Abstract
Background
Implants are preferred for replacement of missing teeth by the clinicians as well as the patients. Lesser alveolar bone density doesn’t preclude any individual for choosing this option but warrants for extra caution. Preclinical studies have explored the osteoinductive potential of statins, but results should be analyzed vigorously before implementing them in humans. There is no meta-analysis to document effect of statins on bone formation around implants in osteoporotic animals.
Methods and material
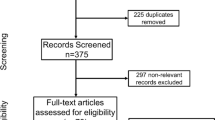
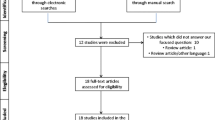
PubMed, Embase and Cochrane were searched for studies investigating the effect of statins on bone implant contact (BIC %), bone mineral density (BMD %) and bone volume (BV %) around implants at 2, 4 and 12 weeks. Meta-analysis was performed on subgroups with osteoporotic animals which were administered statins through different routes.
Results
Quantitative data from 12 studies showed favorable effect of statins on bone around implants. Positive difference was observed at 4 weeks in BIC (parenteral [SMD = 4.33 (2.89, 5.77); I2 = 3%)], BMD (local [SMD = 1.33 (0.51, 2.15); I2 = 0%] and BV (local [SMD = 1.58 (0.76, 2.40); I2 = 0%]. BIC [SMD = 1.40 (0.89, 1.90); I2 = 0%] and BV [SMD = 3.91 (2.33, 5.50); I2 = 43%] were higher in experimental group after 12 weeks of oral administration.
Conclusions
Statins can be investigated as potential bone graft materials to increase the predictability of osseointegration especially in osteoporotic individuals. Future research should focus to reproduce homogeneous data and conclusive recommendations which can be applied in clinical trials.






Similar content being viewed by others
References
Lioubavina-Hack N, Lang NP, Karring T (2006) Significance of primary stability for osseointegration of dental implants. Clin Oral Implant Res 17:244–250
Das S, Gurav S, Soni V, Ingle A, Mohanty BS, Chaudhari P et al (2018) Osteogenic nanofibrous coated titanium implant results in enhanced osseointegration. in vivo preliminary study in a rabbit model. Tissue Eng Regen Med 15:231–237
Ezirganli S, Polat S, Barıs E, Tatar I, Celik HH (2013) Comparative investigation of the effects of different materials used with a titanium barrier on new bone formation. Clin Oral Implant Res 24:312–319
Moriyama Y, Ayukawa Y, Ogino Y, Atsuta I, Koyano K (2008) Topical application of statin affects bone healing around implants. Clin Oral Implants Res 19:600–605
Mundy G, Garrett R, Harris S, Chan J, Chen D, Rossini G et al (1999) Stimulation of bone formation in vitro and in rodents by statins. Science 286:1946–1949
Gupta S, Del Fabbro M, Chang J (2019) The impact of simvastatin intervention on the healing of bone, soft tissue, and TMJ cartilage in dentistry: a systematic review and meta-analysis. Int J Implant Dent 5:17
Başarir K, Erdemli B, Can A, Erdemli E, Zeyrek T (2009) Osseointegration in arthroplasty: can simvastatin promote bone response to implants? Int Orthop 33:855–859
Rogers MJ (2000) Statins: lower lipids and better bones? Nat Med 6:21–23
Li X, Wu F, Zhang Y, Yang J, Shinohara A, Kagami H (2016) Discontinuation of simvastatin leads to a rebound phenomenon and results in immediate peri-implant bone loss. Clin Exp Dent Res 2:65–72
Stone PW (2002) Popping the (PICO) question in research and evidence-based practice. Appl Nurs Res 15:197–198
Apostu D, Lucaciu O, Mester A, Oltean-Dan D, Gheban D, Rares Ciprian Benea H (2020) Tibolone, alendronate, and simvastatin enhance implant osseointegration in a preclinical in vivo model. Clin Oral Implant Res 31:655–668
Ayukawa Y, Okamura A, Koyano K (2004) Simvastatin promotes osteogenesis around titanium implants. Clin Oral Implant Res 15:346–350
Ayukawa Y, Ogino Y, Moriyama Y, Atsuta I, Jinno Y, Kihara M et al (2010) Simvastatin enhances bone formation around titanium implants in rat tibiae. J Oral Rehabil 37:123–130
