [ 78, 155].
Staff rescheduling
When emergency demand for ambulances or in the emergency care facility is significantly higher than predicted or when staff is lower than expected (e.g., absent due to illness), additional staff may be required. Especially when senior doctors, who are required for key decisions such as discharge and particular treatments of a patient, are unexpectedly unavailable, it is recommended to call in an additional senior doctor [322].
Methods: computer simulation [458], mathematical programming [322].
3.3. Surgical care services
Surgeries are physical interventions on tissues, generally involving cutting of a patient's tissues or closure of a previously sustained wound, to investigate or treat a patient's pathological condition. Surgical care services have a large impact on the operations of the hospital as a whole [ 29, 46, 72], and they are the hospital's largest revenue center [ 72, 108]. Surgical care services include ambulatory surgical wards, where patients wait and stay before and after being operated. We do not classify such wards as inpatient care services, since patients served on ambulatory basis do not require an overnight stay. The proportion of ambulatory surgeries, which are typically shorter, less complex and less variable [341], is increasing in many hospitals [301]. There is a vast amount of literature on OR/MS in surgical care services, comprehensively surveyed in [ 45, 72, 111, 192, 196, 197, 287, 301, 345, 386, 436]. These surveys are used to create the taxonomic overview of the planning decisions.
Strategic planning
Regional coverage
At a regional level, the number, types and locations of surgical care facilities have to be determined to find a balanced distribution of facilities with respect to the geographical location of demand [130]. The main trade-off in this decision is between patient accessibility and facility efficiency. Coordination of activities between hospitals in one region can provide significant cost reductions at surgical care facilities and downstream facilities [ 50, 365].
Methods: computer simulation [50], mathematical programming [365].
Service mix
An organization selects the particular services that the surgical care facility provides. The service mix stipulates which surgery types can be performed, and therefore impacts the net contribution of a facility [221]. Specific examples of services are medical devices to perform noninvasive surgeries and robotic services for assisting in specialized surgery [107]. In general, the service mix decision is not made at a surgical care service level, but at the regional or hospital level, as it integrally impacts the ambulatory, emergency, surgical and inpatient care services.
Methods: no papers found.
Case mix
The case mix involves the number and types of surgical cases that are performed at the facility. Often, diagnosis-related groups (DRGs), which classify patient groups by relating common characteristics such as diagnosis, treatment, and age to resource requirements, are used to identify the patient types included in the case mix [225]. The case mix is chosen with the objective to optimize net contribution while considering several internal and external factors [ 192, 225]. Internal factors include the limited resource capacity, the settled service mix, research focus, and medical staff preferences and skills [ 46, 192, 239]. External factors include societal preferences, the disease processes affecting the population in the facility's catchment area [46], the case mix of competing hospitals [127], and the restricted budgets and service agreements in government-funded systems [46]. High profit patient types may be used to cross-subsidize the unprofitable ones, possibly included for research or societal reasons [46].
Methods: computer simulation [239], mathematical programming [ 46, 225], literature review [192].
Capacity dimensioning
Surgical care facilities dimension their resources with the objective to optimize hospital profit, idle time costs, surgery delays, access times and staff overtime [ 285, 370]. Therefore, provider capacity must be matched with patient demand [370] for all surgical resource types. The capacity dimensioning decisions for different resource types are highly interrelated and performance is improved when these decisions are coordinated both within the surgical care facility and with capacity dimension decisions in services outside the surgical care facility, such as medical care units and the Intensive Care Unit (ICU) [ 56, 369, 421, 422]. The following resources are dimensioned:
-
Operating rooms. Operating rooms can be specified by the type of procedures that can be performed [ 21, 196, 240, 370].
-
Operating time capacity. This concerns the number of hours per time period the surgical care services are provided [ 239, 301, 369, 402, 421]. Operating time capacity is determined by the number of operating rooms and their opening hours [285].
-
Presurgical rooms. These rooms are used for preoperative activities, for example induction rooms for anesthetic purposes [301].
-
Recovery wards. At these wards, patients recover from surgery [ 255, 256, 257, 369, 370]. The recovery ward is also called Post Anesthesia Care Unit (PACU) [192].
-
Ambulatory surgical ward. At this ward, outpatients stay before and after surgery.
-
Equipment. Equipment may be required to perform particular surgeries. Examples are imaging equipment [197] or robotic equipment [107]. Equipment may be transferable between rooms, which increases scheduling flexibility.
-
Staff. Staff in surgical care services include surgeons, anesthesiologists, surgical assistants and nurse anesthetists [ 5, 64, 107, 221]. Staffing costs are a large portion of costs in surgical care services [ 10, 107]. Significant cost savings can be achieved by increasing staffing flexibility [107], for example by (i) cross-training surgical assistants for multiple types of surgeries [196], (ii) augmenting nursing staff with short-term contract nurses [107], and (iii) drawing nurses from less critical parts in the hospital during demand surges [107].
Methods: computer simulation [ 239, 255, 256, 257, 285, 369, 370, 421], heuristics [ 64, 107, 221], mathematical programming [ 21, 64, 107, 402], queueing theory [285], literature review [ 240, 301].
Facility layout
The facility layout concerns the positioning and organization of different physical areas in a facility. The aim is to determine the layout of the surgical care facility that maximizes the number of surgeries that can take place, given the budgetary and building constraints. A proper integration of the facility layout decision and the patient routing decision decreases costs and increases the number of patients operated [291]. For example, when patients are not anesthetized in the operating room, but in an adjacent induction room, patients can be operated with shorter switching times in between. In [301], contributions that model a facility layout decision for surgical care services are reviewed.
Methods: computer simulation [291], heuristics [330], literature review [301].
Tactical planning
Patient routing
A surgical process consists of multiple stages. We denote the composition and sequence of these stages as the route of a patient. The surgical process consists of a preoperative, perioperative and postoperative stage [ 192, 196, 341]. The preoperative stage involves waiting and anesthetic interventions, which can take place in induction rooms [291] or in the operating room [301]. The perioperative stage involves surgery in the operating room, and the postoperative stage involves recovery at a recovery ward [192]. Recovery can also take place in the operating room when a recovery bed is not immediately available [13]. Surgical patients requiring a bed are admitted to a (inpatient or outpatient) medical care unit before the start of the surgical process, where they return after the surgical process [235]. Efficient patient routes are designed with the objective to increase resource utilization [291].
Methods: computer simulation [291], heuristics [13], mathematical programming [ 13, 341], literature review [ 192, 301].
Capacity allocation
On the tactical level, resource capacities settled on the strategic level are subdivided over patient groups. The objectives of capacity allocation are to trade off patient access time and the utilization of surgical and postsurgical resources [ 45, 123, 192, 287, 402], to maximize contribution margin per hour of surgical time [72], to maximize the number of patients operated, and to minimize staff overtime [201]. Capacity allocation is a means to achieve an equitable distribution of access times [402]. Hospitals commonly allocate capacity through block scheduling [ 151, 192, 433]. Block scheduling involves the subdivision of operating time capacity in blocks that are assigned to patient groups [ 192, 196]. Capacity is allocated in three consecutive steps. First, patient groups are identified. Second, resource capacities, often in the form of operating time capacity, are subdivided over the identified patient groups. Third, blocks of assigned capacity are scheduled to a specified date and time.
-
Patient group identification. In general, patient groups are classified by (sub)specialty, medical urgency, diagnosis or resource requirements. Identification by medical urgency distinguishes elective, urgent and emergent cases [ 72, 145, 192, 196]. Elective cases can be planned in advance, urgent cases require surgery urgently, but can incur a short waiting period, and emergency patients require surgery immediately [ 51, 72]. Examples of patient grouping by resource requirements are inpatients, day-surgery patients [196] and grouping patients by the equipment that is required for the surgery [107].
-
Time subdivision. With the earlier mentioned objectives, operating time is subdivided over the identified patient groups based on expected surgery demand. This is often a politically charged and challenging task, since various surgical specialties compete for a profitable and scarce resource. What makes it even more complex is that hospital management and surgical specialties may have conflicting objectives [48]. When allocating operating time capacity to elective cases, a portion of total operating time capacity is reserved for emergency cases, which arrive randomly [169]. Staff overtime is the result when the reserved capacity is insufficient to serve all arriving emergency patients, but resource idle time increases when too much capacity is reserved, causing growth in elective waiting lists [ 51, 262, 263, 339, 462]. Capacity can be reserved by dedicating one or more operating rooms to emergency cases, or by reserving capacity in elective operating rooms [ 72, 261, 379].
-
Block scheduling. In the last step of capacity allocation, a date and time are assigned to blocks of allocated capacity [29]. Several factors have to be considered in developing a block schedule. For example, (seasonal) variation in surgery demand, the number of available operating rooms, staff capacities, surgeon preferences, and material and equipment requirements [ 29, 365]. Block schedules are often developed to be cyclic, meaning the block schedule is repeated periodically. A (cyclic) block schedule is also termed a Master Surgical Schedule (MSS) [420]. Cyclic block schedules may not be suitable for rare elective procedures [ 192, 420]. For these procedures, capacity can be reserved in the cyclic block schedule [436], or non-cyclical plans may provide an outcome. When compared with cyclic plans, non-cyclic [ 107, 120, 121], or variable plans [240], increase flexibility, decrease staffing costs [107] and decrease patient access time [ 199, 240]. However, cyclic block schedules have the advantage that they make demand more predictable for surgical and downstream resources, such as the ICU and general wards, so that these resources can increase their utilization by anticipating demand more structurally [420].
In addition to block scheduling, the literature also discusses open scheduling and modified block scheduling. Open scheduling involves directly scheduling all patient groups in the total available operating time capacity, without subdividing this capacity first. Although open scheduling is more flexible than block scheduling, open scheduling is rarely adopted in practice [ 48, 192], because it is not practical with regards to doctor schedules and increases competition for operating time capacity [ 287, 345]. Modified block scheduling is when only a fraction of operating time capacity is allocated by means of block scheduling [ 117, 192]. Remaining capacity is allocated and scheduled in a later stage, which increases flexibility to adapt the capacity allocation decision based on the latest information about fluctuating patient demand [192].
Capacity allocation decisions in surgical care services impact the performance of downstream in-patient care services [ 29, 31, 45, 72, 107, 287, 344, 422, 423, 424]. Variability in bed utilization and staff requirements can be decreased by incorporating information about the required inpatient beds for surgical cases in allocating surgical capacity [ 4, 29, 31, 186, 365, 419, 420]. In contributions that model downstream services, it is often the objective to level the bed occupancy in the wards or the ICU, to decrease the number of elective surgery cancellations [ 29, 72, 344, 365, 395, 402, 419, 420], or to minimize delays for inpatients waiting for surgery [459].
Methods: computer simulation [ 51, 117, 120, 121, 262, 339, 459], heuristics [ 29, 30, 31, 395, 431], Markov processes [ 169, 423, 424, 462], mathematical programming [ 29, 30, 31, 47, 48, 80, 107, 199, 262, 344, 365, 395, 402, 403, 419, 420, 459], queueing theory [462], literature review [ 45, 72, 192, 196, 240, 287, 330, 422, 433, 436].
Temporary capacity change
Available resource capacity could be temporarily changed in response to fluctuations in demand [285]. When additional operating time capacity is available, it can be allocated to a particular patient group, for example based on contribution margin [ 196, 436] or access times [402], or it can be proportionally subdivided between all patient groups [ 48, 402].
Methods: computer simulation [117], mathematical programming [ 48, 107, 402], literature review [ 196, 199, 436].
Unused capacity (re)allocation
Some time periods before the date of carrying out a settled block schedule, capacity allocation decisions may be reconsidered in order to reallocate capacity that remains unused [ 125, 196, 215] and to allocate capacity not allocated before (for example in modified block scheduling, discussed in capacity allocation). When unused capacity is released sufficiently early before the surgery time is planned, better quality reallocations are possible than when the unused capacity is released on the same day it is available [215]. Unused capacity is (re)allocated with the same objectives as the capacity allocation decision.
Methods: computer simulation [ 117, 125], heuristics [125], Markov processes [215], literature review [196].
Admission control
Admission control involves the rules according to which patients from different patient groups are selected to undergo surgery in the available operating time capacity. There is a strong reciprocal relation between admission control decisions and capacity allocation decisions: capacity allocation decisions demarcate the available operating time capacity for surgeries, and admission control decisions influence the required operating time capacity. Admission control has the objective to balance patient service, resource utilization and staff satisfaction [45]. It is established by developing an admission plan that prescribes how many surgeries of each patient group to perform on each day, taking the block schedule into account [4]. Balancing the number of scheduled surgical cases throughout the week prevents high variance in utilization of involved surgical resources, such as operating rooms and recovery beds, and downstream inpatient care resources, such as ICU and general ward beds [ 3, 4, 29, 247, 287, 410]. Resource utilization can be improved by using call-in patients [45] and overbooking [51]. Call-in patients are given a time frame in which they can be called in for surgery when there is sufficient space available in the surgical schedule. Overbooking of patients involves planning more surgical cases than available operating time capacity to anticipate for no-shows [29]. Most patients requiring surgical care enter the hospital through the ambulatory care services. Although this makes admission control and capacity allocation policies for both ambulatory and surgical care services interdependent, not much literature is available on the interaction between ambulatory and surgical care services [422].
Methods: computer simulation [ 51, 115, 247, 410], Markov processes [313], mathematical programming [ 3, 4], literature review [ 45, 192].
Staff-shift scheduling
Shifts are hospital duties with a start and end time [65]. Shift scheduling deals with the problem of selecting what shifts are to be worked and how many employees should be assigned to each shift to meet patient demand [141]. The objective of shift scheduling is to generate shifts that minimize the number of staff hours required to cover the desired staffing levels [345]. The desired staffing levels are impacted by the capacity allocation decisions. Hence, integrated decision making for capacity allocation and staff-shift scheduling minimizes required staff [30]. Flexible shifts can improve performance [ 48, 116]. One example is staggered shift scheduling, which implies that employees have varying start and end times of shifts [330]. It can be used to plan varying, but adequate staffing levels during the day, and to decrease overtime [ 48, 116].
Methods: heuristics [112], mathematical programming [ 30, 63, 126], literature review [ 199, 345].
Offline operational planning
Staff-to-shift assignment
In staff-to-shift assignment, a date and time are given to a staff member to perform a particular shift. The literature on shift scheduling and assignment in health care mainly concerns inpatient care services [141], which we address in the section ‘Inpatient care services’.
Methods: no papers found.
Surgical case scheduling
Surgical case scheduling is concerned with assigning a date and time to a specific surgical case. Availability of the patient, a surgeon, an anesthetist, nursing and support staff, and an operating room is a precondition [45]. Surgical case scheduling is an offline operational planning decision, since it results in an assignment of individual patients to planned resources and not in blueprints for assigning surgical cases to particular slots. The objectives of surgical case scheduling are numerous: to achieve a high utilization of surgical and postsurgical resources, to achieve high staff and patient satisfaction, and to achieve low patient deferrals, patient cancellations, patient waiting time and staff overtime [ 72, 107, 150, 235, 289, 341, 361, 379, 441]. The execution of a surgical case schedule is affected by various uncertainties in the preoperative stage duration, surgical procedure duration, switching time, postsurgical recovery duration, emergency patient interruption, staff availability and the starting time of a surgeon [ 192, 341]. These uncertainty factors should be taken into account in surgical case scheduling.
Although surgical case scheduling can be done integrally in one step [ 13, 119, 120, 151, 287, 341, 361, 389], it is often decomposed in several steps. In the latter case, first, the planned length of a surgical case is decided. Second, a date and an operating room are assigned to a surgical case on the waiting list. (also termed the ‘advance scheduling’ [287]). Third, the sequence of surgical cases on a specific day is determined [ 193, 287] (also termed the ‘allocation scheduling’ [287]). Fourth, starting times for each surgical case are determined. Below, we explain these four steps in more detail.
-
Planned length of a surgical case. The planned length of a surgical case is the reserved operating time capacity in the surgical schedule for the surgical case duration, switching time and slack time. Surgical case duration, which is often estimated for each patient individually [327], is impacted by factors as the involved surgeon's experience, and the acuteness, sex and age of the patient [ 113, 327]. Switching time between surgical cases includes cleaning the operating room, performing anesthetic procedures or changing the surgical team [124]. Slack capacity is reserved as a buffer to deal with longer actual surgery durations than expected in advance [201]. When too little time is reserved, staff overtime and patient waiting time occur, and when too much time is reserved, resources incur idle time [ 124, 327, 441].
-
Assigning dates and operating rooms to surgical cases. Dates and operating rooms are assigned to the elective cases on the surgical waiting list, following the settled admission control decisions [ 21, 149, 150, 201, 235, 292, 355]. The available blocks of operating time capacity are filled with elective cases. When too few cases are planned, utilization decreases, leading to longer waiting lists. Conversely, when too many cases are planned, costs increase due to staff overtime [ 51, 355]. Assigning dates and operating rooms to surgical cases can be done by assigning an individual surgical case, or by jointly assigning multiple cases to various possible dates and times. The latter is more efficient as more assignment possibilities can be considered [120].
-
Sequencing of surgical cases. When the set of surgical cases for a day or for a block is known, the sequence in which they are performed still has to be determined. Factors to consider in the sequencing decision are doctor preference [192], medical or safety reasons [ 69, 235], patient convenience [ 69, 70], and resource restrictions [71]. Various rules for sequencing surgical cases are known [ 21, 69, 70, 194, 341, 355, 379]. In general, the traditional first-come-first-serve (FCFS) rule is outperformed by a longest-processing-time-first (LPTF) rule [ 45, 255, 257, 330]. When the variation of surgical case duration is known, sequencing surgical cases in the order of increasing case duration variation (i.e., lowest-variance-first) may yield further improvements [ 108, 441].
-
Assigning starting times to surgical cases. The planned start time of each surgical case is decided [194]. This provides a target time for planning the presurgical and postsurgical resources, and for planning the doctor schedules [441]. The actual start time of a surgical case is impacted by the planned and actual duration of all preceding surgical cases [ 21, 441] and the completion time of the preoperative stage [122].
Emergency cases may play a significant role during the execution of the surgical case schedule [192]. Hence, incorporating knowledge about emergency cases, for example predicted demand, in surgical case scheduling decreases staff overtime and patient waiting time [ 51, 169, 261, 262, 263]. Often, surgical case scheduling is done in isolation. However, efficiency gains may be achieved by also considering decisions in other care services [ 69, 72, 86, 235, 341]. For example, without coordination with the ICU, a scheduled case may be rejected on its day of surgery due to a full ICU [341]. The contributions [ 13, 69, 86, 151, 221, 288, 314, 341, 370] do incorporate other care services, such as the patient wards and ICUs.
