Abstract
Introduction
Prenatal alcohol exposure (PAE) impacts an estimated 5% or more children born in the USA and is associated with life-long neuropsychological deficits. Early identification is essential but access to diagnostic evaluation is limited. This study reports on the effectiveness of training child psychologists to identify and measure the salient physical features of PAE.
Methods
Children, 8–13 years, were divided into two groups: (1) children meeting criteria for PAE (n = 46) and (2) typically developing controls without PAE (TD; n = 36). Child psychologists were trained to reliability measure height, weight, occipital frontal circumference (OFC), and the characteristic facial features of FASD independent of knowledge of PAE history.
Results
Groups differed significantly on meeting the diagnostic criteria proposed by Hoyme et al. (Pediatrics, 138:e20154256, 2016) on height, OFC, upper vermillion border, philtrum, and palpebral fissure length. They did not differ on weight. All children in the alcohol exposed group could be classified as meeting criteria for an FASD whereas none in the unexposed group met criteria.
Discussion
This study demonstrated that child psychologists, blind to PAE history, could be reliably trained to assess the physical features of children with PAE. Because early diagnosis and intervention is of paramount importance, we propose that inclusive diagnostic criteria for FASD and the use of psychologists and other allied health professionals, trained to screen for the diagnosis, should be expanded in clinical practice.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Prenatal alcohol exposure (PAE) produces a range of developmental deficits collectively referred to under the umbrella term fetal alcohol spectrum disorders (FASDs) (Warren et al., 2011). The most severely affected children on the spectrum show a characteristic pattern of anomalies termed fetal alcohol syndrome (FAS) which consists of prenatal and/or postnatal growth retardation, a unique cluster of facial malformations, and neurodevelopmental disabilities (Hoyme et al., 2016; Jones & Smith, 1973; Mattson et al., 2019; O’Connor, 2014; Pei et al., 2011). Additionally, a substantial body of research has documented significant neuropsychological difficulties among individuals on the spectrum who do not meet full criteria for FAS but who fall along a continuum of disability and who are described as having partial FAS (pFAS), alcohol-related neurodevelopmental disorder (ARND), or alcohol-related birth defects (ARBD) according to the diagnostic schema proposed by the Institute of Medicine (IOM, Stratton et al., 1996) and updated by Hoyme et al. (2016). The demonstrated rate of developmental sequelae associated with PAE is estimated at up to 5% of the population in the USA and globally (Burd & Popova, 2019; May et al., 2018). Even higher rates are reported in populations of children in child-care systems (foster care, child welfare, etc.) ranging from 17 to 86.5% (Chasnoff et al., 2015; Lange et al., 2013). Despite the high prevalence of children suffering from sequelae associated with PAE, parents report that the number one challenge to obtaining a diagnosis for their child is the limited number of providers who can conduct an informed diagnostic evaluation (Petrenko et al., 2014).
Although the gold standard for diagnosis of an individual with PAE is one conducted at an FASD specialty clinic consisting of a team of professionals including clinical geneticists, psychologists, speech and language therapists, and physical therapists, these clinics are few and far between in the USA and elsewhere. As a consequence, it is estimated that less than 1% of individuals suffering from alcohol-related developmental sequelae are diagnosed (Burd & Popova, 2019) and only 11% of children with PAE are diagnosed before the age of 6 years in the USA (Centers for Disease Control and Prevention, 2004). In particular, the number of specialists in clinical genetics is quite low. The national number of active clinical geneticists, the group most likely to be involved in direct patient care, is approximately 4.68 per 1 million people in the USA and is not expected to improve in the near future (Maiese et al., 2019). The situation is even more dire when trying to locate a geneticist specifically trained to identify individuals with an FASD (Petrenko et al., 2014).
The shortage of qualified physicians and specialty FASD clinics speaks to the need to train other health professionals to identify the most prominent features associated with PAE (Burd & Popova, 2019). The importance of training a larger group of professionals to recognize these features is underscored by the fact that more positive developmental outcomes are achieved the earlier the diagnosis is made in the child’s life (Petrenko et al., 2014; Streissguth et al., 2004). According to Burd and Popova (2019), because of their developmental issues, most individuals with FASD are already in systems of care that, with modest modifications, could greatly improve their developmental trajectory. To improve access to expanded diagnosis and care, an ideal solution would be to train mental health professionals, who may already assess and treat a range of individuals with developmental disabilities, to screen for the seminal features associated with FASD. This training would be particularly helpful in areas of the country with limited specialized resources.