Du Z, Chen J, Yan F, Xiao Y (2009) Effects of Simvastatin on bone healing around titanium implants in osteoporotic rats. Clin Oral Implant Res 20:145–150
Dundar S, Bozoglan A (2020) Evaluation of the effects of topically applied simvastatin on titanium implant osseointegration. J Oral Biol Craniofac Res 10:149–152
Fang W, Zhao S, He F, Liu L, Yang G (2015) Influence of simvastatin-loaded implants on osseointegration in an ovariectomized animal model. Biomed Res Int 2015:831504
Fu X, Tan J, Sun CG, Leng HJ, Xu YS, Song CL (2016) Intraosseous injection of simvastatin in poloxamer 407 hydrogel improves pedicle-screw fixation in ovariectomized minipigs. J Bone Joint Surg Am 98:1924–1932
Kwon YD, Yang DH, Lee DW (2015) A titanium surface-modified with nano-sized hydroxyapatite and simvastatin enhances bone formation and osseointegration. J Biomed Nanotechnol 11:1007–1015
Liu H, Li W, Liu C, Tan J, Wang H, Hai B et al (2016) Incorporating simvastatin/poloxamer 407 hydrogel into 3D-printed porous Ti6Al4V scaffolds for the promotion of angiogenesis, osseointegration and bone ingrowth. Biofabrication 8:045012
Liu X, Zhang Y, Li S, Wang Y, Sun T, Li Z et al (2016) Study of a new bone-targeting titanium implant-bone interface. Int J Nanomed 11:6307–6324
Mansour G, Al Ashwah A, Koura A (2014) Evaluation of simvastatin grafting around immediate dental implants in dogs. Implant Dent 23:195–199
Masuzaki T, Ayukawa Y, Moriyama Y, Jinno Y, Atsuta I, Ogino Y et al (2010) The effect of a single remote injection of statin-impregnated poly (lactic-co-glycolic acid) microspheres on osteogenesis around titanium implants in rat tibia. Biomaterials 31:3327–3334
Monjo M, Rubert M, Wohlfahrt JC, Ronold HJ, Ellingsen JE, Lyngstadaas SP (2010) In vivo performance of absorbable collagen sponges with rosuvastatin in critical-size cortical bone defects. Acta biomater 6:1405–1412
Moriyama Y, Ayukawa Y, Ogino Y, Atsuta I, Todo M, Takao Y et al (2010) Local application of fluvastatin improves peri-implant bone quantity and mechanical properties: a rodent study. Acta Biomater 6:1610–1618
Nyan M, Hao J, Miyahara T, Noritake K, Rodriguez R, Kasugai S (2014) Accelerated and enhanced bone formation on novel simvastatin-loaded porous titanium oxide surfaces. Clin Implant Dent Relat Res 16:675–683
Pauly S, Back DA, Kaeppler K, Haas NP, Schmidmaier G, Wildemann B (2012) Influence of statins locally applied from orthopedic implants on osseous integration. BMC Musculoskelet Disord 13:208
Stadlinger B, Korn P, Todtmann N, Eckelt U, Range U, Burki A et al (2013) Osseointegration of biochemically modified implants in an osteoporosis rodent model. Eur Cell Mater 25:326–340
Tan J, Yang N, Fu X, Cui Y, Guo Q, Ma T et al (2015) Single-dose local simvastatin injection improves implant fixation via increased angiogenesis and bone formation in an ovariectomized rat model. Med Sci Monit 21:1428–1439
Tao ZS, Zhou WS, Tu KK, Huang ZL, Zhou Q, Sun T et al (2015) The effects of combined human parathyroid hormone (1–34) and simvastatin treatment on osseous integration of hydroxyapatite-coated titanium implants in the femur of ovariectomized rats. Injury 46:2164–2169
Tao ZS, Zhou WS, Tu KK, Huang ZL, Zhou Q, Sun T et al (2016) The effects of combined human parathyroid hormone (1–34) and simvastatin treatment on the interface of hydroxyapatite-coated titanium rods implanted into osteopenic rats’ femurs. J Mater Sci Mater Med 27:43
Xu R, Shi G, Xu L, Gu Q, Fu Y, Zhang P, Cheng J et al (2018) Simvastatin improves oral implant osseointegration via enhanced autophagy and osteogenesis of BMSCs and inhibited osteoclast activity. J Tissue Eng Regen Med 12:1209–1219
Yang G, Song L, Guo C, Zhao S, Liu L, He F (2012) Bone responses to simvastatin-loaded porous implant surfaces in an ovariectomized model. Int J Oral Maxillofac Implant 27:369–374