Methods: computer simulation [ 10, 51, 86, 114, 117, 119, 120, 123, 145, 194, 255, 257, 261, 262, 370, 403, 441], heuristics [ 10, 13, 71, 108, 113, 149, 151, 193, 194, 221, 261, 263, 292, 355, 361, 389, 418], Markov processes [ 169, 196, 313, 327], mathematical programming [ 13, 21, 69, 70, 71, 80, 86, 106, 107, 108, 149, 150, 151, 193, 235, 261, 262, 263, 289, 292, 339, 341, 355, 361, 379, 402], queueing theory [441], literature review [ 45, 72, 197, 287, 301, 330, 385].
Online operational planning
Emergency case scheduling
Emergency cases requiring immediate surgery are assigned to reserved capacity or to capacity obtained by canceling or delaying elective procedures [420]. It is the objective to operate emergency cases as soon as possible, but also to minimize disturbance of the surgical case schedule [197]. When emergency cases cannot be operated immediately, prioritizing of emergency cases is required to accommodate medical priorities or to minimize average waiting time of emergency cases [ 118, 341].
Methods: mathematical programming [ 118, 341], literature review [197].
Surgical case rescheduling
When the schedule is carried out, unplanned events, such as emergency patients, extended surgery duration and equipment breakdown, may disturb the surgical case schedule [ 3, 289]. Hence, the surgical case schedule often has to be reconsidered during the day to mitigate increasing staff overtime, patient waiting time and resource idle time. Rescheduling may involve moving scheduled surgeries from one operating room to another and delaying, canceling or rescheduling surgeries [289].
Methods: mathematical programming [ 3, 289], literature review [ 196, 197].
Staff rescheduling
At the start of a shift, the staff schedule is reconsidered. Before and during the shift, the staff capacities may be adjusted to unpredicted demand fluctuations and staff absenteeism by using part-time, on-call nurses, staff overtime and voluntary absenteeism [ 191, 342].
Methods: no papers found.
3.4. Inpatient care services
Inpatient care refers to care for a patient who is formally admitted (or ‘hospitalized’) for treatment and/or care and stays for a minimum of one night in the hospital [325]. Owing to progress in medicine inpatient stays have been shortened, with many admissions replaced by more cost-effective outpatient procedures [ 324, 330]. Resource capacity planning has received much attention in the OR/MS literature, with capacity dimensioning being the most prominently studied decision.
Strategic planning
Regional coverage
At a regional planning level, the number, types and locations of inpatient care facilities have to be decided. To meet inpatient service demand, the available budget needs to be spent such that the population of each geographical area has access to a sufficient supply of inpatient facilities of appropriate nature and within acceptable distance [56]. Coordinated regional coverage planning between various geographical areas supports the realization of equity of access to care [ 43, 364]. To achieve this, local and regional bed occupancies need to be balanced with the local and regional probability of admission refusals resulting from a full census. The potential pitfall of deterministic approaches as used in [364] is that resource requirements are underestimated and thus false assurances are provided about the expected service level to patients [209].
Methods: computer simulation [209], mathematical programming [ 56, 364], queueing theory [43].
Service mix
The service mix is the set of services that health care facilities offer. health care facilities that offer inpatient care services can provide a more complex mix of services and can accommodate patient groups with more complex diagnoses [385]. In general, the inpatient care service mix decision is not made at an inpatient care service level, but at the regional or hospital level, as it integrally impacts the ambulatory care facilities, the operating theater and the wards. This may be the reason that we have not found any references focusing on service mix decisions for inpatient care services in specific.
Methods: no papers found.
Case mix
Given the service mix decision, the types and volumes of patients that the facility serves need to be decided. The settled service mix decision restricts the decisions to serve particular patient groups. Patient groups can be classified based on disease type, demographic information and resource requirements [190]. In addition, whether patient admissions are elective or not is an influential characteristic on the variability of the operations of inpatient care services [414]. The case mix decision influences almost all other decisions, in particular the care unit partitioning and capacity dimensioning decisions [24].
Methods: computer simulation [190], heuristics [ 24, 414].
Care unit partitioning
Given the service and case mix decisions, the hospital management has to decide upon the medical care units in which the inpatient care facility is divided. We denote this decision as care unit partitioning. It addresses both the question which units to create and the question which patient groups to consolidate in such care units. Each care unit has its designated staff, equipment and beds (in one or more wards). The objective is to guarantee care from appropriately skilled nurses and required equipment to patients with specific diagnoses, while making efficient use of scarce resources [ 24, 132, 133, 176, 209, 216, 374, 430].
First, the desirability of opening shared higher-level care units like Intensive Care Units (ICU) or Medium Care Units (MCU) should be considered [412]. Second, the general wards need to be specified. Although care unit partitioning is traditionally done by establishing a care unit for each specialty, or sometimes even more diagnosis specific [385], specialty-based categorization is not necessarily optimal. Increasingly, the possibilities and implications of consolidating inpatient services for care related groups is investigated to gain from the economies-of-scale effect, so-called ‘pooling’ [450]. For example, many hospitals merge the cardiac and thoracic surgery unit [186], or allow gynecologic patients in an obstetric unit during periods of low occupancy [303]. In such cases, the overflow rules need to be specified on the tactical level. For geriatric departments, it has to be decided whether to separate or consolidate assessment, rehabilitation and long-stay care [ 307, 308]. Also, multi-specialty wards can be created for patients of similar length of stay, such as day-care, short, week- and long-stay units [ 374, 430], or for acute patients [ 224, 414]. Concentrating emergency activities in one area (a Medical Assessment Unit) can improve efficiency and minimize disruption to other hospital services [323]. One should be cautious when pooling beds for patient groups with diverging service level [186] or nursing requirements [264]. A combined unit would require the highest service and nurse staffing level for all patient groups. As a result, acceptable utilization may be lower than with separate units. Also, pooling gains should be weighed against possible extra costs for installing extra equipment on each bed [264]. To conclude, the question whether to consolidate or separate clinical services from a logistical point of view is one that should be answered for each specific situation, considering demand characteristics but also performance preferences and requirements [209]. Obviously, the care unit partitioning decision is highly interrelated with the capacity dimensioning decisions, to be discussed next.
Methods: computer simulation [ 132, 133, 176, 209, 224, 374], heuristics [ 24, 264, 414], mathematical programming [323], queueing theory [ 186, 216, 303, 307, 308, 412, 450].
Capacity dimensioning
In conjunction with the care unit partitioning, the size of each care unit needs to be determined. Care unit size is generally expressed in the number of staffed beds, as this number is often taken as a guideline for dimensioning decisions for other resources such as equipment and staff.
-
Beds. The common objective is to dimension the number of beds of a single medical care unit such that occupancy of beds is maximized while a predefined performance norm is satisfied [ 178, 319, 321, 354, 428, 447]. The typical performance measure is the percentage of patients that have to be rejected for admission due to lack of bed capacity: the admission refusal rate. Several other consequences of congested wards can be identified, all being a threat to the provided quality of care. First, patients might have to be transferred to another hospital in case of an emergency [ 92, 248, 297, 452]. Second, patients may (temporarily) be placed in less appropriate units, so-called misplacements [ 96, 132, 133, 186, 208, 213, 452]. Third, backlogs may be created in emergency rooms or surgical recovery units [ 88, 176, 186, 322, 323]. Fourth, elective admissions or surgeries may have to be postponed, by which surgical waiting lists may increase [ 7, 96, 178, 451, 452], which negatively impacts the health condition of (possibly critical) patients [ 410, 416]. Finally, to accommodate a new admission in critical care units, one may predischarge a less critical patient to a general ward [ 129, 445]. The number of occupied beds is a stochastic process, because of the randomness in the number of arrivals and lengths of stay [251]. Therefore, slack capacity is required and thus care units cannot operate at 100% utilization [ 102, 186]. Often, inpatient care facilities adopt simple deterministic spreadsheet calculations, leading to an underestimation of the required number of beds [ 88, 96, 102, 204, 209]. Hospitals commonly apply a fixed target occupancy level (often 85%), by which the required number of beds is calculated. Such a policy may result in excessive delays or rejections [ 17, 186, 209, 251, 319]. The desirable occupancy level should be calculated as a complex function of the service mix, the number of beds and the length of stay distribution [ 208, 209]. This nonlinear relationship between number of beds, mean occupancy level and the number of patients that have to be rejected for admission due to lack of bed capacity is often emphasized [ 7, 102, 208, 213, 251, 319, 320, 354]. In determining the appropriate average utilization, the effect of economies-of-scale due to the so-called portfolio effect plays a role: larger facilities can operate under a higher occupancy level than smaller ones in trying to achieve a given patient service level [ 186, 209, 210, 251], since randomness balances out. However, possible economies of scope due to more effective treatment or use of resources should not be neglected [186]. Units with a substantial fraction of scheduled patients can in general operate under a higher average utilization [186]. The effect of variability in length of stay on care unit size requirements is shown to be less pressing than often thought by hospital managers [ 186, 416]. Reducing the average length of stay shows far more potential. For care units that have a demand profile with a clear time-dependent pattern, these effects are preferably explicitly taken into account in modeling and decision making, to capture the seasonal [ 213, 286], day-of-week [ 129, 162, 213, 223] and even hour-of-day effects [ 27, 62, 88, 208]. This especially holds for units with a high fraction of emergencies admissions [385]. Capacity decisions regarding the size of a specific care unit can affect the operations of other units. Therefore, the number of beds needs to be balanced among interdependent inpatient care units [ 7, 60, 88, 89, 190, 209, 216, 224, 278, 297, 385]. Models that consider only a single unit neglect the possibility of admitting patients in a less appropriate care unit and thus the interaction between patient flows and the interrelationship between care units. Next to estimating utilization and the probability of admission rejections or delays, models that do incorporate multiple care units, also focus on the percentage of time that patients are placed in a care unit of a lower level or less appropriate care unit, or in a higher level care unit [ 11, 92, 172, 186, 278, 374]. The first situation negatively impacts quality of care as it can lead to increased morbidity and mortality [410] and the second negatively impacts both quality of care, as it may block admission of another patient, and efficient resource use [ 186, 374]. Some multi-unit models explicitly take the patient's progress through multiple treatment or recovery stages into account and try to dimension the care units such that patients can in each stage be placed in the care units that are most suitable regarding their physical condition [ 88, 92, 102, 146, 166, 171, 206, 211, 212, 224, 297, 374, 412].
-
Equipment. In [430], it is stated that pooling equipment among care units can be highly beneficial. However, no references have been found explicitly focusing on this planning decision. This might be explained by the fact that the care unit partitioning and size decisions are generally assumed to be translatable to equipment capacity requirements. Therefore, many of the references mentioned under these decisions are useful for the capacity dimensioning of equipment.
-
Staff. The highest level of personnel planning is the long-term workforce capacity dimensioning decision. This decision concerns both the number of employees that have to be employed, often expressed in the number of full time equivalents, and the mix in terms of skill categories [ 207, 322]. For inpatient care services it mainly concerns nursing staff. To deliver high-quality care, the workforce capacity needs to be such that an appropriate level of staff can be provided in the different care units in the hospital [ 141, 172]. In addition, holiday periods, training, illness and further education need to be addressed [65]. Workforce flexibility is indicated as a powerful concept in reducing the required size of workforce [ 65, 104, 172, 385]. To adequately respond to patient demand variability and seasonal influences, it pays off to have substitution possibilities of different employee types, to use overtime, and to use part-time employees and temporary agency employees [385]. Just as with pooling bed capacity, economies-of-scale can be gained when pooling nursing staff among multiple care units. Nurses cross-trained to work in more than one unit can be placed in a so-called floating nurse pool [ 65, 172, 264, 385]. Note that flexible staff can be significantly more expensive [191]. Also, [271] indicates that to maintain the desired staff capacity, it is necessary to determine the long-term human resource planning strategies with respect to recruiting, promotion and training. To conclude, integrating the staff capacity dimensioning decision with the care unit size decision yields a significant efficiency gain [172].
Methods: computer simulation [ 7, 17, 88, 92, 96, 132, 133, 176, 190, 191, 204, 207, 208, 209, 210, 224, 248, 251, 297, 319, 320, 321, 322, 354, 374, 410, 428, 445, 447, 451, 452], heuristics [264], Markov processes [ 7, 62, 146, 166, 171, 211, 212, 213, 286], mathematical programming [ 104, 172, 207, 271, 278, 322, 323], queueing theory [ 11, 27, 60, 88, 89, 102, 129, 162, 178, 186, 206, 216, 223, 248, 278, 354, 412, 416], literature review [ 65, 141, 342, 385].
Facility layout
The facility layout concerns the positioning and organization of different physical areas in a facility. To determine the inpatient care facility layout, it needs to be specified which care units should be next to each other [330] and which care units should be close to other services like the surgical, emergency and ambulatory care facilities [67]. Ideally, the optimal physical layout of an inpatient care facility is determined given the decisions on service mix, case mix, care unit partitioning and care unit size. However, in practice, it often happens vice versa: physical characteristics of a facility constraint service mix, care unit partitioning and care unit size decisions [ 67, 430]. Newly built hospitals are preferably designed such that they support resource pooling and have modular spaces so that they are as flexible as possible with respect to care unit partitioning and dimensioning [430].
Methods: computer simulation [67], heuristics [330], mathematical programming [67].
Tactical planning
Bed reallocation
Given the strategic decision making, tactical resource allocation needs to ensure that the fixed capacities are employed such that inpatient care is provided to the right patient groups at the right time, while maximizing resource utilization. Bed reallocation is the first step in tactical inpatient care service planning. Medium-term demand forecasts may expose that the care unit partitioning and size decisions fixed at the strategic level are not optimal. If the ward layout is sufficiently flexible, a reallocation of beds to units or specialties based on more specific demand forecast can be beneficial [ 24, 208, 431]. In addition, demand forecasts can be exploited to realize continuous reallocation of beds in anticipation for seasonality in demand [242]. To this end, hospital bed capacity models should incorporate monthly, daily and hourly demand profiles and meaningful statistical distributions that capture the inherent variability in demand and length of stay [204]. When reallocating beds, the implications for personnel planning, and involved costs for changing bed capacity, should not be overlooked [6].
Methods: computer simulation [ 208, 242], heuristics [ 24, 431], mathematical programming [6], queueing theory [242].
Temporary bed capacity change
To prevent superfluous staffing of beds, beds can temporarily be closed by reducing staff levels [186]. This may for instance be in response to predicted seasonal or weekend demand effects [ 204, 210]. The impact of such closings on the waiting lists at referring outpatient clinics and the operating room is studied by [ 450, 451]. Temporary bed closings may also be unavoidable as a result of staff shortages [297]. In such cases hospitals can act pro-actively, to prevent bed closings during peak demand periods [24].
Methods: computer simulation [ 204, 210, 297, 451], heuristics [24], queueing theory [ 186, 450].
Admission control
To provide timely access for each different patient group, admission control prescribes the rules according to which various patients with different access time requirements are admitted to nursing wards. At this level, patients are often categorized in elective, urgent and emergency patients. Admission control policies have the objective to match demand and supply such that access times, rejections, surgical care cancellations and misplacements are minimized while bed occupancy is maximized. The challenge is to cope with variability in patient arrivals and length of stay. Smoothing patient inflow, and thus workload at nursing wards, prevents large differences between peak and non-peak periods, and so realizes a more efficient use of resources [ 4, 204, 432].
Patient resource requirements are another source of variability in the process of admission control. Most references only focus on maximizing utilization of bed resources. This may lead to extreme variations in the utilization of other resources like diagnostic equipment and nursing staff [385]. Also, as with temporarily closing of beds, possible effects of admission control policies on the waiting lists at referring outpatient clinics and the operating room should not be neglected [378]. Admission control policies can be both static (following fixed rules) and dynamic (changing rules responding to the actual situation).
-
Static bed reservation. To anticipate for the estimated inflow of other patient groups, two types of static bed reservation can be distinguished. The first is refusing admissions of a certain patient type when the bed census exceeds a threshold. For example, to prevent the rejection of emergent admission requests, an inpatient care unit may decide to suspend admissions of elective patients when the number of occupied beds reaches a threshold [ 142, 163, 232, 243, 297, 303, 354, 378]. As such, a certain number of beds is reserved for emergency patients. This reservation concept is also known as ‘earmarking’. Conversely, [ 249, 410] indicate that earmarking beds for elective postoperative patients can minimize operating room cancellations. In the second static level the number of reserved beds varies, for example per weekday. Examples of such a policy are provided in [42], and [413] in which for each work day a maximum reservation level for elective patients is determined.
-
Dynamic bed reservation. Dynamic bed reservation schemes take into account the actual ‘state’ of a ward, expressed in the bed census per patient type. Together with a prediction of demand, the reservation levels may be determined for a given planning horizon [252] or it may be decided to release reserved beds when demand is low. Examples of the latter are found in [249], where bed reservations for elective surgery are released during weekend days, and [28], where admission quota are proposed per weekday. In [214], an extension to dynamic reservation is proposed which concerns calling in semi-urgent patients from an additional waiting list on which patients are placed who needs admission within 1–3 days.
-
Overflow rules. In addition to the bed reservation rules, overflow rules prescribe what happens in the case that all reserved beds for a certain patient type are occupied. In such cases, specific overflow rules prescribe which patient types to place in which units [209]. Generally, patients are reassigned to the correct treatment area as soon as circumstances permit [385]. By allowing overflow and setting appropriate rules, the benefits of bed capacity pooling are utilized (see capacity dimensioning: care unit size), while the alignment of patients with their preferred bed types is maximized [297]. Various references focus on predicting the impact of specific overflow rules [ 180, 209, 216, 297, 374].
-
Influence surgical schedule. For many inpatient care services the authority on admission control is limited due to the high dependency on the operating room schedule (see surgical care services). By adjusting the surgical schedule, extremely busy and slack periods can be avoided [ 4, 24, 129, 132, 145, 180, 186, 204, 402, 423, 424, 431, 432, 452] and cancellation of elective surgeries can be avoided [247]. In practice, the operating room planning is generally done under the assumption that a free bed is available for postoperative care [249], which may result in surgery cancellations. Therefore, both for inpatient and surgical care services coordinated planning is beneficial [ 3, 204].
Methods: computer simulation [ 3, 132, 145, 180, 204, 209, 247, 249, 297, 354, 374, 402, 410, 432, 452], heuristics [ 24, 431], Markov processes [ 42, 142, 214, 216, 252, 423, 424], mathematical programming [ 3, 4, 28, 402], queueing theory [ 28, 129, 163, 186, 232, 243, 303, 378, 413].
