Abstract
This review examined the therapeutic support literature for children with autism and/or an intellectual disability who have experienced interpersonal trauma. We captured studies that implemented a therapeutic support with this population and synthesised articles that made clinical practice recommendations. Fifty-two relevant articles were identified, and four patterns were uncovered. First, primary studies in this research domain are scant, diffuse, and largely lacking in methodological consistency. Second, the literature favoured therapeutic supports that relied less on verbal skills and/or demanded a high cognitive load. Further, parent/caregiver involvement was repeatedly emphasised. Finally, methods of therapeutic support delivery appeared consistent with the broader neurodevelopmental literature. Overall, these results provide an important first step toward establishing best practice for supporting these vulnerable children.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neurodiverse children, including those with autism spectrum disorder (autism) and/or an intellectual disability (ID), are at heightened risk of experiencing interpersonal trauma such as abuse, neglect, and exposure to family violence (Fang et al., 2022b). It is estimated that these children are approximately two to three times more likely to encounter traumatic events of an interpersonal nature relative to their typically developing counterparts (Fang et al., 2022b). Ecological systems theories regarding such vulnerability indicate that child-related factors such as a high dependence on caregivers and/or communication challenges interact with environmental factors such as parent mental health challenges to confer these children’s risk of traumatic exposure (Ammerman et al., 1994; Fisher et al., 2008; Gore & Janssen, 2007; Hibbard & Desch, 2007; Howe, 2006; Sobsey, 2002; Verdugo et al., 1995).
Interpersonal trauma can profoundly impact the mental health of neurodiverse children, as characterised by the onset of depressive symptomatology, self-injurious behaviour, and post-traumatic sequalae including intrusive thoughts, distressing memories, and sleep disturbance (Bleil Walters et al., 2013; Brenner et al., 2017; Mandell et al., 2005; McDonnell et al., 2019; Mehtar & Mukaddes, 2011; Paquette et al, 2017). Kerns et al. (2015) hypothesised that such difficulties manifest due to the emergence of new symptomatology and/or an exacerbation of a child’s existing disability-related characteristics. Indeed, while this conceptual framework was initially developed to explain the intersection between autism and trauma, the high degree of overlap, co-occurrence, and shared interpersonal trauma vulnerability between children with autism and an ID suggests that this framework may further help to explain trauma-related sequalae in children with an ID (Matson & Shoemaker, 2009; McDonnell et al., 2019; Reiter et al., 2007).
Despite the significant research efforts directed toward understanding this group’s vulnerability, it is currently unclear how to best support their mental health. This has likely been due in part to a siloed approach to disability and trauma research (Prock & Fogler, 2018) and a historical tendency to misattribute trauma-related difficulties to a child’s primary neurodevelopmental diagnosis rather than to concurrent psychopathology (Mazefsky et al., 2012; Reiss et al., 1982). As a result, evidence-based therapeutic guidelines for this group of children are lacking, and best practice parameters have yet to be established.
The purpose of the current review was to examine the existing literature regarding therapeutic supports for children with autism and/or an ID who have experienced interpersonal trauma. We included therapeutic supports that emphasised psychological, social, emotional, and/or behavioural factors, and aimed to improve a child’s mental health and/or functioning. We were particularly interested in the types of clinical techniques, strategies, and/or modalities that have been reported in the literature and their associated methods of delivery. The specific aims of our review were: 1) to capture studies that have implemented a therapeutic support directly with this group of children and to understand whether their methodological characteristics were similar enough to allow for comparison across studies; 2) to synthesise literature that has included clinical recommendations for working therapeutically with these children - while such recommendations have been traditionally overlooked, they have the potential to reveal patterns of consensus that can be used to guide future clinical and research endeavours; and 3) to integrate therapeutic supports pertaining to both autism and/or an ID into a cohesive body of work and consolidate research that has used inconsistent terminology to capture the interpersonal trauma construct.
Method
Given the expected paucity of empirical literature in this clinical domain, a scoping review was selected as the preferred review method due to its exploratory approach (Munn et al, 2018). The Joanna Briggs Institute (JBI) scoping review methodology was employed and the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) reporting guideline was followed (Peters et al., 2020; Tricco et al., 2018).
Eligibility Criteria
Eligibility criteria for an article differed based on whether the article had implemented a therapeutic support or made a clinical practice recommendation for working therapeutically with this group of children. Inclusion and exclusion criteria are presented in Table 1.
Search Strategy
The JBI three-step search strategy was employed for this review (Peters et al., 2020).
Step one: A limited search of two online databases relevant to the topic (i.e. MEDLINE and PubMed) was conducted to identify initial keywords in the titles and abstracts. In consultation with a tertiary librarian, a comprehensive list of indexed terms and combinations of synonyms/interchangeable terms (i.e. syntax-combinations) was developed.
Step two: In October 2021, a targeted and comprehensive search using all relevant terms and database-specific age limits was applied across the following four databases: Ovid MEDLINE, Embase, Emcare, and PsychInfo. The search was not limited by date of publication or study design, and indexed terms were adapted to each of the databases. A full search strategy for MEDLINE is presented in Supplementary Table A.
Step three: A manual search of the reference lists of all eligible full-text sources was undertaken to identify additional articles that had not yet been included.
Selection of Literature
Three levels of screening were conducted. First, records which clearly met the exclusion criteria were reviewed and removed by one researcher (LK), after which the remaining records were screened by three researchers on the web-based software platform Covidence (LK, JB, and LM; Veritas Health Innovation 2015) at the title and abstract levels. Remaining records then underwent full-text review by two researchers (LK and JB), wherein any conflict was resolved through verbal consensus.
Data Extraction and Synthesis
An extraction form was developed and updated after trialling it on two eligible sources. Extraction differed according to whether the article had implemented a therapeutic support or made a clinical practice recommendation for working therapeutically with this group of children.
