Abstract
Background
Self-management (SM) interventions are supportive interventions systematically provided by healthcare professionals, peers, or laypersons to increase the skills and confidence of patients in their ability to manage chronic diseases. We had two objectives: (1) to summarise the preferences and experiences of patients and their caregivers (informal caregivers and healthcare professionals) with SM in four chronic diseases and (2) to identify and describe the relevant outcomes for SM interventions from these perspectives.
Methods
We conducted a mixed-methods scoping review of reviews. We searched three databases until December 2020 for quantitative, qualitative, or mixed-methods reviews exploring patients’ and caregivers’ preferences or experiences with SM in type 2 diabetes mellitus (T2DM), obesity, chronic obstructive pulmonary disease (COPD), and heart failure (HF). Quantitative data were narratively synthesised, and qualitative data followed a three-step descriptive thematic synthesis. Identified themes were categorised into outcomes or modifiable factors of SM interventions.
Results
We included 148 reviews covering T2DM (n = 53 [35.8%]), obesity (n = 20 [13.5%]), COPD (n = 32 [21.6%]), HF (n = 38 [25.7%]), and those with more than one disease (n = 5 [3.4%]). We identified 12 main themes. Eight described the process of SM (disease progression, SM behaviours, social support, interaction with healthcare professionals, access to healthcare, costs for patients, culturally defined roles and perceptions, and health knowledge), and four described their experiences with SM interventions (the perceived benefit of the intervention, individualised care, sense of community with peers, and usability of equipment). Most themes and subthemes were categorised as outcomes of SM interventions.
Conclusion
The process of SM shaped the perspectives of patients and their caregivers on SM interventions. Their perspectives were influenced by the perceived benefit of the intervention, the sense of community with peers, the intervention’s usability, and the level of individualised care. Our findings can inform the selection of patient-important outcomes, decision-making processes, including the formulation of recommendations, and the design and implementation of SM interventions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
We identified 12 main themes covering aspects of the process of self-management (SM) alongside the disease trajectory, the factors that influence this process, and experiences of SM interventions from the perspective of patients and caregivers. |
Our findings on what patients with the four chronic diseases (type 2 diabetes mellitus, obesity, chronic obstructive pulmonary disease, or heart failure) and their caregivers describe as relevant regarding SM should be considered when selecting patient-important outcomes in this context. |
This set of themes can help guide the design and implementation of SM interventions. |
Our findings can inform healthcare decision making, including the formulation of recommendations and the development of decision aids. |
1 Introduction
The increasing burden of chronic diseases on healthcare and society has become a significant concern over the last decade. A response to this challenge requires moving towards more patient-centred strategies, one of the main components of which is self-management (SM) interventions [1,2,3]. SM interventions are supportive interventions systematically provided by healthcare professionals, peers, or laypersons to increase the skills of patients and their confidence in their ability to manage chronic diseases [4]. Despite the increasing number of SM interventions and promising evidence of their beneficial effects, no structured and accessible summaries of evidence about their effectiveness, cost effectiveness, and implementation considerations are yet available [5, 6]. In this context, making informed decisions about the use of SM at clinical, organisational, and policy levels is still challenging. To bridge this gap, the project COMPAR-EU was designed to identify the most effective and cost-effective SM interventions for four high-priority diseases in Europe: type 2 diabetes mellitus (T2DM), obesity, chronic obstructive pulmonary disease (COPD), and heart failure (HF) [7].
In COMPAR-EU, the perspectives of patients and caregivers (informal caregivers and healthcare professionals) on SM were contemplated as a key component in, for example, the development of the Core Outcome Sets (COS) of SM interventions and the development of recommendations [8, 9]. Perspectives are conceptualised as the result of preferences for and experiences with SM. Preferences represent the relative desirability of specified alternatives among outcomes [10], and experiences explain the nature and impact of chronic diseases and how a specific intervention affects the health and quality of life of patients [11].
In the last decade, systematic reviews of qualitative and mixed-method research synthesis have provided a more detailed understanding of the complexity of chronic diseases and their treatment from the perspective of patients and their caregivers [12, 13]. More recently, there is a growing interest in assessing patients’ preferences and developing systematic reviews of quantitative preferences studies [14]. However, to date, no systematic analysis has been undertaken of quantitative and qualitative evidence focused on patients’ and caregivers’ preferences for and experiences with SM. This analysis will shed light on what matters most to patients and caregivers and will be informative for healthcare decision making in this field (e.g., design, implementation or evaluation of SM interventions and alignment of recommendations with patients’ values). We believed a mixed-methods scoping review of reviews [15, 16] would be a suitable method to synthesise these sources of evidence. We had two objectives: to summarise the preferences and experiences of patients, informal caregivers, and healthcare professionals with SM in four chronic diseases and to identify and describe the relevant outcomes for SM interventions from these perspectives.
2 Methods
We conducted a mixed-methods scoping review of reviews based on Arksey and O’Malley’s methodology [17,18,19] and reported findings using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) checklist [20].
2.1 Eligibility Criteria
2.1.1 Type of Reviews
We included systematic reviews of primary studies of any design using quantitative, qualitative, or mixed synthesis methods. We considered a review as ‘systematic’ when it reported a search strategy in at least one database. We excluded primary studies and overviews.
2.1.2 Population
We included reviews that covered at least one of the following populations of interest: (1) adult patients (aged ≥ 18 years) with one of the four selected chronic diseases (T2DM, obesity, COPD, or HF), without restrictions on severity; (2) informal caregivers, mostly family members who take care of patients without payment; and (3) healthcare professionals, at any level of care in charge of patients with these chronic diseases. We excluded reviews addressing patients with type 1 diabetes mellitus, gestational diabetes, pregnancy-related obesity, or mental or oncological comorbidities. Reviews addressing more than one chronic disease or type of population were included if they reported disaggregated results.
2.1.3 Phenomenon of Interest
We included reviews that explored (1) patients’ preferences, (2) caregivers’ preferences (informal caregivers and healthcare professionals), (3) health states related to the disease (outcomes), and (4) experiences with SM. SM was conceived as a dynamic, interactive, and daily process in which individuals managed chronic diseases [21]. Preferences regarding health states can be reported as utility and non-utility measures [22,23,24]. Health state utility measures represent the strength of individuals’ preferences for specific health states or conditions, using a scale typically anchored at ‘one’ (full health) and ‘zero’ (dead) [25, 26]. Non-utility measures include other measures explaining patients’ preferences through qualitative (e.g., focus groups) or quantitative (e.g., surveys) methods [24]. Experiences with SM could relate to any processes of SM [21] or experiences with SM interventions. We excluded reviews evaluating the effectiveness or cost effectiveness of SM interventions.
2.1.4 Context or Setting, and Language
We included reviews of studies conducted in any country or setting except those limited to inpatient care. We only included reviews published in the English language.
2.2 Search Strategy
We developed and conducted specific searches in MEDLINE (through PubMed), CINAHL, and PsycINFO from inception to December 2020. We had the assistance of a senior researcher expert in search strategies development (IS). We included CINAHL and PsycINFO as they are considered good sources of qualitative studies and include topics related to nursing and psychological interventions [27]. We included terms designed explicitly for values and preferences studies [28] combined with medical subject heading terms and free text for each chronic disease. To enhance the sensitivity for qualitative reviews, we included qualitative synthesis method terms (e.g., meta-ethnography). We adapted the MEDLINE strategy for each database using database-specific headings. We applied the review filters available in each database [29].
2.3 Selection of Studies
Four authors (ENDG, DF, JP, KS), working in pairs, were involved in the selection of studies. A calibration with 20% of references was conducted by pairs. After achieving 80% agreement in calibration, one author conducted title and abstract screening and a second author cross-checked this selection. Disagreements were solved by discussion or with the help of a third author. The same process was applied for full-text assessment. References were managed with Endnote X9.
2.4 Data Collection
We collected the general characteristics and main findings of each review in a previously pilot-tested data extraction form. Five authors (ENDG, DF, JP, KS, AVG), working in pairs, were involved in data collection. After the first author extraction, a second author cross-checked data. Disagreements were solved by discussion. For reviews exploring preferences quantitatively, we collected the health states assessed, the utility estimates, and methods used to obtain them. For reviews exploring preferences or experiences qualitatively, we included descriptive summaries of findings of primary studies (second-order constructs) or synthesised summaries proposed by the review authors (third-order constructs) [30].
2.5 Analysis and Synthesis
We classified reviews according to the design of included primary studies into (1) quantitative systematic reviews (quantitative research), (2) qualitative evidence synthesis (qualitative research) [31], (3) mixed-methods research synthesis [32] (quantitative and qualitative or mixed-methods designs), and (4) other types of review (literature reviews or scoping reviews).
Quantitative data concerning utility measures for different health states (or outcomes) were tabulated and narratively synthesised by topic and methods applied. Qualitative data concerning the second- and third-order constructs of qualitative evidence synthesis, narrative findings (i.e., non-utility measures) of quantitative systematic reviews, or mixed-methods research synthesis were synthesised applying a descriptive thematic synthesis proposed by Thomas and Harden [33]. This process included (1) inductively codifying the findings line by line, (2) proposing descriptive themes, and (3) identifying the main themes based on conceptual similarities within and across chronic diseases. One author (ENDG) conducted these steps independently, then a second author cross-checked and validated the descriptive and main themes (DF, JP, KS, AVG). Disagreements were solved by discussion or with the help of a third author.
A final step included categorising the identified descriptive themes and subthemes into three categories: SM intervention outcomes, modifiable factors (barriers or facilitators) of SM interventions, or both SM intervention outcomes and modifiable factors. Two authors (ENDG, MH) decided the category to which each theme or subtheme belonged based on their importance for the development of SM interventions, their current use as a measure of effectiveness, and their potential impact. One author (ENDG) first did this independently, and this was cross-checked by a second author (MH). This classification was developed and refined through an iterative process.
3 Results
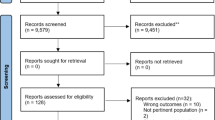
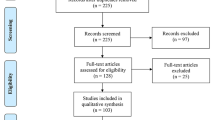
Searches resulted in 11,785 unique references; 448 records were selected for full-text screening, and a total of 148 reviews were finally included (Fig. 1). Excluded reviews and the reasons for their exclusion are available in ESM 2.
PRISMA flowchart. *Reasons for exclusion: method of evaluation (n = 11), phenomenon of interest (n = 208), population (n = 26), study design (n = 48), other reasons (n = 7). 1Only T2DM: 53, with other diseases: 2. 2Only COPD: 32, with other diseases: 3. COPD chronic obstructive pulmonary disease, HF heart failure, T2DM type 2 diabetes mellitus
3.1 Characteristics of Included Reviews
We included 148 reviews, distributed as follows: T2DM (n = 53 [35.8%]), obesity (n = 20 [13.5%]), COPD (n = 32 [21.6%]), HF (n = 38 [25.7%]), and those with more than one chronic disease (n = 5 [3.4%]). Three included both COPD and HF [34,35,36], one included both T2DM and COPD [37], and one included COPD, HF, and T2DM [38] (Table 1; ESM 3). Overall, almost half of the reviews were published after 2015 (n = 70 [47.3%]), were qualitative evidence synthesis (n = 78 [52.7%]), and included ≤20 studies (n = 81 [54.8%]). Most reviews addressed only the perspective of patients (n = 113 [76.4%]), with some including more than one perspective (n = 23 [15.5%]), and a minority focused on informal caregivers or healthcare professionals only (n = 12 [8.1%]). The majority addressed experiences with the SM process (n = 110 [94.4%]); others also focused on experiences with SM interventions (n = 40 [27.0%]) or preferences for health states (n = 19 [12.8%]).
3.2 Identified Themes
We identified 12 main themes, eight regarding the process of SM and four regarding experiences with SM interventions (Fig. 2).
3.2.1 The Process of Self-Management
The process of SM included four themes about the experience of SM, and four referred to factors influencing the SM process.
3.2.1.1 The Experience of Self-Management
Progression of the Disease T2DM was described as a complex experience characterised by ambivalent feelings [39]. Perception of severity changed over time and was influenced by the presence of symptoms and complications [40]. Most patients with COPD had never received a formal diagnosis or were not informed of their diagnosis for many years [41]. They described their disease as a “roller coaster” experience [42,43,44], where dyspnoea was the prominent symptom [42, 44, 45]. In these patients, the extent of symptom relief was considered even more important than treatment for extending life [46]. COPD exacerbations were experienced as “near death” or the “shadow of death”; they were unpredictable and led to the patient living in a state of constant arousal and hypervigilance [44, 45, 47]. HF was also described as an extreme, unpredictable, and confusing disease [48] with ubiquitous, ongoing, and disruptive symptoms [48,49,50,51,52,53].
