Abstract
Purpose
The objective of this study was to determine whether the magnitude of the peripheral inflammatory response to cardiovascular surgery is associated with increases in blood–brain barrier (BBB) permeability as reflected by changes in cerebrospinal fluid (CSF)/plasma S100B concentrations.
Methods
We conducted a secondary analysis from a prospective cohort study of 35 patients undergoing elective thoracoabdominal aortic aneurysm repair with (n = 17) or without (n = 18) cardiopulmonary bypass (CPB). Plasma and CSF S100B, interleukin-6 (IL-6), and albumin concentrations were measured at baseline (C0) and serially for up to five days.
Results
Following CPB, the median [interquartile range] plasma S100B concentration increased from 58 [32–88] pg·mL-1 at C0 to a maximum concentration (Cmax) of 1,131 [655–1,875] pg·mL-1 over a median time (tmax) of 6.3 [5.9–7.0] hr. In the non-CPB group, the median plasma S100B increased to a lesser extent. There was a delayed increase in CSF S100B to a median Cmax of 436 [406–922] pg·mL-1 in the CPB group at a tmax of 23.7 [18.5–40.2] hr. In the non-CPB group, the CSF concentrations were similar at all time points. In the CPB group, we did not detect significant correlations between plasma and CSF S100B with plasma IL-6 [r = 0.52 (95% confidence interval [CI], -0.061 to 0.84)] and CSF IL-6 [r = 0.53 (95% CI, -0.073 to 0.85)] concentrations, respectively. Correlations of plasma or CSF S100B levels with BBB permeability were not significant.
Conclusion
The lack of parallel increases in plasma and CSF S100B following CPB indicates that S100B may not be a reliable biomarker for BBB disruption after thoracoabdominal aortic aneurysm repair employing CPB.
Trial registration
www.clinicaltrials.gov (NCT00878371); registered 7 April 2009.
Résumé
Objectif
L’objectif de cette étude était de déterminer si l’intensité de la réponse inflammatoire périphérique à la chirurgie cardiovasculaire était associée à une augmentation de la perméabilité de la barrière hémato-encéphalique (BHE), telle que reflétée par des changements dans les concentrations de S100B dans le liquide céphalorachidien (LCR) et le plasma.
Méthode
Nous avons mené une analyse secondaire à partir d’une étude de cohorte prospective portant sur 35 patients bénéficiant d’une réparation élective d’un anévrisme aortique thoraco-abdominal avec (n = 17) ou sans (n = 18) circulation extracorporelle (CEC). Les concentrations plasmatiques et dans le LCR de S100B, d’interleukine-6 (IL-6) et d’albumine ont été mesurées au départ (C0) et en série jusqu’à cinq jours.
Résultats
Après la CEC, la concentration médiane [écart interquartile] plasmatique de S100B est passée de 58 [32–88] pg·mL-1 au départ (C0) à une concentration maximale (Cmax) de 1131 [655–1875] pg·mL-1 sur une période médiane (tmax) de 6,3 [5,9–7,0] h. Dans le groupe sans CEC, la concentration plasmatique médiane de S100B a augmenté dans une moindre mesure. Il y a eu une augmentation retardée de S100B dans le LCR à une Cmax médiane de 436 [406–922] pg·mL-1 dans le groupe CEC à une tmax de 23,7 [18,5–40,2] h. Dans le groupe sans CEC, les concentrations dans le LCR étaient similaires à tous les moments. Dans le groupe CEC, nous n’avons pas détecté de corrélations significatives entre la concentration de S100B dans le plasma et le LCR avec les concentrations plasmatiques d’IL-6 [r = 0,52 (intervalle de confiance [IC] à 95 %, -0,061 à 0,84)] et d’IL-6 dans le LCR [r = 0,53 (IC 95 %, -0,073 à 0,85)], respectivement. Les corrélations entre les taux plasmatiques ou dans le LCR de S100B et la perméabilité de la BHE n’étaient pas significatives.
Conclusion
L’absence d’augmentations parallèles de la concentration de S100B dans le plasma et le LCR après la CEC indique que la S100B pourrait ne pas être un biomarqueur fiable de la perturbation de la BHE après une réparation d’anévrisme aortique thoraco-abdominal sous CEC.
Enregistrement de l’étude
www.clinicaltrials.gov (NCT00878371); enregistrée le 7 avril 2009.