Implemented therapeutic supports: Participant and methodological characteristics, together with explicit details of the therapeutic support, were recorded. Therapeutic supports were grouped according to existing psychotherapeutic frameworks (i.e. cognitive-behavioural, attachment-theory).
Recommendations: Recommendations were synthesised using a deductive thematic analysis framework (Braun & Clarke, 2006; Kiger & Varpio, 2020). Recommendations were summarised in both a tabular and descriptive format, and the number of articles that addressed each theme was recorded. Some articles mapped onto multiple themes and were therefore cited more than once.
Results
The search retrieved a total of 3193 records, with a further eight sourced through manually searching the reference lists of the identified articles. After a process of duplicate removal and two stages of screening, 207 articles underwent full text review, with a total 52 articles being deemed eligible for inclusion. A PRISMA diagram presents the selection process (see Fig. 1). The 52 included articles are summarised in Table 2.
Overview of the Literature
Fifty-two articles described therapeutic supports for children with autism and/or an ID who have encountered interpersonal trauma (see Table 2). Of these, 15 were primary studies that implemented the support directly with this group of children (and/or their parents/caregivers), while the remaining 37 provided a clinical recommendation intended to guide future therapeutic efforts.
Primary Studies that Implemented a Therapeutic Support
Across the 15 studies that implemented a support, there was great diversity in therapeutic modality wherein seven clusters of supports were identified. Table 3 presents these support clusters, participant, and methodological characteristics, together with study findings.
Therapeutic Approaches
Four studies reported on eye movement desensitisation and reprocessing therapy (EMDR), one of which had adjunctive elements that included prolonged exposure and physical activity (Mevissen et al., 2020) and another incorporated a dedicated parenting skills component (Ooms-Evers et al., 2021). Three studies delivered cognitive-behavioural support, namely, manualised Trauma Focused Cognitive Behavioural Therapy (TF-CBT; Holstead and Dalton), the trauma narrative component of TF-CBT in conjunction with family therapy (Gerhardt & Smith, 2020), and nonspecific CBT alongside pharmacological treatment (Lin et al., 2020). A separate study employed an exclusively behavioural intervention that involved highly individualised strategies (i.e., reinforcement, arousal modulation, physical activity, and routine; Kildahl et al., 2021), whereas another implemented a blended behaviour-attachment focussed support that aimed to cultivate sensitive and responsive child-caregiver interactions and increase adaptive behaviour (Sterkenburg et al., 2008). A further two studies delivered established attachment interventions that included child parent psychotherapy (CPP; Harley et al., 2014) and Theraplay (Mohamed & Mkabile, 2015), and two others implemented non-directive therapeutic supports that drew upon art and symbolic play (Guest & Ohrt, 2018; Horovitz, 1981). Finally, the two studies remaining implemented “psychotherapy” without mention of a specific therapeutic modality or support target, both of which mentioned parental involvement (Cook et al., 1993; de Pilar Trelles Thorne et al., 2015).
Participant Characteristics
Across the 15 studies, six reported on participants that had a diagnosis of autism, three on children with an ID, and six on those who had both autism and an ID (see Table 3). Additional presenting difficulties included but were not limited to: post-traumatic stress disorder (PTSD) or subthreshold trauma-based symptomatology, self-injurious behaviour, anxiety, depression, attention deficit-hyperactivity disorder, disrupted attachment, and visual impairments. Interpersonal trauma exposure typically occurred within the family system in all but two studies, and nine studies involved parents/caregivers in the intervention process.
Methodological Characteristics
The 15 studies consisted of four case series, eight case reports, a repeated measures study, and a nonrandomised trial (see Table 3). Twelve of the studies described the therapeutic support in replicable detail by citing a treatment manual or by providing explicit details about the nature of the therapeutic support. The remaining three provided a reference to a support modality and/or alluded to an intervention component but did not elaborate. Eight of the studies specified their target outcomes from the outset (i.e., as part of their methodology), and similarly, eight studies utilised standardised assessment instruments to operationalise their target outcomes and collect data on their participants. Instruments varied in focus and assessed for trauma-based symptomatology, daily life impairment, broad mental health and behavioural outcomes, parental stress, and psychopathology. The seven studies remaining collected information on their participants via unstandardised parental report and/or clinical observation.
Only seven studies evaluated the efficacy of their therapeutic support by comparing standardised assessment data pre-to post-intervention. Three plotted their data graphically and/or in tabular form to visually inspect the data for trends, while four utilised formal statistical analysis techniques as their primary analysis method. These seven studies spanned five therapeutic support clusters (i.e., EMDR, TF-CBT, behavioural, behavioural-attachment, and attachment). The remaining eight studies described participants’ characteristics after implementation but, without baseline data, were unable to evaluate efficacy of the therapeutic support.
Findings of Studies that Evaluated Efficacy
Of the seven studies that assessed efficacy, reductions in post-traumatic symptomatology, general psychiatric challenges, behavioural difficulties and daily life impairment were reported. Two studies reported improved parent outcomes (Harley et al., 2014; Mevissen et al., 2020); however, in one study, scores on the majority of parental stress subscales remained elevated post intervention (Harley et al., 2014). Of note, the results of one study indicated that their TF-CBT intervention was largely ineffective in reducing internalising and externalising problems in children; however, aggressive behaviour and rule-breaking did decrease (Holstead & Dalton, 2013).