Staff-shift scheduling
Shifts are hospital duties with a start and end time [65]. Shift scheduling deals with the problem of selecting what shifts are to be worked and how many employees should be assigned to each shift to meet patient demand [ 141, 246]. For inpatient care services, it generally concerns the specification of 24-h-a-day-staffing levels divided in a day, evening and night shift, during which demand varies considerably [ 65, 141]. Typically, this is done for a period of one or two months [342]. Staffing levels need to be set both for each care unit's dedicated nurses and for flexible staff in floating pools [264]. Also, [ 104, 191] investigate the potential of on-call nurses who are planned to be available during certain shifts and only work when required.
The first step in staff shift scheduling is to determine staffing requirements with a demand model [ 141, 199, 246, 396], based on which the bed occupancy levels [385] and medical needs are forecasted [264]. The second step is to translate the forecasted demand in workable shifts and in the number of nurses to plan per shift, taking into account the staff resources made available at the strategic decision level [437]. Often, nurse-to-patient ratios are applied in this step [191], which are assumed to imply acceptable levels of patient care and nurse workload [453]. To improve the alignment of care demand and supply, shift scheduling is preferably coordinated with scheduled admissions and surgeries [342], which also helps avoiding high variation in nurse workload pressure [30].
Methods: computer simulation [191], heuristics [264], mathematical programming [ 30, 104, 437, 453], queueing theory [396], literature review [ 65, 141, 199, 246, 342, 385].
Offline operational planning
Admission scheduling
Governing the rules set by tactical admission control policies, on the operational decision level the admission scheduling determines for a specific elective patient the time and date of admission. We found one reference on this decision: [95] presents a scheduling approach to schedule admissions for a short-stay inpatient facility that only operates during working days, which takes into account various resource availabilities such as beds and diagnostic resources. We suggest two reasons for the lack of contributions on this decision. First, when admission control policies are thoroughly formulated, admission scheduling is fairly straightforward. Second, as described before, for postoperative inpatient care authority of admission planning is generally at the surgical care services [431].
Methods: mathematical programming [95].
Patient-to-bed assignment
Together with the admission scheduling decision, an elective patient needs to be assigned to a specific bed in a specific ward. Typically, this assignment is carried out a few days before the effective admission of the patient. The objective is to match the patient with a bed, such that both personal preferences (for example a single or twin room) and medical needs are satisfied [ 79, 105]. An additional objective may be to balance bed occupancy over different wards.
Methods: heuristics [ 79, 105], mathematical programming [ 79, 105].
Discharge planning
Discharge planning is the development of an individualized discharge plan for a patient prior to leaving the hospital. It should ensure that patients are discharged from the hospital at an appropriate time in their care and that, with adequate notice, the provision of other care services is timely organized. The aim of discharge planning is to reduce hospital length of stay and unplanned readmission, and improve the coordination of services following discharge from the hospital [376]. As such, discharge planning is highly dependent on availability downstream care services, such as rehabilitation, residential or home care. Therefore, a need is identified for integrated coherent planning across services of different health care organizations [ 426, 442]. Patients whose medical treatment is complete but cannot leave the hospital are often referred to as ‘alternative level of care patients’ or ‘bed blockers’ [ 422, 442]. Also in discharge planning it is worthwhile to anticipate for seasonality effects.
Methods: computer simulation [426], queueing theory [442], literature review [376].
Staff-to-shift assignment
Staff-to-shift assignment deals with the allocation of staff members to shifts over a period of several weeks [141]. The term ‘nurse rostering’ is also often used for this step in inpatient care services personnel planning [ 65, 84]. The objective is to meet the required shift staffing levels set on the tactical level, while satisfying a complex set of restrictions involving work regulations and employee preferences [ 40, 65, 84, 234, 246, 415]. Night and weekend shifts, days off and leaves have to be distributed fairly [ 342, 385, 453] and as much as possible according to individual preferences [ 40, 141]. In most cases, to compose a roster for each individual, first sensible combinations or patterns of shifts are generated (cyclic or non-cyclic), called ‘lines-of-work’, after which individuals are assigned to these lines-of-work [141]. Sometimes, staff-to-shift assignment is integrated with staff-shift scheduling [ 65, 453]. ‘Self-scheduling’ is an increasingly popular concept aimed at increased staff satisfaction which allows staff members to first propose individual schedules, which are taken as starting point to create a workable schedule that satisfies the staffing level requirement set on the tactical level [362].
Methods: heuristics [ 40, 415], mathematical programming [ 40, 234, 362, 415, 453], literature review [ 65, 84, 141, 246, 342, 385].
Online operational planning
Elective admission rescheduling
Based on the current status of both the patient and the inpatient care facility, it has to be decided whether a scheduled admission can proceed as planned. Circumstances may require postponing or canceling the admission, to reschedule it to another care unit, or to change the bed assignment. Various factors will be taken into consideration such as severity of illness, age, expected length of stay, the probable treatment outcome, the (estimated) bed availability, and the conditions of other patients (in view of the possibility of predischarging an other patient) [ 248, 282, 377]. This decision is generally made on the planned day of admission or a few days in advance. Rescheduling admissions can have a major impact on the operations at the surgical theater [248].
Methods: computer simulation [248], heuristics [282], queueing theory [ 248, 377].
Acute admission handling
For an acute admission request it has to be decided whether to admit the emergency patient and if so to which care unit, which bed, and on what notice. The tactical admission control rules act as guideline. As with rescheduling elective admissions, the status of both the patient and the inpatient care facility are taken into account [ 248, 377]. In [248], it is calculated how long the waiting will be if the patient is placed on ‘the admission list’ and [377] proposes and evaluates an admission policy to maximize the expected incremental number of lives saved from selecting the best patients for admission to an ICU.
Methods: computer simulation [248], queueing theory [ 248, 377].
Staff rescheduling
At the start of a shift, the staff schedule is reconsidered. Based on severity of need in each care unit, the float nurses and other flexible employees are assigned to a specific unit and a reassignment of dedicated nurses may also take place [ 65, 385]. In addition, before and during the shift, the staff capacities among units may be adjusted to unpredicted demand fluctuations and staff absenteeism by using float, part-time, on-call nurses overtime and voluntary absenteeism [ 191, 342].
Methods: computer simulation [191], mathematical programming [347], literature review [ 65, 342, 385].
Nurse-to-patient assignment
At the beginning of each shift, each nurse is assigned to a group of patients to take care for. This assignment is done with the objective to provide each patient with an appropriate level of care and to balance workloads [ 315, 390]. Distributing work fairly among nurses improves the quality of care [315]. Generally, the assignment has to satisfy specified nurse-to-patient ratios [347]. Additionally, when patient conditions within one care unit can differ considerably, for each specific patient an estimate of the severity of the condition (and thereby expected workload) is made, in most cases on the basis of a certain severity scoring system [315]. In [347], it is explicitly taken into account that patient conditions, and therefore care needs, can vary during a shift. They state that it is preferred to also decide at the beginning of each shift to which nurse(s) unanticipated patients will be assigned.
Methods: computer simulation [390], heuristics [315], mathematical programming [ 315, 347].
Transfer scheduling
Throughout the inpatients’ stay, the transfer scheduling is done to the appropriate inpatient care unit or to other areas within the hospital for treatments or diagnoses [342]. Transfer scheduling includes the planning of transportation. Transfer scheduling is often postponed until the time an already occupied bed is requested by a new patient. However, in [405] it is concluded that when relocation of patients is done proactively, admission delays for other patients can significantly be reduced, which has a positive effect on both quality and efficiency.
Methods: Markov processes [405].
3.5 Home care services
Home care includes medical, paramedical and social services delivered to patients at their homes [268]. It represents an alternative for hospitalization or placement in a residential care facility [34]. Home care services are a growing sector in the health care domain [ 34, 81], which might be because it is in general less costly [268] and it has a positive effect on a patient's quality of life [144]. Their development is accelerated by factors such as the ageing of the population, the increase of chronic diseases, the introduction of innovative technologies and the continuous pressure of governments to contain health care costs [ 34, 81, 144]. Home care is provided in multi disciplinary teams, since patients typically have a mixture of social, physical, psychological needs, and home care professionals may carry out several patient visits during a day. This diversity, multi-disciplinarity and the fact that the patient's home has to be integrated in the care supply chain makes the resource planning of home care delivery complex [ 34, 81, 268]. Coordination between the various disciplines is required to ensure continuity of care and to prevent overlap of care [34].
The body of OR/MS literature focusing on home care resource capacity planning in health care is not extensive compared with other care services. A single review was available [34], which has been a valuable starting point for the taxonomic overview in this section. It has been noted in the literature that due to the nature of home care services, intelligent portable electronic devices have a high potential in supporting home care organization and they are more and more used [ 26, 144]; recall that ICT solutions are not the focus of our review.
Strategic planning
Placement policy
The placement policy decision prescribes which patient types are eligible for home care services, and which are preferably admitted to an inpatient or residential care facility. The aim is to provide patients with the right treatment at the right time in the most cost-effective manner [457]. Defining placement policies requires classification systems by which health status and type of care requirements can be assessed [ 268, 457]. Often, for a single patient there are multiple alternatives for what type of care facility is best suitable. Optimal placement involves the consideration whether or not to treat a patient in a hospital bed, and at which point during recovery a patient is transferred from hospital care to home care [ 81, 457]. This makes coordination of inpatient, residential and home care resource capacities desirable [34].
Methods: heuristics [457], Markov processes [268], mathematical programming [81], literature review [34].
Regional coverage
At a regional planning level, the number, types and locations of home care agencies are decided. Unlike hospitals, which cater to a population not constrained to a specific area, home care agencies are generally responsible for the population in a given area, possibly assigned by the government [ 44, 260]. To meet home care service demand, the available budget needs to be spent such that the population in the area has access to a sufficient supply of home care services. Since care is delivered at a patient's home, the distance between agencies is only a provider efficiency issue, and does not affect patient accessibility [34]. No specific contributions to regional coverage planning in home care have been found.
Methods: literature review [34].
Service mix
A home care organization has to decide which services to offer. With respect to home care services, [144] distinguishes home care and home health care. Home care involves helping patients with everyday activities, such as bathing, dressing, eating, cooking, cleaning, and monitoring the daily medication regime. Home health care involves helping patients recover from an illness or injury. Therefore, home health care is often provided by registered nurses, therapists and home health assistants. Another service is that of social and emotional support to patients and their family [34]. Home care services solely involving medication or meal distribution are outside the scope of our review, as these are secondary services. All found contributions treat the service mix decision as given in their models.
Methods: literature review [34].
Case mix
Aligned with the service mix, an organization needs to determine the types and volumes of patients it will serve. Patient types can be grouped according to pathology or to required type of care [ 34, 144]. Based on duration and content of care, [34] distinguishes four types of care: punctual care, continuous care, palliative care, rehabilitation care. For home care, the variety of required care in type, frequency and time is substantial [ 34, 101]. Therefore, almost all other planning decisions are geared to the case mix. However, as with the service mix decision, all found contributions treat this decision as given.
Methods: literature review [34].
Panel size
The panel size, also called calling population, is the number of potential patients of a home care facility. Since only a fraction of these potential patients actually demands home care services, the panel size can be larger than the number of patients a facility can serve. The goal is to set the panel size such that a minimum standard of service is ensured, while making efficient use of available resources [101], where service is typically measured in access time and efficiency in staff utilization. To achieve this, future care needs originating from the potential patients have to be forecasted. The panel size decision is closely connected to the regional coverage and districting decisions.
Methods: mathematical programming [101].
Districting
Districting involves the partitioning into districts of the area in which an organization is responsible for the logistics of home care visits. Typically, each district falls under the responsibility of one multi-disciplinary care team [ 34, 44]. Districting is done to limit the travel distances and times of care providers between the homes of patients, to improve coordination between different care providers treating the same patient and to encourage long-term relationships between providers and patients [ 34, 144]. Although these reasons plead for small districts, the districts should not be too small, to avoid inefficient operations [44]. Also, the objective of balancing workload among the districts in an area can be taken into account [44].
Methods: heuristics [44], literature review [34].
Capacity dimensioning
Home care organizations dimension their resources, to spend the available budget such that a satisfactory quality of care is realized and access times are minimized [ 34, 66]. To this end, provider capacity must be matched with patient demand. Since individual home care is in general a long-term process, the capacity dimensioning decision also requires long-term demand forecast models based on demographic information [ 202, 417]. In Lahrichi et al [260], it is indicated that true care needs are hard to estimate as care demands stored in historical data tend to be biased by the realized (un)availability of services. Capacity is dimensioned for the following resource types:
-
Staff. Many health care professionals are involved in home care delivery, including nurses, occupational therapists, physiotherapists, speech therapists, nutritionists, home support workers, social workers, physicians and pharmacists [ 66, 260]. For each skill category it is determined whether to employ staff or to (temporarily) hire staff from an external agency when required [34]. Where usually professionals are dedicated to a fixed district, flexibility to respond to fluctuating demand can be achieved by allowing care providers to work in more than one district [260].
-
Equipment. Medical and paramedical equipment and information technology equipment can be involved in providing home care [34]. Sharing resources among multiple districts may induce cost savings [332].
-
Fleet vehicles. Means of transport, rented or bought, are required for visiting patients [34].
When capacity is dimensioned to cover average demand, variations in demand may cause long access times. Basic rules from queueing theory demonstrate the necessity of excess capacity to cope with uncertain demand [66]. Variation arises not only from uncertainty in the arrival process of care requests but also from the different levels of care required per patient [34]. The multi-disciplinary nature of home care causes a diversity of resources to be involved. Therefore, the capacity dimensioning decisions for different resource types are highly interrelated and performance is improved when these decisions are aligned. If dimensions are not properly balanced, some resources may become bottlenecks, while at the same time others are underutilized [ 34, 66].
Methods: computer simulation [ 332, 417], Markov processes [202], queueing theory [66], literature review [34].
Tactical planning
Capacity allocation
On the tactical level, resource capacities settled on the strategic level are subdivided over districts and patient groups. The objective is to equitably allocate resources: workload, access times and quality of care (for example measured in number of visits per patient) should be balanced over districts and patient groups [ 66, 101]. Capacity allocation requires two steps:
-
Patient group identification. Patients are classified by medical urgency or resource requirements [ 34, 66].
-
Time subdivision. Capacity subdivision is provided in the number of care hours available per discipline per district [ 101, 260]. Time subdivision can be done based on number of inhabitants per district. However, [49] proposes to use a detailed demand estimation per patient group, taking into account demographical information including age and gender distributions.
To accurately respond to demand fluctuations, a dynamic subdivision of capacity, updated based on current waiting lists, already planned visits and expected requests for appointments, performs better than a static one [ 101, 260]. Finally, a close cooperation with other health organizations such as residential and inpatient care services may yield better future demand predictions [34].
Methods: heuristics [ 49, 260], mathematical programming [101], queueing theory [66], literature review [34].
Admission control
Admission control involves the rules according to which patients are selected to be admitted to home care services from the waiting lists. Admission control policies have the objective to match demand and supply such that access times are minimized while resource utilization is maximized, taking into account resource availability, current waiting lists and expected demand.
Clearly, admission control and capacity allocation are interrelated. Patient needs and available resources must be balanced to prevent poor service levels or staff overutilization [101]. The challenge in admission control is to cope with various sources of variability such as variation in patient arrivals, patient home locations, urgency, number of visits per week per discipline required, patient health conditions and treatment durations [101].
Multiple waiting lists are created based on geographical area and patient groups [66]. To provide timely access for each urgency class, patients are typically categorized in several priority groups within a waiting list [66]. A possible admission policy is to always take the patient with highest priority into service whenever capacity becomes available [66]. Another option is to develop an admission plan that prescribes how many patients of each patient group are taken into service during a certain planning horizon. The latter has the potential to simultaneously decrease access times and increase resource utilizations on the long run [101]. Incorporating forecasts of future care pathways of patients already in service and of patients on the waiting list can also improve performance [ 101, 268]. Finally, [217] and [260] signify that when case load is high in one district while another district is (temporarily) underutilized, it is beneficial to allow the flexibility of dynamic admissions over district borders.
Methods: Markov processes [268], mathematical programming [ 101, 217], queueing theory [66].
Staff-shift scheduling
Shifts are duties with a start and end time [65]. Shift scheduling deals with the problem of selecting what shifts are to be worked and how many employees should be assigned to each shift to meet patient demand [141]. Staffing levels per discipline and per district need to be such that feasible operational plans can be generated [34]. Shifts for various disciplines need to be synchronized to accommodate simultaneous visits [81] and to facilitate interdisciplinary team meetings [34]. By staffing a surplus team of which the members are able to work in whichever district that is required, the home care organization is able to respond to temporary demand fluctuations, and unplanned staff absence due to sickness [260].
Methods: heuristics [260], literature review [34].
Offline operational planning
Assessment and intake
Upon a home care request, first an assessment and intake process takes place. This process consists of assessing the patient's eligibility for home care, determining the care requirements and assigning a reference care provider. The eligibility is determined based on the strategic placement policy, together with specific personal characteristics, among which the social situation of the patient. The latter is also an important factor in the estimation of the patient's needs, since for example family assistance can reduce demands for professional support [ 34, 383]. The patient's health status and social situation are very specific, hence customized care programs are required [81]. Determining care requirements is in this phase done at an aggregate level, for example in hours per care type per week [144]. This is not only important from a patient's point of view, but also for the home care organization, as it dictates resource requirements on the short term [268]. Estimating a patient's care pathway and possible variation herein facilitates forecasting resource requirements on the medium term [268]. The reference care provider, also called case manager [81], is responsible for coordination of the entire multidisciplinary treatment [34]. Based on the resource requirements estimation, the reference care provider assignment can be done such that case load is balanced among home care employees [ 34, 217]. Inter-organizational coordination in the assessment and intake process is crucial to know about a patient arrival in an early phase [457]. This promotes continuity of care between discharge at inpatient and residential care facilities and admission to home care services [ 34, 81].
Methods: heuristics [ 383, 457], Markov processes [268], mathematical programming [ 81, 144, 217], literature review [34].
Staff-to-shift assignment
Staff-to-shift assignment deals with the allocation of staff members to shifts over a period of several weeks [141]. The objective is to meet the required shift staffing levels set on the tactical level, while satisfying a complex set of restrictions involving work regulations and employee preferences [65]. Weekend shifts, days off and leaves have to be distributed fairly [ 342, 385] and as much as possible according to individual preferences [141], which include working times, preferential days, vacation and performing particular care activities [34]. The decision is often integrated with visit scheduling [ 38, 144], the decision that is discussed next.
Methods: heuristics [ 38, 144], mathematical programming [ 38, 144], literature review [34].
Visit scheduling
Visit scheduling determines which visit will be performed, on which day and time, and by which staff member. It consists of two components: creating detailed care plans per patient, and the appointment scheduling. This visit scheduling is complex, since all patients have to be treated individually at their own home. Therefore, all tasks have to be planned in advance and synchronization of all human and material resources is required [ 34, 81]. Visit scheduling consists of three components:
-
Short-term care plan. For each patient it has to be determined when, which visits by which care disciplines are (medically) necessary [ 26, 34, 143, 144, 217, 268].
