Abstract
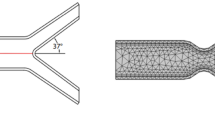
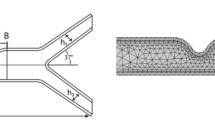
The present study investigated the transient pulsatile blood flow of Herschel–Bulkley fluid through tapered arteries with overlapping stenosis and hyperelastic wall material by employing fully coupled fluid–structure interaction technique. 3D ω-shaped tapered arteries with hyperelastic wall material were ideally modelled with different aspect ratios (ARs), stenosis severities (SSs) and tapering angles (\(\xi \)). The effects of non-Newtonian Herschel–Bulkley fluid model on various parameters, such as \(\xi \), length of stenosed region (\({\overline{L} }_{0}\)) and SS, were explored for converging, diverging and normal arteries in terms of induced wall stresses, flow patterns and wall displacements. The differences in wall stress, flow streamlines, velocity and pressure contours were also highlighted. Wall pressure increases as SS increases; however, wall pressure suddenly decreases with the decrease in AR. The increase in SS in greater wall deformation with higher pressure gradients can be used as a remarkable indicator of hypertension. Higher average wall shear stress (AWSS) values were observed at the regions of high contact areas of stenosis to the fluid. The sudden fall in pressure can cause the stenosed vessel to collapse under the influence of low-pressure gradients. AR and \({\overline{L} }_{0}\) can be considered important parameters to predict hypertension in overlapping stenosed arteries. The contact region of stenosed arteries should be kept under observation to reduce the further development of atherosclerosis. Higher AWSS values may help in reducing the risk of thrombosis after the stenosed region in converging tapering arteries.
Graphical abstract













Similar content being viewed by others
Abbreviations
- AR:
-
Aspect ratio
- CVD:
-
Cardiovascular disease
- \(\overline{d }\) :
-
Location of stenotic region
- \(D\) :
-
Deformation tensor
- E :
-
Young’s modulus
- FSI:
-
Fluid–structure interaction
- I :
-
Identity matrix
- \(k\) :
-
Consistency index
- \({\overline{L} }_{0}\) :
-
Stenotic segment length
- \(p\left(t\right)\) :
-
Exit pressure (Pa)
- \({\overline{R} }_{0}\) :
-
Radius of normal artery
- \(\overline{R }(\overline{z })\) :
-
Stenotic region radius
- SS:
-
Stenosis severity
- VMS:
-
Von Mises stress
- WSS:
-
Wall shear stress
- \(\phi \) :
-
Tapering angle
- \(\rho \) :
-
Density (kg m−3)
- \({\tau }_{0}\) :
-
Yield stress
- \(\tau \) :
-
Stress tensor
- \(\overrightarrow{\nu }\) :
-
Fluid velocity vector
- \(\dot{\gamma }\) :
-
Shear rate (s−1)
- \(\eta \) :
-
Dynamic viscosity (Pa s)
- \({\sigma }_{nn}\) :
-
Traction parallel to normal vector n̂
- \(\overline{\epsilon }\) :
-
Critical stenotic height
- \(\overline{\xi }\) :
-
Slope of tapering artery
- \(\nu \) :
-
Poisson’s ratio
References
Amiri MH, Keshavarzi A, Karimipour A, Bahiraei M, Goodarzi M, Esfahani JA (2019) A 3-D numerical simulation of non-Newtonian blood flow through femoral artery bifurcation with a moderate arteriosclerosis: investigating Newtonian/non-Newtonian flow and its effects on elastic vessel walls. Heat Mass Transf Stoffuebertragung. https://doi.org/10.1007/s00231-019-02583-4
Benjamin EJ et al (2019) Heart disease and stroke statistics-2019 update: a report from the American Heart Association. Circulation 139(10):e56–e66. https://doi.org/10.1161/CIR.0000000000000659
British Heart Foundation (2019) Heart & Circulatory Disease Statistics 2019—Cardiovascular Disease Statistics—BHF
