Abstract
Despite mortality in intensive care units (ICU) being a global public health problem, it is higher in developing countries, including Ethiopia. However, insufficient evidence is established concerning mortality in the ICU and its predictors. This study aimed to assess the magnitude of ICU mortality and its predictors among patients at Tibebe Ghion specialized hospital, Northwest Ethiopia, 2021. A retrospective cross-sectional study was conducted from February 24th, 2019, to January 24th, 2021. Data were collected from medical records by using pretested structured data retrieval checklist. The collected data was entered into Epi-data version 3.1 and analyzed using R version 4.0 software. Descriptive statistics computed. A simple logistic analysis was run (at 95% CI and p-value < 0.05) to identify the determinants for ICU mortality. A total of 568 study participants’ charts were reviewed. The median length of ICU stay was four days. Head trauma and shock were the leading causes of ICU admissions and mortality. The overall mortality rate of the ICU-admitted patients was 29.6% (95% CI: 26%, 33%). Admission in 2020 (AOR = 0.51; 95%CI: 0.31, 0.85), having altered mentation (AOR = 13.44; 95%CI: 5.77, 31.27), mechanical ventilation required at admission (AOR = 4.11; 95%CI: 2.63, 6.43), and stayed < 5 days in the ICU (AOR = 3.74; 95%CI: 2.31, 6.06) were significantly associated with ICU mortality. The magnitude of the ICU mortality rate was moderate. Years of admission, altered mentation, mechanical ventilation required at admission, and days of stay in the ICU were the predictors for ICU mortality. This finding underscores the importance of interventions to reduce ICU mortality.
Similar content being viewed by others
Introduction
The intensive care unit (ICU) is a separate, specially staffed, and equipped hospital unit dedicated to the observation, care, and treatment of patients with life-threatening conditions1,2,3. Intensive care could reduce mortality rates by 15–60% when well-equipped and staffed with intensivists2. Studies in resource-rich settings showed that the physician, nurse, pharmacist, respiratory or physical therapist, and dietician staffing models in use affected the outcomes of critically ill patients4. However, intensive care specialists are unavailable in resource-limited settings, and the ICUs are served by anesthetic officers in collaboration with surgeons, internists, and pediatricians5. In sub-Saharan Africa, ICUs have varying qualities and quantities of infrastructure, mainly determined by the country's economic level6. In Ethiopia, ICU equipment and supplies are also limited, in addition to ICU staff shortages, causing a lag in the quality of ICU services relative to the standard7,8,9.
The mortality rate in critical care units worldwide ranges from 9 to 61%10. Different studies reported that the ICU mortality rate varied across the globe. North America (9.3%), Oceania (10.3%), Europe (18.7%), South America (21.7%), and the Middle East (26.2%) have relatively low rates of ICU mortality11. However, the ICU mortality rate in Africa is high, ranging from 32.9 to 54%12,13. And the ICU mortality rate in Ethiopia fluctuates between 38.7 and 50.4%9,14. This makes it one of Africa's countries with the highest ICU mortality7.
Knowing the magnitude of medical intensive care unit mortality is very important for interventions in the health facilities of the Amhara region. Therefore, the current study is designed to assess the magnitude of mortality and its predictors among patients admitted to the ICU at Tibebe Ghion Specialized Hospital.
Methods
Study design, period, and setting
A retrospective cross-sectional study was conducted from February 24th, 2019, to January 24th, 2021, at Tibebe Ghion Specialized Hospital, which is 565 km away from Addis Ababa, the capital city of Ethiopia, in the North West direction. This hospital has six wards, two intensive care units (pediatric and adult), and 452 beds. The adult ICU had nine beds, six functioning mechanical ventilators, and one bedside ultrasound. This unit is staffed with two anesthesiologists, internal medicine specialists, sub-specialists, trained nurses, medical and surgical residents. It gives service to critically ill medical, surgical and gynecology, and obstetrics patients admitted from the emergency department, wards, operating rooms, and from referrals. The hospital has an average of 24 patients’ ICU admission in a month.
Eligibility criteria
Clinically diagnosed and critically ill patients older than fifteen years and admitted to the adult ICU units were included. While patients whose charts were missing or incomplete or whose COVID-19 test results became positive and transferred to the COVID-19 treatment center were excluded from the study.
