Key summary points
To evaluate inspiratory muscle function and the effect of a multicomponent exercise program including inspiratory muscle training during short-stay hospitalization.
AbstractSection FindingsInspiratory muscle impairment is very prevalent in the hospitalized elderly. Analysis of maximal inhibitory pressure revealed that those patients with inspiratory muscle weakness on admission showed the greatest improvement in inspiratory muscle strength.
AbstractSection MessageThese findings are especially relevant to identify those oldest-old patients who may benefit most from muscle inspiratory training during hospitalization for acute illness.
Abstract
Purpose
The impact of hospitalization for acute illness on inspiratory muscle strength in oldest-old patients is largely unknown, as are the potential benefits of exercise and inspiratory muscle training (IMT) during in-hospital stay.
Design and methods
This was a sub-study of a randomized clinical trial that evaluated the efficiency of a multicomponent exercise program in preventing hospitalization-associated disability. Patients were randomized into control (CG) and intervention (IG) groups. The intervention included two daily sessions of supervised walking, squat, balance, and IMT. Baseline and discharge maximal inspiratory pressure (MIP) and inspiratory muscle weakness (IMW) were determined. The effect of the intervention on inspiratory muscle strength was assessed by analyzing (1) the differences between groups in baseline and discharge MIP and IMW, (2) the association, patient by patient, between baseline and discharge MIP, and the improvement index (MIP discharge/baseline) in patients with or without IMW.
Results
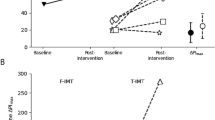
In total, 174 patients were assessed (mean age of 87), 57 in CG and 117 in IG. Baseline MIP was lower than predicted in both sexes (women 29.7 vs 44.3; men 36.7 vs 62.5 cmH2O, P < 0.001, baseline vs predicted, respectively). More than 65% of patients showed IMW at admission. In women in IG, the mean MIP was higher at discharge than at admission (P = 0.003) and was the only variable that reached expected reference levels at discharge (Measured MIP 39.2 vs predicted MIP 45 cmH2O, P = 0.883). Patients with IMW on admission showed a statistically significant improvement in MIP after the intervention.
Conclusion
IMW is very prevalent in oldest-old hospitalized with acute illness. Patients might benefit from a multicomponent exercise program including IMT, even during short-stay hospitalization.
Clinical trial registration
ClinicalTrials.gov; No.: NTC03604640. May 3, 2018.


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author.
References
Covinski KE, Palmer R, Fortinski R, Counsell S, Stewart A, Kresevic D (2003) Loss of independence in activities of daily living in older adults hospitalized with medical illnesses: increased vulnerability with age. JAGS 51:451–458
Fortinsky RH, Covinsky KE, Palmer RM, Landefeld CS (1999) Effects of functional status changes before and during hospitalization on nursing home admission of older adults. J Gerontol A Biol Sci Med Sci 54(10):M521-526
Gill TM, Allore HG, Holford TR, Guo Z (2004) Hospitalization, restricted activity, and the development of disability among older persons. JAMA 292(17):2115–2124
Inouye S, Wagner S, Acampora D, Horwitz D, Cooney LJ, Hurst L (1993) A predictive index for funtinal decline in hospitalized elderly medical patients. J Gen Intern Med 8:645–652
Brown CJ, Redden DT, Flood KL, Allman RM (2009) The underrecognized epidemic of low mobility during hospitalization of older adults. J Am Geriatr Soc 57(9):1660–1665
Van Ancum JM, Scheerman K, Jonkman NH et al (2017) Change in muscle strength and muscle mass in older hospitalized patients: a systematic review and meta-analysis. Exp Gerontol 92:34–41
Bachmann S, Finger C, Huss A, Egger M, Stuck AE, Clough-Gorr KM (2010) Inpatient rehabilitation specifically designed for geriatric patients: systematic review and meta-analysis of randomised controlled trials. BMJ 340:1718–1718
Martinez-Velilla N, Casas-Herrero A, Zambom-Ferraresi F et al (2019) Effect of exercise intervention on functional decline in very elderly patients during acute hospitalization: a randomized clinical trial. JAMA Intern Med 179(1):28–36
Ortiz-Alonso J, Bustamante-Ara N, Valenzuela PL et al (2020) Effect of a simple exercise program on hospitalization-associated disability in older patients: a randomized controlled trial. J Am Med Dir Assoc 21(4):531-537.e1. https://doi.org/10.1016/j.jamda.2019.11.027
Janssens JP, Pache JC, Nicod LP (1999) Physiological changes in respiratory function associated with ageing. Eur Respir J 13(1):197–205
Buchman AS, Boyle PA, Wilson RS, Leurgans S, Shah RC, Bennett DA (2008) Respiratory muscle strength predicts decline in mobility in older persons. Neuroepidemiology 31(3):174–180