Young DF (1968) Effect of a time-dependent stenosis on flow through a tube. J Manuf Sci Eng Trans ASME 90(2):248–254. https://doi.org/10.1115/1.3604621
Merrill EW, Benis AM, Gilliland ER, Sherwood TK, Salzman EW (1965) Pressure-flow relations of human blood in hollow fibers at low flow rates. J Appl Physiol 20(5):954–967. https://doi.org/10.1152/jappl.1965.20.5.954
Wang J et al (2019) Carotid bifurcation with tandem stenosis—a patient-specific case study combined in vivo imaging, in vitro histology and in silico simulation. Front Bioeng Biotechnol 7(November):1–11. https://doi.org/10.3389/fbioe.2019.00349
Suresh A, Rajan V (2019) Study of non-newtonian blood flow through arteries using openfoam. In: AIP Conf. Proc., vol 2134. https://doi.org/10.1063/1.5120211
Liu Y, Liu W (2020) Blood flow analysis in tapered stenosed arteries with the influence of heat and mass transfer. J Appl Math Comput 63(1–2):523–541. https://doi.org/10.1007/s12190-020-01328-5
Lopes D, Puga H, Teixeira JC, Teixeira SF (2019) Influence of arterial mechanical properties on carotid blood flow: comparison of CFD and FSI studies. Int J Mech Sci 160(June):209–218. https://doi.org/10.1016/j.ijmecsci.2019.06.029
Soares AA, Gonzaga S, Oliveira C, Simões A, Rouboa AI (2017) Computational fluid dynamics in abdominal aorta bifurcation: non-Newtonian versus Newtonian blood flow in a real case study. Comput Methods Biomech Biomed Eng 20(8):822–831. https://doi.org/10.1080/10255842.2017.1302433
Bhatia R, Vashisth S, Saini R (2016) Wall shear stress analysis in stenosed carotid arteries with different shapes of plaque. Int J Comput Appl 145(4):9–12. https://doi.org/10.5120/ijca2016910543
Tu C, Deville M (1996) Pulsatile flow of Non-Newtonian fluids through arterial stenoses. J Biomech 29(7):899–908. https://doi.org/10.1016/0021-9290(95)00151-4
Rathish Kumar BV, Naidu KB (1996) A pulsatile suspension flow simulation in a stenosed vessel. Math Comput Model 23(5):75–86. https://doi.org/10.1016/0895-7177(96)00013-1
Deplano V, Siouffi M (1999) Experimental and numerical study of pulsatile flows through stenosis: wall shear stress analysis. J Biomech 32(10):1081–1090. https://doi.org/10.1016/S0021-9290(99)00098-6
Nandakumar N, Sahu KC, Anand M (2015) Pulsatile flow of a shear-thinning model for blood through a two-dimensional stenosed channel. Eur J Mech B Fluids 49(PART A):29–35. https://doi.org/10.1016/j.euromechflu.2014.07.005
Nejad AA, Talebi Z, Cheraghali D, Shahbani-Zahiri A, Norouzi M (2018) Pulsatile flow of non-Newtonian blood fluid inside stenosed arteries: investigating the effects of viscoelastic and elastic walls, arteriosclerosis, and polycythemia diseases. Comput Methods Progr Biomed 154:109–122. https://doi.org/10.1016/j.cmpb.2017.11.016
Chakravarty S, Mandal PK (2000) Two-dimensional blood flow through tapered arteries under stenotic conditions. Int J Non Linear Mech 35(5):779–793. https://doi.org/10.1016/S0020-7462(99)00059-1
Akbar NS, Rahman SU, Ellahi R, Nadeem S (2014) Nano fluid flow in tapering stenosed arteries with permeable walls. Int J Therm Sci 85:54–61. https://doi.org/10.1016/j.ijthermalsci.2014.06.009
Chaturani P, Pralhad RN (1985) Blood flow in tapered tubes with biorheological applications. Biorheology 22(4):303–314. https://doi.org/10.3233/BIR-1985-22403
Lee KW, Xu XY (2002) Modelling of flow and wall behaviour in a mildly stenosed tube. Med Eng Phys 24(9):575–586. https://doi.org/10.1016/S1350-4533(02)00048-6
Ortiz JP, Bessa KL, Legendre DF, Hellmuth RAP (2006) Physiological pulsatile waveform through axisymmetric stenosed arteries: numerical simulation A. In: ABCM Symp. Ser. Bioeng., vol 1
