Abstract
Introduction
Frailty is highly prevalent in heart failure populations and a major risk factor for adverse drug reactions (ADRs) and adverse drug events (ADEs). This review aimed to describe the prevalence, causality and severity of ADRs or ADEs from heart failure medications among frail compared with non-frail older adults.
Methods
A systematic search of CENTRAL, MEDLINE, Embase, Ageline, CINAHL, International Pharmaceutical Abstracts, PsychInfo, Scopus, registries and citations prior to 18 May 2021 was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 checklist. Risk of bias and quality of evidence were assessed. Eligible studies included randomised controlled trials (RCTs) and observational studies of people diagnosed with heart failure, aged ≥ 65 years, with frailty defined by an objective measurement, and reported ADRs/ADEs from/with heart failure medications.
Results
Two reviewers screened 2419 articles; interrater reliability kappa = 0.88. Three observational studies (n = 2596), a secondary analysis of two RCTs (n = 2098) and two cohort studies (n = 498) were included in a narrative synthesis. Frail patients in randomised trials of sacubitril/valsartan, aliskiren, or enalapril had twice the risk of mortality (hazard ratio [HR] 2.09, 1.62–2.71) and hospitalisations (HR 1.82, 1.37–2.41) compared with robust patients, which may reflect responsiveness to medications and/or factors unrelated to medication use. Hospitalisations from falls, tiredness and nausea were probably attributable to digoxin and possibly preventable according to the Naranjo and Hallas scales, respectively.
Conclusion
The potential harms from heart failure medications in frail older people are poorly studied and understood. Clinical trials and pharmacovigilance studies should include frailty as a covariate to inform medication optimisation for this vulnerable and growing population.
Registration
Prospero registration number: CRD 42021253762.
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
The scarcity of knowledge and uncertainty of reported potential harms from heart failure medications in frail older people, suggests this vulnerable population is very underrepresented in studies. |
In three studies, there were very low to low levels of evidence in frail older people to support a twofold risk of hospitalisation and mortality with renin-angiotensin system inhibitors, and that falls, nausea and tiredness from digoxin led to possibly avoidable hospital readmissions. |
There is a need for high-quality research in older heart failure patients to include measures of frailty and frail participants, to inform patient-tailored treatment plans. |
1 Introduction
Heart failure affects approximately 65 million people worldwide and 50–75% die within 5 years of diagnosis [1,2,3]. Heart failure is the most common cause of hospitalisation in older people, accounting for 10% of hospitalisations among adults aged ≥ 75 years, and adults aged ≥ 75 years account for 50% of heart failure-related hospitalisations [4,5,6].
A critical aspect of providing care to older adults with heart failure is medication management, particularly optimising use of disease modifying and symptomatic treatments and minimising adverse drug reactions (ADRs). ADRs refer to “any response to a drug which is noxious and unintended, and which occurs at doses normally used for the prophylaxis, diagnosis, or therapy of disease, or for the modifications of physiological function” [7]. Adverse drug events (ADEs) broadly refer to any adverse outcome occurring in people taking a medication, whereas ADRs involve a causal relationship between medication and adverse reaction. Frailty, a syndrome associated with multisystem deficiencies or disabilities that lower individuals’ resilience to stressors and risk decompensation at lower thresholds, is present in up to 74% of older adults with heart failure [8]. Frailty is associated with increased risk of adverse outcomes and exacerbates the risk of ADRs in older heart failure patients [9, 10].
Yet the risk of ADRs among older people with heart failure and frailty are not well-established and are poorly represented in clinical trials of pharmacological interventions [11]. Understanding ADRs and ADEs in this population could ultimately help inform interventions to improve outcomes in this vulnerable population, since over half the hospital admissions due to ADRs are believed to be preventable [12]. Therefore, this review aimed to describe the prevalence, causality and severity of ADRs or ADEs from heart failure medications among frail compared with non-frail older adults.
2 Methods
A systematic review was conducted according to the protocol (Prospero registration number: CRD 42021253762) [13], and amended with additional authorship and data validation implemented at the data analysis stage. The review was reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 checklist [14]. A search of eight databases, including CENTRAL, MEDLINE, Embase, Ageline, CINAHL, International Pharmaceutical Abstracts, PsychInfo, and Scopus, was performed for human studies prior to 18 May 2021 disseminated in English. Published and unpublished studies were searched in Prospero and ClinicalTrials.gov, as well as citations in relevant studies. The search terms applied were frail older adults, heart failure-specific medications, and ADRs or ADEs. Validated filters for ADRs and ADEs were adapted from Golder et al. [15] (Electronic Supplementary Material [ESM] Table S1). The search was validated using the Peer Review of Electronic Search Strategies (PRESS) checklist [16] (ESM Table S2).
