Abstract
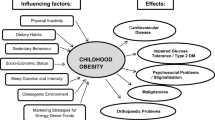
Childhood obesity is an important public health issue worldwide. Urbanization, sedentary lifestyle and change in food habits are the chief reasons behind this pandemic. In a small proportion of children, obesity is the result of endocrine, syndromic or monogenic causes. The present paper summarizes the methods, definitions and cut-offs for identification of obesity in children. We have briefly reviewed the various techniques used for estimation of body fat in children and the cut-offs for defining obesity based on body fat percentage, and the reference curves based on body mass index and waist circumference. The etiology of obesity in children, including individual behaviors, macro- and micro-environmental influences, and endocrine causes have been discussed, and an approach to etiological assessment of obese children has been presented. Special emphasis has been laid on clinical pointers that suggest the presence of syndromic, endocrine or monogenic forms of obesity, such as, short stature, dysmorphism, neurocognitive impairment and early age at onset.

Similar content being viewed by others
References
World Health Organization. Obesity and overweight. Geneva: World Health Organization; 2011. Available at: http://www.who.int/mediacentre/factsheets/fs311/en/index.html.
Khadilkar VV, Khadilkar AV, Cole TJ, Chiplonkar SA, Pandit D. Overweight and obesity prevalence and body mass index trends in Indian children. Int J Pediatr Obes. 2011;6:e216–24.
WHO Technical Counsultation. Obesity: preventing and managing the global epidemic. Report of a WHO consultation 2000. Report No.: 0512-3054 (Print) 0512-3054, 2000. Geneva: WHO; 2000.
Wells JCK, Fewtrell MS. Measuring body composition. Arch Dis Child. 2006;91:612–7.
Ward LC, Poston L, Godfrey KM, Koletzko B. Assessing early growth and adiposity: report from an Early Nutrition Academy workshop. Ann Nutr Metab. 2013;63:120–30.
AACE/ACE Obesity Task Force. AACE/ACE position statement on the prevention, diagnosis, and treatment of obesity. Endocr Pract. 1998;4:297–350.
McCarthy HD, Cole TJ, Fry T, Jebb SA, Prentice AM. Body fat reference curves for children. Int J Obes (Lond). 2006;30:598–602.
Khadgawat R, Marwaha RK, Tandon N, et al. Percentage body fat in apparently healthy school children from northern India. Indian Pediatr. 2013;50:859–66.
Deurenberg P, Weststrate JA, Seidell JC. Body mass index as a measure of body fatness: age- and sex-specific prediction formulas. Br J Nutr. 1991;65:105–14.
Deurenberg P, Deurenberg-Yap M, Guricci S. Asians are different from Caucasians and from each other in their body mass index/body fat per cent relationship. Obes Rev. 2002;3:141–6.
Banerji MA, Faridi N, Atluri R, Chaiken RL, Lebovitz HE. Body composition, visceral fat, leptin, and insulin resistance in Asian Indian men. J Clin Endocrinol Metab. 1999;84:137–44.
Misra A, Chowbey P, Makkar BM, et al; Concensus Group. Consensus statement for diagnosis of obesity, abdominal obesity and the metabolic syndrome for Asian Indians and recommendations for physical activity, medical and surgical management. J Assoc Physicians India. 2009;57:163–70.
American Diabetes Association Position Statement. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2010;33:62–9.
Kuczmarski RJ, Ogden CL, Grummer-Strawn LM, et al. CDC growth charts: United States. Adv Data. 2000;314:1–27.
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ. 2000;320:1240–3.
Multicentre Growth Reference Study WHO Group. WHO Child Growth Standards based on length/height, weight and age. Acta Paediatr. 2006;450:76–85.
de Onis M Onyango AW, Borghi E, Siyan A, Nishida C, Siekmann J. Development of WHO growth reference for school-aged children and adolescents. Bull World Health Organ. 2007;85:660–7.
Khadilkar V, Yadav S, Agrawal KK, et al. Revised IAP growth charts for height, weight and body mass index for 5 to 18 year old Indian children. Indian Pediatr. 2015;52:4755.
Qiao Q, Nyamdorj R. The optimal cut-off values and their performance of waist circumference and waist-to-hip ratio for diagnosing type II diabetes. Eur J Clin Nutr. 2010;64:23–9.
Khadilkar A, Ekbote V, Chiplonkar S, et al. Waist circumference percentiles in 2-18 year old Indian children. J Pediatr. 2014;164:1358–62.
Ashwell M, Gibson S. Waist-to-height ratio as an indicator of ‘early health risk’: simpler and more predictive than using a ‘matrix’ based on BMI and waist circumference. BMJ Open. 2016;6:e010159.
Mehta SK. Waist circumference to height ratio in children and adolescents. Clin Pediatr (Phila). 2015;54:652–8.
