Abstract
Self-report questionnaires are in widespread use in the assessment of adults with suspected attention-deficit and hyperactivity disorder (ADHD). Notwithstanding the high degree of validity, these questionnaires are considered to possess, their stand-alone use in assessment for adult ADHD may result in false-positive diagnoses due to the risk of negative response bias. Most of the self-report questionnaires in typical use are based on the diagnostic systems DSM-5 or ICD-10. From a neuropsychological point of view, however, testing of various executive function abilities and attentional performance is important in the assessment of adult ADHD. The present study (N = 211) found no evidence linking executive function (working memory and inhibitory processes) and attentional performance (processing speed) to the results of a self-report questionnaire, the ADHS-LE. The number of failures on the three symptom or performance validity tests (SVT/PVT) used provided the sole, and significant, explanation for the response behavior reported on the ADHS-LE. Of these three SVT/PVTs (the German version of the Structured Inventory of Malingered Symptomatology, SIMS, the reliable digit span, and the standard deviation of simple reaction time), only the SIMS was found to be a significant predictor variable. In the clinical context of this study, 32.6% of subjects produced at least one invalid SVT/PVT result. The use of a more conservative criterion—failure on at least two of the three SVT/PVTs deemed to be feigning ADHD—reduced the proportion of participants generating invalid values to 5%.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Attention-deficit and hyperactivity disorder (ADHD) is a mental disorder in childhood and adulthood. The global prevalence is 5% in children and around 3% in adults (cf. Hesson & Fowler, 2015; Polanczyk et al., 2014; de Zwaan et al., 2012). The state-of-the-art treatment is a combination of drug therapy and psychotherapeutic intervention (cf. Scholz et al., 2020). Pharmaceutical treatment of ADHD makes a distinction between stimulants and non-stimulants (for an overview see Elliot et al., 2020).
Assessment of ADHD frequently involves the use of self-report questionnaires which ask subjects to indicate the manifestation and frequency of potential ADHD symptoms they experience. These questionnaires are generally based on the DSM-5 (Falkai & Wittchen, 2018) and ICD-10 (Dilling et al., 2015) diagnostic systems and are associated with a high degree of validity with regard to the diagnosis of ADHD (in the case of children, see, e.g., Döpfner et al. (2006) and Alexandre et al. (2018); for adults, see, e.g., De Quiros and Kinsbourne (2001) and Retz et al. (2013)). The ADHS-LE (Schmidt & Petermann, 2013) is a self-report questionnaire for use in German-speaking regions with adult subjects.
Alongside self-report questionnaires, clinical interviews based on the DSM-5 criteria (Falkai & Wittchen, 2018) are available for assessment of possible ADHD (cf. Heine & Exner, 2021, p. 142; Sagar et al., 2017, p. 108). The diagnostic criteria it details reflect behavioral, cognitive, and emotional variables and do not call or provide for the use of neuropsychological assessment procedures. From a neuropsychological point of view, however, a simple description of notable behavior, as the criteria of the DSM-5 envisage, does not seem to suffice; instead, a robust assessment of the disorder’s severity, and a suitable treatment plan, requires psychological testing to the end of quantifying the characteristic behavior displayed. The results of neuropsychological tests, drawing on classical test theory (cf. Pawlik, 2006), enable findings independent of the individual administering the tests and may therefore serve as a corrective to the simple observation of behavior.
Alongside issues with attentional performance—such as imprecision during the completion of a task, the overlooking of details, and problems with sustained attention—the symptoms are listed in DSM-5 reference components of executive function (EF), including impulse control, focus, and the capacity to plan or to complete a task. Including evaluating EF in the assessment of ADHD is challenging. One difficulty in this regard is defining the constituent components of EF. This is why clinical neuropsychology considers disorders of EF to be syndrome diagnoses, that is, collections of discrete symptoms that do not necessarily always occur together. The overview by Duff and Sulla (2015), considering the extent to which psychological testing can assess EF in children, found the neuropsychological tests typically used to assess EF to be insufficiently specific for the symptomatology of ADHD. Barkley and Murphy (2011) failed to identify any connection between symptoms of adult ADHD and several neuropsychological tests of EF. They used the digit span test from the Learning and Memory Battery (LAMB, Schmidt & Tombaugh, 1995), the Conners Continuous Performance Test (CPT, Conners, 2014), the Stroop Color and Word Test (Trenerry et al., 1989), the Wisconsin Card Sorting Test (Heaton et al., 1993), and the Five-Point Test of Design Fluency (Ruff, 2011). The group of subjects with ADHD did not differ significantly, in terms of performance on EF tests, from a clinical control group (Barkley & Murphy, 2011, Table 5, p. 151). Suhr et al. (2008) likewise demonstrated that tests of EF (TMT-B, Reitan, 1992; Stroop Color and Word Test, Golden, 1978) were unable to distinguish between subjects with ADHD and those with symptoms of other psychological disorders.
In spite of these findings, Duff and Sulla (2015, p. 192f) hold that there is an overall benefit to the use of neuropsychological tests of performance for assessing EF in subjects with possible symptoms of ADHD. They argue that assessment of EF has the potential to improve the quality of the assessment of ADHD symptomatology, including making differential diagnoses and predicting the future course of the patient’s ADHD symptoms. Boonstra et al. (2005), while affirming the need for improved neuropsychological tests in this area, were disinclined to deny the significance of components of EF to ADHD symptomatology. Findings from genetic research likewise support the utility of assessing EF in the presence of possible ADHD symptoms. For example, Pinto et al. (2016) found that children with symptoms of ADHD experienced deficits in response inhibition exhibited in errors of commission and omission during a go/no-go task. Similarly, Frazier-Wood et al. (2012), drawing on genetic data, emphasize the importance of working memory, as an EF, among the symptoms of ADHD. A final point in favor of assessing EF is the fact that symptoms of ADHD are accompanied by a disturbance of the frontoparietal network and additional fiber structures associated with the frontal lobe (Chen et al., 2016; Gao et al., 2019; Munro et al., 2018). There are also abnormalities of the dopaminergic transmitter systems that affect the frontostriatal brain regions and consequently executive functions (cf. Cools et al., 2019).
For some years now, pharmaceuticals used to treat ADHD in adults have increasingly been subject to abuse; students, for example, may endeavor to enhance their cognitive performance by taking stimulants. In a systematic review, Wilens et al. (2008) identified 21 studies that addressed the abuse of stimulants in adolescent subjects and young adults with and without ADHD. They found that, in addition to taking stimulants themselves, 16–29% of the students involved in the studies also gave them to others or acted as dealers. In 2011, Looby and Earlywine noted that the non-medical use of stimulants (such as methylphenidate) had increased and was being monitored by the US Drug Enforcement Administration. More recently, Faraone et al. (2020) reviewed 111 studies addressing the non-medical use of stimulants, with students representing the largest group examined in this context.
