Abstract
Objectives
Platelets are playing a crucial role in acute cardiovascular events. We investigated if physical stress activates platelets and whether this activation can be inhibited by a polyphenol-enriched diet.
Methods
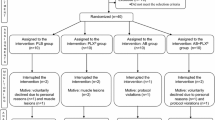
Blood samples were taken from a total of 103 athletes three weeks before, one day before, immediately as well as 24 hours and 72 hours after a marathon run. Participants were randomized, double-blinded and divided into two groups. One group received a polyphenol-rich beverage the other the same beverage without polyphenols. Besides analysis of platelet counts and impedance-aggregometric-measurement of platelet activity, soluble P-selectin and Endothelin-A measurements were performed.
Results
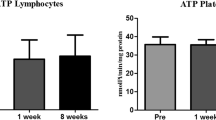
In the control group, runners showed a 2.2-fold increased platelet aggregation directly after completing a marathon and within the following three days when compared with baseline values (p<0.01). In accordance, significant increases in sP-selectin (57.52ng/ml vs. 94.86ng/ml;p<0.01) were detectable. In contrast, for the group consuming a beverage with increased polyphenol content (upper quartile of study beverage intake) we did not find any increase of platelet aggregation.
Discussion
Physical stress causes a significant increase in platelet activity. Our results demonstrate that a diet enriched in polyphenols is capable of preventing platelet activation. These findings might indicate a diminished cardiovascular stress-reaction following pre-exposition to polyphenol-enriched diet.











Similar content being viewed by others
Abbreviations
- ADP:
-
adenosindiphosphat
- AUC:
-
area under the curve
- BeMaGIC:
-
Beer Marathon Genetics Inflammation and Cardiovascular System
- BNP:
-
brain natriuretic peptide
- cAMP:
-
cyclisches Adenosinmonophosphat
- CGA:
-
Chromogranin A
- ELISA:
-
enzyme linked immunosorbent assay
- GbIIb/IIIa:
-
glycol-protein IIb-IIIa complex
- GAE:
-
gallic acid equivalents
- IQR:
-
interquartile range
- NADPH:
-
nicotinamide adenine dinucleotide phosphate-oxidase
- NO:
-
nitric oxide
- ROS:
-
reactive oxygen species
References
Libby, P. and P. Theroux. Pathophysiology of coronary artery disease. Circulation. 2005;111(25): p. 3481–8.
Hansson, G.K. Inflammation, atherosclerosis, and coronary artery disease. N Engl J Med. 2005;352(16): p. 1685–95.
Bombeli, T., B.R. Schwartz, and J.M. Harlan. Adhesion of activated platelets to endothelial cells: evidence for a GPIIbIIIa-dependent bridging mechanism and novel roles for endothelial intercellular adhesion molecule 1 (ICAM-1), alphavbeta3 integrin, and GPIbalpha. J Exp Med. 1998;187(3): p. 329–39.
Nickel, T., D. Schmauss, H. Hanssen, Z. Sicic, B. Krebs, S. Jankl, C. Summo, P. Fraunberger, A.K. Walli, S. Pfeiler, and M. Weis. oxLDL uptake by dendritic cells induces upregulation of scavenger-receptors, maturation and differentiation. Atherosclerosis. 2009;205(2): p. 442–50.
Mittleman, M.A., M. Maclure, G.H. Tofler, J.B. Sherwood, R.J. Goldberg, and J.E. Muller. Triggering of Acute Myocardial-Infarction by Heavy Physical Exertion-Protection against Triggering by Regular Exertion. New England Journal of Medicine. 1993;329(23): p. 1677–1683.
Trivax, J.E., B.A. Franklin, J.A. Goldstein, K.M. Chinnaiyan, M.J. Gallagher, A.T. deJong, J.M. Colar, D.E. Haines, and P.A. McCullough. Acute cardiac effects of marathon running. Journal of Applied Physiology. 2010;108(5): p. 1148–1153.
Hanssen, H., A. Keithahn, G. Hertel, V. Drexel, H. Stern, T. Schuster, D. Lorang, A.J. Beer, A. Schmidt-Trucksass, T. Nickel, M. Weis, R. Botnar, M. Schwaiger, and M. Halle. Magnetic resonance imaging of myocardial injury and ventricular torsion after marathon running. Clin Sci (Lond). 2011;120(4): p. 143–52.
Kratz, A., M.J. Wood, A.J. Siegel, J.R. Hiers, and E.M. Van Cott. Effects of marathon running on platelet activation markers: direct evidence for in vivo platelet activation. Am J Clin Pathol. 2006;125(2): p. 296–300.
Rocker, L., M. Taenzer, W.K. Drygas, H. Lill, B. Heyduck, and H.U. Altenkirch. Effect of prolonged physical exercise on the fibrinolytic system. Eur J Appl Physiol Occup Physiol. 1990;60(6): p. 478–81.
