Abstract
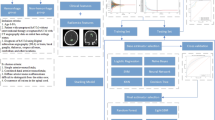
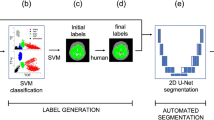
The diffuseness of brain arteriovenous malformations (bAVMs) is a significant factor in surgical outcome evaluation and hemorrhagic risk prediction. However, there are still predicaments in identifying diffuseness, such as the judging variety resulting from different experience and difficulties in quantification. The purpose of this study was to develop a machine learning (ML) model to automatically identify the diffuseness of bAVM niduses using three-dimensional (3D) time-of-flight magnetic resonance angiography (TOF-MRA) images. A total of 635 patients with bAVMs who underwent TOF-MRA imaging were enrolled. Three experienced neuroradiologists delineated the bAVM lesions and identified the diffuseness on TOF-MRA images, which were considered the ground-truth reference. The U-Net-based segmentation model was trained to segment lesion areas. Eight mainstream ML models were trained through the radiomic features of segmented lesions to identify diffuseness, based on which an integrated model was built and yielded the best performance. In the test set, the Dice score, F2 score, precision, and recall for the segmentation model were 0.80 [0.72–0.84], 0.80 [0.71–0.86], 0.84 [0.77–0.93], and 0.82 [0.69–0.89], respectively. For the diffuseness identification model, the ensemble-based model was applied with an area under the Receiver-operating characteristic curves (AUC) of 0.93 (95% CI 0.87–0.99) in the training set. The AUC, accuracy, precision, recall, and F1 score for the diffuseness identification model were 0.95, 0.90, 0.81, 0.84, and 0.83, respectively, in the test set. The ML models showed good performance in automatically detecting bAVM lesions and identifying diffuseness. The method may help to judge the diffuseness of bAVMs objectively, quantificationally, and efficiently.




Similar content being viewed by others
Data and Code Availability
The algorithm was published in “https://github.com/qizhaoaoe/AVM_diffuseness”. Deidentified data not published within this article will be made available to any qualified investigator upon request. To gain access, those requesting access to data will need to sign data access and use agreement. Data will be shared via a secure portal.
Abbreviations
- bAVM:
-
Brain arteriovenous malformation
- S-M grading:
-
Spetzler-Martin grading
- ML:
-
Machine learning
- TOF-MRA:
-
Time-of-flight magnetic resonance angiography
- ROC:
-
Receiver-operating characteristic
- AUC:
-
Area under the ROC curves
- DSA:
-
Digital subtraction angiography
- 3D:
-
Three-dimensional
- 2D:
-
Two-dimensional
- CNNs:
-
Convolutional neural networks
- LR:
-
Logistic regression
- SVM:
-
Support vector machine
- KNN:
-
K-nearest neighbor classification
- GBDT:
-
Gradient boosting decision tree
- SRS:
-
Stereotactic radiosurgery
References
Solomon RA, Connolly ES Jr. Arteriovenous malformations of the brain. N Engl J Med. 2017;376(19):1859–66. https://doi.org/10.1056/NEJMra1607407.
Lawton MT. The role of AVM microsurgery in the aftermath of a randomized trial of unruptured brain arteriovenous malformations. AJNR Am J Neuroradiol. 2015;36(4):617–9. https://doi.org/10.3174/ajnr.A4193.
Kandai S, Abdullah MS, Naing NN. Angioarchitecture of brain arteriovenous malformations and the risk of bleeding: an analysis of patients in northeastern Malaysia. Malay J Med Sci. 2010;17(1):44–8.
Tayebi Meybodi A, Lawton MT. Modern classification and outcome predictors of surgery in patients with brain arteriovenous malformations. J Neurosurg Sci. 2018;62(4):454–66. https://doi.org/10.23736/S0390-5616.18.04394-1.
Lawton MT, Kim H, McCulloch CE, Mikhak B, Young WL. A supplementary grading scale for selecting patients with brain arteriovenous malformations for surgery. Neurosurgery. 2010;66(4):702–13; discussion 713. https://doi.org/10.1227/01.Neu.0000367555.16733.E1.