Competing comorbidities were described as barriers to SM across the four chronic diseases [51, 54,55,56,57,58,59,60,61]. We identified utility estimates for eight health states: T2DM diagnosis [62, 63], weight change in T2DM and obesity [62, 64], COPD severity [46, 65, 66], moderate and severe exacerbations [46, 65, 67, 68], dyspnoea and its progression [46], HF diagnosis [69, 70], chronic heart disease [71], changes in severity levels [69], and angina and its progression [70]. These health states reflect how the perceived importance increased with disease severity. This theme included four subthemes: physical functioning, psychological distress and stigma, fear of complications, and mortality.
Physical Functioning Life transitions, getting older, and cognitive issues could inhibit SM in T2DM [54]. Most patients with obesity perceived themselves as having poor fitness and low confidence in their physical capability [61]. In COPD and HF, fatigue was a common symptom with a negative impact on patient quality of life [35]. In these patients, damaged lung function, declines in cognitive status, and effects of symptoms and treatments interrupted patients’ previous functioning and increased dependency [42, 43, 49, 51, 52, 55, 72, 73]. Because of symptoms, some patients lost the ability to engage in favourite pastimes and social activities [50, 56, 74], leading to involuntary social isolation [41].
Psychological Distress and Stigma Patients’ psychological distress was expressed across the four chronic diseases in terms of a sense of failure, loss of control, self-blame, anxiety, frustration, fear, sense of isolation, negative attitudes or impaired mood, depression, and loss of independence and well-being [40, 41, 51, 54, 56, 59, 61, 74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98]. Informal caregivers of patients with HF or COPD also described conflicting emotions [36]. Some healthcare professionals experienced negative emotions in dealing with patients with T2DM, such as frustration around patient compliance [93] or inadequacy and helplessness at not being able to address psychosocial concerns [99].
In patients with T2DM, obesity, or COPD, external stigma included experiences of blame or negative judgement from healthcare professionals or others. Stigma was associated with severed relationships; social isolation; reduced work opportunities; and distress, depression, anxiety, and lowered self-esteem, self-worth, and patient self-efficacy [37, 41, 81, 88, 89, 91, 100]. In patients with T2DM, the perceived stigma was related to their experience of insulin self-injection [37, 76, 79, 101]; in patients with COPD, the internalised stigma was evident when they described their disease as “self-inflicted” [41].
Fear of Complications The relevance of acute and chronic complications of T2DM from the perspective of patients varied [62, 63, 78, 102,103,104]. The health states with the highest impact on patients’ quality of life (lowest utility values) were severe painful diabetic polyneuropathy [102], stroke, end-stage renal disease, and amputation [63]. Achieving glycaemic control was valued more highly than avoiding hypoglycaemia, except for nocturnal hypoglycaemia [105]. Older patients were more concerned about detecting low than high blood glucose levels [106]. The main concerns related to hypoglycaemic episodes were not being able to predict and manage them. These factors influenced patients’ emotional state, daily functioning, and engagement with their insulin treatment [75, 79, 107].
Mortality In T2DM, COPD, and HF, both patients and informal caregivers recognised feeling fear about worsening symptoms and about dying prematurely and uncertainty about the future, especially during acute events that required hospitalisation [36, 56, 73, 75]. In HF, both patients and healthcare professionals waited for the other to initiate end-of-life conversations, differentiating between a “good” and “bad” death, the latter defined as being unexpected and unprepared [49, 51, 56, 86, 108, 109].
Self-Management Behaviours Only when patients accepted their T2DM were they motivated to take care of their health. Some were motivated to SM because of fear of leg amputation [106]. Hypoglycaemia, as a learning experience in patients, contributed towards reflective learning, which was important in effective SM of blood glucose [107]. Patients with T2DM preferred flexible SM routines to ensure minimal disruption of their everyday life [54, 110]. In this subpopulation, having patience predicted more self-care behaviours [111]. In COPD, and HF, previous experiences also helped patients gain expertise in their body responses, allowing them to adopt a regulatory role and adjust their lifestyle [41, 73, 92, 112]. These changes were sometimes driven by their motivation to prevent a COPD exacerbation [45, 73, 74]. Stable COPD management was perceived to be integrated into everyday life rather than being a priority [41]. Having a greater sense of control, using problem-focused coping strategies, and perceived self-efficacy appeared to be associated with favourable outcomes in COPD [45, 84, 113, 114] and HF [34, 56, 58, 109, 115,116,117,118,119,120]. This theme included four subthemes: help or health-seeking behaviour, adherence to treatment, smoking behaviours, and weight control.
Help or Health-Seeking Behaviour Patients with obesity, especially women, reported personal barriers to attending appointments or discussing their concerns with healthcare professionals [81, 89]. Patients with COPD typically sought initial treatment for an acute episode rather than for early symptoms. Most patients articulated ambivalent attitudes towards help seeking, even in emergencies, which were driven by a fear of dying, and most also often expressed a strong desire to maintain autonomy [43,44,45, 47, 72, 121]. Similarly, some patients with HF chose to take an active role, whereas others relinquished the responsibility to others [59] with feelings of losing control [56]. In obesity, healthcare professionals’ uncertainty over their responsibilities could lead them to take a limited or inconsistent role in delivering services [81].
Adherence to Treatment Patients’ adherence to treatment usually refers to both medication-taking and lifestyle behaviours [40]. The influence of habits on adherence to treatment, diet, and lifestyle plans was challenging for most patients with T2DM [83, 92,93,94,95,96, 99, 106, 122, 123]. In T2DM, successful experiences reinforced treatment beliefs [40], whereas, in obesity, most patients were attracted to realistic, feasible, and inclusive diet plans [90, 124, 125]. Reasons for weight loss failure included stress, slow weight loss, boredom, comfort and reward eating, lack of time, and feeling depressed or upset [126]. In patients with COPD, those who generally adhered well to medication were motivated by the fear of dyspnoea and vulnerability [44]. Lower adherence was associated with disease severity, concerns about adverse effects, smoking, forgetfulness, comorbidities, and polypharmacy [55]. In HF, medication management and compliance with a sodium-restricted diet were reported to be influenced by physical, social, and material determinants, knowledge, and cost-benefit analysis [109, 127]. In T2DM and HF, integrating SM strategies into everyday routines increased adherence [40, 109, 117] where informal caregiver support was a facilitator [117]. In contrast, frequent changes of healthcare professionals or conflicting advice between services were barriers to adherence [128]. In T2DM, most healthcare professionals viewed non-adherence mostly as patients’ failure [99]. This subtheme included two more specific themes: adverse events and treatment burden.
-
Adverse events: Some patients with T2DM highly valued avoiding transient nausea and gastrointestinal adverse effects, as measured in willingness-to-pay or discrete-choice exercises [105, 129]. Fear and anxiety about hypoglycaemia, injection pain, and weight gain were perceived as significant mediators in insulin utilisation [130], whereas, in COPD, some considered avoiding an adverse event to be more important than other treatment aspects [46].
-
Treatment burden: Emotional reactions to treatment progression (diet to pills to insulin) affected the way patients coped with T2DM [40, 96]. Misconceptions and a lack of knowledge led some patients to fear insulin therapy [76, 131]. Insulin therapy and dose adjustments were burdensome, time consuming, complicated, and a cause of discomfort [75,76,77, 95, 130, 131]. For patients who had never been treated with insulin, oral administration and reduction of the number of insulin injections were preferred [105]. Patients with COPD and their informal caregivers found it challenging to balance daily life activities with the treatment workload [41]. In HF, some patients recognised cognitive vulnerabilities in adhering to treatment regimens [109].
Smoking Behaviours Smoking in patients with COPD was associated with anger, guilt, self-blame, and shame, all of which can adversely impact motivation for SM [43, 44, 47, 73, 91]. Healthcare professionals need to be aware of patients’ smoking history when providing advice to quit smoking [47]. However, for patients who smoked, this advice could conflict with their increased desire to smoke as a coping strategy [43]. Some patients identified smoking cessation as a desirable goal yet had no conviction that they could realistically achieve this [132].
Weight Control For some patients with T2DM, weight control was ranked as very important, as measured in willingness-to-pay or discrete-choice exercises [105, 129], and was a concern when starting insulin therapy [131, 133]. Weight self-monitoring in obesity was considered as fostering ownership and self-knowledge, increasing the ability to understand and self-control weight loss and maintenance success [134]. Patients with heart failure were also concerned about weight-related problems and weight monitoring [50].
Social Support Social networks, perceived social support (financial or emotional), gender roles, and marital status appeared to influence self-care and the perceived barriers to SM across the four chronic diseases [37, 41, 42, 45, 50, 60, 85, 92, 95, 96, 98, 107, 110, 114, 119,120,121, 123, 130, 131, 135,136,137,138,139,140]. A lack of or insufficient social support could affect mortality and morbidity outcomes [57, 85, 92, 98]. In T2DM, the desire to participate in family events was a powerful motivator [141]. Patients with COPD described family and friends as the main support for treatment workload [41]. However, the obstructive behaviours of some families were barriers to SM [96, 123, 124, 130, 141]. Social relationships influenced the perceptions of patients with obesity [142]. In HF and COPD, informal caregivers reported perceiving insufficient social support [36, 143, 144]. This theme included two subthemes: informal caregivers’ burden and patient–informal caregiver partnership.
Informal Caregivers’ Burden Most informal caregivers of patients with COPD [41, 43, 44, 145] or HF [36, 143, 144, 146, 147] considered their role to be challenging and burdensome, affectively and cognitively demanding, and involving feelings of anxiety, fear, loss of control, sense of duty, loss of intimacy, social isolation, declining energy levels, and adverse effects on quality of life. Informal caregivers described undergoing a significant role change, with more domestic tasks and less personal time [36]. Despite the difficulties experienced, they recognised their role as rewarding and reported having increased satisfaction and self-esteem, a sense of solidarity, and experiencing positive effects on family relationships [36, 146,147,148].
Patient–Informal Caregiver Partnership Positive care partnerships contributed to SM and included shared activities in T2DM [106, 141] and HF [36, 119, 120, 140]. Patients valued informal caregivers’ help in identifying acute and chronic clinical status changes and contributing daily and positively to self-care [141]. Informal caregivers of patients with COPD described that they had to adjust their routines and be vigilant [36]. In HF, informal caregiver support was seen to facilitate adherence, especially during symptom exacerbation [117].
Interaction with Healthcare Professionals Across the four chronic diseases, factors that enhanced adherence to SM tasks included adequate communication with healthcare professionals; empathy, emotional support, relational, and compassionate care from healthcare professionals, and feeling confident in their competence [41, 42, 44, 45, 47, 50, 54,55,56, 59, 60, 81, 86, 89, 95, 96, 98, 106, 108, 121, 123, 130, 149]. Nevertheless, fear of being judged, not wanting to disappoint healthcare professionals, embarrassment, language discordance, and experiences of lack of respect, support, and understanding from healthcare professionals hindered effective collaborative management [57, 85, 89, 99, 107, 110, 128, 149]. Patients felt ownership when their views and experiences were valued [150], but in some cases, patients were not always good at expressing their needs [98]. Most patients with HF had trouble explaining breathlessness [53]. In COPD and HF, most informal caregivers felt like outsiders or abandoned in care processes [36, 143, 151].
Healthcare professionals considered limited resources, heavy workloads, or environmental constraints to be barriers to implementing SM [93, 143]. Of these, consultation time was the most frequently reported by both patients and healthcare professionals [41, 89, 96, 99, 123, 128, 130]. In T2DM, some healthcare professionals reported not being able to directly address patients’ broader psychosocial SM because of a lack of experience or training in effective communication, counselling, goal setting, and shared decision making [57, 99]. In obesity, some healthcare professionals reported feeling frustrated with the scarcity of weight loss alternatives [81, 152]. In COPD, others stated that they preferred to wait for patients to ask questions [108]. In HF, for some healthcare professionals, contemplating questions was challenging because they felt patients were distracted and unable to pay attention [112]. This theme included two subthemes: perceived quality of care and visits or contacts with healthcare professionals.