The purpose of this research was to report on the effectiveness of training child psychologists to identify and measure the most salient physical features used to make alcohol-associated diagnoses (Hoyme et al., 2016). Their assessments were performed, without knowledge of PAE history, on a group of children with known PAE versus a group of typically developing (TD) controls.
Materials and Methods
Participants
All procedures performed were in accordance with the ethical standards of the University Institutional Review Board (IRB) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Written copies of the consent/assent forms were given to all participants. Procedures were thoroughly described and read to participants with an opportunity to ask questions. All physical measurements were made in the presence of the child’s parent(s). All participants gave their informed consent/assent prior to study inclusion.
Children were recruited from community and parent organizations, national websites, community-posted flyers, direct mailings, and local child psychiatry/pediatric clinics. Recruitment flyers invited families of typically developing children or children who may have been exposed to alcohol prenatally to participate. This recruitment strategy yielded 196 inquiries with 82 children meeting screening and eligibility criteria.
Inclusion criteria for all participants were: Full-Scale IQ > 70 on the Wechsler Abbreviated Scale of Intelligence, Second Edition (WASI-II, Wechsler, 2011); gestation > 34 weeks; and English as the primary language in the home. Participants were excluded if they had been diagnosed with autism spectrum disorder, a specific genetic disorder, or neurological disorder.
Two groups of children, aged 8–13 years, were included in the sample: (1) children with PAE (n = 46) and (2) TD controls without PAE (TD; n = 36).
Regarding sample characteristics, 58.5% of the children were male, their mean age was 10.30 (SD = 1.61) years, 39% identified as White, non-Hispanic, 8.5% as Black/African American, 20.7% as Hispanic, 22% as Mixed Race, and 9.8% as Other. Average mother’s education (a proxy for socioeconomic status) was 16.70 (SD = 3.46 years).
Procedures
Overview
Briefly, all participants were screened for study eligibility including questions about prenatal alcohol exposure. Families meeting research inclusion criteria were asked to participate in the study. A demographic questionnaire and medical/developmental history were completed for every child. Eligible children were first administered the physical examination by the trained examiners and then completed a neuropsychological test battery conducted by different examiners naïve to prenatal alcohol history. Neurocognitive/behavioral impairment was used to finalize FASD classifications and was scored using criteria described in detail below. The mother was interviewed regarding her prenatal alcohol use privately in a one-to-one setting. In the absence of the biological mother, information was obtained via birth, medical, or adoption records, or from reports from reliable informants (see section on “Prenatal Alcohol Exposure” below).
Physical Examination
Every child was assessed for the presence of the diagnostic features of FASD using the modified IOM criteria according to the updated guidelines proposed in the Clinical Guidelines for Diagnosing Fetal Alcohol Spectrum Disorders (Hoyme et al., 2016). This system is the most commonly used methodology in ascertainment prevalence studies in the USA and in other countries (May et al., 2018). Moreover, it was designed for clinicians and is more inclusive in identifying individuals with salient physical feature of an FASD. The system examines the expression of four key diagnostic features of FAS: (1) growth retardation; (2) the FAS facial phenotype, including a flat upper vermillion border, flat philtrum, and short palpebral fissures; (3) neurocognitive/behavioral impairment; and (4) gestational alcohol exposure. Growth retardation was defined as height and/or weight at or below the 10th percentile on national growth charts at any point in time from birth. With regard to facial features, two of the three seminal facial features of FAS were required to be present (Hoyme et al., 2016). The upper vermillion border and philtrum were scored using a racially normed Lip-Philtrum Guide with scores of 4 or 5 meeting criteria consistent with PAE (Astley, 2013). Palpebral fissure length was scored using the Canadian palpebral fissure guidelines (Clarren et al., 2010) and the guidelines for Black/African American and Hispanic children from Iosub et al. (1985). The parent(s) provided information on preferred racial identity which determined which guide to use in the assessment of the face.
