Abstract
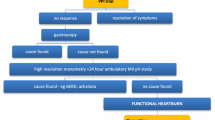
Patients with oesophageal symptoms in whom the presence of structural disorders, motility disorders, malignancy and gastro-oesophageal reflux disease has been excluded may be diagnosed as having a functional oesophageal disorder. Functional chest pain is the best studied of these disorders, with very limited evidence of the effectiveness of various treatments for functional heartburn, functional dysphagia and globus.

Similar content being viewed by others
References
Galmiche JP, Clouse RE, Bálint A, et al. Functional esophageal disorders. Gastroenterology. 2006;130(5):1459–65.
Amarasinghe G, Sifrim D. Functional esophageal disorders: pharmacological options. Drugs. 2014;74(12):1335–44.
Vakil N, van Zanten SV, Kahrilas P, et al. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101(8):1900–20.
Ostovaneh MR, Saeidi B, Hajifathalian K, et al. Comparing omeprazole with fluoxetine for treatment of patients with heartburn and normal endoscopy who failed once daily proton pump inhibitors: double-blind placebo-controlled trial. Neurogastroenterol Motil. 2014;26(5):670–8.
Miner PB Jr, Rodriguez-Stanley S, Proskin HM, et al. Tegaserod in patients with mechanical sensitivity and overlapping symptoms of functional heartburn and functional dyspepsia. Curr Med Res Opin. 2008;24(8):2159–72.
Rodriguez-Stanley S, Zubaidi S, Proskin HM, et al. Effect of tegaserod on esophageal pain threshold, regurgitation, and symptom relief in patients with functional heartburn and mechanical sensitivity. Clin Gastroenterol Hepatol. 2006;4(4):442–50.
Kumar AR, Katz PO. Functional esophageal disorders: a review of diagnosis and management. Expert Rev Gastroenterol Hepatol. 2013;7(5):453–61.
Jeon HK, Kim GH, Choi MK, et al. Clinical predictors for response to proton pump inhibitor treatment in patients with globus. J Neurogastroenterol Motil. 2013;19(1):47–53.
Kirch S, Gegg R, Johns MM, et al. Globus pharyngeus: effectiveness of treatment with proton pump inhibitors and gabapentin. Ann Otol Rhinol Laryngol. 2013;122(8):492–5.
Deary IJ, Wilson JA. Problems in treating globus pharyngis. Clin Otolaryngol Allied Sci. 1994;19(1):55–60.
You LQ, Liu J, Jia L, et al. Effect of low-dose amitriptyline on globus pharyngeus and its side effects. World J Gastroenterol. 2013;19(42):7455–60.
Tokashiki R, Okamoto I, Funato N, et al. Rikkunshito improves globus sensation in patients with proton-pump inhibitor-refractory laryngopharyngeal reflux. World J Gastroenterol. 2013;19(31):5118–24.
Kiebles JL, Kwiatek MA, Pandolfino JE, et al. Do patients with globus sensation respond to hypnotically assisted relaxation therapy? A case series report. Dis Esophagus. 2010;23(7):545–53.
Khalil HS, Reddy VM, Bos-Clark M, et al. Speech therapy in the treatment of globus pharyngeus: how we do it. Clin Otolaryngol. 2011;36(4):388–92.
Millichap F, Lee M, Pring T. A lump in the throat: should speech and language therapists treat globus pharyngeus? Diabil Rehabil. 2005;27(3):124–30.
Park SW, Lee H, Lee HJ, et al. Low-dose amitriptyline combined with proton pump inhibitor for functional chest pain. World J Gastroenterol. 2013;19(30):4958–65.
Prakash C, Clouse RE. Long-term outcome from tricyclic antidepressant treatment of functional chest pain. Dig Dis Sci. 1999;44(12):2373–9.
Cannon RO 3rd, Quyyumi AA, Mincemoyer R, et al. Imipramine in patients with chest pain despite normal coronary angiograms. N Engl J Med. 1994;330(20):1411–7.
Cox ID, Hann CM, Kaski JC. Low dose imipramine improves chest pain but not quality of life in patients with angina and normal coronary angiograms. Eur Heart J. 1998;19(2):250–4.
Lee H, Kim JH, Min BH, et al. Efficacy of venlafaxine for symptomatic relief in young adult patients with functional chest pain: a randomized, double-blind, placebo-controlled, crossover trial. Am J Gastroenterol. 2010;105(7):1504–12.
Keefe FJ, Shelby RA, Somers TJ, et al. Effects of coping skills training and sertraline in patients with non-cardiac chest pain: a randomized controlled study. Pain. 2011;152(4):730–41.
Doraiswamy PM, Varia I, Hellegers C, et al. A randomized controlled trial of paroxetine for noncardiac chest pain. Psychopharmacol Bull. 2006;39(1):15–24.
Broekaert D, Fischler B, Sifrim D, et al. Influence of citalopram, a selective serotonin reuptake inhibitor, on oesophageal hypersensitivity: a double-blind, placebo-controlled study. Aliment Pharmacol Ther. 2006;23(3):365–70.
Shapiro M, Shanani R, Taback H, et al. Functional chest pain responds to biofeedback treatment but functional heartburn does not: what is the difference? Eur J Gastroenterol Hepatol. 2012;24(6):708–14.
Gasiorowska A, Navarro-Rodriguez T, Dickman R, et al. The effect of Johrei on symptoms of patients with functional chest pain. Aliment Pharmaco Ther. 2009;29(1):126–34.
Jonsbu E, Dammen T, Morken G, et al. Short-term cognitive behavioral therapy for non-cardiac chest pain and benign palpitations: a randomized controlled trial. J Psychosom Res. 2011;70(2):117–23.
Jones H, Cooper P, Miller V, et al. Treatment of non-cardiac chest pain: a controlled trial of hypnotherapy. Gut. 2006;55(10):1403–8.
Disclosure
This article was adapted from Drugs 2014;74(12):1335–44 [2] by salaried/contracted employees of Adis/Springer. The preparation of this article was not supported by any external funding.
Author information
Authors and Affiliations
Consortia
Rights and permissions
About this article
Cite this article
Adis Medical Writers. Functional oesophageal disorders must be diagnosed properly and treated accordingly. Drugs Ther Perspect 31, 62–65 (2015). https://doi.org/10.1007/s40267-015-0182-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40267-015-0182-4