Sample size
In this study, 648 patients were admitted in the last two years. All of the patient charts were reviewed. However, 568 critically ill patients who fulfilled the eligibility criteria were included.
Study variables
Dependent variable
ICU mortality (No = 0, Yes = 1).
Independent variables
Sociodemographic characteristics
Age, sex, residence, and years of admission.
ICU admission-related characteristics
Source of admission, admission category, admission diagnosis, admission outcome, cause of death, length of stay in ICU, mechanical ventilation used, and the mental status during admission.
Data collection tools and procedures
Data from ICU medical records were collected by trained ICU nurses using pretested structured data retrieval checklist. Regular check-up of data completeness and consistency was made daily.
Data processing and analysis
Data were entered into Epi-data version 3.1 and analyzed using R version 4.0 software. Descriptive statistics were computed. Bivariate and multivariable logistic regression analyses were employed to assess the association between the exploratory variables and ICU mortality. A p-value of less than 0.2 in the bivariate analysis was considered for variables to be included in the multivariable logistic regression analysis. Variables with a p-value < 0.05 (AOR at 95%CI) on multivariable analysis were considered statistically significant predictors of ICU mortality.
Ethical consideration and consent to participate
Ethical clearance was obtained from the institutional review board of Bahir Dar University with ethical approval number: 0034/2021. All the methods were carried out in accordance with relevant guidelines and regulations. All the experimental protocols were approved by an institutional review board of Bahir Dar University, and informed consent was obtained from the legal guardian (hospital director) as the study was conducted through a review of patient charts. Accordingly, a support letter was obtained from the Department of Internal Medicine and the chief clinical director of the hospital for permission to conduct the study and access patient charts from the Archive. Confidentiality of the patient's charts was kept secure, in which patients’ addresses and other identifications (Card No) were removed before analysis.
Results
Demographic characteristics among patients admitted to ICU
Six hundred forty-eight patients were admitted over two years period. Of these, 568 (88%) patients' charts had complete data. The median (± IQR) age of the respondents was 45 (± 33) years. More than one-third of the patients were in the age groups of 21–40 years. Nearly 59% of the patients were males and were admitted in 2020. Half of the admitted patients came from rural areas (Table 1).
The intensive care unit admission related characteristics
About 74% of patients were admitted from the emergency department,, followed by the operation theatre (12.3%) and surgical ward (9.7%). Nearly 66% of the admitted patients were medical patients. Of this, infectious diseases (septic shock, pneumonia, and ARDS) were the commonest admission and causes of death. Near 1/3rd of patients were ventilated (Table 2).
Trends of ICU admission and its outcomes
In this study, 334 and 224 patients were admitted to the ICU in 2020 and 2019, respectively. The peak admission was observed in July 2020. In contrast, the lowest admission was seen in February 2019 (Fig. 1).
Regarding, the ICU admission outcomes, 20.9% (49/234) of the admitted patients died in 2019. While 35.6% (119/334) of the admitted patients died in 2020 (Fig. 2).
The magnitude of ICU Mortality
The magnitude of death among patients admitted to ICU was 29.6% (95% CI: 26, 33).
Factors associated with ICU mortality
Logistic regression analysis was conducted to identify independent predictors of mortality among patients admitted to the intensive care unit. Five predictor variables having a p-value < 0.2 at bivariate regression analysis were taken into a multivariable logistic regression analysis to see associations between dependent and independent variables. On the multivariable logistic regression model, four variables, namely year of admission, Glasgow comma scale, length of stay, and mechanical ventilation required at admission, were significantly associated with ICU mortality at a p-value of 0.05.
Accordingly, for those patients who were admitted in 2020 to the ICU, the odds of ICU mortality were about 49% (AOR = 0.51; 95% CI: 0.31, 0.85) less compared to patients who were admitted in 2019.
For those patients who had altered mentation, the odds of ICU mortality were 13.5 (AOR = 13.44; 95% CI: 5.77, 31.27) times higher than those who had stable mentation. Similarly, for patients who required mechanical ventilation at admission, the odds of ICU mortality were about four (AOR = 4.11; 95% CI: 2.63, 6.43) times higher than those who did not require mechanical ventilation at admission.
Similarly, for those patients who stayed < 5 days in the ICU, the odds of ICU mortality were about 3.7 (AOR = 3.74; 95%CI: 2.31, 6.06) times higher compared to those who stayed five and more days (Table 3).