Prenatal Alcohol Exposure
Alcohol exposure was assessed using the Health Interview for Women (HIW) or the Health Interview for Adoptive and Foster Parents (HIAFP, Quattlebaum & O’Connor, 2013). The HIW assesses frequency and quantity of typical and binge drinking and use of other teratogens prior to and following recognition of pregnancy. For adopted/fostered participants, information on prenatal exposure to alcohol and other teratogens was obtained via birth, medical, or adoption records or reports by reliable informants. Because many individuals with FASD are adopted or fostered, it is often necessary to use such records, and this is a method accepted in the scientific community for establishing PAE (Centers for Disease Control and Prevention, 2004). Criteria for alcohol exposure reported by the biological mother included > 6 drinks/week for ≥ 2 weeks and/or ≥ 3 drinks on ≥ 2 occasions including the time periods prior to and following pregnancy recognition (Hoyme et al., 2016). These criteria are based on findings that 1 drink/day (or > 6 drinks/week) is an adequate measure of exposure for an FASD, and on epidemiologic studies demonstrating adverse fetal effects of episodic drinking of ≥ 3 drinks per occasion (Hoyme et al., 2016). No child in the alcohol exposed group was accepted without a clear history of PAE. Alcohol inclusion criterion for the TD group was PAE < 2 standard drinks throughout gestation.
Training Procedures and Measures
Training
Diagnostic training of two child psychologists began with exposure to reading materials on PAE, a thorough description of the criteria for diagnosis of FAS that included pictures of children’s faces, followed by a description of the measurements they were being trained to take on each child, and practice performing these measurements. Both examiners were observed administering the physical examination of several children with immediate feedback provided by the study senior alcohol researcher who had extensive training and expertise in the assessment of FASD. The examiners were trained to reliability and fidelity was checked throughout the study by the senior alcohol researcher. Both examiners were blind to the child’s history of exposure to alcohol prenatally.
Child Measurements
Child height and weight were measured in cm and kg, respectively, to assess for growth retardation. Children were asked to remove their shoes and heavy clothing. To measure height, children were asked to stand with feet flat together, with legs straight, arms at their sides, and shoulders level against a wall in front of a height chart calibrated in centimeters. They were instructed that their head, shoulders, and heels had to be touching the wall. A flat headpiece forming a right angle with the wall was lowered until it firmly touched the crown of the child’s head making sure the examiner’s eyes were at the same level as the headpiece. Height was measured to the nearest cm. Weight was measured using a digital scale on a flat surface. Children were instructed to stand still with both feet in the center of the scale. Weight was measured in kg to the nearest decimal fraction (for example, 25.1 kg) and then .5 kg was subtracted to account for clothing.
The occipital frontal circumference (OFC), considered a screening measure of central nervous system (CNS) integrity, was assessed using the standardized method of measurement with a flexible tape measure calibrated in cm. OFC was measured over the most prominent part of the back of the head (occiput) and just above the eyebrows (supraorbital ridges) in order to measure the largest circumference of the head. Measurements were repeated until 2 measurements yielded identical results.
Assessment of facial features included the use of the Astley (2013) Lip-Philtrum Guides for White or Black/African American children. The Lip-Philtrum Guide is a 5-point photographic guide that is used to objectively measure the flatness of the upper vermillion border and philtrum smoothness. A rank of 1 reflects a well-formed upper lip and a deeply grooved philtrum. As one moves up the guide from a rank of 1 to a rank of 5, the upper vermillion border is portrayed as becoming flatter and the philtrum as becoming smoother. The rank of 5 reflects an upper vermillion border that is completely flat or philtrum that is completely smooth. A score of 4 or 5 on each feature meets criterion for face. Measurements were taken with the child and examiner seated facing one another at eye level with the guide held to the side of the child’s face. Children were asked to relax their facial expression, without smiling, and with their lips gently closed (a smile can cause the upper lip and philtrum to appear flatter and smoother than they actually are). Lip and philtrum were each measured separately.
To measure the length of the palpebral fissures, the examiner sat at eye level in front of the child and placed one hand lightly on the top of the child’s head to prevent the child from lifting the head. The children were asked to open their eyes widely and to direct their gaze up to the ceiling without lifting their heads. The lengths of the right and left palpebral fissures were measured with a plastic ruler (1 cm by 14 cm in size) calibrated in mm held as closely as possible to the bottom of the opening of the eye without touching the eye or eye lashes. Measurements were taken between the endocanthion and the exocanthion landmarks (Astley, 2013). The measurement of the smallest of the two palpebral fissures was used in analysis.