In similar studies conducted outside the USA, Fuermaier et al. (2021) found, working in the Netherlands, that 16% of students in higher education were taking stimulants without a prescription. Among the intentions behind the students’ behavior was to obtain adjustments and accommodations for a putative health condition and in so doing boost their attainments. Gudmundsdottir et al. (2020) record that 13% of students in their Iceland-based sample were taking stimulants without a prescription. Work on this issue in the wider English-speaking world has included the finding by Lucke et al. (2018) that 6.5% of Australian students are abusing stimulants.
Efforts to improve cognitive performance by taking of stimulants or the wish to obtain them to sell on for financial gain represent extraneous motivations for undergoing assessment for ADHD (cf. Rabiner, 2013). In our internet age, information on symptoms of ADHD is easily accessible, providing easy means of feigning ADHD symptoms during assessment. As is to be expected, the frequency of negative response bias varies with the type and number of symptom validity tests (SVT) or performance validity tests (PVT) used in the various studies and with their designs (subjects pre-instructed to simulate, as in, for example, Becke et al. (2021) versus clinical control groups, as in, for instance, Pollock et al. (2021)). An overview by Sagar et al. (2017) placed the percentage of university students presenting for ADHD assessment who feigned ADHD symptoms at 25 to 50%. Johnson and Suhr (2021) found that 22.3% of students made an invalid symptom presentation on at least one of three embedded SVT indices in the CAARS. These indices were the inconsistent responding index and cutoff T-score > 80 (Conners et al., 1999) and the CAARS infrequency index (Suhr et al., 2011). Potts et al. (2021) have proposed the multidimensional ADHD rating scale (MARS) as a way of identifying research subjects (undergraduate students from psychology classes) that show invalid response behaviors. Alongside symptom-relevant items, MARS encompasses a further 108 potential SVT items. Potts et al. (2021) calculated a symptom validity index based on 11 of these 108 items. Of the students included in the study, 58.9% produced an invalid MARS validity index score. Using a stand-alone PVT (medical symptom validity test (MSVT) Green (2004)) as well as the CAARS infrequency index, Pollock et al. (2021) found that 43.8% of the participants failed at least one of the three MSVT parameters.
The present study investigates the relationship between the results of an ADHD self-report questionnaire and the results of executive function (EF) and attention tests when SVT/PVTs are used to identify possible negative response bias arising from secondary motivations.
Methods
Participants
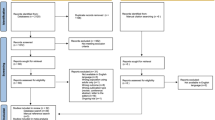
The adult subjects had presented themselves consecutively to the first author’s clinical practice for neuropsychological testing for suspected adult ADHD and, thus, were an unselected, clinical sample. Two hundred and twenty-one subjects were involved, of whom 102 were men and 119 women. Because the men (M = 39.0 years of age, SD = 12.6) were significantly older than the women (M = 34.5 years of age, SD = 10.2; t = 3.0, df = 219, p < .01), we included age and gender as covariates in subsequent statistical analyses.
Tests of Neuropsychological Performance
The present study used neuropsychological tests that primarily assess inhibitory processes and working memory, supplemented by TMT-B (Reitan, 1992). Drawing on recent research, we additionally included tests of processing speed in the test battery used (e.g., LeRoy et al., 2019; Onandia-Hinchado et al., 2021). Table 1 provides an overview of the neuropsychological tests selected for the study. The test of attentional performance (TAP) (Zimmermann & Fimm, 2016) is a computer-aided procedure for examining various aspects of attentional and executive functions. The TAP subtests employed in this study each involved speed and accuracy components. The accuracy component consists of commission errors and omission errors. We treated the speed component as pertaining to attentional performance and accuracy as being executive functions.
In the alertness subtest, subjects react to an “X” that appears at a fixation point in the center of the screen. The test is run a total of four times under two different sets of conditions: for the first and fourth times, the “X” appears on the screen without any warning; for the second and third times, an aural warning signal precedes its appearance. In the go/no-go subtest, either an “X” or a plus sign appears on the screen. Prior to the subtest’s commencement, subjects are instructed not to react to the plus sign. This subtest measures both reaction speed and the number of errors made. The visual scanning subtest consists of a 5 × 5 matrix comprising 25 boxes with openings facing upwards, to the left, right, or downwards. Only 50% of the matrices contain a box with an opening facing upwards, which is the type participants are required to find. Finally, the incompatibility subtest uses the Simon effect (Simon, 1969) to test susceptibility to interference. Arrows pointing left or right are displayed to the left or right of a fixation point. This exercise involves subjects pressing an appropriate reaction button with their left or right hand, depending on the direction of the arrow shown; they are supposed to respond in this way regardless of whether the arrow appears to the left or right of the fixation point.
Self-Report Questionnaire for ADHD
We used the ADHS-LE (Schmidt & Petermann, 2013), developed for adults, as a self-report questionnaire for ADHD symptoms. The questionnaire is based on the ICD-10 (Dilling et al., 2015) and DSM-IV-TR (Sass et al., 2003) diagnostic manuals and diagnostic guidelines pursuant to Wender (Utah criteria, Ward et al., 1993). It consists of 64 items, with standardization based on a representative sample (N = 1 296). It encompasses six separate scales: attentional regulation, impulse control/inhibition, stress tolerance, emotion/affect, restlessness/over activity, and extraversion. The values attained in these scales go to calculate an overall score which represents the global severity of the patient’s symptoms and is intended to assist with monitoring the course of treatment. Completion of the ADHS-LE takes 10–15 min. The reliability of the overall score is α = .93, while the reliabilities attained by the individual scales are between α = .77 and α = .84. It is possible to convert the raw scores into T-scores or percentiles to aid diagnostic assessment. Scores that diverge from the mean by more than one standard deviation are classified as abnormal, and clinical significance attaches to scores more than two standard deviations from the mean. The sensitivity of the ADHD-LE is 95%; the specificity is 83% (Schmidt & Petermann, 2011). Each separate scale correlates significantly (p = .01) with each of the others (0.27 < r < .61) and with the overall score (0.56 < r < .83); for this reason, we selected the overall score for the questionnaire as the independent variable for the present study.