Jiao Y, Lin F, Wu J, Li H, Wang L, Jin Z, Wang S, Cao Y. A supplementary grading scale combining lesion-to-eloquence distance for predicting surgical outcomes of patients with brain arteriovenous malformations. J Neurosurg. 2018;128(2):530–40. https://doi.org/10.3171/2016.10.Jns161415.
Chin LS, Raffel C, Gonzalez-Gomez I, Giannotta SL, McComb JG. Diffuse arteriovenous malformations: a clinical, radiological, and pathological description. Neurosurgery. 1992;31(5):863–8; discussion 868–869.
Du R, Keyoung HM, Dowd CF, Young WL, Lawton MT. The effects of diffuseness and deep perforating artery supply on outcomes after microsurgical resection of brain arteriovenous malformations. Neurosurgery. 2007;60(4):638–46; discussion 646–638. https://doi.org/10.1227/01.Neu.0000255401.46151.8a.
Braileanu M, Yang W, Caplan JM, Lin LM, Radvany MG, Tamargo RJ, Huang J. Interobserver agreement on arteriovenous malformation diffuseness using digital subtraction angiography. World Neurosurg. 2016;95:535-541.e533. https://doi.org/10.1016/j.wneu.2016.08.051.
Mossa-Basha M, Chen J, Gandhi D. Imaging of cerebral arteriovenous malformations and dural arteriovenous fistulas. Neurosurg Clin N Am. 2012;23(1):27–42. https://doi.org/10.1016/j.nec.2011.09.007.
Kim H, Abla AA, Nelson J, McCulloch CE, Bervini D, Morgan MK, Stapleton C, Walcott BP, Ogilvy CS, Spetzler RF, Lawton MT. Validation of the supplemented Spetzler-Martin grading system for brain arteriovenous malformations in a multicenter cohort of 1009 surgical patients. Neurosurgery. 2015;76(1):25–31; discussion 31–22; quiz 32–33. https://doi.org/10.1227/neu.0000000000000556.
LeCun Y, Bengio Y, Hinton G. Deep learning. Nature. 2015;521(7553):436–44. https://doi.org/10.1038/nature14539.
Wang T, Lei Y, Tian S, Jiang X, Zhou J, Liu T, Dresser S, Curran WJ, Shu HK, Yang X. Learning-based automatic segmentation of arteriovenous malformations on contrast CT images in brain stereotactic radiosurgery. Med Phys. 2019;46(7):3133–41. https://doi.org/10.1002/mp.13560.
Behboodi B, Rivaz H. Ultrasound segmentation using U-Net: learning from simulated data and testing on real data. Proc 41st Annu Int Conf IEEE Eng Med Biol Soc, (EMBC). 2019;6628–31. https://doi.org/10.1109/embc.2019.8857218.
Makropoulos A, Counsell SJ, Rueckert D. A review on automatic fetal and neonatal brain MRI segmentation. Neuroimage. 2018;170:231–48. https://doi.org/10.1016/j.neuroimage.2017.06.074.
Zaki M, Ghalwash A, Elkouny AA. CNN: a speaker recognition system using a cascaded neural network. Int J Neural Syst. 1996;7(2):203–12. https://doi.org/10.1142/s0129065796000178.
Krizhevsky A, Sutskever I, Hinton GE. ImageNet classification with deep convolutional neural networks. Communications of ACM. 2012;1097–105. https://doi.org/10.1145/3065386.
Ronneberger O, Fisher P, Brox T. U-net: convolutional networks for biomedical image segmentation. MICCAI 2015. 2015;234–41. https://doi.org/10.1007/978-3-319-24574-4_28.
Lee B, Yamanakkanavar N, Choi JY. Automatic segmentation of brain MRI using a novel patch-wise U-net deep architecture. PLoS ONE. 2020;15(8): e0236493. https://doi.org/10.1371/journal.pone.0236493.