Diagnostic Criteria for Physical Characteristics
Physical features of height, weight, and OFC were converted to percentiles according to sex and age-based CDC Growth Charts: United States (Kuczmarski, 2002) for individuals 2 to 20 years using the Simulconsult calculator (Simulconsult.com). Upper vermillion border and philtrum ratings were scored using the Astley Lip-Philtrum Guide (Astley, 2013). The smallest of the right or left palpebral fissure was scored based on sex and age percentile norms for White/non-Hispanic children reported by Clarren et al. (2010) and norms for Black/African American and Hispanic children reported by Iosub et al. (1985). All measurements then were scored as “yes” or “no” based on whether or not participants met the physical diagnostic criteria proposed by Hoyme et al. (2016): height (≤ 10th percentile), weight (≤ 10th percentile), OFC (≤ 10th percentile), upper vermillion border (≥ rank 4), philtrum (≥ rank 4), and palpebral fissure (≤ 10th percentile).
Reliability of Measurements of Facial Features
Deidentified digital photographs of participants’ faces were scored for reliability in meeting facial criteria by the study senior investigator who had extensive training and experience using the diagnostic system. Taken together, kappas for the whole sample were 0.95 for upper vermillion border, 0.93 for philtrum, and 0.90 for palpebral fissure length.
Confirmatory Diagnoses of an FASD
Deidentified scoring sheets containing all physical and neurocognitive/behavioral findings for each participant were assigned a confirmatory diagnostic classification for each child along the FASD spectrum. Neurocognitive/behavioral impairment was defined less conservatively than the criterion proposed by Hoyme et al. (2016) and was considered significant if the participant demonstrated functioning more than 1 standard deviation below or above the mean depending on whether or not a lower or higher score indicated higher levels of deficit functioning on standardized measures of neurocognitive and socioemotional development. Given the relatively higher IQs of our subjects (IQs of > 70), we determined that it was unlikely that 1 ½ standard deviations from the mean, as proposed by Hoyme et al. (2016), would adequately capture subtler deficits that might characterize this group of individuals. Moreover, these criteria are in accordance with the report by Doyle and Mattson (2015) suggesting that for most standardized neurocognitive measures, 1 standard deviation from the mean typically indicates problems in behavior or neurocognitive development.
Statistical Analysis
Group differences in demographic and morphological characteristics were evaluated using ANOVA for continuous variables and two-tailed Fisher’s exact tests for categorical variables using SPSS v27 (IBM Corp., Armonk, NY).
Results
Physical Features
Group differences on demographic and morphological variables are presented in Table 1. Groups did not differ on demographic characteristics of sex, ethnicity, or current primary caregiver’s education. Although groups differed on age, all physical parameters in the study had already been adjusted for sex and age and presented as meeting (yes) or not meeting (no) diagnostic criteria, so outcome variables were not adjusted for age. Fisher’s exact tests of whether or not participants’ scores met criteria of ≤ 10th percentile revealed statistically significant group differences in height and OFC but not weight. Similarly, analyses of upper vermillion border (score ≥ 4), philtrum (score ≥ 4), and palpebral fissure lengths (≤ 10th percentile) revealed significant differences between groups (Table 1). Table 2 presents a summary of the percentages of physical features seen in each diagnostic classification along the spectrum.
Final Diagnostic Classifications
All children in the PAE group met Hoyme et al. (2016) confirmatory criteria for a diagnosis along the spectrum of prenatal alcohol exposure while none of the children in the TD control group met criteria. Using this classification scheme, 26% (n = 12) of children in the PAE group were classified as having FAS; 50% (n = 23) as having pFAS; and 24% (n = 11) as having ARND.
Discussion
The importance of this study is highlighted by the finding that screening for an FASD can be mastered by child psychologists who are often in positions to evaluate and treat children with PAE. They are typically trained to assess neuropsychological functioning using standardized instruments and treatment approaches and are often familiar with other therapeutic resources in the community. Given the scarcity of FASD specialists in the USA, this approach to the public health needs of children affected by PAE and their families is promising. According to the parents of children with PAE, systems level barriers interfere with their ability to obtain a diagnosis primarily due to a lack of knowledge and understanding of FASD in the health community (Petrenko et al., 2014). Training not only child psychologists but also other professionals such as nurse practitioners, pediatricians, child psychiatrists, family medicine physicians, speech pathologists, and school nurses to recognize this developmental disability that affects more than 1 in 20 children in the USA can go a long way to breaking down these barriers to care.