Method of Delivery
Eight of the studies that implemented a therapeutic support used nonverbal, sensory, and/or play-based therapeutic techniques (Guest & Ohrt, 2018; Harley et al., 2014; Horovitz, 1981; Kildahl et al., 2021; Mevissen et al., 2011, 2017, 2020; Mohamed & Mkabile, 2015), and an additional study made an explicit attempt to integrate their participant’s interests and preferred activities into the intervention process (Gerhardt & Smith, 2020). Efforts to modify language and match the communication abilities of participants were reported across five studies, which included the provision of clear instructions (Mevissen et al., 2011, 2017, 2020), simplified communication (Guest & Ohrt, 2018; Ooms-Evers et al., 2021), and the use of positive language (Harley et al., 2014). A further study emphasised the importance of reinforcing and validating verbal communication attempts (Kildahl et al., 2021). Finally, structural modifications to sessions were noted across a small number of studies and included ensuring predictability (Sterkenburg et al., 2008), slowing down the pace of sessions (Guest & Ohrt, 2018), prioritising one task at a time (Mevissen et al., 2020), and providing frequent breaks (Harley et al., 2014).
A Synthesis of Recommendations
Article Characteristics
The 37 articles that made a recommendation for working therapeutically with this group of children comprised two book chapters, 12 reviews, and 12 commentaries, with a small proportion (n = 11) being primary and secondary studies (see Table 2). As demonstrated in Table 2, the primary objective of a large portion (n = 23) of these articles was to provide recommendations, whereas the recommendations made by the remaining 14 were a subsidiary of a separate yet related research endeavour.
A visual inspection of these articles’ reference lists revealed that only nine of the 15 studies that implemented a therapeutic support were cited (Cook et al., 1993; Harley et al., 2014; Holstead & Dalton, 2013, Mevissen et al., 2011, 2017, 2020; Mohamed & Mkabile, 2015; Sterkenburg et al., 2008; De Pillar Trelles Thorne et al., 2015). The remaining citations were comprised of commentaries, opinion pieces and reviews, or primary studies that reported on therapeutic supports for adults with a history of childhood trauma, neurodiverse children who had not encountered trauma, and children who had experienced trauma but did not have an identified neurodevelopmental diagnosis.
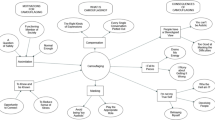
Thematic analysis of the 37 articles revealed two distinct clusters of recommendations: child-focussed and parent/caregiver-focussed. Four different categories of therapeutic support were identified within each cluster, which are summarised below and detailed in Table 4.
Child Focussed
Seventeen articles recommended that children be assisted with their emotional literacy and/or adaptive emotional regulation, wherein explicit strategies like mindfulness and progressive muscle relaxation were frequently mentioned. Eighteen articles indicated that behavioural targets should be, at least in part, the focus of therapeutic support efforts, with a large portion advocating for education about safety skills, intimacy, and interpersonal relationships. Fourteen articles made a recommendation that centred on modifying children’s thinking patterns, with many advising that clinicians should address children’s cognitive distortions, support children to construct an accurate trauma narrative, and provide psychoeducation about trauma. Finally, twelve suggested general psychotherapeutic approaches (e.g. CBT, EMDR, and counselling); however the majority of these did not elaborate on a specific therapeutic target.
Parent/Caregiver Focussed
Twenty-four articles recommended that parents/caregivers be part of the therapeutic work with this group of children. Eight of these articles did not specify what such involvement would entail (Byrne 2020; Dion et al., 2013; Mansell et al., 1996; Rose & Hardman, 1981; Schneider et al., 2019; Sullivan, 1993; Tharinger et al., 1990; Vervoort-Schel et al., 2021); however, fourteen emphasised that parents may require individual support with their own challenges. Ten articles advocated for parent psychoeducation, with the most common suggestion being that parents should be educated about trauma and its widespread effects, the unique needs of neurodiverse children, what is and is not within their child’s control, and that harsh discipline will. Additionally, thirteen articles recommended that parents be taught specific, practical skills to assist them in their parenting role (i.e. how to attune to their child’s needs and engage in emotion-focussed conversations about trauma), and separately, seven recommended that therapeutic support should focus on parent–child attachment with child-parent psychotherapy emerging as a recurrent suggestion (Lieberman et al., 2005).
Recommended Methods of Delivery
Twelve articles recommended that interactive, creative, play-based, and sensory tools be utilised when supporting children in a therapeutic capacity (e.g., role plays, art, drama, and social stories). The utilisation of visual and pictorial strategies was explicitly recommended by six articles and included the use of visual timers, visual activity schedules, story boards, and index cards. Nine articles recommended that clinicians should modify their language to meet the needs of this group of children, while, similarly, nine articles suggested that adaptations be made to session structure and content. Specific recommendations centred on ensuring predictability, shortening the length of sessions, providing ample breaks, and slowly introducing emotionally laden topics.
Discussion
To date, there has been a lack of clarity regarding what constitutes best therapeutic practice for children with autism and/or an ID who have a history of interpersonal trauma. To form a more coherent picture of this clinical domain, the current review identified studies that have implemented a therapeutic support with this group of children and synthesised clinical practice recommendations intended to guide future support endeavours.
Paradoxically, despite their high-risk status, only 15 studies were identified that implemented a therapeutic support with our population of interest. Across these studies, seven main types of therapeutic approaches emerged, which were marked by diverse participant characteristics and methodologies that varied in terms of their study design, target outcomes, the operationalisation of variables, and use of efficacy analyses. Unfortunately, the sheer paucity of primary studies in this body of literature and the significant participant and methodological heterogeneity observed limited even preliminary empirical assertions from being made in this review. As such, the extent to which one therapeutic support modality may have more “clinical promise” or “best practice potential” over another could not be reliably determined.
That said, a noteworthy discovery was that the types of therapeutic support implemented largely parallel first-line evidence-based treatments recommended by the National Institute for Health and Care Excellence (NICE) for children in the general population who have experienced interpersonal trauma. These include TF-CBT, attachment-based therapies, CPP, and EMDR (NICE, 2017, 2018). While further research is needed to develop an empirical approach to supporting the mental health of neurodiverse children with a history of interpersonal trauma, it is reassuring that several of the implementation studies drew upon existing therapies that are both scientifically grounded and widely endorsed within the general population.
