Abstract
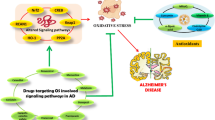
The level of lipopolysaccharide (LPS) is higher in the blood and brains of patients with Alzheimer's disease (AD), and this phenomenon is strongly linked to AD-related neuronal damage and β-amyloid (Aβ) generation. However, the mechanism by which LPS causes neuronal damage has still not been fully clarified. Oxidative stress, neuroinflammation, and Ca2+ overload are regarded as important factors influencing AD. NADPH oxidase 2 (NOX2) and the NOD-like receptor family protein 1 (NLRP1) inflammasome play important roles in promoting oxidative stress and inflammation in neurons. Ca2+ overload can activate calcineurin (CN), which further dephosphorylates nuclear factor of activated T cells (NFAT), leading to its translocation into the nucleus to regulate gene transcription. In the present study, LPS (250 µg/kg) exposure for 14 days was used to induce cognitive dysfunction in mice and LPS (20 µg/ml) exposure for 48 h was used to induce neuronal damage in HT22 cells. The results showed that LPS exposure activated phospholipase C (PLC), CN, and NFAT1; increased the expressions of NOX2- and NLRP1-related proteins; and promoted neuronal damage and Aβ deposition in mice and HT22 cells. However, treatment with 2-APB (SOCE inhibitor), apocynin (NOX inhibitor), or tempol (reactive oxygen species scavenger) significantly reversed these LPS-induced changes, and improved neuronal damage and Aβ deposition. Moreover, LPS exposure promoted PLC phosphorylation, increased the level of inositol-1,4,5-triphosphate, elevated the intracellular Ca2+ concentration ([Ca2+]i), and disrupted [Ca2+]i homeostasis in HT22 cells. These data indicated that the activation of SOCE-mediated NFAT1–NOX2–NLRP1 inflammasome involves in LPS-induced neuronal damage and Aβ generation.
Graphical abstract











Similar content being viewed by others
Data availability
The data from this manuscript are available from the corresponding author upon reasonable request.
Abbreviations
- LPS:
-
Lipopolysaccharide
- DAG:
-
Diacylglycerol
- AD:
-
Alzheimer's disease
- NOX2:
-
NADPH oxidase 2
- IP3:
-
Inositol-1,4,5-triphosphate
- SOCC:
-
Store-operated calcium channels
- SOCE:
-
Store-operated calcium entry
- CN:
-
Calcineurin
- NFAT1:
-
Nuclear factor of activated T cells 1
- 2-APB:
-
2-Aminoethyl diphenylborinate
- TLR4:
-
Toll-like receptor 4
- PLC:
-
Phospholipase C
- SOD:
-
Superoxide dismutase
- ROS:
-
Reactive oxygen species
- ALS:
-
Amyotrophic lateral sclerosis
- PSD95:
-
Postsynaptic density protein 95
- MWM:
-
Morris water maze
- [Ca2 +]i :
-
Intracellular Ca2+ concentration
- Aβ:
-
β-Amyloid
- IP3R:
-
Inositol-1,4,5-triphosphate receptor
- PIP2:
-
Phosphatidylinositol bisphosphate
References
Zarifkar A, Choopani S, Ghasemi R, Naghdi N, Maghsoudi AH, Maghsoudi N, Rastegar K, Moosavi M (2010) Agmatine prevents LPS-induced spatial memory impairment and hippocampal apoptosis. Eur J Pharmacol 634(1–3):84–88. https://doi.org/10.1016/j.ejphar.2010.02.029
Lee JW, Lee YK, Yuk DY, Choi DY, Ban SB, Oh KW, Hong JT (2008) Neuro-inflammation induced by lipopolysaccharide causes cognitive impairment through enhancement of beta-amyloid generation. J Neuroinflammation 5:37. https://doi.org/10.1186/1742-2094-5-37
Zhao WX, Zhang JH, Cao JB, Wang W, Wang DX, Zhang XY, Yu J, Zhang YY et al (2017) Acetaminophen attenuates lipopolysaccharide-induced cognitive impairment through antioxidant activity. J Neuroinflammation 14(1):17. https://doi.org/10.1186/s12974-016-0781-6
Zhang XY, Cao JB, Zhang LM, Li YF, Mi WD (2015) Deferoxamine attenuates lipopolysaccharide-induced neuroinflammation and memory impairment in mice. J Neuroinflammation 12:20. https://doi.org/10.1186/s12974-015-0238-3
Yang Y, Wandler AM, Postlethwait JH, Guillemin K (2012) Dynamic Evolution of the LPS-Detoxifying Enzyme Intestinal Alkaline Phosphatase in Zebrafish and Other Vertebrates. Front Immunol 3:314. https://doi.org/10.3389/fimmu.2012.00314
Zhan X, Stamova B, Jin LW, DeCarli C, Phinney B, Sharp FR (2016) Gram-negative bacterial molecules associate with Alzheimer disease pathology. Neurology 87(22):2324–2332.