Eligible studies included randomised controlled trials (RCTs), meta-analyses, or observational study designs, across all health care settings. Qualitative studies, self-reports, case reports, case series, expert opinion, reviews and trials of pharmacotherapy with cardiovascular agents for indications other than heart failure were excluded. In cases where outcomes were reported in parallel studies that were ineligible, authors were contacted to request missing data of subgroup analysis. We included studies of individuals or analysis of subgroups for participants who were diagnosed with heart failure, treated with heart failure-specific medications, aged ≥ 65 years and described as frail using an objective criteria or frailty measurement. The term ‘frail’ was defined using systematically defined criteria specified by the authors (e.g., Frailty Phenotype [17], Frailty Index (FI) score [18], Clinical Frailty Score [19]). Guideline-directed heart failure-specific medications (ESM Table S3) were administered alone or in combination and in fixed or titrated (up/down) regimens. We included studies that measured ADRs or ADEs with definitions and/or causality assessment criteria secondary to a specific medication or pharmacological class, or specific ADRs or ADEs. Categories of severity ranged from mild or moderate clinical symptoms to severe outcomes of serious clinical risk or leading to death. Studies that only reported prevalence of heart failure medication use without reporting ADR or ADE outcomes were excluded.
The eligibility criteria were pilot tested on a 5% random sample of studies by the entire research team. Two review authors (MD and MS) independently performed screening and risk of bias, and disagreements were resolved by consultation with a third reviewer (DG/AM/PG/SH). Search results were screened with Covidence software (Melbourne, VIC, Australia) and duplicates were removed using the automated duplicate removal function, or manually identified. Data from the included studies were entered into a standard data form for participant and study characteristics, quality or risk of bias, outcomes and adverse events. Studies were grouped by study design and frailty status. One reviewer (MD) collected data into spreadsheets and a second reviewer (MS) validated 30% of the data for accuracy of reporting. Results were reviewed by the entire research team. A narrative synthesis of the key findings was summarised in tables and/or described, and forest plots were generated using R studio software. Study design and frailty groups were presented separately.
Risk of bias was assessed using the ROBINS-I Cochrane Collaboration risk of bias assessment tool for non-randomised studies of interventions (ESM Fig. S1) [20]. The Grading of Recommendations Assessment, Development and Evaluation (GRADE) approach (ESM Table S4) [21, 22] was used to summarise the overall quality of evidence for outcomes assessed by two reviewers (MD and MS). Analysis of prevalence, causality and severity of ADRs and ADEs was stratified according to the assessment model or GRADE score.
3 Results
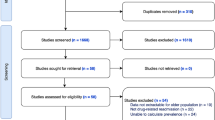
The search identified 2419 studies; 923 studies were identified as eligible and 3 met the inclusion criteria selected for analysis (Fig. 1). The kappa statistic was 0.88 for interrater reliability of screening. Three observational studies (n = 2596), including a secondary analysis of two RCTs (n = 2098) and two prospective observational cohort studies (n = 498), were identified and are summarised in Table 1. All studies reported severe ADEs of mortality and/or hospitalisation and one study reported mild to moderate ADRs leading to preventable hospitalisation [23]. The adapted FI [24] and modified frailty phenotype criteria [17] were used to define frailty in these studies.