Bloch EH (1962) A quantitative study of the hemodynamics in the living microvascular system. Am J Anat 110(2):125–153. https://doi.org/10.1002/aja.1001100204
Cheng AL, Pahlevan NM, Rinderknecht DG, Wood JC, Gharib M (2018) Experimental investigation of the effect of non-Newtonian behavior of blood flow in the Fontan circulation. Eur J Mech B/Fluids 68:184–192. https://doi.org/10.1016/j.euromechflu.2017.12.009
Shahid N (2018) Role of a structural parameter in modelling blood flow through a tapering channel. Bound Value Probl 2018(1):1–22. https://doi.org/10.1186/s13661-018-1001-3
Saqr KM, Mansour O, Tupin S, Hassan T, Ohta M (2019) Evidence for non-Newtonian behavior of intracranial blood flow from Doppler ultrasonography measurements. Med Biol Eng Comput 57(5):1029–1036. https://doi.org/10.1007/s11517-018-1926-9
Jung H, Choi JW, Park CG (2004) Asymmetric flows of non-Newtonian fluids in symmetric stenosed artery. Korea Aust Rheol J 16(2):101–108
Mehrabi M, Setayeshi S (2012) Computational fluid dynamics analysis of pulsatile blood flow behavior in modelled stenosed vessels with different severities. Math Probl Eng 2012:1–13. https://doi.org/10.1155/2012/804765
Nadeem S, Akbar NS, Hendi AA, Hayat T (2011) Power law fluid model for blood flow through a tapered artery with a stenosis. Appl Math Comput 217(17):7108–7116. https://doi.org/10.1016/j.amc.2011.01.026
Fisher C, Rossmann JS (2009) Effect of non-Newtonian behavior on hemodynamics of cerebral aneurysms. J Biomech Eng. https://doi.org/10.1115/1.3148470
Chen J, Lu XY, Wang W (2006) Non-Newtonian effects of blood flow on hemodynamics in distal vascular graft anastomoses. J Biomech 39(11):1983–1995. https://doi.org/10.1016/j.jbiomech.2005.06.012
Vimmr J, Jonášová A (2008) On the modelling of steady generalized Newtonian flows in a 3D coronary bypass. Eng Mech 15(3):193–203
Mandal PK (2005) An unsteady analysis of non-Newtonian blood flow through tapered arteries with a stenosis. Int J Non Linear Mech 40(1):151–164. https://doi.org/10.1016/j.ijnonlinmec.2004.07.007
Valencia A, Zarate A, Galvez M, Badilla L (2006) Non-Newtonian blood flow dynamics in a right internal carotid artery with a saccular aneurysm. Int J Numer Methods Fluids 50(6):751–764. https://doi.org/10.1002/fld.1078
Johnston BM, Johnston PR, Corney S, Kilpatrick D (2004) Non-Newtonian blood flow in human right coronary arteries: steady state simulations. J Biomech 37(5):709–720. https://doi.org/10.1016/j.jbiomech.2003.09.016
Buchanan JR, Kleinstreuer C, Comer JK (2000) Rheological effects on pulsatile hemodynamics in a stenosed tube. Comput Fluids 29(6):695–724. https://doi.org/10.1016/S0045-7930(99)00019-5
Ali N, Zaman A, Sajid M (2014) Unsteady blood flow through a tapered stenotic artery using Sisko model. Comput Fluids 101:42–49. https://doi.org/10.1016/j.compfluid.2014.05.030
Akbar NS, Nadeem S (2014) Carreau fluid model for blood flow through a tapered artery with a stenosis. Ain Shams Eng J 5(4):1307–1316. https://doi.org/10.1016/j.asej.2014.05.010
Liu B, Tang D (2019) Influence of distal stenosis on blood flow through coronary serial stenoses: a numerical study. Int J Comput Methods. https://doi.org/10.1142/S0219876218420033
Chakravarty S, Mandal PK (1994) Mathematical modelling of blood flow through an overlapping arterial stenosis. Math Comput Model 19(1):59–70. https://doi.org/10.1016/0895-7177(94)90116-3
Srivastava VP, Rastogi R (2010) Blood flow through a stenosed catheterized artery: effects of hematocrit and stenosis shape. Comput Math Appl 59(4):1377–1385. https://doi.org/10.1016/j.camwa.2009.12.007