Symptom and Performance Validity Testing
The now seminal factor analysis conducted by Van Dyke et al., (2013, p. 1240) distinguishes between cognitive performance, performance validity, and self-reported symptoms including both standard and symptom validity measures. Tests of self-reported symptoms encompass both clinical self-report questionnaires and tests that measure over-reporting. Stand-alone tests and embedded parameters calculable using items from existing psychological assessment methods (cf., e.g., Sagar et al., 2017, p. 107) are available for both of these types of tests (SVT/PVT). In line with these definitions, the present study used one SVT and two PVT. The German version of the Structured Inventory of Malingered Symptomatology (SIMS; German abbreviation, SFSS; Cima et al. (2003)) was employed as a stand-alone SVT. We made this choice to enable us to control for participants’ exaggerated accounts of psychiatric symptoms. Grant et al. (2020) had used this test with subjects who had been instructed to simulate symptoms of ADHD and found it to have high specificity (100%) but lower sensitivity (cutoff score of > 16: 36%; cutoff score of > 14: 52%). Van Impelen et al. (2014) identified a good ability of SIMS to distinguish between groups of pre-instructed simulators and control groups in relation to simulated psychopathological symptoms. In an ADHD context, the results generated by SIMS remained stable even where the person administering the test made a strong moral appeal to the subject’s honesty (Niesten et al., 2017). Scores equal to or greater than 20 were classified as invalid (Van Impelen et al., 2014). As impairments in cognitive performance capacity are—at least from a neuropsychological point of view—concomitants of ADHD symptoms, we additionally ran two PVT. The reliable digit span (RDS, e.g., Babikan et al. (2006)) and the standard deviation of simple reaction time (SDRT, Bodenburg, 2014; Czornik et al., 2021; Stevens et al., 2016) were used as embedded PVT. In relation to ADHD, the RDS demonstrated its strong capacity, as found in other studies, to distinguish between pre-instructed simulators and a control group (Rogers, Velsor, Donnelly 2nd & Dean, 2021). The RDS was classified as invalid if equal to or lower than 7. We measured the SDRT under two sets of conditions (with and without a prior warning signal) and classified the results as invalid if they were at least two standard deviations below the mean value of standard deviation of simple reaction time in the TAP normative sample (percentile < 2.3).
Statistical Analysis
Raw values of the ADHS-LE questionnaire were dependent variables in this study. Continuous predictor variables in the ANCOVA were the subjects’ age and the number of years of formal schooling education they had completed, the number of invalid SVT/PVT, and the total (added-up) number of instances of impaired attentional performance. An instance of attentional performance was classified as impaired if the individual test value was at least one standard deviation below the published mean value of the normative sample (percentile < 16). This classification was required because raw values were available for the TMT-A and TMT-B only, while for the other tests of attention, the data set solely included percentiles of the raw values. Categorical predictor variables in the ANCOVA were the gender of subjects and dichotomized EF. If two or more of the six tests of EF showed impairment, EF overall was classified as impaired (cf. Lovejoy et al., 1999). A test of EF was classified as impaired if the individual raw test value was at least one standard deviation below the published mean value of the normative sample (percentile < 16).
Results
Impairments of EF appeared in 54 subjects (24.4%). Table 2 shows the number of years of formal schooling completed in the sample and frequencies of each number/category of years.
Table 3 contains the number of invalid SVT/PVT; fails were most frequent in the SFSS.
Using the criteria of Berthelson et al. (2013) and Larrabee (2014), 5% of subjects in the present study exhibited at least two invalid SVT/PVT and, consequently, negative response bias. Table 4 illustrates the frequency of invalid SVT/PVT.
Univariate covariance analysis using the ADHS-LE questionnaire as the dependent variable was, on the whole, statistically significant (F = 4.7, p < .001, df = 7, η2 = .13). Of the predictor variables, only the number of invalid SVT/PVT represented a significant source of variance. None of the other predictor variables (age, gender, years of formal schooling, EF, attentional performance) attained statistical significance (see Table 5 for details).
The probability of error of p = .12 arose in relation to age. While age also had no statistically significant effect, a slightly negative, insignificant correlation (r = − .1, p = .17) emerged between age and the raw values in the ADHS-LE; this took the form of a tendency among older subjects to attain lower raw values in the ADHS-LE. There was a positive correlation of the raw values of the ADHS-LE with the number of invalid SVT/PVT (r = .33, p < .001). This means that a greater number of invalid SVT/PVT correlated with higher values in the ADHS-LE questionnaire. The post hoc comparison indicated that, on average, subjects with negative response bias (two or three invalid SVT/PVTs) had considerably higher total values in the ADHS-LE than subjects who did not meet the criterion for negative response bias (no or only one invalid SVT/PVT, see Table 6 for details).
The explained variance in the statistical model increases somewhat if the individual raw scores of the SVT/PVT, instead of the total of invalid SVT/PVTs, are added as predictor variables when examining symptom validity assessment (F = 4.7, p < .001, df = 10, η2 = .18). EF, attentional performance, age, years of formal schooling, and gender also remained statistically insignificant here. Of the three SVT/PVTs, only the SFSS (the German version of the Structured Inventory of Malingered Symptomatology) was a significant predictor variable (see Table 7 for details).
Discussion
From a neuropsychological point of view, components of EF and attentional performance are constituent elements of the symptoms of adult attention-deficit and hyperactivity disorder. This study found no correlation between components of these two neuropsychological functions and the results attained in an ADHD self-report questionnaire (ADHS-LE). Of the three PVT/SVT used—the SFSS (the German version of the Structured Inventory of Malingered Symptomatology), the reliable digit span and the standard deviation of simple reaction time—only the SFSS was a significant predictor of the ADHS-LE scores. Further, 32.6% of subjects failed at least one of the three SVT/PVTs used. Five percent of subjects met the more conservative criterion for negative response bias, i.e., the failure of at least two of the three SVT/PVTs.
The fact that an SVT accounted for so much variance on the ADHS-LE does not fundamentally call into question the validity of self-report questionnaires in assessing ADHD symptoms nor their widespread use. This said, the use of such self-report questionnaires in isolation brings with it the risk of false-positive diagnostic decisions. We therefore do not recommend the use of these questionnaires as stand-alone diagnostic procedures. Indeed, Sagar et al. (2017) found that, without taking into account the possibility of their being completed in an invalid manner, stand-alone self-report questionnaires are unable to distinguish reliably between subjects with and without ADHD.
In the present study, the results of an ADHD self-report questionnaire did not reveal an association with components of EF and attentional performance. However, this appears to be due to the lack of specificity and sensitivity of the tests of EF and attentional performance used here in assessing ADHD symptomatology. Research findings on the relationship of components of EF in particular to ADHD symptomatology are mixed (Barkley & Murphy, 2011; Boonstra et al., 2005; Butzbach et al., 2019; Duff & Sulla, 2015; Frazier-Wood et al., 2012; Gawrilow et al., 2011; Heine & Exner, 2021; Merkt et al., 2013; Onandia-Hinchado et al., 2021; Pinto et al., 2016; Rosch & Mostofsky, 2019; Sebastian et al., 2014). Heine and Exner (2021, p. 146) attribute this principally to the heterogeneity of ADHD symptoms and the plethora of different neuropsychological tests of performance employed in research in this area to date. They opined that neuropsychological tests are of minor importance in the assessment of ADHD.