Zhan X, Stamova B, Sharp FR (2018) Lipopolysaccharide Associates with Amyloid Plaques, Neurons and Oligodendrocytes in Alzheimer’s Disease Brain: A Review. Front Aging Neurosci 10:42. https://doi.org/10.3389/fnagi.2018.00042
Zhang R, Miller RG, Gascon R, Champion S, Katz J, Lancero M, Narvaez A, Honrada R et al (2009) Circulating endotoxin and systemic immune activation in sporadic amyotrophic lateral sclerosis (sALS). J Neuroimmunol 206(1–2):121–124. https://doi.org/10.1016/j.jneuroim.2008.09.017
Zhan X, Cox C, Ander BP, Liu D, Stamova B, Jin LW, Jickling GC, Sharp FR (2015) Inflammation Combined with Ischemia Produces Myelin Injury and Plaque-Like Aggregates of Myelin, Amyloid-beta and AbetaPP in Adult Rat Brain. J Alzheimers Dis 46(2):507–523. https://doi.org/10.3233/JAD-143072
Sun Y, Ge X, Li M, Xu L, Shen Y (2017) Dyrk2 involved in regulating LPS-induced neuronal apoptosis. Int J Biol Macromol 104(Pt A):979–986. https://doi.org/10.1016/j.ijbiomac.2017.06.087
Tarafdar A, Pula G (2018) The Role of NADPH Oxidases and Oxidative Stress in Neurodegenerative Disorders. Int J Mol Sci 19 (12). https://doi.org/10.3390/ijms19123824
Park L, Anrather J, Girouard H, Zhou P, Iadecola C (2007) Nox2-derived reactive oxygen species mediate neurovascular dysregulation in the aging mouse brain. J Cereb Blood Flow Metab 27(12):1908–1918. https://doi.org/10.1038/sj.jcbfm.9600491
Zhang B, Zhang Y, Xu T, Yin Y, Huang R, Wang Y, Zhang J, Huang D et al (2017) Chronic dexamethasone treatment results in hippocampal neurons injury due to activate NLRP1 inflammasome in vitro. Int Immunopharmacol 49:222–230.
Kaushal V, Dye R, Pakavathkumar P, Foveau B, Flores J, Hyman B, Ghetti B, Koller BH et al (2015) Neuronal NLRP1 inflammasome activation of Caspase-1 coordinately regulates inflammatory interleukin-1-beta production and axonal degeneration-associated Caspase-6 activation. Cell Death Differ 22(10):1676–1686. https://doi.org/10.1038/cdd.2015.16
Masters SL, Gerlic M, Metcalf D, Preston S, Pellegrini M, O’Donnell JA, McArthur K, Baldwin TM et al (2012) NLRP1 inflammasome activation induces pyroptosis of hematopoietic progenitor cells. Immunity 37(6):1009–1023. https://doi.org/10.1016/j.immuni.2012.08.027
Sun L, Chen Y, Shen X, Xu T, Yin Y, Zhang H, Ding S, Zhao Y et al (2019) Inhibition of NOX2-NLRP1 signaling pathway protects against chronic glucocorticoids exposure-induced hippocampal neuronal damage. Int Immunopharmacol 74:105721 (S1567-5769(19)30374-1)
Xu T, Sun L, Shen X, Chen Y, Yin Y, Zhang J, Huang D, Li W et al (2019) NADPH oxidase 2-mediated NLRP1 inflammasome activation involves in neuronal senescence in hippocampal neurons in vitro. Int Immunopharmacol 69:60–70. https://doi.org/10.1016/j.intimp.2019.01.025
Xu TZ, Shen XY, Sun LL, Chen YL, Zhang BQ, Huang DK, Li WZ (2019) Ginsenoside Rg1 protects against H2O2induced neuronal damage due to inhibition of the NLRP1 inflammasome signalling pathway in hippocampal neurons in vitro. Int J Mol Med 43(2):717–726. https://doi.org/10.3892/ijmm.2018.4005