Perceived Quality of Care In T2DM and COPD, most patients felt the information provided during visits was often insufficiently explained [41, 106]. Informal caregivers also found that information was often inadequate [36]. Most patients with obesity were dissatisfied with healthcare professionals’ management of the disease and their professional knowledge [89]. Patients with COPD noted that some encounters with generalist healthcare professionals led to delays in accessing specialist care [41]. Similarly, in HF, some patients expressed dissatisfaction with the ability of healthcare professionals to deal with the broad spectrum of symptoms and complex medication regimens [86].
Visits or Contacts with Healthcare Professionals In obesity, women with a high body mass index were more likely to delay or cancel appointments because of embarrassment or other concerns [89]. Lack of confidence in community-based services could lead some patients with COPD to seek hospital admission [43]. Patients with COPD experienced relief from the demands of SM when hospitalised [41]. However, others considered the hospital stay to be a chaotic, confusing, and disruptive experience [41].
3.2.1.2 Factors that Influenced Self-Management
Access to Healthcare Factors that restricted timely access to healthcare services were reported across the four chronic diseases and included the associated cost of treatment, lack of health insurance, lack of community-based resources, distance, weather, transportation, and structural or cultural barriers [43, 72, 94, 121, 123, 130, 153, 154]. Access to a specialist, nursing care, SM programmes, and alternative therapy was an essential factor for SM [54, 98, 110]. However, most patients found it challenging to access dedicated services [48, 72, 121, 128] and perceived a lack of care coordination at different levels [41, 86, 99, 108, 155].
Cost for Patients Costs associated with treatment, transport, lack of insurance, and financial instability were reported as major barriers for SM and accessing healthcare in all chronic diseases [41, 54, 83, 96, 110, 119, 120, 122, 137]. Weight maintenance was affected by limited finances and competing responsibilities [125]. However, some patients were less concerned about costs than about weight loss, glycaemic control [129], and adverse events [46, 109]. The benefits of weight loss in obesity also came with costs such as the time and effort needed to control weight, stress, frustration, and guilt over control failures [90].
Culturally Defined Roles and Perceptions Religious beliefs or cultural backgrounds could affect patients' willingness to improve their health [54, 57, 83, 94, 96, 98, 110, 115, 119, 122, 136, 156]. In T2DM, patients from ethnic minorities living in Western countries found it challenging to follow dietary, activity, or treatment (insulin) recommendations that conflicted with their beliefs or traditions [54, 122, 130, 135, 138, 139]. Patients from ethnic minorities with HF were less likely than Western patients to adhere to an SM programme [136].
Health Knowledge Most patients across the four chronic diseases felt they had limited knowledge or skills and that this reduced their capacity to engage in active SM [43, 49, 51, 54, 56, 59,60,61, 72,73,74, 78, 86, 93, 106, 109, 117, 118, 120, 128, 153, 157]. Most patients gained knowledge from experiences, whereas others learned from the literature [123]. Patients with HF often had aetiology misconceptions or did not perceive breathlessness as an indication of worsening disease [53]. In T2DM [54, 57, 78, 82], HF [53], and obesity [88], some patients, despite having adequate knowledge or information, reported that it was difficult to apply in practice or to reconcile with other advice. Knowledge gaps should ideally be addressed at each patient’s pace; for example, some patients reported conflict between wanting information and fear of diminishing hope in COPD [42, 98, 150] and HF [112].
In HF and COPD, informal caregivers experienced ambiguity and uncertainty in their role [36, 59, 117, 143, 151]. Most had no formal care training and devised personal strategies [36, 144]. In T2DM, some healthcare professionals also reported that remaining aware of changing recommendations [93] or methods to help patients to manage insulin effectively was challenging [79]; others expressed difficulties identifying end-of-life stages in patients with COPD [43]. Healthcare professionals reported some misconceptions about the provision of care; for instance, some did not consider early COPD to be a fatal disease [43].
3.2.2 Experience with Self-Management Interventions
The SM interventions assessed by the reviews in our study included SM education programmes, physical activity programmes, weight loss interventions, telehealth interventions, and self-monitoring programmes. Four themes were identified from patients’ and caregivers’ preferences and experiences regarding SM interventions: perceived benefit (importance) of the intervention, individualised care, sense of community, and usability.
3.2.2.1 Perceived Benefit (Importance) of the Intervention
The absence of symptoms and the perceived non-importance of the intervention, not recognising the risk of complications, pessimistic beliefs, and negative perceptions on the programme diminished SM efforts in patients with T2DM [54, 60, 78, 82, 153], COPD [149, 159], or HF [70, 160]. Moreover, those who experienced adverse effects related to SM or threats of further harm were less willing to continue with the type of intervention involved [54].
In SM educational programmes for T2DM or COPD, most patients reported increased confidence when getting prompt, tailored advice from qualified and competent healthcare professionals [41, 155, 161]. They used the information as a motivator and supported technologies that allowed them to receive support from healthcare teams [161]. Increased knowledge provided a greater sense of control [41], increased confidence in SM intervention, improved communication with healthcare professionals, reduced fears of deterioration, prevented hospitalisation, improved anxiety and depression, and increased ability to deal with negative emotions [132, 155]. However, some informal caregivers believed that COPD SM counselling provided insufficient practical advice [151].
Motivation to undertake physical activity was developed from expected or experienced benefits. Patients with T2DM, obesity, and COPD remarked on several benefits of physical activity and weight loss interventions, including improved disease management; increased energy, enjoyment, and sense of well-being; regaining or maintaining mobility, fitness, and longevity; improved quality of life; and positive body image [87, 124, 126, 132, 153].
Telehealth interventions (provision of care from a distance using communications technologies) in T2DM, COPD, and HF were generally perceived as increasing social connectedness and enabling positive user experiences. They were perceived as contributing to increased knowledge, triggering actions, supporting SM, and promoting shared decision making [38, 113, 155, 158, 162, 163]. Some patients perceived this type of intervention to be as satisfactory as a nurse home visit [34]. However, others experienced initial apprehension because of their unfamiliarity with and doubts regarding the reliability of the technology or because of their limited motor skills and vision [38, 163]. Others were concerned about the loss of personal contact, increased out-of-pocket costs, loss of privacy, and unavailability of some services, and preferred face-to-face communication [34, 38, 163, 164]. For some healthcare professionals, telehealth interventions reduced the number of emergency department visits and hospital admissions [34]. However, for others, it represented an increase in workload [47, 113].
The perceptions of patients with T2DM and healthcare professionals regarding interventions that encouraged self-monitoring blood glucose were disparate. Healthcare professionals emphasised strict control, whereas patients focused on quality of life [77]. Most patients felt that self-monitoring in COPD provided greater clinical insight with time and further education [155]. This theme was influenced by three subthemes: physical activity barriers, psychological barriers to uptake of SM interventions, and technological (digital) literacy.
Physical Activity Barriers Physical impairments were barriers to physical activity. Common physical impairments included perceived physical state, weakness, cardiovascular endurance, frailty, range of motion, muscular strength, and balance in HF [42, 159, 165] and T2DM [153]. Although most patients acknowledged the benefits of regular exercise, some considered it burdensome [75, 153]. Patients’ feelings of being too old, having an altered body, and being forced to do more than they could manage were barriers to exercise in HF [98, 137]. However, patients completing SM programmes reported having more energy and requiring assistance less often [163]. Attitudes towards pulmonary rehabilitation varied [47, 162, 165,166,167]. In COPD, barriers to exercise were symptoms that evoked anxiety and fear, restricted social support and maintenance sessions, and lack of positive feedback [168].
Psychological Barriers to Uptake of Self-Management Interventions In patients with T2DM, feelings of helplessness, anger, frustration, and fear limited their participation in physical activity [169]. Other factors included having a poor body perception and feelings of powerlessness and disappointment, mainly influenced by unrealistic expectations, in obesity [88,89,90, 125, 170]; anxiety about dyspnoea in COPD [42, 44, 73, 113, 165]; and technology anxiety in COPD and HF [34]. Reframing the dietary regimen made weight control seem less burdensome [171]. Participating in a weight loss programme required inner strength, despite many patients feeling they were dealing with addiction, and maintenance was a constant struggle [126].
Technological (Digital) Literacy Most healthcare professionals and patients with T2DM [156, 164], COPD, and HF [37] found telehealth to be easy to use and a non-intimidating intervention. However, some others felt uncomfortable since it often required a steep learning curve [34, 172], which, in some cases, produced “technology anxiety” [34]. In technology-assisted programmes, a lack of technical skills and the complexity and difficulty of text messaging or editing their data were barriers in T2DM [161] and obesity [87].
Individualised Care Across the four chronic diseases, patients valued and responded better to education and advice tailored to their changing needs over time and to their personal factors [153, 155, 161, 173], but healthcare professionals did not always do this [95]. Patients valued being heard by their healthcare professionals and appreciated when they enquired about their personal circumstances [99, 155]. Patients with T2DM reported that self-monitoring blood glucose without tailored education was challenging [99, 150], and patients with diabetic foot ulcer required more holistic care [78]. Some patients with COPD preferred more instrumental support [156] and continued support from healthcare professionals [168]. Patients using wearable technology for weight management found necessary tailoring interventions to be motivating [174]. In HF, some women felt that cardio-rehabilitation programmes failed to meet their preferences [137]. Some nurses in charge of patients with COPD perceived an absence of individualised care [44]. When exploring participants' perceptions of culturally tailored interventions, most reported feeling motivated, supported, and empowered [138, 173].
3.2.2.2 Sense of Community with Peers
Across the four chronic diseases, online forums and self-help/support groups allowed patients to gain acceptance, with a sense of community and belonging being fostered [41, 106, 112, 132, 155, 163, 175]. Supportive relationships helped motivate attendance at programmes and promote healthy eating and exercise [132, 175]. Some patients did not participate in forums and preferred to keep their privacy or real-life contacts [161]. Informal caregivers of patients with HF found support groups useful [144].
3.2.2.3 Usability of Self-Management Equipment
Some patients with T2DM reported that the equipment required for glucose monitoring was burdensome [77]. Both healthcare professionals and patients often found foot care telemonitoring equipment easy to use [156]. Telehealth problems included difficulty connecting to the system, equipment failure, loss of data, and failed transmission [34, 47, 163]. Patients preferred technology-assisted programmes that were easy to navigate and appreciated concise information without medical jargon [161]. Healthcare professionals considered that few patients could independently navigate these programmes [161]. The specific design of wearable devices for weight management in obesity could decrease their adoption [174]. Digital games in HF were valued for their convenience and functionality, whereas barriers included sensory limitations [176].
3.3 Identified Themes by Disease and Perspective
Figure 3 presents the distribution of themes and subthemes by chronic disease and perspectives. Most themes were consistently identified across the four conditions, with only a few disease-specific themes. For example, fear of complications emerged only in T2DM, and smoking behaviour emerged only in COPD. Two themes were reported only in two diseases: adverse events in T2DM and COPD, and visits or contacts with healthcare professionals in obesity and COPD. The three perspectives (patients, informal caregivers, and healthcare professionals) were identified in five themes: (1) mortality in HF, (2) adherence to treatment in T2DM, and (3) interactions with healthcare professionals, (4) health knowledge, and (5) perceived benefit of the intervention in COPD and HF. In contrast, for obesity, we did not identify themes exploring the perspectives of informal caregivers.
Identified themes by disease and perspective. Coloured cells are themes (rows) in a specific disease (columns) with available data. White cells represent the absence of data for a particular theme/disease. The included perspectives were obtained from patients (



3.4 Outcomes and Modifiable Factors of Self-Management Interventions
In principle, most of the themes and subthemes identified can be measured and represent potential outcomes of SM interventions (e.g., adherence to treatment). Other themes are more likely to be considered modifiable barriers or facilitators (e.g., access to healthcare). Finally, a third group can be conceived as both outcomes and modifiable factors since some SM interventions are also aimed at improving these factors (e.g., health knowledge) (Table 2).
4 Discussion
4.1 Main Findings
In this mixed-methods scoping review of reviews, we identified the most relevant themes from the perspectives of patients, informal caregivers, and healthcare professionals on the SM of chronic disease, based on 148 reviews exploring preferences and experiences. We identified 12 main themes, of which four described the process of SM (progression of the disease, SM behaviours, social support, interaction with healthcare providers), four referred to factors influencing the SM process (access to healthcare, costs for patients, culturally defined roles and perceptions, and health knowledge), and four were specific to experiences with SM interventions (the perceived benefit of the intervention, individualised care, sense of community and usability). Some themes included subthemes describing particular features (e.g., weight control in SM behaviours). Most themes were consistently identified across the four diseases, with only a few disease-specific themes. Regarding the population included, the three perspectives were recognised for five themes only, as perspectives of informal caregivers were not identified in obesity. We categorised the themes and subthemes in an illustrative list of SM intervention outcomes and/or modifiable factors that can be considered, for example, in the COS development process for these types of interventions.