-
Staff-to-visit assignment. Each visit has to be assigned to a certain staff member [ 26, 34, 38, 59, 143, 144, 217, 268].
-
Route creation. For each care provider individual routes are constructed that determine at which day and what time each visit will be done [ 26, 34, 38, 59, 57, 58, 81, 143, 144].
Since the three components are highly interdependent, an integrated approach is required to determine the complete visit schedule all at once [ 26, 38, 81, 143, 144]. It may even be necessary to integrate the staff-to-shift assignment decision [ 38, 143, 144]. This integration of different planning and scheduling decisions makes home care operational planning also mathematically difficult [ 26, 38, 143, 144]. Typically, a visit base plan is made a few weeks in advance for a planning horizon of several weeks, which assigns specific visits to specific weekly time buckets. Then, around a week in advance the detailed visit schedule is established [ 26, 143, 144]. A wide set of constraints needs to be satisfied, like provider skill qualifications, working hours, geographical coherence between the district of patient and staff member, and allowed time windows for each visit [ 26, 34, 38, 57, 58, 143, 144]. In addition, precedence and synchronization requirements need to be satisfied, since some patients need simultaneous or sequential tasks requiring multiple resources [ 26, 59]. Also, the uncertainty of travel times and visit durations needs to be taken into account [34]. The goal is to design visit schedules that are efficient in terms of minimizing labor costs, travel time and distance [ 26, 57, 58, 59, 81] and such that preferences of both patient and providers are considered. Preferences of patients include preferential days, preferred staff, minimize unplanned visits and continuity of care reflected in same day, same time and same staff [ 26, 38, 59, 143, 144]. Staff preference mainly concerns equity of workload, expressed in visit load and travel load [ 26, 143, 144, 217]. Workload imbalance can be reduced by allowing temporary deployment of staff outside their own district [ 26, 217].
Methods: heuristics [ 26, 38, 57, 58, 143, 144], Markov processes [268], mathematical programming [ 26, 38, 57, 58, 59, 81, 143, 144, 217], literature review [34].
Online operational planning
Visit rescheduling
The visit schedule is updated a few days in advance, the day in advance and on the day of execution itself. Rescheduling is required to respond to unplanned events such as unplanned staff absenteeism, changed visit requirements due to changed patient health conditions, and incoming urgent care requests [ 26, 143, 144, 409]. It involves integrally rescheduling care plans, staff rescheduling and rerouting [ 26, 143, 144]. One has to decide whether to arrange staff replacements (internally or externally) or to fit additional tasks into the routes of the available staff, and whether to postpone some less time-critical tasks to a later day. Weather conditions such as snowfalls, floods or storms, can be a source for the necessity of visit rescheduling [409].
Methods: heuristics [ 26, 143, 144, 409], mathematical programming [ 26, 143, 144, 409].
Residential care services
Residential care services cover a range of health care services for patients, often elderly, who have acute, chronic, palliative or rehabilitative health care needs that do not allow them to stay at home, but who do not strictly require a hospital stay [202]. Making residential care available to such patients avoids long-term hospital admissions, which are in general more costly [22]. The body of OR/MS literature directed to residential care services is limited. The literature has mainly focused on predicting patients’ health progress, to support the strategic decisions placement policy and capacity dimensioning. The dynamics of residential care services, although on a slower time scale, are similar to that of inpatient care services. Therefore, most planning decisions and insights described under inpatient care services also apply to residential care services. This fact and the low variety in addressed planning decisions in the literature are the reasons that we choose for residential care services, as opposed to the other care services, to only present planning decisions for which we found references.
Strategic planning
Placement policy
The placement policy decision prescribes which patient types are eligible for which type of residential care services, and which are preferably admitted to inpatient or home care services. The aim is to provide patients with the right treatment at the right time using means which are most cost-efficient [22]. Defining a placement policy requires classification systems by which the health status and care requirements of a patient can be assessed [ 22, 457]. Often, for a single patient there are multiple alternatives for what type of care facility is most suitable. This especially holds for elderly patients, since they often suffer from multiple pathologies [306]. The placement policy involves the consideration whether to treat a patient in a hospital bed, and at which point during recovery a patient is transferred from the hospital to residential care [ 296, 306, 375]. This makes coordination between inpatient and residential care resource capacity planning desirable. Although hospital beds are in general more costly, a relatively short hospital stay may prevent a long stay in residential care, which may therefore be less expensive in the long run [ 181, 312, 373].
To derive optimal placement policies, many contributions model the movement of patients through the health care system including both hospital and residential care [ 306, 375, 400, 435, 456], the progress of patients through different health states [ 87, 147, 148, 165, 231, 304, 306, 307, 308, 312, 375, 397, 398, 399, 400, 456], and part of them include an estimation of related cost [ 293, 294, 296, 308, 337, 455]; other contributions model the relation between gender, age and clinical patient characteristics to length-of-stay and resource consumption in each stage [ 148, 293, 294, 295, 305, 312, 375, 417, 455, 456]. Various cost evaluations include analysis of demographics and individual life-expectations [ 87, 202, 337, 455, 456].
Methods: computer simulation [ 304, 417], heuristics [ 22, 457], Markov processes [ 87, 147, 148, 165, 202, 231, 293, 294, 295, 296, 304, 305, 306, 307, 308, 312, 337, 373, 375, 397, 398, 399, 400, 435, 455, 456], queueing theory [181].
Regional coverage
At a regional planning level, the number, types and locations of residential care facilities have to be decided. To meet residential care service demand, the available budget needs to be spent such that the population of each geographical area has access to a sufficient supply of facilities of appropriate nature [ 56, 97]. In general, the primary criteria for the locations are not so much closeness to customer bases but costs of site acquisition and construction, cost of operation, and speed of access to acute care facilities [342]. However, for rehabilitation care, where patients stay for a relatively short period, distance between the facility and the patients home and family is of importance to stimulate reintegration into their communities [97]. When the locations of facilities are well-spread over a region and load is balanced between facilities, equity of access to care is maximized, since the situation is avoided that some facilities have long waiting lists while other facilities have idle beds [131].
Methods: mathematical programming [ 56, 97, 131], literature review [342].
Case mix
Aligned with the service mix, an organization needs to determine the types and volumes of patients it will serve. Patient types can be grouped according to pathology, required type of care and resource requirements. For example, in [159], resource-utilization groups (RUGs) are presented which classifies patient groups by relating diagnosis, mental condition and mobility to resource requirements. The case mix decision is an influential factor with respect to almost all other planning decisions, especially to staff-related decisions [159], since the length-of-stay of different patient types can be significantly different (i.e., a rehabilitation short-stay vs a geriatric long-stay).
Methods: heuristics [159].
Capacity dimensioning
Residential care organizations dimension their resources, to spend the available budget such that a satisfactory quality of care is realized, while access time is minimized and resource utilization is maximized [137]. To this end, provider capacity must be matched with patient demand. To estimate patient demand (in number and length-of stay), the earlier mentioned models for the movement of patients through health states and through the health system are applicable [ 147, 148, 171, 231, 293, 294, 295, 296, 304, 305, 307, 308, 312, 375, 397, 398, 399, 400, 435, 455, 456].
Owing to the long-term character of residential care, long-term demand forecast models that include demographic information and survival analysis as presented in [ 87, 109, 202, 337, 417] have additional value. To anticipate for the uncertainty of long-term demand developments such as population ageing, scenario analysis can be applied to answer what-if questions [ 398, 399]. Capacity is dimensioned for the following resource types:
-
Beds. The size of residential care facilities is generally expressed in the number of beds. This number can be taken as a guideline for dimensioning decisions for other resources such as equipment and staff. The common objective is to dimension the number of beds of facilities such that occupancy of beds is maximized while admission rejection and delay is minimized [179]. Delay in admission of patients to appropriate care facilities negatively affects therapeutic effectiveness [179]. To be able to realize quick turn-over for short-stay patients, strict separation within a facility of short-stay and long-stay patients might be preferred [137]. However, allowing overflow between longs-stay and short-stay beds potentially increases bed utilization. In that case, an appropriate balance between short-stay and long-stay beds is required [ 83, 137, 165, 179], to avoid short-stay bed blocking by long-stay patients. A relatively small decrease in the number of long-stay beds, with a corresponding rise in the number of short-stay beds, has a dramatic effect on the number of patients that can be treated [ 83, 181, 373]. In addition, balancing capacities between facilities is required, since for instance hospital discharges are highly dependent on availability of downstream care services [337]. When patients find the facilities to which they are referred to be full, they are forced to wait at their current, often unnecessarily intensive (and generally more expensive) care facilities. These patients unnecessarily block the current beds while waiting, preventing utilization by potential patients who require care at these facilities [250]. Hence, inappropriate bed dimensioning for residential services causes both degradation of quality of care and financial losses due to these ‘alternative level of care’ patients [ 83, 333]. Again, a need is identified for integrated coherent planning across services of different health care organizations [442].
-
Staff. In view of the increasing residential care demand and a declining labor force, changes in staff skill mix are worthwhile to consider. It might be able to identify subtasks for which can be carried out by less qualified staff [109].
Methods: computer simulation [ 109, 137, 250, 304, 333, 417], Markov processes [ 87, 147, 148, 165, 171, 202, 231, 293, 294, 295, 296, 304, 305, 307, 308, 312, 333, 337, 373, 375, 397, 398, 399, 400, 435, 455, 456], queueing theory [ 83, 179, 181, 250, 442].
Tactical planning
Admission control
Admission control involves the rules according to which patients are selected to be admitted to residential care services from the waiting lists. Taking into account resource availability, current waiting lists and expected demand, admission control policies have the objective to match demand and supply such that access times are minimized, while resource utilization is maximized. In addition, access times should be equitable among patient groups [275]. Admission control requires patient group identification, which is done by clustering patients with similar pathologies and similar resource requirements [ 166, 275]. For each of these groups, waiting lists are created. To provide timely access for different urgency classes, patients are typically categorized in several priority groups based on medical urgency and current accommodation [333]. A patient's current accommodation plays a role, since waiting at upstream facilities leads to bed blocking, while waiting at home might lead to added stress on families. Estimating the future transitions between patient groups and urgency classes for both patients already in service and patient on the waiting lists can support the design of good admission control policies [ 166, 275].
A possible admission policy is to always take the patient with highest priority into service whenever capacity becomes available. Another option is to develop an admission plan that prescribes how many patients of each patient group are taken into service during a certain planning horizon. The latter has the potential to simultaneously decrease access times and increase resource utilizations on the long run [ 166, 275]. In [333], a dynamic admission rule is proposed which, under the assumption that the total bed capacity is sufficient, maintains ‘alternative level of care’ census at hospitals below a certain threshold and maintains access times from home below a certain access time target. For such dynamic rules, a close cooperation with upstream health organizations is required, which might be challenging since reducing hospital bed blocking may not be the primary interest of residential care organizations.
Methods: computer simulation [333], mathematical programming [ 166, 275, 333].
Offline operational planning
Treatment scheduling
For rehabilitation patients the therapeutic process generally takes several weeks during which multiple treatments with clinicians from different disciplines have to take place. Usually, the treatment requirements are known in advance, at least for a number of weeks, so that the appointments can be scheduled in advance. The treatment is planned in an appointment series, in which appointments may have precedence relations and certain guidelines for the time intervals in between. The goal is to provide treatments at the right time and in the right sequence, while resource utilization is maximized. The quality of the schedules is highly important for the medical effectiveness and the economic efficiency of rehabilitation centers [367]. Since the amount of variables is tremendous, treatment scheduling for a complete rehabilitation center is highly complex. In [367], it is claimed that if scheduling is done by hand, it is generally done on a patient-by-patient or even appointment-for-appointment basis. Therefore, decision support tools based on OR/MS are considered as indispensable to achieve high-quality treatment scheduling.
Methods: mathematical programming [367].
4. Conclusion
This article is directed to both health care professionals and OR/MS researchers. It has introduced a taxonomy to identify, break down and classify decisions to be made in the managerial field of health care resource capacity planning and control. It has provided a structured overview of the planning decisions in six identified care services and the corresponding state of the art in OR/MS literature. Having done this, we aim for an impact that is threefold. First, we aim to support health care professionals in improved decision making. Second, we aim to inspire OR/MS researchers in formulating future research objectives and to position their research in a hierarchical framework. Third, we aim for interconnecting health care professionals and OR/MS researchers so that the potential of OR/MS can be discovered and exploited in improving health care delivery performance.
The vertical axis in our taxonomy represents the hierarchical nature of decision making in health care organizations. Aggregate decisions are made in an early stage, and finer granularity is added in later stages when more detailed information becomes available. The observed literature explicitly substantiates the relations between planning decisions both within and between hierarchical levels. Planning decisions on higher levels shape decision making on lower levels by imposing restrictions. Performance on lower levels concerns feedback about the realization of higher level objectives, thereby potentially impacting decision making on higher levels. We have seen many examples of these interactions in our review. Incorporating flexibility in planning reduces restrictions imposed by decisions settled in higher levels on lower level decision making. Increased planning flexibility involves specifying and adjusting planning decisions closer to the time of actual health care delivery, thereby giving the opportunity to incorporate more detailed and accurate information in decision making. The observed contributions that incorporate planning flexibility provide opportunities to improve the response to fluctuations in patient demand and thus to improve performance.
Although organized by different organizations, the health care delivery process from the patient's perspective generally is a composition of several care services. A patient's pathway typically includes several care stages performed by various health care services. The effectiveness and efficiency of health care delivery is a result of planning and control decisions made for the care services involved in each care stage. The quality of decisions in each care service depends on the information available from and the restrictions imposed by other care services. Therefore, in the perspective of the presented taxonomy, in addition to the vertical interaction, a strong horizontal interaction can be recognized. Suboptimization is a threat when these decisions are taken in isolation. At various points in our overview, we have observed that taking an integrated approach in decision making is beneficial. Such an integration is not straightforward as it also emerged that different care services may have conflicting objectives. Our categorization of planning decisions in the previous section based on the taxonomy presented in Section 2 ‘Taxonomy’ enables identification of interactions between different care services, allows detection of conflicting objectives and helps to discover opportunities for coordinated decision making.
Owing to the segmented organizational structure of health care delivery, also the OR/MS literature has initially focused predominantly on autonomous, isolated decision making. Such models ignore the inherent complex interactions between decisions for different services in different organizations and departments. In 1999, the survey [240] identified a void in OR/MS literature focusing on integrated health care systems. The level of complexity of such models is depicted as main barrier. In 2010, the survey [422], reviewing OR/MS models that encompass patient flows across multiple departments, addressed the question whether this void has since been filled. The authors conclude that the lack of models for complete health care processes still existed. Although a body of literature focusing on two-departmental interactions was identified, very few contributions were found on complete hospital interactions, let alone on complete health care system interactions. The present review of the literature reconfirms these observations.
To conclude, the specification of planning decisions in our taxonomy allows for identifying relations within and between hierarchical levels. Recognizing and incorporating these relationships in decision making improves health care delivery performance. Creating more planning flexibility in decision making demonstrates great potential. By specifying and adjusting planning decisions closer to the time of actual health care delivery, more detailed and accurate information can be incorporated, providing opportunities to adjust planning decisions to better match care supply and demand. Furthermore, integrated decision making for multiple care services along a care chain shows great potential. With the growing awareness of the potential benefit of such integrated decision making, an increase in the number of publications in which integrated models are presented is noticeable [ 72, 422]. However, it remains a challenge for OR/MS researchers to develop integral models that on the one hand provide an extensive health care system scope, while on the other hand incorporating a satisfactory level of detail and insight. Summarizing, for the sake of patient centeredness and cost reductions required by societal voices and pressures, we claim that both health care professionals and OR/MS researchers should address coordinated and integrated decision making for interrelated planning decisions, should explore the opportunities of increased flexibility and should take an integral care chain perspective.
References
Aarts EHL and Lenstra JK (2003) Local Search in Combinatorial Optimization. Princeton University Press, Princeton, NJ.
Abernathy WJ and Hershey JC (1972) A spatial-allocation model for regional health-services planning. Operations Research 20 (3), 629–642.
Adan I, Bekkers J, Dellaert N, Jeunet J and Vissers J (2011) Improving operational effectiveness of tactical master plans for emergency and elective patients under stochastic demand and capacitated resources. European Journal of Operational Research 213 (1), 290–308.
Adan I, Bekkers J, Dellaert N, Vissers J and Yu X (2009) Patient mix optimisation and stochastic resource requirements: a case study in cardiothoracic surgery planning. Health Care Management Science 12 (2), 129–141.
Aiken LH, Clarke SP, Sloane DM, Sochalski J and Silber JH (2002) Hospital nurse staffing and patient mortality, nurse burnout, and job dissatisfaction. Journal of the American Medical Association 288 (16), 1987–1993.
Akcali E, Côté MJ and Lin C (2006) A network flow approach to optimizing hospital bed capacity decisions. Health Care Management Science 9 (4), 391–404.
Akkerman R and Knip M (2004) Reallocation of beds to reduce waiting time for cardiac surgery. Health Care Management Science 7 (2), 119–126.
Andersson T and Värbrand P (2006) Decision support tools for ambulance dispatch and relocation. Journal of the Operational Research Society 58 (2), 195–201.
Anthony RN (1965) Planning and Control Systems: A Framework for Analysis. Division of Research, Graduate School of Business Administration, Harvard University, Boston, MA.
Arnaout JP (2010) Heuristics for the maximization of operating rooms utilization using simulation. Simulation 86 (8–9), 573–583.
Asaduzzaman M, Chaussalet TJ and Robertson NJ (2010) A loss network model with overflow for capacity planning of a neonatal unit. Annals of Operations Research 178 (1), 67–76.
Ashton R, Hague L, Brandreth M, Worthington D and Cropper S (2005) A simulation-based study of a NHS walk-in centre. Journal of the Operational Research Society 56 (2), 153–161.
Augusto V, Xie X and Perdomo V (2010) Operating theatre scheduling with patient recovery in both operating rooms and recovery beds. Computers & Industrial Engineering 58 (2), 231–238.
Babes M and Sarma GV (1991) Out-patient queues at the Ibn-Rochd health centre. Journal of the Operational Research Society 42 (10), 845–855.
Bagust A, Place M and Posnett JW (1999) Dynamics of bed use in accommodating emergency admissions: stochastic simulation model. British Medical Journal 319 (7203), 155–158.
Ball MO and Lin FL (1993) A reliability model applied to emergency service vehicle location. Operations Research 41 (1), 18–36.
Barado J, Guergué JM, Esparza L, Azcárate C, Mallor F and Ochoa S (2011) A mathematical model for simulating daily bed occupancy in an intensive care unit. Critical Care Medicine 40 (4), 1098–1104.