Muhammad T, Ikram M, Ullah R, Rehman SU, Kim MO (2019) Hesperetin, a Citrus Flavonoid, Attenuates LPS-Induced Neuroinflammation, Apoptosis and Memory Impairments by Modulating TLR4/NF-kappaB Signaling. Nutrients 11(3). https://doi.org/10.3390/nu11030648
d’Avila JC, Siqueira LD, Mazeraud A, Azevedo EP, Foguel D, Castro-Faria-Neto HC, Sharshar T, Chretien F et al (2018) Age-related cognitive impairment is associated with long-term neuroinflammation and oxidative stress in a mouse model of episodic systemic inflammation. J Neuroinflammation 15(1):28. https://doi.org/10.1186/s12974-018-1059-y
Qin L, Liu Y, Hong JS, Crews FT (2013) NADPH oxidase and aging drive microglial activation, oxidative stress, and dopaminergic neurodegeneration following systemic LPS administration. Glia 61(6):855–868. https://doi.org/10.1002/glia.22479
Chakroborty S, Stutzmann GE (2011) Early calcium dysregulation in Alzheimer’s disease: setting the stage for synaptic dysfunction. Sci China Life Sci 54(8):752–762. https://doi.org/10.1007/s11427-011-4205-7
Pascual-Caro C, Espinosa-Bermejo N, Pozo-Guisado E, Martin-Romero FJ (2018) Role of STIM1 in neurodegeneration. World J Biol Chem 9(2):16–24. https://doi.org/10.4331/wjbc.v9.i2.16
Bavencoffe A, Zhu MX, Tian JB (2017) New Aspects of the Contribution of ER to SOCE Regulation: TRPC Proteins as a Link Between Plasma Membrane Ion Transport and Intracellular Ca(2+) Stores. Adv Exp Med Biol 993:239–255. https://doi.org/10.1007/978-3-319-57732-6_13
Darbellay B, Arnaudeau S, Konig S, Jousset H, Bader C, Demaurex N, Bernheim L (2009) STIM1- and Orai1-dependent store-operated calcium entry regulates human myoblast differentiation. J Biol Chem 284(8):5370–5380. https://doi.org/10.1074/jbc.M806726200
Wegierski T, Kuznicki J (2018) Neuronal calcium signaling via store-operated channels in health and disease. Cell Calcium 74:102–111.
Calvo-Rodriguez M, Hernando-Perez E, Nunez L, Villalobos C (2019) Amyloid beta Oligomers Increase ER-Mitochondria Ca(2+) Cross Talk in Young Hippocampal Neurons and Exacerbate Aging-Induced Intracellular Ca(2+) Remodeling. Front Cell Neurosci 13:22. https://doi.org/10.3389/fncel.2019.00022
Chandran R, Kumar M, Kesavan L, Jacob RS, Gunasekaran S, Lakshmi S, Sadasivan C, Omkumar RV (2019) Cellular calcium signaling in the aging brain. J Chem Neuroanat 95:95–114. https://doi.org/10.1016/j.jchemneu.2017.11.008
He RL, Wu ZJ, Liu XR, Gui LX, Wang RX, Lin MJ (2018) Calcineurin/NFAT Signaling Modulates Pulmonary Artery Smooth Muscle Cell Proliferation, Migration and Apoptosis in Monocrotaline-Induced Pulmonary Arterial Hypertension Rats. Cell Physiol Biochem 49(1):172–189. https://doi.org/10.1159/000492852
Foster TC, Sharrow KM, Masse JR, Norris CM, Kumar A (2001) Calcineurin links Ca2+ dysregulation with brain aging. J Neurosci 21(11):4066–4073