This notwithstanding, there are a number of arguments in support of assessing EF in the context of symptoms suggestive of adult ADHD. Genetic research suggests that inhibitory processes and working memory, both components of EF, appear to be significant symptoms of ADHD (Frazier-Wood et al., 2012; Pinto et al., 2016). In addition to the concomitance of symptoms of ADHD and disturbances of the frontoparietal network and additional frontal lobe fiber structures (Chen et al., 2016; Gao et al., 2019; Munro et al., 2018), there are abnormalities of the dopaminergic transmitter systems that influence the frontostriatal brain regions in ADHD (cf. Cools et al., 2019). Disturbances in inhibitory processes are also component elements of major symptoms of ADHD as defined in DSM-5 (Falkai & Wittchen, 2018). The present study includes two components of EF as established by prior research (i.e., inhibition and working memory). It therefore appears improbable that the lack of a statistically significant relationship between the measures of response inhibition and working memory and the ADHS-LE in the present study stems from there being fundamentally no link between EF as assessed in neuropsychological testing and the symptomatology of adult ADHD. The nature of the neuropsychological test data may impose a limitation on the interpretation of this study’s findings. The data set does not provide the raw data but the percentiles regarding performance on the EF and attention tests. The associated loss of explained variance might explain why EF and attentional performance did not appear—statistically—as significant predictors of the results of the ADHS-LE self-report questionnaire.
The increased risk of false-positive diagnoses on the basis of the results of ADHD self-report questionnaires is of particular concern given the widespread non-medically indicated stimulant use. The research literature reviewed for this paper found studies examining the abuse of stimulants has increased considerably in the last two decades (Faraone et al., 2020; Fuermaier et al., 2021; Gudmundsdottir et al., 2020; Looby & Earlywine, 2011; Wilens et al., 2008). It is apparent that up to 13–29% of students not only take stimulants themselves, but also give them to others or act as dealers. Consideration of possible secondary motives for pursuing ADHD assessment appears necessary, particularly as these motives may not be limited to attempts to improve cognitive performance; they may include the desire to attain accommodations to possible ADHD symptoms in a student’s degree course (cf. Weis et al., 2021).
Overall, the effectiveness of stimulants in subjects without adult ADHD is low, and considerable side effects may ensue (Faraone et al., 2020). Side effects of stimulants not taken orally were particularly serious, even resulting in death on occasion. In addition to this, Dolder et al. (2018) detected an increase in anxiety symptoms among healthy subjects who had taken methylphenidate. These findings call, above and beyond the general consideration of secondary motivations, for measures to protect subjects without adult ADHD from the abuse of stimulants and the associated side effects.
In the present study, the greatest proportion of invalid scores appeared in the SFSS. This notwithstanding, the frequency of invalid scores in the SFSS (17.6%) was relatively low when compared to findings of prior studies on simulated symptoms of ADHD (examples include Becke et al. (2021); Fuermaier et al. (2021); Johnson and Suhr (2021); Pollock et al., 2021; Potts et al., 2021; Sagar et al. (2017)). The frequencies of invalid results in the two PVT were lower still than that observed in the SFSS (RDS: 12.7%, SDRT: 8.1%). We further note in this context that, although at least one of the three SVT/PVTs used in the present study identified an invalid result in 32.6% of subjects, the percentage of invalid results fell to just 5% when the criterion was a failure on at least two of three invalid SVT/PVTs. Failure on all three SVT/PVTs occurred in only 0.9% of participants. While a failure rate of 32.6% on one SVT/PVT is similar to that found in previous studies, the failure rate of 5% on at least two of three SVT/PVTs is substantially smaller. Given the risk of false-positive or false-negative diagnostic judgments, it is important to consider the work of Berthelson et al. (2013) and of Larrabee (2014). They found that using a greater number of SVT/PVT increases the certainty with which negative response bias can be identified. These authors caution that the failure of only one SVT/PVT is not uncommon and therefore cannot be construed as establishing negative response bias. However, when three or four SVT/PVTs are used, at least two of them should show invalid results for an acceptably reliable identification of negative response bias.
There are other possible causes for this comparatively low base rate of negative response bias. First, the fact that the sample used in the present study did not consist solely of undergraduate and graduate students or who make up the samples typically involved in the work on simulated symptoms of ADHD. One-third (34.4%) of participants in the present study had formal schooling of only 10 years. Although the duration of formal schooling was not a significant predictor variable of the subject’s completion of the ADHS-LE, the mix of educational attainment in the sample may exert a certain influence. For example, in a study by Dandachi-FitzGerald et al. (2016), only 4.1% of whom were students in higher education. They found that 14.1% of the subjects attained invalid scores in the SIMS. Furthermore, the participants in this study have undergone assessment for psychopathological disorders (i.e., not solely due to ADHD). It may also have been the case that the sensitivity of the RDS used in this study was too low to uncover any negative response bias. While finding the RDS distinguished well between pre-instructed simulators of ADHD and a control group, Rogers et al. (2021) also found that it did not correlate with other embedded PVT from the WAIS-IV (Wechsler, 2008). It is also unclear if the sensitivity of the RDS remains acceptable when samples do not consist of people with a high level of education. The relatively low frequency of invalid RDS scores may also be the result of its insufficient sensitivity as a PVT when trying to identify the feigning of ADHD symptoms on self-report questionnaires. For example, Marshall et al. (2010) found that the RDS had a sensitivity of only 13.5%. They attributed this low sensitivity to the fact that the RDS may be construed as a test of short-term memory rather than sustained attention. Simulators of ADHD rarely feign short-term memory problems. Nelson and Lovett (2019, pp. 797f.) found a larger number of invalid scores on an SVT (CAARS, Conners et al., 1999) than on a PVT embedded in a continuous performance test. Although the SDRT as a PVT has previously proved useful in the identification of negative response bias in some studies (cf. Bodenburg, 2014; Czornik et al., 2021; Stevens et al., 2016), in the present study, it did not contribute to the explained variance of the ADHD self-report questionnaire used. This may be due to the selection of an excessively conservative criterion (x < [M – 2 SD]) for the identification of an invalid standard deviation.