An interesting finding regarding the growth criterion was that although height distinguished between children with PAE and typically developing controls, weight did not. Further, both the PAE and TD control groups’ average percentiles for both height and weight were in the normal range with wide variability. Although growth retardation was a requirement for a diagnosis of FAS in our sample, no child meeting facial features or neurocognitive/behavioral impairment criteria for pFAS demonstrated growth retardation. This finding calls into question the use of growth retardation as a criterion for distinguishing between FAS and pFAS. Of note, the most recent Canadian diagnostic guidelines for FASD were updated deleting growth as a diagnostic criterion as experts determined it was not a distinguishing feature (Cook et al., 2016).
The importance of facial dysmorphology for distinguishing between children with PAE and their typically developing peers deserves further discussion. Facial features described in children with PAE reflect development of the neural crest during the first trimester of gestation, often before a woman even knows she is pregnant (Smith et al., 2014). Ethanol disrupts multiple events of neural crest development, including induction, survival, migration, and differentiation (Smith et al., 2014). Due to the shared molecular mechanisms and genetic influences on face and brain, brain development can also be understood in the context of the alcohol-induced facial malformations. One possible explanation for the teratology of alcohol during gestation includes excessive cell death or apoptosis during both embryogenesis (4th week of gestation) and synaptogenesis (third trimester of gestation) which can cause the death of cell populations that are essential for normal development of both the face and the brain including brain mass (Creeley & Olney, 2013).
Although OFC (assumed to be related to brain mass) in the PAE group met criterion (≤ 10th percentile) at a statistically significant greater frequency than in the TD control group, only 9/46 participants or 19.6% in the total PAE group could be classified as deficient. This deficiency was largely accounted for by participants diagnosed with FAS (n = 8/12, 66.7%) as opposed to those with pFAS (n = 0) or ARND (n = 1/11, 9.1%). No child in the TD control group met criterion (n = 0). The fact that few study participants met criterion for a small OFC in the PAE group might relate to the possibility that the majority of women in our sample may have decreased or stopped drinking in the third trimester of their pregnancies, a period of rapid brain growth during which EtOH causes accelerated cell death (Creeley & Olney, 2013). This is consistent with previous findings that 7% or less women report alcohol use at the end of pregnancy in the USA (Burd & Popova, 2019; Substance Abuse and Mental Health Data Archive, 2015). Unfortunately, we did not collect drinking data by trimester so we cannot confirm this speculation.
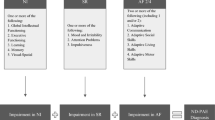
As a final note, we address issues in convergent validity among different clinical classification systems currently used to identify children with PAE (Coles et al., 2013). Coles et al. (2013) found the percentage of individuals diagnosed with an FASD across various classification systems currently in use ranged from 4.7 to 59.6%. Variability across various systems was attributed to differences in classification criteria, a lack of standardized norms for different ethnic groups, and problems achieving interrater reliability of diagnosis among clinicians. Because reliance on the physical characteristics of individuals with PAE can yield different diagnostic conclusions, the NIAAA organized a diagnostic working group that met with experts in the field to establish criteria that could be used by clinicians without the need for assessment of physical features (Kabel et al., 2016). This group proposed diagnostic criteria for what they coined, Neurobehavioral Disorder Associated with Prenatal Alcohol Exposure (ND-PAE), which is published in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5, 2013, p. 783). This behavioral description of individuals with PAE allows clinicians, from a variety of professional backgrounds, to make a diagnosis in the presence or absence of the morphological characteristics of FAS. According to the DSM-5, ND-PAE requires dysfunction in three symptom domains: neurocognitive, self-regulation, and adaptive functioning. Currently, ND-PAE is classified as a “condition for further study” in the DSM-5; however, clinicians can make a diagnosis under “Other Specified Neurodevelopmental Disorder Associated with Prenatal Alcohol Exposure” (DSM-5, 2013, p. 86) using the behavioral phenotype described in ND-PAE as a basis for diagnosis. This diagnosis allows for professional reimbursement for services related to the condition. Results of research comparing ND-PAE criteria to a checklist of ARND diagnostic criteria in a clinic-referred sample revealed agreement of 85.7% between the two systems suggesting the practical clinical utility of this approach (Johnson et al., 2018). If future research clearly demonstrates that the behavioral phenotype described under ND-PAE is unique to individuals with PAE, the need for more sophisticated morphological assessment may become less important (Burd & Popova, 2019).
