Abstract
Hemoglobin level determines blood viscosity and as hemoglobin level rises, blood pressure rises. However, hemoglobin level in individuals is not fixed and change in hemoglobin is affected by various clinical conditions. The purpose of this study is to investigate whether the hemoglobin variability affects the development of hypertension using Korean cohort database. This study was conducted with 94,798 adults (age ≥ 40 years) who visited the health screening in 2006 or 2007 (index year) and had at least 3 health screenings from 2002 to 2007. Hemoglobin variability was assessed by 3 indices of coefficient of variation (CV), standard deviation, and variability independent of the mean. Cox proportional hazard regression analysis was performed for each index of quartile groups (Q1–Q4). A total of 29,145 participants (30.7%) had the incidence of hypertension during a median follow-up of 7.4 ± 2.5 years. In the multivariable adjusted model, the hazard ratio and 95% confidence interval for incidence of hypertension of Q2, Q3, and Q4 compared with Q1 of hemoglobin variability CV were 1.014 [0.981–1.047], 1.064 [1.030–1.099] and 1.094 [1.059–1.131] respectively. The results were consistent in various sensitivity and subgroup analyses. This study showed that hemoglobin variability could be associated with hypertension development.
Similar content being viewed by others
Introduction
Hypertension is one of the major risk factors for cardiovascular diseases. It is known that 54% of cerebral infarction and 47% of myocardial infarction are caused by hypertension1. Especially, about 60% of cardiovascular diseases in Asia are contributed by hypertension2,3. Therefore, lowering blood pressure is considered to reduce the risk of cardiovascular diseases4. Hypertension is a multifactorial disease caused by various environmental and genetic factors. Aging, obesity, drinking, and lack of exercise are regarded as risk factors for hypertension5. Identifying the potential risk factors and predicting hypertension can help us understand the physiological mechanisms associated with blood pressure, improve the treatment of hypertension, and prevent hypertension.
Hemoglobin is an important factor in determining the viscosity of blood6, and several studies reported that as hemoglobin level rises, systolic and diastolic blood pressure rise7,8. Hemoglobin level is also associated with arterial stiffness9. In animal studies, it is also demonstrated that mean arterial pressure increases with increasing the infusion rate of cross-linked hemoglobin during cardiopulmonary bypass surgery10. Besides, it is suggested that the injection of erythropoietin for the treatment of anemia in patients with end-stage renal disease is associated with elevated blood pressure11. Although many studies investigated the relationship between blood pressure and hemoglobin levels measured at a one-time point, hemoglobin level in individuals is not fixed and change in hemoglobin is affected by various clinical conditions or diseases12. However, no study of the relationship between blood pressure and hemoglobin variability has been reported. The purpose of this study is to investigate whether the hemoglobin variability affects the development of hypertension using large-scale Korean cohort data of the National Health Insurance Service-Health Screening (NHIS-HealS) database.
Methods
Data source and study population
This study was approved by the Institutional Review Board of Gwangju Institute of Science and Technology (20190902-EX-02-02) and was performed based on the Declaration of Helsinki. Since the NHIS-Heals data was provided anonymously according to strict confidentiality guidelines, this study was exempted from receiving the subject's informed consent by Institutional Review Board of Gwangju Institute of Science and Technology.
The NHIS database is registered with 98% of Koreans and includes all insurance claims. We analyzed the data using the health screening cohort, which was extracted from a random sampling of approximately 10% of a total 5 million people over 40 years received a health screening in 2002 or 2003. The NHIS provided a mandatory biennial general health screening for people over 40 years. The NHIS-HealS database includes demographic factors (sex, age, and income), hospital utilization (information about the use of medical facilities, admission date, and discharge date), and biennial health screening (height, weight, blood pressure, and blood tests). More information about the database can be found on the relevant website13. The NHIS-HealS database has been used in many epidemiological studies and its validity is demonstrated elsewhere14.
This study was conducted with adults (age ≥ 40 years) who visited the health screening in 2006 or 2007 (index year) and had at least 3 health screenings from 2002 to 2007. Subjects meeting the criteria for the diagnosis of hypertension before the index year were excluded. Subjects with one or more missing values were also excluded. Finally, 94,798 subjects (male: 48,235, female: 46,563) were included in this study (Fig. 1).
