Abstract
Background
Interest in physical and mental health outcomes in caregivers of patients with dementia is increasing. However, there is limited data available on the prevalence of suicidal ideation, suicidal attempts, and suicide rates among caregivers of those with dementia. Therefore, we aimed to systematically review these outcomes to address this gap in the literature and thus provide information to inform future policy and intervention for the benefit of caregivers of dementia patients.
Methods
We searched several databases from inception to the 10th November 2021, for studies investigating suicidal ideation, suicidal attempts, and suicide rates of caregivers of patients with dementia. We report data regarding suicidal ideation as prevalence, with the 95% confidence intervals (CIs), applying a random-effect model; since less than three studies were available for suicide attempt and suicide, these data are reported descriptively.
Results
Among 194 articles, eight comprising 1,209 informal caregivers of people with dementia (mean age: 63.9 years, 74% females) were included. The prevalence of suicide ideation was 32.32% (95% CI: 16.01–48.64%; I2 = 98.5%, p < 0.0001). The prevalence of suicide ideation varied between studies from 4.69% to 77.78%. Two studies reported the rate of suicidal attempt in caregivers of patients with dementia, with the prevalence ranging from 5.9% to 16.1%. One study reported one in 17 caregivers of patients with dementia died by suicide.
Conclusions
The prevalence of suicide ideation is high, affecting several caregivers of patients with dementia. These findings suggest intervention and/or policy are urgently needed to address suicidal behavior in this at-risk population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The number of people living with dementia worldwide in 2015 was estimated at 47.5 million, reaching 75.6 million in 2030 [1]. Future projections indicate that this number will be 135.46 million in 2050 [1]. Approximately 7.7 million new cases of dementia are anticipated each year [1]. In the US, costs attributable to their care range between 157 and 215 billion dollars and are expected to more than double by 2040 [2]. Moreover, the cost linked to informal caregiving in older people with dementia are difficult to estimate, but it is likely to be overall increasing.
Family members are the main careers for people with dementia living at home in almost all countries. It has been widely reported that the caregivers of patients with dementia have high levels of stress and high rates of depression and anxiety [3]. Therefore, often experiencing worse physical health than non-caregivers. Indeed, all these factors are potential risk factors for suicidal behavior [4]. It is largely known that caregivers of people with dementia witness a progressive decline in the person’s cognitive capacity, communication skills, and functional abilities, and thus learn new skills to manage behavioral and psychological symptoms common in dementia [5]. These daily problems may contribute to a range of negative physical and mental health outcomes [6], with a consequent increase in caregiver’s morbidity and mortality [7].
In recent years, there has been a rapid increase in scientific literature examining caregiver’s health and the difficulties encountered in caring for people with dementia. In addition, literature relating to suicidal behavior among caregivers of those with dementia is now emerging but to date no attempt has been made to collate, synthesis, and understand this literature as a whole. Given this background, we aimed to systematically review the prevalence of suicidal ideation, suicidal attempt, and suicide rates in caregivers of patients with dementia to address this gap in the literature and thus provide important information to inform future policy and intervention for the benefit of caregivers of dementia patients.
Materials and methods
This systematic review adhered to the PRISMA statement [8] and followed a pre-planned protocol that can be requested by contacting the corresponding author.
Data sources and searches
Four investigators (LS, MF, SC, NV) independently conducted a literature search using Web of Science, Pubmed/Medline, and PsycINFO from database inception until 10 November 2021.
In PubMed/Medline the following search strategy was used: “(Caregiver* OR Carer* OR Care Giver) AND (dement* OR alzheimer* OR Lewy OR “Posterior cortical atrophy” OR Binswanger OR “Progressive supranuclear palsy” OR Frontotemporal disorder* OR Frontotemporal degeneration OR Corticobasal degeneration OR Corticobasal syndrome) AND (suicide OR Suicidal Ideation OR Ideation, Suicidal [mh])”, adapting the search for the other databases. Any inconsistencies during title, abstract and finally full-text screening were resolved by consensus with a third senior author (LJD).