The differences in frequency of invalid scores between the SFSS as an SVT and the RDS and SDRT as PVTs are striking even though Sagar et al. (2017) have found a mixed relationship between SVTs and PVTs. The major part of the ADHS-LE, utilized in the present study as a self-report questionnaire, is assessing the presence and severity of ADHD symptoms (Schmidt & Petermann, 2013). This common method variance could account for the relatively close statistical association between the SFSS and the ADHS-LE. Similarly, the lack of common method variance would account for the lack of statistical association between the ADHS-LE and the PVTs (cf. Fuermaier et al., 2015).
The results of the present study suggest a need to incorporate SVT/PVT into clinical assessments of adult ADHD. Lovett and Harrison (2021) currently recommend the inclusion of SVT/PVT in the process of assessment for ADHD, independently of the assessment’s aim to identify symptoms and their causality. It would appear inappropriate to limit such an assessment to the completion of self-report questionnaires such as the ADHS-LE. This view concurs with the recommendation issued by Davidson (2008) for valid and reliable assessment of suspected adult ADHD, which requires a multimethod investigation (cf. Mühlig & Petermann, 2006). Davidson (2008) recommends that examination in these cases encompasses the use of ADHD behavior rating scales, a clinical interview, neuropsychological tests, and patients’ description of their symptoms. As DSM-5 (Falkai & Wittchen, 2018) calls for clinicians to examine the extent to which the symptoms detected may not be explained by ADHD alone, but may possibly stem from other mental disorders (E-criterion), the use of symptom checklists for other mental disorders and a psychiatric examination would be of additional benefit. These measures would not serve to uncover potential negative response bias; instead, they would enable the assessment of comorbid or other possible mental disorders alongside adult ADHD. Some very effective instruments for conducting the necessary checks for negative response bias would be a stand-alone SVT (e.g., SFSS, Cima et al. (2003)) and the validity scales embedded in the Conners’ adult ADHD rating scales (CAARS, Conners et al., 1999). These embedded validity scales have demonstrated adequate sensitivity and high specificity and have the capacity to identify negative response bias (Harrison & Armstrong, 2016; Suhr et al., 2011). Finally, Davis (2021) suggested that an assessment includes one embedded PVT for each cognitive domain (e.g., sustained attention, working memory, response inhibition) evaluated during the assessment, at least one stand-alone PVT, and at least one embedded or stand-alone SVT.
References
Alexandre, J. L., Lange, A. M., Bilenberg, N., Gorrissen, A. M., Søbye, N., & Lambek, R. (2018). The ADHD rating scale-IV preschool version: Factor structure, reliability, validity, and standardisation in a Danish community sample. Research in Developmental Disabilities, 78, 125–135. https://doi.org/10.1016/j.ridd.2018.05.006
Babikan, T., Brauer Boone, K., Lu, P., & Arnold, G. (2006). Sensitivity and specificity of various digit span scores in the detection of suspect effort. The Clinical Neuropsychologist, 20, 145–159. https://doi.org/10.1080/13854040590947362
Barkley, R. A., & Murphy, K. R. (2011). The nature of executive function (EF) deficits in daily life activities in adults with ADHD and their relationship to performance on EF tests. Journal of Psychopathology and Behavioral Assessment, 33, 137–158. https://doi.org/10.1007/s10862-011-9217-x
Becke, M., Tucha, L., Weisbrod, M., Aschenbrenner, S., Tucha, O., & Fuermaier, A. (2021). Non-credible symptom report in the clinical evaluation of adult ADHD: Development and initial validation of a new validity index embedded in the Conners’ adult ADHD rating scales. Journal of Neural Transmission, 128(7), 1045–1063. https://doi.org/10.1007/s00702-021-02318-y
Berthelson, L., Mulchan, S. S., Odland, A. P., Miller, L. J., & Mittenberg, W. (2013). False positive diagnosis of malingering due to the use of multiple effort tests. Brain Injury, 27, 909–916. https://doi.org/10.3109/02699052.2013.793400
Bodenburg, S. (2014). Die Standardabweichung der Reaktionszeiten als ein Maß für negative Antwortverzerrungen. Zeitschrift für Neuropsychologie, 25, 89–97. https://doi.org/10.1024/1016-264X/a000123
Boonstra, A. M., Oosterlaan, J., Sergeant, J. A., & Buitelaar, J. K. (2005). Executive functioning in adult ADHD: A meta-analytic review. Psychological Medicine, 35(8), 1097–1108. https://doi.org/10.1017/s003329170500499x
Butzbach, M., Fuermaier, A., Aschenbrenner, S., Weisbrod, M., Tucha, L., & Tucha, O. (2019). Basic processes as foundations of cognitive impairment in adult ADHD. Journal of Neural Transmission (Vienna, Austria: 1996), 126(10), 1347–1362. https://doi.org/10.1007/s00702-019-02049-1
Chen, L., Hu, X., Ouyang, L., He, N., Liao, Y., Liu, Q., Zhou, M., Wu, M., Huang, X., & Gong, Q. (2016). A systematic review and meta-analysis of tract-based spatial statistics studies regarding attention-deficit/hyperactivity disorder. Neuroscience and Biobehavioral Reviews, 68, 838–847. https://doi.org/10.1016/j.neubiorev.2016.07.022
Cima, M., Hollnack, S., Kremer, K., Knauer, E., Schellbach-Matties, R., Klein, B., & Merckelbach, H. (2003). Strukturierter Fragebogen Simulierter Symptome. Die deutsche Version des Structured Inventory of Malingered Symptomatology: SIMS. Der Nervenarzt, 74(11), 977–986. https://doi.org/10.1007/s00115-002-1438-5
Conners, C. K. (2014). Conners’ continuous performance test 3rd Edition (Conners CPT 3). Pearson.
Conners, C. K., Erhardt, D., & Sparrow, M. A. (1999). Conners’ adult ADHD rating scales (CAARS): Technical manual. Multi Health Systems.
Cools, R., Froböse, M., Aarts, E., & Hofmans, L. (2019). Dopamine and the motivation of cognitive control. Handbook of Clinical Neurology, 163, 123–143. https://doi.org/10.1016/B978-0-12-804281-6.00007-0
Czornik, M., Seidl, D., Tavakoli, S., Merten, T., & Lehrner, J. (2021). Motor reaction times as an embedded measure of performance validity: A study with a sample of Austrian early retirement claimants. Psychological Injury and Law, published online, 6. November 2021. https://doi.org/10.1007/s12207-021-09431-z
Dandachi-FitzGerald, B., van Twillert, B., van de Sande, P., van Os, Y., & Ponds, R. W. (2016). Poor symptom and performance validity in regularly referred hospital outpatients: Link with standard clinical measures, and role of incentives. Psychiatry Research, 239, 47–53. https://doi.org/10.1016/j.psychres.2016.02.061
Davidson, M. A. (2008). ADHD in adults: A review of the literature. Journal of Attention Disorders, 11(6), 628–641. https://doi.org/10.1177/1087054707310878
Davis, J. J. (2021). Interpretation of data from multiple performance validity tests. In K. B. Boone (Ed.), Assessment of feigned cognitive impairment (2nd ed., pp. 283–306). Guilford Press.
