Abstract
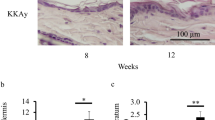
This study was designed to determine the impairment of the skin structure in experimentally-induced diabetes with injection of streptozotocin (STZ). Experimental groups consisted of controls (group 1, N = 10) and diabetes groups (group 2, N = 10). Dorsal skin was removed for routine histological tissue procedures. Hematoxylene and Eosin (HE), Masson’s Trichrome and Periodic Acid Schiff (PAS) stainings, immunohistochemical connexin 43 (Cx43) and type IV collagen stainings were applied. Morphometry of epidermal thickness were also determined. Group 2 revealed decrease in epidermal thickness with disintegration of epithelium and decrease of dermal collagen fibers. Stratum spinosum were morphologically abnormal for group 2. Measurements of epidermal thickness revealed statistically significant decrease (P = 0.000). PAS staining for group 2 revealed disruption of the basement membrane. Epithelial scar formation, deterioration of transformation in the polyhedral cells, degradation of epidermis and decrease in PAS staining for vascular structures were observed, whereas the reticular dermis and hair follicles were normal. Collagen fiber density in group 2 were found to be prominently decreased in dermis with Masson’s Trichrome staining. Evident decrease in immunostaining of Cx43 and type IV collagen were also shown in diabetic group in comparison to the controls. In conclusion, diabetes not only induced impairment of the epidermal integrity and deterioration in the epidermis via loss of gap junctions (the most prominent cellular junctional complex), but also caused dramatically negative impact on the dermal collagen content, and integrity of the basement membrane.







Similar content being viewed by others
References
Cowie CC, Rust KF, Ford ES, Eberhardt MS, Byrd-Holt DD, et al. Full accounting of diabetes and pre-diabetes in the U.S. population in 1988–1994 and 2005–2006. Diab Care. 2009;32:287–94.
Kahn CR, Weir GC, King GL, Jacobson AM, Moses AC, Smith RJ. Joslin’s Diabetes Mellitus. 14th ed. Boston: Lippincott Williams and Wilkins; 2005. p. 331–8.
Cotran RS., Kumar V, Collins T. Robbins pathologic basis of disease. 6th ed, Philadelphia: WB Saunders, 1999.
Kosova B, Cetintaş VB, Yavaşoğlu A, Altay B, Aktuğ H. From a molecular biological viewpoint, does endothelin type A receptor antagonist therapy reduce diabetes-induced testicular damage in rats? Urology. 2011;77:250.7–13.
Masuzawa K, Jesmin S, Maeda S, Zaedi S, Shimojo N, Miyauchi T, et al. Effect of endothelin dual receptor antagonist on VEGF levels in streptozotocin-induced diabetic rat retina. Exp Biol Med (Maywood). 2006;231:1090–4.
Gartner LP, Hiatt JL. Color Textbook of Histology. 3rd ed. Philadelphia: Saunders/Elsevier; 2007.
Kanitakis J. Anatomy, histology and immunohistochemistry of normal human skin. Eur J Dermatol. 2002;12:390–9.
Kierszenbaum AL. Histology and cell biology: an introduction to pathology. 2nd ed. Philadelphia: Mosby/Elsevier; 2007.
Lee SH, Jeong SK, Ahn SK. An update of the defensive barrier function of skin. Yonsei Med J. 2006;47:293–306.
Goodenough DA, Paul DL. Beyond the gap: functions of unpaired connexon channels. Nat Rev Mol Cell Biol. 2003;4:285–94.
Meşe G, Richard G, White TW. Gap junctions: basic structure and function. J Invest Dermatol. 2007;127:2516–24.
Brissette JL, Kumar NM, Gilula NB, Dotto GP. The tumor promoter 12-O-tetradecanoylphorbol-13-acetate and the ras oncogene modulate expression and phosphorylation of gap junction proteins. Mol Cell Biol. 1991;11:5364–71.
Laird DW. Life cycle of connexins in health and disease. Biochem J. 2006;394:527–43.
Risek B, Klier FG, Gilula NB. Multiple gap junction genes are utilized during rat skin and hair development. Development. 1992;116:639–51.
Rossello RA, Kohn DH. Gap junction intercellular communication: a review of a potential platform to modulate craniofacial tissue engineering. J Biomed Mater Res B Appl Biomater. 2009;88:509–18.
Salomon D, Masgrau E, Vischer S, Ullrich S, Dupont E, Sappino P, et al. Topography of mammalian connexins in human skin. J Invest Dermatol. 1994;103:240–7.
Burgeson RE, Christiano AM. The dermal-epidermal junction. Curr Opin Cell Biol. 1997;9:651–8.
Inoue S. Ultrastructure of basement membranes. Int Rev Cytol. 1989;117:57–98.
