Abstract
The cellular prion protein, encoded by the gene Prnp, has been reported to be a receptor of β-amyloid. Their interaction is mandatory for neurotoxic effects of β-amyloid oligomers. In this study, we aimed to explore whether the cellular prion protein participates in the spreading of α-synuclein. Results demonstrate that Prnp expression is not mandatory for α-synuclein spreading. However, although the pathological spreading of α-synuclein can take place in the absence of Prnp, α-synuclein expanded faster in PrPC-overexpressing mice. In addition, α-synuclein binds strongly on PrPC-expressing cells, suggesting a role in modulating the effect of α-synuclein fibrils.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The cellular prion protein (PrPC), a glycosylphosphatidylinositol (GPI)-anchored protein, participates in several neural functions [1–3]. Relevantly, one of the most recently described functions of the protein points to PrPC is as a receptor for β-amyloid (Aβ) [4]. Indeed, today it is well established that Aβ oligomers can bind with great affinity to PrPC [5, 6, 4, 7, 8] and to recombinant prion protein (e.g. [9, 10]). After binding, it was also proposed, although with some controversy [9, 11–13], that this interaction plays a crucial role in neurotoxic effects of Aβ oligomers such as inhibition of long-term potentiation (LTP), neuronal cell death and memory impairment in some mouse models of Alzheimer’s disease [14, 6, 4, 15–17]. Amyloid aggregates are present in many neurodegenerative diseases, and their formation occurs in a multistep process including the misfolding of healthy soluble proteins and their association into amyloid fibrils that form cell inclusions. In fact, among other aggregates (e.g. SOD1, CEPB3, TDP-43, etc.), those of Tau and α-synuclein, characteristic of tauopathies/Alzheimer’s disease and Parkinson’s disease, respectively, showed cell-to-cell transport in healthy cells through their uptake of misfolded polymers, which can propagate and spread throughout the neural parenchyma [18–23].
α-Synuclein is a key player in the pathogenesis of synucleinopathies, including Parkinson’s disease, dementia with Lewy bodies and multiple system atrophy [24]. Transmission of synthetic α-synuclein aggregates has been demonstrated in several cellular and animal models (see [25–27] for reviews). Several groups have reported that α-synuclein shows prion-like propagation in wild-type mice [28–30]. However, the basis of the spreading process remains poorly understood although cell-to-cell transport via exocytosis has been suggested [31–33]. For this reason, PrPC is proposed as an Aβ receptor (see above), and in this study, we aimed to explore whether PrPC is involved in the propagation and spreading of α-synuclein. Results demonstrated that α-synuclein could propagate and spread in mice lacking or overexpressing Prnp, including wild-type mice. However, increased quantities of p-α-synuclein can be seen in the motor cortex of PrPC-overexpressing mice as compared to Prnp +/+ and Prnp 0/0 mice. In addition, in vitro experiments also corroborated that although not required to trigger α-synuclein transport, Prnp overexpression enhances transported α-synuclein. In fact, α-synuclein binds strongly to Prnp-transfected HEK293 cells in contrast to mock-transfected ones. Moreover, the absence of the charged cluster (CC) domain of PrPC impairs α-synuclein binding in transfected cells. In conclusion, our results point to a non-mandatory but relevant role of Prnp in α-synuclein transport.