Another interesting pattern to emerge across implementation studies was that few had an exclusively verbal emphasis and/or demanded a high cognitive load. This pattern further traversed the clinical practice recommendations wherein therapeutic support with a behavioural focus and/or an emotional target garnered the highest number of recommendations. While it is a common misconception that children with autism and/or an ID are unable to benefit from talk-based therapies (Gaus, 2007; Weston et al., 2016), future research may benefit from comparing the relative effectiveness of purist cognitive modalities, over other more behavioural and/or emotion-focussed therapeutic approaches when supporting this group of children.
Of note, recommendations that were behaviourally focussed centred on enhancing children’s communication skills and providing education on interpersonal relationships, safety, and abuse. This aligns with converging evidence demonstrating that a lack of skills and/or knowledge in these areas is significant risk factor for interpersonal trauma exposure in children with autism and/or an ID (Miller et al., 2017) and is core component of primary, secondary, and tertiary prevention programs for neurotypical children who have encountered similar traumatic experiences (Kim, 2010). With respect to the emotionally anchored recommendations, it was repeatedly suggested that children’s emotional vocabulary and regulation be the focus of therapeutic support efforts. Indeed, given that these emotional domains already prove challenging for neurodiverse children and are often amplified following interpersonal trauma exposure, it is unsurprising that recommendations of this nature repeatedly surfaced (Haruvi-Lamdan et al., 2018; Hill et al., 2004; Mazefsky et al., 2013; McClure et al., 2009; Rieffe et al., 2007).
Despite the consistency observed, the clinical practice recommendations did not appear to explicitly favour one particular type of therapeutic support over another. This could simply suggest that there is no “one size fits all” approach to working with this group of children. More likely however, is that in the absence of a substantial and robust evidence base wherein the majority of recommendations were not empirically supported, there exists considerable variation across clinical and research opinion. As such, the recommendations detailed in this review must be viewed as potential signposts for future clinical research but not as definitive evidence of what therapeutic supports should be implemented with this population.
Perhaps of greatest clinical utility was the discovery that the bulk of the literature presented in this review indicated that parents/caregivers be involved in the therapeutic work. While historically research tended to over-emphasise characteristics of the individual child in the attribution of interpersonal trauma vulnerability (Manders & Stoneman, 2009; Thomas-Skaf & Jenney, 2021), the findings of this review reinforce ecological risk models demonstrating the role of the systemic context in this complex clinical picture (Algood et al., 2011). Whether parents/caregivers are instigators of harm, inadvertent contributors, or are unclear about how to respond to their child’s traumatic encounter, a systems-approach to therapy is widely acknowledged as fundamental to harm reduction and therapeutic success in this group.
An ancillary discovery was that the methods of intervention delivery endorsed across the literature were consistent with those that have been well-defined in the broader neurodevelopmental literature (Spain & Happé, 2020; Surley & Dagnan, 2019). While this could suggest that therapeutic modifications for children with autism and/or an ID are homogenous irrespective of whether the child has experienced interpersonal trauma or not, this supposition has yet to be formally tested.
There were some limitations in the present study that should also be considered. First, despite employing a rigorous and systematic literature search with a diversity of terms, as well as a manual search of the reference list of all included articles, it is possible that not all studies of relevance were captured. Further, the frequency with which similar recommendations emerged is not necessarily a proxy of their relative significance. While it is hoped that a degree of intentionality underscored the provision of each recommendation, authors may have respectfully echoed recommendations of relevance in a somewhat perfunctory manner. It is, however, plausible that recommendations with high frequency counts do reflect areas of priority in the field and certainly provide possible avenues for exploration. Finally, as the literature on therapeutic supports for this group had yet to be sufficiently integrated, a systematic review with a comprehensive quality appraisal was deemed premature. That said, given that the primary objective of this review was to map and synthesise the “current state of affairs” in this clinical space, we were able to capture nuanced information that would have been lost had a systematic review been conducted instead.
In conclusion, this review highlights that the literature on therapeutic supports for children with autism and/or an ID and a history of interpersonal trauma is scant, diffuse, and largely lacking in methodological consistency. While there is clearly an absence of evidence to guide best practice, the emphasis on parent/caregiver involvement and the ever-so-slight shift away from verbal and/or cognitively demanding modalities make important progress toward understanding potential therapeutic support models for this group of children. Ultimately, it is hoped that this timely synthesis will incentivise researchers to work alongside families and clinicians to develop and systematically evaluate potential therapeutic supports for this vulnerable population, and that an empirical consensus will materialise in the not-too-distant future.
References
Algood, C. L., Hong, J. S., Gourdine, R. M., & Williams, A. B. (2011). Maltreatment of children with developmental disabilities: An ecological systems analysis. Children and Youth Services Review, 33, 1142–1148.
Allington-Smith, P., Ball, R., & Haytor, R. (2002). Management of sexually abused children with learning disabilities. Advances in Psychiatric Treatment, 8, 66–72.