Discussion
The outcomes of patients admitted to the intensive care unit depend on the clinical condition of the patient’s arrival, the level of training and experience of staff, the resources, infrastructure, and capacity of the ICU unit1,9.
This study identified the magnitude of mortality and the predictors among patients admitted to the adult ICU of Tibebe Ghion specialized hospital. The study revealed that 29.6% (95% CI: 26, 33) of the admitted patients have died in the ICU. This finding was consistent with an indigenous study from Mekele of 27%15. This finding was higher than the studies done in South Africa, 19.7%16, and Canada, 19%17. However, it was lower compared to the studies from Gondar: 38.7%9, Addis Ababa 39%14, Jimma 50.4%18, Nigeria 34.6%13, and Tanzania 41.1%6. This discrepancy might be due to a lack of necessary medical equipment (an ABG analyzer machine, a portable dialysis machine, and a portable x-ray service), infrastructure, and training. In addition, the lack of a high-dependency unit in the study area and the fact that TGSH ICU is still in the new establishment might be contributing factors to the higher rate of ICU mortality. The other possible justification for the discrepancy might be differences in sample size, level of ICU care, availability of medical supplies, and stratification of skilled staff. However, compared to other study areas in Ethiopia and other African countries mentioned above, the mortality rate is lower. It may be justified by ongoing improvements in ICU services and training.
According to this study, patients admitted in 2020 had a 49% lower mortality rate than those admitted in 2019 (AOR = 0.51: 0.31, 0.85). As the first confirmed COVID-19 case was identified in Ethiopia on March 13, 2020, this low risk of death may be attributed to undiagnosed COVID-19 admissions as a result of the lack of COVID-19 screening tests during the early pandemic. However, after hearing about the COVID-19 instances, the majority of Ethiopia's health facilities were prepared to handle a crisis19. As a result, patients who are brought to an ICU in 2020 may benefit from high-quality care and show signs of recovery.
Patients who stayed in ICU for less than 5 days were five times more likely to die than patients who stayed five or more days (AOR = 3.74: 2.31, 6.06), which is analogous to the study finding in Uganda20. However, the current finding varied from the study conducted in Hosanna; the length of ICU stay was more than 14 days, with ICU mortality21. The majority of the patients in the current study were elderly, with a mean age of 44.5 (± SD, 19.1) as opposed to study participants in Hossana (mean = 31.27 (± SD, 14.019)), which may be the likely explanation. Similar to this, in the current study 87.3%, of patients brought to the ICU were unconsciously compared to Hossana's study result (59.6%). While small intestinal obstruction (15.4%), brain injury (13.9%), and shock (10.4%) were the top causes of admission in Hossana’s study, head injury (16.9%), general surgery (16.2%), and septic shock (10.7%) were the leading causes in our study. Besides, the shortage of functional mechanical ventilators delays and denies the admission of critically ill patients to the medical ICU22.
The current study reported that those patients who required mechanical ventilation at admission had fourfold higher odds of ICU mortality than those who didn’t require mechanical ventilation. This finding was in agreement with the study findings of Gondar9, Kenya12, the United States of America23,24,25, the United Kingdom26, and Singapore27. The possible explanation for this association could be related to mechanical ventilation initiated for patients with respiratory failure who are unable to protect the airway and have hemodynamic instability. Furthermore, patients requiring mechanical ventilation are more vulnerable to ventilator-associated pneumonia and other nosocomial infections28,29. The other possible explanation could be that patients who used mechanical ventilation might be at a critical stage and have organ failure; this leads to a poor prognosis for their health problem and may end in death.
This study revealed that patients admitted with an abnormal mental status were more likely to die than conscious patients. The conscious disturbance is connected to severe decompensated disease, cerebral hypoperfusion due to sepsis, blood loss, poisoning, and neurological disorders30. In addition, in this study, severe head injury secondary to bullet injury was the most common cause of abnormal mental status and mortality.