Foster TC, Norris CM (1997) Age-associated changes in Ca(2+)-dependent processes: relation to hippocampal synaptic plasticity. Hippocampus 7(6):602–612. https://doi.org/10.1002/(SICI)1098-1063(1997)7:6%3c602::AID-HIPO3%3e3.0.CO;2-G
Quang CT, Leboucher S, Passaro D, Fuhrmann L, Nourieh M, Vincent-Salomon A, Ghysdael J (2015) The calcineurin/NFAT pathway is activated in diagnostic breast cancer cases and is essential to survival and metastasis of mammary cancer cells. Cell Death Dis 6:e1658. https://doi.org/10.1038/cddis.2015.14
Abdul HM, Sama MA, Furman JL, Mathis DM, Beckett TL, Weidner AM, Patel ES, Baig I et al (2009) Cognitive decline in Alzheimer’s disease is associated with selective changes in calcineurin/NFAT signaling. J Neurosci 29(41):12957–12969. https://doi.org/10.1523/JNEUROSCI.1064-09.2009
Calvo-Rodriguez M, de la Fuente C, Garcia-Durillo M, Garcia-Rodriguez C, Villalobos C, Nunez L (2017) Aging and amyloid beta oligomers enhance TLR4 expression, LPS-induced Ca(2+) responses, and neuron cell death in cultured rat hippocampal neurons. J Neuroinflammation 14(1):24. https://doi.org/10.1186/s12974-017-0802-0
Boutajangout A, Lindberg H, Awwad A, Paul A, Baitalmal R, Almokyad I, Hoiden-Guthenberg I, Gunneriusson E et al (2019) Affibody-Mediated Sequestration of Amyloid beta Demonstrates Preventive Efficacy in a Transgenic Alzheimer’s Disease Mouse Model. Front Aging Neurosci 11:64. https://doi.org/10.3389/fnagi.2019.00064
Zhao Y, Jaber V, Lukiw WJ (2017) Secretory Products of the Human GI Tract Microbiome and Their Potential Impact on Alzheimer’s Disease (AD): Detection of Lipopolysaccharide (LPS) in AD Hippocampus. Front Cell Infect Microbiol 7:318. https://doi.org/10.3389/fcimb.2017.00318
Zhou J, Yu W, Zhang M, Tian X, Li Y, Lu Y (2019) Imbalance of Microglial TLR4/TREM2 in LPS-Treated APP/PS1 Transgenic Mice: A Potential Link Between Alzheimer’s Disease and Systemic Inflammation. Neurochem Res 44(5):1138–1151. https://doi.org/10.1007/s11064-019-02748-x
Liu Y, Zhang Y, Zheng X, Fang T, Yang X, Luo X, Guo A, Newell KA et al (2018) Galantamine improves cognition, hippocampal inflammation, and synaptic plasticity impairments induced by lipopolysaccharide in mice. J Neuroinflammation 15(1):112. https://doi.org/10.1186/s12974-018-1141-5
Blennow K, de Leon MJ, Zetterberg H (2006) Alzheimer’s disease. Lancet 368(9533):387–403. https://doi.org/10.1016/S0140-6736(06)69113-7
De Strooper B, Karran E (2016) The Cellular Phase of Alzheimer’s Disease. Cell 164(4):603–615. https://doi.org/10.1016/j.cell.2015.12.056
Badshah H, Ali T, Kim MO (2016) Osmotin attenuates LPS-induced neuroinflammation and memory impairments via the TLR4/NFkappaB signaling pathway. Sci Rep 6:24493. https://doi.org/10.1038/srep24493
Selkoe DJ (1998) The cell biology of beta-amyloid precursor protein and presenilin in Alzheimer’s disease. Trends Cell Biol 8(11):447–453. https://doi.org/10.1016/s0962-8924(98)01363-4