Jain V, Singhal A. Catch up growth in low birth weight infants: striking a healthy balance. Rev Endocr Metab Disord. 2012;13:141–7.
Khandelwal P, Jain V, Gupta AK, Kalaivani M, Paul VK. Association of early postnatal growth trajectory with body composition in term low birth weight infants. J Dev Orig Health Dis. 2014;5:189–96.
Hill JO, Peters JC. Environmental contributions to the obesity epidemic. Science. 1998;280:1371–4.
Swinburn B, Egger G, Raza F. Dissecting obesogenic environments:the development and application of a framework for identifying and prioritizing environmental interventions for obesity. Prev Med. 1999;29:563–70.
Bowman SA, Gortmaker SL, Ebbeling CB, Pereira MA, Ludwig DS. Effects of fast-food consumption on energy intake and diet quality among children in a national household survey. Pediatrics. 2004;113:112–8.
Al Mamun A, Lawlor DA, Cramb S, O’Callaghan M, Williams G, Najman J. Do childhood sleeping problems predict obesity in young adulthood? Evidence from a prospective birth cohort study. Am J Epidemiol. 2007;166:1368–73.
Hancox RJ, Milne BJ, Poulton R. Association between child and adolescent television viewing and adult health: a longitudinal birth cohort study. Lancet. 2004;364:257–62.
Spruijt-Metz D, Lindquist CH, Birch LL, Fisher JO, Goran MI. Relation between mothers’ child-feeding practices and children’s adiposity. Am J Clin Nutr. 2002;75:581–6.
Johnson SL, Birch LL. Parents’ and children’s adiposity and eating styles. Pediatrics. 1994;94:653–61.
Cutting TA, Fisher JO, Grimm-Thomas K, Birch LL. Like mother, like daughter: familial patterns of overweight are mediated by mothers dietary disinhibition. Am J Clin Nutr. 1999;69:608–13.
Shah P, Misra A, Gupta N, et al. Improvement in nutrition-related knowledge and behaviour of urban Asian Indian school children: findings from the ‘Medical education for children/ adolescents for realistic prevention of obesity and diabetes and for healthy aGeing’ (MARG) intervention study. Br J Nutr. 2010;104:427–36.
French SA, Wechsler H. School-based research and initiatives: fruit and vegetable environment, policy, and pricing workshop. Prev Med. 2004;39:101–7.
Davison KK, Lawson CT. Do attributes in the physical environment influence children’s physical activity? A review of the literature. Int J Behav Nutr Phys Act. 2006;3:19. https://doi.org/10.1186/1479-5868-3-19.
Timperio A, Ball K, Roberts R, Campbell K, Andrianopoulos N, Crawford D. Children’s fruit and vegetable intake: associations with the neighbourhood food environment. Prev Med. 2008;46:331–5.
Spence JC, Cutumisu N, Edwards J, Evans J. Influence of neighbourhood design and access to facilities on overweight among preschool children. Int J Pediatr Obes. 2008;3:109–16.
Osei-Assibey G, Dick S, Macdiarmid J, et al. The influence of the food environment on overweight and obesity in young children: a systematic review. BMJ Open. 2012;2:e001538.
Crino A, Greggio NA, Beccaria L, et al. Diagnosis and differential diagnosis of obesity in childhood. Minerva Pediatr. 2003;55:461.
Crocker MK, Yanovski JA. Pediatric obesity: etiology and treatment. Pediatr Clin N Am. 2011;58:1217–40.
Mason K, Page L, Balikcioglu PG. Screening for hormonal, monogenic, and syndromic disorders in obese infants and children. Pediatr Ann. 2014;43:e218–24.
Niranjan U, Wright NP. Should we treat subclinical hypothyroidism in obese children? BMJ. 2016;352:i941.
Verma N, Jain V. Iatrogenic Cushing syndrome. Indian Pediatr. 2012;49:765.
Bougnères P, Pantalone L, Linglart A, Rothenbühler A, Le Stunff C. Endocrine manifestations of the rapid-onset obesity with hypoventilation, hypothalamic, autonomic dysregulation, and neural tumor syndrome in childhood. J Clin Endocrinol Metab. 2008;93:3971–80.
Styne DM, Arslanian SA, Connor EL, et al. Pediatric obesity-assessment, treatment, and prevention: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2017;102:709–57.
Contributions
BA and VJ conceptualized the paper, searched the literature and drafted the paper. Both authors have seen and approved the final version. VJ will act as guarantor for this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
None.
Rights and permissions
About this article
Cite this article
Aggarwal, B., Jain, V. Obesity in Children: Definition, Etiology and Approach. Indian J Pediatr 85, 463–471 (2018). https://doi.org/10.1007/s12098-017-2531-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-017-2531-x