Limitations of the study
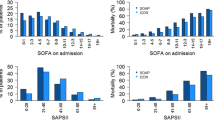
Due to the nature of the study design, a retrospective study based on the ICU registries and charts, only limited data were retrieved. So the necessary variables, which help identify independent risk factors for the clinical outcomes of patients admitted to the ICU, were not collected. In addition, data related to physiological and laboratory variables necessary to calculate severity and prognostic scores such as sequential organ failure assessment (SOFA), Simplified Acute Physiology Score (SAPS), and Acute Physiology and Chronic Health, Disease Classification System (APACHE) to predict ICU mortality were not collected due to an inability to locate them in the available written chart and incomplete ICU registry books.
Conclusion
The magnitude of ICU mortality was moderate. The leading cause of death was shock, followed by head injuries. Years of admission, altered mentation, mechanical ventilation required at admission, and days of stay in the ICU were the predictors for ICU mortality.
Data availability
All data generated or analyzed during this study are included in this published article. However, the data can also be accessed from the corresponding author upon request.
Abbreviations
- AOR:
-
Adjusted odds ratio
- ARDS:
-
Acute respiratory distress syndrome
- CI:
-
Confidence interval
- GBS:
-
Guliam barie syndrome
- ICU:
-
Intensive care unit
- MV:
-
Mechanical ventilation
References
Chong, M. Patient early mobilization: A Malaysia’s study of nursing practices. J. Intens. Critic. Care 3(3), 29 (2017).
Haftu, H., Hailu, T. & Medhaniye, A. Assessment of pattern and treatment outcome of patients admitted to pediatric intensive care unit, Ayder Referral Hospital, Tigray, Ethiopia, 2015. BMC. Res. Notes 11(1), 1–6 (2018).
Ikhwan, M., Mr, N. S. Z., Nadia, A. & Aidalina, M. Policies on intensive care unit (ICU) admission during COVID-19 pandemic. Int. J. Pub. Health Clin. Sci. 8(4), 1–15 (2021).
Kerlin, M. P. et al. An official American thoracic society systematic review: the effect of nighttime intensivist staffing on mortality and length of stay among intensive care unit patients. Am. J. Respir. Crit. Care Med. 195(3), 383–393 (2017).
Chamberlain, S. et al. Mortality related to acute illness and injury in rural Uganda: Task shifting to improve outcomes. PLoS ONE 10(4), e0122559 (2015).
Sawe, H. R. et al. Disease patterns and clinical outcomes of patients admitted in intensive care units of tertiary referral hospitals of Tanzania. BMC Int. Health Hum. Rights 14(1), 1–8 (2014).
Alebachew A, Waddington C. Improving health system efficiency: Ethiopia: Human resources for health reforms. World Health Organization, (2015).
Kifle, F. et al. Intensive care in sub-saharan Africa: A national review of the service status in Ethiopia. Anesth. Analg. 134(5), 930–937 (2022).
Tessema HG, Lema GF, Mesfin N, Fentie DY, Arefaynie NR. Admission pattern, clinical outcomes and associated factors among patients admitted in medical intensive care unit at University of Gondar Comprehensive and specialized hospital, Northwest Ethiopia, 2019. A retrospective cross-sectional study. (2019).
Abate, S. M., Assen, S., Yinges, M. & Basu, B. Survival and predictors of mortality among patients admitted to the intensive care units in southern Ethiopia: A multi-center cohort study. Ann. Med. Surg. 65, 102318 (2021).
Vincent, J.-L. et al. Assessment of the worldwide burden of critical illness: The intensive care over nations (ICON) audit. Lancet Respir. Med. 2(5), 380–386 (2014).
Lalani, H. S. et al. Intensive care outcomes and mortality prediction at a national referral hospital in western Kenya. Ann. Am. Thorac. Soc. 15(11), 1336–1343 (2018).
Onyekwulu, F. & Anya, S. Pattern of admission and outcome of patients admitted into the intensive care unit of University of Nigeria teaching hospital Enugu: A 5-year review. Niger. J. Clin. Pract. 18(6), 775–779 (2015).
Bayisa, T., Berhane, A., Kedir, S. & Wuletaw, T. Admission patterns and outcomes in the medical intensive care unit of St. Paul’s hospital millennium medical college, Addis Ababa, Ethiopia. Ethiopian Med. J. 55(1), 19–26 (2017).
Gidey, K., Hailu, A. & Bayray, A. Pattern and outcome of medical intensive care unit admissions to ayder comprehensive specialized hospital in tigray, Ethiopia. Ethiopian Med. J. https://doi.org/10.2147/IJGM.S385578 (2018).