A secondary analysis of two RCTs [25] compared outcomes by frailty group among participants with heart failure with reduced ejection fraction (HFrEF) from the PARADIGM-HF [26] (sacubitril/valsartan vs. enalapril) and ATMOSPHERE [27] (aliskiren with/without enalapril vs. enalapril) trials, which had identical inclusion and exclusion criteria and similar study protocols (ESM Table S5). For both trials, frailty was defined from an adapted FI [24], involving cumulative deficits in a 42-item FI. Participants with an FI ≤ 0.210 were considered non-frail/robust and patients with an FI > 0.210 were considered frail, and were further divided into groups by increments of 0.100 (0.211–0.310 or ≥ 0.311). Increased frailty score was associated with increased risk of adverse outcomes in a subgroup analysis of participants aged ≥ 75 years from both trials [25], but the prevalence of mortality and/or hospitalisation was not reported in this subgroup. Figure 2 shows an exposure–response trend between increasing frailty and risk of mortality and hospitalisations for participants taking sacubitril/valsartan, enalapril or aliskiren. Frail participants with an FI > 0.311 had an approximately twofold increase in mortality and hospitalisation compared with non-frail participants with an FI < 0.210. Frail participants with an FI > 0.311 had a higher risk of cardiovascular mortality (sub-distribution hazard ratio [sHR] 2.09, 1.62–2.71), all-cause mortality (hazard ratio [HR] 2.28, 1.81–2.87), heart failure hospitalisation (sHR 1.82, 1.37–2.41) and primary composite (sHR 2.03, 1.64–2.52) than those with an FI < 0.210. However, only all-cause mortality was statistically significantly higher in patients with FI scores between 0.211 and 0.310 than in those with an FI < 0.210 (HR 1.37, 1.08–1.74). There was no significant difference (p = 0.77, 0.54, 0.26, 0.83) in treatment effect of sacubitril/valsartan compared with enalapril between the frailty groups across all age groups, non-specific to ages ≥ 75 years, among the reported outcomes in Fig. 2. These outcomes (all-cause mortality and hospitalisation) were scored as having a low level of evidence and low risk of bias (ESM Fig. S1 and Table S4).
Severe adverse drug events by Frailty Index Score for sacubitril/valsartan, or enalapril [25]. The p-value interaction for each outcome is provided for treatment effect on overall frailty. HR hazard ratio, CI confidence interval, HF heart failure, CV cardiovascular
FRAIL-HF [28] was a prospective cohort study that evaluated the impact of frailty in non-dependent people aged ≥ 70 years hospitalised for HF. A twofold risk of mortality and heart failure readmission, as well as increased disability in frail compared with non-frail older inpatients, was reported [25]. The modified frailty phenotype definition [17] was applied to identify frail participants. The reported use of angiotensin-converting enzyme inhibitors (ACEIs) or angiotensin receptor blockers (ARBs) in frail compared with non-frail participants was 66.5% and 82.7%, respectively (p = 0.002). Frailty was associated with an increased risk of 1-year mortality (HR 2.13, 1.07–4.23), with no interaction between frailty and the effect of ACEIs/ARBs on survival (p = 0.14). During the 1-year follow-up period, deaths were reported in 25.0% (n = 79) of frail participants and 11.0% (n = 11) of non-frail participants (p < 0.001). The risk of mortality with frailty in heart failure patients was scored as having a very low level of evidence and moderate risk of bias (ESM Fig. S1 and Table S4).
The TREEE study [23] was a prospective cohort study examining the impact of medications on hospital readmission within 30 days in frail patients, defined using the modified frailty phenotype criteria [17], aged ≥ 75 years. ADRs were identified using the Naranjo score and the avoidability of readmissions was determined using the Hallas criteria and clinical judgement [29, 30]. The TREEE study reported 13 ADRs that were causes of readmissions. Of the 96 patients readmitted, heart failure was the most common diagnosis (n = 48, 50%), chronic heart failure was reported as an independent predictor for early hospitalisation (p = 0.024), and no deaths were reported. In the heart failure subgroup, two ADRs were classified as probably caused by digoxin use indicated for heart failure. The reasons for ADRs leading to hospitalisation were falls (Naranjo score = 5) and tiredness and nausea (Naranjo score = 6). Hospitalisation due to these ADRs were reported as possibly avoidable according to the Hallas criteria, with at least one or more alternative approaches or prevention available in theory. Readmissions attributed to adverse effects of dyspnoea (n = 8), tiredness (n = 2) and worsened general condition (n = 1) from under-use of ACEIs, ARBs or β-blockers were more frequently reported than ADRs from digoxin use (n = 2). Only the TREEE study reported the likelihood and preventability of ADRs from heart failure-specific medications in this review; however, the quality of evidence for falls, nausea, tiredness and hospitalisation was very low and with serious risk of bias. Due to the paucity of data, we could not report the prevalence for many common ADRs for other drug classes, reflected in the grading of evidence (ESM Fig. S1 and Table S4). Figure 3 summarises the prevalence of ADRs and ADEs with heart failure medications in frail compared with non-frail older people according to the GRADE quality of evidence.