Similar content being viewed by others
S100B is a calcium-binding protein that is highly expressed in the brain and found within a variety of cells including astrocytes, Schwann cells, and certain neuronal cells.1,2 Increases in the serum concentration of S100B are thought to be indicative of glial or neuronal injury and blood–brain barrier (BBB) disruption.3,4 Surgical procedures, especially those conducted during cardiopulmonary bypass (CPB), trigger systemic inflammation, as evidenced by increases in the plasma levels of pro-inflammatory cytokines such as interleukin-6 (IL-6).5,6,7,8,9 This may lead to disruption of the BBB and the appearance of S100B in the circulation.6,10,11,12,13 Increases in serum S100B after cardiovascular surgery have been reported to be associated with an increased risk of radiologically diagnosed cerebral damage, postoperative neurologic disorders, and late mortality.14,15,16,17
Nevertheless, the role of S100B as a serum biomarker for increased BBB permeability and neurologic injury after cardiovascular surgery remains controversial for several reasons. First, some have suggested that the increase in S100B after cardiovascular surgery-associated neurologic injury occurs too late to allow for early detection and treatment.18 Second, some studies have suggested that most post-surgical spikes in serum S100B arise from extracerebral instead of cerebral sources including the surgical incision, sternal bone marrow, adipose tissue, skeletal muscle, and the heart into mediastinal blood.19,20,21,22 Additionally, the failure to include measurements of cerebrospinal fluid (CSF) S100B in some studies may have precluded their assessment of the potential central nervous system (CNS) contribution to the post-surgical increase in the serum concentration of this protein. Despite these uncertainties, S100B continues to be evaluated as a systemic biomarker of adverse neurologic outcomes in a number of settings including following cardiovascular surgery, cardiac arrest, stroke, infection, and traumatic brain injury.4,23,24,25,26,27,28,29,30
To address this knowledge gap, we studied patients undergoing open and endovascular thoracoabdominal aortic aneurysm (TAA) repair. We studied these patients because the onset of the surgical inflammatory response is known (incision) and patients are routinely fitted with a lumbar CSF drain and an arterial catheter, allowing simultaneous CSF and plasma S100B measurements to be obtained in the perioperative and postoperative periods.13 The primary study objective was to determine whether the magnitude of the peripheral inflammatory response to cardiovascular surgery was associated with increases in BBB permeability and CSF/plasma S100B concentrations. We hypothesized that: 1) CSF S100B concentrations would be higher in patients undergoing TAA repair with CPB vs without CPB; 2) higher CSF S100B concentrations would be related to elevated plasma levels of the pro-inflammatory cytokine IL-6 as a marker for the peripheral inflammatory response; and 3) S100B concentrations in the CSF would parallel those in plasma because of an associated increase in BBB permeability.
Methods
Design
We conducted a secondary analysis from a prospective cohort study designed to evaluate whether surgically induced inflammation is associated with altered distribution of morphine and its metabolites across the BBB.13 The study was registered with ClinicalTrials.gov (identifier NCT00878371), was approved by the Capital District Health Authority Research Ethics Board a priori (ethics ID: CDHA –RS/2010-004), and was reported according to STROBE guidelines.31 The principal investigators (K.B.G., R.I.H.) had complete access to the study data. The authors analyzed and interpreted the data and each author was responsible for authorship of the manuscript and verification of the completeness and accuracy of the data.
Study participants and interventions
Between May 2009 and February 2013, 36 consecutive adult patients presenting to the Queen Elizabeth II Health Sciences Centre in Halifax, NS, Canada for elective repair of a TAA were screened for study eligibility. We included consecutive adults undergoing elective endovascular or open surgical repair of these aneurysms with or without CPB who required insertion of a lumbar CSF drain and provided written informed consent. Lumbar CSF drains are routinely placed in these patients to reduce the risk of spinal cord ischemia. Samples of CSF (5–15 mL) and blood (5 mL) were taken from all participants immediately prior to incision, at wound closure, and then every six hours for five days or until the lumbar CSF drain was removed for clinical reasons. Participants undergoing open surgery with CPB also had CSF and blood samples obtained immediately prior to initiation of CPB and immediately following return of native circulation post-CPB. Cerebrospinal fluid and plasma samples were divided into working aliquots and stored at –70°C prior to analysis. Further details of the study participants and interventions have been described.13
S100B, IL-6, and albumin determination
S100B in CSF was determined using a BioVendor S100B enzyme-linked immunosorbent assay (ELISA) kit (BioVendor LLC, Candler, NC, USA). For sample compatibility reasons, a Millipore S100B ELISA kit (Millipore, St. Charles, MO, USA) was used for S100B measurements in plasma. The rationale and methodology for measurement of CSF and plasma IL-6 as markers of inflammation and CSF and plasma albumin as markers of BBB integrity have previously been described.13
Data analysis
The size of this study was based on a power calculation for the primary study, which utilized the same participants and samples to evaluate whether surgically induced inflammation was associated with altered distribution of morphine and its metabolites across the BBB.13 The primary analysis compared subjects that underwent open repair with CPB (CPB group) vs those that underwent open or endovascular repair without CPB (non-CPB group). We expected a greater systemic inflammatory response and greater S100B plasma concentrations in participants undergoing open repair with CPB vs other types of repair.6,32,33 In a secondary analysis, we compared participants who underwent open repair with or without CPB vs endovascular repair (Electronic Supplementary Material [ESM]; eTables 2–4 and 11–16 and eFigs 2–4).
To compare the systemic (plasma) and central (CSF) S100B release patterns within each group, the median and interquartile range (IQR) of plasma and CSF S100B concentrations (pg·mL-1) and the S100B CSF/plasma ratio were determined for each time point and plotted against the average sample collection time. Within each group, the plasma and CSF S100B concentrations and CSF/plasma S100B ratio at each time point were compared across time using the Kruskal–Wallis test. For significant results (P < 0.01), pairwise comparisons were then made for baseline values (time 0) vs all other time points using the Wilcoxon-Mann–Whitney test with a Bonferroni correction for multiple comparisons.