Study selection
Inclusion criteria for this systematic review were: (i) presence of informal caregiving, i.e., persons who provide some type of unpaid, ongoing assistance with activities of daily living or instrumental activities of daily living to a person with a chronic illness or disability [9]; (ii) report data regarding suicide or suicidal ideation or suicidal attempt; (iii) presence of patients with dementia. We excluded: (i) papers not relating to patients with dementia; (ii) data regarding suicidal behavior in patients with dementia per se.
Data extraction
Three independent investigators (LS, MF, SC) extracted key data from the included articles in a standardized Excel spreadsheet, with another independent investigator (NV) checking the data. For each article, we extracted data on authors’ name, year of publication, country, sample size, mean age and percentage of female caregivers, type of dementia, how suicide/suicidal ideation/suicidal attempt were defined, and tools for identifying suicide attempt/ideation.
Outcomes
The primary outcome of our systematic review was the prevalence of suicidal ideation in informal caregivers of people affected by dementia. Suicidal attempt and (completed) suicide were considered as co-primary outcomes.
Data synthesis and analysis
The primary analysis compared the overall prevalence of suicide ideation in caregivers of people with dementia. We, therefore, report this information as prevalence, weighted for sample sizes with the 95% confidence intervals (CIs), applying a random-effect model [10]. Since less than three studies were available for suicide attempt and complete suicide, these data are reported descriptively.
Heterogeneity across studies was assessed by the I2 metric and χ2 statistics. Given significant heterogeneity (I2 ≥ 50%, p < 0.05) and for outcomes having at least ten studies, we conducted a series of meta-regression analyses [11], using as moderators mean age, percentage of female caregivers and type of dementia. Publication bias was assessed by visually inspecting funnel plots and using the Egger bias test [12] and in case of publication bias a fill and trim analysis was performed [13].
For all analyses, a P-value less than 0.05 was considered statistically significant. All analyses were performed using STATA version 14.0 (StataCorp).
Results
Literature search
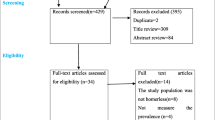
As shown in Fig. 1, we initially screened 194 articles. After removing 172 records, based on the tile and the abstract, 22 full texts were examined and eight articles were finally included [14,15,16,17,18,19,20,21].
Descriptive characteristics
As reported in Table 1, 1209 informal caregivers of people affected by dementia were included. Caregivers had a mean age of 63.9 years and were mainly female (74%). Two studies included only patients with Alzheimer’s disease [14, 20], one study with either Alzheimer’s disease or fronto-temporal dementia [16], whilst the other five did not specify syndrome type. The tools used for identifying suicidal ideation or attempt varied across studies (full details in Table 1).
Informal caregiving and suicide
As shown in Fig. 2, all studies reported data on suicidal ideation. Overall, the prevalence of suicidal ideation in the 1209 caregivers included was 32.32% (95% CI: 16.01–48.64%) characterized by a high heterogeneity (I2 = 98.5%, p < 0.0001). The prevalence of suicidal ideation varied between the studied from 4.69% [19] to 77.78% [20]. This outcome did not suffer from any publication bias, based on the Egger’s test (5.68 ± 4.67; p = 0.27) and the visual inspection of the funnel plot.
Since the prevalence of suicidal ideation was characterized by high heterogeneity, we performed several meta-regression analyses showing that a higher mean age was associated with a lower prevalence of suicidal ideation: for each one-year increase in mean age, the rate of suicidal ideation decreased by approximately 5% (beta = − 0.05; 95% CI: − 0.07 to − 0.02; p = 0.009; R2 = 91.7%). Moreover, when stratifying the data by type of dementia, no significant differences across strata emerged (p = 0.34) and the heterogeneity (described by the I2) remained more than 50% in all the strata.
Two studies reported the rate of suicide attempt in caregivers of patients with dementia. One study performed on 566 caregivers [17], reported a prevalence of suicide attempt of 16.1%, whilst the other study 5.9% [14].
