Abstract
Background
The prevalence of chronic kidney disease (CKD) is high. Identification of cases with CKD or at high risk of developing it is important to tailor early interventions. The objective of this study was to identify blood metabolites associated with prevalent and incident severe CKD, and to quantify the corresponding improvement in CKD detection and prediction.
Methods
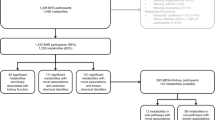
Data from four cohorts were analyzed: Singapore Epidemiology of Eye Diseases (SEED) (n = 8802), Copenhagen Chronic Kidney Disease (CPH) (n = 916), Singapore Diabetic Nephropathy (n = 714), and UK Biobank (UKBB) (n = 103,051). Prevalent CKD (stages 3–5) was defined as estimated glomerular filtration rate (eGFR) < 60 mL/min/1.73 m2; incident severe CKD as CKD-related mortality or kidney failure occurring within 10 years. We used multivariable regressions to identify, among 146 blood metabolites, those associated with CKD, and quantify the corresponding increase in performance.
Results
Chronic kidney disease prevalence (stages 3–5) and severe incidence were 11.4% and 2.2% in SEED, and 2.3% and 0.2% in UKBB. Firstly, phenylalanine (Odds Ratio [OR] 1-SD increase = 1.83 [1.73, 1.93]), tyrosine (OR = 0.75 [0.71, 0.79]), docosahexaenoic acid (OR = 0.90 [0.85, 0.95]), citrate (OR = 1.41 [1.34, 1.47]) and triglycerides in medium high density lipoprotein (OR = 1.07 [1.02, 1.13]) were associated with prevalent stages 3–5 CKD. Mendelian randomization analyses suggested causal relationships. Adding these metabolites beyond traditional risk factors increased the area under the curve (AUC) by 3% and the sensitivity by 7%. Secondly, lactate (HR = 1.33 [1.08, 1.64]) and tyrosine (HR = 0.74 [0.58, 0.95]) were associated with incident severe CKD among individuals with eGFR < 90 mL/min/1.73 m2 at baseline. These metabolites increased the c-index by 2% and sensitivity by 5% when added to traditional risk factors.
Conclusion
The performance improvements of CKD detection and prediction achieved by adding metabolites to traditional risk factors are modest and further research is necessary to fully understand the clinical implications of these findings.
Graphical Abstract



Similar content being viewed by others
Data availability
Regarding Singapore Epidemiology of Eye Diseases data, in order to adhere to local IRB guidelines, we regret to inform that we are unable to share data relevant to this study openly. Nevertheless, we respectfully urge interested parties to contact corresponding author for further enquiries if necessary.
References
Bikbov B, Purcell CA, Levey AS, Smith M, Abdoli A, Abebe M et al (2020) Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. The Lancet 395:709–733
Coresh J, Selvin E, Stevens LA, Manzi J, Kusek JW, Eggers P et al (2007) Prevalence of chronic kidney disease in the United States. JAMA 298:2038–2047
Hsu C, Vittinghoff E, Lin F, Shlipak MG (2004) The incidence of end-stage renal disease is increasing faster than the prevalence of chronic renal insufficiency. Ann Intern Med 141:95–101
Plantinga LC, Boulware LE, Coresh J, Stevens LA, Miller ER, Saran R et al (2008) Patient awareness of chronic kidney disease: trends and predictors. Arch Intern Med 168:2268–2275
Jha V, Garcia-Garcia G, Iseki K, Li Z, Naicker S, Plattner B et al (2013) Chronic kidney disease: global dimension and perspectives. Lancet 382:260–272
Dunkler D, Kohl M, Heinze G, Teo KK, Rosengren A, Pogue J et al (2015) Modifiable lifestyle and social factors affect chronic kidney disease in high-risk individuals with type 2 diabetes mellitus. Kidney Int 87:784–791
Stanzick KJ, Li Y, Schlosser P, Gorski M, Wuttke M, Thomas LF et al (2021) Discovery and prioritization of variants and genes for kidney function in >1.2 million individuals. Nat Commun 12:4350
Collins AJ, Foley RN, Gilbertson DT, Chen S-C (2015) United states renal data system public health surveillance of chronic kidney disease and end-stage renal disease. Kidney Int Suppl 5:2–7
Fassett RG, Venuthurupalli SK, Gobe GC, Coombes JS, Cooper MA, Hoy WE (2011) Biomarkers in chronic kidney disease: a review. Kidney Int 80:806–821
Wang Y-N, Ma S-X, Chen Y-Y, Chen L, Liu B-L, Liu Q-Q et al (2019) Chronic kidney disease: biomarker diagnosis to therapeutic targets. Clin Chim Acta 499:54–63
Chen H, Chen L, Liu D, Chen D-Q, Vaziri ND, Yu X-Y et al (2017) Combined clinical phenotype and lipidomic analysis reveals the impact of chronic kidney disease on lipid metabolism. J Proteome Res 16:1566–1578
Duranton F, Lundin U, Gayrard N, Mischak H, Aparicio M, Mourad G et al (2014) Plasma and urinary amino acid metabolomic profiling in patients with different levels of kidney function. CJASN 9:37–45
Goek O-N, Döring A, Gieger C, Heier M, Koenig W, Prehn C et al (2012) Serum metabolite concentrations and decreased GFR in the general population. Am J Kidney Dis 60:197–206
Chen D-Q, Cao G, Chen H, Liu D, Su W, Yu X-Y et al (2017) Gene and protein expressions and metabolomics exhibit activated redox signaling and wnt/β-catenin pathway are associated with metabolite dysfunction in patients with chronic kidney disease. Redox Biol 12:505–521