Material and Methods
Mouse Strains and Genotyping
Adult male C57Bl6/129sv-Prnp 0/0 (B6129 Prnp Zrchl/Zrchl Zurich I) mice were purchased from the European Mouse Mutant Archive (EMMA, Monterotondo, Italy) [34]. We backcrossed to C57BL/6 J for at least 8–9 generations to obtain 6–7% of 129 microsatellites in B6.129 Prnp 0/0 and control littermates B6.129 Prnp +/+ [35]. These Prnp 0/0 and Prnp +/+ mice were used in the present study. Specific primers for Prnp genotyping were designed in our laboratory based on the original P3 and P10 primers as described [34]: neo: 5′-gccttctatcgccttcttgac-3′; 3′ NCnew: 5′-gctacaggtggataacccctc-3′ and P10new: 5′-cataatcagtggaacaagccc-3’ [36]. Forty cycling conditions were 45″ 95 °C; 45″ 62 °C; 1′ 72 °C, followed by a final extension at 72 °C for 5 min. Prnp-overexpressing mice (Tga20) were purchased from EMMA (Monterotondo, Italy). They were generated as described by Marek et al. [37] and backcrossed in our lab with B6.129 Prnp 0/0 mice for seven generations [36]. The backcrossed mice were used in the study. For Tga20 mice, the transgene was detected using primers specific to the Tg20 allele 5′-caaccgacgtgaagcattctgccta-3′ and 5′-cctgggactccttctggtaccgggtgacgc-3′ as indicated [38]. The Ethics Committee on Animal Experimentation (CEEA) of the University of Barcelona approved all procedures described in this study. All housing, breeding and procedures were performed under the guidelines and protocols #276/16 and #141/15 of CEEA.
Preparation of Recombinant α-Synuclein Monomer and Fibrils
Mouse and human α-synuclein complementary DNAs (cDNAs) in bacterial expression plasmid pRK172 were used. α-Synuclein was expressed in Escherichia coli BL21 (DE3) cells and purified using boiling, Q-sepharose ion exchange chromatography and ammonium sulphate precipitation. Purified α-synuclein protein was dialyzed against 30 mM Tris–HCl, pH 7.5, and cleared using ultracentrifugation at 113,000g for 20 min. Protein concentration was determined with reverse phase HPLC. Proteins were loaded on an Aquapore RP-300 column (Brownlee) Perkin Elmer (Waltham, MA, USA) (equilibrated in 0.09% trifluoroacetic acid with a linear gradient of acetonitrile 0 to 50% at a flow rate of 1 ml/min). Purified mouse α-synuclein monomer (7 mg/ml) in 30 mM Tris–HCl, pH 7.5, containing 0.1% NaN3, was incubated at 37 °C in a shaking incubator at 200 rpm for 72 h. α-Synuclein fibrils were pelleted by spinning at 113,000g for 20 min and then suspended in PBS. α-Synuclein fibrils were sonicated with an ultrasonic homogenizer (VP-5S) Taitec (Nishikata, Japan) (at high power for 10 cycles (30 s on, 30 s off at 10 °C) before use. Aliquots of sonicated and non-sonicated fibrils were processed for transmission electron microscope (TEM) analysis and negative staining (Supplementary Fig. 1). In parallel, SDS-PAGE and western blot revealed the presence of a relevant 17 KDa and upper bands >35 KDa after sonication typical of protofibril preparations (Supplementary Fig. 1). To determine the concentration, fibrils were dissolved in 7 M guanidine hydrochloride and analysed with RP-HPLC as described above. Generated fibrils were tested to insure that they were endotoxin-free to avoid unwanted effects as described [39].
Transmission Electron Microscopy Procedures
Fibril solutions were fixed to carbon-forward-coated copper supports, and negative staining was performed using a 2% PTA-based (phosphotungstic acid) stain (pH 7.4), after which samples were placed in silica-based desiccant for a minimum of 2 h. Finally, we proceeded to TEM observation using a Leica electron microscope (Wetzlar, Germany) at SCT, University of Barcelona, Barcelona, Spain (Supplementary Fig. 1).