For each participant, we recorded patient characteristics and surgical parameters and the baseline (C0) and peak concentration (Cmax) of plasma and CSF S100B and IL-6 as measures of the magnitude of the central and systemic S100B and IL-6 responses, respectively. The time (tmax) required to reach Cmax for S100B and IL-6 in the plasma and CSF provided a measure of the onset of the responses. As a measure of the overall central and peripheral exposures to S100B and IL-6 over time, we used an area under the curve (AUC) analysis as previously described.13,34 For this analysis, the plasma and CSF AUCs between each two adjacent serial time points (interval AUCs) for IL-6 and S100B were calculated using the formula: Cavg interval/Δt, where Cavg interval is the average concentration determined from the adjacent serial time points and Δt is the time elapsed between the adjacent serial time points. The interval AUCs were then summed to provide the cumulative AUC from 0 to each serial time point, up to the last measured time point for each participant. The cumulative AUC values for each serial time point were then divided by the corresponding time to provide an average hourly plasma or CSF exposure (pg·mL-1).
To assess passive permeability of the BBB, the CSF/plasma albumin ratio was determined for each serial time point using the formula CSF albumin (g·L-1) × 1000/plasma albumin (g·L-1).35 Similar to that described for S100B and IL-6 analysis, the baseline (R0), maximal (Rmax), average CSF/plasma albumin ratio, and time to reach the Rmax were determined. Each variable was compared between the CPB and non-CPB groups using a Wilcoxon-Mann–Whitney test. Within-subjects comparisons of S100B Cmax and S100B average exposure in plasma vs CSF and IL-6 (C0 vs Cmax) and albumin (R0 vs Rmax) in plasma and CSF (i.e., two related samples) were compared using Wilcoxon signed-ranks tests. For each variable, the calculated P value and corresponding 95% confidence interval (CI) were adjusted for the number of total comparisons using Bonferroni correction as described in the Figure and Table legends. Between-subjects weighted (for the number of paired observations) Spearman correlations of the average plasma and CSF S100B exposure with average plasma and CSF IL-6 exposures and the average CSF/plasma albumin ratios were calculated as per published methodology.13,36 The following scale was used to describe correlations as weak positive (0 to 0.3) or weak negative (0 to -0.3), moderate positive (0.3 to 0.7) or moderate negative (-0.3 to -0.7), and strong positive (0.7 to 1) or strong negative (-0.7 to -1.0).37 Adjusted 95% CIs for Spearman correlations were calculated using a custom program created within the SPSS syntax editor (https://youtu.be/gKHgCq5E864).38
P values between 0.01 and 0.05 may be significant and P values less than 0.01 were considered significant. All statistical analyses were performed using IBM SPSS® Statistics version 26 (IBM Corporation, Armonk, NY, USA). All figures were created using GraphPad Prism version 9.1.2 (GraphPad Software, San Diego, CA, USA).
Results
Patients
The flow of participants through the study is summarized in Fig. 1. Baseline characteristics of the patients were similar (Table 1). Some participants were excluded from some but not all analyses. One non-CPB participant was excluded from the S100B analysis because of insufficient plasma and CSF to measure S100B. One CPB participant had plasma samples only and was excluded from the CSF S100B, IL6, and albumin analyses. Two non-CPB participants had undetectable albumin concentrations in all CSF samples and were excluded from the albumin analyses, and two non-CPB participants had undetectable IL-6 concentrations in all plasma and CSF samples and were excluded from the IL-6 analysis.
Measures of systemic and central inflammation and BBB permeability
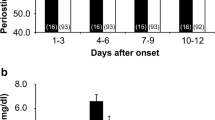
A summary of the post-surgical systemic and central inflammatory responses and BBB permeability in the CPB vs non-CPB groups is provided in Table 2. Systemic and central inflammation was evident in both groups as shown by significantly higher plasma and CSF peak (Cmax) vs baseline concentrations of IL-6 in the postoperative phase. Plasma IL-6 Cmax was significantly higher in the CPB vs non-CPB group. The overall systemic and central inflammatory responses may also be more robust in the CPB vs non-CPB group as determined by higher average IL-6 exposures in the plasma and CSF compartments. The CSF/plasma albumin ratio increased significantly in the early postoperative period in both groups relative to the baseline, suggesting mechanical BBB disruption early after surgery.
S100B plasma and CSF concentrations vs time
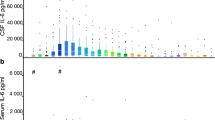
Following CPB, the median [IQR] plasma S100B concentration increased from 58 [32–88] pg·mL-1 at C0 to a maximum concentration (Cmax) of 1,131 [655–1,875] pg·mL-1 over a median time (tmax) of 6.3 [5.9–7.0] hr (Fig. 2A). In the non-CPB group, the median plasma S100B increased to a much lower extent (approximately two-fold in the immediate postoperative period) over a span of approximately one hour. In the CPB group, there was a small (1.3–1.4-fold) but significant increase in CSF S100B at the later intensive care unit recovery time points compared with baseline (Fig. 2B). In the non-CPB group, the median CSF S100B concentration was similar at all time points.