The results of the present study should be interpreted in light of its limitations. First, study findings are limited by sampling constraints. This study relied on a sample from the greater Los Angeles area and stratified sampling techniques were not applied. Although our sample was not drawn from a clinic population, we found that 26% of alcohol exposed children in our sample met criteria for FAS, a percentage higher than reported in the ascertainment prevalence literature (May et al., 2018). One reason for this discrepancy may have been our less conservative criterion for neurocognitive/behavioral deficits. A second reason may be that some parents may have brought their child to our neuropsychiatric setting because they had concerns about PAE being a possible etiology of the child’s developmental issues as our flyers advertised for children with and without PAE. Finally, 59% of study participants in the PAE group were adopted or living in foster care rather than with their biological mothers compared to none of the TD controls introducing another possible bias resulting in a higher proportion of children in the PAE group receiving an FAS diagnostic classification. This possibility is of concern because the majority of children who receive a diagnosis of an FASD are not living with their biological parents due to early removal from the home; adoption from Eastern European countries with high levels of maternal alcohol misuse; or physician reluctance to inquire of biological mothers about past alcohol use during pregnancy because of its associated stigma (Petrenko & Alto, 2017).
In conclusion, this study demonstrated that child psychologists could be trained to identify the physical features of children with an FASD. A benefit of training these professionals to identify the physical features of FASD is that many are already skilled in standardized methods of assessment of neuropsychological functioning and treatment to address the individual needs of children and their families. Moreover, it is paramount that all professionals working with families be trained to take a sensitive history of alcohol use. Positive findings should be explained to the parent and concerns addressed. The results of this study are particularly encouraging given that resources for evaluation and treatment of individuals with FASD in much of the USA are extremely scarce. Because early diagnosis and initiation of intervention should be of paramount importance, we propose that inclusive diagnostic criteria for FASD and the use of child psychologists and other allied health professionals trained to screen for the diagnosis should be expanded in clinical practice.
References
Astley, S. J. (2013). Validation of the fetal alcohol spectrum disorder (FASD) 4-digit diagnostic code. Journal of population therapeutics and clinical pharmacology = Journal de la therapeutique des populations et de la pharmacologie clinique, 20(3), e416–e467.
Burd, L., & Popova, S. (2019). Fetal alcohol spectrum disorders: Fixing our aim to aim for the fix. International Journal of Environmental Research and Public Health, 16, 3978. https://doi.org/10.3390/ijerph16203978 PMID: 31635265; PMCID: PMC6843765.
Centers for Disease Control and Prevention. (2004). Fetal alcohol syndrome: Guidelines for referral and diagnosis. Atlanta, GA: Department of Health and Human Services. http://www.cdc.gov/ncbddd/fasd/documents/fas_guidelines_accessible.pdf. Accessed February 2016.
Chasnoff, I. J., Wells, A. M., & King, L. (2015). Misdiagnosis and missed diagnoses in foster and adopted children with prenatal alcohol exposure. Pediatrics, 135(2), 264–270. https://doi.org/10.1542/peds.2014-2171 PMID: 25583914.
Clarren, S. K., Chudley, A. E., Wong, L., Friesen, J., & Brant, R. (2010). Normal distribution of palpebral fissure lengths in Canadian school age children. The Canadian Journal of Clinical Pharmacology, 17(1), 68–78.
Coles, C. D., Gailey, A. R., Mulle, J. G., Kable, J. A., Lynch, M. E., & Jones, K. L. (2016). A comparison among 5 methods for the clinical diagnosis of fetal alcohol spectrum disorders. Alcoholism, Clinical and Experimental Research, 40(5), 1000–1009. https://doi.org/10.1111/acer.13032.