Bard JF and Purnomo HW (2005) Hospital-wide reactive scheduling of nurses with preference considerations. IIE Transactions 37 (7), 589–608.
Barthel ER, Pierce JR, Goodhue CJ, Ford HR, Grikscheit TC and Upperman JS (2011) Availability of a pediatric trauma center in a disaster surge decreases triage time of the pediatric surge population: a population kinetics model. Theoretical Biology and Medical Modelling 8 (1), 38.
Başar A, Çatay B and Ünlüyurt T (2010) A multi-period double coverage approach for locating the emergency medical service stations in Istanbul. Journal of the Operational Research Society 62 (4), 627–637.
Batun S, Denton BT, Huschka TR and Schaefer AJ (2011) Operating room pooling and parallel surgery processing under uncertainty. INFORMS Journal on Computing 23 (2), 220–237.
Bay KS, Leatt P and Stinson SM (1982) A patient-classification system for long-term care. Medical Care 20 (5), 468–488.
Beaulieu H, Ferland JA, Gendron B and Michelon P (2000) A mathematical programming approach for scheduling physicians in the emergency room. Health Care Management Science 3 (3), 193–200.
Beech R, Brough RL and Fitzsimons BA (1990) The development of a decision-support system for planning services within hospitals. Journal of the Operational Research Society 41 (11), 995–1006.
Begen MA and Queyranne M (2011) Appointment scheduling with discrete random durations. Mathematics of Operations Research 36 (2), 240–257.
Begur SV, Miller DM and Weaver JR (1997) An integrated spatial DSS for scheduling and routing home-health care nurses. Interfaces 27 (4), 35–48.
Bekker R and de Bruin AM (2010) Time-dependent analysis for refused admissions in clinical wards. Annals of Operations Research 178 (1), 45–65.
Bekker R and Koeleman PM (2011) Scheduling admissions and reducing variability in bed demand. Health Care Management Science 14 (3), 1–13.
Beliën J and Demeulemeester E (2007) Building cyclic master surgery schedules with leveled resulting bed occupancy. European Journal of Operational Research 176 (2), 1185–1204.
Beliën J and Demeulemeester E (2008) A branch-and-price approach for integrating nurse and surgery scheduling. European Journal of Operational Research 189 (3), 652–668.
Beliën J, Demeulemeester E and Cardoen B (2009) A decision support system for cyclic master surgery scheduling with multiple objectives. Journal of Scheduling 12 (2), 147–161.
Bennett JC and Worthington DJ (1998) An example of a good but partially successful OR engagement: improving outpatient clinic operations. Interfaces 28 (5), 56–69.
Benveniste R (1985) Solving the combined zoning and location problem for several emergency units. Journal of the Operational Research Society 36 (5), 433–450.
Benzarti E, Sahin E and Dallery Y (2010) A literature review on operations management based models developed for home health care services. Technical report, Cahier d’fitudes et de Recherche, Ecole Centrale Paris.
Beraldi P and Bruni ME (2009) A probabilistic model applied to emergency service vehicle location. European Journal of Operational Research 196 (1), 323–331.
Beraldi P, Bruni ME and Conforti D (2004) Designing robust emergency medical service via stochastic programming. European Journal of Operational Research 158 (1), 183–193.
Berlin GN, ReVelle C and Elzinga DJ (1976) Determining ambulance-hospital locations for on-scene and hospital services. Environment and Planning A 8 (5), 553–561.
Bertels S and Fahle T (2006) A hybrid setup for a hybrid scenario: combining heuristics for the home health care problem. Computers & Operations Research 33 (10), 2866–2890.
Bertrand JWM, Wortmann JC and Wijngaard J (1990) Production Control: A Structural and Design Oriented Approach. Elsevier Science Inc. New York, NY.
Bester MJ, Nieuwoudt I and Van Vuuren JH (2007) Finding good nurse duty schedules: a case study. Journal of Scheduling 10 (6), 387–405.
Bianchi G and Church RL (1988) A hybrid fleet model for emergency medical service system design. Social Science & Medicine 26 (1), 163–171.
Bithell JF (1969) A class of discrete-time models for the study of hospital admission systems. Operations Research 17 (1), 48–69.
Blair EL and Eric CE (1981) A queueing network approach to health care planning with an application to burn care in New York state. Socio-Economic Planning Sciences 15 (5), 207–216.
Blais M, Lapierre SD and Laporte G (2003) Solving a home-care districting problem in an urban setting. Journal of the Operational Research Society 54 (11), 1141–1147.
Blake JT and Carter MW (1997) Surgical process scheduling: a structured review. Journal of the Society for Health Systems 5 (3), 17–30.
Blake JT and Carter MW (2002) A goal programming approach to strategic resource allocation in acute care hospitals. European Journal of Operational Research 140 (3), 541–561.
Blake JT, Dexter F and Donald J (2002) Operating room managers’ use of integer programming for assigning block time to surgical groups: a case study. Anesthesia & Analgesia 94 (1), 143–148.
Blake JT and Donald J (2002) Mount Sinai hospital uses integer programming to allocate operating room time. Interfaces 32 (2), 63–73.
Boldy D and Howell N (1980) The geographical allocation of community care resources – a case study. Journal of the Operational Research Society 31 (2), 123–129.
Bowers J and Mould G (2002) Concentration and the variability of orthopaedic demand. Journal of the Operational Research Society 53 (2), 203–210.
Bowers J and Mould G (2004) Managing uncertainty in orthopaedic trauma theatres. European Journal of Operational Research 154 (3), 599–608.
Brahimi M and Worthington DJ (1991) Queueing models for out-patient appointment systems – a case study. Journal of the Operational Research Society 42 (9), 733–746.
Brailsford SC, Harper PR, Patel B and Pitt M (2009) An analysis of the academic literature on simulation and modelling in health care. Journal of Simulation 3 (3), 130–140.
Brailsford SC, Lattimer VA, Tarnaras P and Turnbull JC (2004) Emergency and on-demand health care: modelling a large complex system. Journal of the Operational Research Society 55 (1), 34–42.
Brailsford SC and Vissers JMH (2011) OR in healthcare: a European perspective. European Journal of Operational Research 212 (2), 223–234.
Brandeau ML, Sainfort F and Pierskalla WP (Eds) (2004) Operations research and health care: a handbook of methods and applications. In International Series in Operations Research & Management Science Vol. 70. Kluwer Academic Publishers, Dordrecht, The Netherlands.
Bräysy O, Dullaert W and Nakari P (2009) The potential of optimization in communal routing problems: case studies from Finland. Journal of Transport Geography 17 (6), 484–490.
Bräysy O, Nakari P, Dullaert W and Neittaanmäki P (2009) An optimization approach for communal home meal delivery service: a case study. Journal of Computational and Applied Mathematics 232 (1), 46–53.
Bredström D and Rönnqvist M (2008) Combined vehicle routing and scheduling with temporal precedence and synchronization constraints. European Journal of Operational Research 191 (1), 19–31.
Bretthauer KM, Heese HS, Pun H and Coe E (2011) Blocking in healthcare operations: a new heuristic and an application. Production and Operations Management 20 (3), 375–391.
Brotcorne L, Laporte G and Semet F (2003) Ambulance location and relocation models. European Journal of Operational Research 147 (3), 451–463.
Broyles JR, Cochran JK and Montgomery DC (2010) A statistical Markov chain approximation of transient hospital inpatient inventory. European Journal of Operational Research 207 (3), 1645–1657.
Brunner JO, Bard JF and Kolisch R (2011) Midterm scheduling of physicians with flexible shifts using branch and price. IIE Transactions 43 (2), 84–109.
Brunner JO and Edenharter G (2011) Long term staff scheduling of physicians with different experience levels in hospitals using column generation. Health Care Management Science 14 (2), 189–202.
Burke EK, De Causmaecker P, Berghe GV and Van Landeghem H (2004) The state of the art of nurse rostering. Journal of Scheduling 7 (6), 441–499.
Busby CR and Carter MW (2006) A decision tool for negotiating home care funding levels in Ontario. Home Health Care Services Quarterly 2 (3–4), 91.
Butler TW, Karwan KR, Sweigart JR and Reeves GR (1992) An integrative model-based approach to hospital layout. IIE transactions 24 (2), 144–152.
Calvo AB and Marks DH (1973) Location of health care facilities: an analytical approach. Socio-Economic Planning Sciences 7 (5), 407–422.
Cardoen B and Demeulemeester E (2011) A decision support system for surgery sequencing at UZ Leuven's day-care department. International Journal of Information Technology and Decision Making 10 (3), 435.
Cardoen B, Demeulemeester E and Beliën J (2009) Optimizing a multiple objective surgical case sequencing problem. International Journal of Production Economics 119 (2), 354–366.
Cardoen B, Demeulemeester E and Beliën J (2009) Sequencing surgical cases in a day-care environment: an exact branch-and-price approach. Computers and Operations Research 36 (9), 2660–2669.
Cardoen B, Demeulemeester E and Beliën J (2010) Operating room planning and scheduling: a literature review. European Journal of Operational Research 201 (3), 921–932.
Carpenter AP, Leemis LM, Papir AS, Phillips DJ and Phillips GS (2011) Managing magnetic resonance imaging machines: support tools for scheduling and planning. Health Care Management Science 14 (2), 158–173.
Carter GM, Chaiken JM and Ignall E (1972) Response areas for two emergency units. Operations Research 20 (3), 571–594.
Carter MW and Lapierre SD (2001) Scheduling emergency room physicians. Health Care Management Science 4 (4), 347–360.
Cayirli T and Veral E (2003) Outpatient scheduling in health care: a review of literature. Production and Operations Management 12 (4), 519–549.
Cayirli T, Veral E and Rosen H (2006) Designing appointment scheduling systems for ambulatory care services. Health Care Management Science 9 (1), 47–58.
Ceglowski R, Churilov L and Wasserthiel J (2006) Combining data mining and discrete event simulation for a value-added view of a hospital emergency department. Journal of the Operational Research Society 58 (2), 246–254.
Ceschia S and Schaerf A (2011) Local search and lower bounds for the patient admission scheduling problem. Computers and Operations Research 38 (10), 1452–1463.
Chaabane S, Meskens N, Guinet A and Laurent M (2008) Comparison of two methods of operating theatre planning: application in Belgian hospital. Journal of Systems Science and Systems Engineering 17 (2), 171–186.
Chahed S, Marcon E, Sahin E, Feillet D and Dallery Y (2009) Exploring new operational research opportunities within the home care context: the chemotherapy at home. Health Care Management Science 12 (2), 179–191.
Chand S, Moskowitz H, Norris JB, Shade S and Willis DR (2009) Improving patient flow at an outpatient clinic: study of sources of variability and improvement factors. Health Care Management Science 12 (3), 325–340.
Chaussalet TJ, Xie H and Millard P (2006) A closed queueing network approach to the analysis of patient flow in health care systems. Methods of Information in Medicine 45 (5), 492–497.
Cheang B, Li H, Lim A and Rodrigues B (2003) Nurse rostering problems-a bibliographic survey. European Journal of Operational Research 151 (3), 447–460.
Chien CF, Tseng FP and Chen CH (2008) An evolutionary approach to rehabilitation patient scheduling: a case study. European Journal of Operational Research 189 (3), 1234–1253.
Chow VS, Puterman ML, Salehirad N, Huang W and Atkins D (2011) Reducing surgical ward congestion through improved surgical scheduling and uncapacitated simulation. Production and Operations Management 20 (3), 418–430.
Christodoulou G and Taylor GJ (2001) Using a continuous time hidden Markov process, with covariates, to model bed occupancy of people aged over 65 years. Health Care Management Science 4 (1), 21–24.
Cochran JK and Bharti A (2006) Stochastic bed balancing of an obstetrics hospital. Health Care Management Science 9 (1), 31–45.
Cochran JK and Roche K (2007) A queuing-based decision support methodology to estimate hospital inpatient bed demand. Journal of the Operational Research Society 59 (11), 1471–1482.
Cochran JK and Roche KT (2009) A multi-class queuing network analysis methodology for improving hospital emergency department performance. Computers & Operations Research 36 (5), 1497–1512.
Coelli T, Prasada Rao DS and Battese GE (2005) An Introduction to Efficiency and Productivity Analysis. Kluwer Academic Publishers, Dordrecht, The Netherlands.
Cohen MA, Hershey JC and Weiss EN (1980) Analysis of capacity decisions for progressive patient care hospital facilities. Health Services Research 15 (2), 145.
Conforti D, Guerriero F and Guido R (2008) Optimization models for radiotherapy patient scheduling. 4OR: A Quarterly Journal of Operations Research 6 (3), 263–278.
Conforti D, Guerriero F and Guido R (2010) Non-block scheduling with priority for radiotherapy treatments. European Journal of Operational Research 201 (1), 289–296.
Conforti D, Guerriero F, Guido R, Cerinic MM and Conforti ML (2011) An optimal decision making model for supporting week hospital management. Health Care Management Science 14 (1), 74–88.
Costa AX, Ridley SA, Shahani AK, Harper PR, De Senna V and Nielsen MS (2003) Mathematical modelling and simulation for planning critical care capacity. Anaesthesia 58 (4), 320–327.
Cêté MJ, Syam SS, Vogel WB and Cowper DC (2007) A mixed integer programming model to locate traumatic brain injury treatment units in the department of veterans affairs: a case study. Health Care Management Science 10 (3), 253–267.
Creemers S and Lambrecht M (2009) An advanced queueing model to analyze appointment-driven service systems. Computers & Operations Research 36 (10), 2773–2785.
Daskin MS and Stern EH (1981) A hierarchical objective set covering model for emergency medical service vehicle deployment. Transportation Science 15 (2), 137.
Day RW, Dean MD, Garfinkel R and Thompson S (2010) Improving patient flow in a hospital through dynamic allocation of cardiac diagnostic testing time slots. Decision Support Systems 49 (4), 463–473.
De Angelis V (1998) Planning home assistance for AIDS patients in the city of Rome, Italy. Interfaces 48 (3), 75–83.
de Bruin AM, van Rossum AC, Visser MC and Koole GM (2007) Modeling the emergency cardiac in-patient flow: an application of queuing theory. Health Care Management Science 10 (2), 125–137.
De Grano ML, Medeiros DJ and Eitel D (2009) Accommodating individual preferences in nurse scheduling via auctions and optimization. Health Care Management Science 12 (3), 228–242.
Dellaert N, Jeunet J and Mincsovics G (2011) Budget allocation for permanent and contingent capacity under stochastic demand. International Journal of Production Economics 131 (1), 128–138.
Demeester P, Souffriau W, De Causmaecker P and Vanden Berghe G (2010) A hybrid Tabu search algorithm for automatically assigning patients to beds. Artificial Intelligence in Medicine 48 (1), 61–70.
Denton BT and Gupta D (2003) A sequential bounding approach for optimal appointment scheduling. IIE Transactions 35 (11), 1003–1016.
Denton BT, Miller AJ, Balasubramanian HJ and Huschka TR (2010) Optimal allocation of surgery blocks to operating rooms under uncertainty. Operations Research 58 (4-Part-1), 802–816.
Denton BT, Viapiano J and Vogl A (2007) Optimization of surgery sequencing and scheduling decisions under uncertainty. Health Care Management Science 10 (1), 13–24.
Desai MS, Penn ML, Brailsford S and Chipulu M (2008) Modelling of Hampshire adult services – gearing up for future demands. Health Care Management Science 11 (2), 167–176.
Dexter F (1999) Design of appointment systems for preanesthesia evaluation clinics to minimize patient waiting times: a review of computer simulation and patient survey studies. Anesthesia & Analgesia 89 (4), 925–931.
Dexter F (2012) Bibliography of operating room management articles. Retrieved 10 May 2012, from: http://www.franklindexter.com/.
Dexter F, Epstein RH and Marsh HM (2001) A statistical analysis of weekday operating room anesthesia group staffing costs at nine independently managed surgical suites. Anesthesia & Analgesia 92 (6), 1493–1498.
Dexter F and Ledolter J (2005) Bayesian prediction bounds and comparisons of operating room times even for procedures with few or no historic data. Anesthesiology 103 (6), 1259–1267.
Dexter F and Macario A (1999) Decrease in case duration required to complete an additional case during regularly scheduled hours in an operating room suite: a computer simulation study. Anesthesia & Analgesia 88 (1), 72–76.
Dexter F, Macario A and Lubarsky DA (2001) The impact on revenue of increasing patient volume at surgical suites with relatively high operating room utilization. Anesthesia & Analgesia 92 (5), 1215–1221.
Dexter F, Macario A and O’Neill L (1999) A strategy for deciding operating room assignments for second-shift anesthetists. Anesthesia & Analgesia 89 (4), 920–924.
Dexter F, Macario A and O’Neill L (2000) Scheduling surgical cases into overflow block time – Computer simulation of the effects of scheduling strategies on operating room labor costs. Anesthesia & Analgesia 90 (4), 980–988.
Dexter F, Macario A and Traub RD (1999) Optimal sequencing of urgent surgical cases. Journal of Clinical Monitoring and Computing 15 (3), 153–162.
Dexter F, Macario A and Traub RD (1999) Which algorithm for scheduling add-on elective cases maximizes operating room utilization?: Use of bin packing algorithms and fuzzy constraints in operating room management. Anesthesiology 91 (5), 1491–1500.
Dexter F, Macario A, Traub RD, Hopwood M and Lubarsky DA (1999) An operating room scheduling strategy to maximize the use of operating room block time: computer simulation of patient scheduling and survey of patientsŠ preferences for surgical waiting time. Anesthesia & Analgesia 89 (1), 7–20.
Dexter F, Macario A, Traub RD and Lubarsky DA (2003) Operating room utilization alone is not an accurate metric for the allocation of operating room block time to individual surgeons with low caseloads. Anesthesiology 98 (5), 1243–1249.
Dexter F and Traub RD (2000) Statistical method for predicting when patients should be ready on the day of surgery. Anesthesiology 93 (4), 1107.
Dexter F and Traub RD (2002) How to schedule elective surgical cases into specific operating rooms to maximize the efficiency of use of operating room time. Anesthesia & Analgesia 94 (4), 933–942.
Dexter F, Traub RD and Lebowitz P (2001) Scheduling a delay between different surgeons’ cases in the same operating room on the same day using upper prediction bounds for case durations. Anesthesia & Analgesia 92 (4), 943–946.
Dexter F, Traub RD and Macario A (2003) How to release allocated operating room time to increase efficiency: predicting which surgical service will have the most underutilized operating room time. Anesthesia & Analgesia 96 (2), 507–512.
Dexter F, Wachtel RE, Epstein RH, Ledolter J and Todd MM (2010) Analysis of operating room allocations to optimize scheduling of specialty rotations for anesthesia trainees. Anesthesia & Analgesia 111 (2), 520–524.