Jin WS, Shen LL, Bu XL, Zhang WW, Chen SH, Huang ZL, Xiong JX, Gao CY et al (2017) Peritoneal dialysis reduces amyloid-beta plasma levels in humans and attenuates Alzheimer-associated phenotypes in an APP/PS1 mouse model. Acta Neuropathol 134(2):207–220. https://doi.org/10.1007/s00401-017-1721-y
Choi SI, Lee B, Woo JH, Jeong JB, Jun I, Kim EK (2019) APP processing and metabolism in corneal fibroblasts and epithelium as a potential biomarker for Alzheimer’s disease. Exp Eye Res 182:167–174. https://doi.org/10.1016/j.exer.2019.03.012
Al-Atrache Z, Lopez DB, Hingley ST, Appelt DM (2019) Astrocytes infected with Chlamydia pneumoniae demonstrate altered expression and activity of secretases involved in the generation of beta-amyloid found in Alzheimer disease. BMC Neurosci 20(1):6. https://doi.org/10.1186/s12868-019-0489-5
Fischer R, Maier O (2015) Interrelation of oxidative stress and inflammation in neurodegenerative disease: role of TNF. Oxid Med Cell Longev 2015:610813. https://doi.org/10.1155/2015/610813
Magi S, Castaldo P, Macri ML, Maiolino M, Matteucci A, Bastioli G, Gratteri S, Amoroso S et al (2016) Intracellular Calcium Dysregulation: Implications for Alzheimer’s Disease. Biomed Res Int 2016:6701324. https://doi.org/10.1155/2016/6701324
Taupin P (2010) A dual activity of ROS and oxidative stress on adult neurogenesis and Alzheimer’s disease. Cent Nerv Syst Agents Med Chem 10(1):16–21. https://doi.org/10.2174/187152410790780172
Shah SA, Khan M, Jo MH, Jo MG, Amin FU, Kim MO (2017) Melatonin Stimulates the SIRT1/Nrf2 Signaling Pathway Counteracting Lipopolysaccharide (LPS)-Induced Oxidative Stress to Rescue Postnatal Rat Brain. CNS Neurosci Ther 23(1):33–44. https://doi.org/10.1111/cns.12588
Quick KL, Ali SS, Arch R, Xiong C, Wozniak D, Dugan LL (2008) A carboxyfullerene SOD mimetic improves cognition and extends the lifespan of mice. Neurobiol Aging 29(1):117–128. https://doi.org/10.1016/j.neurobiolaging.2006.09.014
Dugan LL, Ali SS, Shekhtman G, Roberts AJ, Lucero J, Quick KL, Behrens MM (2009) IL-6 mediated degeneration of forebrain GABAergic interneurons and cognitive impairment in aged mice through activation of neuronal NADPH oxidase. PLoS ONE 4(5):e5518. https://doi.org/10.1371/journal.pone.0005518
Cahill-Smith S, Li JM (2014) Oxidative stress, redox signalling and endothelial dysfunction in ageing-related neurodegenerative diseases: a role of NADPH oxidase 2. Br J Clin Pharmacol 78(3):441–453. https://doi.org/10.1111/bcp.12357
Ali SS, Young JW, Wallace CK, Gresack J, Jeste DV, Geyer MA, Dugan LL, Risbrough VB (2011) Initial evidence linking synaptic superoxide production with poor short-term memory in aged mice. Brain Res 1368:65–70. https://doi.org/10.1016/j.brainres.2010.11.009
Tammariello SP, Quinn MT, Estus S (2000) NADPH oxidase contributes directly to oxidative stress and apoptosis in nerve growth factor-deprived sympathetic neurons. J Neurosci 20(1):RC53
Bedard K, Krause KH (2007) The NOX family of ROS-generating NADPH oxidases: physiology and pathophysiology. Physiol Rev 87(1):245–313.
