Abstract
Purpose of Review
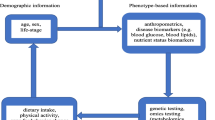
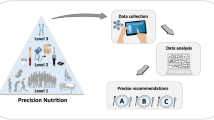
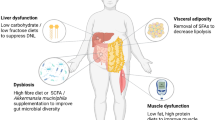
Precision nutrition requires a solid understanding of the factors that determine individual responses to dietary treatment. We review the current state of knowledge in identifying human metabotypes – based on circulating biomarkers – that can predict weight loss or other relevant physiological outcomes in response to diet treatment.
Recent Findings
Not many studies have been conducted in this area and the ones identified here are heterogeneous in design and methodology, and therefore difficult to synthesize and draw conclusions. The basis of the creation of metabotypes varies widely, from using thresholds for a single metabolite to using complex algorithms to generate multi-component constructs that include metabolite and genetic information. Furthermore, available studies are a mix of hypothesis-driven and hypothesis-generating studies, and most of them lack experimental testing in human trials.
Summary
Although this field of research is still in its infancy, precision-based dietary intervention strategies focusing on the metabotype group level hold promise for designing more effective dietary treatments for obesity.

Similar content being viewed by others
Abbreviations
- BMI:
-
Body mass index
- BCAA:
-
Branched-chain amino acid
- CRP:
-
C-reactive protein
- HOMA-IR:
-
Homeostatic model assessment of insulin resistance
- HETE:
-
Hydroxyeicosatetraenoic
- SDS:
-
Standard deviation score
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Haslam D, James W. Curbing the obesity epidemic. Lancet, The. 2005;367:1549. https://doi.org/10.1016/S0140-6736(05)67483-1.
Calle E, Rodriguez C, Walker-thurmond K, Thun M. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003;348:1625–38. https://doi.org/10.1056/NEJMoa021423.
Andersson CX, Gustafson B, Hammarstedt A, et al. Inflamed adipose tissue, insulin resistanceand vascular injury. Diabetes Metab Res Rev. 2008;24:595–603. https://doi.org/10.1002/dmrr.889.
Chooi YC, Ding C, Magkos F. The epidemiology of obesity. Metabolism. 2019;92:6–10. https://doi.org/10.1016/j.metabol.2018.09.005.
• Blüher M. Obesity : global epidemiology and pathogenesis. Nat Rev Endocrinol. 2019;15. https://doi.org/10.1038/s41574-019-0176-8. A recent comprehensive overview of the epidemiology and pathogenesis of obesity.
Yancy WS, Westman EC, McDuffie JR, et al. A randomized trial of a low-carbohydrate diet vs orlistat plus a low-fat diet for weight loss. Arch Intern Med. 2010;170:136–45. https://doi.org/10.1001/archinternmed.2009.492.
Greenberg I, Stampfer MJ, Schwarzfuchs D, Shai I. Adherence and success in long-term weight loss diets: the dietary intervention randomized controlled trial (direct). J Am Coll Nutr. 2009;28:159–68. https://doi.org/10.1080/07315724.2009.10719767.
Gardner CD, Kiazand A, Kim S, et al. Comparison of the Atkins, Zone, Ornish, and LEARN diets for change in weight and related risk factors among overweight premenopausal women. The A TO Z Weight Loss Study: A Randomized Trial. J Am Med Assoc. 2007;297:969–78.
• Ritz C. Statistical analysis of continuous outcomes from parallel-arm randomized controlled trials in nutrition – a tutorial. Eur J Clin Nutr. 2020. https://doi.org/10.1038/s41430-020-00750-z. A treatise on modern statistical analysis methods used in nutrition research.
Dansinger ML, Gleason JA, Griffith JL, et al. Comparison of the Atkins, Ornish, weight watchers, and zone diets for weight loss and heart disease risk reduction: a randomized trial. J Am Med Assoc. 2005;293:43–53. https://doi.org/10.1001/jama.293.1.43.
Sacks FM, Bray GA, Carey VJ, et al. Comparison of weight-loss diets with different compositions of fat, protein, and carbohydrates. N Engl J Med. 2009;360:859–73. https://doi.org/10.1056/NEJMoa0804748.
Astrup A, Hjorth MF. Classification of obesity targeted personalized dietary weight loss management based on carbohydrate tolerance. Eur J Clin Nutr. 2018;72:1300–4. https://doi.org/10.1038/s41430-018-0227-6.
Dragsted LO. The metabolic nature of individuality. Nat Food. 2020;1:327–8. https://doi.org/10.1038/s43016-020-0104-z.
Biesiekierski JR, Livingstone KM. Personalised nutrition: updates, gaps and next steps. Nutrients. 2019;11:1793. https://doi.org/10.3390/nu11081793.
Gibney MJ, Walsh MC. The future direction of personalised nutrition: my diet, my phenotype, my genes. Proc Nutr Soc. 2013;72:219–25. https://doi.org/10.1017/S0029665112003436.
