Abstract
Introduction
To compare 2-year safety and efficacy outcomes after Aquablation or transurethral resection of the prostate (TURP) for the treatment of lower urinary tract symptoms related to benign prostate hyperplasia (BPH).
Methods
One hundred eighty-one patients with BPH were assigned at random (2:1 ratio) to either Aquablation or TURP. Patients and follow-up assessors were blinded to treatment. Assessments included the International Prostate Symptom Score (IPSS), Male Sexual Health Questionnaire (MSHQ), International Index of Erectile Function and uroflow. The focus of analysis was 2-year outcomes.
Results
At 2 years, IPSS scores improved by 14.7 points in the Aquablation group and 14.9 points in TURP (p = .8304, 95% CI for difference − 2.1 to 2.6 points). Two-year improvements in maximum flow rate (Qmax) were large in both groups at 11.2 and 8.6 cc/s for Aquablation and TURP, respectively (p = 0.1880, 95% CI for difference − 1.3 to 6.4). Sexual function as assessed by MSHQ was stable in the Aquablation group and decreased slightly in the TURP group. At 2 years, PSA was reduced significantly in both groups by 0.7 and 1.2 points, respectively; the reduction was similar across groups (p = 0.1816). Surgical retreatment rates after 12 months for Aquablation were 1.7% and 0% for TURP. Over 2 years, surgical BPH retreatment rates were 4.3% and 1.5% (p = 0.4219), respectively.
Conclusion
Two-year efficacy outcomes after TURP and Aquablation were similar, and the rate of surgical retreatment was low and similar to TURP.
Trial Registration
ClinicalTrials.gov no. NCT02505919.
Funding
PROCEPT BioRobotics.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lower urinary tract symptoms (LUTS) related to benign prostatic hyperplasia (BPH) or bladder outlet obstruction (BOO) commonly present in men over the age of 50 years and increases significantly with age [1, 2]. Medical refractory BPH patients will seek surgical options to address their symptoms.
There are a variety of interventional treatment options of BPH from that range from non-ablative techniques to resective techniques such as open simple prostatectomy, laser enucleation, photovaporization (PVP), and monopolar or bipolar transurethral resection of the prostate (TURP). While these options are effective, they typically cause sexual dysfunction [3,4,5,6,7]. The most common sexual dysfunction side effect with TURP is retrograde ejaculation occurring in over 2/3 of men [8].
Aquablation combines real-time, multi-dimensional imaging, autonomous robotics and heat-free waterjet ablation for targeted, controlled and immediate removal of prostate tissue for the treatment of lower urinary tract symptoms caused by BPH. The first report of Aquablation from a randomized study compared against TURP was previously reported with 6-month results [9].
Methods
The WATER (NCT02505919) study is a prospective, double-blinded, multicenter, international, randomized trial [9]. Seventeen sites participated, 12 in the US, 3 in the UK and 2 in Australia/New Zealand. The study, which enrolled subjects between October 2015 and December 2016, included men age 45–80 years with a prostate size between 30–80 cc (measured with transrectal ultrasound), moderate-to severe LUTS as indicated by an International Prostate Symptom Score (IPSS [10]) ≥ 12 and a maximum urinary flow rate (Qmax) < 15 ml/s. Men were excluded if they had a history of prostate or bladder cancer, neurogenic bladder, bladder calculus or clinically significant bladder diverticulum, active infection, treatment for chronic prostatitis, diagnosis of urethral stricture, meatal stenosis or bladder neck contracture, damaged external urinary sphincter, stress urinary incontinence, post-void residual > 300 ml or urinary retention, use of self-catheterization or prior prostate surgery. Men taking anticoagulants or on bladder anticholinergics or with severe cardiovascular disease were also excluded. The control group, TURP using electrocautery, represents the gold standard for the surgical treatment of moderate-to-severe BPH for patients within this volume range. All participants provided informed consent prior to participating.
The randomization scheme was a 2:1 ratio (Aquablation:TURP). Stratification was done by study site and baseline IPSS score category with random block sizes. The assignment was generated by a web-based system prior to treatment.