Regarding the nature of findings, health state utility measures were reported and informed the following themes: disease progression (e.g., moderate and severe COPD exacerbations), fear of complications (e.g., painful diabetic polyneuropathy), adverse events (e.g., transient nausea), and weight control. Non-utility measures were reported narratively and summarised, with qualitative results reported in mixed-methods research synthesis and qualitative evidence synthesis. These findings were homogeneously distributed and informed all themes.
4.2 Our Findings in the Context of Previous Research
To our knowledge, this is the first mixed-methods scoping review of reviews exploring and summarising the preferences and experiences of patients and their caregivers with SM for the four selected chronic diseases. Other overviews that helped characterise the experiences or preferences of patients with other chronic diseases were diverse in length and depth of scope [177,178,179,180]. For example, whereas some focused only on SM interventions and included only qualitative evidence for specific conditions, such as stroke [179], rheumatic diseases, cancer, and fibromyalgia [177], others explored health utilities in oncology [178] or focused specifically on a particular aspect such as chronic non-malignant pain [180]. Themes describing the perceived support from family or friends, the perceived quality of care, and relationships with healthcare professionals from our scoping review were consistently identified in these overviews and recognised as important factors for SM in chronic diseases [177, 179, 180]. Pearce et al. [179] described the impact on stroke patients’ self-image and the varying needs for SM support across the condition trajectory. Likewise, our findings identified patients’ conflicted views regarding their diagnosis [39], the process of accepting a new identity [106], the progression of the disease and the burden of physical limitations [42, 153, 159, 165] or psychological distress [40, 41, 51, 54, 56, 59, 61, 74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98]. Toye et al. [180] described how patients with chronic pain tended to perceive their life as “impoverished and confined” and as being in a “constant battle against their body”. Similarly, our findings identified a risk of isolation for some patients because of the burden of symptoms [41, 50, 56, 74], the physical limitations as a consequence of disease progression [35, 42, 43, 49, 51, 52, 54, 55, 61, 72, 73] and complications [62, 63, 78, 102,103,104], and the impact of perceived or experienced stigma [37, 41, 81, 88, 89, 91, 100].
One overview of qualitative reviews also explored patients’ and caregivers’ experiences of care with chronic diseases and included two of our selected diseases (HF and COPD) [181]. Most of our themes resonated with their findings, especially those describing “the experience of SM” and “factors that influence SM.” They reported that patients’ and caregivers’ behaviours in chronic healthcare and decision-making processes were influenced by their characteristics, the type of patient–caregiver interaction, the healthcare system, and their resilience with challenging situations in the disease trajectory [181].
Our findings are aligned with some theoretical frameworks developed to explain chronic healthcare and guide behavioural interventions. The ‘common sense model of self-regulation of health and illness’ states that individuals form common-sense representations of illnesses that guide how patients cope with the disease’s challenges [182]. Across the four chronic diseases, our findings include some aspects of the five dimensions that determine illness representations [182]: (1) identity (e.g., patients with COPD described their disease as a “roller coaster experience” [42,43,44] and patients with T2DM had ambivalent feelings regarding the diagnosis [39]); (2) cause (e.g., patients with HF often had aetiology misconceptions or did not perceive breathlessness as an indication of worsening [53]); (3) timeline (e.g., in T2DM, COPD, and HF, patients and informal caregivers often recognised feeling a fear of worsening of symptoms and of dying prematurely and uncertainty about the future [36, 44, 56, 73, 75]); (4) consequences (e.g., some patients did not recognise the risk of complications and had pessimistic beliefs and negative perceptions [54, 60, 70, 78, 82, 149, 153, 159, 160]); and (5) controllability (e.g., patients and informal caregivers reported that it could be challenging to balance daily life activities with the treatment workload [41] or found barriers to understanding and adhering to treatment regimens [109]).
The variable and sometimes opposing views reported within patients’ and caregivers’ experiences with SM were also aligned with the “shifting perspectives model of chronic illness,” which states that living with a chronic disease is an ongoing and continually shifting process [183]. Patients’ perspectives of their disease reflect their needs and situations in a particular moment. Across the four chronic diseases, most patients recognised having limited knowledge [43, 49, 51, 54, 56, 59,60,61, 72,73,74, 78, 86, 93, 106, 109, 117, 118, 120, 128, 153, 157], with most reporting that they learned from their own experiences [41, 73, 92, 112, 123] or with the help of other stakeholders [41, 155, 161]. Throughout this process, patients and caregivers learned and developed SM behaviours [36, 144], such as help-seeking behaviour or adherence to treatment with different engagement stages. This process was particularly challenging since adherence to SM is complex; it refers not only to medicines but also mostly to lifestyle behaviours [40]. Patients and their caregivers need to learn to live with the disease, finding a balance between symptom burden [42, 43, 49, 51, 52, 55, 72, 73], the emotional distress of having a chronic disease [40, 41, 51, 54, 56, 59, 61, 74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98], and—in some cases—the stigma they perceive and experience [37, 41, 81, 88, 89, 91, 100].
Another model that could help to explain our findings is the ‘integrative model of behaviour prediction’ [184], which predicts that people act on their intentions when they have the necessary skills and when environmental factors do not impede behavioural performance. More specifically, this model describes that intention to perform a behaviour follows reasonably (but not necessarily rationally) from specific beliefs that patients hold about the behaviour. The factors that could influence the process of SM were repeatedly described across the four chronic diseases and included (1) access to healthcare, (2) cost for patients, (3) culturally defined roles and perceptions (more relevant in ethnic minorities), and (4) health knowledge, reported as limiting patients’ and caregivers’ capacity to engage in (or provide) adequate SM strategies. Moreover, the perceived benefit from or importance of the SM interventions might also be influenced by (1) physical activity barriers, (2) psychological barriers to SM uptake, and (3) technological (digital) literacy.
Finally, the ‘self-determination theory’ (macro-theory of human motivation, personality development, and well-being) suggests a set of primary and universal psychological needs, including autonomy, competence, and relatedness [185]. This theory outlines the process of self-regulation, describing how people internalise social values and extrinsic contingencies, thereby moving from controlled to autonomously motivated behaviours that align with personal values and goals [185]. Our findings reflect some mechanisms that patients use to change their behaviours, such as (1) competence (e.g., in COPD and HF, patients gain expertise about their body responses, which helps them adopt a regulatory role and adjust their lifestyle [41, 73, 92, 112]); (2) autonomy (e.g., in COPD, adjustments or behaviour modifications were sometimes driven by patients’ motivation to prevent exacerbation [45, 73, 74] and physical activity motivation was driven by the expected or experienced benefits [87, 124, 126, 132, 153]), and (3) relatedness (e.g., patients from ethnic minorities living in Western countries found SM recommendations challenging when they conflicted with their beliefs or traditions [54, 122, 130, 135, 138, 139]).
One consistent finding across the four chronic diseases was the perception that high-quality interactions between patients and healthcare professionals facilitated positive SM behaviours. Other reviews also highlighted that patients need their concerns, fears, and feelings to be acknowledged and integrated into the SM process [186, 187]. However, our findings reflect that the traditional didactic approach was still more frequently experienced by patients and informal caregivers than collaborative patient–provider interactions. Moreover, the quality of care was generally perceived to be insufficient or unsatisfactory, with several complaints reported (e.g., the lack of coordination of services or inadequate treatment provision).
In the context of the COMPAR-EU project, themes from this scoping review helped inform COS selection for the four chronic diseases. The COS development process included, as a first step, developing an initial list of outcomes derived mainly from systematic reviews of the effectiveness of SM interventions. In a second step, a panel of patients ranked the importance of outcomes through a two-round Delphi process. We designed four infographics based on the initial list of outcomes. We found corresponding related information in our scoping review, showing a summary of findings and associated graphics by each outcome. The results of the Delphi process and the infographics were sent to participants before the final consensus meeting for outcomes selection. During this meeting, the infographics were used as needed. The resulting COS and the information provided in the infographics are published elsewhere [188].
4.3 Strengths and Limitations
Our study has several strengths. The first was our broad eligibility criteria concerning the phenomena of interest and the design and methods of included studies. The scope of reviews ranged from the experience of diabetes management in general [57] to more specific topics, such as the use of telehealth in patients with diabetic foot ulcer [156]. Quantitative and qualitative findings helped to configure the impact of specific outcomes from the patient’s perspective. For example, utility estimates reported for dyspnoea and its progression showed an ascending effect consistent with its severity [46]. When explored through patients’ experiences, dyspnoea was the most prominent symptom in the “roller coaster” experience of having COPD [42, 44, 45]. Our methods included a sensitive search strategy using a filter designed explicitly for values and preferences studies [28], including additional terms related to qualitative methods to enhance the sensitivity of qualitative reviews. We also sought to describe and summarise themes related to the outcomes of SM interventions for four chronic diseases based on different stakeholder perspectives (patients, informal caregivers, and healthcare professionals), helping to better characterise experiences with SM. For example, informal caregivers described their experiences as challenging with a potentially negative impact on their quality of life [43, 44, 145,146,147], whereas patients recognised the caregiver’s role as fundamental for achieving SM goals [119, 120, 140].
Our mixed-methods scoping review of reviews also has some limitations. By including only reviews, we applied a relatively novel methodology [16]. By limiting our search to only English-language publications, we may have missed some studies in specific populations. The experience of codifying themes was methodologically challenging because of the diversity of synthesis and reporting methods used in the included reviews. However, despite this variability, the identified themes were generally consistent. For example, the influence of social networks, perceived social support, and marital status on self-care was identified in reviews that used quite different methods such as meta-ethnography [110], mixed-methods research synthesis [139], thematic analysis [60], or meta-aggregation [93]. Finally, screening and extraction processes were not conducted by two reviewers independently, and applying a descriptive approach for synthesis limited our ability to provide a more in-depth analysis [33].
4.4 Implications for Practice and Research
This mixed-methods scoping review identified a set of main themes that can guide policy makers, healthcare professionals, and patient organisations to outline the design of SM interventions tailored to the needs of the primary stakeholders. They can also help with the design of implementation strategies to support both patients and caregivers in specific areas of SM and healthcare, considering under-explored areas, such as the psychological distress faced by some healthcare professionals during the SM care process [81, 93, 152]. Since these themes represent relevant areas identified mainly from the patient’s perspective, our findings could also help select quality indicators to evaluate SM support programmes. Moreover, the selected themes may help to delineate other COS for related interventions or similar populations. Our findings will also inform the development of decision-making tools for the COMPAR-EU project [7], including evidence for decision frameworks to develop recommendations and decision aids.
Further research is needed in areas in which we found scarce evidence, including (1) an overall approach to address the views of healthcare professionals and informal caregivers regarding SM and (2) a more specific approach to explore the preferences and experiences of patients with obesity or caregivers’ perspectives in T2DM and obesity. In this mixed-methods scoping review, we identified the most relevant themes regarding SM from the perspectives of patients, informal caregivers, and healthcare professionals regarding the process of SM and SM interventions. In a second stage within COMPAR-EU, we are conducting four overviews (one per each chronic disease) to offer a more detailed and in-depth analysis, better characterising how the different populations value the importance of the different outcomes of SM interventions and identifying factors that potentially affect the acceptability and feasibility of SM interventions [189].
5 Conclusion
The process of SM shaped the perspectives of patients and their caregivers on SM interventions. Their perspectives were influenced by the perceived benefit of the intervention, the sense of community, the usability of the intervention, and the level of individualised care. Our findings can inform the selection of patient-important outcomes and decision-making processes, including the formulation of recommendations and the design and implementation of SM interventions.
Abbreviations
- COPD:
-
Chronic obstructive pulmonary disease
- COS:
-
Core outcome set
- HF:
-
Heart failure
- SM:
-
Self-management
- T2DM:
-
Type 2 diabetes mellitus
References
Bodenheimer T, Lorig K, Holman H, Grumbach K. Patient self-management of chronic disease in primary care. JAMA. 2002;288(19):2469–75. https://doi.org/10.1001/jama.288.19.2469.
Epping-Jordan JE, Pruitt SD, Bengoa R, Wagner EH. Improving the quality of health care for chronic conditions. Qual Saf Health Care. 2004;13(4):299–305. https://doi.org/10.1136/qhc.13.4.299.