Dexter F, Wachtel RE, Sohn MW, Ledolter J, Dexter EU and Macario A (2005) Quantifying effect of a hospital's caseload for a surgical specialty on that of another hospital using multi-attribute market segments. Health Care Management Science 8 (2), 121–131.
Dobson G, Hasija S and Pinker EJ (2011) Reserving capacity for urgent patients in primary care. Production and Operations Management 20 (3), 456–473.
Dobson G, Lee HH and Pinker E (2010) A model of ICU bumping. Operations Research 58 (6), 1564–1576.
Dokmeci VF (1976) Planning ambulatory health care delivery systems. Omega 4 (5), 617–622.
Dong-Guen K and Yeong-Dae K (2010) A branch and bound algorithm for determining locations of long-term care facilities. European Journal of Operational Research 206 (1), 168–177.
Dumas MB (1984) Simulation modeling for hospital bed planning. Simulation 43 (2), 69.
Dumas MB (1985) Hospital bed utilization: an implemented simulation approach to adjusting and maintaining appropriate levels. Health Services Research 20 (1), 43.
Eaton DJ (1986) Determining ambulance deployment in Santo Domingo, Dominican Republic. Journal of the Operational Research Society 37 (2), 113–126.
EBSCOhost (2012) http://www.ebscohost.com/, accessed 10 May 2012.
Edward GM, Das SF, Elkhuizen SG, Bakker PJM, Hontelez JAM, Hollmann MW, Preckel B and Lemaire LC (2008) Simulation to analyse planning difficulties at the preoperative assessment clinic. British Journal of Anaesthesia 100 (2), 195–202.
El-Darzi E, Vasilakis C, Chaussalet T and Millard PH (1998) A simulation modelling approach to evaluating length of stay, occupancy, emptiness and bed blocking in a hospital geriatric department. Health Care Management Science 1 (2), 143–149.
Elkhuizen SG, Das SF, Bakker PJM and Hontelez JAM (2007) Using computer simulation to reduce access time for outpatient departments. British Medical Journal 16 (5), 382–386.
Erdogan G, Erkut E, Ingolfsson A and Laporte G (2010) Scheduling ambulance crews for maximum coverage. Journal of the Operational Research Society 61 (4), 543–550.
Erkut E, Ingolfsson A and Erdoğan G (2008) Ambulance location for maximum survival. Naval Research Logistics 55 (1), 42–58.
Ernst AT, Jiang H, Krishnamoorthy M and Sier D (2004) Staff scheduling and rostering: a review of applications, methods and models. European Journal of Operational Research 153 (1), 3–27.
Esogbue AO and Singh AJ (1976) A stochastic model for an optimal priority bed distribution problem in a hospital ward. Operations Research 24 (5), 884–898.
Eveborn P, Flisberg P and Ronnqvist M (2006) Laps care-an operational system for staff planning of home care. European Journal of Operational Research 171 (3), 962–976.
Eveborn P, Rönnqvist M, Einarsdóttir H, Eklund M, Lidén K and Almroth M (2009) Operations research improves quality and efficiency in home care. Interfaces 39 (1), 18–34.
Everett JE (2002) A decision support simulation model for the management of an elective surgery waiting system. Health Care Management Science 5 (2), 89–95.
Faddy MJ, Graves N and Pettitt A (2009) Modeling length of stay in hospital and other right skewed data: comparison of phase-type, gamma and log-normal distributions. Value in Health 12 (2), 309–314.
Faddy MJ and McClean SI (2005) Markov chain modelling for geriatric patient care. Methods of Information in Medicine-Methodik der Information in der Medizin 44 (3), 369–373.
Faddy MJ and McClean SI (2007) Using a multi-state model to enhance understanding of geriatric patient care. Australian Health Review 31 (1), 91–97.
Fei H, Chu C and Meskens N (2009) Solving a tactical operating room planning problem by a column-generation-based heuristic procedure with four criteria. Annals of Operations Research 166 (1), 91–108.
Fei H, Chu C, Meskens N and Artiba A (2008) Solving surgical cases assignment problem by a branch-and-price approach. International Journal of Production Economics 112 (1), 96–108.
Fei H, Meskens N and Chu C (2010) A planning and scheduling problem for an operating theatre using an open scheduling strategy. Computers & Industrial Engineering 58 (2), 221–230.
Fetter RB and Thompson JD (1965) The simulation of hospital systems. Operations Research 13 (5), 689–711.
Fetter RB and Thompson JD (1966) Patients’ waiting time and doctors’ idle time in the outpatient setting. Health Services Research 1 (1), 66–90.
Fitzsimmons JA (1973) A methodology for emergency ambulance deployment. Management Science 19 (6), 627–636.
Fletcher A, Halsall D, Huxham S and Worthington D (2006) The DH accident and emergency department model: a national generic model used locally. Journal of the Operational Research Society 58 (12), 1554–1562.
Fone D, Hollinghurst S, Temple M, Round A, Lester N, Weightman A, Roberts K, Coyle E, Bevan G and Palmer S (2003) Systematic review of the use and value of computer simulation modelling in population health and health care delivery. Journal of Public Health 25 (4), 325.
Fries BE (1976) Bibliography of operations research in health care systems. Operations Research 24 (5), 801–814.
Fries BE and Marathe VP (1981) Determination of optimal variable-sized multiple-block appointment systems. Operations Research 29 (2), 324–345.
Fries BE, Schneider DP, Foley WJ, Gavazzi M, Burke R and Cornelius E (1994) Refining a case-mix measure for nursing homes: resource utilization groups (RUG-III). Medical Care 32 (7), 668.
Fujiwara O, Makjamroen T and Gupta KK (1987) Ambulance deployment analysis: a case study of Bangkok. European Journal of Operational Research 31 (1), 9–18.
Fung Kon Jin PHP, Dijkgraaf MGW, Alons CL, van Kuijk C, Beenen LFM, Koole GM and Goslings JC (2011) Improving CT scan capabilities with a new trauma workflow concept: simulation of hospital logistics using different CT scanner scenarios. European Journal of Radiology 80 (2), 504–509.
Gallivan S and Utley M (2011) A technical note concerning emergency bed demand. Health Care Management Science 14 (3), 1–3.
Gallivan S, Utley M, Treasure T and Valencia O (2002) Booked inpatient admissions and hospital capacity: mathematical modelling study. British Medical Journal 324 (7332), 280–282.
Ganguli S, Tham JC and D’Othee BMJ (2007) Establishing an outpatient clinic for minimally invasive vein care. American Journal of Roentgenology 188 (6), 1506–1511.
Garcia-Navarro JA and Thompson WA (2001) Analysis of bed usage and occupancy following the introduction of geriatric rehabilitative care in a hospital in Huesca, Spain. Health Care Management Science 4 (1), 63–66.
Garg L, McClean S, Meenan B and Millard P (2010) A non-homogeneous discrete time Markov model for admission scheduling and resource planning in a cost or capacity constrained healthcare system. Health Care Management Science 13 (2), 155–169.
Gendreau M, Laporte G and Semet F (2005) The maximal expected coverage relocation problem for emergency vehicles. Journal of the Operational Research Society 57 (1), 22–28.
Geng N, Xie X, Augusto V and Jiang Z (2011) A Monte Carlo optimization and dynamic programming approach for managing MRI examinations of stroke patients. IEEE Transactions on Automatic Control 56 (11), 2515–2529.
Gerchak Y, Gupta D and Henig M (1996) Reservation planning for elective surgery under uncertain demand for emergency surgery. Management Science 42 (3), 321–334.
Geroliminis N, Kepaptsoglou K and Karlaftis MG (2011) A hybrid hypercube-genetic algorithm approach for deploying many emergency response mobile units in an urban network. European Journal of Operational Research 210 (2), 287–300.
Gillespie J, McClean S, Scotney B, Garg L, Barton M and Fullerton K (2011) Costing hospital resources for stroke patients using phase-type models. Health Care Management Science 14 (13), 1–13.
Gnanlet A and Gilland WG (2009) Sequential and simultaneous decision making for optimizing health care resource flexibilities. Decision Sciences 40 (2), 295–326.
Gocgun Y, Bresnahan BW, Ghate A and Gunn ML (2011) A Markov decision process approach to multi-category patient scheduling in a diagnostic facility. Artificial Intelligence in Medicine 53 (2), 73–81.
Goldberg J, Dietrich R, Chen JM, Mitwasi M, Valenzuela T and Criss E (1990) A simulation model for evaluating a set of emergency vehicle base locations: development, validation, and usage. Socio-Economic Planning Sciences 24 (2), 125–141.
Goldberg J, Dietrich R, Chen JM, Mitwasi MG, Valenzuela T and Criss E (1990) Validating and applying a model for locating emergency medical vehicles in Tuczon, AZ. European Journal of Operational Research 49 (3), 308–324.
Goldman J, Knappenberger HA and Eller JC (1968) Evaluating bed allocation policy with computer simulation. Health Services Research 3 (2), 119–129.
Görmez N, Köksalan M and Salman FS (2010) Locating disaster response facilities in Istanbul. Journal of the Operational Research Society 62 (7), 1239–1252.
Gorunescu F, McClean SI and Millard PH (2002) A queueing model for bed-occupancy management and planning of hospitals. Journal of the Operational Research Society 53 (1), 19–24.
Gorunescu F, McClean SI and Millard PH (2002) Using a queueing model to help plan bed allocation in a department of geriatric medicine. Health Care Management Science 5 (4), 307–312.
Gove D, Hewett D and Shahani A (1995) Towards a model for hospital case-load decision support. Mathematical Medicine and Biology 12 (3–4), 329–338.
Graves SC, Leff HS, Natkins J and Senger M (1983) A simple stochastic model for facility planning in a mental health care system. Interfaces 13 (5), 101–110.
Green LV (2006) Queueing analysis in healthcare. In International Series in Operations Research & Management Science (Hall RW, Ed), Vol. 91, pp 281–307.
Green LV and Kolesar PJ (2004) Improving emergency responsiveness with management science. Management Science 50 (8), 1001–1014.
Green LV, Kolesar PJ and Soares J (2001) Improving the SIPP approach for staffing service systems that have cyclic demands. Operations Research 49 (4), 549–564.
Green LV, Kolesar PJ and Whitt W (2007) Coping with time-varying demand when setting staffing requirements for a service system. Production and Operations Management 16 (1), 13–39.
Green LV and Nguyen V (2001) Strategies for cutting hospital beds: the impact on patient service. Health Services Research 36 (2), 421–442.
Green LV and Savin S (2008) Reducing delays for medical appointments: a queueing approach. Operations Research 56 (6), 1526–1538.
Green LV, Savin S and Wang B (2006) Managing patient service in a diagnostic medical facility. Operations Research 54 (1), 11–25.
Green LV, Soares J, Giglio JF and Green RA (2006) Using queueing theory to increase the effectiveness of emergency department provider staffing. Academic Emergency Medicine 13 (1), 61–68.
Griffin J, Xia S, Peng S and Keskinocak P (2012) Improving patient flow in an obstetric unit. Health Care Management Science 15 (1), 1–14.
Griffiths JD, Price-Lloyd N, Smithies M and Williams JE (2005) Modelling the requirement for supplementary nurses in an intensive care unit. Journal of the Operational Research Society 56 (2), 126–133.
Guerriero F and Guido R (2011) Operational research in the management of the operating theatre: a survey. Health Care Management Science 14 (1), 89–114.
Guinet A and Chaabane S (2003) Operating theatre planning. International Journal of Production Economics 85 (1), 69–81.
Gul S, Denton BT, Fowler JW and Huschka T (2011) Bi-criteria scheduling of surgical services for an outpatient procedure center. Production and Operations Management 20 (3), 406–417.
Güneş ED (2009) Modeling time allocation for prevention in primary care. Central European Journal of Operations Research 17 (3), 359–380.
Gupta D (2007) Surgical suites’ operations management. Production and Operations Management 16 (6), 689–700.
Gupta D and Denton B (2008) Appointment scheduling in health care: challenges and opportunities. IIE Transactions 40 (9), 800–819.
Gupta D and Wang L (2008) Revenue management for a primary-care clinic in the presence of patient choice. Operations Research-Baltimore 56 (3), 576–592.
Hall R.W. (Ed.) (2006) Patient flow: reducing delay in healthcare delivery. In International Series in Operations Research & Management Science, Vol. 91, Springer, New York, NY.
Hans E.W., van Houdenhoven M and Hulshof PJH (2012) A framework for health care planning and control. In International Series in Operations Research & Management Science (Hall RW, Ed), pp 303–320, Vol. 168, Springer, New York, NY.
Hans EW, Wullink G, van Houdenhoven M and Kazemier G (2008) Robust surgery loading. European Journal of Operational Research 185 (3), 1038–1050.
Hare WL, Alimadad A, Dodd H, Ferguson R and Rutherford A (2009) A deterministic model of home and community care client counts in British Columbia. Health Care Management Science 12 (1), 80–98.
Harewood SI (2002) Emergency ambulance deployment in Barbados: a multi-objective approach. Journal of the Operational Research Society 53 (2), 185–192.
Harper PR (2002) A framework for operational modelling of hospital resources. Health Care Management Science 5 (3), 165–173.
Harper PR and Gamlin HM (2003) Reduced outpatient waiting times with improved appointment scheduling: a simulation modelling approach. OR Spectrum 25 (2), 207–222.
Harper PR, Knight VA and Marshall AH (2011) Discrete conditional phase-type models utilising classification trees: application to modelling health service capacities. European Journal of Operational Research 219 (3), 522–530.
Harper PR, Powell NH and Williams JE (2009) Modelling the size and skill-mix of hospital nursing teams. Journal of the Operational Research Society 61 (5), 768–779.
Harper PR and Shahani AK (2002) Modelling for the planning and management of bed capacities in hospitals. Journal of the Operational Research Society 53 (1), 11–18.
Harper PR, Shahani AK, Gallagher JE and Bowie C (2005) Planning health services with explicit geographical considerations: a stochastic location-allocation approach. Omega 33 (2), 141–152.
Harris RA (1986) Hospital bed requirements planning. European Journal of Operational Research 25 (1), 121–126.
Harrison GW and Escobar GJ (2010) Length of stay and imminent discharge probability distributions from multistage models: variation by diagnosis, severity of illness, and hospital. Health Care Management Science 13 (3), 268–279.
Harrison GW and Millard PH (1991) Balancing acute and long-term care: the mathematics of throughput in departments of geriatric medicine. Methods of Information in Medicine 30 (3), 221.
Harrison GW, Shafer A and Mackay M (2005) Modelling variability in hospital bed occupancy. Health Care Management Science 8 (4), 325–334.
Helm JE, Ahmad Beygi S and Van Oyen MP (2011) Design and analysis of hospital admission control for operational effectiveness. Production and Operations Management 20 (3), 359–374.
Herring WL and Herrmann JW (2012) The single-day surgery scheduling problem: sequential decision making and threshold-based heuristics. OR Spectrum 34 (2), 429–459.
Hershey JC, Weiss EN and Cohen MA (1981) A stochastic service network model with application to hospital facilities. Operations Research 29 (1), 1–22.
Hertz A and Lahrichi N (2009) A patient assignment algorithm for home care services. Journal of the Operational Research Society 60 (4), 481–495.
Hillier F (2009) Introduction to Operations Research 9th edn, McGraw-Hill Science/Engineering/Math, New York, NY.
Hoand CJ and Lau HS (1992) Minimizing total cost in scheduling outpatient appointments. Management Science 38 (12), 1750–1764.
Ho CJ and Lau HS (1999) Evaluating the impact of operating conditions on the performance of appointment scheduling rules in service systems. European Journal of Operational Research 112 (3), 542–553.
Hsu VN, de Matta R and Lee CY (2003) Scheduling patients in an ambulatory surgical center. Naval Research Logistics 50 (3), 218–238.
Huang R, Kim S and Menezes MBC (2010) Facility location for large-scale emergencies. Annals of Operations Research 181 (1), 271–286.
Huang XM (1995) A planning model for requirement of emergency beds. Mathematical Medicine and Biology 12 (3–4), 345.
Huang XM (1998) Decision making support in reshaping hospital medical services. Health Care Management Science 1 (2), 165–173.
Hughes WL and Soliman SY (1985) Short-term case mix management with linear programming. Hospital & Health Services Administration 30 (1), 52–60.
Hulshof PJH, Boucherie R.J., van Essen JT, Hans EW, Hurink JL, Kortbeek N, Litvak N, Vanberkel PT, Van der Veen E, Veltman B, Vliegen IMH and Zonderland ME (2011) ORchestra: an online reference database of OR/MS literature in health care. Health Care Management Science 14 (4), 383–384.
Hulshof PJH, Vanberkel PT, Boucherie RJ, Hans EW, Van Houdenhoven M and van Ommeren JCW (2012) Analytical models to determine room requirements in outpatient clinics. OR Spectrum 34 (2, SI), 391–405.
INFORMS Website (2012) http://www.informs.org/, accessed 10 May 2012.
Ingolfsson A, Budge S and Erkut E (2008) Optimal ambulance location with random delays and travel times. Health Care Management Science 11 (3), 262–274.
Ingolfsson A, Erkut E and Budge S (2003) Simulation of single start station for Edmonton EMS. Journal of the Operational Research Society 54 (7), 736–746.
Irvine V, McClean S and Millard P (1994) Stochastic models for geriatric in-patient behaviour. Mathematical Medicine and Biology 11 (3), 207.
Isken MW, Ward TJ and Littig SJ (2011) An open source software project for obstetrical procedure scheduling and occupancy analysis. Health Care Management Science 14 (1), 56–73.
Jack EP and Powers TL (2009) A review and synthesis of demand management, capacity management and performance in health care services. International Journal of Management Reviews 11 (2), 149–174.
Jaumard B, Semet F and Vovor T (1998) A generalized linear programming model for nurse scheduling. European Journal of Operational Research 107 (1), 1–18.
Jebali A, Alouane H, Atidel B and Ladet P (2006) Operating rooms scheduling. International Journal of Production Economics 99 (1–2), 52–62.
Jensen PA and Bard JF (2003) Operations Research Models and Methods. Wiley, New York, NY.
Jia H, Ordóñez F and Dessouky M (2007) A modeling framework for facility location of medical services for large-scale emergencies. IIE Transactions 39 (1), 41–55.
Joustra P.E., de Wit J, Struben VMD, Overbeek BJH, Fockens P and Elkhuizen SG (2010) Reducing access times for an endoscopy department by an iterative combination of computer simulation and linear programming. Health Care Management Science 13 (1), 17–26.
Joustra P.E., de Wit J, Van Dijk N and Bakker PJM (2011) How to juggle priorities? An interactive tool to provide quantitative support for strategic patient-mix decisions: an ophthalmology case. Health Care Management Science 14 (4), 348–360.