Liu L, Chan C (2014) The role of inflammasome in Alzheimer’s disease. Ageing Res Rev 15:6–15. https://doi.org/10.1016/j.arr.2013.12.007
Wyss-Coray T, Rogers J (2012) Inflammation in Alzheimer disease-a brief review of the basic science and clinical literature. Cold Spring Harb Perspect Med 2(1):a006346. https://doi.org/10.1101/cshperspect.a006346
Venegas C, Heneka MT (2019) Inflammasome-mediated innate immunity in Alzheimer’s disease. FASEB J 33(12):13075–13084. https://doi.org/10.1096/fj.201900439
Man SM, Kanneganti TD (2015) Regulation of inflammasome activation. Immunol Rev 265(1):6–21. https://doi.org/10.1111/imr.12296
Arioz BI, Tastan B, Tarakcioglu E, Tufekci KU, Olcum M, Ersoy N, Bagriyanik A, Genc K et al (2019) Melatonin Attenuates LPS-Induced Acute Depressive-Like Behaviors and Microglial NLRP3 Inflammasome Activation Through the SIRT1/Nrf2 Pathway. Front Immunol 10:1511. https://doi.org/10.3389/fimmu.2019.01511
Zhang Q, Zhao S, Zheng W, Fu H, Wu T, Hu F (2020) Plumbagin attenuated oxygen-glucose deprivation/reoxygenation-induced injury in human SH-SY5Y cells by inhibiting NOX4-derived ROS-activated NLRP3 inflammasome. Biosci Biotechnol Biochem 84(1):134–142. https://doi.org/10.1080/09168451.2019.1664893
Mamik MK, Power C (2017) Inflammasomes in neurological diseases: emerging pathogenic and therapeutic concepts. Brain 140(9):2273–2285. https://doi.org/10.1093/brain/awx133
Ma C, Li S, Hu Y, Ma Y, Wu Y, Wu C, Liu X, Wang B, Hu G, Zhou J, Yang S (2021) AIM2 controls microglial inflammation to prevent experimental autoimmune encephalomyelitis. J Exp Med 218(5). https://doi.org/10.1084/jem.20201796
Zhang F, Jiang L (2015) Neuroinflammation in Alzheimer’s disease. Neuropsychiatr Dis Treat 11:243–256. https://doi.org/10.2147/NDT.S75546
Sastre M, Dewachter I, Landreth GE, Willson TM, Klockgether T, van Leuven F, Heneka MT (2003) Nonsteroidal anti-inflammatory drugs and peroxisome proliferator-activated receptor-gamma agonists modulate immunostimulated processing of amyloid precursor protein through regulation of beta-secretase. J Neurosci 23(30):9796–9804
Ehrenmann M, Tomakidi P, Hellwig E, Schulz SD, Polydorou O (2017) Effects of low-dose Bisphenol A on calcium ion influx and on genes of proliferation and differentiation in immortalized human gingival cells in vitro: The role of estrogen receptor beta. Dent Mater 33(9):1021–1032.
Tojima T, Hines JH, Henley JR, Kamiguchi H (2011) Second messengers and membrane trafficking direct and organize growth cone steering. Nat Rev Neurosci 12(4):191–203. https://doi.org/10.1038/nrn2996
Berridge MJ (2010) Calcium hypothesis of Alzheimer’s disease. Pflugers Arch 459(3):441–449. https://doi.org/10.1007/s00424-009-0736-1
Bezprozvanny I (2009) Calcium signaling and neurodegenerative diseases. Trends Mol Med 15(3):89–100. https://doi.org/10.1016/j.molmed.2009.01.001
Mattson MP (2007) Calcium and neurodegeneration. Aging Cell 6(3):337–350. https://doi.org/10.1111/j.1474-9726.2007.00275.x
Avila-Medina J, Calderon-Sanchez E, Gonzalez-Rodriguez P, Monje-Quiroga F, Rosado JA, Castellano A, Ordonez A, Smani T (2016) Orai1 and TRPC1 Proteins Co-localize with CaV1.2 Channels to Form a Signal Complex in Vascular Smooth Muscle Cells. J Biol Chem 291(40):21148–21159
Beziau DM, Toussaint F, Blanchette A, Dayeh NR, Charbel C, Tardif JC, Dupuis J, Ledoux J (2015) Expression of phosphoinositide-specific phospholipase C isoforms in native endothelial cells. PLoS ONE 10(4):e0123769. https://doi.org/10.1371/journal.pone.0123769
Jiao FZ, Wang Y, Zhang HY, Zhang WB, Wang LW, Gong ZJ (2018) Histone Deacetylase 2 Inhibitor CAY10683 Alleviates Lipopolysaccharide Induced Neuroinflammation Through Attenuating TLR4/NF-kappaB Signaling Pathway. Neurochem Res 43(6):1161–1170. https://doi.org/10.1007/s11064-018-2532-9