The effect of cardiovascular surgery on S100B plasma and CSF concentrations vs time. Plasma (A) and CSF (B) S100B concentrations and the CSF/plasma S100B ratio (C) were measured in participants undergoing open surgical procedures with CPB (CPB group) or in participants undergoing endovascular or open surgical procedures without CPB (non-CPB group). Each symbol represents the median concentration, and the error bars denote the IQR. *P < 0.05 may be different and **P < 0.01 as well as ***P < 0.001 are significantly different compared the within group baseline control value at time 0 (Wilcoxon-Mann–Whitney test with Bonferroni adjustments for 8 [CPB] or 7 [non-CPB] multiple comparisons). The adjusted P values for each comparison are listed in ESM, eTables 5 and 6. CPB = cardiopulmonary bypass; CSF = cerebrospinal fluid; IQR = interquartile range.
Relative to the median baseline ratio of 5.3 [3.4–7.7], the CSF/plasma S100B ratio dropped significantly to 0.33 [0.24–0.61] at the post-CPB time point and remained significantly reduced in the early postoperative period in the CPB group (Fig. 2C). In the non-CPB group there was a smaller reduction in the CSF/plasma S100B ratio to 2.5 [1.6–8.6] and 3.2 [1.7–5.3] at time points three and four, respectively, in the immediate postoperative period compared with baseline 5.8 [4.7–11.5].
The plasma S100B Cmax, but not the CSF S100B Cmax, was significantly higher in the CPB vs non-CBP group (Fig. 3A). In the CPB group only, the CSF S100B tmax was significantly longer than the plasma S100B tmax (Fig. 3B). Similar to the plasma and CSF S100B Cmax values, the average plasma S100B exposure, but not the average CSF S100B exposure, was higher in the CPB group compared with the non-CPB group (Fig. 3C). Consistent with this, the median S100B CSF/plasma ratio was significantly lower in the CPB vs non-CPB groups (Fig. 3D).
Comparison of CSF and plasma S100B exposures in CPB vs non-CPB surgical groups. Plasma and CSF S100B Cmax (A), tmax (B), average S100B exposure (C), and the median S100B CSF/plasma ratios (D) are shown for the CPB vs the non-CPB group. For each measured parameter, Tukey box plots were used to show the mean (+), median (middle line), IQR (outer lines), 1.5 × the IQR (error bars) and outlier values that were greater than 1.5 × IQR (filled circles). Within each group, the S100B Cmax, tmax, and average exposure in the plasma vs the CSF were compared by Wilcoxon signed-ranks test. Each reported variable was also compared between groups using a Wilcoxon-Mann–Whitney test. The P values (panels A, B, and C) were adjusted for four comparisons using the Bonferroni correction. ***P < 0.001, significantly different compared with the non-CPB group. ††P < 0.01 and †††P < 0.001, significantly different compared with the within group CSF samples. The adjusted P values, median difference, or difference in paired medians and the 95% confidence intervals for each comparison are listed in ESM, eTables 7–10. CPB = cardiopulmonary bypass; CSF = cerebrospinal fluid; IQR = interquartile range.
Correlations between plasma and CSF S100B exposures
Spearman correlation analysis between the average CSF S100B exposure vs average plasma S100B exposure in both the CPB and non-CPB groups yielded wide adjusted 95% CIs that included zero values and were not significant (Fig. 4A). Similarly, we did not detect a significant correlation between plasma S100B Cmax and CSF S100B Cmax values in both groups (Fig. 4B).
Between-subjects correlations of plasma vs CSF S100B. The mean values for plasma and CSF S100B exposures were calculated and weighted for the number of paired measurements in each participant. The paired weighted plasma and CSF S100 B exposures (A) and the plasma S100B Cmax vs CSF S100B Cmax for each individual participant (B) are shown as scatter plots. The r (adj 95% CI) obtained from Spearman correlations are shown for the CPB (open squares) and non-CPB groups (filled squares). The 95% confidence intervals were adjusted for two comparisons using the Bonferroni correction. CPB = cardiopulmonary bypass; CSF = cerebrospinal fluid.
Correlations between plasma and CSF S100B exposures with measures of systemic and CNS inflammation and BBB permeability
The results of the Spearman correlation analyses between plasma S100B exposure with plasma IL-6 exposure (measure of systemic inflammatory response), average CSF S100B exposure with CSF IL-6 exposure (measure of the central inflammatory response), and the plasma and CSF S100B exposures with the CSF/plasma albumin ratio (measure of BBB permeability) are reported in Table 3. In all cases, the adjusted 95% Cis for the correlations were wide and included zero values, indicating that the correlations were not significant.
CSF S100B concentrations in participants with moderate or severe adverse events
Three participants in the CPB group and one in the non-CPB group displayed substantially higher peak CSF S100B concentrations (Figs 5A–B). In the three CPB patients, the typical spike in plasma S100B was observed at the post-CPB time point (Figs 5C–E). In comparison, the elevation in CSF S100B was delayed (Figs 5C–F) and corresponded with the onset of moderate or severe adverse events, including a spinal cord infarction, ischemic bowel, postoperative hemorrhage, and hyperglycemia (ESM, eTable 1). An approximately parallel increase in plasma and CSF S100B was only observed in the participant with ischemic bowel. Further, an elevation in CSF IL-6 was observed in all four outlying participants at later time points (Figs 5G–J). Nevertheless, two participants that experienced severe cardiac adverse events requiring cardiopulmonary resuscitation and two participants that experienced delirium displayed relatively low and constant CSF S100B (or a low-magnitude brief spike, participant 12) over the sampling period (ESM, eTable 1 and eFig. 1). Low concentrations of IL-6 were measurable in the CSF of three of these participants and were below the lower limit of quantification in all samples of the fourth participant, supporting a relatively limited CNS inflammatory response.