Ammerman, R. T., Hersen, M., van Hasselt, V. B., Lubetsky, M. J., & Sieck, W. R. (1994). Maltreatment in psychiatrically hospitalized children and adolescents with developmental disabilities: Prevalence and correlates. Journal of the American Academy of Child & Adolescent Psychiatry, 33, 567–576. https://doi.org/10.1097/00004583-199405000-00015
Bleil Walters, J., Hughes, T. L., Sutton, L. R., Marshall, S. N., Crothers, L. M., Lehman, C., Paserba, D., Talkington, V., Taormina, R., & Huang, A. (2013). Maltreatment and depression in adolescent sexual offenders with an autism spectrum disorder. Journal of Child Sexual Abuse: Research, Treatment, & Program Innovations for Victims, Survivors, & Offenders, 22(1), 72–89. https://doi.org/10.1080/10538712.2013.735357
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3(2), 77–101. https://doi.org/10.1191/1478088706qp063oa
Brenner, J., Pan, Z., Mazefsky, C., Smith, K., & Gabriels, R. (2017). Behavioral symptoms of reported abuse in children and adolescents with autism spectrum disorder in inpatient settings. Journal of Autism and Developmental Disorders, 48(11), 3727–3735. https://doi.org/10.1007/s10803-017-3183-4
Byrne, G. (2020). A Systematic Review of Treatment Interventions for Individuals With Intellectual Disability and Trauma Symptoms: A Review of the Recent Literature. Trauma, Violence & Abuse, 23(2), 541–554. https://doi.org/10.1177/1524838020960219
Chan, K. K. S., & Lam, C. B. (2016). Parental maltreatment of children with autism spectrum disorder: A developmental-ecological analysis. Research in Autism Spectrum Disorders, 32, 106–114. https://doi.org/10.1016/j.rasd.2016.09.006
Cohen, J. A., Mannarino, A. P., & Deblinger, E. (2006). Treating trauma and traumatic grief in children and adolescents. Guilford Press.
Cook, E., Kieffer, J., Charak, D., & Leventhal, B. (1993). Autistic disorder and post-traumatic stress disorder. Journal of the American Academy of Child & Adolescent Psychiatry, 32(6), 1292–1294. https://doi.org/10.1097/00004583-199311000-00025
De Pillar Trelles Thorne, M. P., Khinda, N., & Coffey, B. J. (2015). Posttraumatic stress disorder in a child with autism spectrum disorder: Challenges in management. Journal of Child and Adolescent Psychopharmacology, 25(6), 514–517. https://doi.org/10.1089/cap.2015.29011.mptt
Dion, J., Paquette, G., Tremblay, K. N., Cyr, M., & Dionne, C. (2013). Sexual abuse of intellectually disabled youths: A review. The Prevention Researcher, 20(3), 14–16.
Dodds, R. L. (2021). An exploratory review of the associations between adverse experiences and autism. Journal of Aggression, Maltreatment & Trauma, 30(8), 1093–1112.
Duan, G., Chen, J., Zhang, W., Yu, B., Jin, Y., Wan, Y., & Yao, M. (2015). Physical maltreatment of children with autism in Henan province in China: A cross-sectional study. Child Abuse and Neglect, 48, 140–147. https://doi.org/10.1016/j.chiabu.2015.03.018
Fang, Z., Barlow, J., & Zhang, C. (2022a). Parenting programs that address physical abuse in childhood for families of children with developmental disabilities in mainland China: Systematic review and meta-regression. Trauma, Violence, & Abuse, 23(2), 457–475. https://doi.org/10.1177/1524838020915599
Fang, Z., Cerna-Turoff, I., Zhang, C., Lu, M., Lachman, J. M., & Barlow, J. (2022b). Global estimates of violence against children with disabilities: An updated systematic review and meta-analysis. The Lancet Child and Adolescent Health, 6(5), 313–323. https://doi.org/10.1016/S2352-4642(22)00033-5
Fisher, M. H., Hodapp, R. M., & Dykens, E. M. (2008). Child abuse among children with disabilities: What we know and what we need to know. International Review of Research in Mental Retardation, 35, 251–289. https://doi.org/10.1016/S0074-7750(07)35007-6
Gardiner, E., Iarocci, G., & Moretti, M. (2017). Integrative care for adolescents with dual diagnosis: Considering trauma and attachment within an innovative model for clinical practice. Journal of Mental Health Research in Intellectual Disabilities, 10(4), 321–344. https://doi.org/10.1080/19315864.2017.1337835
Gaus, V. (2007). Cognitive-behavioral therapy for adult Asperger syndrome. Guilford Press.
Gerhardt, L., & Smith, J. (2020). The use of Minecraft in the treatment of trauma for a child with autism spectrum disorder. Journal of Family Therapy, 42, 365–384. https://doi.org/10.1111/1467-6427.12297
Gore, M., & Janssen, K. (2007). What educators need to know about abused children with disabilities. Preventing School Failure, 52, 49–55.
Grosso, C. A. (2012). Children with developmental disabilities. Treatment Applications: Trauma-Focused CBT for Children and Adolescents.
Guest, J. D., & Ohrt, J. H. (2018). Utilizing child-centered play therapy with children diagnosed with autism spectrum disorder and endured trauma: A case example. International Journal of Play Therapy, 27(3), 157–165. https://doi.org/10.1037/pla0000074
Gupta, S. (2019). Sexual Abuse of Children and Adults With Intellectual Disabilities: Preventive, Supportive, and Intervention Strategies for Clinical Practice. In Social Issues Surrounding Harassment and Assault:Breakthroughs in Research and Practice, (pp. 578–587).