De Quiros, G. B., & Kinsbourne, M. (2001). Adult ADHD. Analysis of self-ratings on a behavior questionnaire. Annals of the New York Academy of Sciences, 931, 140–147.
De Zwaan, M., Gruss, B., Müller, A., Graap, H., Martin, A., Glaesmer, H., Hilbert, A., & Philipsen, A. (2012). The estimated prevalence and correlates of adult ADHD in a German community sample. European Archives of Psychiatry and Clinical Neuroscience, 262, 79–86. https://doi.org/10.1007/s00406-011-0211-9
Dilling, H., Mombour, W., & Schmidt, M. H. (2015). Internationale Klassifikation psychischer Störungen, ICD-10, Kapitel V (F) – Klinisch-diagnostische Leitlinien (10th ed.). Hogrefe.
Döpfner, M., Steinhausen, H. C., Coghill, D., Dalsgaard, S., Poole, L., Ralston, S. J., Rothenberger, A., & ADORE Study Group. (2006). Cross-cultural reliability and validity of ADHD assessed by the ADHD rating scale in a pan-European study. European Child & Adolescent Psychiatry, 15. Supplement, 1, I46–I55. https://doi.org/10.1007/s00787-006-1007-8
Dolder, P. C., Müller, F., Schmid, Y., Borgwardt, S. J., & Liechti, M. E. (2018). Direct comparison of the acute subjective, emotional, autonomic, and endocrine effects of MDMA, methylphenidate, and modafinil in healthy subjects. Psychopharmacology (berl), 235, 467–479. https://doi.org/10.1007/s00213-017-4650-5
Duff, C. T., & Sulla, E. M. (2015). Measuring executive function in the differential diagnosis of attention-deficit/hyperactivity disorder: Does it really tell us anything? Applied Neuropsychology. Child, 4(3), 188–196. https://doi.org/10.1080/21622965.2013.848329
Elliott, J., Johnston, A., Husereau, D., Kelly, S. H., Eagles, C., Charach, A., Hsieh, S.-C., Bai, Z., Hossain, A., Skidmore, B., Tsakonas, E., Chojecki, D., Mamdani, M., & Wells, G. A. (2020). Pharmacologic treatment of attention deficit hyperactivity disorder in adults: A systematic review and network meta-analysis. PLoS ONE, 15(10), e0240584. https://doi.org/10.1371/journal.pone.0240584
Falkai, P., & Wittchen, H. U. (Eds.). (2018). DSM-5 - Diagnostisches und Statistisches Manual Psychischer Störungen, 2 (korrigierte). Hogrefe.
Faraone, S. V., Rostain, A. L., Montano, C. B., Mason, O., Antshel, K. M., & Newcorn, J. H. (2020). Systematic review: Nonmedical use of prescription stimulants: Risk factors, outcomes, and risk reduction strategies. Journal of the American Academy of Child and Adolescent Psychiatry, 59(1), 100–112. https://doi.org/10.1016/j.jaac.2019.06.012
Frazier-Wood, A. C., Bralten, J., Arias-Vasquez, A., Luman, M., Ooterlaan, J., Sergeant, J., Faraone, S. V., Buitelaar, J., Franke, B., Kuntsi, J., & Rommelse, N. N. (2012). Neuropsychological intra-individual variability explains unique genetic variance of ADHD and shows suggestive linkage to chromosomes 12, 13, and 17. American Journal of Medical Genetics. Part B, Neuropsychiatric genetics, 159B(2), 131–140. https://doi.org/10.1002/ajmg.b.32018
Fuermaier, A., Tucha, L., Koerts, J., Aschenbrenner, S., Kaunzinger, I., Hauser, J., Weisbrod, M., Lange, K. W., & Tucha, O. (2015). Cognitive impairment in adult ADHD–perspective matters! Neuropsychology, 29(1), 45–58. https://doi.org/10.1037/neu0000108
Fuermaier, A., Tucha, O., Koerts, J., Tucha, L., Thome, J., & Faltraco, F. (2021). Feigning ADHD and stimulant misuse among Dutch university students. Journal of Neural Transmission, 128(7), 1079–1084. https://doi.org/10.1007/s00702-020-02296-7
Gao, Y., Shuai, D., Bu, X., Hu, X., Tang, S., Zhang, L., Li, H., Hu, X., Lu, L., Gong, Q., & Huang, X. (2019). Impairments of large-scale functional networks in attention-deficit/hyperactivity disorder: A meta-analysis of resting-state functional connectivity. Psychological Medicine, 49(15), 2475–2485. https://doi.org/10.1017/S003329171900237X
Gawrilow, C., Merkt, J., Goossens-Merkt, H., Bodenburg, S., & Wendt, M. (2011). Multitasking in adults with ADHD. Attention Deficit and Hyperactivity Disorders, 3(3), 253–264. https://doi.org/10.1007/s12402-011-0056-0
Golden, C. J. (1978). Stroop color and word test: A manual for clinical and experimental uses. Stoelting Co.
Grant, A. F., Lace, J. W., Teague, C. L., Lowell, K. T., Ruppert, P. D., Garner, A. A., & Gfeller, J. D. (2020). Detecting feigned symptoms of depression, anxiety, and ADHD, in college students with the structured inventory of malingered symptomatology. Applied neuropsychology: Adult, 1–9. Advance online publication, 2020, May 26. https://doi.org/10.1080/23279095.2020.1769097
Green, P. (2004). Green’s medical symptom validity test (MSVT). Green’s Publishing.
Gudmundsdottir, B. G., Weyandt, L., & Ernudottir, G. B. (2020). Prescription stimulant misuse and ADHD symptomatology among college students in Iceland. Journal of Attention Disorders, 24(3), 384–401. https://doi.org/10.1177/1087054716684379
Härting, C., Markowitsch, H. J., Neufeld, H., Calabrese, P., Deisinger, K., & Kessler, J. (2000). WMS – R, Wechsler Gedächtnistest – Revidierte Fassung. Huber.