Definition of hemoglobin variability
Hemoglobin variability was defined as the variability in measured hemoglobin levels for independent measurements of health screenings. The 3 indicators of hemoglobin variability were used: coefficient of variation (CV), standard deviation (SD), and variability independent of the mean (VIM). CV was calculated as SD × 100/mean and VIM was calculated as SD × 100/meanbeta. Beta is the regression coefficient based on the natural logarithm of SD over the natural logarithm of the mean15. These indicators have already been used in many studies and have been proved to be valid16,17,18. The frequency of hemoglobin measurements ranged from 3 to 6, with 63,099 in 3 measurements, 8,632 in 4 measurements, 9,964 in 5 measurements, and 13,103 in 6 measurements.
Study outcomes
The endpoint of this study was defined as the incidence of hypertension. Criteria for hypertension were established using the criteria from previous studies16,17,18. The presence of hypertension was defined as the following criteria: (1) the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD-10) codes for hypertension (I10, I11) with at least one claim per year for prescription of the anti-hypertensive drug, or (2) systolic blood pressure (SBP) ≥ 140 mmHg or diastolic blood pressure (DBP) ≥ 90 mmHg. The main analyses were carried out with the above definition, and in addition to the hypertension criteria proposed by the Eighth Joint National Committee (JNC8) guidelines, we performed additional analysis on the hypertension criteria (SBP ≥ 130 mmHg or DBP ≥ 80 mmHg) recently proposed by the American College of Cardiology/American Heart Association (ACC/AHA). Furthermore, for sensitivity analysis, we used another definition of hypertension which includes ICD-10 codes for hypertension with admission ≥ 1 or outpatient department visit ≥ 2, and at least one prescription of anti-hypertensive drug per year19. The study population was followed from the day of health screening at index year to the date of incidence of hypertension, the date of death, or December 31, 2015, whichever came first. The follow-up duration was calculated as the difference between the date of outcome and the date of health screening at index year.
Measurements and definitions
Body mass index (BMI) was calculated by dividing body weight (kg) by the square meter of height (m2). Information on smoking status, alcohol consumption, regular exercise, and family history of hypertension was obtained through questionnaires. Smoking status was classified as non-smokers, ex-smokers, and smokers. Drinking status was classified as non-drinking, < 3, and ≥ 3 times per week. Regular exercise was defined as at least five exercises per week. Income level was divided into quintile groups. Samples for the blood test of fasting glucose and total cholesterol were collected after overnight fasting. Hemoglobin variability can be affected by renal function20, but the NHIS database doesn’t have creatinine information until 2008. As an alternative, we used urine protein as a confounder. Urine protein was measured with clean, midstream urine by dipstick. It was reported with the following grades: absent, trace, + 1 to + 4. Urine protein was classified as absent, trace, and + 1 or higher in this study21. In 2009, creatinine information can be used, and we calculated glomerular filtration rate (GFR) by Modification of Diet in Renal Disease (MDRD) equation22. We used this GFR as a confounder in one of the sensitivity analyses. The mean hemoglobin level was calculated by measured hemoglobin levels at health screenings.
The presence of diabetes was defined as the following criteria16,17,18: (1) ICD-10 codes for diabetes (E10–E14) with at least one claim per year for prescription of an anti-diabetic drug, or (2) fasting glucose level ≥ 126 mg/dL. The presence of dyslipidemia was defined as the following criteria16,17,18: (1) ICD-10 codes (E78) for dyslipidemia with at least one claim per year for prescription of lipid-lowering agents or (2) total cholesterol level ≥ 240 mg/dL. We included information about NSAID because Use of NSAID can change hemoglobin and increase blood pressure23. The NSAID user was defined with at least one claim per year for prescription of NSAID24,25. The Charlson comorbidity index (CCI) was calculated based on the preexisting disease including myocardial infarction, congestive heart failure, peripheral vascular disease, cerebrovascular disease, dementia, chronic pulmonary disease, connective tissue disease, peptic ulcer, mild liver disease, diabetes with and without complications, paraplegia or hemiplegia, renal disease, any or metastatic cancer, moderate or severe liver disease, and acquired immune deficiency syndrome before the start of follow-up period26,27.