Zwart, B., T.C. Van Kerkvoorde, J.W. van Werkum, N.J. Breet, J.M. Ten Berg, and A.W. Van’t Hof. Vigorous exercise as a triggering mechanism for late stent thrombosis: A description of three cases. Platelets. 2010;21(1): p. 72–6.
Nickel, T., H. Hanssen, Z. Sisic, S. Pfeiler, C. Summo, D. Schmauss, E. Hoster, and M. Weis. Immunoregulatory effects of the flavonol quercetin in vitro and in vivo. Eur J Nutr. 2011;50(3): p. 163–72.
Oomen, C.M., M.C. Ocke, E.J. Feskens, F.J. Kok, and D. Kromhout. alpha-Linolenic acid intake is not beneficially associated with 10-y risk of coronary artery disease incidence: the Zutphen Elderly Study. Am J Clin Nutr. 72001;4(4): p. 457–63.
Nickel, T., C.L. Schlichting, and M. Weis. Drugs modulating endothelial function after transplantation. Transplantation. 2006;82(1 Suppl): p. S41–6.
Gaytan, R.J. and L.M. Prisant. Oral nutritional supplements and heart disease: a review. Am J Ther. 2001;8(4): p. 255–74.
Duffy, S.J. and J.A. Vita. Effects of phenolics on vascular endothelial function. Curr Opin Lipidol. 2003;14(1): p. 21–7.
Olas, B., J. Kolodziejczyk, B. Wachowicz, D. Jedrejek, A. Stochmal, and W. Oleszek. The extract from hop cones (Humulus lupulus) as a modulator of oxidative stress in blood platelets. Platelets. 2011;22(5): p. 345–52.
Scherr, J., D.C. Nieman, T. Schuster, J. Habermann, M. Rank, S. Braun, A. Pressler, B. Wolfarth, and M. Halle. Nonalcoholic beer reduces inflammation and incidence of respiratory tract illness. Med Sci Sports Exerc. 2012;44(1): p. 18–26.
Dill, D.B. and D.L. Costill. Calculation of percentage changes in volumes of blood, plasma, and red cells in dehydration. J Appl Physiol. 1974;37(2): p. 247–8.
Sibbing, D., S. Braun, S. Jawansky, W. Vogt, J. Mehilli, A. Schomig, A. Kastrati, and N. von Beckerath. Assessment of ADP-induced platelet aggregation with light transmission aggregometry and multiple electrode platelet aggregometry before and after clopidogrel treatment. Thromb Haemost. 2008;99(1): p. 121–6.
Sibbing, D., T. Morath, J. Stegherr, S. Braun, W. Vogt, M. Hadamitzky, A. Schomig, A. Kastrati, and N. von Beckerath. Impact of proton pump inhibitors on the antiplatelet effects of clopidogrel. Thromb Haemost. 2009;101(4): p. 714–9.
Sibbing, D., S. Braun, T. Morath, J. Mehilli, W. Vogt, A. Schomig, A. Kastrati, and N. von Beckerath. Platelet reactivity after clopidogrel treatment assessed with point-of-care analysis and early drug-eluting stent thrombosis. J Am Coll Cardiol. 2009;53(10): p. 849–56.
Siller-Matula, J.M., G. Christ, I.M. Lang, G. Delle-Karth, K. Huber, and B. Jilma. Multiple electrode aggregometry predicts stent thrombosis better than the vasodilator-stimulated phosphoprotein phosphorylation assay. J Thromb Haemost. 2010;8(2): p. 351–9.
Rock, G., P. Tittley, and A. Pipe. Coagulation factor changes following endurance exercise. Clin J Sport Med. 1997;7(2): p. 94–9.
Gremmel, T., S. Steiner, D. Seidinger, R. Koppensteiner, S. Panzer, and C.W. Kopp. Comparison of methods to evaluate aspirin-mediated platelet inhibition after percutaneous intervention with stent implantation. Platelets. 2011;22(3): p. 188–95.
Jurk, K. and B.E. Kehrel. Platelets: physiology and biochemistry. Semin Thromb Hemost. 2005;31(4): p. 381–92.
Anfossi, G. and M. Trovati. Role of catecholamines in platelet function: pathophysiological and clinical significance. Eur J Clin Invest. 1996;26(5): p. 353–70.
Nickel, T., H. Hanssen, I. Emslander, V. Drexel, G. Hertel, A. Schmidt-Trucksass, C. Summo, Z. Sisic, M. Lambert, E. Hoster, M. Halle, and M. Weis. Immunomodulatory effects of aerobic training in obesity. Mediators Inflamm. 2011: p. 308965.
Starkie, R.L., J. Rolland, D.J. Angus, M.J. Anderson, and M.A. Febbraio. Circulating monocytes are not the source of elevations in plasma IL-6 and TNF-alpha levels after prolonged running. Am J Physiol Cell Physiol. 2001;280(4): p. C769–74.