Zhao C, Hou W, Lei H, Huang L, Wang S, Cui D, Xing C, Wang X et al (2017) Potassium 2-(l-hydroxypentyl)-benzoate attenuates neuroinflammatory responses and upregulates heme oxygenase-1 in systemic lipopolysaccharide-induced inflammation in mice. Acta Pharm Sin B 7(4):470–478. https://doi.org/10.1016/j.apsb.2017.04.007
Bittremieux M, Gerasimenko JV, Schuermans M, Luyten T, Stapleton E, Alzayady KJ, De Smedt H, Yule DI et al (2017) DPB162-AE, an inhibitor of store-operated Ca(2+) entry, can deplete the endoplasmic reticulum Ca(2+) store. Cell Calcium 62:60–70. https://doi.org/10.1016/j.ceca.2017.01.015
Furman JL, Sompol P, Kraner SD, Pleiss MM, Putman EJ, Dunkerson J, Mohmmad Abdul H, Roberts KN et al (2016) Blockade of Astrocytic Calcineurin/NFAT Signaling Helps to Normalize Hippocampal Synaptic Function and Plasticity in a Rat Model of Traumatic Brain Injury. J Neurosci 36(5):1502–1515. https://doi.org/10.1523/JNEUROSCI.1930-15.2016
Rajput MS, Nirmal NP, Rathore D, Dahima R (2020) Dimethyl fumarate exerts neuroprotection by modulating calcineurin/NFAT1 and NFkappaB dependent BACE1 activity in Abeta1-42 treated neuroblastoma SH-SY5Y cells. Brain Res Bull 165:97–107. https://doi.org/10.1016/j.brainresbull.2020.08.024
Thapak P, Khare P, Bishnoi M, Sharma SS (2020) Neuroprotective Effect of 2-Aminoethoxydiphenyl Borate (2-APB) in Amyloid beta-Induced Memory Dysfunction: A Mechanistic Study. Cell Mol Neurobiol. https://doi.org/10.1007/s10571-020-01012-z
Hou L, Sun F, Huang R, Sun W, Zhang D, Wang Q (2019) Inhibition of NADPH oxidase by apocynin prevents learning and memory deficits in a mouse Parkinson’s disease model. Redox Biol 22:101134. https://doi.org/10.1016/j.redox.2019.101134
Joseph E, Villalobos-Acosta DMA, Torres-Ramos MA, Farfan-Garcia ED, Gomez-Lopez M, Miliar-Garcia A, Fragoso-Vazquez MJ, Garcia-Marin ID et al (2020) Neuroprotective Effects of Apocynin and Galantamine During the Chronic Administration of Scopolamine in an Alzheimer’s Disease Model. J Mol Neurosci 70(2):180–193. https://doi.org/10.1007/s12031-019-01426-5
Chiarotto GB, Cartarozzi LP, Perez M, Biscola NP, Spejo AB, Gubert F, Franca Junior M, Mendez-Otero R et al (2019) Tempol improves neuroinflammation and delays motor dysfunction in a mouse model (SOD1(G93A)) of ALS. J Neuroinflammation 16(1):218. https://doi.org/10.1186/s12974-019-1598-x
Chonpathompikunlert P, Han J, Toh K, Isoda H, Nagasaki Y (2011) TEMPOL protects human neuroblastoma SH-SY5Y cells against beta-amyloid-induced cell toxicity. Eur J Pharmacol 650(2–3):544–549. https://doi.org/10.1016/j.ejphar.2010.10.028
Dohare P, Hyzinski-Garcia MC, Vipani A, Bowens NH, Nalwalk JW, Feustel PJ, Keller RW Jr, Jourd’heuil D et al (2014) The neuroprotective properties of the superoxide dismutase mimetic tempol correlate with its ability to reduce pathological glutamate release in a rodent model of stroke. Free Radic Biol Med 77:168–182. https://doi.org/10.1016/j.freeradbiomed.2014.08.029
Zheng J, Fang F, Zeng X, Medler TR, Fiorillo AA, Clevenger CV (2011) Negative cross talk between NFAT1 and Stat5 signaling in breast cancer. Mol Endocrinol 25(12):2054–2064. https://doi.org/10.1210/me.2011-1141
Gorlach A, Bertram K, Hudecova S, Krizanova O (2015) Calcium and ROS: A mutual interplay. Redox Biol 6:260–271. https://doi.org/10.1016/j.redox.2015.08.010
Madreiter-Sokolowski CT, Thomas C, Ristow M (2020) Interrelation between ROS and Ca(2+) in aging and age-related diseases. Redox Biol 36:101678. https://doi.org/10.1016/j.redox.2020.101678
Acknowledgements
We would like to thank Zhirui Fang in the Department of Pharmacology and Dake Huang in the Synthetic Laboratory of Basic Medicine College for their technical assistance.
Funding
This study was supported by the Major projects of Anhui Provincial Department of Education (KJ2020ZD14), the National Natural Science Foundation of China (81970630, 81671384) and Basic and Clinical Cooperative Research Promotion Program of Anhui Medical University (2019xkjT021).