Grady PA, Gough LL. Self-management: a comprehensive approach to management of chronic conditions. Am J Public Health. 2014;104(8):e25-31. https://doi.org/10.2105/AJPH.2014.302041.
Institute of Medicine. In: (US) NAP, editor. Priority areas for national action: transforming health care quality. Washington (DC). 2003.
Barlow J, Wright C, Sheasby J, Turner A, Hainsworth J. Self-management approaches for people with chronic conditions: a review. Patient Educ Couns. 2002;48(2):177–87. https://doi.org/10.1016/s0738-3991(02)00032-0.
Murphy LA, Harrington P, Taylor SJ, Teljeur C, Smith SM, Pinnock H, et al. Clinical-effectiveness of self-management interventions in chronic obstructive pulmonary disease: an overview of reviews. Chron Respir Dis. 2017;14(3):276–88. https://doi.org/10.1177/1479972316687208.
Ballester M, Orrego C, Heijmans M, Alonso-Coello P, Versteegh MM, Mavridis D, et al. Comparing the effectiveness and cost-effectiveness of self-management interventions in four high-priority chronic conditions in Europe (COMPAR-EU): a research protocol. BMJ Open. 2020;10(1):e034680. https://doi.org/10.1136/bmjopen-2019-034680.
Williamson PR, Altman DG, Blazeby JM, Clarke M, Devane D, Gargon E, et al. Developing core outcome sets for clinical trials: issues to consider. Trials. 2012;13:132. https://doi.org/10.1186/1745-6215-13-132.
Young B, Bagley H. Including patients in core outcome set development: issues to consider based on three workshops with around 100 international delegates. Res Involv Engagem. 2016;2:25. https://doi.org/10.1186/s40900-016-0039-6.
FDA Guidance Patient Preference Information—voluntary submission, review in premarket approval applications, humanitarian device exemption applications, and de novo requests, and inclusion in decision summaries and device labeling. FDA. 2016.
Rand L, Dunn M, Slade I, Upadhyaya S, Sheehan M. Understanding and using patient experiences as evidence in healthcare priority setting. Cost Eff Resour Alloc. 2019;17:20. https://doi.org/10.1186/s12962-019-0188-1.
Lewin S, Booth A, Glenton C, Munthe-Kaas H, Rashidian A, Wainwright M, et al. Applying GRADE-CERQual to qualitative evidence synthesis findings: introduction to the series. Implement Sci. 2018;13(Suppl 1):2. https://doi.org/10.1186/s13012-017-0688-3.
Noyes J, Booth A, Flemming K, Garside R, Harden A, Lewin S, et al. Cochrane Qualitative and Implementation Methods Group guidance series-paper 3: methods for assessing methodological limitations, data extraction and synthesis, and confidence in synthesized qualitative findings. J Clin Epidemiol. 2018;97:49–58. https://doi.org/10.1016/j.jclinepi.2017.06.020.
Yu T, Enkh-Amgalan N, Zorigt G. Methods to perform systematic reviews of patient preferences: a literature survey. BMC Med Res Methodol. 2017;17(1):166. https://doi.org/10.1186/s12874-017-0448-8.
Munn Z, Peters MDJ, Stern C, Tufanaru C, McArthur A, Aromataris E. Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med Res Methodol. 2018;18(1):143. https://doi.org/10.1186/s12874-018-0611-x.
Schultz A, Goertzen L, Rothney J, Wener P, Enns J, Halas G, et al. A scoping approach to systematically review published reviews: adaptations and recommendations. Res Synth Methods. 2018;9(1):116–23. https://doi.org/10.1002/jrsm.1272.
Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32.
Noyes J, Booth A, Moore G, Flemming K, Tuncalp O, Shakibazadeh E. Synthesising quantitative and qualitative evidence to inform guidelines on complex interventions: clarifying the purposes, designs and outlining some methods. BMJ Glob Health. 2019;4(Suppl 1):e000893. https://doi.org/10.1136/bmjgh-2018-000893.
Peters M GC, McInerney P, Baldini Soares C, Khalil H, Parker D. Reviewer's manual: the Joanna Briggs Institute. In: Institute JB, editor. 2017.
Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467–73. https://doi.org/10.7326/M18-0850.
Schulman-Green D, Jaser S, Martin F, Alonzo A, Grey M, McCorkle R, et al. Processes of self-management in chronic illness. J Nurs Scholarsh. 2012;44(2):136–44. https://doi.org/10.1111/j.1547-5069.2012.01444.x.
Andrews J, Guyatt G, Oxman AD, Alderson P, Dahm P, Falck-Ytter Y, et al. GRADE guidelines: 14. Going from evidence to recommendations: the significance and presentation of recommendations. J Clin Epidemiol. 2013;66(7):719-25. https://doi.org/10.1016/j.jclinepi.2012.03.013.
Zhang Y, Coello PA, Brozek J, Wiercioch W, Etxeandia-Ikobaltzeta I, Akl EA, et al. Using patient values and preferences to inform the importance of health outcomes in practice guideline development following the GRADE approach. Health Qual Life Outcomes. 2017;15(1):52. https://doi.org/10.1186/s12955-017-0621-0.
Zhang Y, Alonso-Coello P, Guyatt GH, Yepes-Nunez JJ, Akl EA, Hazlewood G, et al. GRADE guidelines: 19. Assessing the certainty of evidence in the importance of outcomes or values and preferences—risk of bias and indirectness. J Clin Epidemiol. 2019;111:94–104. https://doi.org/10.1016/j.jclinepi.2018.01.013.
Hunink MGMWM, Wittenberg E, Drummond MF, Pliskin JS, Wong JB, et al. Decision making in health and medicine: integrating evidence and values. 2nd ed. Cambridge: Cambridge University Press; 2014.
Torrance GW. Utility approach to measuring health-related quality of life. J Chronic Dis. 1987;40(6):593–603. https://doi.org/10.1016/0021-9681(87)90019-1.
Wright K, Golder S, Lewis-Light K. What value is the CINAHL database when searching for systematic reviews of qualitative studies? Syst Rev. 2015;4:104. https://doi.org/10.1186/s13643-015-0069-4.
Selva A, Sola I, Zhang Y, Pardo-Hernandez H, Haynes RB, Martinez Garcia L, et al. Development and use of a content search strategy for retrieving studies on patients’ views and preferences. Health Qual Life Outcomes. 2017;15(1):126. https://doi.org/10.1186/s12955-017-0698-5.
Search strategy used to create the pubmed systematic reviews filter. https://www.nlm.nih.gov/bsd/pubmed_subsets/sysreviews_strategy.html. Accessed 8 Jan 2021.
Campbell R, Pound P, Morgan M, Daker-White G, Britten N, Pill R, et al. Evaluating meta-ethnography: systematic analysis and synthesis of qualitative research. Health Technol Assess. 2011;15(43):1–164. https://doi.org/10.3310/hta15430.
Flemming K, Booth A, Garside R, Tuncalp O, Noyes J. Qualitative evidence synthesis for complex interventions and guideline development: clarification of the purpose, designs and relevant methods. BMJ Glob Health. 2019;4(Suppl 1):e000882. https://doi.org/10.1136/bmjgh-2018-000882.
Sandelowski M, Voils CI, Barroso J. Defining and designing mixed research synthesis studies. Res Sch. 2006;13(1):29.
Thomas J, Harden A. Methods for the thematic synthesis of qualitative research in systematic reviews. BMC Medical Research Methodology. 2008;8(1):45. doi:https://doi.org/10.1186/1471-2288-8-45.35.
Gorst SL, Armitage CJ, Brownsell S, Hawley MS. Home telehealth uptake and continued use among heart failure and chronic obstructive pulmonary disease patients: a systematic review. Ann Behav Med. 2014;48(3):323–36. https://doi.org/10.1007/s12160-014-9607-x.
Jaime-Lara RB, Koons BC, Matura LA, Hodgson NA, Riegel B. A qualitative metasynthesis of the experience of fatigue across five chronic conditions. J Pain Symptom Manag. 2020;59(6):1320–43. https://doi.org/10.1016/j.jpainsymman.2019.12.358.
Noonan MC, Wingham J, Taylor RS. “Who Cares?” The experiences of caregivers of adults living with heart failure, chronic obstructive pulmonary disease and coronary artery disease: a mixed methods systematic review. BMJ Open. 2018;8(7):e020927. https://doi.org/10.1136/bmjopen-2017-020927.
Rai SS, Syurina EV, Peters RMH, Putri AI, Zweekhorst MBM. Non-communicable diseases-related stigma: a mixed-methods systematic review. Int J Environ Res Public Health. 2020. https://doi.org/10.3390/ijerph17186657.
Walker RC, Tong A, Howard K, Palmer SC. Patient expectations and experiences of remote monitoring for chronic diseases: systematic review and thematic synthesis of qualitative studies. Int J Med Inform. 2019;124:78–85. https://doi.org/10.1016/j.ijmedinf.2019.01.013.
Inga-Britt L, Kerstin B. Challenges faced in daily life by persons with type 2 diabetes: a meta-synthesis. Chronic Illn. 2018. https://doi.org/10.1177/1742395318757852.
Psarou A, Cooper H, Wilding JPH. Patients’ perspectives of oral and injectable type 2 diabetes medicines, their body weight and medicine-taking behavior in the UK: a systematic review and meta-ethnography. Diabetes Ther. 2018;9(5):1791–810. https://doi.org/10.1007/s13300-018-0490-5.
Lippiett KA, Richardson A, Myall M, Cummings A, May CR. Patients and informal caregivers’ experiences of burden of treatment in lung cancer and chronic obstructive pulmonary disease (COPD): a systematic review and synthesis of qualitative research. BMJ Open. 2019;9(2):e020515. https://doi.org/10.1136/bmjopen-2017-020515.
Disler RT, Green A, Luckett T, Newton PJ, Inglis S, Currow DC, et al. Experience of advanced chronic obstructive pulmonary disease: metasynthesis of qualitative research. J Pain Symptom Manag. 2014;48(6):1182–99. https://doi.org/10.1016/j.jpainsymman.2014.03.009.
Giacomini M, DeJean D, Simeonov D, Smith A. Experiences of living and dying with COPD: a systematic review and synthesis of the qualitative empirical literature. Ont Health Technol Assess Ser. 2012;12(13):1–47.
Gysels M, Bausewein C, Higginson IJ. Experiences of breathlessness: a systematic review of the qualitative literature. Palliat Support Care. 2007;5(3):281–302.
Harrison SL, Apps L, Singh SJ, Steiner MC, Morgan MD, Robertson N. ’Consumed by breathing’—a critical interpretive meta-synthesis of the qualitative literature. Chronic Illn. 2014;10(1):31–49. https://doi.org/10.1177/1742395313493122.
Zhang Y, Morgan RL, Alonso-Coello P, Wiercioch W, Bała MM, Jaeschke RR, et al. A systematic review of how patients value COPD outcomes. Eur Respir J. 2018. https://doi.org/10.1183/13993003.00222-2018.
Kirkpatrick P, Wilson E, Wimpenny P. Support for older people with COPD in community settings: a systematic review of qualitative research. JBI Libr Syst Rev. 2012;10(57):3649–763. https://doi.org/10.11124/01938924-201210570-00001.
Clark AM, Savard LA, Spaling MA, Heath S, Duncan AS, Spiers JA. Understanding help-seeking decisions in people with heart failure: a qualitative systematic review. Int J Nurs Stud. 2012;49(12):1582–97. https://doi.org/10.1016/j.ijnurstu.2012.05.010.
Falk H, Ekman I, Anderson R, Fu M, Granger B. Older patients’ experiences of heart failure-an integrative literature review. J Nurs Scholarsh. 2013;45(3):247–55. https://doi.org/10.1111/jnu.12025.
Hopp FP, Thornton N, Martin L. The lived experience of heart failure at the end of life: a systematic literature review. Health Soc Work. 2010;35(2):109–17.
Olano-Lizarraga M, Oroviogoicoechea C, Errasti-Ibarrondo B, Saracibar-Razquin M. The personal experience of living with chronic heart failure: a qualitative meta-synthesis of the literature. J Clin Nurs. 2016;25(17–18):2413–29. https://doi.org/10.1111/jocn.13285.
Yu DS, Lee DT, Kwong AN, Thompson DR, Woo J. Living with chronic heart failure: a review of qualitative studies of older people. J Adv Nurs. 2008;61(5):474–83. https://doi.org/10.1111/j.1365-2648.2007.04553.x.