Statistical analysis
Baseline characteristics are presented as mean with standard deviation for continuous variables and as number with percentage (%) for categorical variables. The subjects of this study were divided into 4 groups and 10 groups according to hemoglobin variability indices (CV, SD, VIM). Statistical analysis was performed for each indicator in the quartile groups (Q1–Q4) and decile groups (D1–D10). In addition, we performed additional analyses by dividing male and female subjects. The incidence rate of hypertension was calculated by dividing the number of hypertension cases to the total follow-up duration (person-years). The graphs for the incidence rate of hypertension according to the quartiles of hemoglobin variability were calculated using Kaplan–Meier curves and evaluated by the log-rank test. The hazard ratio (HR) and the 95% confidence interval (CI) for the incidence of hypertension were evaluated using the Cox proportional hazards model. The proportional hazard assumption was evaluated by Schoenfeld residuals test with the logarithm of cumulative hazards function based on Kaplan–Meier estimates. There was no interference with the assumption of proportional hazard risk over time. The multivariable-adjusted cox proportional hazard models were adjusted for age, sex, BMI, urine protein, mean hemoglobin level, CCI category, diabetes, dyslipidemia, NSAID use, smoking, exercise, income and family history of hypertension.
Sensitivity analysis was performed as follows: First, we performed the analysis with another definition of hypertension19. Second, the additional sensitivity analysis was performed with hypertension criteria recently proposed by the ACC/AHA. Third, we analyzed with participants who received 4 or more health screenings between 2002 and 2009. Fourth, since creatinine information was available in 2009, we conducted the analysis using GFR data with participants in 2009. Fifth, as hemoglobin can be affected in various clinical situations, we conducted the analysis with subjects who didn’t have the hematopoietic disorder, cancer, chronic kidney disease for the study period28. Sixth, to investigate the effects of hemoglobin variability in the healthy participants, we performed the additional analysis with CCI = 0 participants. Seventh, we performed the analysis with the absent of urine protein participants to exclude renal effect to hemoglobin variability. Eighth, we also performed the analysis with GFR ≥ 90 participants at the final health screening during the follow-up period. Finally, to exclude the influence of the number of hemoglobin measurements, further analysis was performed with a fixed number of hemoglobin measurements (n = 3).
The stratified analyses were performed to evaluate the potential effect modification by BMI, presence of anemia, family history of hypertension, presence of comorbidities, presence of diabetes, and use of NSAID. In subgroup analysis, we divided 2 subgroups of BMI based on the definition of obesity (BMI ≥ 25 kg/m2). The anemia was defined as hemoglobin < 13 g/dL for male and hemoglobin < 12 g/dL for female, as suggested by World Health Organization (WHO) and the presence of comorbidities was defined as the case where CCI is not 0. Furthermore, hemoglobin level can be affected by menstruation, and a stratified analysis was conducted in female subjects dividing by 50 years. Statistical analyses were performed using SAS version 9.4 (SAS Institute Inc., Cary, NC, USA) and using nonlinear regression analysis (PROC NLIN) in SAS, VIM was determined15. All figures were produced by R 3.6.0 (https://www.r-project.org/). The p value < 0.05 was considered to be statistically significant.
Results
Baseline characteristics
The characteristics of the participants divided into 4 groups according to hemoglobin variability CV are shown in Table 1. As the hemoglobin variability increased, the proportion of male gender and current smoker decreased. As the hemoglobin variability increased, the proportion of high CCI category and lower income increased. Mean hemoglobin levels decreased from Q1 to Q4, and the mean CVs in the 4 groups were 1.9%, 3.5%, 5.2%, and 9.7%, respectively. Baseline characteristics of hemoglobin variability SD and VIM are described at Supplementary Table S1. Besides, we divided all subject to male and female and further analyzed. Baseline characteristics in male and female subjects of hemoglobin variability CV are described at Supplementary Table S2.
Association between hemoglobin variability and incidence of hypertension
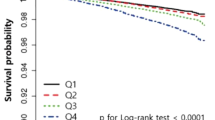
A total of 29,145 participants (30.7%) had the incidence of hypertension during a median follow-up of 7.4 ± 2.5 years. Kaplan–Meier curves and log-rank tests showed that the incidence rate of hypertension was higher in the higher quartiles (Fig. 2). The incidence rate of hypertension increased in Q3 and Q4 groups than Q1 and Q2 groups at all of hemoglobin variability indices. Hemoglobin variability and incidence of hypertension were associated in multivariable-adjusted Cox proportional hazard models regardless of gender at all hemoglobin variability indices (Table 2, Supplementary Table S3-S4). In particular, the HR and 95% CIs of Q2, Q3, and Q4 in comparison with Q1 of hemoglobin variability CV in the adjusted model at all subjects were as follows (Q2: 1.014 [0.981–1.047], Q3: 1.064 [1.030–1.099], Q4: 1.094 [1.059–1.131]). This trend was observed in SD and VIM as well. The adjusted HR and 95% CI of female subjects were slightly higher than those of male subjects. We also investigated the HR and 95% CIs of the decile group comparing with D1 as a reference group in the adjusted model to determine the linear trends of the risk. As results, statistical significance was detected in D6 of all hemoglobin variability indices (Fig. 3).