The graded quality of evidence in frail compared with non-frail older people summarising the risk of ADRs or ADEs from heart failure medications. *The causes and avoidability of ADRs were defined using the Naranjo and Hallas scales. All other studies were limited to reporting of ADEs. ADRs adverse drug reactions, ADEs adverse drug events, GRADE Grading of Recommendations Assessment, Development and Evaluation
4 Discussion
The scarcity of knowledge in the literature highlights the poor representation of older frail populations in standard clinical trial and observational study protocols. ADRs and ADEs were not frequently reported for well-defined frail older populations with heart failure, and when investigated, very few outcomes were included. Regardless of the definition of frailty applied, increased risk was reported in frail compared with robust older people. While some increased risk of adverse outcomes from heart failure treatments were observed in frail compared with non-frail older people, these results were difficult to interpret and were uncertain.
The lack of high-quality studies in the literature reflects the widespread exclusion of vulnerable populations from heart failure clinical trials [31, 32]. Standard trial protocols often report findings for subgroups by age, sex, ethnicity, geography, and various cardiac-related factors. However, frailty and advancing age remain underrepresented in clinical and observational study designs despite evidence they are independent risk factors in heart failure. Most clinical trials related to heart failure were in those aged < 65 years, even though most real-world patients were older, had increased risk of multimorbidity and polypharmacy, and 50% of heart failure-related hospitalisations occur in those ≥ 75 years of age [6, 32]. The participation prevalence ratio (PPR), used to indicate underrepresentation (PPR < 0.8) or overrepresentation (PPR > 1.2) of older people compared with their ‘real world’ disease population, was significantly lower for people ≥ 65 years (PPR 0.48–0.62) and ≥ 75 years (PPR 0.20-0.33) of age in cardiovascular drug trials for heart failure [31]. This was further exacerbated by similar trends excluding frail participants from clinical trials and reported in limited observational studies [33, 34]. Additionally, clinical trials designed with run-in phases exclude patients who were non-adherent or unable to tolerate the intervention drug. However, this step may inadvertently exclude people at higher risk of adverse effects and may potentially lead to ADE estimations that do not reflect general populations and/or report biased underestimates of potential medication-related harms. In the PARADIGM-HF trial, approximately 20% of participants did not complete the run-in phase and were at higher risk of lower blood pressure (odds ratio [OR] 1.11, 1.07–1.14), lower glomerular filtration rate (OR 1.49, 1.35–1.65) or more severe heart failure with increased NT-ProBNP (1.20, 1.14–1.26) [35].
The overall prevalence of ADRs and ADEs were additionally challenging to generalise due to the varying definitions of frailty across studies [36]. The reporting of prevalence can vary in the same study population depending on the wide range of frailty measurements used. In the study by Purser et al. [37], the prevalence of frailty was reported as 63% with the FI score and 27% with the phenotype criteria. Regardless of the frailty definition used, frail compared with non-frail participants had a similar direction and increased magnitude of risk associated with adverse outcomes. Frailty is an independent risk factor of heart failure and has been associated with an approximately 1.5-fold increase in death and hospitalisation [9]. Although there was a study of frail heart failure with preserved ejection fraction (HFpEF) patients aged ≥ 50 years, taking spironolactone in the TOPCAT trial, this was not included because the study population was aged < 65 years [38]. However, the TOPCAT trial also demonstrated a similar exposure–response trend between increasing FI score and increased risk of mortality and hospitalisations. Those with higher FI scores (FI > 0.5) had an approximately twofold increase in cardiovascular mortality (HR 1.89, 1.24–2.89) and a fourfold increase in heart failure hospitalisations (HR 4.12, 3.00–5.65) compared with non-frail patients, with no significant difference in treatment effect on the outcomes between the frailty groups. Therefore, the findings in this review parallel the trends reported in younger frail populations, other heart failure types and drug classes [9, 38].
Although clear CONSORT guidance [39] for the appropriate reporting of harms for clinical trials exist, ADRs and ADEs were poorly represented in the literature, limiting the generalisability of the prevalence, severity and causality of ADRs and ADEs for the reported heart failure medications. This challenge is not unique to heart failure. Zorzela et al. [40] found similar limitations existed in general reporting of harms data in primary studies across all diseases. The challenges observed in non-specific disease studies were paralleled in studies of frail older heart failure populations. Older people are at increased risk of adverse events due to complex comorbidities, frailty, polypharmacy, and advanced stages of heart failure. Conversely, confounding can make it difficult to differentiate whether ADEs were due to the medication or pathology of disease progression [41, 42]. This review builds on work by Sztramko et al. [43], which found risk factors for ADEs with heart failure medications included advanced age, poor left ventricular function and increased New York Heart Association class. Although frailty was not evaluated, it supported that ADEs were poorly represented in the literature and reinforced the need to improve the characterisation and understanding of the magnitude and frequency of adverse events in this vulnerable population.