Aquablation was performed using the AquaBeam System (PROCEPT BioRobotics, Redwood Shores, CA, USA) [11]. Following Aquablation hemostasis was achieved using either low-pressure inflation of a Foley balloon catheter in the prostatic fossa or non-resective electrocautery [12]. TURP was performed with either a monopolar or bipolar loop per surgeon preference followed by continuous bladder irrigation.
A blinded research team (physician and coordinator) performed all follow-up assessments. The visits included IPSS, uroflow measurements, quality of life, adverse events and blinding assessment. The initial protocol blinded subjects through the primary end point. A subsequent protocol modification during enrollment had extended blinding out to 3 years. The latter asked subjects to guess (at each visit) which treatment was received. Reasons for perceived unblinding were collected.
The primary efficacy end point, non-inferiority for the 6-month change in IPSS, was met and previously reported [9]. The focus herein is 2-year efficacy outcomes. Repeated measures analysis of variance was used for continuous variable changes at postoperative time points. The primary safety end point, the occurrence of procedure-related complications rated as Clavien-Dindo [13] grade 1 persistent or higher at 3 months, showed superiority. Events to month 12 were also reported previously. The focus of analysis herein is events occurring between months 12 and 24; differences in event rates were compared using Fisher’s test. Note that per the study protocol, adverse events occurring after month 12 were not adjudicated by the CEC. All study data were verified by independent study monitors.
Compliance with Ethics Guidelines
All procedures performed to gather the data presented here were approved by all of the institutional research committees (see Supplementary Material 5). They also adhered to the relevant national research committees and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Results
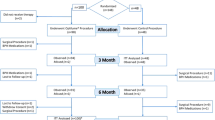
One hundred eighty-four subjects were randomized with three subjects (2 TURP, 1 Aquablation) voluntarily withdrawing before treatment, resulting in a cohort of 181. Baseline characteristics were balanced across treatment assignment (Table 1). Mean prostate size was 53 cc, and 91% of the subjects were sexually active. A 24-month follow-up was obtained in 169 subjects (93%, Fig. 1).
Blinding was preserved through 2 years. At 2 years, the proportion of subjects guessing they underwent Aquablation was higher in the Aquablation group compared with TURP (35% vs. 11%, p = 0.0021). Those reporting potential unblinding were more likely to correctly guess their treatment; those not reporting unblinding were not. The root cause of this is mostly due to earlier versions of the protocol when patients were only blinded through the primary end point. Unblinding was associated with slightly higher IPSS and IPSS QOL improvements; however, there were no systematic differences across treatment groups in subjects reporting unblinding or not.
IPSS reduction at 2 years was 14.7 (7.1) in the Aquablation group and 14.9 (7.3) in the TURP group (p = 0.8304 for difference, Fig. 2); 89% and 95% of each group had an improvement of at least five points from baseline IPSS, respectively. Repeated measures analysis showed no statistically significant difference in postoperative change scores across groups or any statistical interaction between time and treatment. Mean 2-year IPSS quality of life score improvement was also similar in both groups [3.2 (1.7) vs. 3.3 (1.5), p = 0.7007] (see Supplementary Tables 1, 2).
Two-year urinary flow rates increased markedly within 1 month after surgery for both groups and were maintained at 2 years, with mean improvements of 11.2 (11) cc/s for Aquablation vs. 8.6 (12.2) cc/s for TURP (Fig. 3, p = 0.1880). Two-year reduction in post-void residual was 57 (78) and 70 (101) cc (p = 0.3894). In patients with an elevated (> 100 cc) post-void residual, mean 2-year reductions in post-void residual were 107 and 114 cc, respectively (see Supplementary Table 3). At 2 years, PSA was reduced significantly in both groups by 1 point (p < 0.01).
Among sexually active men without the condition at baseline, anejaculation was less common after Aquablation (10%) vs. TURP (36%), p = 0.0003. The rate of anejaculation after Aquablation was somewhat lower when post-Aquablation cautery was avoided (7% vs. 16%, p = 0.1774). Ejaculatory function as assessed by MSHQ-EjD was better in Aquablation compared with TURP through 2 years (Fig. 4). There were no de novo erectile dysfunction events in either arm. Of note, the Aquablation arm change scores for all IIEF-15 domains showed no changes compared with baseline (Fig. 5).