Srikanth D, Ramana Reddy JV, Jain S, Kale A (2015) Unsteady polar fluid model of blood flow through tapered ω-shape stenosed artery: effects of catheter and velocity slip. Ain Shams Eng J 6(3):1093–1104. https://doi.org/10.1016/j.asej.2015.01.003
Abbas Z, Shabbir MS, Ali N (2017) Analysis of rheological properties of Herschel–Bulkley fluid for pulsating flow of blood in ω-shaped stenosed artery. AIP Adv. https://doi.org/10.1063/1.5004759
Turjman AS, Turjman F, Edelman ER (2014) Role of fluid dynamics and inflammation in intracranial aneurysm formation. Circulation 129(3):373–382. https://doi.org/10.1161/CIRCULATIONAHA.113.001444
Pedley TJ (1980) The fluid mechanics of large blood vessels. Cambridge University Press, Cambridge
Berger SA, Jou L-D (2000) Flows in stenotic vessels. Annu Rev Fluid Mech 32(1):347–382. https://doi.org/10.1146/annurev.fluid.32.1.347
McDonald DA (1960) Blood flow in arteries. Williams & Wilkins, Baltimore
Fung YC (1997) Biomechanics. Springer New York, New York
Perktold K, Resch M, Florian H (1991) Pulsatile Non-Newtonian flow characteristics in a three-dimensional human carotid bifurcation model. J Biomech Eng 113(4):464–475. https://doi.org/10.1115/1.2895428
Kumar D, Vinoth R, Raviraj A, Vijay Shankar CS (2017) Non-Newtonian and Newtonian blood flow in human aorta: a transient analysis. Biomed Res 28(7):3194–3203
Khanafer KM, Gadhoke P, Berguer R, Bull JL (2006) Modeling pulsatile flow in aortic aneurysms: effect of non-Newtonian properties of blood. Biorheology 43(5):661–679
Kim S (2002) A study of non-Newtonian viscosity and yield stress of blood in a scanning capillary-tube rheometer. Drexel Univ., vol. PhD Thesis
V. 5. 4. COMSOL Multiphysics®, “www.comsol.com,” Stockholm, Sweden, 2018. Accessed 30 Oct 2019. www.comsol.com/blogs.
Morris L, Delassus P, Grace P, Wallis F, Walsh M, McGloughlin T (2006) Effects of flat, parabolic and realistic steady flow inlet profiles on idealised and realistic stent graft fits through Abdominal Aortic Aneurysms (AAA). In: Medical engineering and physics, vol 28, no. 1 SPEC. ISS., pp 19–26. https://doi.org/10.1016/j.medengphy.2005.04.012
Shek TLT, Tse LW, Nabovati A, Amon CH (2012) Computational fluid dynamics evaluation of the cross-limb stent graft configuration for endovascular aneurysm repair. J Biomech Eng 134(12):121002. https://doi.org/10.1115/1.4007950
Matsuzaki Y, Ikeda T, Matsumoto T, Kitagawa T (1998) Experiments on steady and oscillatory flows at moderate reynolds numbers in a quasi-two-dimensional channel with a throat. J Biomech Eng 120(5):594–601. https://doi.org/10.1115/1.2834749
Cho SW, Kim SW, Sung MH, Rou KC, Ryou HS (2011) Fluid-structure interaction analysis on the effects of vessel material properties on blood flow characteristics in stenosed arteries under axial rotation. Korea Aust Rheol J 23(1):7–16. https://doi.org/10.1007/s13367-011-0002-x
Kawasaki R et al (2009) Retinal vessel diameters and risk of hypertension: The Multiethnic Study of Atherosclerosis. J Hypertens 27(12):2386–2393. https://doi.org/10.1097/HJH.0b013e3283310f7e
Acknowledgements
This study was supported by the National Research Foundation of Korea and funded by the Korean government (MSIP Grant Nos. 2020R1A2B5B02002512 and 2020R1A4A1018652).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ashraf, F., Park, C.W. Fluid–structure interaction analysis of non-Newtonian Herschel–Bulkley fluid viscosity model for pulsating flow of blood in ω-shaped stenosed arteries. Korea-Aust. Rheol. J. 34, 51–67 (2022). https://doi.org/10.1007/s13367-022-00025-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13367-022-00025-y