Cook, J. L., Green, C. R., Lilley, C. M., Anderson, S. M., Baldwin, M. E., Chudley, A. E., Conry, J. L., LeBlanc, N., Loock, C. A., Lutke, J., Mallon, B. F., McFarlane, A. A., Temple, V. K., Rosales, T., & Canada Fetal Alcohol Spectrum Disorder Research Network. (2016). Fetal alcohol spectrum disorder: A guideline for diagnosis across the lifespan. CMAJ: Canadian Medical Association journal = journal de l’Association medicale canadienne, 188(3), 191–197. https://doi.org/10.1503/cmaj.14159310.1503/cmaj.141593 Epub 2015 Dec 14. PMID: 26668194; PMCID: PMC4754181.
Creeley, C. E., & Olney, J. W. (2013). Drug-induced apoptosis: Mechanism by which alcohol and many other drugs can disrupt brain development. Brain Sciences, 3(3), 1153–1181. https://doi.org/10.3390/brainsci3031153
Doyle, L. R., & Mattson, S. N. (2015). Neurobehavioral disorder associated with prenatal alcohol exposure (ND-PAE): Review of evidence and guidelines for assessment. Current Developmental Disorders Reports, 2, 175–186.
Hoyme, H. E., Kalberg, W. O., Elliott, A. J., Blankenship, J., Buckley, D., Marais, A. S., Manning, M. A., Robinson, L. K., Adam, M. P., Abdul-Rahman, O., Jewett, T., Coles, C. D., Chambers, C., Jones, K. L., Adnams, C. M., Shah, P. E., Riley, E. P., Charness, M. E., Warren, K. R., & May, P. A. (2016). Updated clinical guidelines for diagnosing fetal alcohol spectrum disorders. Pediatrics, 138(2), e20154256.
Iosub, S., Fuchs, M., Bingol, N., Stone, R. K., Gromisch, D. S., & Wasserman, E. (1985). Palpebral fissure length in Black and Hispanic children: Correlation with head circumference. Pediatrics, 75(2), 318–320.
Johnson, S., Moyer, C. L., Klug, M. G., & Burd, L. (2018). Comparison of alcohol-related neurodevelopmental disorders and neurodevelopmental disorders associated with prenatal alcohol exposure diagnostic criteria. Journal of developmental and behavioral pediatrics: JDBP, 39(2), 163–167. https://doi.org/10.1097/DBP.0000000000000523
Jones, K. L., & Smith, D. W. (1973). Recognition of the fetal alcohol syndrome in early infancy. The Journal-Lancet, 302, 999–1001.
Kabel, J. A., O’Connor, M. J., Carmichael Olson, H., Paley, B., Mattson, S. N., Anderson, S. M., & Riley, E. P. (2016). Neurobehavioral disorder associated with prenatal alcohol exposure (ND-PAE); proposed DSM-5 diagnosis. Child Psychiatry and Human Development, 47(2), 335–346. https://doi.org/10.1007/s10578-015-0566-7
Kuczmarski, R. J., Ogden, C. L., Guo, S. S., Grummer-Strawn, L. M., Flegal, K. M., Mei, Z., Wei, R., Curtin, L. R., Roche, A. F., & Johnson, C. L. (2002). 2000 CDC Growth Charts for the United States: methods and development. Vital and health statistics. Series 11, Data from the National Health Survey, (246), 1–190
Lange, S., Shield, K., Rehm, J., & Popova, S. (2013). Prevalence of fetal alcohol spectrum disorders in child care settings: A meta-analysis. Pediatrics, 132(4), e980–e995. https://doi.org/10.1542/peds.2013-0066
Maiese, D. R., Keehn, A., Lyon, M., Flannery, D., Watson, M., & Working Groups of the National Coordinating Center for Seven Regional Genetics Service Collaboratives. (2019). Current conditions in medical genetics practice. Genetics in Medicine: Official journal of the American College of Medical Genetics, 21(8), 1874–1877. https://doi.org/10.1038/s41436-018-0417-6
Mattson, S. N., Bernes, G. A., & Doyle, L. R. (2019). Fetal alcohol spectrum disorders: A review of the neurobehavioral deficits associated with prenatal alcohol exposure. Alcoholism, Clinical and Experimental Research, 43(6), 1046–1062. https://doi.org/10.1111/acer.14040
May, P. A., Chambers, C. D., Kalberg, W. O., Zellner, J., Feldman, H., et al.. (2018). Prevalence of fetal alcohol spectrum disorders in 4 US communities. Journal of the American Medical Association, 319(5), 474–482. https://doi.org/10.1001/jama.2017.21896