There was inconsistency between the increased risk of mortality and hospitalisation in frail compared with non-frail older patients and the general efficacy of heart failure medications to reduce mortality and hospitalisation. These factors confound our understanding of the pharmacological efficacy in older frail patients with advancing heart failure. Without factoring in frailty risk, Catananti et al. [10] found older hospitalised heart failure patients were at increased risk of developing ADRs (unadjusted OR 1.78, 1.52–2.09; adjusted OR 1.29, 1.06–1.56) compared with those without heart failure, commonly caused by diuretics, digoxin, and ACEIs. Overall, the ADRs were considered severe (52, 4.9%), moderate (508, 47.8%) and mild (499, 47%). Despite vulnerability to frequent heart failure medication adjustments and polypharmacy-related adverse effects, the reporting in frail older people of mild to moderate ADRs and ADEs (e.g., clinical symptoms, quality of life, activities of daily living) from common heart failure medications was rare (ESM Table S5). However, there were no statistically significant differences in treatment efficacy between frailty groups reported in this review [25]. Findings highlight the uncertainty of how the potential benefits of guideline-directed medical therapy (GDMT) can be weighed against potential medication-related harms due to lack of high-quality evidence in frail older people, necessitating cautious interpretation, individualised treatment plans and close monitoring.
Strategies to rehabilitate and reverse frailty status can offer valuable opportunities to improve prognosis and customise medication management to mitigate the increased risk of adverse outcomes in frail older people with heart failure. Age and frailty are important characteristics to predict mortality and rehospitalisation [44]. Due to potential multisystem deficiencies, frailty and associated disabilities may predispose patients to decompensate at lower thresholds and increase health care utilisation, requiring more outpatient and hospital visits [8]. Identifying this risk can support frailty-based management in older heart failure patients to improve prognosis and patient tolerance, optimise medication management, or support safe withdrawal of medications [45]. With the growing complexities attributed to aging, older age and frailty are independent risk factors that should be factored into emerging research and patient-tailored interventions, particularly since frailty is a potentially reversable syndrome [46]. These patients would benefit from a referral to a heart failure specialty team to review the management of their heart failure and potential ADRs and ADEs of GDMT [47]. Adequate reporting of ADRs and ADEs is critical to delivering clear communication that supports clinicians’ and patients’ shared decision making to improve medication adherence and identify triggers that merit safe withdrawal of these medications. The communication and confidence between prescribers and patients can be strengthened during initiation and adjustments of medications through understanding how the balance of treatment benefits with potential medication-related harms can impact clinical outcomes [48, 49]. This complementary knowledge combines individual patient values with tailored interventions to optimise quality of life and/or accommodate palliative care [50].
There were several limitations in this study. The very low to low grades of evidence and the absence of evidence for many common potential ADRs in frail older cohorts and drug classes significantly contributed to uncertainty in the reported outcomes. For example, we were careful to draw conclusions from a single study that reported ADRs from digoxin use in two participants [23]. Furthermore, cautious interpretation was applied in studies that extrapolated characteristics from clinical trials originally designed to evaluate efficacy of aliskiren or sacubitril/valsartan compared with enalapril, but not randomised to compare efficacy and potential harms between frailty groups. The review included data from the ATMOSPHERE [27] trial, which compared enalapril with aliskiren, even though aliskiren has limited use in practice. A meta-analysis was not performed on the few and variable outcomes, nor were subanalyses conducted by drug classes, frailty status, heart failure types, or predictors of advancing heart failure due to limited data. Therefore, we must be careful not to overestimate the impact of the findings that showed increased mortality and hospitalisation in frail older patients from these heart failure medications unless more evidence is available to adequately inform decision making on the potential harms of heart failure medications in frail older people. Both clinical trials and observational studies are necessary to fill this knowledge gap.