Finally, one study [14] reported one in 17 caregivers of patients with dementia died by suicide.
Discussion
In this systematic review and meta-analysis using eight studies including 1,209 informal caregivers of people with dementia, a high prevalence of suicidal ideation was present, approximately one in three informal caregivers.
Our data showed that the prevalence of suicidal ideation is more evident in younger compared to older caregivers; however, the analyzed data only concerned caregivers, without comparing the rate of suicidal ideation with the data of the general population. Therefore, it would be important to investigate the prevalence of these conditions with population-based studies. In this way, it would be possible to utilize more accurate data on risk of suicidal ideation in the interested population. In addition, it would be relevant to value how these results change according to the country where the study was conducted. Indeed, we observed that the prevalence of suicidal ideation varied by country where the study was conducted. In a study carried out in Japan, in contrast to the other studies included, an increase in suicidal ideation was not observed, likely owing to differences in cultural background [18]. Unfortunately, in Japan, the rate of suicide and suicidal ideation is high in the general population, potentially explaining the non-significant results [22]. In addition, in this study, in contrast to the others, depression was not a risk factor for suicidal ideation [18]. Finally, only two studies reported data regarding suicide attempt indicating that prevalence is high.
Several studies demonstrated that specific factors may influence the way in which family members address caregiving, e.g., caregiver’s sense of competence. This is defined as a state related to the caregiver’s feeling of being capable to manage the caregiving role [23]. A positive sense of competence has been associated with a reduced risk of the person with dementia being institutionalized [24]. Approximately 80% of people with dementia are cared for by their family and they are often institutionalized after 6.5 years, as demonstrated by several studies [25]. One potential reason for institutionalization may be owing to the presence of depression in patients, which is also associated with lower quality of life in caregivers, combined these lower the self-sufficiency of demented patients [25]. Moreover, reduction of activities of daily living may result in a greater level of care that consequently increases caregiver’s stress. Caregiver depression is thought to be a consequence of care due to a complex interplay of factors that comprises dimensions of the patient, caregiver, and cultural background [26]. It is important to note that a potential increase in suicidal behavior is associated with all caregivers and not just caregivers of those with dementia. For example, a large study has demonstrated that suicide rates are twice as high as that of the general population among caregivers of patients with cancer [27]. An important risk factor, as also described in our systematic review, is depression, even though other risk factors (such as psychiatric history, previous suicide attempts, hopelessness, demoralization, pain, lack of social support, feeling of being a burden to others, and existential concerns) also may confer increased suicidality [28].
The findings of our study must be interpreted within its limitations. First, the number of studies and participants are limited, prohibiting some analyses. Another limitation is represented by the difference in tools used across these studies to identify suicidal ideation, often self-reported during interviews. Moreover, the prevalence of suicide and suicidal ideation in caregivers of those with dementia was not compared with general population data. Finally, we were not able to describe the specificity in the definition of suicidal ideation (i.e., active or passive or intermittently), but this topic is of critical importance and merits further research.
In conclusion, our systematic review and meta-analysis reported that the prevalence of suicidal ideation is high, affecting a high proportion of caregivers of patients with dementia. Since the topic of suicide is often not discussed in daily clinical practice, we encourage further research of a qualitative nature to further inform intervention and policy on suicide reduction among caregivers of those with dementia.