O’Connor, M. J. (2014). Mental health outcomes associated with prenatal alcohol exposure: Genetic and environmental factors. Current Developmental Disorders Reports. https://doi.org/10.1007/s40474-014-0021-7
Pei, J., Denys, K., Hughes, J., & Rasmussen, C. (2011). Mental health issues in fetal alcohol spectrum disorder. Journal of Mental Health, 20(5), 473–483. https://doi.org/10.3109/09638237.2011.577113
Petrenko, C. L., & Alto, M. E. (2017). Interventions in fetal alcohol spectrum disorders: An international perspective. European Journal of Medical Genetics, 60(1), 79–91. https://doi.org/10.1016/j/ejmg.2016.10.005
Petrenko, C. L., Tahir, N., Mahoney, E. C., & Chin, N. P. (2014). Prevention of secondary conditions in fetal alcohol spectrum disorders: Identification of systems-level barriers. Maternal and Child Health Journal, 18(6), 496–505. https://doi.org/10.1007/s10995-013-1390-y PMID: 24178158; PMCID: PMC4007413.
Quattlebaum, J. L., & O’Connor, M. J. (2013). Higher functioning children with prenatal alcohol exposure: Is there a specific neurocognitive profile? Child Neuropsychology, 19(6), 561–578. https://doi.org/10.1080/09297049.2012.713466.
Smith, S. M., Garic, A., Flentke, G. R., & Berres, M. E. (2014). Neural crest development in fetal alcohol syndrome. Birth Defects Research. Part C, Embryo Today: Reviews, 102(3), 210–220. https://doi.org/10.1002/bdrc.21078
Stratton, K. R., Howe, C. J., & Battaglia, F. C. (eds.). (1996). Fetal alcohol syndrome: Diagnosis, epidemiology, prevention, and treatment. Washington, DC: National Academy Press.
Streissguth, A. P., Bookstein, F. L., Barr, H. M., Sampson, P. D., O’Malley, K., & Young, J. K. (2004). Risk factors for adverse life outcomes in fetal alcohol syndrome and fetal alcohol effects. Journal of Developmental and Behavioral Pediatrics: JDBP, 25(4), 228–238. https://doi.org/10.1097/00004703-200408000-00002SPSSv27 (IBM Corp., Armonk, NY).
Substance Abuse and Mental Health Data Archive. (2015). National survey on drug use and health: 10-year substate R-DAS (NSDUH-2002-2011). Volume 2018. https://www.datafiles.samhsa.gov/study/national-survey-drug-use-and-health-nsduh-2002-nid13623. Accessed on 15 May 1021.
Warren, K. R., Hewitt, B. G., & Thomas, J. D. (2011). Fetal alcohol spectrum disorders: Research challenges and opportunities. Alcohol Research & Health, 34, 4–14.
Wechsler, D. (2011). Wechsler abbreviated scale of intelligence–second edition (WASI-II). NCS Pearson.
Availability of Data and Material
Deidentified data are available.
Funding
This research was supported by a grant from the National Institute on Alcohol Abuse and Alcoholism Number RO1AA025066 (M. O’Connor and J. Levitt, Co-PIs). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute on Alcohol Abuse and Alcoholism or the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
MJOC, JGL, and JON contributed to study design and oversight; AD and KMB measured and scored the physical features of the children; JRA and SHJ provided statistical guidance and edits to the manuscript; and MJOC prepared the manuscript with the assistance of LAK. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
All procedures performed involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Consent to Participate
The University Institutional Review Board approved all procedures. All procedures were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Parents and children gave their informed consent/assent prior to study inclusion.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
O’Connor, M.J., Dillon, A., Best, K.M. et al. Identification of Seminal Physical Features of Prenatal Alcohol Exposure by Child Psychologists. J Pediatr Neuropsychol 8, 60–67 (2022). https://doi.org/10.1007/s40817-022-00123-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40817-022-00123-3