Walthall H, Floegel T. The lived experience of breathlessness for people diagnosed with heart failure: a qualitative synthesis of the literature. Curr Opin Support Palliat Care. 2019;13(1):18–23. https://doi.org/10.1097/spc.0000000000000405.
Schulman-Green D, Jaser SS, Park C, Whittemore R. A metasynthesis of factors affecting self-management of chronic illness. J Adv Nurs. 2016;72(7):1469–89. https://doi.org/10.1111/jan.12902.
Bhattarai B, Walpola R, Mey A, Anoopkumar-Dukie S, Khan S. Barriers and strategies for improving medication adherence among people living with COPD: a systematic review. Respir Care. 2020;65(11):1738–50. https://doi.org/10.4187/respcare.07355.
Jeon YH, Kraus SG, Jowsey T, Glasgow NJ. The experience of living with chronic heart failure: a narrative review of qualitative studies. BMC Health Serv Res. 2010;10:77. https://doi.org/10.1186/1472-6963-10-77.
Nam S, Chesla C, Stotts NA, Kroon L, Janson SL. Barriers to diabetes management: patient and provider factors. Diabetes Res Clin Pract. 2011;93(1):1–9 (S0168-8227(11)00051-9).
Graven LJGJ, Vance DE, Pryor ER, Grubbs L, Karioth S. Coping styles associated with heart failure outcomes: a systematic review. J Nurs Educ Pract. 2014;4(2):227–42.
Ivynian SE, DiGiacomo M, Newton PJ. Care-seeking decisions for worsening symptoms in heart failure: a qualitative metasynthesis. Heart Fail Rev. 2015;20(6):655–71. https://doi.org/10.1007/s10741-015-9511-x.
Matricciani L, Jones S. Who cares about foot care? Barriers and enablers of foot self-care practices among non-institutionalized older adults diagnosed with diabetes: an integrative review. Diabetes Educ. 2015;41(1):106–17 (0145721714560441).
McIntosh T, Hunter DJ, Royce S. Barriers to physical activity in obese adults: a rapid evidence assessment. J Res Nurs. 2016;21(4):271–87. https://doi.org/10.1177/1744987116647762.
Beaudet A, Clegg J, Thuresson PO, Lloyd A, McEwan P. Review of utility values for economic modeling in type 2 diabetes. Value Health. 2014;17(4):462–70 (S1098-3015(14)00054-0).
Lung TW, Hayes AJ, Hayen A, Farmer A, Clarke PM. A meta-analysis of health state valuations for people with diabetes: explaining the variation across methods and implications for economic evaluation. Qual Life Res. 2011;20(10):1669–78. https://doi.org/10.1007/s11136-011-9902-y.
Doyle S, Lloyd A, Moore L, Ray J, Gray A. A systematic review and critical assessment of health state utilities: weight change and type 2 diabetes mellitus. Pharmacoeconomics. 2012;30(12):1133–43. https://doi.org/10.2165/11599420-000000000-00000.
Einarson TR, Bereza BG, Nielsen TA, Hemels ME. Utilities for asthma and COPD according to category of severity: a comprehensive literature review. J Med Econ. 2015;18(7):550–63. https://doi.org/10.3111/13696998.2015.1025793.
Moayeri F, Hsueh Y-S, Clarke P, Dunt D. Do model-based studies in chronic obstructive pulmonary disease measure correct values of utility? A meta-analysis. Value Health. 2016;19(4):363–73. https://doi.org/10.1016/j.jval.2016.01.012.
Dretzke J, Blissett D, Dave C, Mukherjee R, Price M, Bayliss S, et al. The cost-effectiveness of domiciliary non-invasive ventilation in patients with end-stage chronic obstructive pulmonary disease: a systematic review and economic evaluation. Health Technol Assess. 2015;19(81):1–246. https://doi.org/10.3310/hta19810.
Jordan RE, Majothi S, Heneghan NR, Blissett DB, Riley RD, Sitch AJ, et al. Supported self-management for patients with moderate to severe chronic obstructive pulmonary disease (COPD): an evidence synthesis and economic analysis. Health Technol Assess. 2015;19(36):1–516. https://doi.org/10.3310/hta19360.
Blieden Betts M, Gandra SR, Cheng LI, Szatkowski A, Toth PP. Differences in utility elicitation methods in cardiovascular disease: a systematic review. J Med Econ. 2018;21(1):74–84. https://doi.org/10.1080/13696998.2017.1379410.
Dyer MT, Goldsmith KA, Sharples LS, Buxton MJ. A review of health utilities using the EQ-5D in studies of cardiovascular disease. Health Qual Life Outcomes. 2010;8:13. https://doi.org/10.1186/1477-7525-8-13.
Stevanovic J, Pechlivanoglou P, Kampinga MA, Krabbe PF, Postma MJ. Multivariate meta-analysis of preference-based quality of life values in coronary heart disease. PLoS ONE. 2016;11(3):e0152030. https://doi.org/10.1371/journal.pone.0152030.
Clari M, Ivziku D, Casciaro R, Matarese M. The unmet needs of people with chronic obstructive pulmonary disease: a systematic review of qualitative findings. COPD. 2018;15(1):79–88. https://doi.org/10.1080/15412555.2017.1417373.
Russell S, Ogunbayo OJ, Newham JJ, Heslop-Marshall K, Netts P, Hanratty B, et al. Qualitative systematic review of barriers and facilitators to self-management of chronic obstructive pulmonary disease: views of patients and healthcare professionals. NPJ Prim Care Respir Med. 2018;28(1):2. https://doi.org/10.1038/s41533-017-0069-z.
Clari M, Matarese M, Ivziku D, Marinis M. Self-care of people with chronic obstructive pulmonary disease: a meta-synthesis. Patient. 2017;10(4):407–27. https://doi.org/10.1007/s40271-017-0218-z.
Gorst SL, Young B, Williamson PR, Wilding JPH, Harman NL. Incorporating patients’ perspectives into the initial stages of core outcome set development: a rapid review of qualitative studies of type 2 diabetes. BMJ Open Diabetes Res Care. 2019;7(1):e000615. https://doi.org/10.1136/bmjdrc-2018-000615.
Brod M, Kongso JH, Lessard S, Christensen TL. Psychological insulin resistance: patient beliefs and implications for diabetes management. Qual Life Res. 2009;18(1):23–32. https://doi.org/10.1007/s11136-008-9419-1.
Chen CM, Chang YM. The experiences of diabetics on self-monitoring of blood glucose: a qualitative metasynthesis. J Clin Nurs. 2015;24(5–6):614–26. https://doi.org/10.1111/jocn.12691.
Coffey L, Mahon C, Gallagher P. Perceptions and experiences of diabetic foot ulceration and foot care in people with diabetes: a qualitative meta-synthesis. Int Wound J. 2019;16(1):183–210. https://doi.org/10.1111/iwj.13010.
Ellis K, Mulnier H, Forbes A. Perceptions of insulin use in type 2 diabetes in primary care: a thematic synthesis. BMC Fam Pract. 2018;19(1):70. https://doi.org/10.1186/s12875-018-0753-2.
Ho AY, Berggren I, Dahlborg-Lyckhage E. Diabetes empowerment related to Pender’s Health Promotion Model: a meta-synthesis. Nurs Health Sci. 2010;12(2):259–67 (NHS517).
Henderson E. Obesity in primary care: a qualitative synthesis of patient and practitioner perspectives on roles and responsibilities. Br J Gen Pract. 2015;65(633):e240–7. https://doi.org/10.3399/bjgp15X684397.
Horigan G, Davies M, Findlay-White F, Chaney D, Coates V. Reasons why patients referred to diabetes education programmes choose not to attend: a systematic review. Diabet Med. 2017;34(1):14–26. https://doi.org/10.1111/dme.13120.
Jones V, Crowe M. How people from ethnic minorities describe their experiences of managing type-2 diabetes mellitus: a qualitative meta-synthesis. Int J Nurs Stud. 2017;76:78–91 (S0020-7489(17)30196-7).
Kaptein AA, Scharloo M, Fischer MJ, Snoei L, Cameron LD, Sont JK, et al. Illness perceptions and COPD: an emerging field for COPD patient management. J Asthma. 2008;45(8):625–9. https://doi.org/10.1080/02770900802127048.
Li J, Drury V, Taylor B. A systematic review of the experience of older women living and coping with type 2 diabetes. Int J Nurs Pract. 2014;20(2):126–34. https://doi.org/10.1111/ijn.12135.
Low J, Pattenden J, Candy B, Beattie JM, Jones L. Palliative care in advanced heart failure: an international review of the perspectives of recipients and health professionals on care provision. J Card Fail. 2011;17(3):231–52. https://doi.org/10.1016/j.cardfail.2010.10.003.
Lyzwinski LN, Caffery LJ, Bambling M, Edirippulige S. Consumer perspectives on mHealth for weight loss: a review of qualitative studies. J Telemed Telecare. 2017. https://doi.org/10.1177/1357633x17692722.
Malterud K, Ulriksen K. Obesity, stigma, and responsibility in health care: a synthesis of qualitative studies. Int J Qual Stud Health Well-Being. 2011. https://doi.org/10.3402/qhw.v6i4.8404.
Mold F, Forbes A. Patients’ and professionals’ experiences and perspectives of obesity in health-care settings: a synthesis of current research. Health Expect. 2013;16(2):119–42. https://doi.org/10.1111/j.1369-7625.2011.00699.x.
Ohsiek S, Williams M. Psychological factors influencing weight loss maintenance: an integrative literature review. J Am Acad Nurse Pract. 2011;23(11):592–601. https://doi.org/10.1111/j.1745-7599.2011.00647.x.
Rose S, Paul C, Boyes A, Kelly B, Roach D. Stigma-related experiences in non-communicable respiratory diseases: a systematic review. Chron Respir Dis. 2017;14(3):199–216. https://doi.org/10.1177/1479972316680847.
Ru TZ, Associate A, Hegney DG. A qualitative systematic review on the experiences of self-management in community-dwelling older women living with chronic illnesses. JBI Libr Syst Rev. 2011;9(62):2778–828. https://doi.org/10.11124/01938924-201109620-00001.
Rushforth B, McCrorie C, Glidewell L, Midgley E, Foy R. Barriers to effective management of type 2 diabetes in primary care: qualitative systematic review. Br J Gen Pract. 2016;66(643):e114–27 (66/643/e114).
Spenceley SM, Williams BA. Self-care from the perspective of people living with diabetes. Can J Nurs Res. 2006;38(3):124–45.
Stiffler D, Cullen D, Luna G. Diabetes barriers and self-care management: the patient perspective. Clin Nurs Res. 2014;23(6):601–26 (1054773813507948).
Suglo JN, Evans C. Factors influencing self-management in relation to type 2 diabetes in Africa: a qualitative systematic review. PLoS ONE. 2020;15(10):e0240938. https://doi.org/10.1371/journal.pone.0240938.
Tierney S, Mamas M, Skelton D, Woods S, Rutter MK, Gibson M, et al. What can we learn from patients with heart failure about exercise adherence? A systematic review of qualitative papers. Health Psychol. 2011;30(4):401–10. https://doi.org/10.1037/a0022848.
Wilkinson A, Whitehead L, Ritchie L. Factors influencing the ability to self-manage diabetes for adults living with type 1 or 2 diabetes. Int J Nurs Stud. 2014;51(1):111–22. https://doi.org/10.1016/j.ijnurstu.2013.01.006.
Franklin M, Lewis S, Willis K, Bourke-Taylor H, Smith L. Patients’ and healthcare professionals’ perceptions of self-management support interactions: Systematic review and qualitative synthesis. Chronic Illn. 2018;14(2):79–103. https://doi.org/10.1177/1742395317710082.
Papadopoulos S, Brennan L. Correlates of weight stigma in adults with overweight and obesity: a systematic literature review. Obesity (19307381). 2015;23(9):1743–60. https://doi.org/10.1002/oby.21187.
Valencia WM, Florez HJ, Palacio AM. Suitable use of injectable agents to overcome hypoglycemia risk, barriers, and clinical inertia in community-dwelling older adults with type 2 diabetes mellitus. Drugs Aging. 2019;36(12):1083–96. https://doi.org/10.1007/s40266-019-00706-4.
Alleman CJ, Westerhout KY, Hensen M, Chambers C, Stoker M, Long S, et al. Humanistic and economic burden of painful diabetic peripheral neuropathy in Europe: a review of the literature. Diabetes Res Clin Pract. 2015;109(2):215–25 (S0168-8227(15)00229-6).