Cerebrospinal fluid S100B concentrations increased in some participants that experienced severe adverse events. A before and after plot shows the matching C0 and Cmax CSF S100B concentrations for all individual participants (A). A Tukey Box plot was used to identify outliers (participants 10, 11, 27, and 35) for measured CSF S100B concentrations (B). Outliers were values greater than 1.5 × IQR above the top bar of the box plot and are shown by the filled circles. The plasma and CSF S100B (C–F) and IL-6 (G–H) concentrations are shown for participants 10, 11, 27, and 35 that had high outlying CSF S100B Cmax values. CSF = cerebrospinal fluid; IL = interleukin; IQR = interquartile range
Secondary analyses
A comparison between participants undergoing open surgical procedures with or without CPB (n = 20) vs those undergoing endovascular procedures (n = 15) was performed for all analyses (ESM, eTables 2–4 and eFigs 2–4). The overall results were similar to the primary analysis that compared CPB vs non-CPB groups.
Discussion
In our study, transient opening of the BBB (as measured by the increased CSF/plasma albumin ratio) was observed immediately after CPB, which in theory could allow for the distribution of S100B from the brain to the peripheral circulation.39,40 Nevertheless, the bulk of our experimental evidence indicates that most observed increases in plasma S100B following CPB do not occur secondary to increased BBB permeability and release of S100B from the brain to the circulation. First, the observed CSF/plasma albumin ratios suggested similar increases in BBB permeability in the CPB vs non-CPB groups, but the peak plasma S100B and average S100B exposure were significantly higher in the CPB group. Second, the peak plasma S100B occurred earlier than the more gradual increase in CSF S100B, which was primarily attributed to the few outlying participants that experienced moderate or severe adverse responses. Third, the S100B CSF/plasma ratio decreased significantly in the CPB group. If the source of plasma S100B was the CNS, the ratio should remain constant or increase. Finally, we did not detect significant correlations between the average CSF S100B exposure and plasma S100B exposure over the total sample duration in either group.
These findings agree with the limited number of previous studies that have measured both CSF and serum concentrations of S100B simultaneously in patients undergoing open TAA repair with CPB.41,42,43 Additionally, in the non-CPB group, the relatively small rise in plasma S100B preceded the peak change in BBB permeability as assessed by the CSF/plasma albumin ratio. Based on our data, we conclude that the general early increases in plasma S100B in the two groups are not the result of increased BBB permeability and transfer of S100B from the brain to the periphery. Rather, as has been previously suggested, extracerebral sources are most likely. Our results therefore reaffirm the poor predictive value of serum/plasma S100B as a predictor of CNS injury after major cardiac or vascular surgery.9,19,20,22,43,44
Given the apparent limitations of serum or plasma S100B as a predictor of increased BBB permeability and neurologic injury in the setting of cardiovascular surgery, others have suggested that CSF S100B may be more reliable.42,45,46 This brings us to a key observation of four outlying participants that had large increases in CSF S100B. Each of these individuals experienced a moderate or severe adverse event during or after the surgical procedure, which coincided with the rise in CSF S100B. The most dramatic increase in CSF S100B occurred in a patient that developed a spinal cord infarction. This observation is consistent with previous reports of dramatically increased CSF S100B in patients who developed spinal cord infarction while undergoing cardiovascular surgeries with CPB.41,42,45,47 While this suggests CSF S100B could have predictive value in identifying those at risk for spinal cord injury, our data identifies two important caveats. First, the timing of the increase in CSF S100B occurred with the onset of injury rather than prior to it. Thus, the increase in CSF S100B happened too late to allow implementation of preventative measures, as has been previously suggested.41,48 Second, the increase in CSF S100B was not specific to spinal cord injury, and also occurred in some but not all individuals that experienced moderate or severe adverse events that originated outside the CNS. This result is similar to elevations in serum S100B, which are also not specific to neuronal injury.49 For these reasons, there appears to be limited usefulness of CSF S100B as a specific marker for predicting increased BBB permeability and spinal cord injury after cardiovascular surgery.
A graded systemic inflammatory response (as shown by measures of plasma IL-6) was observed in this study after open and endovascular TAA repair, with the greatest systemic inflammation observed in the CPB group. The secondary analysis does not exclude a potential correlation between the surgically induced inflammatory response (i.e., plasma IL-6) and S100B in the open surgery ± CPB group. Nevertheless, unlike previous observations,6,50 we cannot definitively link systemic inflammation with increased BBB permeability based on our results because of the likely extracerebral release of S100B. The secondary analysis also suggested a potential correlation between CSF IL-6 and S100B in participants that underwent endovascular surgery. In addition, in all the outlying cases where there was an increase in CSF S100B, a subsequent increase in CSF IL-6 also occurred. In converse, those participants that experienced adverse events but no increase in CSF S100B also did not have increases in CSF IL-6. Thus, our data reveal the novel observation that elevations in CSF S100B occur prior to IL-6, which is an established marker of acute inflammation. Future studies are needed to analyze this relationship and the potential utility of CSF S100B to identify patients at risk for CNS inflammation.