Pegorari MS, Ruas G, Patrizzi LJ (2013) Relationship between frailty and respiratory function in the community-dwelling elderly. Braz J Phys Ther 17(1):9–16
Vidal MB, Pegorari MS, Santos EC, Matos AP, Pinto A, Ohara DG (2020) Respiratory muscle strength for discriminating frailty in community-dwelling elderly: a cross-sectional study. Arch Gerontol Geriatr 89:104082
American Thoracic Society/European Respiratory S (2002) ATS/ERS Statement on respiratory muscle testing. Am J Respir Crit Care Med 166(4):518–624
Laveneziana P, Albuquerque A, Aliverti A et al (2019) ERS statement on respiratory muscle testing at rest and during exercise. Eur Respir J. 53:6
Enright PL, Adams AB, Boyle PJ, Sherrill DL (1995) Spirometry and maximal respiratory pressure references from healthy Minnesota 65- to 85-year-old women and men. Chest 108(3):663–669
Rodrigues A, Da Silva ML, Berton DC et al (2017) Maximal inspiratory pressure: does the choice of reference values actually matter? Chest 152(1):32–39
Sclauser Pessoa IM, Franco Parreira V, Fregonezi GA, Sheel AW, Chung F, Reid WD (2014) Reference values for maximal inspiratory pressure: a systematic review. Can Respir J 21(1):43–50
Black LF, Hyatt RE (1969) Maximal respiratory pressures: normal values and relationship to age and sex. Am Rev Respir Dis 99(5):696–702
Evans JA, Whitelaw WA (2009) The assessment of maximal respiratory mouth pressures in adults. Respir Care 54(10):1348–1359
Dall’Ago P, Chiappa GR, Guths H, Stein R, Ribeiro JP (2006) Inspiratory muscle training in patients with heart failure and inspiratory muscle weakness: a randomized trial. J Am Coll Cardiol 47(4):757–763
Huang CH, Yang GG, Wu YT, Lee CW (2011) Comparison of inspiratory muscle strength training effects between older subjects with and without chronic obstructive pulmonary disease. J Formos Med Assoc 110(8):518–526. https://doi.org/10.1016/S0929-6646(11)60078-8
Seixas MB, Almeida LB, Trevizan PF et al (2020) Effects of inspiratory muscle training in older adults. Respir Care 65(4):535–544
Hill K, Jenkins SC, Philippe DL et al (2006) High-intensity inspiratory muscle training in COPD. Eur Respir J 27(6):1119–1128
Hill K, Jenkins SC, Hillman DR, Eastwood PR (2004) Dyspnoea in COPD: can inspiratory muscle training help? Aust J Physiother 50(3):169–180
Kendall F, Oliveira J, Peleteiro B, Pinho P, Bastos PT (2018) Inspiratory muscle training is effective to reduce postoperative pulmonary complications and length of hospital stay: a systematic review and meta-analysis. Disabil Rehabil 40(8):864–882
Nepomuceno BRV Jr, Barreto MS, Almeida NC, Guerreiro CF, Xavier-Souza E, Neto MG (2017) Safety and efficacy of inspiratory muscle training for preventing adverse outcomes in patients at risk of prolonged hospitalisation. Trials 18(1):626
Sanchez Riera H, Montemayor Rubio T, Ortega Ruiz F et al (2001) Inspiratory muscle training in patients with COPD: effect on dyspnea, exercise performance, and quality of life. Chest 120(3):748–756
Watsford M, Murphy A (2008) The effects of respiratory-muscle training on exercise in older women. J Aging Phys Act 16(3):245–260
Cebria IIMA, Balasch-Bernat M, Tortosa-Chulia MA, Balasch-Parisi S (2018) Effects of resistance training of peripheral muscles versus respiratory muscles in older adults with sarcopenia who are institutionalized: a randomized controlled trial. J Aging Phys Act 26(4):637–646
Cebria IIMD, Arnall DA, Igual Camacho C, Tomas JM, Melendez JC (2013) Physiotherapy intervention for preventing the respiratory muscle deterioration in institutionalized older women with functional impairment. Arch Bronconeumol 49(1):1–9
Souza H, Rocha T, Pessoa M et al (2014) Effects of inspiratory muscle training in elderly women on respiratory muscle strength, diaphragm thickness and mobility. J Gerontol A Biol Sci Med Sci 69(12):1545–1553
Ferraro FV, Gavin JP, Wainwright TW, McConnell AK (2022) Association between inspiratory muscle function and balance ability in older people: a pooled data analysis before and after inspiratory muscle training. J Aging Phys Act 30(3):421–433
Rodrigues GD, Gurgel JL, Goncalves TR, da Silva Soares (2018) Inspiratory muscle training improves physical performance and cardiac autonomic modulation in older women. Eur J Appl Physiol. 118(6):1143–1152
Manifield J, Winnard A, Hume E et al (2021) Inspiratory muscle training for improving inspiratory muscle strength and functional capacity in older adults: a systematic review and meta-analysis. Age Ageing 50(3):716–724
Altman DG, Schulz KF, Moher D et al (2001) The revised CONSORT statement for reporting randomized trials: explanation and elaboration. Ann Intern Med 134(8):663–694
Neder JA, Andreoni S, Lerario MC, Nery LE (1999) Reference values for lung function tests. II. Maximal respiratory pressures and voluntary ventilation. Braz J Med Biol Res. 32(6):719–727