Kennedy-Martin T, Paczkowski R, Rayner S. Utility values in diabetic kidney disease: a literature review. Curr Med Res Opin. 2015;31(7):1271–82. https://doi.org/10.1185/03007995.2015.1041895.
Poku E, Brazier J, Carlton J, Ferreira A. Health state utilities in patients with diabetic retinopathy, diabetic macular oedema and age-related macular degeneration: a systematic review. BMC Ophthalmol. 2013;13:74 (1471-2415-13-74).
von Arx LB, Kjeer T. The patient perspective of diabetes care: a systematic review of stated preference research. Patient. 2014;7(3):283–300. https://doi.org/10.1007/s40271-014-0057-0.
Pennbrant S, Berg A, Fohlin JL. Self-care experiences of older patients with diabetes mellitus: a qualitative systematic literature review. Nordic J Nurs Res. 2020;40(2):64–72. https://doi.org/10.1177/2057158519868803.
Tan P, Chen HC, Taylor B, Hegney D. Experience of hypoglycaemia and strategies used for its management by community-dwelling adults with diabetes mellitus: a systematic review. Int J Evid Based Healthc. 2012;10(3):169–80. https://doi.org/10.1111/j.1744-1609.2012.00276.x.
Barclay S, Momen N, Case-Upton S, Kuhn I, Smith E. End-of-life care conversations with heart failure patients: a systematic literature review and narrative synthesis. Br J Gen Pract. 2011;61(582):e49-62. https://doi.org/10.3399/bjgp11X549018.
Wingham J, Harding G, Britten N, Dalal H. Heart failure patients’ attitudes, beliefs, expectations and experiences of self-management strategies: a qualitative synthesis. Chronic Illn. 2014;10(2):135–54. https://doi.org/10.1177/1742395313502993.
Foss C, Knutsen I, Kennedy A, Todorova E, Wensing M, Lionis C, et al. Connectivity, contest and the ties of self-management support for type 2 diabetes: a meta-synthesis of qualitative literature. Health Soc Care Community. 2016;24(6):672–86. https://doi.org/10.1111/hsc.12272.
Madsen KP, Kjaer T, Skinner T, Willaing I. Time preferences, diabetes self-management behaviours and outcomes: a systematic review. Diabet Med. 2019;36(11):1336–48. https://doi.org/10.1111/dme.14102.
Daley C, Al-Abdulmunem M, Holden RJ. Knowledge among patients with heart failure: a narrative synthesis of qualitative research. Heart Lung. 2019;48(6):477–85. https://doi.org/10.1016/j.hrtlng.2019.05.012.
Brunton L, Bower P, Sanders C. The contradictions of telehealth user experience in chronic obstructive pulmonary disease (COPD): a qualitative meta-synthesis. PLoS ONE. 2015;10(10):e0139561. https://doi.org/10.1371/journal.pone.0139561.
Lindenmeyer A, Greenfield SM, Greenfield C, Jolly K. How do people with COPD value different activities? an adapted meta-ethnography of qualitative research. Qual Health Res. 2017;27(1):37–50. https://doi.org/10.1177/1049732316644430.
Harkness K, Spaling MA, Currie K, Strachan PH, Clark AM. A systematic review of patient heart failure self-care strategies. J Cardiovasc Nurs. 2015;30(2):121–35. https://doi.org/10.1097/JCN.0000000000000118.
Kane PM, Murtagh FE, Ryan K, Mahon NG, McAdam B, McQuillan R, et al. The gap between policy and practice: a systematic review of patient-centred care interventions in chronic heart failure. Heart Fail Rev. 2015;20(6):673–87. https://doi.org/10.1007/s10741-015-9508-5.
Clark AM, Spaling M, Harkness K, Spiers J, Strachan PH, Thompson DR, et al. Determinants of effective heart failure self-care: a systematic review of patients’ and caregivers’ perceptions. Heart (British Cardiac Society). 2014;100(9):716–21. https://doi.org/10.1136/heartjnl-2013-304852.
Karimi M, Clark AM. How do patients’ values influence heart failure self-care decision-making?: A mixed-methods systematic review. Int J Nurs Stud. 2016;59:89–104. https://doi.org/10.1016/j.ijnurstu.2016.03.010.
Li CC, Shun SC. Understanding self care coping styles in patients with chronic heart failure: a systematic review. Eur J Cardiovasc Nurs. 2016;15(1):12–9. https://doi.org/10.1177/1474515115572046.
Siabani S, Leeder SR, Davidson PM. Barriers and facilitators to self-care in chronic heart failure: a meta-synthesis of qualitative studies. Springerplus. 2013;2:320. https://doi.org/10.1186/2193-1801-2-320.
Brundisini F, Giacomini M, DeJean D, Vanstone M, Winsor S, Smith A. Chronic disease patients’ experiences with accessing health care in rural and remote areas: a systematic review and qualitative meta-synthesis. Ont Health Technol Assess Ser. 2013;13(15):1–33.
Fleming E, Gillibrand W. An exploration of culture, diabetes, and nursing in the South Asian community: a metasynthesis of qualitative studies. J Transcult Nurs. 2009;20(2):146–55 (1043659608330058).
Sibounheuang P, Olson PS, Kittiboonyakun P. Patients’ and healthcare providers’ perspectives on diabetes management: a systematic review of qualitative studies. Res Social Admin Pharm. 2020;16(7):854–74. https://doi.org/10.1016/j.sapharm.2019.09.001.
Archibald D, Douglas F, Hoddinott P. A qualitative evidence synthesis on the management of male. Obesity. 2015;5(10):e008372. https://doi.org/10.1136/bmjopen-2015-008372.
Garip G, Yardley L. A synthesis of qualitative research on overweight and obese people’s views and experiences of weight management. Clin Obes. 2011;1(2–3):110–26. https://doi.org/10.1111/j.1758-8111.2011.00021.x.
Harper C, Maher J, Grunseit A, Seimon RV, Sainsbury A. Experiences of using very low energy diets for weight loss by people with overweight or obesity: a review of qualitative research. Obes Rev. 2018;19(10):1412–23. https://doi.org/10.1111/obr.12715.
Chan A. An integrative review: adherence barriers to a low-salt diet in culturally diverse heart failure adults. Aust J Adv Nurs. 2018;36(1):37–47.
Currie K, Strachan PH, Spaling M, Harkness K, Barber D, Clark AM. The importance of interactions between patients and healthcare professionals for heart failure self-care: a systematic review of qualitative research into patient perspectives. Eur J Cardiovasc Nurs. 2015;14(6):525–35. https://doi.org/10.1177/1474515114547648.
Purnell TS, Joy S, Little E, Bridges JF, Maruthur N. Patient preferences for noninsulin diabetes medications: a systematic review. Diabetes Care. 2014;37(7):2055–62. https://doi.org/10.2337/dc13-2527.
Ellis K, Mulnier H, Forbes A. Perceptions of insulin use in type 2 diabetes in primary care: a thematic synthesis. BMC Fam Pract. 2018;19(1):N.PAG-N.PAG. https://doi.org/10.1186/s12875-018-0753-2.
Ng CJ, Lai PS, Lee YK, Azmi SA, Teo CH. Barriers and facilitators to starting insulin in patients with type 2 diabetes: a systematic review. Int J Clin Pract. 2015;69(10):1050–70. https://doi.org/10.1111/ijcp.12691.
Baker E, Fatoye F. Patient perceived impact of nurse-led self-management interventions for COPD: a systematic review of qualitative research. Int J Nurs Stud. 2019;91:22–34. https://doi.org/10.1016/j.ijnurstu.2018.12.004.
Toroski M, Kebriaeezadeh A, Esteghamati A, Karyani AK, Abbasian H, Nikfar S. Patient and physician preferences for type 2 diabetes medications: a systematic review. J Diabetes Metab Disord. 2019;18(2):643–56. https://doi.org/10.1007/s40200-019-00449-4.
Hartmann-Boyce J, Boylan A-M, Jebb SA, Aveyard P. Experiences of self-monitoring in self-directed weight loss and weight loss maintenance: systematic review of qualitative studies. Qual Health Res. 2019;29(1):124–34. https://doi.org/10.1177/1049732318784815.
Albanese AM, Huffman JC, Celano CM, Malloy LM, Wexler DJ, Freedman ME, et al. The role of spousal support for dietary adherence among type 2 diabetes patients: a narrative review. Soc Work Health Care. 2019;58(3):304–23. https://doi.org/10.1080/00981389.2018.1563846.
Galdas PM, Ratner PA, Oliffe JL. A narrative review of South Asian patients’ experiences of cardiac rehabilitation. J Clin Nurs. 2012;21(1–2):149–59. https://doi.org/10.1111/j.1365-2702.2011.03754.x.
Grace SL, Racco C, Chessex C, Rivera T, Oh P. A narrative review on women and cardiac rehabilitation: program adherence and preferences for alternative models of care. Maturitas. 2010;67(3):203–8. https://doi.org/10.1016/j.maturitas.2010.07.001.
Li-Geng T, Kilham J, McLeod KM. Cultural influences on dietary self-management of type 2 diabetes in East Asian Americans: a mixed-methods systematic review. Health Equity. 2020;4(1):31–42. https://doi.org/10.1089/heq.2019.0087.
Majeed-Ariss R, Jackson C, Knapp P, Cheater FM. A systematic review of research into black and ethnic minority patients’ views on self-management of type 2 diabetes. Health Expect. 2015;18(5):625–42. https://doi.org/10.1111/hex.12080.
Strachan PH, Currie K, Harkness K, Spaling M, Clark AM. Context matters in heart failure self-care: a qualitative systematic review. J Card Fail. 2014;20(6):448–55. https://doi.org/10.1016/j.cardfail.2014.03.010.
Vongmany J, Luckett T, Lam L, Phillips JL. Family behaviours that have an impact on the self-management activities of adults living with Type 2 diabetes: a systematic review and meta-synthesis. Diabet Med. 2018;35(2):184–94. https://doi.org/10.1111/dme.13547.
Brown I, Gould J. Decisions about weight management: a synthesis of qualitative studies of obesity. Clin Obes. 2011;1(2–3):99–109. https://doi.org/10.1111/j.1758-8111.2011.00020.x.
Grant JS, Graven LJ. Problems experienced by informal caregivers of individuals with heart failure: an integrative review. Int J Nurs Stud. 2018;80:41–66. https://doi.org/10.1016/j.ijnurstu.2017.12.016.
Kim EY, Oh S, Son Y-J. Caring experiences of family caregivers of patients with heart failure: a meta-ethnographic review of the past 10 years. Eur J Cardiovasc Nurs. 2020;19(6):473–85. https://doi.org/10.1177/1474515120915040.
Rosa F, Bagnasco A, Aleo G, Kendall S, Sasso L. Resilience as a concept for understanding family caregiving of adults with Chronic Obstructive Pulmonary Disease (COPD): an integrative review. Nurs Open. 2017;4(2):61–75. https://doi.org/10.1002/nop2.63.
Kang X, Li Z, Nolan MT. Informal caregivers’ experiences of caring for patients with chronic heart failure: systematic review and metasynthesis of qualitative studies. J Cardiovasc Nurs. 2011;26(5):386–94. https://doi.org/10.1097/JCN.0b013e3182076a69.
Whittingham K, Barnes S, Gardiner C. Tools to measure quality of life and carer burden in informal carers of heart failure patients: a narrative review. Palliat Med. 2013;27(7):596–607. https://doi.org/10.1177/0269216313477179.
Kim K, Heinze K, Xu J, Kurtz M, Park H, Foradori M, et al. Theories of health care decision making at the end of life: a meta-ethnography. West J Nurs Res. 2018;40(12):1861–84. https://doi.org/10.1177/0193945917723010.
Peimani M, Nasli-Esfahani E, Sadeghi R. Patients’ perceptions of patient-provider communication and diabetes care: a systematic review of quantitative and qualitative studies. Chronic Illn. 2018. https://doi.org/10.1177/1742395318782378.
Frost J, Garside R, Cooper C, Britten N. A qualitative synthesis of diabetes self-management strategies for long term medical outcomes and quality of life in the UK. BMC Health Serv Res. 2014;14:348. (1472-6963-14-348).
Siltanen H, Jylhä V, Holopainen A, Paavilainen E. Family members’ experiences and expectations of self-management counseling while caring for a person with chronic obstructive pulmonary disease: a systematic review of qualitative evidence. JBI Database Syst Rev Implement Rep. 2019;17(11):2214–47. https://doi.org/10.11124/jbisrir-d-19-00056.