Author information
Authors and Affiliations
Contributions
Z.S. performed the experiment, analyzed the data, and prepared the manuscript. X.L. and L.Y. performed the behavior test and collected the data. X.D., Y.H., and Y.L. helped to complete the experiment. J.L. and W.L. designed and directed the study and revised the manuscript.
Corresponding author
Ethics declarations
Ethics approval
All experimental procedures were approved by the Ethics Committee for Experimental Animal Use and Care of Anhui Medical University.
Competing interests
The authors report no competing interests.
Consent to Participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
12035_2021_2717_MOESM2_ESM.jpg
Supplementary Figure S2 The effects of 2-APB,apocynin and tempol treatment on apoptosis-related proteins in LPS-induced mice(Western blot). (A) The bands of Bax, cleaved-caspase-3 and Bcl-2 inhippocampus tissues; (B-D) The relative expressions of Bax, cleaved-caspase-3and Bcl-2. The data are expressed as mean ± SD, n = 4, **P<0.01compared with LPS group (JPG 487 KB)
12035_2021_2717_MOESM3_ESM.jpg
Supplementary Figure S3 LPS exposureincreases the level of ROS production in HT22 cells (DCFH-DA staining, 200×).(A) The effect of LPS (5, 10, 20 and 40 μg/ml) on ROS generation. (B) Theeffect of 2-APB, apocynin and tempol treatment on ROS generation in LPS-inducedHT22 cells. (C) Quantitative analysis of different doses of LPS on ROSgeneration. (D) Quantitative analysis of 2-APB, apocynin and tempol treatmenton ROS generation. The data are expressed as mean ± SD, n = 3, *P<0.05,**P<0.01 compared with control or LPS group (JPG 1922 KB)
12035_2021_2717_MOESM4_ESM.jpg
Supplementary Figure S4 Chronic LPS exposureincreases the expressions of NOX2 and NLRP1-related mRNAs in HT22 cells(q-PCR). (A-F) The relative mRNA levels of NOX2, p22phox, p47phox, NLRP1,caspase-1 and ASC in HT22 cells. The data are expressed as mean ± SD, n = 3, *P<0.05,**P<0.01 compared with LPS group (JPG 297 KB)
12035_2021_2717_MOESM5_ESM.jpg
Supplementary Figure S5 LPS increased IP3generation and the level of p-PLC in HT22 cells. (A) The levels of IP3 in HT22cells after LPS (20μg/ml) treatment for 5 min, 20 min and 48 h (ELISA, n = 3).(B) The bands of p-PLC and PLC after LPS (20μg/ml) treatment for 5 min, 20 minand 48 h (Western blot, n = 3). (C and D) The relative expressions of PLC andp-PLC. The data are expressed as mean ± SD, no significant (ns), *P<0.05,**P<0.01 compared with control group (JPG 451 KB)
12035_2021_2717_MOESM6_ESM.jpg
Supplementary Figure S6 VIVIT treatment decreases theexpressions of NFAT1, NLRP1 and NOX2 in LPS-induced HT22 cells (Western blot). (A) The bands of NFAT1, NLRP1and NOX2 in HT22 cells; (B-D) The relative expressions of NFAT1, NLRP1 andNOX2. The data are expressed as mean ± SD, n = 3, *P<0.05, **P<0.01 compared with LPS group (JPG 424 KB)
12035_2021_2717_MOESM7_ESM.jpg
Supplementary Figure S7 Chronic LPS exposureincreases the levels of NLRP3, NLRC4 and AIM2 in hippocampus tissues in mice(Western blot). (A) The bands of NLRP3, NLRC4 and AIM2 in hippocampus tissues;(B-D) The relative expressions of NLRP3, NLRC4 and AIM2. The data are expressed as mean ± SD, n = 4, *P<0.05, **P<0.01 compared with LPS group (JPG 576 KB)
Rights and permissions
About this article
Cite this article
Sun, Z., Li, X., Yang, L. et al. SOCE-mediated NFAT1–NOX2–NLRP1 inflammasome involves in lipopolysaccharide-induced neuronal damage and Aβ generation. Mol Neurobiol 59, 3183–3205 (2022). https://doi.org/10.1007/s12035-021-02717-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-021-02717-y