Harrison, A. G., & Armstrong, I. T. (2016). Development of a symptom validity index to assist in identifying ADHD symptom exaggeration or feigning. The Clinical Neuropsychologist, 30(2), 265–283. https://doi.org/10.1080/13854046.2016.1154188
Heaton, R. K., Chelune, G. J., Talley, J. L., Kay, G. G., & Curtiss, G. (1993). Wisconsin card sorting test. Lutz, FL: Psychological Assessment Resources
Heine, S., & Exner, C. (2021). Aufmerksamkeitsdefizit-/Hyperaktivitätsstörung (ADHS) im Erwachsenenalter. Zeitschrift für Neuropsychologie, 32(3), 141–157. https://doi.org/10.1024/1016-264X/a000329
Hesson, J., & Fowler, K. (2015). Prevalence and correlates of self-reported ADHD/ADHD in a large national sample of Canadian adults. Journal of Attention Disorders, 22, 191–200. https://doi.org/10.1177/1087054715573992
Johnson, E. E. H., & Suhr, J. (2021). Self-reported functional impairment in college students: Relationship to noncredible reporting, ADHD, psychological disorders, and other psychological factors. Journal of Clinical and Experimental Neuropsychology, 43(4), 399–411. https://doi.org/10.1080/13803395.2021.1935490
Larrabee, G. J. (2014). Minimizing false positive error with multiple performance validity tests: Response to Bilder, Sugar, and Hellemann. The Clinical Neuropsychologist, 28, 1230–1242. https://doi.org/10.1080/13854046.2014.988754
LeRoy, A., Jacova, C., & Young, C. (2019). Neuropsychological performance patterns of adult ADHD subtypes. Journal of Attention Disorders, 23(10), 1136–1147. https://doi.org/10.1177/1087054718773927
Looby, A., & Earleywine, M. (2011). Expectation to receive methylphenidate enhances subjective arousal but not cognitive performance. Experimental and Clinical Psychopharmacology, 19(6), 433–444. https://doi.org/10.1037/a0025252
Lovejoy, D., Ball, J., Keats, M., Stutts, M., Spain, E., Janda, L., & Janusz, J. (1999). Neuropsychological performance of adults with attention deficit hyperactivity disorder (ADHD): Diagnostic classification estimates for measures of frontal lobe/executive functioning. Journal of the International Neuropsychological Society, 5(3), 222–233. https://doi.org/10.1017/S1355617799533055
Lovett, B. J., & Harrison, A. G. (2021). Assessing adult ADHD: New research and perspectives. Journal of Clinical and Experimental Neuropsychology, 43(4), 333–339. https://doi.org/10.1080/13803395.2021.1950640
Lucke, J., Jensen, C., Dunn, M., Chan, G., Forlini, C., Kaye, S., Partridge, B., Farrell, M., Racine, E., & Hall, W. (2018). Non-medical prescription stimulant use to improve academic performance among Australian university students: Prevalence and correlates of use. BMC Public Health, 18(1), 1270. https://doi.org/10.1186/s12889-018-6212-0
Marshall, P., Schroeder, R., O’Brien, J., Fischer, R., Ries, A., Blesi, B., & Barker, J. (2010). Effectiveness of symptom validity measures in identifying cognitive and behavioral symptom exaggeration in adult attention-deficit/hyperactivity disorder. The Clinical Neuropsychologist, 24, 1204–1237.
Merkt, J., Singmann, H., Bodenburg, S., Goossens-Merkt, H., Kappes, A., Wendt, M., & Gawrilow, C. (2013). Flanker performance in female college students with ADHD: A diffusion model analysis. ADHD Attention Deficit and Hyperactivity Disorders, 5, 321–341. https://doi.org/10.1007/s12402-013-0110-1
Mühlig, S., & Petermann, F. (2006). Grundprinzipien multimethodaler Diagnostik. In F. Petermann & M. Eid (Eds.), Handbuch der psychologischen Diagnostik (pp. 99–108). Hogrefe.
Munro, B. A., Weyandt, L. L., Hall, L. E., Oster, D. R., Gudmundsdottir, B. G., & Kuhar, B. G. (2018). Physiological substrates of executive functioning: A systematic review of the literature. ADHD Attention Deficit and Hyperactivity Disorders, 10, 1–20. https://doi.org/10.1007/s12402-017-0226-9
Nelson, J. M., & Lovett, B. J. (2019). Assessing ADHD in college students: Integrating multiple evidence sources with symptom and performance validity data. Psychological Assessment, 31(6), 793–804. https://doi.org/10.1037/pas0000702
Niesten, I., Müller, W., Merckelbach, H., Dandachi-FitzGerald, B., & Jelicic, M. (2017). Moral reminders do not reduce symptom over-reporting tendencies. Psychological Injury and Law, 10(4), 368–384. https://doi.org/10.1007/s12207-017-9303-9
Onandia-Hinchado, I., Pardo-Palenzuela, N., & Diaz-Orueta, U. (2021). Cognitive characterization of adult attention deficit hyperactivity disorder by domains: A systematic review. Journal of Neural Transmission, 128, 893–937. https://doi.org/10.1007/s00702-021-02302-6
Pawlik, K. (2006). Psychologische Diagnostik I: Methodische Grundlagen. In K. Pawlik (Ed.), Handbuch Psychologie, Wissenschaft, Anwendung, Berufsfelder (pp. 563–580). Springer.