Hall-Lande, J., Hewitt, A., Mishra, S., Piescher, K., & LaLiberte, T. (2015). Involvement of children with autism spectrum disorder (ASD) in the child protection system. Focus on Autism and Other Developmental Disabilities, 30(4), 237–248. https://doi.org/10.1177/1088357614539834
Harley, E. K., Williams, M. E., Zamora, I., & Lakatos, P. P. (2014). Trauma treatment in young children with developmental disabilities: Applications of the child-parent psychotherapy (CPP) model to the cases of “James” and “Juan.” Pragmatic Case Studies in Psychotherapy, 10(3), 156–195. https://doi.org/10.14713/pcsp.v10i3.1869
Haruvi-Lamdan, N., Horesh, D., & Golan, O. (2018). PTSD and autism spectrum disorder: Co-morbidity, gaps in research, and potential shared mechanisms. Psychological Trauma: Theory, Research, Practice, and Policy, 10(3), 290. https://doi.org/10.1037/tra0000298
Hibbard, R. A., & Desch, L. W. (2007). Maltreatment of children with disabilities. Pediatrics, 119, 1018–1025. https://doi.org/10.1542/peds.2007-0565
Hill, E., Berthoz, S., & Frith, U. (2004). Brief report: Cognitive processing of own emotions in individuals with autistic spectrum disorder and in their relatives. Journal of Autism and Developmental Disorders, 34(2), 229–235.
Holstead, J., & Dalton, J. (2013). Utilization of trauma-focused cognitive behavioral therapy (TF-CBT) for children with cognitive disabilities. Journal of Public Child Welfare, 7(5), 536–548.
Hoover, D. W., & Kaufman, J. (2018). Adverse childhood experiences in children with autism spectrum disorder. Current Opinion in Psychiatry, 31(2), 128.
Horovitz, E. G. (1981). Art therapy in arrested development of a pre-schooler. The Arts in Psychotherapy, 8(2), 119–125. https://doi.org/10.1016/0197-4556(81)90005-8
Howe, D. (2006). Disabled children, parent-child interaction and attachment. Child and Family Social Work, 11, 95–106. https://doi.org/10.1111/j.1365-2206.2006.00397
Ippen, C. G., Noroña, C. R., & Lieberman, A. F. (2014). Clinical considerations for conducting child-parent psychotherapy with young children with developmental disabilities who have experienced trauma. Pragmatic Case Studies in Psychotherapy, 10(3), 196–211. https://doi.org/10.14713/pcsp.v10i3.1870
Jahng, K. E. (2020). South Korean mothers’ childhood abuse experience and their abuse of their children with intellectual and developmental disabilities: Moderating effect of parenting self-efficacy. Child Abuse & Neglect, 101, 104324. https://doi.org/10.1016/j.chiabu.2019.104324
Kerns, C. M., Newschaffer, C. J., & Berkowitz, S. J. (2015). Traumatic childhood events and autism spectrum disorder. Journal of Autism and Developmental Disorders, 45, 3475–3486.
Kiger, M. E., & Varpio, L. (2020). Thematic analysis of qualitative data: AMEE Guide No. 131. Medical Teacher, 42(8), 846–854. https://doi.org/10.1080/0142159X.2020.1755030
Kildahl, A. N., Bakken, T. L., Matre, E. A. W., Hellerud, J. M. A., Engebretsen, M. H., & Helverschou, S. B. (2021). Case study: Identification of anxiety and subsequent intervention in an adolescent male with autism, severe intellectual disability and self-injurious behaviour. International Journal of Developmental Disabilities, 67(5), 327–338.
Kim, Y. R. (2010). Personal safety programs for children with intellectual disabilities. Education and Training in Autism and Developmental Disabilities, 45(2), 312–319.
King, R., & Desaulnier, C. L. (2011). Commentary: Complex post-traumatic stress disorder. Implications for individuals with autism spectrum disorders—Part 2. Journal on Developmental Disabilities, 17(1), 47–59.
Lieberman, A. F., Van Horn, P., & Ippen, C. G. (2005). Toward evidence-based treatment: Child-parent psychotherapy with preschoolers exposed to marital violence. Journal of the American Academy of Child and Adolescent Psychiatry, 44(12), 1241–1248. https://doi.org/10.1097/01.chi.0000181047.59702.58
Lin, I. C., Tseng, L. Y., & Lee, Y. T. (2020). Post-traumatic stress disorder in an adolescent with Asperger syndrome. PsychiatriaDanubina, 32(34), 436–437. https://doi.org/10.24869/psyd.2020.436
Maclean, M. J., Sims, S., Bower, C., Leonard, H., Stanley, F. J., & O'Donnell, M. (2017). Maltreatment risk among children with disabilities. Pediatrics, 139(4). https://doi.org/10.1542/peds.2016-1817
Mandell, D. S., Walrath, C. M., Manteuffel, B., Sgro, G., & Pinto-Martin, J. A. (2005). The prevalence and correlates of abuse among children with autism served in comprehensive community-based mental health settings. Child Abuse & Neglect, 29(12), 1359–1372. https://doi.org/10.1016/j.chiabu.2005.06.006
Manders, J. E., & Stoneman, Z. (2009). Children with disabilities in the child protective services system: An analog study of investigation and case management. Child Abuse & Neglect, 33(4), 229–237.
Mansell, S., Sobsey, D., Wilgosh, L., & Zawallich, A. (1996). The sexual abuse of young people with disabilities: Treatment considerations. International Journal for the Advancement of Counselling, 19(3), 293–302.
Matson, J. L., & Shoemaker, M. (2009). Intellectual disability and its relationship to autism spectrum disorders. Research in Developmental Disabilities, 30(6), 1107–1114.
Mazefsky, C., Oswald, D., Day, T., Eack, S., Minshew, N., & Lainhart, J. (2012). ASD, a psychiatric disorder, or both? psychiatric diagnoses in adolescents with high-functioning ASD. Journal of Clinical Child & Adolescent Psychology, 41(4), 516–523.
Mazefsky, C. A., Herrington, J., Siegel, M., Scarpa, A., Maddox, B. B., Scahill, L., & White, S. W. (2013). The role of emotion regulation in autism spectrum disorder. Journal of the American Academy of Child & Adolescent Psychiatry, 52(7), 679–688.