Hazard ratio and 95% confidence interval for incidence of hypertension by the deciles of hemoglobin variability. Adjusted for age, sex, BMI, urine protein, mean hemoglobin level, CCI category, diabetes, dyslipidemia, NSAID use, smoking, exercise, income, and family history of hypertension. BMI body mass index, CCI Charlson comorbidity index, CV coefficient of variation, SD standard deviation, VIM variability independent of the mean, D decile.
Sensitivity analysis
The first sensitivity analysis was conducted with another definition of hypertension, and the significant results were observed in all, male and female subject groups (Supplementary Table S5). In the second analysis, we analyzed data with the definition of hypertension (SBP ≥ 130 mmHg or DBP ≥ 80 mmHg) proposed by the ACC/AHA (Supplementary Table S6). The HR and 95% CIs of Q2, Q3, and Q4 in comparison with the Q1 of hemoglobin variability CV in the adjusted model were prominent as follows (Q2: 1.085 [1.035–1.140], Q3: 1.117 [1.064–1.174], Q4: 1.201 [1.142–1.262]). The third sensitivity analysis was performed for subjects who received more than 4 health screenings from 2002 to 2009, and the significant results were also observed in all of hemoglobin variability indices (Supplementary Table S7). The HR and 95% CIs of Q2, Q3, and Q4 in comparison with the Q1 of hemoglobin variability CV in the adjusted model were shown as follows (Q2: 0.980 [0.937–1.025], Q3: 1.051 [1.005–1.099], Q4: 1.117 [1.067–1.168]). The fourth analysis was conducted with GFR information on the subjects who receive the health screening in 2009 (Supplementary Tables S8). The results of hemoglobin variability CV in the adjusted model were more prominent as follows (Q2: 1.013 [0.952–1.077], Q3: 1.102 [1.037–1.172], Q4: 1.176 [1.104–1.253]). The fifth analysis was performed with subjects who didn’t have the hematopoietic disorder, cancer, chronic kidney disease (Supplementary Table S9). The significant results were observed in all of the hemoglobin variability indices. The sixth analysis for participants with CCI = 0 was performed (Supplementary Table S10). The HR and 95% CIs of Q2, Q3, and Q4 in comparison with the Q1 of hemoglobin variability CV in the adjusted model were shown as follows (Q2: 0.990 [0.949–1.032], Q3: 1.060 [1.017–1.105], Q4: 1.084 [1.038–1.131]). The seventh analysis for participants with absent of urine protein was performed (Supplementary Table S11). The HR and 95% CIs of Q2, Q3, and Q4 in comparison with the Q1 of hemoglobin variability CV in the adjusted model were shown as follows (Q2: 1.007 [0.974–1.040], Q3: 1.063 [1.029–1.098], Q4: 1.087 [1.051–1.123]). The eighth analysis for participants with GFR ≥ 90 at the final health screening during the follow-up period was performed (Supplementary Table S12). The significant results were also observed in all of the hemoglobin variability indices. Furthermore, the number of health screenings could act as a confounder, we performed the statistical analysis with the fixed number of hemoglobin measurements (n = 3). The HR and 95% CIs of Q2, Q3, and Q4 in comparison with the Q1 of hemoglobin variability CV in the adjusted model were shown as follows (Q2: 1.007 [0.968–1.047], Q3: 1.061 [1.021–1.103], Q4: 1.083 [1.042–1.124]).
Subgroup analysis
Stratified analyses were performed according to BMI, presence of anemia, family history of hypertension, presence of comorbidities, presence of diabetes, and use of NSAID (Fig. 4). As a result, there were marked increases of HR from Q1 to Q4, below 25 kg/m2 in BMI, with anemia, having the family history of hypertension, having comorbidities, and no NSAID user. In stratified analyses according to the presence of diabetes, the HR has a more trend in the subgroup without diabetes. Because of menstruation, the stratified analysis was performed with dividing female subjects by 50 years (Supplementary Figure S1). The HR for the incidence of hypertension of Q4 is higher than that of Q1 at all female subgroups.