Pinto, R., Asherson, P., Ilott, N., Cheung, C. H., & Kuntsi, J. (2016). Testing for the mediating role of endophenotypes using molecular genetic data in a twin study of ADHD traits. American Journal of Medical Genetics. Part B, Neuropsychiatric Genetics: The Official Publication of the International Society of Psychiatric Genetics, 171(7), 982–992. https://doi.org/10.1002/ajmg.b.32463
Potts, H. E., Lewandowski, L. J., & Lovett, B. J. (2021). The multidimensional ADHD rating scale: A measure of symptoms, impairment, and symptom validity. Journal of Clinical and Experimental Neuropsychology, 43(4), 426–436. https://doi.org/10.1080/13803395.2021.1942795
Polanczyk, G. V., Willcutt, E. G., Salum, G. A., Kieling, C., & Rohde, L. A. (2014). ADHD prevalence estimates across three decades: An updated systematic review and meta-regression analysis. International Journal of Epidemiology, 43, 434–442. https://doi.org/10.1093/ije/dyt261
Pollock, B., Harrison, A. G., & Armstrong, I. T. (2021). What can we learn about performance validity from TOVA response profiles? Journal of Clinical and Experimental Neuropsychology, 43(4), 412–425. https://doi.org/10.1080/13803395.2021.1932762
Rabiner, D. L. (2013). Stimulant prescription cautions: Addressing misuse, diversion and malingering. Current Psychiatry Reports, 15(7), 375. https://doi.org/10.1007/s11920-013-0375-2
Retz, W., Retz-Junginger, P., Römer, K., & Rösler, M. (2013). Standardisierte Skalen zur strukturierten Diagnostik der ADHS im Erwachsenenalter. Fortschritte Der Neurologie - Psychiatrie, 81(7), 381–389. https://doi.org/10.1055/s-0033-1335740
Reitan, R. M. (1992). Trail making test. Tucson: Reitan Neuropsychology Laboratory
Rogers, R., Velsor, S. F., Donnelly, J. W., 2nd., & Dean, B. (2021). Embedded WAIS-IV detection strategies and feigned cognitive impairment: An investigation of malingered ADHD. Assessment, 28(1), 44–56. https://doi.org/10.1177/1073191120927788
Rosch, K. S., & Mostofsky, S. (2019). Chapter 19 - Development of the frontal lobe. Handbook of Clinical Neurology, 163, 351–367. https://doi.org/10.1016/B978-0-12-804281-6.00019-7
Ruff, R. (2011). Figural Fluency Test. In: J. S. Kreutzer, J. DeLuca, B. Caplan (Eds.), Encyclopedia of Clinical Neuropsychology. Springer, New York, NY. https://doi.org/10.1007/978-0-387-79948-3_2048
Sagar, S., Miller, C. J., & Erdodi, L. A. (2017). Detecting feigned attention-deficit/hyperactivity disorder (ADHD): Current methods and future directions. Psychological Injury and Law, 10, 105–113. https://doi.org/10.1007/s12207-017-9286-6
Sass, H., Wittchen, H. U., Zaudig, M., & Houben, I. (2003). Diagnostisches und Statistisches Manual Psychischer Störungen – Textrevision – DSM-IV-TR. Hogrefe.
Schmidt, J. P., & Tombaugh, T. N. (1995). Learning and memory battery. Multi-Health Systems Inc.
Schmidt, S., & Petermann, F. (2011). Zur Sensitivität und Spezifität des ADHS-Screening für Erwachsene (ADHS-E). Zeitschrift für Psychiatrie, Psychologie und Psychotherapie, 59(1), 73–78. https://doi.org/10.1024/1661-4747/a000054
Schmidt, S., & Petermann, F. (2013). ADHS-Screening für Erwachsene. Ein Verfahren zur Erfassung von Symptomen einer ADHS, 2. korrigierte und (überarbeitete). Pearson.
Scholz, L., Werle, J., Philipsen, A., Schulze, M., Collonges, J., & Gensichen, J. (2020). Effects and feasibility of psychological interventions to reduce inattention symptoms in adults with ADHD: A systematic review. Journal of Mental Health, 1–14. Advance online publication. https://doi.org/10.1080/09638237.2020.1818189
Sebastian, A., Jung, P., Krause-Utz, A., Lieb, K., Schmahl, Chr., & Tüscher, O. (2014). Frontal dysfunctions of impulse control – A systematic review in borderline personality disorder and attention-deficit/hyperactivity disorder. Frontiers in Human Neuroscience, 8, Article 698. https://doi.org/10.3389/fnhum.2014.00698
Simon, J. R. (1969). Reactions toward the source of stimulation. Journal of Experimental Psychology, 81(1), 174–176. https://doi.org/10.1037/h0027448
Stevens, A., Bahlo, S., Licha, C., Liske, B., & Vossler-Thies, E. (2016). Reaction time as an indicator of insufficient effort: Development and validation of an embedded performance validity parameter. Psychiatry Research, 245, 74–82. https://doi.org/10.1016/j.psychres.2016.08.022
Suhr, J. A., Buelow, M., & Riddle, T. (2011). Development of an infrequency index for the CAARS. Journal of Psychoeducational Assessment, 29(2), 160–170. https://doi.org/10.1177/0734282910380190
Suhr, J., Hammers, D., Dobbins-Buckland, K., Zimak, E., & Hughes, C. (2008). The relationship of malingering test failure to self-reported symptoms and neuropsychological findings in adults referred for ADHD evaluation. Archives of Clinical Neuropsychology, 23(5), 521–530. https://doi.org/10.1016/j.acn.2008.05.003
Trenerry, M. R., Crosson, B., DeBoe, J., & Leber, W. R. (1989). Stroop neuropsychological screening test manual. Lutz, FL: Psychological Assessment Resources
Van Dyke, S. A., Millis, S. R., Axelrod, B. N., & Hanks, R. A. (2013). Assessing effort: Differentiating performance and symptom validity. The Clinical Neuropsychologist, 27(8), 1234–1246. https://doi.org/10.1080/13854046.2013.835447
Van Impelen, A., Merckelbach, H., Jelicic, M., & Merten, T. (2014). The structured inventory of malingered symptomatology, SIMS: A systematic review and meta-analysis. The Clinical Neuropsychologist, 28(8), 1336–1365. https://doi.org/10.1080/13854046.2014.984763
Ward, M. F., Wender, P. H., & Reimherr, F. W. (1993). The Wender Utah rating scale: An aid in the retrospective diagnosis of childhood attention deficit hyperactivity disorder. The American Journal of Psychiatry, 150(6), 885–890. https://doi.org/10.1176/ajp.150.6.885
Wechsler, D. (2008). Manual for the Wechsler adult intelligence scale (4th ed.). The Psychological Corporation.
Weis, R., Hombosky, M. L., Schafer, K. K., Shulman, D., & Tull, J. K. (2021). Accommodation decision-making for postsecondary students with ADHD: Implications for neuropsychologists. Journal of Clinical and Experimental Neuropsychology, 43(4), 370–383. https://doi.org/10.1080/13803395.2021.1918645
Wilens, T. E., Adler, L. A., Adams, J., Sgambati, S., Rotrosen, J., Sawtelle, R., Utzinger, L., & Fusillo, S. (2008). Misuse and diversion of stimulants prescribed for ADHD: A systematic review of the literature. Journal of the American Academy of Child and Adolescent Psychiatry, 47(1), 21–31. https://doi.org/10.1097/chi.0b013e31815a56f1
Zimmermann, M., & Fimm, B. (2016). Testbatterie zur Aufmerksamkeitsprüfung, V2.3.1. Herzogenrath: Psytest
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bodenburg, S., Wendiggensen, J. & Kasten, E. Scores in Self-Report Questionnaires Assessing Adult ADHD Can Be Influenced by Negative Response Bias but Are Unrelated to Performance on Executive Function and Attention Tests. Psychol. Inj. and Law 15, 189–199 (2022). https://doi.org/10.1007/s12207-022-09448-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12207-022-09448-y