Celis-Morales C, Livingstone KM, Marsaux CFM, et al. Effect of personalized nutrition on health-related behaviour change: evidence from the Food4Me European randomized controlled trial. Int J Epidemiol. 2017;46:578–88. https://doi.org/10.1093/ije/dyw186.
McGuire S. Scientific report of the 2015 dietary Guidelines Advisory Committee. Washington, DC: US Departments of Agriculture and Health and Human Services, 2015. Adv Nutr. 2016;7:202–4. https://doi.org/10.3945/an.115.011684.
•• Garcia-Perez I, Posma JM, Chambers ES, et al. Dietary metabotype modelling predicts individual responses to dietary interventions. Nat Food. 2020;1:355–364. https://doi.org/10.1038/s43016-020-0092-z. A well-designed crossover study exploring the individuality in response to same diet. An important study that highlights the variability in response for different diets and a tool that can be used in future decision-making strategies within preventing of e.g. obesity treatment.
Chatelan A, Bochud M, Frohlich KL. Precision nutrition: hype or hope for public health interventions to reduce obesity? Int J Epidemiol. 2019;48:332–42. https://doi.org/10.1093/ije/dyy274.
Zeisel SH. Precision (personalized) nutrition: understanding metabolic heterogeneity. Annu Rev Food Sci Technol. 2020;11:71–92. https://doi.org/10.1146/annurev-food-032519-051736.
• Palmnäs M, Brunius C, Shi L, et al. Perspective: metabotyping–a potential personalized nutrition strategy for precision prevention of cardiometabolic disease. Adv Nutr. 2020;11:524–532. https://doi.org/10.1093/advances/nmz121. An inspiring perspective that discuss the concept of metabotyping.
Riedl A, Gieger C, Hauner H, et al. Metabotyping and its application in targeted nutrition: an overview. Br J Nutr. 2017;117:1631–44. https://doi.org/10.1017/S0007114517001611.
Tebani A, Bekri S. Paving the way to precision nutrition through metabolomics. Front Nutr. 2019;6:1–10. https://doi.org/10.3389/fnut.2019.00041.
de Toro-Martín J, Arsenault BJ, Després JP, Vohl MC. Precision nutrition: a review of personalized nutritional approaches for the prevention and management of metabolic syndrome. Nutrients. 2017;9:1–28. https://doi.org/10.3390/nu9080913.
Guijas C, Montenegro-Burke JR, Warth B, et al. Metabolomics activity screening for identifying metabolites that modulate phenotype. Nat Biotechnol. 2018;36:316–20. https://doi.org/10.1038/nbt.4101.
Laddu D, Hauser M. Addressing the nutritional phenotype through personalized nutrition for chronic disease prevention and management. Prog Cardiovasc Dis. 2019;62:9–14. https://doi.org/10.1016/j.pcad.2018.12.004.
Zhang A, Sun H, Wang X. Power of metabolomics in biomarker discovery and mining mechanisms of obesity. Obes Rev. 2013;14:344–9. https://doi.org/10.1111/obr.12011.
Aleksandrova K, Egea Rodrigues C, Floegel A, Ahrens W. Omics biomarkers in obesity: novel etiological insights and targets for precision prevention. Curr Obes Rep. 2020;9:219–30. https://doi.org/10.1007/s13679-020-00393-y.
•• Kirk D, Catal C, Tekinerdogan B. Precision nutrition: a systematic literature review. Comput Biol Med. 2021;133:104365. https://doi.org/10.1016/j.compbiomed.2021.104365. This systematic review presents an overview of where and how machine learning has been used in precision nutrition from various aspects.
Martorell-Marugán J, Tabik S, Benhammou Y, et al. Deep learning in omics data analysis and precision medicine. Comput Biol. 2019;37–53. https://doi.org/10.15586/computationalbiology.2019.ch3.
Johnson CH, Ivanisevic J, Siuzdak G. Metabolomics: beyond biomarkers and towards mechanisms. Nat Rev Mol Cell Biol. 2016;17:451–9. https://doi.org/10.1038/nrm.2016.25.
Newgard CB. Metabolomics and metabolic diseases: where do we stand? Cell Metab. 2017;25:43–56. https://doi.org/10.1016/j.cmet.2016.09.018.
Xie B, Waters MJ, Schirra HJ. Investigating potential mechanisms of obesity by metabolomics. J Biomed Biotechnol. 2012. https://doi.org/10.1155/2012/805683.
Payab M, Tayanloo-Beik A, Falahzadeh K, et al. Metabolomics prospect of obesity and metabolic syndrome; a systematic review. J Diabetes Metab Disord. 2021. https://doi.org/10.1007/s40200-021-00917-w.
• Hjorth MF, Bray GA, Zohar Y, et al. Pretreatment fasting glucose and insulin as determinants of weight loss on diets varying in macronutrients and dietary fibers–the POUNDS LOST study. Nutrients. 2019;11:1–12. https://doi.org/10.3390/nu11030586. A retrospective study reanalyzes data and presents different groups of individuals with obesity who respond differently to different diets.