Hazard ratio and 95% confidence interval for incidence of hypertension in the stratified analysis according to the quartiles of hemoglobin variability (CV). Adjusted for age, sex, BMI, urine protein, mean hemoglobin level, CCI category, diabetes, dyslipidemia, NSAID use, smoking, exercise, income, and family history of hypertension. CV coefficient of variation, BMI body mass index, CCI Charlson comorbidity index, HR hazard ratio, CI confidence interval, Q quartile, Hx history.
Discussion
This study showed the relationship between hemoglobin variability and the incidence of hypertension through a nationwide population-based cohort study. To the best of our knowledge, there has been no study discussing the association between hemoglobin variability and development of hypertension. Previous studies found the association between hemoglobin level and hypertension, confirming that blood pressure increases as the hemoglobin level rises7,8. Kawamoto et al.29 reported that hemoglobin level correlates with the pulse wave velocity which is related to the arterial stiffness, leading to elevated blood pressure. Through this study, hemoglobin variability is also associated with the development of hypertension. Our results demonstrated that the incidence of hypertension was higher in the higher hemoglobin variability group than in the lower hemoglobin variability group regardless of hypertension diagnosis criteria of JNC and ACC/AHA guideline (Table 2, Supplementary Table S6). Furthermore, the results were valid when the number and period for measurements of hemoglobin levels (6 years for the main study) were extended (Supplementary Table S7). Hemoglobin variability is affected by renal function, we analyzed the subjects with GFR information (Supplementary Table S8), the subject with absent of urine protein (Supplementary Table S11), and the subject with GFR ≥ 90 at the final health screening during the follow-up period (Supplementary Table S12). When analyzed for participants with CCI = 0, the results were consistent (Supplementary Table S10). In the stratified analysis, most of the results were consistent with our main findings (Fig. 4).
The concept of hemoglobin variability comes from patients of end-stage renal disease, who are susceptible to anemia20. There are many methods to define hemoglobin variability. However, with no gold standard to measure variability, we used 3 representative indices of variability based on various studies that refer to variability15,16,17,18. SD is the most widely used indicator and used in this study. As SD can be affected by the mean30, CV and VIM, where SD is adjusted to mean, were also used. We evaluated the effect of hemoglobin variability on hypertension development with the mentioned 3 indices (CV, SD, and VIM) and verified that the results were all valid.
The exact mechanism that explains this result is not yet clearly identified, however, some hypotheses may be suggested. First of all, the hemoglobin level can be considered as a biomarker that reflects the inflammatory state of the body. Red blood cell distribution width (RDW) is suggested as an inflammatory marker that can worsen the arteriosclerosis and RDW is related to cardiovascular disease31,32. Furthermore, RDW is higher in patients with hypertension than in healthy persons33. The systemic chronic inflammation hinders the activity of bone marrow, reducing the production of red blood cell12. Thus, the inflammatory condition not only increases RDW but also can cause changes in hemoglobin level, and inflammation can lead to atherosclerosis as a principal pathophysiological inducer34. Similarly, high hemoglobin variability is thought to be a sign of inflammation and oxidative stress, which are important factors underlying hypertension35,36.
In addition, hemoglobin itself is a factor that can affect blood pressure. Firstly, Vázquez et al.37 reported that a rapid decrease in 10% of hematocrit can raise the blood pressure of 8.6 mmHg and long-term hematocrit change can have the same tendency as acute change has. Hematocrit can affect blood pressure as it determines blood viscosity and regulates peripheral vascular resistance38. Christine et al.39 suggested that red blood cell affects the function of endothelial nitric oxide synthase (eNOS) and smooth muscle contractility through regulation of oxygen transport. Ganidagli et al.40 presented that the carotid intima-media thickness, which is the result of atherosclerosis, was significantly higher in higher hemoglobin variability group among hemodialysis patients and Orcun et al. described that higher hemoglobin variability group showed a significant increase on left ventricular mass index, which is associated with blood pressure41. Secondly, hemoglobin has a high affinity with nitric oxide (NO)42. Especially, scavenging of NO caused by hemoglobin outside the erythrocytes can cause vasoconstriction39. Furthermore, cell-free hemoglobin has pro-oxidant and pro-inflammatory activities43. Although the hemoglobin level is affected by various situations, cell-free hemoglobin generated by hemolysis can cause vasoconstriction and hypertension. Therefore, considering the above mechanisms, hemoglobin variability can be associated with the development of hypertension.