Adverse events to 1 year have been previously reported (see Supplementary Tables 4, 5). Between year 1 and 2, the rate of most individual events was low (Table 2) and similar across groups. Two Aquablation subjects (1.7%) and zero TURP subjects underwent surgical retreatment for BPH between 1 and 2 years of index treatment (p = 1). Overall, 2-year retreatment rates were 4.3% and 1.5% (p = 0.4219), respectively.
Discussion
Aquablation is a novel treatment for LUTS due to BPH, and its evidence base is increasing. In this prospective randomized trial, prospective 2-year follow-up showed continued improvements in symptom scores, quality of life and uroflow parameters after Aquablation with effects of nearly identical size to that of TURP. As reported previously, subjects undergoing Aquablation had a lower risk of anejaculation soon after the procedure compared with TURP. We observed no adverse events related to erectile function, and all other perioperative risks were similar between the two treatments. Between year 1 and 2, no adverse events occurred more commonly in the Aquablation group compared with TURP, and the overall risk of adverse urologic outcomes was low. Importantly, the cumulative rate of surgical retreatment for BPH symptoms was very low (4.3% Aquablation, 1.5% TURP), and, as reported previously, most men were able to stop BPH-related medications (alpha blockers, 5-ARIs). Combined with results of other prospective trials, 2-year results from our study provide compelling medium-term evidence for the safety and effectiveness of Aquablation in men with LUTS due to BPH.
Improvements in the objective measure of urinary flow rate and post-void residual were similar to those observed for other resective surgeries, including laser enucleation [14] and laser photovaporisation [15] Aquablation’s symptom score improvements appeared to be larger than those reported for non-resective techniques, such as the convective water vapor energy (rezum®, 3.3 points higher) [16] and UroLift® procedure (3.7 points higher) [17].
The lower rate of anejaculation after Aquablation is consistent with the procedure’s overall design, which avoids damage to tissues involved in ejaculation through precise, image-based targeting and robotic execution.
Advantages of our study included prospective assessment of symptom score and urinary function in an international, randomized design. Subject blinding, as assessed by the ability of subjects to guess which treatment they received, was preserved to year 2, when some amount of unblinding occurred. Subgroup analysis confirmed that this modest unblinding did not affect symptom score changes across treatments.
The high levels of efficacy observed in our study were obtained by urology surgeons with years of TURP experience but had much less, in most cases no, experience with Aquablation, suggesting a more abbreviated learning curve for Aquablation.
The study’s maximum prostate size was 80 cc, which is a potential limitation to generalizability. However, a similar study in large prostates (WATER II, prostate size 80–150 cc) has shown similarly high levels of symptom relief and a markedly lower rate of postoperative anejaculation [18].
Conclusion
In summary, the study provides longer term, durable evidence of the safety and effectiveness of Aquablation for LUTS due to BPH in men with prostates < 80 cc. Aquablation may be an alternative for men who strongly prefer maintenance of ejaculatory function.
References
Trueman P, Hood SC, Nayak US, et al. Prevalence of lower urinary tract symptoms and self-reported diagnosed “benign prostatic hyperplasia”, and their effect on quality of life in a community-based survey of men in the UK. BJU Int. 1999;83:410–5.
Naslund MJ, Gilsenan AW, Midkiff KD, et al. Prevalence of lower urinary tract symptoms and prostate enlargement in the primary care setting. Int J Clin Pract. 2007;61:1437–45.
Madersbacher S, Marberger M. Is transurethral resection of the prostate still justified? BJU Int. 1999;83:227–37.
McVary KT, Roehrborn CG, Avins AL, et al. Update on AUA guideline on the management of benign prostatic hyperplasia. J Urol. 2011;185:1793–803.
Miano R, De Nunzio C, Asimakopoulos AD, et al. Treatment options for benign prostatic hyperplasia in older men. Med Sci Monit Int Med J Exp Clin Res. 2008;14:RA94–R102.
Rassweiler J, Teber D, Kuntz R, et al. Complications of transurethral resection of the prostate (TURP)—incidence, management, and prevention. Eur Urol. 2006;50:969–79 (discussion 980).
Montorsi F, Moncada I. Safety and tolerability of treatment for BPH. Eur Urol Suppl. 2006;5:1004–122.