Dünser, M., Towey, R., Amito, J. & Mer, M. Intensive care medicine in rural sub-Saharan Africa. Anaesthesia 72(2), 181–189 (2017).
Garland, A., Olafson, K., Ramsey, C. D., Yogendran, M. & Fransoo, R. A population-based observational study of intensive care unit–related outcomes. With emphasis on post-hospital outcomes. Ann. Am. Thoracic Soc. 12(2), 202–208 (2015).
Smith, Z., Ayele, Y. & McDonald, P. Outcomes in critical care delivery at jimma university specialised hospital Ethiopia. Anaesth. Intens. Care 41(3), 363–368 (2013).
Lanyero, B. et al. Readiness and early response to COVID-19: achievements, challenges and lessons learnt in Ethiopia. BMJ Glob. Health 6(6), e005581 (2021).
Murthy, S., Leligdowicz, A. & Adhikari, N. K. Intensive care unit capacity in low-income countries: A systematic review. PLoS ONE 10(1), e0116949 (2015).
Mohammed, S. O., Abdi, O. A. & Getish, B. G. Clinical outcomes of patients admitted in intensive care units of Nigist Eleni Mohammed Memorial Hospital of Hosanna, Southern Ethiopia. Int. J. Med. Med. Sci. 9(6), 79–85 (2017).
Marshall, J. C. et al. What is an intensive care unit? A report of the task force of the world federation of societies of intensive and critical care medicine. J. Crit. Care 37, 270–276 (2017).
Arentz, M. et al. Characteristics and outcomes of 21 critically ill patients with COVID-19 in Washington State. JAMA 323(16), 1612–1614 (2020).
Bhatraju, P. K. et al. Covid-19 in critically ill patients in the Seattle region—case series. N. Engl. J. Med. 382(21), 2012–2022 (2020).
Richardson, S. et al. Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area. JAMA 323(20), 2052–2059 (2020).
Napier House: Intensive care national audit and research center report on COVID-19 in critical care. April. 2020;10. (2020).
Mukhopadhyay, A. et al. Risk factors for hospital and long-term mortality of critically ill elderly patients admitted to an intensive care unit. BioMed Res. Int. https://doi.org/10.1155/2014/960575 (2014).
Bouadma, L. et al. Ventilator-associated events: Prevalence, outcome, and relationship with ventilator-associated pneumonia. Crit. Care Med. 43(9), 1798–1806 (2015).
Fialkow, L. et al. Mechanical ventilation in patients in the intensive care unit of a general university hospital in southern Brazil: An epidemiological study. Clinics 71, 144–151 (2016).
Desalegn, N. Causes of admission and clinical outcomes among adult ICU admitted patients at wollega university referral hospital. Int. J. Anesthesiol. Res. 9(3), 636–641 (2021).
Acknowledgements
We want to thank our study participants, data collectors, supervisor, and Tibebe Ghion specialized hospital staff for their cooperation and support during the data collection.
Author information
Authors and Affiliations
Contributions
Conceptualization: T.B.D., A.G.G., T.B.M., G.M.B. Data curation:T.B.D., A.G.G., T.B.M., G.M.B. Formal analysis: T.B.D., A.G.G., T.B.M., G.M.B. Funding acquisition: T.B.D. Investigation: T.B.D., A.G.G., T.B.M., G.M.B. Methodology: T.B.D., A.G.G., T.B.M., G.M.B. Project administration: T.B.D., A.G.G., T.B.M., G.M.B. Software: T.B.D., A.G.G., T.B.M., G.M.B. Supervision: A.G.G., T.B.M., G.M.B. Writing—original draft: T.B.D., A.G.G., T.B.M., G.M.B., Z.A.B., A.A.M., A.A.B., L.G.M., F.E.W. Writing—review & editing: T.B.D., A.G.G., T.B.M.,G.M.B., Z.A.B., A.A.M., A.A.B., L.G.M., F.E.W.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Demass, T.B., Guadie, A.G., Mengistu, T.B. et al. The magnitude of mortality and its predictors among adult patients admitted to the Intensive care unit in Amhara Regional State, Northwest Ethiopia. Sci Rep 13, 12010 (2023). https://doi.org/10.1038/s41598-023-39190-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-39190-7
- Springer Nature Limited