Zhao S, Wen F, He F, Liu L, Yang G (2014) In vitro and in vivo evaluation of the osteogenic ability of implant surfaces with a local delivery of simvastatin. Int J Oral Maxillofac Implant 29:211–220
Zhao B, Li X, Xu H, Jiang Y, Wang D, Liu R (2020) Influence of simvastatin-strontium-hydroxyapatite coated implant formed by micro-arc oxidation and immersion method on osteointegration in osteoporotic rabbits. Int J Nanomed 15:1797–1807
Hooijmans CR, Rovers MM, de Vries RBM, Leenaars M, Ritskes-Hoitinga M, Langendam MW (2014) SYRCLE’s risk of bias tool for animal studies. BMC Med Res Methodol 14:43
Kilkenny C, Browne WJ, Cuthill IC, Emerson M, Altman DG (2010) Improving bioscience research reporting: the ARRIVE guidelines for reporting animal research. PLoS Biol 8:e1000412
Schwarz F, Iglhaut G, Becker J (2012) Quality assessment of reporting of animal studies on pathogenesis and treatment of peri-implant mucositis and peri-implantitis. a systematic review using the ARRIVE guidelines. J Clin Periodontol 39:63–72
Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) (2021) Cochrane handbook for systematic reviews of interventions version 6.2 (updated February 2021). Cochrane, 2021 (Available from www.training.cochrane.org/handbook)
Kellesarian SV, Al Amri MD, Al-Kheraif AA, Ghanem A, Malmstrom H, Javed F (2017) Efficacy of local and systemic statin delivery on the osseointegration of implants: a systematic review. Int J Oral Maxillofac Implants 32:497–506
Moraschini V, Almeida DCF, Calasans-Maia JA, Diuana Calasans-Maia M (2018) The ability of topical and systemic statins to increase osteogenesis around dental implants: a systematic review of histomorphometric outcomes in animal studies. Int J Oral Maxillofac Surg 47:1070–1078
Sendyk DI, Deboni MC, Pannuti CM, Naclério-Homem MG, Wennerberg A (2016) The influence of statins on osseointegration: a systematic review of animal model studies. J Oral Rehabil 43:873–882
Stechow DV, Fish S, Yahalom D, Bab I, Chorev M, Muller R et al (2003) Does simvastatin stimulate bone formation in vivo? BMC Musculoskelet Disord 4:8
Schachter M (2005) Chemical, pharmacokinetic and pharmacodynamic properties of statins: an update. Fundam Clin Pharmacol 19:117–125
Villar CC, Huynh-Ba G, Mills MP, Cochran DL (2011) Wound healing around dental implants. Endod Topics 5:44–62
Parithimarkalaignan S, Padmanabhan TV (2013) Osseointegration: an update. J Indian Prosthodont Soc 13:2–6
Wong RW, Rabie AB (2005) Early healing pattern of statin-induced osteogenesis. Br J Oral Maxillofac Surg 43:46–50
Chou R, Dana T, Blazina I, Daeges M, Jeanne TL (2016) Statins for prevention of cardiovascular disease in adults: evidence report and systematic review for the us preventive services task force. JAMA 316(19):2008. https://doi.org/10.1001/jama.2015.15629
Kiliç E, Ozeç I, Yeler H, Korkmaz A, Ayas B, Gumuş C (2008) Effects of simvastatin on mandibular distraction osteogenesis. J Oral Maxillofac Surg 66:2233–2238
Gutierrez GE, Lalka D, Garrett IR, Rossini G, Mundy GR (2006) Transdermal application of lovastatin to rats causes profound increases in bone formation and plasma concentrations. Osteoporos Int 17:1033–1042
Rutledge J, Schieber MD, Chamberlain JM, Byarlay M, Killeen AC, Giannini PJ et al (2011) Simvastatin application to augment facial jawbone in a dog model: pilot study. J Periodontol 82:597–605
Wang JW, Xu SW, Yang DS, Lv RK (2007) Locally applied simvastatin promotes fracture healing in ovariectomized rat. Osteoporos Int 18:1641–1650
Maritz FJ, Conradie MM, Hulley PA, Gopal R, Hough S (2001) Effect of statins on bone mineral density and bone histomorphometry in rodents. Arterioscler Thromb Vasc Biol 21:1636–1641
Stein D, Lee Y, Schmid MJ, Killpack B, Genrich MA, Narayana N et al (2005) Local simvastatin effects on mandibular bone growth and inflammation. J Periodontol 76:1861–1870