Emberton M, Neal DE, Black N, et al. The effect of prostatectomy on symptom severity and quality of life. Br J Urol. 1996;77:233–47.
Gilling P, Barber N, Bidair M, et al. WATER: a double-blind, randomized, controlled trial of Aquablation® vs transurethral resection of the prostate in benign prostatic hyperplasia. J Urol. 2018;199:1252–61.
Barry MJ, Fowler FJ, O’Leary MP, et al. The American Urological Association symptom index for benign prostatic hyperplasia. The Measurement Committee of the American Urological Association. J Urol. 1992;148:1549–57 (discussion 1564).
Gilling P, Reuther R, Kahokehr A, et al. Aquablation—image-guided robot-assisted waterjet ablation of the prostate: initial clinical experience. BJU Int. 2016;117:923–9.
Aljuri N, Gilling P, Roehrborn C. How I do it: balloon tamponade of prostatic fossa following Aquablation. Can J Urol. 2017;24:8937–40.
Dindo D, Demartines N, Clavien P-A. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Li S, Zeng X-T, Ruan X-L, et al. Holmium laser enucleation versus transurethral resection in patients with benign prostate hyperplasia: an updated systematic review with meta-analysis and trial sequential analysis. PLoS One. 2014;9:e101615.
Bachmann A, Tubaro A, Barber N, et al. 180-W XPS GreenLight laser vaporisation versus transurethral resection of the prostate for the treatment of benign prostatic obstruction: 6-month safety and efficacy results of a European Multicentre Randomised Trial–the GOLIATH study. Eur Urol. 2014;65:931–42.
McVary KT, Roehrborn CG. Three-year outcomes of the prospective, randomized controlled Rezūm system study: convective radiofrequency thermal for treatment of lower urinary tract symptoms due to benign prostatic hyperplasia. Urology. 2018;111:1–9.
Roehrborn CG, Gange SN, Shore ND, et al. The prostatic urethral lift for the treatment of lower urinary tract symptoms associated with prostate enlargement due to benign prostatic hyperplasia: the L.I.F.T. study. J Urol. 2013;190:2161–7.
Chughtai B, Thomas D. Pooled aquablation results for american men with lower urinary tract symptoms due to benign prostatic hyperplasia in large prostates (60–150 cc). Adv Ther. 2018;35:832–8.
Acknowledgements
The authors wish to acknowledge the research coordinators and patients who participated in this study.
Funding
WATER, the article processing fees and the Open Access fee were funded by PROCEPT BioRobotics. All authors had full access to all of the data in this study and take complete responsibility for the integrity of the data and accuracy of the data analysis.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole and have given their approval for this version to be published.
Disclosures
Mihir Desai is a consultant for PROCEPT BioRobotics and Auris Surgical. Mo Bidair is a consultant for PROCEPT BioRobotics and has performed commercial Aquablation procedures. Eugene Kramalowsky is a consultant for PROCEPT BioRobotics. Peter Gilling has performed commercial Aquablation procedures. Neil Barber has performed commercial Aquablation procedures. Paul Anderson has performed commercial Aquablation procedures. Mark Sutton, Tev Aho, Andrew Thomas, Barrett Cowan, Ronald P. Kaufman, Jr., Andrew Trainer, Andrew Arther, Gopal Badlani, Mark Plante, Leo Doumanian, Alexis E. Te, Mark DeGuenther and Claus Roehrborn have nothing to disclose.
Compliance with Ethics Guidelines
All procedures performed to gather the data presented here were approved by all of the institutional research committees [see Supplementary Material Table 5]. They also adhered to the relevant national research committees and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Data Availability
The datasets generated during and/or analyzed during the current study are not publicly available due to confidentially and intellectual property reasons, but some data may be available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced Digital Features
To view enhanced digital features for this article go to https://doi.org/10.6084/m9.figshare.7937555.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Gilling, P., Barber, N., Bidair, M. et al. Two-Year Outcomes After Aquablation Compared to TURP: Efficacy and Ejaculatory Improvements Sustained. Adv Ther 36, 1326–1336 (2019). https://doi.org/10.1007/s12325-019-00952-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-019-00952-3