Dewhurst A, Peters S, Devereux-Fitzgerald A, Hart J. Physicians’ views and experiences of discussing weight management within routine clinical consultations: a thematic synthesis. Patient Educ Couns. 2017;100(5):897–908. https://doi.org/10.1016/j.pec.2016.12.017.
Miller MJ, Jones J, Anderson CB, Christiansen CL. Factors influencing participation in physical activity after dysvascular amputation: a qualitative meta-synthesis. Disabil Rehabil. 2019;41(26):3141–50. https://doi.org/10.1080/09638288.2018.1492031.
Moredich CA, Kessler TA. Physical activity and nutritional weight loss interventions in obese, low-income women: an integrative review. J Midwifery Womens Health. 2014;59(4):380–7. https://doi.org/10.1111/jmwh.12061.
O’Connell S, McCarthy VJ, Savage E. Self-management support preferences of people with asthma or chronic obstructive pulmonary disease: a systematic review and meta-synthesis of qualitative studies. Chronic Illn. 2019. https://doi.org/10.1177/1742395319869443.
Singh TP, Vangaveti VN, Kennedy RL, Malabu UH. Role of telehealth in diabetic foot ulcer management—a systematic review. Aust J Rural Health. 2016;24(4):224–9. https://doi.org/10.1111/ajr.12284.
Dickson VV, Riegel B. Are we teaching what patients need to know? Building skills in heart failure self-care. Heart Lung. 2009;38(3):253–61. https://doi.org/10.1016/j.hrtlng.2008.12.001.
Sohanpal R, Steed L, Mars T, Taylor SJ. Understanding patient participation behaviour in studies of COPD support programmes such as pulmonary rehabilitation and self-management: a qualitative synthesis with application of theory. NPJ Prim Care Respir Med. 2015;25:15054. https://doi.org/10.1038/npjpcrm.2015.54.
Sorensen SS, Weinreich UM, Ehlers L. Rationale and development of a patient-tailored complex intervention of case management for patients suffering from chronic obstructive pulmonary disease. Home Health Care Serv Q. 2017;36(3–4):178–95. https://doi.org/10.1080/01621424.2017.1393481.
Cooper AF, Jackson G, Weinman J, Horne R. Factors associated with cardiac rehabilitation attendance: a systematic review of the literature. Clin Rehabil. 2002;16(5):541–52. https://doi.org/10.1191/0269215502cr524oa.
Jain SR, Sui Y, Ng CH, Chen ZX, Goh LH, Shorey S. Patients’ and healthcare professionals’ perspectives towards technology-assisted diabetes self-management education. A qualitative systematic review. PLoS ONE. 2020;15(8):e0237647. https://doi.org/10.1371/journal.pone.0237647.
de Sousa Pinto JM, Martin-Nogueras AM, Morano MT, Macedo TE, Arenillas JI, Troosters T. Chronic obstructive pulmonary disease patients’ experience with pulmonary rehabilitation: a systematic review of qualitative research. Chron Respir Dis. 2013;10(3):141–57. https://doi.org/10.1177/1479972313493796.
Woo K, Dowding D. Factors affecting the acceptance of telehealth services by heart failure patients: an integrative review. Telemed e-Health. 2018;24(4):292–300. https://doi.org/10.1089/tmj.2017.0080.
Alvarado MM, Kum HC, Gonzalez Coronado K, Foster MJ, Ortega P, Lawley MA. Barriers to remote health interventions for type 2 diabetes: a systematic review and proposed classification scheme. J Med Internet Res. 2017;19(2):e28. https://doi.org/10.2196/jmir.6382.
Keating A, Lee A, Holland AE. What prevents people with chronic obstructive pulmonary disease from attending pulmonary rehabilitation? A systematic review. Chronic Respir Dis. 2011;8(2):89–99. https://doi.org/10.1177/1479972310393756.
Cox NS, Oliveira CC, Lahham A, Holland AE. Pulmonary rehabilitation referral and participation are commonly influenced by environment, knowledge, and beliefs about consequences: a systematic review using the Theoretical Domains Framework. J Physiother (Elsevier). 2017;63(2):84–93. https://doi.org/10.1016/j.jphys.2017.02.002.
Mathar H, Fastholm P, Hansen IR, Larsen NS. Why do patients with COPD decline rehabilitation. Scand J Caring Sci. 2016;30(3):432–41. https://doi.org/10.1111/scs.12268.
Robinson H, Williams V, Curtis F, Bridle C, Jones AW. Facilitators and barriers to physical activity following pulmonary rehabilitation in COPD: a systematic review of qualitative studies. NPJ Prim Care Respir Med. 2018;28(1):19. https://doi.org/10.1038/s41533-018-0085-7.
Miller MJ, Jones J, Anderson CB, Christiansen CL. Factors influencing participation in physical activity after dysvascular amputation: a qualitative meta-synthesis. Disabil Rehabil. 2019;41(26):3141–50. https://doi.org/10.1080/09638288.2018.1492031.
Greaves C, Poltawski L, Garside R, Briscoe S. Understanding the challenge of weight loss maintenance: a systematic review and synthesis of qualitative research on weight loss maintenance. Health Psychol Rev. 2017;11(2):145–63. https://doi.org/10.1080/17437199.2017.1299583.
Hartmann-Boyce J, Nourse R, Boylan AM, Jebb SA, Aveyard P. Experiences of reframing during self-directed weight loss and weight loss maintenance: systematic review of qualitative studies. Appl Psychol Health Well Being. 2018;10(2):309–29. https://doi.org/10.1111/aphw.12132.
Jones L, Grech C. The patient experience of remote telemonitoring for heart failure in the rural setting: a literature review. Contemp Nurse. 2016;52(2–3):230–43. https://doi.org/10.1080/10376178.2015.1111154.
Joo JY, Liu MF. Experience of culturally-tailored diabetes interventions for ethnic minorities: a qualitative systematic review. Clin Nurs Res. 2019. https://doi.org/10.1177/1054773819885952.
Hu R, van Velthoven MH, Meinert E. Perspectives of people who are overweight and obese on using wearable technology for weight management: systematic review. JMIR Mhealth Uhealth. 2020;8(1):e12651. https://doi.org/10.2196/12651.
Sutcliffe K, Melendez-Torres GJ, Burchett HED, Richardson M, Rees R, Thomas J. The importance of service-users’ perspectives: a systematic review of qualitative evidence reveals overlooked critical features of weight management programmes. Health Expect. 2018;21(3):563–73. https://doi.org/10.1111/hex.12657.
Radhakrishnan K, Baranowski T, Julien C, Thomaz E, Kim M. Role of digital games in self-management of cardiovascular diseases: a scoping review. Games Health. 2019;8(2):65–73. https://doi.org/10.1089/g4h.2018.0011.
Dwarswaard J, Bakker EJ, van Staa A, Boeije HR. Self-management support from the perspective of patients with a chronic condition: a thematic synthesis of qualitative studies. Health Expect. 2016;19(2):194–208. https://doi.org/10.1111/hex.12346.
Earle CC, Chapman RH, Baker CS, Bell CM, Stone PW, Sandberg EA, et al. Systematic overview of cost-utility assessments in oncology. J Clin Oncol. 2000;18(18):3302–17. https://doi.org/10.1200/JCO.2000.18.18.3302.
Pearce G, Pinnock H, Epiphaniou E, Parke HL, Heavey E, Griffiths CJ, et al. Experiences of self-management support following a stroke: a meta-review of qualitative systematic reviews. PLoS ONE. 2015;10(12):e0141803. https://doi.org/10.1371/journal.pone.0141803.
Toye F, Seers K, Hannink E, Barker K. A mega-ethnography of eleven qualitative evidence syntheses exploring the experience of living with chronic non-malignant pain. BMC Med Res Methodol. 2017;17(1):116. https://doi.org/10.1186/s12874-017-0392-7.
May CR, Cummings A, Myall M, Harvey J, Pope C, Griffiths P, et al. Experiences of long-term life-limiting conditions among patients and carers: what can we learn from a meta-review of systematic reviews of qualitative studies of chronic heart failure, chronic obstructive pulmonary disease and chronic kidney disease? BMJ Open. 2016;6(10):e011694. https://doi.org/10.1136/bmjopen-2016-011694.
Leventhal H, Leventhal EA, Contrada RJ. Self-regulation, health, and behavior: a perceptual-cognitive approach. Psychol Health. 1998;13(4):717–33. https://doi.org/10.1080/08870449808407425.
Paterson BL. The shifting perspectives model of chronic illness. J Nurs Scholarsh. 2001;33(1):21–6. https://doi.org/10.1111/j.1547-5069.2001.00021.x.
Yzer MC. The integrated model of behavioral prediction as a tool for designing health messages: theory and practice. In: Cho H, editor. Designing messages for health communication campaigns: theory and practice. Sage; 2012. p. 21–40.
Ryan RM, Deci EL. Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. Am Psychol. 2000;55(1):68–78. https://doi.org/10.1037//0003-066x.55.1.68.
Hudon C, Fortin M, Haggerty J, Loignon C, Lambert M, Poitras ME. Patient-centered care in chronic disease management: a thematic analysis of the literature in family medicine. Patient Educ Couns. 2012;88(2):170–6. https://doi.org/10.1016/j.pec.2012.01.009.
Pinto RZ, Ferreira ML, Oliveira VC, Franco MR, Adams R, Maher CG, et al. Patient-centred communication is associated with positive therapeutic alliance: a systematic review. J Physiother. 2012;58(2):77–87. https://doi.org/10.1016/s1836-9553(12)70087-5.
Camus-García E, González-González AI, Heijmans M, Niño de Guzmán E, Valli C, Beltran J, et al. Self-management interventions for adults living with chronic obstructive pulmonary disease (COPD): the development of a Core Outcome Set for COMPAR-EU project. PLOS ONE. 2021;16(3):e0247522. https://doi.org/10.1371/journal.pone.0247522.
Niño de Guzmán E, Martínez García L, González A, Heijmans M, Huaringa J, Immonen K, et al. The perspectives of patients and their caregivers on self-management interventions for chronic conditions: a protocol for a mixed-methods overview [version 1; peer review: 1 approved]. F1000Research. 2020. https://doi.org/10.12688/f1000research.22125.1.
Acknowledgements
The authors thank Ivan Solà for his invaluable help in the design of the search strategy. We also thank Héctor Pardo Hernández for his collaboration during the initial stages of this scoping review. Ena Niño de Guzmán is a doctoral candidate at the Paediatrics, Obstetrics and Gynaecology and Preventive Medicine Department, Universitat Autònoma de Barcelona, Barcelona, Spain.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the European Union’s Horizon 2020 research and innovation programme [754936]. ENDG was funded by a Rio Hortega contract from the Instituto de Salud Carlos III [CM17/00199]. LMG is funded by a Miguel Servet contract from the Instituto de Salud Carlos III [CP18/00007]. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Conflict of interest
Ena Niño de Guzmán Quispe, Laura Martínez García, Carola Orrego Villagrán, Monique Heijmans, Rosa Sunol, David Fraile-Navarro, Javier Pérez-Bracchiglione, Lyudmil Ninov, Karla Salas-Gama, Andrés Viteri García, and Pablo Alonso-Coello have no conflicts of interest that are directly relevant to the content of this article.
Ethics approval
Ethical approval was obtained from the Clinical Research Ethics Committee of the Avedis Donabedian Research Institute, the coordinator partner of the COMPAR-EU Project (EU 754936), and the University Institute for Primary Care Research (IDIAP Jordi Gol) and was signed on March 2018.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Data availability and materials
All the findings from the available data have been published in this manuscript.
Author contributions
ENDG, LMG, and PAC made substantial contributions to the conception and design of the study. ENDG, DF, JP, KS, and AVG collected all relevant data related to the studies. ENDG, LMG, RS, MH, COV, DF, JP, LN, KS, AVG, and PAC discussed and interpreted the results. ENDG, LMG, and PAC wrote the first draft of the manuscript. All authors revised the manuscript critically for important intellectual content and approved the final version submitted.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Niño de Guzmán Quispe, E., Martínez García, L., Orrego Villagrán, C. et al. The Perspectives of Patients with Chronic Diseases and Their Caregivers on Self-Management Interventions: A Scoping Review of Reviews. Patient 14, 719–740 (2021). https://doi.org/10.1007/s40271-021-00514-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40271-021-00514-2