Petidis, K., S. Douma, M. Doumas, I. Basagiannis, K. Vogiatzis, and C. Zamboulis. The interaction of vasoactive substances during exercise modulates platelet aggregation in hypertension and coronary artery disease. BMC Cardiovasc Disord. 2008;8: p. 11.
el-Sayed, M.S. Effects of exercise on blood coagulation, fibrinolysis and platelet aggregation. Sports Med. 1996;22(5): p. 282–98.
Shimomura, H., H. Ogawa, H. Arai, Y. Moriyama, K. Takazoe, N. Hirai, K. Kaikita, O. Hirashima, K. Misumi, H. Soejima, K. Nishiyama, and H. Yasue. Serial changes in plasma levels of soluble P-selectin in patients with acute myocardial infarction. Am J Cardiol. 1998;81(4): p. 397–400.
Blann, A.D., W.M. Noteboom, and F.R. Rosendaal. Increased soluble P-selectin levels following deep venous thrombosis: cause or effect? Br J Haematol. 2000;108(1): p. 191–3.
Eifert, S., S. Kofler, T. Nickel, S. Horster, A.K. Bigdeli, A. Beiras-Fernandez, B. Meiser, and I. Kaczmarek. Gender-based analysis of outcome after heart transplantation. Exp Clin Transplant. 2012;10(4): p. 368–74.
Wilbert-Lampen, U., T. Nickel, D. Leistner, D. Guthlin, T. Matis, C. Volker, S. Sper, H. Kuchenhoff, S. Kaab, and G. Steinbeck. Modified serum profiles of inflammatory and vasoconstrictive factors in patients with emotional stress-induced acute coronary syndrome during World Cup Soccer 2006. J Am Coll Cardiol. 2010;55(7): p. 637–42.
Li, N., N.H. Wallen, and P. Hjemdahl. Evidence for prothrombotic effects of exercise and limited protection by aspirin. Circulation. 1999;100(13): p. 1374–9.
Perneby, C., N.H. Wallen, H. Hu, N. Li, and P. Hjemdahl. Prothrombotic responses to exercise are little influenced by clopidogrel treatment. Thromb Res. 2004;114(4): p. 235–43.
Nardini, M., F. Natella, and C. Scaccini. Role of dietary polyphenols in platelet aggregation. A review of the supplementation studies. Platelets. 2007;18(3): p. 224–43.
Landolfi, R., R.L. Mower, and M. Steiner. Modification of platelet function and arachidonic acid metabolism by bioflavonoids. Structure-activity relations. Biochem Pharmacol. 1984;33(9): p. 1525–30.
Chang, G.T., S.K. Kang, J.H. Kim, K.H. Chung, Y.C. Chang, and C.H. Kim. Inhibitory effect of the Korean herbal medicine, Dae-Jo-Whan, on platelet-activating factor-induced platelet aggregation. J Ethnopharmacol. 2005;102(3): p. 430–9.
Son, D.J., M.R. Cho, Y.R. Jin, S.Y. Kim, Y.H. Park, S.H. Lee, S. Akiba, T. Sato, and Y.P. Yun. Antiplatelet effect of green tea catechins: a possible mechanism through arachidonic acid pathway. Prostaglandins Leukot Essent Fatty Acids. 2004;71(1): p. 25–31.
Pignatelli, P., S. Di Santo, B. Buchetti, V. Sanguigni, A. Brunelli, and F. Violi. Polyphenols enhance platelet nitric oxide by inhibiting protein kinase C-dependent NADPH oxidase activation: effect on platelet recruitment. FASEB J. 2006;20(8): p. 1082–9.
Ovaskainen, M.L., R. Torronen, J.M. Koponen, H. Sinkko, J. Hellstrom, H. Reinivuo, and P. Mattila. Dietary intake and major food sources of polyphenols in Finnish adults. J Nutr. 2008;138(3): p. 562–6.
Scalbert, A. and G. Williamson. Dietary intake and bioavailability of polyphenols. J Nutr. 2000;130(8S Suppl): p. 2073S–85S.
Rautiainen, S., E.B. Levitan, N. Orsini, A. Akesson, R. Morgenstern, M.A. Mittleman, and A. Wolk. Total antioxidant capacity from diet and risk of myocardial infarction: a prospective cohort of women. Am J Med. 2012;125(10): p. 974–80.
Piazzon, A., M. Forte, and M. Nardini. Characterization of phenolics content and antioxidant activity of different beer types. J Agric Food Chem. 2010;58(19): p. 10677–83.
Author information
Authors and Affiliations
Corresponding author
Additional information
These authors contributed equally to this work
Both senior authors contributed equally to this work.
Rights and permissions
About this article
Cite this article
Nickel, T., Lackermair, K., Scherr, J. et al. Influence of high polyphenol beverage on stress-induced platelet activation. J Nutr Health Aging 20, 586–593 (2016). https://doi.org/10.1007/s12603-016-0697-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-016-0697-y