Luo S, Coresh J, Tin A, Rebholz CM, Appel LJ, Chen J et al (2019) Serum metabolomic alterations associated with proteinuria in CKD. CJASN 14:342–353
Hallan S, Afkarian M, Zelnick LR, Kestenbaum B, Sharma S, Saito R et al (2017) Metabolomics and gene expression analysis reveal down-regulation of the citric acid (TCA) cycle in non-diabetic CKD patients. EBioMedicine 26:68–77
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF, Feldman HI et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612
Soininen P, Kangas AJ, Würtz P, Suna T, Ala-Korpela M (2015) Quantitative serum nuclear magnetic resonance metabolomics in cardiovascular epidemiology and genetics. Circ Cardiovasc Genet 8:192–206
Ellul S, Wake M, Clifford SA, Lange K, Würtz P, Juonala M et al (2019) Metabolomics: population epidemiology and concordance in Australian children aged 11–12 years and their parents. BMJ Open 9:106–117
Qian C, Nusinovici S, Thakur S, Soh ZD, Majithia S, Chee ML et al (2022) Machine learning identifying peripheral circulating metabolites associated with intraocular pressure alterations. Br J Ophthalmol. https://doi.org/10.1136/bjophthalmol-2021-320584
Lee J, Choi J-Y, Kwon Y-K, Lee D, Jung H-Y, Ryu H-M et al (2016) Changes in serum metabolites with the stage of chronic kidney disease: comparison of diabetes and non-diabetes. Clin Chim Acta 459:123–131
Kopple JD (2007) Phenylalanine and tyrosine metabolism in chronic kidney failure. J Nutr 137:1586S-1590S
Jia L, Chen J, Yin P, Lu X, Xu G (2008) Serum metabonomics study of chronic renal failure by ultra performance liquid chromatography coupled with Q-TOF mass spectrometry. Metabolomics 4:183–189
Toyohara T, Akiyama Y, Suzuki T, Takeuchi Y, Mishima E, Tanemoto M et al (2010) Metabolomic profiling of uremic solutes in CKD patients. Hypertens Res 33:944–952
Qi S, Ouyang X, Wang L, Peng W, Wen J, Dai Y (2012) A pilot metabolic profiling study in serum of patients with chronic kidney disease Based on 1 H-NMR-spectroscopy. Clin Transl Sci 5:379–385
Roointan A, Gheisari Y, Hudkins KL, Gholaminejad A (2021) Non-invasive metabolic biomarkers for early diagnosis of diabetic nephropathy: meta-analysis of profiling metabolomics studies. Nutr Metab Cardiovasc Dis 31:2253–2272
Zhang Z-H, Li M-H, Liu D, Chen H, Chen D-Q, Tan N-H et al (2018) Rhubarb protect against tubulointerstitial fibrosis by inhibiting TGF-β/Smad pathway and improving abnormal metabolome in chronic kidney disease. Front Pharmacol 9:1029
Bermúdez-López M, Arroyo D, Betriu À, Masana L, Fernández E, Valdivielso JM (2017) New perspectives on CKD-induced dyslipidemia. Expert Opin Ther Targets 21:967–976
Yu Z, Kastenmüller G, He Y, Belcredi P, Möller G, Prehn C et al (2011) Differences between human plasma and serum metabolite profiles. PLoS ONE 6:e21230
Funding
This study was funded by: Singapore Epidemiology of Eye Diseases: National Medical Research Council (NMRC): NMRC/CIRG/1371/2013, NMRC/CIRG/1488/2018, NMRC/STaR/016/2013 and NMRC/OFLCG/001/2017. Singapore Diabetic Nephropathy cohort: Singapore Alexandra Health Fund Research Program and STAR grant 20201, National Medical Research Council NMRC/MOH-000066, NMRC/MOH-0000714 and OFLCG/001/2017. The Augustinus Foundation, the Danish Kidney Foundation, the Danish Society of Nephrology Foundation, the Helen and Ejnar Bjørnow Foundation, the Research Fund at Rigshospitalet, the Advokat Bent Thorbergs Foundation, and the Danish Diabetes Academy.
Author information
Authors and Affiliations
Contributions
Substantial contributions to the conception or design of the work (SN, TYW, GSWT, CS); or the acquisition (MY, IMHS, LSB, CC, SB, JJL, LSC, CYC), analysis (SN, HL, CC, MY, SL), or interpretation of data for the work (SN, HL, IMHS, LSB, CC, SB, JJL, LSC, TYW, GSWT, CYC, CS). Drafting the work (SN, HL, IMHS, LSB, JJL, CS) or revising it critically for important intellectual content (CC, MY, CC, SB, SL, LSC, TYW, GSWT, CYC). Final approval of the version to be published (all the authors). Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved (all the authors).
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Ethical approval
This study was performed in line with the principles of the 1964 Declaration of Helsinki. Approvals were granted by the Institutional Review Board of SingHealth (Singapore Epidemiology of Eye Disease study), the Regional Scientific Ethical Committee and the Danish Data Protection Agency (Copenhagen Chronic Kidney Disease study), the Singapore National Healthcare Group ethics committee (Singapore Diabetic Nephropathy study), and the North West Multi-centre Research Ethics Committee (MREC), the Research Tissue Bank (RTB) as well as a Human Tissue Authority (HTA) licence (UK Biobank study).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nusinovici, S., Li, H., Chong, C. et al. Blood biomarkers improve the prediction of prevalent and incident severe chronic kidney disease. J Nephrol (2024). https://doi.org/10.1007/s40620-023-01872-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40620-023-01872-w