Our findings should be interpreted in the context of the study’s strengths and limitations. First, this was a single-centre study with a relatively small sample size, which may potentially limit its generalizability. Nevertheless, our results are in keeping with previous observations in similar populations.41,42,43 Second, although it has repeatedly been reported that CPB induces a marked peripheral inflammatory response, it is also likely that the peripheral inflammatory response is higher in those who received open instead of endovascular repair. Therefore, the observed difference in the peripheral inflammatory response between the CPB and non-CPB groups may have been exaggerated by the predominance of endovascular repairs performed among the non-CPB group patients. Third, the S100B assay does not discern between the S100A1-B heterodimer and S100B-B homodimer and differential effects of BBB disruption on the release of S100B isoforms has been reported.40 Nevertheless, following cardiovascular surgery with CPB, the patterns of the individual isoforms (S100A1-B and S100B-B) were similar to those of total S100B.20 Thus, our choice to measure total S100B is supported by the literature and measuring the individual isoforms would be unlikely to reveal different results. Some S100B immunoassays have been reported to cross-react with contaminating proteins from the surgical field giving a falsely elevated reading.51 It is unknown if the S100B kits that we used showed similar cross-reactivity or if there were potential cross-reacting proteins in CSF. Finally, we measured plasma S100B whereas previous studies have measured serum S100B. The similarity of the plasma S100B concentration vs time profiles in our study compared with those that monitored serum S100B concentrations9,14,15,16,32,42,52 provides validation that plasma is also an appropriate biological matrix for assessing S100B concentrations.
Conclusions
Our study suggests that increased plasma S100B concentrations after open and endovascular TAA repair with or without CPB are not due to increased BBB permeability and therefore may not serve as a reliable biomarker for neurologic (cerebral or spinal cord) injury in cardiovascular surgery patients. Given that the increase in CSF S100B is not specific to BBB disruption after these procedures, CSF S100B may also have limited value. Further research would be appropriate to confirm the findings of our study, which had a small sample size.
References
Allore RJ, Friend WC, O’Hanlon D, et al. Cloning and expression of the human S100 beta gene. J Biol Chem 1990; 265: 15537-43.
Vives V, Alonso G, Solal AC, Joubert D, Legraverend C. Visualization of S100B-positive neurons and glia in the central nervous system of EGFP transgenic mice. J Comp Neurol 2003; 457: 404-19.
Kleindienst A, Hesse F, Bullock MR, Buchfelder M. The neurotrophic protein S100B: value as a marker of brain damage and possible therapeutic implications. Prog Brain Res 2007; 161: 317-25.
Lindblad C, Nelson DW, Zeiler FA, et al. Influence of blood-brain barrier integrity on brain protein biomarker clearance in severe traumatic brain injury: a longitudinal prospective study. J Neurotrauma 2020; 37: 1381-91.
Gabriel EA, Locali RF, Romano CC, da Silva Duarte AJ, Palma JH, Buffolo E. Analysis of the inflammatory response in endovascular treatment of aortic aneurysms. Eur J Cardiothorac Surg 2007; 31: 406-12.
Mazzone A, Gianetti J, Picano E, et al. Correlation between inflammatory response and markers of neuronal damage in coronary revascularization with and without cardiopulmonary bypass. Perfusion 2003; 18: 3-8.
Prondzinsky R, Knupfer A, Loppnow H, et al. Surgical trauma affects the proinflammatory status after cardiac surgery to a higher degree than cardiopulmonary bypass. J Thorac Cardiovasc Surg 2005; 129: 760-6.
Rowlands TE, Homer-Vanniasinkam S. Pro- and anti-inflammatory cytokine release in open versus endovascular repair of abdominal aortic aneurysm. Br J Surg 2001; 88: 1335-40.
Nakamura K, Ueno T, Yamamoto H, Iguro Y, Yamada K, Sakata R. Relationship between cerebral injury and inflammatory responses in patients undergoing cardiac surgery with cardiopulmonary bypass. Cytokine 2005; 29: 95-104.
Abrahamov D, Levran O, Naparstek S, et al. Blood-brain barrier disruption after cardiopulmonary bypass: diagnosis and correlation to cognition. Ann Thorac Surg 2017; 104: 161-9.
Danielson M, Wiklund A, Granath F, et al. Neuroinflammatory markers associate with cognitive decline after major surgery: findings of an explorative study. Ann Neurol 2020; 87: 370-82.
Okamura T, Ishibashi N, Zurakowski D, Jonas RA. Cardiopulmonary bypass increases permeability of the blood-cerebrospinal fluid barrier. Ann Thorac Surg 2010; 89: 187-94.
Wang Y, Goralski KB, Roberts DJ, et al. An observational study examining the effects of a surgically induced inflammatory response on the distribution of morphine and its metabolites into cerebrospinal fluid. Can J Anesth 2017; 64: 1009-22.