5 Conclusions
The complexities associated with advancing age, frailty, polypharmacy, comorbidities and complications from heart failure emphasise the importance of incorporating frailty into decision making and patient-tailored interventions. While pharmacotherapy utilisation data were collected, there remains opportunity for further evaluation and reporting on the impact of drug use patterns in frail older heart failure patients on specific and global health outcomes. Improved understanding of the prevalence, severity, causes and predictors of potential harms of these critical medications in frail older people can facilitate communication and trust between clinicians and patients and/or their careers. This may inform shared decision making on prescribing and deprescribing medications to not only optimise management of these patients but also improve the quality of decision making. We may unknowingly harm patients with frailty simply because data are limited on how they are impacted by these medications. Emerging heart failure-related clinical trials and observational study protocols should include frailty subgroups of older participants to improve reporting of efficacy and potential harms. Improvement in our understanding of the safety and potential medication-related harms of foundational therapies can support optimal prescription of and adherence with medications critical in improving clinical outcomes in vulnerable patients.
References
Groenewegen A, Rutten FH, Mosterd A, Hoes AW. Epidemiology of heart failure. Eur J Heart Fail. 2020;22:1342–56.
Shah KS, Xu H, Matsouaka RA, Bhatt DL, Heidenreich PA, Hernandez AF, et al. Heart failure with preserved, borderline, and reduced ejection fraction: 5-year outcomes. J Am Coll Cardiol. 2017;70(20):2476–86.
Jones NR, Roalfe AK, Adoki I, Hobbs FDR, Taylor CJ. Survival of patients with chronic heart failure in the community: a systematic review and meta-analysis. Eur J Heart Fail. 2019;21(11):1306–25.
Jackson SL, Tong X, King RJ, Loustalot F, Hong Y, Ritchey MD. National Burden of heart failure events in the United States, 2006 to 2014. Circ Heart Fail. 2018;11(12): e004873. https://doi.org/10.1161/CIRCHEARTFAILURE.117.004873.
Benjamin EJ, Virani SS, Callaway CW, Chamberlain AM, Chang AR, Cheng S, et al. Heart disease and stroke statistics-2018 update: a report From the American Heart Association. Circulation. 2018;137(12):e67–492. https://doi.org/10.1161/CIR.0000000000000558.
Rossignol P, Hernandez AF, Solomon SD, Zannad F. Heart failure drug treatment. Lancet. 2019;393(10175):1034–44.
World Health Organization. International drug monitoring. The role of the hospital. World Health Organ Tech Rep Ser. 1969;425:5–24.
McNallan SM, Singh M, Chamberlain AM, Kane RL, Dunlay SM, Redfield MM, et al. Frailty and healthcare utilization among patients with heart failure in the community. JACC Heart Fail. 2013;1(2):135–41.
Yang X, Lupon J, Vidan MT, Ferguson C, Gastelurrutia P, Newton PJ, et al. Impact of frailty on mortality and hospitalization in chronic heart failure: a systematic review and meta-analysis. J Am Heart Assoc. 2018;7(23): e008251. https://doi.org/10.1161/JAHA.117.008251.
Catananti C, Liperoti R, Settanni S, Lattanzio F, Bernabei R, Fialova D, et al. Heart failure and adverse drug reactions among hospitalized older adults. Clin Pharm Ther. 2009;86(3):307–10.
Hanlon P, Butterly E, Lewsey J, Siebert S, Mair FS, McAllister DA. Identifying frailty in trials: an analysis of individual participant data from trials of novel pharmacological interventions. BMC Med. 2020;18(1):309.
Chan M, Nicklason F, Vial JH. Adverse drug events as a cause of hospital admission in the elderly. Intern Med J. 2001;31(4):199–205.
Duong MH, Gnjidic D, McLachlan AJ, Sakiris MA, Goyal P, Hilmer SN. The Prevalence of Adverse Drug Reactions or Adverse Drug Events with Heart Failure Management in Frail Older Adults: A Systematic Review and Meta-Analysis. PROSPERO: International prospective register of systematic reviews [cited 2022 Jan 31]. https://www.crd.york.ac.uk/prospero/display_record.php?RecordID=253762.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. J Clin Epidemiol. 2021;134:178–89.
Golder S, Peryer G, Loke YK. Overview: comprehensive and carefully constructed strategies are required when conducting searches for adverse effects data. J Clin Epidemiol. 2019;113:36–43.
McGowan J, Sampson M, Salzwedel DM, Cogo E, Foerster V, Lefebvre C. PRESS peer review of electronic search strategies: 2015 guideline statement. J Clin Epidemiol. 2016;75:40–6.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146–56.
Mitnitski AB, Song X, Rockwood K. The estimation of relative fitness and frailty in community-dwelling older adults using self-report data. J Gerontol A Biol Sci Med Sci. 2004;59(6):M627–32.
Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, et al. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173(5):489–95.
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:4919. Doi: https://doi.org/10.1136/bmj.i4919.
Atkins D, Best D, Briss PA, Eccles M, Falck-Ytter Y, Flottorp S, et al. Grading quality of evidence and strength of recommendations. BMJ. 2004;328(7454):1490.
Guyatt GH, Oxman AD, Kunz R, Vist GE, Falck-Ytter Y, Schunemann HJ, et al. What is “quality of evidence” and why is it important to clinicians? BMJ. 2008;336(7651):995–8.
Ekerstad N, Bylin K, Karlson BW. Early rehospitalizations of frail elderly patients - the role of medications: a clinical, prospective, observational trial. Drug Healthc Patient Saf. 2017;9:77–88.
Rockwood K, Mitnitski A. Frailty in relation to the accumulation of deficits. J Gerontol A Biol Sci Med Sci. 2007;62(7):722–7.
Dewan P, Jackson A, Jhund PS, Shen L, Ferreira JP, Petrie MC, et al. The prevalence and importance of frailty in heart failure with reduced ejection fraction—an analysis of PARADIGM-HF and ATMOSPHERE. Eur J Heart Fail. 2020;22(11):2123–33.
McMurray JJ, Packer M, Desai AS, Gong J, Lefkowitz MP, Rizkala AR, et al. Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med. 2014;371(11):993–1004.
McMurray JJ, Krum H, Abraham WT, Dickstein K, Køber LV, Desai AS, et al. Aliskiren, enalapril, or aliskiren and enalapril in heart failure. N Engl J Med. 2016;374(16):1521–32.
Vidán MT, Blaya-Novakova V, Sánchez E, Ortiz J, Serra-Rexach JA, Bueno H. Prevalence and prognostic impact of frailty and its components in non-dependent elderly patients with heart failure. Eur J Heart Fail. 2016;18(7):869–75.
Naranjo CA, Busto U, Sellers EM, Sandor P, Ruiz I, Roberts EA, et al. A method for estimating the probability of adverse drug reactions. Clin Pharm Ther. 1981;30(2):239–45.
Hallas J, Harvald B, Gram LF, Grodum E, Brosen K, Haghfelt T, et al. Drug related hospital admissions: the role of definitions and intensity of data collection, and the possibility of prevention. J Intern Med. 1990;228(2):83–90.
Caughey GE, Inacio MC, Bell JS, Vitry AI, Shakib S. Inclusion of older people reflective of real-world clinical practice in cardiovascular drug trials. J Am Heart Assoc. 2020;9(21): e016936. https://doi.org/10.1161/JAHA.120.016936.
Cherubini A, Oristrell J, Pla X, Ruggiero C, Ferretti R, Diestre G, et al. The persistent exclusion of older patients from ongoing clinical trials regarding heart failure. Arch Intern Med. 2011;171(6):550–6.
Wang X, Zhou C, Li Y, Li H, Cao Q, Li F. Prognostic value of frailty for older patients with heart failure: a systematic review and meta-analysis of prospective studies. BioMed Res Int. 2018. https://doi.org/10.1155/2018/8739058.
Lien CT, Gillespie ND, Struthers AD, McMurdo ME. Heart failure in frail elderly patients: diagnostic difficulties, co-morbidities, polypharmacy and treatment dilemmas. Eur J Heart Fail. 2002;4:91–8.
Desai AS, Solomon S, Claggett B, McMurray JJ, Rouleau J, Swedberg K, et al. Factors associated with noncompletion during the run-in period before randomization and influence on the estimated benefit of LCZ696 in the PARADIGM-HF trial. Circ Heart Fail. 2016;9(6): e002735. https://doi.org/10.1161/CIRCHEARTFAILURE.115.002735.
Uchmanowicz I, Młynarska A, Lisiak M, Kałużna-Oleksy M, Wleklik M, Chudiak A, et al. Heart failure and problems with frailty syndrome: why it is time to care about frailty syndrome in heart failure. Card Fail Rev. 2019;5(1):37–43.
Purser JL, Kuchibhatla MN, Fillenbaum GG, Harding T, Peterson ED, Alexander KP. Identifying frailty in hospitalized older adults with significant coronary artery disease. J Am Geriatr Soc. 2006;54:1674–81.