McCarthy, J. (2001). Post-traumatic stress disorder in people with learning disability. Advances in Psychiatric Treatment, 7(3), 163–169. https://doi.org/10.1192/apt.7.3.163
McClure, K. S., Halpern, J., Wolper, P. A., & Donahue, J. J. (2009). Emotion regulation and intellectual disability. Journal on Developmental Disabilities, 15(2), 38–44. https://doi.org/10.13016/M28P01
McDonnell, C. G., Boan, A. D., Bradley, C. C., Seay, K. D., Charles, J. M., & Carpenter, L. A. (2019). Child maltreatment in autism spectrum disorder and intellectual disability: Results from a population-based sample. Journal of Child Psychology and Psychiatry, 60(5), 576–584. https://doi.org/10.1111/jcpp.12993
Mehtar, M., & Mukaddes, N. (2011). Posttraumatic stress disorder in individuals with diagnosis of autistic spectrum disorders. Research in Autism Spectrum Disorders, 5(1), 539–546. https://doi.org/10.1016/j.rasd.2010.06.020
Mevissen, L., Lievegoed, R., & De Jongh, A. (2011). EMDR treatment in people with mild ID and PTSD: 4 cases. Psychiatric Quarterly, 82(1), 43–57.
Mevissen, L., Didden, R., Korzilius, H., & de Jongh, A. (2017). Eye movement desensitisation and reprocessing therapy for posttraumatic stress disorder in a child and an adolescent with mild to borderline intellectual disability: A multiple baseline across subjects study. Journal of Applied Research in Intellectual Disabilities, 30, 34–41.
Mevissen, L., Ooms-Evers, M., Serra, M., de Jongh, A., & Didden, R. (2020). Feasibility and potential effectiveness of an intensive trauma-focused treatment programme for families with PTSD and mild intellectual disability. European Journal of Psychotraumatology, 11(1), 1777809.
Mevissen, L., Didden, R., & de Jongh, A. (2016). Assessment and treatment of PTSD in people with intellectual disabilities. In C. R. Martin, V. R. Preedy, & V. B. Patel (Eds.), Comprehensive guide to Post-Traumatic Stress Disorders, (pp. 281–299). https://doi.org/10.1007/978-3-319-08359-9_95
Miller, H. L., Pavlik, K. M., Kim, M. A., & Rogers, K. C. (2017). An exploratory study of the knowledge of personal safety skills among children with developmental disabilities and their parents. Journal of Applied Research in Intellectual Disabilities, 30(2), 290–300. https://doi.org/10.1111/jar.12239
Mohamed, A. R., & Mkabile, S. (2015). An attachment-focused parent–child intervention for biting behaviour in a child with intellectual disability: A clinical case study. Journal of Intellectual Disabilities, 19(3), 251–265.
Morgart, K., Harrison, J. N., Hoon, A. H., Jr., & Wilms Floet, A. M. (2021). Adverse childhood experiences and developmental disabilities: Risks, resiliency, and policy. Developmental Medicine & Child Neurology, 63(10), 1149–1154.
Munn, Z., Peters, M. D., Stern, C., Tufanaru, C., McArthur, A., & Aromataris, E. (2018). Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Medical Research Methodology, 18(1), 1–7.
NICE guidelines for supporting children who have experienced abuse and neglect (2017).https://www.nice.org.uk/guidance/ng76/resources/child-abuse-and-neglect-pdf-1837637587141.
NICE guidelines for supporting young people with PTSD (2018). https://www.nice.org.uk/guidance/ng116/resources/posttraumatic-stress-disorder-pdf-66141601777861.
Ooms-Evers, M., Van der Graaf-Loman, S., van Duijvenbode, N., Mevissen, L., & Didden, R. (2021). Intensive clinical trauma treatment for children and adolescents with mild intellectual disability or borderline intellectual functioning: A pilot study. Research in Developmental Disabilities, 117, 104030.
Paquette, G., Dion, J., Tremblay, K., Tourigny, M., Sonia, H., Bouchard, J., & Matteau, S. (2017). Differences between sexually abused children with and without intellectual disabilities. International Journal of Victimology, 14(34), 29–42.
Paquette, G., Bouchard, J., Dion, J., Tremblay, K. N., Tourigny, M., Tougas, A. M., & Hélie, S. (2018). Factors associated with intellectual disabilities in maltreated children according to caseworkers in child protective services. Children and Youth Services Review, 90, 38–45.
Peters, M. D., Marnie, C., Tricco, A. C., Pollock, D., Munn, Z., Alexander, L., ... & Khalil,H. (2020). Updated methodological guidance for the conduct of scoping reviews. JBI evidence synthesis, 18(10), 2119–2126.
Peterson, J. L., Earl, R. K., Fox, E. A., Ma, R., Haidar, G., Pepper, M., ... & Bernier, R. A. (2019). Trauma and autism spectrum disorder: Review, proposed treatment adaptations and future directions. Journal of child & adolescent trauma, 12(4), 529–547.
Prock, L., & Fogler, J. M. (2018). Trauma and neurodevelopmental disorder: Assessment, treatment, and triage. In J. M. Fogler & R. A. Phelps (Eds.), Trauma, autism, and neurodevelopmental disorders: Integrating research, practice, and policy, (pp. 55–71). Switzerland: Springer Nature. https://doi.org/10.1007/978-3-030-00503-0_4
Reiss, S., Levitan, G. W., & Szyszko, J. (1982). Emotional disturbance and mental retardation: Diagnostic overshadowing. American Journal of Mental Deficiency, 86(6), 567–574.
Reiter, S., Bryen, D. N., & Shachar, I. (2007). Adolescents with intellectual disabilities as victims of abuse. Journal of Intellectual Disabilities, 11(4), 371–387. https://doi.org/10.1177/1744629507084602
Rieffe, C., MeerumTerwogt, M., & Kotronopoulou, K. (2007). Awareness of single and multiple emotions in high-functioning children with autism. Journal of Autism and Developmental Disorders, 37(3), 455–465.