da Silva Mello AS, dos Santos PL, Marquesi A, Queiroz TP, Margonar R, de Souza Faloni AP (2016) Some aspects of bone remodeling around dental implants. Rev Clín Periodoncia Implantol Rehabil Oral. https://doi.org/10.1016/j.piro.2015.12.001
Garg S, Pradeep AR (2017) 1.2% Rosuvastatin and 1.2% atorvastatin gel local drug delivery and redelivery in the treatment of class II furcation defects: a randomized controlled clinical trial. J Periodontol 88:259–265
Martande S, Kumari M, Pradeep AR, Pal Singh S, Kumar Suke D (2017) Comparative evaluation of efficacy of subgingivally delivered 1.2% atorvastatin and 1.2% simvastatin in the treatment of intrabony defects in chronic periodontitis: a randomized controlled trial. J Dent Res Dent Clin Dent Prospect 11:18–25
Kumari M, Martande SS, Pradeep AR, Naik SB (2016) Efficacy of Subgingivally delivered 1.2% atorvastatin in the treatment of chronic periodontitis in patients with type 2 diabetes mellitus: a randomized controlled clinical trial. J Periodontol 87:1278–1285
Rosenberg DR, Vega MP, Chaparro A, Kernitsky JR, Andrade CX, Violant D et al (2019) Association between the use of statins and periodontal status: a review. Rev Clín Periodoncia ImplantolRehabil Oral 12:41–46
Pradeep AR, Priyanka N, Kalra N, Naik SB, Singh SP, Martande S (2012) Clinical efficacy of subgingivally delivered 1.2-mg simvastatin in the treatment of individuals with class II furcation defects: a randomized controlled clinical trial. J Periodontol 83:1472–1479
Ranjan R, Patil SR, Veena HR (2017) Effect of in-situ application of simvastatin gel in surgical management of osseous defects in chronic periodontitis—a randomized clinical trial. J Oral BiolCraniofac Res 7:113–118
Rath A, Mahenra J, Thomas L, Sandhu M, Namasi A, Ramakrishna T (2012) A clinical, radiological and IL-6 evaluation of subgingivally delivered simvastatin in the treatment of chronic periodontitis. Int J Drug Deliv 4:70
Pankaj D, Sahu I, Kurian IG, Pradeep AR (2018) Comparative evaluation of subgingivally delivered 1.2% rosuvastatin and 1% Metformin gel in treatment of intrabony defects in chronic periodontitis: a randomized controlled clinical trial. J Periodontol 89:1318–1325
Meisel P, Kroemer HK, Nauck M, Holtfreter B, Kocher T (2014) Tooth loss, periodontitis, and statins in a population-based follow-up study. J Periodontol 85:e160–e168
Sommer NG, Hahn D, Okutan B, Marek R, Weinberg AM (2019) Animal models in orthopedic research: the proper animal model to answer fundamental questions on bone healing depending on pathology and implant material. In animal models in medicine and biology. Intech Open. https://doi.org/10.5772/intechopen.89137
Hohlweg-Majert B, Schmelzeisen R, Pfeiffer BM, Schneider E (2006) Significance of osteoporosis in craniomaxillofacial surgery: a review of the literature. Osteoporos Int 17(2):167–179
Taguchi A, Tsuda M, Ohtsuka M, Kodama I, Sanada M, Nakamoto T et al (2006) Use of dental panoramic radiographs in identifying younger postmenopausal women with osteoporosis. Osteoporos Int 17(3):387–394
Ohtsuki H, Kawakami M, Kawakami T, Takahashi K, Kirita T, Komasa Y (2017) Risk of osteoporosis in elderly individuals attending a dental clinic. Int Dent J 67:117–122
Acknowledgements
Authors acknowledge the contribution of Dr. Vedha V.P.K. and Dr. Shweta Sharda for cross-checking all the values used for calculations in the meta-analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that we do not have any financial interest in the companies whose materials are included in this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pruthi, G., Mahajan, R., Gupta, A. et al. The Effects of Statins on Bone Formation Around Implants Placed in Animal Bones: A Systematic Review and Meta-Analysis. J. Maxillofac. Oral Surg. 22, 265–286 (2023). https://doi.org/10.1007/s12663-023-01873-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12663-023-01873-z