Charlson M, Szatrowski TP, Peterson J, Gold J (1994) Validation of a combined comorbidity index. J Clin Epidemiol 47(11):1245–1251
Fried LP, Tangen CM, Walston J et al (2001) Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 56(3):M146-156
Kurczewska-Michalak M, Lewek P, Jankowska-Polanska B et al (2021) Polypharmacy management in the older adults: a scoping review of available interventions. Front Pharmacol 12:734045
Mahoney FI, Barthel DW (1965) Functional evaluation: the barthel index. Md State Med J 14:61–65
Holden MK, Gill KM, Magliozzi MR, Nathan J, Piehl-Baker L (1984) Clinical gait assessment in the neurologically impaired. Reliability and meaningfulness. Phys Ther 64(1):35–40
Guralnik JM, Winograd CH (1994) Physical performance measures in the assessment of older persons. Aging (Milano) 6(5):303–305
Kim SH, Shin MJ, Lee JM, Huh S, Shin YB (2022) Effects of a new respiratory muscle training device in community-dwelling elderly men: an open-label, randomized, non-inferiority trial. BMC Geriatr 22(1):155
Martin-Sanchez C, Barbero-Iglesias FJ, Amor-Esteban V, Martin-Nogueras AM (2021) Comparison between two inspiratory muscle training protocols, low loads versus high loads, in institutionalized elderly women: a double-blind randomized controlled trial. Gerontology 67(1):1–8
Morisawa T, Kunieda Y, Koyama S et al (2021) The relationship between sarcopenia and respiratory muscle weakness in community-dwelling older adults. Int J Environ Res Public Health 18(24):13257. https://doi.org/10.3390/ijerph182413257
Giua R, Pedone C, Scarlata S et al (2014) Relationship between respiratory muscle strength and physical performance in elderly hospitalized patients. Rejuvenation Res 17(4):366–371
Valenzuela PL, Ortiz-Alonso J, Bustamante-Ara N et al (2020) Individual responsiveness to physical exercise intervention in acutely hospitalized older adults. J Clin Med 9:3
Vidan MT, Sanchez E, Alonso M, Montero B, Ortiz J, Serra JA (2009) An intervention integrated into daily clinical practice reduces the incidence of delirium during hospitalization in elderly patients. J Am Geriatr Soc 57(11):2029–2036
Basso-Vanelli RP, Di Lorenzo VA, Labadessa IG et al (2016) Effects of inspiratory muscle training and calisthenics-and-breathing exercises in COPD with and without respiratory muscle weakness. Respir Care 61(1):50–60
Saez de Asteasu ML, Martinez-Velilla N, Zambom-Ferraresi F et al (2019) Inter-individual variability in response to exercise intervention or usual care in hospitalized older adults. J Cachexia Sarcopenia Muscle 10(6):1266–1275
Acknowledgements
We thank the geriatric ward staff for their valuable help and their contribution to our results, especially the following professionals: J. Ortiz, MT. Vidán, E. Santana, I. Ariza, FJ. Gómez-Olano, JP. Vasquez, S. González, P. Lavandera, A. Grau, P. Aldama, R. Valdovinos, G. Hernández, J. Ballesteros, J. Lozano, JM. García de Viguera, G. Fajardo and A. Paredes. We also thank the participants and their families.
Funding
The research reported in this study was supported by the following grants: Instituto de la Salud Carlos III (PI17/02021), CIBERFES, Fondo Europeo de Desarrollo Regional (FEDER). The work of JMC is supported by a contract granted by Biomedical Research Networking Center on Frailty and Healthy Aging (CIBERFES, Spain).
Author information
Authors and Affiliations
Contributions
All authors meet the criteria for authorship stated in the Uniform Requirements for Manuscripts Submitted to Biomedical Journals. Study concept and design: TZL, JASR, JMC. Acquisition of data: TZL, CCP, VRE. Analysis and interpretation of data: TZL, JASR, JMC. Drafting of the manuscript: TZL, JASR, JMC. Critical revision of the manuscript for important intellectual content: TZL, JASR, JMC.
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical approval
The Ethics Committee of the “Fundación para la Investigación Biomédica” from the “Hospital Universtario Gregorio Marañon, Madrid” approved the study (No. 07/2018). All the data were analyzed anonymously, and clinical investigations have been conducted according to the principles expressed in the Declaration of Helsinki.
Informed consent
Written informed consent for participation was obtained from all patients/relatives.
Role of sponsors
The sponsors were not involved in the design of this study, the data analysis, or the preparation of the manuscript.
Financial/nonfinancial disclosures
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zarralanga-Lasobras, T., Romero-Estarlich, V., Carrasco-Paniagua, C. et al. “Inspiratory muscle weakness in acutely hospitalized patients 75 years and over”: a secondary analysis of a randomized controlled trial on the effectiveness of multicomponent exercise and inspiratory muscle training. Eur Geriatr Med 15, 83–94 (2024). https://doi.org/10.1007/s41999-023-00865-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-023-00865-z