Jun JB, Jacobson SH and Swisher JR (1999) Application of discrete-event simulation in health care clinics: a survey. Journal of the Operational Research Society 50 (2), 109–123.
Kaandorp GC and Koole G (2007) Optimal outpatient appointment scheduling. Health Care Management Science 10 (3), 217–229.
Kao EPC and Tung GG (1981) Bed allocation in a public health care delivery system. Management Science 27 (5), 507–520.
Kapadia AS and Fasihullah YKCM (1985) Finite capacity priority queues with potential health applications. Computers & Operations Research 12 (4), 411–420.
Katsaliaki K and Mustafee N (2010) Applications of simulation within the healthcare context. Journal of the Operational Research Society 62 (8), 1431–1451.
Katz JH (1969) Simulation of outpatient appointment systems. Communications of the ACM 12 (4), 215–222.
Kellogg DL and Walczak S (2007) Nurse scheduling: from academia to implementation or not? Interfaces 37 (4), 355.
Kim SC and Horowitz I (2002) Scheduling hospital services: the efficacy of elective-surgery quotas. Omega 30 (5), 335–346.
Kim SC, Horowitz I, Young KK and Buckley TA (1999) Analysis of capacity management of the intensive care unit in a hospital. European Journal of Operational Research 115 (1), 36–46.
Kim SC, Horowitz I, Young KK and Buckley TA (2000) Flexible bed allocation and performance in the intensive care unit. Journal of Operations Management 18 (4), 427–443.
Koizumi N, Kuno E and Smith TE (2005) Modeling patient flows using a queuing network with blocking. Health Care Management Science 8 (1), 49–60.
Kokangul A (2008) A combination of deterministic and stochastic approaches to optimize bed capacity in a hospital unit. Computer Methods and Programs in Biomedicine 90 (1), 56–65.
Kolesar P (1970) A Markovian model for hospital admission scheduling. Management Science 16 (6), 384–396.
Kolisch R and Sickinger S (2008) Providing radiology health care services to stochastic demand ofdifferentcustomerclasses. OR Spectrum 30 (2), 375–395.
Kros J, Dellana S and West D (2009) Overbooking increases patient access at East Carolina University's student health services clinic. Interfaces 39 (3), 271–287.
Kuzdrall PJ, Kwak NK and Schmitz HH (1981) Simulating space requirements and scheduling policies in a hospital surgical suite. Simulation 36 (5), 163–172.
Kwak NK, Kuzdrall PJ and Schmitz HH (1975) Simulating the use of space in a hospital surgical suite. Simulation 25 (5), 147–151.
Kwak NK, Kuzdrall PJ and Schmitz HH (1976) The GPSS simulation of scheduling policies for surgical patients. Management Science 22 (9), 982–989.
LaGanga LR and Lawrence SR (2007) Clinic overbooking to improve patient access and increase provider productivity. Decision Sciences 38 (2), 251–276.
Lagergren M (1998) What is the role and contribution of models to management and research in the health services? A view from Europe. European Journal of Operational Research 105 (2), 257–266.
Lahrichi N, Lapierre SD, Hertz A, Talib A and Bouvier L (2006) Analysis of a territorial approach to the delivery of nursing home care services based on historical data. Journal of Medical Systems 30 (4), 283–291.
Lamiri M, Grimaud F and Xie X (2009) Optimization methods for a stochastic surgery planning problem. International Journal of Production Economics 120 (2), 400–410.
Lamiri M, Xie X, Dolgui A and Grimaud F (2008) A stochastic model for operating room planning with elective and emergency demand for surgery. European Journal of Operational Research 185 (3), 1026–1037.
Lamiri M, Xie X and Zhang S (2008) Column generation approach to operating theater planning with elective and emergency patients. IIE Transactions 40 (9), 838–852.
Landau TP, Thiagarajan TR and Ledley RS (1983) Cost containment in the concentrated care center: a study of nursing, bed and patient assignment policies. Computers in Biology and Medicine 13 (3), 205–238.
Lane DC and Husemann E (2007) System dynamics mapping of acute patient flows. Journal of the Operational Research Society 59 (2), 213–224.
Lane DC, Monefeldt C and Rosenhead JV (2000) Looking in the wrong place for healthcare improvements: a system dynamics study of an accident and emergency department. Journal of the Operational Research Society 51 (5), 518–531.
Langabeer JR (2007) Health Care Operations Management: A Quantitative Approach to Business and Logistics. Jones & Bartlett Publishers, Sudbury, WA.
Lanzarone E, Matta A and Scaccabarozzi G (2010) A patient stochastic model to support human resource planning in home care. Production Planning and Control 21 (1), 3–25.
Larson RC (1975) Approximating the performance of urban emergency service systems. Operations Research 23 (5), 845–868.
Lattimer V, Brailsford S, Turnbull J, Tarnaras P, Smith H, George S, Gerard K and Maslin-Prothero S (2004) Reviewing emergency care systems I: insights from system dynamics modelling. Emergency Medicine Journal 21 (6), 685–691.
Lavieri MS and Puterman ML (2009) Optimizing nursing human resource planning in British Columbia. Health Care Management Science 12 (2), 119–128.
Law AM (2006) Simulation Modeling and Analysis 4th edn, McGraw-Hill Publishing Co, New York.
Lee DKK and Zenios SA (2009) Optimal capacity overbooking for the regular treatment of chronic conditions. Operations Research 57 (4), 852–865.
Lee S (2010) The role of preparedness in ambulance dispatching. Journal of the Operational Research Society 62 (10), 1888–1897.
Leff HS, Dada M and Graves SC (1986) An LP planning model for a mental health community support system. Management Science 32 (2), 139–155.
Lehaney B, Clarke SA and Paul RJ (1999) A case of an intervention in an outpatients department. Journal of the Operational Research Society 50 (9), 877–891.
Li LX and Benton WC (1996) Performance measurement criteria in health care organizations: review and future research directions. European Journal of Operational Research 93 (3), 449–468.
Li X, Beullens P, Jones D and Tamiz M (2009) An integrated queuing and multi-objective bed allocation model with application to a hospital in china. Journal of the Operational Research Society 60 (3), 330–338.
Li X, Zhao Z, Zhu X and Wyatt T (2011) Covering models and optimization techniques for emergency response facility location and planning: a review. Mathematical Methods of Operations Research 74 (3), 1–30.
Liao CJ, Pegden CD and Rosenshine M (1993) Planning timely arrivals to a stochastic production or service system. IIE Transactions 25 (5), 63–73.
Lim CS, Mamat R and Bräunl T (2011) Impact of ambulance dispatch policies on performance of emergency medical services. Intelligent Transportation Systems, IEEE Transactions on 12 (2), 624–632.
Littig SJ and Isken MW (2007) Short term hospital occupancy prediction. Health Care Management Science 10 (1), 47–66.
Liu L and Liu X (1998) Block appointment systems for outpatient clinics with multiple doctors. Journal of the Operational Research Society 49 (12), 1254–1259.
Liu N, Ziya S and Kulkarni VG (2010) Dynamic scheduling of outpatient appointments under patient no-shows and cancellations. Manufacturing & Service Operations Management 12 (2), 347–364.
Lovejoy WS and Li Y (2002) Hospital operating room capacity expansion. Management Science 48 (11), 1369–1387.
Mackay M (2001) Practical experience with bed occupancy management and planning systems: an Australian view. Health Care Management Science 4 (1), 47–56.
Magerlein JM and Martin JB (1978) Surgical demand scheduling: a review. Health Services Research 13 (4), 418–433.
Marcon E and Dexter F (2006) Impact of surgical sequencing on post anesthesia care unit staffing. Health Care Management Science 9 (1), 87–98.
Marcon E, Kharraja S and Simonnet G (2003) The operating theatre planning by the follow-up of the risk of no realization. International Journal of Production Economics 85 (1), 83–90.
Marianov V and ReVelle C (1996) The queueing maximal availability location problem: a model for the sitting of emergency vehicles. European Journal of Operational Research 93 (1), 110–120.
Marjamaa RA, Torkki PM, Hirvensalo EJ and Kirvelä OA (2009) What is the best workflow for an operating room? A simulation study of five scenarios. Health Care Management Science 12 (2), 142–146.
Marques I, Captivo ME and Vaz Pato M (2011) An integer programming approach to elective surgery scheduling. OR Spectrum 34 (2), 407–427.
Marshall AH and McClean SI (2004) Using Coxian phase-type distributions to identify patient characteristics for duration of stay in hospital. Health Care Management Science 7 (4), 285–289.
Marshall AH, McClean SI and Millard PH (2004) Addressing bed costs for the elderly: a new methodology for modelling patient outcomes and length of stay. Health Care Management Science 7 (1), 27–33.
Marshall AH, McClean SI, Shapcott CM and Millard PH (2002) Modelling patient duration of stay to facilitate resource management of geriatric hospitals. Health Care Management Science 5 (4), 313–319.
Marshall AH, Shaw B and McClean SI (2007) Estimating the costs for a group of geriatric patients using the Coxian phase-type distribution. Statistics in Medicine 26 (13), 2716–2729.
Masterson BJ, Mihara TG, Miller G, Randolph SC, Forkner ME and Crouter AL (2004) Using models and data to support optimization of the military health system: a case study in an intensive care unit. Health Care Management Science 7 (3), 217–224.
Matta ME and Patterson SS (2007) Evaluating multiple performance measures across several dimensions at a multi-facility outpatient center. Health Care Management Science 10 (2), 173–194.
Maull RS, Smart PA, Harris A and Karasneh AAF (2009) An evaluation of ‘fast track’ in A&E: a discrete event simulation approach. The Service Industries Journal 29 (7), 923–941.
Maxwell MS, Restrepo M, Henderson SG and Topaloglu H (2010) Approximate dynamic programming for ambulance redeployment. INFORMS Journal on Computing 22 (2), 266–281.
May JH, Spangler WE, Strum DP and Vargas LG (2011) The surgical scheduling problem: current research and future opportunities. Production and Operations Management 20 (3), 392–405.
Mayhew L and Smith D (2008) Using queuing theory to analyse the government's 4-h completion time target in accident and emergency departments. Health Care Management Science 11 (1), 11–21.
McClain JO (1978) A model for regional obstetric bed planning. Health Services Research 13 (4), 378–394.
McClean S, Barton M, Garg L and Fullerton K (2011) A modeling framework that combines Markov models and discrete-event simulation for stroke patient care. ACM Transactions on Modeling and Computer Simulation 21 (4), 25.
McClean S and Millard P (1993) Patterns of length of stay after admission in geriatric medicine: an event history approach. The Statistician 42 (3), 263–274.
McClean S and Millard P (2007) Where to treat the older patient? Can Markov models help us better understand the relationship between hospital and community care? Journal of the Operational Research Society 58 (2), 255–261.
McClean SI, McAlea B and Millard PH (1998) Using a Markov reward model to estimate spend-down costs for a geriatric department. Journal of the Operational Research Society 49 (10), 1021–1025.
McClean SI and Millard PH (1998) A three compartment model of the patient flows in a geriatric department: a decision support approach. Health Care Management Science 1 (2), 159–163.
McLaughlin DB and Hays JM (2008) Healthcare Operations Management. Health Administration Press; AUPHA Press, Chicago, IL.
Medical Subject Headings (MeSH) (2010) Retrieved 10 May 2012, from: http://www.nlm.nih.gov/mesh/.
Mielczarek B and Uzialko-Mydlikowska J (2012) Application of computer simulation modeling in the health care sector: a survey. Simulation 88 (2), 197–216.
Millard PH, Christodoulou G, Jagger C, Harrison GW and McClean SI (2001) Modelling hospital and social care bed occupancy and use by elderly people in an English health district. Health Care Management Science 4 (1), 57–62.
Min D and Yih Y (2010) An elective surgery scheduling problem considering patient priority. Computers & Operations Research 37 (6), 1091–1099.
Min D and Yih Y (2010) Scheduling elective surgery under uncertainty and downstream capacity constraints. European Journal of Operational Research 206 (3), 642–652.
Mullinax C and Lawley M (2002) Assigning patients to nurses in neonatal intensive care. Journal of the Operational Research Society 53 (1), 25–35.
Mustafee N, Katsaliaki K and Taylor SJE (2010) Profiling literature in healthcare simulation. Simulation 86 (8–9), 543.
Muthuraman K and Lawley M (2008) A stochastic overbooking model for outpatient clinical scheduling with no-shows. IIE Transactions 40 (9), 820–837.
NBII (2012) Website of the National Biological Information Infrastructure (NBII). Retrieved 10 May 2012, from: http://www.nbii.gov.
Nguyen JM, Six P, Antonioli D, Glemain P, Potel G, Lombrail P and Le Beux P (2005) A simple method to optimize hospital beds capacity. International Journal of Medical Informatics 74 (1), 39–49.
Nguyen JM, Six P, Chaussalet T, Antonioli D, Lombrail P and Le Beux P (2007) An objective method for bed capacity planning in a hospital department – a comparison with target ratio methods. Methods of Information in Medicine 46 (4), 399–405.
Nguyen JM, Six P, Parisot R, Antonioli D, Nicolas F and Lombrail P (2003) A universal method for determining intensive care unit bed requirements. Intensive Care Medicine 29 (5), 849–852.
Oddoye JP, Jones DF, Tamiz M and Schmidt P (2009) Combining simulation and goal programming for healthcare planning in a medical assessment unit. European Journal of Operational Research 193 (1), 250–261.
Oddoye JP, Yaghoobi MA, Tamiz M, Jones DF and Schmidt P (2006) A multi-objective model to determine efficient resource levels in a medical assessment unit. Journal of the Operational Research Society 58 (12), 1563–1573.
Organisation of Econonmic Co-operation and Development (OECD) (2011) Health at a Glance 2011: OECD Indicators. OECD Publishing, Retrieved 10 May 2012, from: http://dx.doi.org/10.1787/health_glance-2011-en.
OECD Glossary (2012) http://stats.oecd.org/glossary/, accessed 10 May 2012.
Oh HC and Chow WL (2011) Scientific evaluation of polyclinic operating strategies with discrete-event simulation. International Journal of Simulation Modelling 10 (4), 165–176.
Olivares M, Terwiesch C and Cassorla L (2008) Structural estimation of the newsvendor model: an application to reserving operating room time. Management Science 54 (1), 41–55.
ORchestra (2012) Developed by Center for Healthcare Operations and Improvement Research (CHOIR) at the University of Twente. Retrieved 10 May 2012, from: http://www.utwente.nl/choir/en/orchestra/.
Organisation of Economic Co-operation and Development (OECD) (2012) Data retrieved 10 May 2012, from: http://www.oecd.org/health.
Ozcan YA (2009) Quantitative Methods in Health Care Management: Techniques and Applications 2nd edn, Jossey Bass/Wiley, San Francisco, CA.
Papadimitriou CH and Steiglitz K (1998) Combinatorial Optimization: Algorithms and Complexity. Courier Dover Publications, Mineola, New York.
Pasin F, Jobin MH and Cordeau JF (2002) An application of simulation to analyse resource sharing among health care organisations. International Journal of Operations and Production Management 22 (4), 381–393.
Patrick J (2011) Access to long-term care: the true cause of hospital congestion? Production and Operations Management 20 (3), 347–358.
Patrick J (2012) A Markov decision model for determining optimal outpatient scheduling. Health Care Management Science 15 (2), 91–102.
Patrick J, Puterman ML and Queyranne M (2008) Dynamic multi-priority patient scheduling for a diagnostic resource. Operations Research 56 (6), 1507–1525.
Paul SA, Reddy MC and DeFlitch CJ (2010) A systematic review of simulation studies investigating emergency department overcrowding. Simulation 86 (8–9), 559–571.
Pelletier C, Chaussalet TJ and Xie H (2004) A framework for predicting gross institutional long-term care cost arising from known commitments at local authority level. Journal of the Operational Research Society 56 (2), 144–152.
Pérez E, Ntaimo L, Bailey C and McCormack P (2010) Modeling and simulation of nuclear medicine patient service management in DEVS. Simulation 86 (8–9), 481–501.
Persson MJ and Persson JA (2010) Analysing management policies for operating room planning using simulation. Health Care Management Science 13 (2), 182–191.
Petrovic D, Morshed M and Petrovic S (2011) Multi-objective genetic algorithms for scheduling of radiotherapy treatments for categorised cancer patients. Expert Systems with Applications 38 (6), 6994–7002.
Pham DN and Klinkert A (2008) Surgical case scheduling as a generalized job shop scheduling problem. European Journal of Operational Research 185 (3), 1011–1025.
Pierskalla WP and Brailer DJ (1994) Applications of operations research in health care delivery. Handbooks in OR & MS (Pollock, SM, Rothkopf, MH and Barnett A Eds) pp 469–505, Elsevier, Amsterdam, The Netherlands.
Porter ME (1985) Competitive Advantage, Vol. 15, Free Press, New York, NY.
Price C, Golden B, Harrington M, Konewko R, Wasil E and Herring W (2011) Reducing boarding in a post-anesthesia care unit. Production and Operations Management 20 (3), 431–441.
Przasnyski ZH (1986) Operating room scheduling: a literature review. Association of PeriOperative Registered Nurses Journal 44 (1), 67–82.
PubMed (2012) Retrieved 10 May 2012, from: http://www.pubmed.gov/.
Punnakitikashem P, Rosenberger JM and Buckley Behan D (2008) Stochastic programming for nurse assignment. Computational Optimization and Applications 40 (3), 321–349.
Qu X, Rardin RL, Williams JAS and Willis DR (2007) Matching daily healthcare provider capacity to demand in advanced access scheduling systems. European Journal of Operational Research 183 (2), 812–826.
Qu X and Shi J (2011) Modeling the effect of patient choice on the performance of open access scheduling. International Journal of Production Economics 129 (2), 314–327.
Rais A and Viana A (2011) Operations research in healthcare: a survey. International Transactions in Operational Research 18 (1), 1–31.
Reilly TA, Marathe VP and Fries BE (1978) A delay-scheduling model for patients using a walk-in clinic. Journal of Medical Systems 2 (4), 303–313.
Repede JF and Bernardo JJ (1994) Developing and validating a decision support system for locating emergency medical vehicles in Louisville, Kentucky. European Journal of Operational Research 75 (3), 567–581.
ReVelle C (1989) Review, extension and prediction in emergency service siting models. European Journal of Operational Research 40 (1), 58–69.
Ridge JC, Jones SK, Nielsen MS and Shahani AK (1998) Capacity planning for intensive care units. European Journal of Operational Research 105 (2), 346–355.
Riise A and Burke EK (2011) Local search for the surgery admission planning problem. Journal of Heuristics 17 (4), 389–414.