Sanders NA, Supiano MA, Lewis EF, Liu J, Claggett B, Pfeffer MA, et al. The frailty syndrome and outcomes in the TOPCAT trial. Eur J Heart Fail. 2018;20(11):1570–7.
Boutron I, Altman DG, Moher D, Schulz KF, Ravaud P. CONSORT statement for randomized trials of nonpharmacologic treatments: a 2017 update and a CONSORT extension for nonpharmacologic trial abstracts. Ann Intern Med. 2017;167(1):40–7.
Zorzela L, Golder S, Liu Y, Pilkington K, Hartling L, Joffe A, et al. Quality of reporting in systematic reviews of adverse events: systematic review. BMJ. 2014;348: f7668. https://doi.org/10.1136/bmj.f7668.
Caughey GE, Shakib S, Barratt JD, Roughead EE. Use of medicines that may exacerbate heart failure in older adults: therapeutic complexity of multimorbidity. Drugs Aging. 2019;36(5):471–9.
Murray NP, Daly MJ. Gynecomastia and heart failure-adverse drug reaction or disease process? J Clin Pharm Ther. 1991;16(4):275–9.
Sztramko R, Chau V, Wong R. Adverse drug events and associated factors in heart failure therapy among the very elderly. Can Geriatr J. 2011;14(4):79–92.
Goyal P, Yum B, Navid P, Chen L, Kim DH, Roh J, et al. Frailty and post-hospitalization outcomes in patients with heart failure with preserved ejection fraction. Am J Cardiol. 2021;148:84–93.
Martín-Sánchez FJ, Christ M, Miró Ò, Peacock WF, McMurray JJ, Bueno H, et al. Practical approach on frail older patients attended for acute heart failure. Int J Cardiol. 2016;222:62–71.
Pulignano G, Del Sindaco D, Di Lenarda A, Tarantini L, Cioffi G, Gregori D, et al. Usefulness of frailty profile for targeting older heart failure patients in disease management programs: a cost-effectiveness, pilot study. J Cardiovasc Med. 2010;11:739–47.
Heidenreich PA, Bozkurt B, Aguilar D, Allen LA, Byun JJ, Colvin MM, et al. 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022;145(18):e895–1032. https://doi.org/10.1161/CIR.0000000000001063.
van der Wal MH, Jaarsma T. Adherence in heart failure in the elderly: problem and possible solutions. Int J Cardiol. 2008;125(2):203–8.
Ruppar TM, Cooper PS, Mehr DR, Delgado JM, Dunbar-Jacob JM. Medication adherence interventions improve heart failure mortality and readmission rates: systematic review and meta-analysis of controlled trials. J Am Heart Assoc. 2016;5(6):17.
Teixeira A, Arrigo M, Tolppanen H, Gayat E, Laribi S, Metra M, et al. Management of acute heart failure in elderly patients. Arch Cardiovasc Dis. 2016;109(6–7):422–30.
Acknowledgements
The authors acknowledge the collaboration of Prof. Geoffrey Tofler for his clinical specialist advice, librarian Dr Yulia Ulyannikova for technical assistance and PRESS validation, Mr Ryan Snow for graphic design support, and the technical assistance of Mr Jim Matthews of the Sydney Informatics Hub, a Core Research Facility of the University of Sydney.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
MD is supported by a grant funded by the Commonwealth of Australia for the National Health and Medical Research Council (NHMRC) Postgraduate Scholarship Grant APP1191018 awarded in 2020.
Conflicts of interest
Mai H. Duong, Danijela Gnjidic, Andrew J. McLachlan, Marissa A. Sakiris, Parag Goyal, and Sarah N. Hilmer declare that they have no potential conflicts of interest that might be relevant to the contents of this manuscript.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Availability of data and material
Not applicable.
Code availability
Not applicable.
Authors’ contributions
MD, DG, AM and SH contributed to the study conception and design. MD performed project administration and data collection. MD and MS screened all studies and assessed the risk of bias and quality of evidence. SH and PG provided clinical expertise. The manuscript was written by MD. All authors contributed to validation of eligible studies, data analysis, and visualisation, commented on previous versions of the manuscript and approved the final draft.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Duong, M.H., Gnjidic, D., McLachlan, A.J. et al. The Prevalence of Adverse Drug Reactions and Adverse Drug Events from Heart Failure Medications in Frail Older Adults: A Systematic Review. Drugs Aging 39, 631–643 (2022). https://doi.org/10.1007/s40266-022-00957-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-022-00957-8