References
Prince M, Guerchet M, Prina M (2013) The global impact of dementia 2013–2050. Alzheimer's Disease International
Hurd MD, Martorell P, Delavande A et al (2013) Monetary costs of dementia in the United States. N Engl J Med 368:1326–1334
Schulz R, Sherwood PR (2008) Physical and mental health effects of family caregiving. J Soc Work Educ 44:105–113
Vitaliano PP, Zhang J, Scanlan JM (2003) Is caregiving hazardous to one’s physical health? A meta-analysis. Psychol Bull 129:946–972
Moniz-Cook E, Elston C, Gardiner E et al (2008) Can training community mental health nurses to support family carers reduce behavioural problems in dementia? An exploratory pragmatic randomised controlled trial. Int J Geriatr Psychiatry 23:185–191
Cooper C, Balamurali T, Livingston G (2007) A systematic review of the prevalence and covariates of anxiety in caregivers of people with dementia. Int Psychogeriatr 19:175–195
Monin JK, Schulz R (2009) Interpersonal effects of suffering in older adult caregiving relationships. Psychol Aging 24:681–695
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62:e1–e34
Roth DL, Fredman L, Haley WE (2015) Informal caregiving and its impact on health: a reappraisal from population-based studies. Gerontologist 55:309–319
Der Simonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Higgins JP, Thomas J, Chandler J et al (2019) Cochrane handbook for systematic reviews of interventions. John Wiley & Sons, Chichester
Egger M, Smith GD, Schneider M et al (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot–based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56:455–463
Shaji KS, Smitha K, Lal KP et al (2003) Caregivers of people with Alzheimer’s disease: a qualitative study from the Indian 10/66 Dementia Research Network. Int J Geriatr Psychiatry 18:1–6
O’Dwyer S, Moyle W et al (2013) Suicidal ideation and resilience in family carers of people with dementia: a pilot qualitative study. Aging Ment Health 17:753–760
O’Dwyer ST, Moyle W, Zimmer-Gembeck M et al (2013) Suicidal ideation in family carers of people with dementia: a pilot study. Int J Geriatr Psychiatry 28:1182–1188
O’Dwyer ST, Moyle W, Zimmer-Gembeck M et al (2016) Suicidal ideation in family carers of people with dementia. Aging Ment Health 20:222–230
Koyama A, Matsushita M, Hashimoto M et al (2017) Mental health among younger and older caregivers of dementia patients. Psychogeriatrics 17:108–114
Joling KJ, O’Dwyer ST, Hertogh C et al (2018) The occurrence and persistence of thoughts of suicide, self-harm and death in family caregivers of people with dementia: a longitudinal data analysis over 2 years. Int J Geriatr Psychiatry 33:263–270
Anderson JG, Eppes A, O’Dwyer ST (2019) “Like death is near”: expressions of suicidal and homicidal ideation in the blog posts of family caregivers of people with dementia. Behav Sci (Basel) 9:22
Parkinson B (2018) Risk of suicidal thinking in caregivers of people with dementia should be assessed and monitored by health professionals. Evid Based Nurs 21:73
Kawashima Y, Yonemoto N, Inagaki M et al (2014) Prevalence of suicide attempters in emergency departments in Japan: a systematic review and meta-analysis. J Affect Disord 163:33–39
Vernooij-Dassen MJ, Persoon JM, Felling AJ (1996) Predictors of sense of competence in caregivers of demented persons. Soc Sci Med 43:41–49
Borsje P, Hems MA, Lucassen PL et al (2016) Psychological distress in informal caregivers of patients with dementia in primary care: course and determinants. Fam Pract 33:374–381
Haley WE (1997) The family caregiver’s role in Alzheimer’s disease. Neurology 48:25S-29S
Huang S-S (2022) Depression among caregivers of patients with dementia: associative factors and management approaches. World J Psychiatry 12:59
McFarland DC, Walsh L, Napolitano S et al (2019) Suicide in patients with cancer: identifying the risk factors. Oncology (Williston Park) 33:221–226
Jovanović N, Beezhold J, Tateno M et al (2019) Depression and suicidality among psychiatric residents-results from a multi-country study. J Affect Disord 249:192–198
Funding
Open access funding provided by Università degli Studi di Palermo within the CRUI-CARE Agreement. None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethics approval
Not needed.
Consent to participate
Not needed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Solimando, L., Fasulo, M., Cavallero, S. et al. Suicide risk in caregivers of people with dementia: a systematic review and meta-analysis. Aging Clin Exp Res 34, 2255–2260 (2022). https://doi.org/10.1007/s40520-022-02160-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-022-02160-6