There are some limitations of this study. Firstly, inconsistencies between actual medical practices performed on individuals and recorded claims data may lead to inaccurate analysis. To reduce the risk of inaccuracy, we defined hypertension using the definition used in previous studies16,17,18. But, there was the possibility of misclassification bias for hypertension. Secondly, Hemoglobin variability may vary with an individual’s status, and all of these conditions can be potential covariates. However, as we cannot evaluate all kinds of comorbidities, we used CCI, the most widely used comorbidity assessment tool26,27. Thirdly, there is the possibility of unadjusted confounders, such as inflammatory markers. Besides, we used the use of NSAID as a covariate, but due to the variety of ingredients and formulations of the drug, we could not consider the dose. Considering these points, further studies are needed. Finally, since this study is conducted only for Koreans, it is needed to perform the additional research to find out whether our results could be applied to other countries.
Despite these limitations, this study has several strengths. This study was a large-scale, long-term follow-up study representing the middle-aged Korean population. The incidence rate of hypertension per 1,000 person-years is about 37 to 44 in the Atherosclerosis Risk In Communities (ARIC) study44, which is similar to our results, supporting that our study population was well-established. Through various sensitivity analyses and subgroup analyses, we showed that hemoglobin variability could be related to hypertension development. Hemoglobin test is a routine blood test in health screening and easily identified. Predicting for hypertension with simple periodic health screening results would be a meaningful approach for individuals.
This retrospective cohort study showed the association between hemoglobin variability and incidence of hypertension over 40 years and suggested that the higher hemoglobin variability is correlated with the higher incidence of hypertension. Hemoglobin variability may be a predictor and risk factor for the development of hypertension, but further studies are needed to confirm the exact pathophysiological mechanism for hemoglobin variability and hypertension.
References
Lawes, C. M., Vander Hoorn, S., Rodgers, A. & International Society of Hypertension. Global burden of blood-pressure-related disease, 2001. Lancet 371, 1513–1518. https://doi.org/10.1016/S0140-6736(08)60655-8 (2008).
Ueshima, H. et al. Cardiovascular disease and risk factors in Asia: a selected review. Circulation 118, 2702–2709. https://doi.org/10.1161/CIRCULATIONAHA.108.790048 (2008).
Martiniuk, A. L. et al. Hypertension: its prevalence and population-attributable fraction for mortality from cardiovascular disease in the Asia-Pacific region. J. Hypertens. 25, 73–79. https://doi.org/10.1097/HJH.0b013e328010775f (2007).
Ettehad, D. et al. Blood pressure lowering for prevention of cardiovascular disease and death: a systematic review and meta-analysis. Lancet 387, 957–967. https://doi.org/10.1016/S0140-6736(15)01225-8 (2016).
Kornitzer, M., Dramaix, M. & De Backer, G. Epidemiology of risk factors for hypertension: implications for prevention and therapy. Drugs 57, 695–712. https://doi.org/10.2165/00003495-199957050-00003 (1999).
Ho, C. H. White blood cell and platelet counts could affect whole blood viscosity. J. Chin. Med. Assoc. 67, 394–397 (2004).
Gobel, B. O. et al. Arterial blood pressure, correlation with erythrocyte count, hematocrit, and hemoglobin concentration. Am. J. Hypertens. 4, 14–19 (1991).
Atsma, F. et al. Hemoglobin level is positively associated with blood pressure in a large cohort of healthy individuals. Hypertension 60, 936–941. https://doi.org/10.1161/hypertensionaha.112.193565 (2012).
Strazhesko, I., Staroverova, A., Borisov, E. & Orlova, Y. Red blood cells count and hemoglobin level are associated with arterial stiffness in healthy subjects. J. Hypertens. 36, e250–e251. https://doi.org/10.1097/01.hjh.0000539713.89078.08 (2018).
Ferrera, R. et al. Effect of diaspirin cross-linked haemoglobin (DCLHb) on mean arterial pressure during cardiopulmonary bypass in swine. Transfus. Med. 12, 311–316 (2002).