Hjorth MF, Ritz C, Blaak EE, et al. Pretreatment fasting plasma glucose and insulin modify dietary weight loss success: results from 3 randomized clinical trials. Am J Clin Nutr. 2017;106:499–505. https://doi.org/10.3945/ajcn.117.155200.
• Kwee LC, Ilkayeva O, Muehlbauer MJ, et al. Metabolites and diabetes remission after weight loss. Nutr Diabetes. 2021;11. https://doi.org/10.1038/s41387-021-00151-6. This study presented metabolites predictive for weight loss-induced remission in different groups of subjects with obesity.
Bonaventura A, Liberale L, Carbone F, et al. High baseline C-reactive protein levels predict partial type 2 diabetes mellitus remission after biliopancreatic diversion. Nutr Metab Cardiovasc Dis. 2017;27:423–9. https://doi.org/10.1016/j.numecd.2017.01.007.
Carbone F, Nulli Migliola E, Bonaventura A, et al. High serum levels of C-reactive protein (CRP) predict beneficial decrease of visceral fat in obese females after sleeve gastrectomy. Nutr Metab Cardiovasc Dis. 2018;28:494–500. https://doi.org/10.1016/j.numecd.2018.01.014.
Marco-Ramell A, Tulipani S, Palau-Rodriguez M, et al. Untargeted profiling of concordant/discordant phenotypes of high insulin resistance and obesity to predict the risk of developing diabetes. J Proteome Res. 2018;17:2307–17. https://doi.org/10.1021/acs.jproteome.7b00855.
Heianza Y, Sun D, Zheng Y, et al. Early changes in metabolomics signature and prediction of long-term successful weight-loss: the POUNDS LOST trial. Circulation. 2017;136:A14483.
Stroeve JHM, Saccenti E, Bouwman J, et al. Weight loss predictability by plasma metabolic signatures in adults with obesity and morbid obesity of the DiOGenes study. Obesity. 2016;24:379–88. https://doi.org/10.1002/oby.21361.
Geidenstam N, Al-Majdoub M, Ekman M, et al. Metabolite profiling of obese individuals before and after a one year weight loss program. Int J Obes. 2017;41:1369–78. https://doi.org/10.1038/ijo.2017.124.
Geidenstam N, Magnusson M, Danielsson APH, et al. Amino acid signatures to evaluate the beneficial effects of weight loss. Int J Endocrinol. 2017. https://doi.org/10.1155/2017/6490473.
• Geidenstam N, Hsu YHH, Astley CM, et al. Using metabolite profiling to construct and validate a metabolite risk score for predicting future weight gain. PLoS One. 2019;14:1–20. https://doi.org/10.1371/journal.pone.0222445. A metabolic profiling study proved their constructed metabolite risk score to be a strong marker for insulin sensitivity and as a weight gain predictor.
Wahl S, Holzapfel C, Yu Z, et al. Metabolomics reveals determinants of weight loss during lifestyle intervention in obese children. Metabolomics. 2013;9:1157–67. https://doi.org/10.1007/s11306-013-0550-9.
PREVENTOMICS: Empowering consumers to PREVENT diet-related diseases through "omics" science. https://preventomics.eu/. Accessed 6 Dec 2021.
Celis-Morales C, Livingstone KM, Marsaux CFM, et al. Design and baseline characteristics of the Food4Me study: a web-based randomised controlled trial of personalised nutrition in seven European countries. Genes Nutr. 2015;10. https://doi.org/10.1007/s12263-014-0450-2.
O’Donovan CB, Walsh MC, Woolhead C, et al. Metabotyping for the development of tailored dietary advice solutions in a European population: the Food4Me study. Br J Nutr. 2017;118:561–9. https://doi.org/10.1017/S0007114517002069.
•• Berry SE, Valdes AM, Drew DA, et al. Human postprandial responses to food and potential for precision nutrition. Nat Med. 2020;26:964–973. https://doi.org/10.1038/s41591-020-0934-0. This comprehensive study presents postprandial metabolic responses to nutritional challenges from 1002 subjects. A tool that can be relevant in the future of precision nutrition.
Gijbels A, Trouwborst I, Jardon KM, et al. The PERSonalized Glucose Optimization Through Nutritional Intervention (PERSON) study: rationale, design and preliminary screening results. Front Nutr. 2021;8. https://doi.org/10.3389/fnut.2021.694568.
Aleksandrova K, Mozaffarian D, Pischon T. Addressing the perfect storm: biomarkers in obesity and pathophysiology of cardiometabolic risk. Clin Chem. 2018;64:142–53. https://doi.org/10.1373/clinchem.2017.275172.
Torres N, Tovar AR. The present and future of personalized nutrition. Rev Invest Clin. 2021;73:321–325. https://doi.org/10.24875/RIC.21000346.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Diabetes and Obesity
Rights and permissions
About this article
Cite this article
Pigsborg, K., Magkos, F. Metabotyping for Precision Nutrition and Weight Management: Hype or Hope?. Curr Nutr Rep 11, 117–123 (2022). https://doi.org/10.1007/s13668-021-00392-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13668-021-00392-y