Herrmann M, Ebert AD, Galazky I, Wunderlich MT, Kunz WS, Huth C. Neurobehavioral outcome prediction after cardiac surgery: role of neurobiochemical markers of damage to neuronal and glial brain tissue. Stroke 2000; 31: 645-50.
Ueno T, Iguro Y, Yamamoto H, Sakata R, Kakihana Y, Nakamura K. Serial measurement of serum S-100B protein as a marker of cerebral damage after cardiac surgery. Ann Thorac Surg 2003; 75: 1892-7; discussion 1897-8.
Jonsson H, Johnsson P, Alling C, Westaby S, Blomquist S. Significance of serum S100 release after coronary artery bypass grafting. Ann Thorac Surg 1998; 65: 1639-44.
Johnsson P, Backstrom M, Bergh C, Jonsson H, Luhrs C, Alling C. Increased S100B in blood after cardiac surgery is a powerful predictor of late mortality. Ann Thorac Surg 2003; 75: 162-8.
Vaage J, Anderson R. Biochemical markers of neurologic injury in cardiac surgery: the rise and fall of S100beta. J Thorac Cardiovasc Surg 2001; 122: 853-5.
Anderson RE, Hansson LO, Liska J, Settergren G, Vaage J. The effect of cardiotomy suction on the brain injury marker S100beta after cardiopulmonary bypass. Ann Thorac Surg 2000; 69: 847-50.
Anderson RE, Hansson LO, Nilsson O, Liska J, Settergren G, Vaage J. Increase in serum S100A1-B and S100BB during cardiac surgery arises from extracerebral sources. Ann Thorac Surg 2001; 71: 1512-7.
Snyder-Ramos SA, Bottiger BW. Molecular markers of brain damage—clinical and ethical implications with particular focus on cardiac arrest. Restor Neurol Neurosci 2003; 21: 123-39.
Jonsson H, Johnsson P, Alling C, Backstrom M, Bergh C, Blomquist S. S100beta after coronary artery surgery: release pattern, source of contamination, and relation to neuropsychological outcome. Ann Thorac Surg 1999; 68: 2202-8.
Bar-Yosef O, Greidinger D, Iskilova M, Hemi R, Tirosh T, Vardi A. Neurological deficit is predicted by S100B in children after cardiac surgery. Clin Chim Acta 2018; 481: 56-60.
Duez CH, Grejs AM, Jeppesen AN, et al. Neuron-specific enolase and S-100b in prolonged targeted temperature management after cardiac arrest: a randomised study. Resuscitation 2018; 122: 79-86.
Moss BP, Patel DC, Tavee JO, Culver DA. Evaluating S100B as a serum biomarker for central neurosarcoidosis. Respir Med 2020; DOI: https://doi.org/10.1016/j.rmed.2019.105855.
Park DW, Park SH, Hwang SK. Serial measurement of S100B and NSE in pediatric traumatic brain injury. Childs Nerv Syst 2019; 35: 343-8.
Pearlman DM, Brown JR, MacKenzie TA, Hernandez F Jr, Najjar S. Blood levels of S-100 calcium-binding protein B, high-sensitivity C-reactive protein, and interleukin-6 for changes in depressive symptom severity after coronary artery bypass grafting: prospective cohort nested within a randomized, controlled trial. PloS One 2014; DOI : https://doi.org/10.1371/journal.pone.0111110.
Perrin P, Collongues N, Baloglu S, et al. Cytokine release syndrome-associated encephalopathy in patients with COVID-19. Eur J Neurol 2021; 28 : 248-58.
Pironkova RP, Giamelli J, Seiden H, et al. Brain injury with systemic inflammation in newborns with congenital heart disease undergoing heart surgery. Exp Ther Med 2017; 14: 228-38.
Silva FP, Schmidt AP, Valentin LS, et al. S100B protein and neuron-specific enolase as predictors of cognitive dysfunction after coronary artery bypass graft surgery: a prospective observational study. Eur J Anaesthesiol 2016; 33: 681-9.
von Elm E, Altman DG, Egger M, et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ 2007; 335: 806-8.
Wandschneider W, Thalmann M, Trampitsch E, Ziervogel G, Kobinia G. Off-pump coronary bypass operations significantly reduce S100 release: an indicator for less cerebral damage? Ann Thorac Surg 2000; 70: 1577-9.
Yuan SM. Biomarkers of cerebral injury in cardiac surgery. Anadolu Kardiyol Derg 2014; 14: 638-45.
Roberts DJ, Goralski KB, Renton KW, et al. Effect of acute inflammatory brain injury on accumulation of morphine and morphine 3- and 6-glucuronide in the human brain. Crit Care Med 2009; 37: 2767-74.
Reinsfelt B, Ricksten SE, Zetterberg H, Blennow K, Freden-Lindqvist J, Westerlind A. Cerebrospinal fluid markers of brain injury, inflammation, and blood-brain barrier dysfunction in cardiac surgery. Ann Thorac Surg 2012; 94: 549-55.
Bland JM, Altman DG. Correlation, regression, and repeated data. BMJ 1994; DOI: https://doi.org/10.1136/bmj.308.6933.896.
Geher G, Hall S. Straightforward Statistics: Understanding the Tools of Research. NY; Oxford: Oxford University Press; 2014.