Kanbay, M. et al. Comparison of effects of darbepoetin alfa and epoetin alfa on serum endothelin level and blood pressure. Adv. Ther. 24, 346–352 (2007).
Weiss, G. & Goodnough, L. T. Anemia of chronic disease. N. Engl. J. Med. 352, 1011–1023. https://doi.org/10.1056/NEJMra041809 (2005).
National Health Insurance Sharing Service, 2019.
Cheol Seong, S. et al. Data resource profile: the national health information database of the National Health Insurance Service in South Korea. Int. J. Epidemiol. 46, 799–800. https://doi.org/10.1093/ije/dyw253 (2017).
Fukuda, K. et al. Day-by-day blood pressure variability and functional outcome after acute ischemic stroke: Fukuoka Stroke Registry. Stroke 46, 1832–1839. https://doi.org/10.1161/STROKEAHA.115.009076 (2015).
Kim, J. A. et al. Impact of visit-to-visit fasting plasma glucose variability on the development of type 2 diabetes: a nationwide population-based cohort study. Diabetes Care 41, 2610–2616. https://doi.org/10.2337/dc18-0802 (2018).
Kim, M. K. et al. Cholesterol variability and the risk of mortality, myocardial infarction, and stroke: a nationwide population-based study. Eur. Heart J. 38, 3560–3566. https://doi.org/10.1093/eurheartj/ehx585 (2017).
Kim, M. K. et al. Effects of variability in blood pressure, glucose, and cholesterol concentrations, and body mass index on end-stage renal disease in the general population of Korea. J Clin Med 8, 755. https://doi.org/10.3390/jcm8050755 (2019).
Lee, S. R. et al. Effectiveness and safety of contemporary oral anticoagulants among Asians with nonvalvular atrial fibrillation. Stroke 50, 2245–2249. https://doi.org/10.1161/strokeaha.119.025536 (2019).
Kalantar-Zadeh, K. & Aronoff, G. R. Hemoglobin variability in anemia of chronic kidney disease. J. Am. Soc. Nephrol. 20, 479–487. https://doi.org/10.1681/ASN.2007070728 (2009).
Lee, H. et al. Risk of end-stage renal disease in patients with hypertrophic cardiomyopathy: a nationwide population-based cohort study. Sci. Rep. 9, 14565. https://doi.org/10.1038/s41598-019-50993-5 (2019).
Levey, A. S. et al. A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann. Intern. Med. 130, 461–470 (1999).
Wilson, S. L. & Poulter, N. R. The effect of non-steroidal anti-inflammatory drugs and other commonly used non-narcotic analgesics on blood pressure level in adults. J. Hypertens. 24, 1457–1469. https://doi.org/10.1097/01.hjh.0000239278.82196.a5 (2006).
Neubert, A. et al. The prescribing of analgesics and non-steroidal anti-inflammatory drugs in paediatric primary care in the UK, Italy and the Netherlands. Pharmacol. Res. 62, 243–248. https://doi.org/10.1016/j.phrs.2010.04.006 (2010).
Han, M. H., Noh, E., Nam, J. H., Lee, S. W. & Lee, E.-K. Prescribing pattern and safety analysis of nonsteroidal anti-inflammatory drug and gastro-protective agent following reimbursement guidelines relaxation. Korean J. Clin. Pharm. 27, 250–257. https://doi.org/10.24304/kjcp.2017.27.4.250 (2017).
de Groot, V., Beckerman, H., Lankhorst, G. J. & Bouter, L. M. How to measure comorbidity. A critical review of available methods. J. Clin. Epidemiol. 56, 221–229. https://doi.org/10.1016/s0895-4356(02)00585-1 (2003).
Kim, K. H. Comparative study on three algorithms of the ICD-10 Charlson comorbidity index with myocardial infarction patients. J. Prev. Med. Public Health 43, 42–49. https://doi.org/10.3961/jpmph.2010.43.1.42 (2010).
Lee, S. R. et al. Comparison of once-daily administration of edoxaban and Rivaroxaban in Asian patients with Atrial Fibrillation. Sci. Rep. 9, 6690. https://doi.org/10.1038/s41598-019-43224-4 (2019).
Kawamoto, R. et al. A slightly low hemoglobin level is beneficially associated with arterial stiffness in Japanese community-dwelling women. Clin. Exp. Hypertens. 34, 92–98. https://doi.org/10.3109/10641963.2011.618202 (2012).
