Abstract
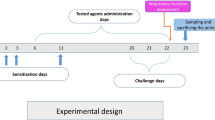
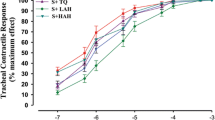
Effects of quercetin inhalation on immediate (IAR), late-phase (LAR) and late late-phase (LLAR) asthmatic responses by exposure to aerosolized-ovalbumin (AOA) (2w/v% in saline, inhalation for 3 min) were studied in conscious guinea-pigs sensitized with AOA. We measured specific airway resistance (sRaw), and recruitment of leukocytes, histamine and protein contents and phospholipase A2 (PLA2) activity in bronchoalveolar lavage fluid (BALF). Effects of quercetin (10 mg/mL, inhalation for 2 min) compared with cromolyn sodium, salbutamol, and dexamethasone inhalations, respectively. Quercetin inhalation decreased sRaw by 57.15 ± 3.82% in IAR, 57.72 ± 7.28% in LAR, and 55.20 ± 5.69% in LLAR compared with AOA-inhaled control. Salbutamol inhalation (5 mg/mL) significantly inhibited sRaw in IAR, but inhalations of cromolyn sodium (10 mg/mL) and dexamethasone (5 mg/mL) significantly inhibited sRaw in IAR, LAR and LLAR, respectively. Inhibitory activity of quercetin inhalation on sRaw was similar to effect of its oral administration (10 mg/kg) in asthmatic responses. Quercetin (10 mg/mL, inhalation for 2 min) significantly decreased histamine and protein contents, PLA2 activity, and recruitments of leukocytes in BALF and also improved slightly infiltration of eosinophils and neutrophils in histopathological survey. Its anti-asthmatic activity was similar to cromolyn sodium and dexamethasone.
Similar content being viewed by others
Abbreviations
- AOA:
-
Aerosolized ovalbumin
- BALF:
-
Brochoalveolar lavage fluid
- BSA:
-
Bovine serum albumin
- BSS:
-
Balanced salt solution
- DMSO:
-
Dimethylsulfoxide
- EOS:
-
Eosinophils
- H & E:
-
Hematoxylin and eosin
- HEPES:
-
4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid
- IAR:
-
Immediate-phase asthmatic response
- IgE:
-
Immunoglobulin E
- LAR:
-
Late-phase asthmatic response
- LLAR:
-
Late late-phase asthmatic response
- OA:
-
Ovalbumin
- PLA2 :
-
Phospholipase A2
- PMN:
-
Polymorphonuclear leukocytes
- 10-Pyrene PC:
-
Pyrene-labeled phospholipids
- sRaw:
-
Specific airway resistance
References
Benhamou, A. H., Vanini, G., Lantin, J. P., and Eigenman, P. A., Antihistamine and sodium cromoglycate medication for food cold water exercise-induced anaphylaxis. Allergy, 62, 1471–1472 (2007).
Crompton, G., A brief history of inhaled asthma therapy over the last fifty years. Prim. Care Respir. J., 15, 326–331 (2006).
Fewtrell, C. M. S. and Gomperts, B. D., Effect of flavone inhibitors of transport ATPases on histamine secretion from rat mast cells. Nature, 265, 635–636 (1997).
Hirai, S., Kim, Y. I., Goto, T., Kang, M. S., Yoshimura, M., Obata, A., Yu, R., and Kawada, T., Inhibitory effect of naringenin chalcone on inflammatory changes in the interaction between adipocytes and macrophages. Life Sci., 81, 1272–1279 (2007).
Huston, P. A., Chuch, M. K., Clay, T. P., Miller, P., and Holgate, S. P., Early and late-phase bronchoconstriction after allergen challenge of nonanesthetized guinea pigs. I. The association of disordered airway physiology to leukocyte infiltration. Am. Rev. Respir. Dis., 137, 548–557 (1988).
Hutson, P. A., Holgate, S. T., and Church, M. K., The effect of cromolyn sodium and albuterol on early and late phase bronchoconstriction and airway leukocyte infiltration after allergen challenge of nonanesthetized guinea pigs. Am. Rev. Respir. Dis., 138, 1157–1163 (1988).
Jiang, J. S., Shih, C. M., Wang, S. H., Chen, T. T., Lin, C. N., and Ko, W. C., Mechanisms of suppression of nitric oxide production by 3-O-methylquercetin in RAW 264.7 cells. J. Ethnopharmacol., 103, 281–287 (2006).
Jung, C. H., Lee, J. Y., Cho, C. H., and Kim, C. J., Anti-asthmatic action of quercetin and rutin in conscious guinea-pigs challenged with aerosolized ovalbumin. Ach. Pharm. Res., 30, 1599–1607 (2007).
Li, W. G., Zhang, X. Y., Wu, Y. J., and Tian, X., Anti-inflammatory effect and mechanism of proanthocyanidins from grape seeds. Acta Pharmacol. Sin., 22, 1117–1120 (2001).
Matsumoto, T., Ashida, Y., and Tsukuda, R., Pharmacological modulation of immediate and late airway response and leukocyte infiltration in the guinea pig. J. Pharmacol. Exp. Ther., 269, 1236–1244 (1994).