Romney, J. S., & Garcia, M. (2021). TF-CBT informed teletherapy for children with autism and their families. Journal of Child & Adolescent Trauma, 14(3), 415–424.
Rose, E., & Hardman, M. L. (1981). The abused mentally retarded child. Education and Training of the Mentally Retarded, 114–118.
Rumball, F. (2019). A systematic review of the assessment and treatment of posttraumatic stress disorder in individuals with autism spectrum disorders. Review Journal of Autism and Developmental Disorders, 6(3), 294–324.
Schneider, M., VanOrmer, J., & Zlomke, K. (2019). Adverse childhood experiences and family resilience among children with autism spectrum disorder and attention-deficit/hyperactivity disorder. Journal of Developmental & BehavioralPediatrics, 40(8), 573–580.
Schuengel, C., de Schipper, J. C., Sterkenburg, P. S., & Kef, S. (2013). Attachment, intellectual disabilities and mental health: Research, assessment and intervention. Journal of Applied Research in Intellectual Disabilities, 26(1), 34–46.
Shabalala, N., & Jasson, A. (2011). PTSD symptoms in intellectually disabled victims of sexual assault. South African Journal of Psychology, 41(4), 424–436.
Shannon, P., & Tappan, C. (2011). A qualitative analysis of child protective services practice with children with developmental disabilities. Children and Youth Services Review, 33(9), 1469–1475.
Sobsey, D. (2002). Exceptionality, education, and maltreatment. Exceptionality, 10(1), 29–46.
Spain, D., & Happé, F. (2020). How to optimise cognitive behaviour therapy (CBT) for people with autism spectrum disorders (ASD): A Delphi study. Journalof Rational-Emotive & Cognitive-Behavior Therapy, 38, 184–208. https://doi.org/10.1007/s10942-019-00335-1
Stack, A., & Lucyshyn, J. (2019). Autism spectrum disorder and the experience of traumatic events: Review of the current literature to inform modifications to a treatment model for children with autism. Journal of Autism and Developmental Disorders, 49(4), 1613–1625.
Sterkenburg, P. S., Janssen, C. G. C., & Schuengel, C. (2008). The effect of an attachment-based behaviour therapy for children with visual and severe intellectual disabilities. Journal of Applied Research in Intellectual Disabilities, 21(2), 126–135.
Strickler, H. L. (2001). Interaction between family violence and mental retardation. Mental Retardation, 39(6), 461–471. https://doi.org/10.1352/0047-6765
Sullivan, P. M. (1993). Sexual abuse therapy for special children. Journal of Child Sexual Abuse, 2(2), 117–125. https://doi.org/10.1300/J070v02n02_13
Surley, L., & Dagnan, D. (2019). A review of the frequency and nature of adaptations to cognitive behavioural therapy for adults with intellectual disabilities. Journal of Applied Research in Intellectual Disabilities, 32(2), 219–237.
Tharinger, D., Horton, C. B., & Millea, S. (1990). Sexual abuse and exploitation of children and adults with mental retardation and other handicaps. Child Abuse & Neglect, 14(3), 301–312. https://doi.org/10.1016/0145-2134(90)90002-B. PMID:2207799.
World Health Organisation. (2014) WHO traditional medicine strategy: 2014–2023 (p. 76). Geneva Switzerland: World Health Organisation.
Thomas-Skaf, B. A., & Jenney, A. (2021). Bringing social justice into focus: “Trauma-informed” work with children with disabilities. Child Care in Practice, 27(4), 316–332.
Tricco, A. C., et al. (2018). PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Annals of Internal Medicine, 169, 467. https://doi.org/10.7326/M18-0850
Verdugo, M. A., Bermejo, B. G., & Fuertes, J. (1995). The maltreatment of intellectually handicapped children and adolescents. Child Abuse & Neglect, 19(2), 205–215.
Vervoort-Schel, J., Mercera, G., Wissink, I., Van der Helm, P., Lindauer, R., & Moonen X. (2021). Prevalence of and relationship between adverse childhood experiences and family context risk factors among children with intellectual disabilities and borderline intellectual functioning. Research in Developmental Disabilities, 113. https://doi.org/10.1016/j.ridd.2021.103935.
Weiss, J. A., & Lunsky, Y. (2011). The brief family distress scale: A measure of crisis in caregivers of individuals with autism spectrum disorders. Journal of Child and Family Studies, 20, 521–528. https://doi.org/10.1007/s10826-010-9419-y
Weston, L., Hodgekins, J., & Langdon, P. E. (2016). Effectiveness of cognitive behavioural therapy with people who have autistic spectrum disorders: A systematic review and meta-analysis. Clinical Psychology Review, 49, 41–54.
Wissink, I. B., Van Vugt, E., Moonen, X., Stams, G. J. J., & Hendriks, J. (2015). Sexual abuse involving children with an intellectual disability (ID): A narrative review. Research in Developmental Disabilities, 36, 20–35.
Acknowledgements
The authors wish to thank Ms. Louise Marbina for her assistance in the screening process.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions
Author information
Authors and Affiliations
Contributions
LK, AU, and KL conceptualised the study. LK conducted the literature search. LK, JB, and LM completed data screening, and LK undertook extraction. LK, AU, KL, and MSS completed the data analysis and interpretation, and LK drafted the manuscript. LK, AU, KL, MSS, and JB revised drafts and approved the final version for publication.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kalisch, L.A., Lawrence, K.A., Baud, J. et al. Therapeutic Supports for Neurodiverse Children Who Have Experienced Interpersonal Trauma: a Scoping Review. Rev J Autism Dev Disord (2023). https://doi.org/10.1007/s40489-023-00363-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40489-023-00363-9