Gignac G. Spearman Correlation Confidence Intervals SPSS. In: how2statsbook (Ed.): Youtube; 2019. Available from URL: https://www.youtube.com/watch?v=gKHgCq5E864&t=2s (accessed August 2021).
Marchi N, Rasmussen P, Kapural M, et al. Peripheral markers of brain damage and blood-brain barrier dysfunction. Restor Neurol Neurosci 2003; 21: 109-21.
Pham N, Fazio V, Cucullo L, et al. Extracranial sources of S100B do not affect serum levels. PloS One 2010; DOI: https://doi.org/10.1371/journal.pone.0012691.
Khaladj N, Teebken OE, Hagl C, et al. The role of cerebrospinal fluid S100 and lactate to predict clinically evident spinal cord ischaemia in thoraco-abdominal aortic surgery. Eur J Vasc Endovasc Surg 2008; 36: 11-9.
Kunihara T, Shiiya N, Yasuda K. Changes in S100beta protein levels in cerebrospinal fluid after thoracoabdominal aortic operations. J Thorac Cardiovasc Surg 2001; 122: 1019-20.
Anderson RE, Winnerkvist A, Hansson LO, et al. Biochemical markers of cerebrospinal ischemia after repair of aneurysms of the descending and thoracoabdominal aorta. J Cardiothorac Vasc Anesth 2003; 17: 598-603.
Missler U, Orlowski N, Notzold A, Dibbelt L, Steinmeier E, Wiesmann M. Early elevation of S-100B protein in blood after cardiac surgery is not a predictor of ischemic cerebral injury. Clin Chim Acta 2002; 321: 29-33.
van Dongen EP, Ter Beek HT, Boezeman EH, Schepens MA, Langemeijer HJ, Aarts LP. Normal serum concentrations of S-100 protein and changes in cerebrospinal fluid concentrations of S-100 protein during and after thoracoabdominal aortic aneurysm surgery: is S-100 protein a biochemical marker of clinical value in detecting spinal cord ischemia? J Vasc Surg 1998; 27: 344-6.
van Dongen EP, ter Beek HT, Schepens MA, et al. The relationship between evoked potentials and measurements of S-100 protein in cerebrospinal fluid during and after thoracoabdominal aortic aneurysm surgery. J Vasc Surg 1999; 30: 293-300.
Shiiya N, Kunihara T, Miyatake T, Matsuzaki K, Yasuda K. Tau protein in the cerebrospinal fluid is a marker of brain injury after aortic surgery. Ann Thorac Surg 2004; 77: 2034-8.
Winnerkvist A, Anderson RE, Hansson LO, et al. Multilevel somatosensory evoked potentials and cerebrospinal proteins: indicators of spinal cord injury in thoracoabdominal aortic aneurysm surgery. Eur J Cardiothorac Surg 2007; 31: 637-42.
Anderson RE, Hansson LO, Nilsson O, Dijlai-Merzoug R, Settergren G. High serum S100B levels for trauma patients without head injuries. Neurosurgery 2001; 48: 1255-8; discussion 1258-60.
Ashraf S, Bhattacharya K, Tian Y, Watterson K. Cytokine and S100B levels in paediatric patients undergoing corrective cardiac surgery with or without total circulatory arrest. Eur J Cardiothorac Surg 1999; 16: 32-7.
Fazio V, Bhudia SK, Marchi N, Aumayr B, Janigro D. Peripheral detection of S100beta during cardiothoracic surgery: what are we really measuring? Ann Thorac Surg 2004; 78: 46-52; discussion 52-3.
Blomquist S, Johnsson P, Luhrs C, et al. The appearance of S-100 protein in serum during and immediately after cardiopulmonary bypass surgery: a possible marker for cerebral injury. J Cardiothorac Vasc Anesth 1997; 11: 699-703.
Author contributions
Kerry B. Goralski and Richard I. Hall were the study co-principal investigators and conceived and designed the research; Yan Wang performed the research and generated experimental data. Lisa C. Julien coordinated the clinical trial and recruited participants. Jeremy Wood was the study surgeon and recruited participants. Jeremy Wood, Derek J. Roberts, Kerry B. Goralski, and Richard I. Hall analyzed and interpreted the study data. Derek J. Roberts, Kerry B. Goralski, Yan Wang, and Richard I. Hall wrote the manuscript. Kerry B. Goralski supervised the trainee Yan Wang.
Acknowledgements
We are indebted to the patients for their willingness to participate in this investigation, and the CVICU intensive care unit nurses for their help with collection of samples.
Disclosures
None.
Funding statement
Financial support for this investigation was provided by the Heart and Stroke Foundation of Canada (Nova Scotia Chapter), the Canadian Anesthesiologists’ Society, and the Dalhousie University Pharmacy Endowment Fund.
Editorial responsibility
This submission was handled by Dr. Alana Flexman, Associate Editor, Canadian Journal of Anesthesia/Journal canadien d’anesthésie.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Roberts, D.J., Hall, R.I., Wang, Y. et al. S100B as a biomarker of blood–brain barrier disruption after thoracoabdominal aortic aneurysm repair: a secondary analysis from a prospective cohort study. Can J Anesth/J Can Anesth 68, 1756–1768 (2021). https://doi.org/10.1007/s12630-021-02110-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-021-02110-2