Marinkovich MP, Keene DR, Rimberg CS, Burgeson RE. Cellular origin of the dermal-epidermal basement membrane. Dev Dyn. 1993;197:255–67.
Wang TW, Sun JS, Huang YC, Wu HC, Chen LT, Lin FH. Skin basement membrane and extracellular matrix proteins characterization and quantification by real time RT-PCR. Biomaterials. 2006;27:5059–68.
Dai FX, Diederich A, Skopec J, Diederich D. Diabetes-induced endothelial dysfunction in streptozotocin-treated rats: role of prostaglandin endoperoxides and free radicals. J Am Soc Nephrol. 1993;4:1327–36.
Paron NG, Lambert PW. Cutaneous manifestations of diabetes mellitus. Prim Care. 2000;27:371–83.
Ferringer T, Miller 3rd F. Cutaneous manifestations of diabetes mellitus. Dermatol Clin. 2002;20:483–92.
Huntley AC. The cutaneous manifestations of diabetes mellitus. J Am Acad Dermatol. 1982;7:427–55.
Richard G, Abdullah S. Connexins: a connection with the skin. Getting to the heart of gap junction pathology. Novartis Foundations Symposium: Gap junction-mediated intercellular signalling in health and disease. Exp Dermatol. 2000;9:77–96.
Feldman EC: Disease of Endocrine Pancreas. In Textbook of Veterinary Internal Medicine. Disease of the Dog and Cat. 2nd ed. Philadelphia: Saunders; 1983; 67: 1615–1650
Chithra P, Sajithlal GB, Chandrakasan G. Influence of Aloe vera on collagen characteristics in healing dermal wounds in rats. Mol Cell Biochem. 1998;181:71–6.
Schneir M, Ramamurthy N, Golub L. Skin collagen metabolism in the streptozotocin-induced diabetic rat. Enhanced catabolism of collagen formed both before and during the diabetic state. Diabetes. 1982;31:426–31.
Cox NH, More IA, McCruden D, Jones SK, Ong-Tone L, Finlay AY, et al. Electron microscopy of clinically normal skin of diabetic patients. Clin Exp Dermatol. 1988;13:11–5.
Sternberg M, Cohen-Forterre L, Peyroux J. Connective tissue in diabetes mellitus: biochemical alterations of the intercellular matrix with special reference to proteoglycans, collagens and basement membranes. Diabete Metab. 1985;11:27–50.
Chen XF, Lin WD, Lu SL, Xie T, Ge K, Shi YQ, et al. Mechanistic study of endogenous skin lesions in diabetic rats. Exp Dermatol. 2010;19:1088–95.
Şensoy N, Gençoğlan G. Tip II diyabetli hastalarda deri bulgularının vücut kitle indeksi ve HBA1c ile ilişkisi (Association of cutaneous manifestations with body mass index and HbA1c levels in type II diabetes mellitus patients). Anatol J Clin Investig. 2009;3:213–7.
Yurchenco PD, Patton BL. Developmental and pathogenic mechanisms of basement membrane assembly. Curr Pharm Des. 2009;15:1277–94.
Goliger JA, Paul DL. Wounding alters epidermal connnexin expression and gap junction-mediated intercellular communication. Mol Biol Cell. 1995;6:1491–501.
Solan JL, Lampe PD. Connexin43 phosphorylation: structural changes and biological effects. Biochem J. 2009;419:261–72.
Kelsell DP, Wilgoss AL, Richard G, Stevens HP, Munro CS, Leigh IM. Connexin mutations associated with palmoplantar keratoderma and profound deafness in a single family. Eur J Hum Genet. 2000;8:469–72.
Di WL, Rugg EL, Leigh IM, Kelsell DP. Multiple epidermal connexins are expressed in different keratinocyte subpopulations including connexin 31. J Invest Dermatol. 2001;117:958–64.
Wang CM, Lincoln J, Cook JE, Becker DL. Abnormal connexin expression underlies delayed wound healing in diabetic skin. Diabetes. 2007;56:2809–17.
Acknowledgments
The authors would like to thank Ege University Faculty of Medicine, Turkey for funding. This study is the master thesis of the first author. It was funded by Ege University Faculty of Medicine-Research
Funds Izmir, Turkiye (Project number 2009\139).
No commercial support was obtained for this study.
Conflict of Interest
Authors have no conflict of interest (financial or otherwise).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Akarca, S.Ö., Yavaşoğlu, A., Ayşegül, U. et al. Investigation on the effects of experimental STZ-induced diabetic rat model on basal membrane structures and gap junctions of skin. Int J Diabetes Dev Ctries 32, 82–89 (2012). https://doi.org/10.1007/s13410-012-0070-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13410-012-0070-6