Abstract
Objective
To evaluate pulse oximetry for detection of congenital cyanotic heart disease in sick neonates using echocardiography as gold standard.
Methods
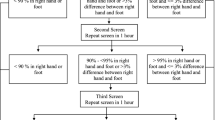
Pulse oximetry readings were taken at admission from 950 neonates from right upper limb and either foot with infant breathing room air. Pulse oximetry was considered abnormal if oxygen saturation at room air measured <90% or difference between right hand and foot was more than 3%. Persistent abnormality was considered positive result. Echocardiography was performed on all neonates with positive pulse oximetry (study group) and on one subsequent neonate with negative screen for each neonate with positive screen (controls).
Results
Pulse oximetry was positive in 210 neonates. It detected 20 out of 21 (95.2%) true positives. The sensitivity, specificity, positive predictive value, negative predictive value and odds ratio (95% CI) of pulse oximetry was 95.2%, 52.4 %, 9.5, 99.5 and 22 (5.3, 91.4), respectively.
Conclusion
Pulse oximetry screening is useful in detecting cyanotic heart diseases in sick newborns.
Similar content being viewed by others
References
Wren C, Reinhardt Z, Khwaja K. Twenty year trends in diagnosis of life threatening neonatal cardiovascular malformations. Arch Dis Child Fetal Neonatal Ed. 2008;93:F33–7.
Vaidyanathan B, Satish G, Mohannan ST, Sundaram KR, Warrier KKR, Kumar RK. Clinical screening for congenital heart disease at birth: A prospective study in a community hospital in Kerala. Indian Pediatr. 2011;48:25–30.
Bakshi KD, Vaidyanathan B, Sundaram KR, Roth SJ, Shivaprakasha K, Rao SG, et al. Determinants of early outcome after neonatal heart surgery in a developing country. J Thoracic Cardio Vascular Surgery. 2007;134:765–71.
Brown KL, Ridout DA, Hoskote A, Verhulst L, Ricci M, Bull C. Delayed diagnosis of congenital heart disease worsens preoperative condition and outcome of surgery in neonates. Heart. 2006;92:1298–302.
Kemper AR, Mahle WT, Martin GR, Cooley WC, Kumar P, Morrow WR, et al. Strategies for implementing screening for critical congenital heart disease. Pediatrics. 2011;128:e1259–67.
Sendelbach DM, Jackson GL, Lai SS, Fixler DE, Stehel EK, Engle WD. Pulse oximetry screening at 4 hours of age to detect critical congenital heart defects. Pediatrics. 2008;122:e815–20.
Ewer AK, Middleton LJ, Furmston AT, Bhoyar A, Daniels JP, Thangaratinam S, et al. Pulseox Study Group. Pulse oximetry screening for congenital heart defects in newborn infants (Pulseox): A test accuracy study. Lancet. 2011;378:785–94.
Arlettaz R, Bauschatz AS, Monkoff Messers B, Bauersfeld U. The contribution of pulse oximetry for early diagnosis of congenital heart disease in newborns. Eur J Pediatr. 2006;165:94–8.
de-Wahl Granelli A, Wennergren M, Sandberg K, Mellander M, Bejlum C, Inganas N, et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: A Swedish prospective screening study in 39, 821 newborns. BMJ. 2009;338: 3037.
Meberg A, Andreasson A, Brunvand L, Markestad T, Moster D, Nietsch L, et al. Pulse oximetry screening as a complimentary strategy to detect critical congenital heart defects. Acta Paediatr. 2009;98:682–6.
Koppel LR, Druschel CM, Carter T, Goldberg BE, Mehta PN, Talwar R, et al. Effectiveness of pulse oximetry screening for congenital heart disease in asymptomatic newborns. Pediatrics. 2003;111:451–5.
Thangaratinam S, Brown K, Zamora J, Khan KS, Ewer AK. Pulse oximetry screening for critical congenital heart defects in asymptomatic newborn babies: a systematic review and meta-analysis. Lancet. 2012;379:2459–64.
Haq FU, Jalil F, Hashmi S, Jumani MI, Imdad A, Jabeen M, et al. Risk factors predisposing to congenital heart defects. Ann Pediatr Cardiol. 2011;4:117–21.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mathur, N.B., Gupta, A. & Kurien, S. Pulse oximetry screening to detect cyanotic congenital heart disease in sick neonates in a neonatal intensive care unit. Indian Pediatr 52, 769–772 (2015). https://doi.org/10.1007/s13312-015-0714-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-015-0714-y