Morales, M. A., Tortoriello, J., Meckes, M., Paz, D., and Lozoya, X., Calcium-antagonist effect of quercetin and its relation with the spasmolytic properties of Psidium guajava L. Arch. Med. Res., 25, 17–21 (1994).
Nishino, H., Iwashima, A., Fujiki, H., and Suginuma, T., Inhibition by quercetin of the promoting effect of teleocidin on skin papilloma formation in mice initiated with 7,12-dimethylbenz [a]anthracene. Jpn. J. Cancer Res., 75, 113–116 (1984).
Chew Nora Y. K., Bagster Ddvid F., and Chan Hak-Kim, Effect of particle size, air fow and inhaler device on the aerosolisation of disodium cromoglycate powders, Int J Pharmaceut., 206, 75–83 (2000).
Omisore, N. O., Adewunmi, C. O., Iwalewa, E. O., Ngadjui, B. T., Adenowo, T. K., Abegaz, B. M., Ojewole, J. A., and Watchueng, J., Antitrichomonal and antioxidant activities of Dorstenia barteri and Dorstenia convexa. Braz. J. Med. Biol. Res., 38, 1087–1094 (2005).
Pennock, B. E., Pennock, C. P., Rogers, R. M., Cain, W. A., and Wells, J. H., A noninvasive technique for measurement of changes in specific airway resistance. J. Appl. Physiol., 46, 399–406 (1979).
Pettinari, A., Amici, M., Cuccioloni, M., Angeletti, M., Fioretti, E., and Eleuteri, A. M., Effect of polyphenolic compounds on the proteolytic activities of constitutive and immunoproteasomes. Antioxid. Redox. Signal., 8, 121–129 (2006).
Radvanyi, F., Jordan, L., Russo-Marie, F., and Bon, C., A sensitive and continuous fluorometric assay for phospholipase A2 using pyrene-labeled phospholipids in the presence of serum albumin. Anal. Biochem., 177, 103–109 (1989).
Ramesh, M., Rao, Y. N., Rao, A. V., Prabhakar, M. C., Rao, C. S., Muralidhar, N., and Reddy, B. M.., Antinociceptive and anti-inflammatory activity of a flavonoid isolated from Caralluma attenuata. J. Ethnopharmacol., 62, 63–66 (1998).
Sanjar, S., Aoki, S., Kristersson, Smith, D., and Moley, J., Antigen challenge induces pulmonary airway eosinophil accumulation and airway hyperreactivity in sensitized guinea-pigs: the effect of anti-asthma drugs. Br. J. Pharmacol., 99, 679–686 (1990).
Shibata, S., Inoue, H., Iwata, S., Ma, R. D., Yu, L. J., Ueyama, H., Takayasu, J., Hasegawa, T., Tokuda, H., and Nishino, A., Inhibitory effects of licochalcone A isolated from Glycyrrhiza inflata root on inflammatory ear edema and tumour promotion in mice. Planta Med., 57, 221–224 (1991).
Shore, P. A., Burkhalter, A., and Cohn, V. H. Jr., A method for the fluorometric assay of histamine in tissues. J. Pharmacol. Exp. Ther., 127, 182–186 (1959).
Skaltsa, H., Bermejo, P., Lazari, D., Silvan, A. M., Skaltsounis, A. L., Sanz, A., and Abad, M. J., Inhibition of prostaglandin E2 and leukotriene C4 in mouse peritoneal macrophages and thromboxane B2 production in human platelets by flavonoids from Stachys chrysantha and Stachys candida. Biol. Pharm. Bull., 23, 47–53 (2000).
Su, Y. C., Peng, H. J., Wang, S. R., Han, S. H., and Tsai, J. J., Effect of BCG on ovalbumin-induced bronchial hyperreactivity in a guinea pig asthma model. J. Microbiol., Immunol. Infect. 34, 25–34 (2001).
Toward, T. J. and Broadley, K. J., Early and late bronchoconstrictions, airway hyper-reactivity, leucocyte influx and lung histamine and nitric oxide after inhaled antigen: effects of dexamethasone and rolipram. Clin. Exp. Allergy, 34, 91–102 (2004).
Villar, A., Gasco, M. A., and Alcaraz, M. J., Anti-inflammatory and anti-ulcer properties of hypolaetin-8-glucoside, a novel plant flavonoid. J. Pharm. Pharmacol., 36, 820–823 (1984).
Wu, M. J., Wang, L., Ding, H. Y., Weng, C. Y., and Yen, J. H., Glossogyne tenuifolia acts to inhibit inflammatory mediator production in a macrophage cell line by down-regulating LPS-induced NF-kappa B. J. Biomed. Sci., 11, 186–199 (2004).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moon, H., Choi, H.H., Lee, J.Y. et al. Quercetin inhalation inhibits the asthmatic responses by exposure to aerosolized-ovalbumin in conscious guinea-pigs. Arch. Pharm. Res. 31, 771–778 (2008). https://doi.org/10.1007/s12272-001-1225-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12272-001-1225-2