Parati, G., Stergiou, G. S., Dolan, E. & Bilo, G. Blood pressure variability: clinical relevance and application. J. Clin. Hypertens. (Greenwich) 20, 1133–1137. https://doi.org/10.1111/jch.13304 (2018).
Arbel, Y. et al. Red blood cell distribution width (RDW) and long-term survival in patients with ST elevation myocardial infarction. Thromb. Res. 134, 976–979. https://doi.org/10.1016/j.thromres.2014.08.016 (2014).
Lippi, G. et al. Relation between red blood cell distribution width and inflammatory biomarkers in a large cohort of unselected outpatients. Arch. Pathol. Lab. Med. 133, 628–632. https://doi.org/10.1043/1543-2165-133.4.628 (2009).
Tanindi, A., Topal, F. E., Topal, F. & Celik, B. Red cell distribution width in patients with prehypertension and hypertension. Blood Press. 21, 177–181. https://doi.org/10.3109/08037051.2012.645335 (2012).
Libby, P., Ridker, P. M. & Maseri, A. Inflammation and atherosclerosis. Circulation 105, 1135–1143. https://doi.org/10.1161/hc0902.104353 (2002).
Dinh, Q. N., Drummond, G. R., Sobey, C. G. & Chrissobolis, S. Roles of inflammation, oxidative stress, and vascular dysfunction in hypertension. Biomed. Res. Int. 2014, 406960. https://doi.org/10.1155/2014/406960 (2014).
Son, M. & Yang, S. Association between long-term hemoglobin variability and mortality in Korean adults: a nationwide population-based cohort study. Sci. Rep. 9, 17285. https://doi.org/10.1038/s41598-019-53709-x (2019).
Vazquez, B. Y. et al. The variability of blood pressure due to small changes of hematocrit. Am. J. Physiol. Heart Circ. Physiol. 299, H863-867. https://doi.org/10.1152/ajpheart.00496.2010 (2010).
Emamian, M. et al. Association of hematocrit with blood pressure and hypertension. J. Clin. Lab. Anal. 31, e22124. https://doi.org/10.1002/jcla.22124 (2017).
Helms, C. C., Gladwin, M. T. & Kim-Shapiro, D. B. Erythrocytes and vascular function: oxygen and nitric oxide. Front. Physiol. 9, 125. https://doi.org/10.3389/fphys.2018.00125 (2018).
Ganidagli, S. E. et al. The relation between hemoglobin variability and carotid intima-media thickness in chronic hemodialysis patients. Int. Urol. Nephrol. 49, 1859–1866. https://doi.org/10.1007/s11255-017-1651-6 (2017).
Altunoren, O. et al. Effect of hemoglobin variability on mortality and some cardiovascular parameters in hemodialysis patients. Ren. Fail. 35, 819–824. https://doi.org/10.3109/0886022x.2013.801270 (2013).
Cooper, C. E. Nitric oxide and iron proteins. Biochim. Biophys. Acta 1411, 290–309. https://doi.org/10.1016/s0005-2728(99)00021-3 (1999).
Jeney, V., Balla, G. & Balla, J. Red blood cell, hemoglobin and heme in the progression of atherosclerosis. Front. Physiol. 5, 379. https://doi.org/10.3389/fphys.2014.00379 (2014).
Diez Roux, A. V. et al. Socioeconomic disadvantage and change in blood pressure associated with aging. Circulation 106, 703–710. https://doi.org/10.1161/01.cir.0000025402.84600.cd (2002).
Acknowledgements
This study was conducted using the database from the National Health Insurance System (NHIS-2019-2-132), and the results do not necessarily represent the opinion of the National Health Insurance Corporation. This study was supported by the National Research Foundation of Korea (NRF) grant funded by the Korean Government (MSIP) (NRF-2016M3A7B4910556). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. M.S., J.P. and K.P. contributed to the analysis and interpretation of data and drafting of the manuscript. K.P. and S.Y. contributed to critical revision of the manuscript for important intellectual content and statistical analysis, obtained funding, administrative, technical, material support and study supervision. All authors reviewed the manuscript and approved it for publication.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Son, M., Park, J., Park, K. et al. Association between hemoglobin variability and incidence of hypertension over 40 years: a Korean national cohort study. Sci Rep 10, 12061 (2020). https://doi.org/10.1038/s41598-020-69022-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-69022-x
- Springer Nature Limited