Hu J, Shen L, Albanie S, Sun G, Wu E. Squeeze-and-excitation networks. IEEE Trans Pattern Anal Mach Intell. 2020;2011–23. https://doi.org/10.1109/TPAMI.2019.2913372.
He K, Zhang X, Ren S, Sun J, Recognition P. Deep residual learning for image recognition. CVPR. 2016;770–8. https://doi.org/10.1109/CVPR.2016.90.
Wong KCL, Moradi M, Tang H, Syeda-Mahmood T. 3D segmentation with exponential logarithmic loss for highly unbalanced object sizes. Cham: Springer International Publishing; 2018. p. 612–9.
Solmaz I, Secer HI, Tehlı O, Temız C, Izcı Y, Gonul E. Diffuse cerebral arteriovenous malformation. Turk Neurosurg. 2010;20(4):536–9. https://doi.org/10.5137/1019-5149.Jtn.2362-09.1.
Gillies RJ, Kinahan PE, Hricak H. Radiomics: images are more than pictures, they are data. Radiology. 2016;278(2):563–77. https://doi.org/10.1148/radiol.2015151169.
Oermann EK, Rubinsteyn A, Ding D, Mascitelli J, Starke RM, Bederson JB, Kano H, Lunsford LD, Sheehan JP, Hammerbacher J, Kondziolka D. Using a machine learning approach to predict outcomes after radiosurgery for cerebral arteriovenous malformations. Sci Rep. 2016;6:21161. https://doi.org/10.1038/srep21161.
Shi T, Jiang H, Zheng B. A stacked generalization U-shape network based on zoom strategy and its application in biomedical image segmentation. Comput Methods Programs Biomed. 2020;197:105678. https://doi.org/10.1016/j.cmpb.2020.105678.
Spears J, Terbrugge KG, Moosavian M, Montanera W, Willinsky RA, Wallace MC, Tymianski M. A discriminative prediction model of neurological outcome for patients undergoing surgery of brain arteriovenous malformations. Stroke. 2006;37(6):1457–64. https://doi.org/10.1161/01.Str.0000222937.30216.13.
Yu S, Yan L, Yao Y, Wang S, Yang M, Wang B, Zhuo Y, Ai L, Miao X, Zhao J, Wang DJ. Noncontrast dynamic MRA in intracranial arteriovenous malformation (AVM), comparison with time of flight (TOF) and digital subtraction angiography (DSA). Magn Reson Imaging. 2012;30(6):869–77. https://doi.org/10.1016/j.mri.2012.02.027.
Hadizadeh DR, Kukuk GM, Steck DT, Gieseke J, Urbach H, Tschampa HJ, Greschus S, Kovacs A, Mohlenbruch M, Bostroem A, Schild HH, Willinek WA. Noninvasive evaluation of cerebral arteriovenous malformations by 4D-MRA for preoperative planning and postoperative follow-up in 56 patients: comparison with DSA and intraoperative findings. AJNR Am J Neuroradiol. 2012;33(6):1095–101. https://doi.org/10.3174/ajnr.A2921.
Acknowledgements
We would like to acknowledge the support of Professor Jian-Min Li from the Department of Computer Science and Technology at Tsinghua University in the study design and article revision.
Funding
This study was supported by the National Natural Science Foundation of China (Grant No. 81901175, principal investigator, Yuming Jiao), the “National Key Research and Development Program of China during the 13th Five-Year Plan Period” (Grant No. 2016YFC1301803, principal investigator, Prof. Yong Cao, and Grant No. 2016YFC1301801, principal investigator, Prof. Shuo Wang).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in this study were in accordance with the ethical standards of the Institutional Review Board of Beijing Tiantan Hospital and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jiao, Y., Zhang, JZ., Zhao, Q. et al. Machine Learning-Enabled Determination of Diffuseness of Brain Arteriovenous Malformations from Magnetic Resonance Angiography. Transl. Stroke Res. 13, 939–948 (2022). https://doi.org/10.1007/s12975-021-00933-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-021-00933-1