Rising EJ, Baron R and Averill B (1973) A systems analysis of a university-health-service outpatient clinic. Operations Research 21 (5), 1030–1047.
Robinson LW and Chen RR (2003) Scheduling doctors’ appointments: optimal and empirically-based heuristic policies. IIE Transactions 35 (3), 295–307.
Robinson LW and Chen RR (2010) A comparison of traditional and open-access policies for appointment scheduling. Manufacturing Service Operations Management 12 (2), 330–346.
Rohleder TR, Bischak DP and Baskin LB (2007) Modeling patient service centers with simulation and system dynamics. Health Care Management Science 10 (1), 1–12.
Rohleder TR, Lewkonia P, Bischak DP, Duffy P and Hendijani R (2011) Using simulation modeling to improve patient flow at an outpatient orthopedic clinic. Health Care Management Science 14 (2), 135–145.
Roland B, Di Martinelly C, Riane F and Pochet Y (2010) Scheduling an operating theatre under human resource constraints. Computers & Industrial Engineering 58 (2), 212–220.
Rönnberg E and Larsson T (2010) Automating the self-scheduling process of nurses in Swedish healthcare: a pilot study. Health Care Management Science 13 (1), 35–53.
Ross SM (2007) Introduction to Probability Models 9th edn, Academic Press, New York, NY.
Ruth RJ (1981) A mixed integer programming model for regional planning of a hospital inpatient service. Management Science 7 (5), 521–533.
Santibáñez P, Begen M and Atkins D (2007) Surgical block scheduling in a system of hospitals: an application to resource and wait list management in a British Columbia health authority. Health Care Management Science 10 (3), 269–282.
Savas ES (1969) Simulation and cost-effectiveness analysis of New York's emergency ambulance service. Management Science 15 (12), 608–627.
Schimmelpfeng K, Helber S and Kasper S (2010) Decision support for rehabilitation hospital scheduling. OR Spectrum 32 (2), 1–29.
Schmid V (2012) Solving the dynamic ambulance relocation and dispatching problem using approximate dynamic programming. European Journal of Operational Research 219 (3), 611–621.
Schmitz HH and Kwak NK (1972) Monte Carlo simulation of operating-room and recovery-room usage. Operations Research 20 (6), 1171–1180.
Schmitz HH, Kwak NK and Kuzdrall PJ (1978) Determination of surgical suite capacity and an evaluation of patient scheduling policies. RAIRO – Operations Research 12 (1), 3–14.
Schrijver A (2003) Combinatorial Optimization: Polyhedra and Efficiency. Springer Verlag, Berlin.
Scopus (2012) Retrieved 10 May 2012, from: http://www.scopus.com/.
Seymour DG (2001) Health care modelling and clinical practice: theoretical exercise or practical tool? Health Care Management Science 4 (1), 7–12.
Shahani AK, Ridley SA and Nielsen MS (2008) Modelling patient flows as an aid to decision making for critical care capacities and organisation. Anaesthesia 63 (10), 1074–1080.
Shaw B and Marshall AH (2006) Modeling the health care costs of geriatric inpatients. Information Technology in Biomedicine, IEEE Transactions on 10 (3), 526–532.
Shepperd S, McClaran J, Phillips CO, Lannin NA, Clemson LM, McCluskey A, Cameron ID and Barras SL (2010) Discharge planning from hospital to home. Cochrane Database of Systematic Reviews 1, CD000313.
Shmueli A, Sprung CL and Kaplan EH (2003) Optimizing admissions to an intensive care unit. Health Care Management Science 6 (3), 131–136.
Shonick W and Jackson JR (1973) An improved stochastic model for occupancy-related random variables in general-acute hospitals. Operations Research 21 (4), 952–965.
Sier D, Tobin P and McGurk C (1997) Scheduling surgical procedures. Journal of the Operational Research Society 48 (9), 884–891.
Singer M and Donoso P (2008) Assessing an ambulance service with queuing theory. Computers & Operations Research 35 (8), 2549–2560.
Sinreich D and Jabali O (2007) Staggered work shifts: a way to downsize and restructure an emergency department workforce yet maintain current operational performance. Health Care Management Science 10 (3), 293–308.
Sinreich D, Jabali O and Dellaert NP (2012) Reducing emergency department waiting times by adjusting work shifts considering patient visits to multiple care providers. IIE Transactions 44 (3), 163–180.
Smith CE, Kleinbeck SVM, Fernengel K and Mayer LS (1997) Efficiency of families managing home health care. Annals of Operations Research 73 (1), 157–175.
Smith K.R., Over Jr. AM, Hansen MF, Golladay FL and Davenport EJ (1976) Analytic framework and measurement strategy for investigating optimal staffing in medical practice. Operations Research 24 (5), 815–841.
Smith-Daniels VL, Schweikhart SB and Smith-Daniels DE (1988) Capacity management in health care services: review and future research directions. Decision Sciences 19 (4), 889–919.
Sobolev BG, Sanchez V and Vasilakis C (2011) Systematic review of the use of computer simulation modeling of patient flow in surgical care. Journal of Medical Systems 35 (1), 1–16.
Sonnenberg A (2009) How to overbook procedures in the endoscopy unit. Gastrointestinal Endoscopy 69 (3-Part-2), 710–715.
Stafford Jr. EF and Aggarwal SC (1979) Managerial analysis and decision making in outpatient health clinics. Journal of the Operational Research Society 30 (10), 905–915.
Su MC, Lai SC, Wang PC, Hsieh YZ and Lin SC (2011) A SOMO-based approach to the operating room scheduling problem. Expert Systems with Applications 38 (12), 15447–15454.
Sundaramoorthi D, Chen VCP, Rosenberger JM, Kim SB and Buckley-Behan DF (2009) A data-integrated simulation model to evaluate nurse–patient assignments. Health Care Management Science 12 (3), 252–268.
Swisher JR and Jacobson SH (2002) Evaluating the design of a family practice healthcare clinic using discrete-event simulation. Health Care Management Science 5 (2), 75–88.
Swisher JR, Jacobson SH, Jun JB and Balci O (2001) Modeling and analyzing a physician clinic environment using discrete-event (visual) simulation. Computers and Operations Research 28 (2), 105–125.
Swoveland C, Uyeno D, Vertinsky I and Vickson R (1973) Ambulance location: a probabilistic enumeration approach. Management Science 20 (4), 686–698.
Taha HA (2010) Operations Research: An Introduction 9th edn, Prentice-Hall, Englewood Cliffs, NJ.
Tànfani E and Testi A (2010) A pre-assignment heuristic algorithm for the master surgical schedule problem (MSSP). Annals of Operations Research 178 (1), 105–119.
Tarakci H, Ozdemir Z and Sharafali M (2009) On the staffing policy and technology investment in a specialty hospital offering telemedicine. Decision Support Systems 46 (2), 468–480.
Taylor GJ, McClean SI and Millard PH (1996) Geriatric-patient flow-rate modelling. Mathematical Medicine and Biology 13 (4), 297.
Taylor GJ, McClean SI and Millard PH (1997) Continuous-time Markov models for geriatric patient behaviour. Applied Stochastic Models Anddata Analysis 13 (3–4), 315–323.
Taylor GJ, McClean SI and Millard PH (1998) Using a continuous-time Markov model with poisson arrivals to describe the movements of geriatric patients. Applied Stochastic Models and Data Analysis 14 (2), 165–174.
Taylor GJ, McClean SI and Millard PH (2000) Stochastic models of geriatric patient bed occupancy behaviour. Journal of the Royal Statistical Society: Series A (Statistics in Society) 163 (1), 39–48.
Taylor IDS and Templeton JGC (1980) Waiting time in a multi-server cutoff-priority queue, and its application to an urban ambulance service. Operations Research 28 (5), 1168–1188.
Testi A and Tànfani E (2009) Tactical and operational decisions for operating room planning: efficiency and welfare implications. Health Care Management Science 12 (4), 363–373.
Testi A, Tànfani E and Torre G (2007) A three-phase approach for operating theatre schedules. Health Care Management Science 10 (2), 163–172.
Thomas SJ (2003) Capacity and demand models for radiotherapy treatment machines. Clinical Oncology 15 (6), 353–358.
Thompson S, Nunez M, Garfinkel R and Dean MD (2009) Efficient short-term allocation and reallocation of patients to floors of a hospital during demand surges. Operations Research 57 (2), 261–273.
Tijms HC (2003) A First Course in Stochastic Models. John Wiley & Sons, New York, NY.
Toregas C, Swain R, ReVelle C and Bergman L (1971) The location of emergency service facilities. Operations Research 19 (6), 1363–1373.
Toth P and Vigo D (2001) The Vehicle Routing Problem. SIAM, Philadelphia.
Trautsamwieser A, Gronalt M and Hirsch P (2011) Securing home health care in times of natural disasters. OR Spectrum 33 (3), 1–27.
Troy PM and Rosenberg L (2009) Using simulation to determine the need for ICU beds for surgery patients. Surgery 146 (4), 608–620.
Tunnicliffe WJC (1980) A review of operational problems tackled by computer simulation in health care facilities. Health and Social Service Journal 90 (4702), 73–80.
Utley M, Gallivan S, Davis K, Daniel P, Reeves P and Worrall J (2003) Estimating bed requirements for an intermediate care facility. European Journal of Operational Research 150 (1), 92–100.
Utley M, Gallivan S, Treasure T and Valencia O (2003) Analytical methods for calculating the capacity required to operate an effective booked admissions policy for elective inpatient services. Health Care Management Science 6 (2), 97–104.
Utley M, Jit M and Gallivan S (2008) Restructuring routine elective services to reduce overall capacity requirements within a local health economy. Health Care Management Science 11 (3), 240–247.
Valouxis C and Housos E (2000) Hybrid optimization techniques for the workshift and rest assignment of nursing personnel. Artificial Intelligence in Medicine 20 (2), 155–175.
Van Dijk NM and Kortbeek N (2009) Erlang loss bounds for OT-ICU systems. Queueing Systems 63 (1), 253–280.
Van Gameren E and Woittiez I (2005) Transitions between care provisions demanded by Dutch elderly. Health Care Management Science 8 (4), 299–313.
Van Houdenhoven M, van Oostrum JM, Hans EW, Wullink G and Kazemier G (2007) Improving operating room efficiency by applying bin-packing and portfolio techniques to surgical case scheduling. Anesthesia & Analgesia 105 (3), 707–714.
Van Houdenhoven M, van Oostrum JM, Wullink G, Hans E, Hurink JL, Bakker J and Kazemier G (2008) Fewer intensive care unit refusals and a higher capacity utilization by using a cyclic surgical case schedule. Journal of Critical Care 23 (2), 222–226.
van Oostrum JM, Van Houdenhoven M, Hurink JL, Hans EW, Wullink G and Kazemier G (2008) A master surgical scheduling approach for cyclic scheduling in operating room departments. OR Spectrum 30 (2), 355–374.
Vanberkel PT and Blake JT (2007) A comprehensive simulation for wait time reduction and capacity planning applied in general surgery. Health Care Management Science 10 (4), 373–385.
Vanberkel PT, Boucherie RJ, Hans EW, Hurink JL and Litvak N (2010) A survey of health care models that encompass multiple departments. International Journal of Health Management and Information 1 (1), 37–69.
Vanberkel PT, Boucherie RJ, Hans EW, Hurink J.L., van Lent WAM and van Harten WH (2011) Accounting for inpatient wards when developing master surgical schedules. Anesthesia & Analgesia 112 (6), 1472–1479.
Vanberkel PT, Boucherie RJ, Hans EW, Hurink J.L., van Lent WAM and van Harten WH (2011) An exact approach for relating recovering surgical patient workload to the master surgical schedule. Journal of the Operational Research Society 62 (10), 1851–1860.
Vanderby S and Carter MW (2009) An evaluation of the applicability of system dynamics to patient flow modelling. Journal of the Operational Research Society 61 (11), 1572–1581.
Vasilakis C and El-Darzi E (2001) A simulation study of the winter bed crisis. Health Care Management Science 4 (1), 31–36.
Vasilakis C, Sobolev BG, Kuramoto L and Levy AR (2007) A simulation study of scheduling clinic appointments in surgical care: individual surgeon versus pooled lists. Journal of the Operational Research Society 58 (2), 202–211.
Vassilacopoulos G (1985) A simulation model for bed allocation to hospital inpatient departments. Simulation 45 (5), 233–241.
Vermeulen IB, Bohte SM, Elkhuizen SG, Lameris H, Bakker PJM and Poutré HL (2009) Adaptive resource allocation for efficient patient scheduling. Artificial Intelligence in Medicine 46 (1), 67–80.
Villa S, Barbieri M and Lega F (2009) Restructuring patient flow logistics around patient care needs: implications and practicalities from three critical cases. Health Care Management Science 12 (2), 155–165.
Vissers JMH (1998) Patient flow-based allocation of inpatient resources: a case study. European Journal of Operational Research 105 (2), 356–370.
Vissers JMH, Adan IJBF and Dellaert NP (2007) Developing a platform for comparison of hospital admission systems: an illustration. European Journal of Operational Research 180 (3), 1290–1301.
Vissers JMH and Beech R. (Eds) (2005) Health Operations Management: Patient Flow Logistics in Health Care. Routledge Health Management, Routledge, London, UK.
Vissers JMH and Wijngaard J (1979) The outpatient appointment system: design of a simulation study. European Journal of Operational Research 3 (6), 459–463.
Von Korff M (1979) A statistical model of the duration of mental hospitalization: the mixed exponential distribution. Journal of Mathematical Sociology 6 (2), 169–175.
Wachtel RE and Dexter F (2008) Tactical increases in operating room block time for capacity planning should not be based on utilization. Anesthesia & Analgesia 106 (1), 215.
Walts LM and Kapadia AS (1996) Patient classification system: an optimization approach. Health Care Management Review 21 (4), 75.
Wang J, Quan S, Li J and Hollis A (2012) Modeling and analysis of work flow and staffing level in a computed tomography division of University of Wisconsin Medical Foundation. Health Care Management Science 15 (2), 108–120.
Wang WY and Gupta D (2011) Adaptive appointment systems with patient preferences. Manufacturing and Service Operations Management 13 (3), 373–389.
Web of Science (WoS) (2012) Retrieved 10 May 2012, from: http://www.isiknowledge.com/.
Weiss EN (1990) Models for determining estimated start times and case orderings in hospital operating rooms. IIE transactions 22 (2), 143–150.
Weiss EN and McClain JO (1987) Administrative days in acute care facilities: a queueing-analytic approach. Operations Research 35 (1), 35–44.
Welch JD and Bailey NTJ (1952) Appointment systems in hospital outpatient departments. The Lancet 259 (6718), 1105–1108.
Werker G, Sauré A, French J and Shechter S (2009) The use of discrete-event simulation modelling to improve radiation therapy planning processes. Radiotherapy and Oncology 92 (1), 76–82.
Wharton F (1996) On the risk of premature transfer from coronary care units. Omega 24 (4), 413–423.
White MJB and Pike MC (1964) Appointment systems in out-patients’ clinics and the effect of patients’ unpunctuality. Medical Care 2 (3), 133–145.
Williams SV (1983) How many intensive care beds are enough? Critical Care Medicine 11 (6), 412–416.
Winston WL (2003) Operations Research: Applications and Algorithms. Duxbury Press, Pacific Grove, CA.
Wolff RW (1989) Stochastic Modeling and the Theory of Queues. Prentice-Hall, Englewoods Cliffs, NJ.
Worthington DJ (1987) Queueing models for hospital waiting lists. Journal of the Operational Research Society 38 (5), 413–422.
Worthington DJ (1991) Hospital waiting list management models. Journal of the Operational Research Society 42 (10), 833–843.
Wright MB (1987) The application of a surgical bed simulation model. European Journal of Operational Research 32 (1), 26–32.
Wright PD, Bretthauer KM and Côté MJ (2006) Reexamining the nurse scheduling problem: staffing ratios and nursing shortages. Decision Sciences 37 (1), 39–70.
Wu CH and Hwang KP (2009) Using a discrete-event simulation to balance ambulance availability and demand in static deployment systems. Academic Emergency Medicine 16 (12), 1359–1366.
Xie H, Chaussalet TJ and Millard PH (2005) A continuous time Markov model for the length of stay of elderly people in institutional long-term care. Journal of the Royal Statistical Society: Series A (Statistics in Society 168 (1), 51–61.
Xie H, Chaussalet TJ and Millard PH (2006) A model-based approach to the analysis of patterns of length of stay in institutional long-term care. Information Technology in Biomedicine, IEEETransactions on 10 (3), 512–518.
Xie H, Chaussalet TJ, Thompson WA and Millard PH (2006) A simple graphical decision aid for the placement of elderly people in long-term care. Journal of the Operational Research Society 58 (4), 446–453.
Zeltyn S, Marmor YN, Mandelbaum A, Carmeli B, Greenshpan O, Mesika Y, Wasserkrug S, Vortman P, Shtub A, Lauterman T, Schwartz D, Moskovitch K, Tzafrir S and Basis F (2011) Simulation-based models of emergency departments: operational, tactical, and strategic staffing. ACM Transactions on Modeling and Computer Simulation 21 (4), 24.
Zhang B, Murali P, Dessouky MM and Belson D (2009) A mixed integer programming approach for allocating operating room capacity. Journal of the Operational Research Society 60 (5), 663–673.
Zijm WHM (2000) Towards intelligent manufacturing planning and control systems. OR Spectrum 22 (3), 313–345.
Zonderland ME, Boer F, Boucherie RJ, de Roode A and van Kleef JW (2009) Redesign of a university hospital Preanes-Thesia evaluation clinic using a queuing theory approach. Anesthesia & Analgesia 109 (5), 1612–1614.
Zonderland ME, Boucherie RJ, Litvak N and Vleggert-Lankamp CLAM (2010) Planning and scheduling of semi-urgent surgeries. Health Care Management Science 13 (3), 256–267.
Acknowledgements
This research is supported by the Dutch Technology Foundation STW, applied science division of NWO and the Technology Program of the Ministry of Economic Affairs.
Author information
Authors and Affiliations
Corresponding author
Appendices
Appendix A
Appendix B
Appendix C
Overview tables of the identified planning decisions
This appendix displays the overview tables of the identified planning decisions and the applied OR/MS methods for each of the six care services: ambulatory care (Table C.1), emergency care (Table C.2), surgical care (Table C.3), inpatient care (Table C.4), home care (Table C.5) and residential care (Table C.6).
In the overview tables, the following acronyms are used when referring to the methods:

Rights and permissions
About this article
Cite this article
Hulshof, P., Kortbeek, N., Boucherie, R. et al. Taxonomic classification of planning decisions in health care: a structured review of the state of the art in OR/MS. Health Syst 1, 129–175 (2012). https://doi.org/10.1057/hs.2012.18
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1057/hs.2012.18