Stereotaxic Surgery
Five- to 6-month-old mice were anaesthetised with 50 mg/kg pentobarbital sodium and then were unilaterally injected with 5 μg (1 μg/μL solution) of recombinant mouse sonicated α-synuclein into postcommissural striatum (A-P 3.5 mm; M-L: 3.5 mm; D-V −0.9 mm from Bregma) at a rate of 0.1 μL/min. In parallel, some mice (n = 3) were sham-operated (Supplementary Fig. 1d). In these mice, the skull was opened and a glass pipette was placed in the abovementioned coordinates. After 10 min, the pipette was removed and the skin sutured. Sham-operated and fibril-injected mice were anaesthetised 45 days later with isofluorane and perfused with 4% buffered paraformaldehyde (pH 7.3). For immunohistochemistry, free-floating sections were rinsed in 0.1 M PBS, and endogenous peroxidase activity was blocked by incubation in 3% H2O2 and 10% methanol dissolved in 0.1 M PBS. After extensive rinsing, sections were incubated in 0.1 M PBS containing 0.2% gelatin, 10% normal serum, 0.2% glycine and 0.2% Triton X-100 for 1 h at room temperature. Afterwards, the sections were incubated for 24 h at 4 °C with the primary antibody: p-α-synuclein (p129S, clone 81A (cat. ab184674), 1:2000 diluted, Abcam, Cambridge, UK). After that, the sections were incubated with secondary biotinylated antibodies (2 h, 1:200 diluted) and streptavidin-horseradish peroxidase complex (2 h, 1:400 diluted). Peroxidase activity was revealed with 0.025% diaminobenzidine (DAB) and 0.003% hydrogen peroxide. After rinsing, the sections were mounted onto slides, dehydrated and coverslipped with Eukitt™ (Merck, Darmstadt, Germany). Samples were photodocumented using an Olympus (Hamburg, Germany) BX61 microscope equipped with a cooled digital DP72L camera. For quantification of Lewy body-like (LBL) p-α-synuclein-positive aggregates in motor cortex, equivalent sections at the level of the frontal cortex between Bregma 0 and 1 were selected (2–3 sections per mouse), and the total number of neuronal aggregates (LBL) of p-α-synuclein in layer V (300 μm w × 150 μm h box) was counted using a ×40 objective (oil immersion Zeiss, N.A. 0.85). Statistical analysis of the obtained data was performed with Bonferroni post hoc test (multiple comparison test) using GraphPad Prism 6 (Mac OsX, Graphpad). Data are presented as mean ± standard error of the mean (SEM). Differences between groups were considered statistically significant at **P < 0.01 and *P < 0.05.
Microfluidic Devices
Two different devices were used in an optimized modification of our previous design of large dual-chamber, open neuronal co-culture and of designs reported by Taylor et al. [40]. The open microfluidic device consists of two main open chambers interconnected by 100 microchannels. The large chamber areas (9 mm × 16 mm) facilitate effective cell culture and easy handling. The small cross-section areas of microchannels (3 μm × 10 μm or 10 μm × 10 μm) restrict the crossing of cortical neuron cell bodies but permit the passage of neuronal processes. The microfluidic device was made of poly(dimethylsiloxane) (PDMS) using standard photolithography and soft lithography.
Primary Embryonic Neuronal Cultures
E15.5 mouse embryo brains were dissected and washed in ice-cold 0.1 M phosphate-buffered saline (PBS) containing 6.5 mg/ml glucose. The meninges were removed and the cortices isolated. Tissue pieces were trypsinized for 15 min at 37 °C. After the addition of horse serum and centrifugation, cells were dissociated by trituration in 0.1 M PBS containing 0.025% DNAse with a fire-polished pipette. Dissociated cells were plated at ~10,000 cells/mm2 on one of the two reservoirs of microfluidic devices (A and B in Fig. 3) coated with poly-D-lysine (Sigma, Madrid, Spain). The culture medium was Neurobasal supplemented with 2 mM glutamine, 6.5 mg/ml glucose, antibiotics and B27 (Invitrogen-Life Technologies, Barcelona, Spain). After 72 h, 5 μM AraC (cytosine β-D-arabinofuranoside hydrochloride, Sigma) was added for 48 h to inhibit the growth of dividing non-neuronal cells. For characterization, cultures were immunostained using anti-glial fibrillary acidic protein (GFAP, cat. z0334; 1:500, Sigma), basic helix-loop-helix (bHLH) transcription factor olig2 (cat. AB9610, 1:200; Abcam) and class III β-tubulin (TUJ1, cat. 801201, 1:3000; Biolegend, CA, USA). Cultures contained up to 90% neurons (TUJ1-positive) and were used after 5–7 days in vitro. In parallel, some cultures were stained with Fluo4-AM (1 mg/ml, F14201, Invitrogen-Life Technologies) to confirm axonal interconnection between reservoirs prior to their processing.
Plasmids and Construction of PrPC-Deleted Forms
Mouse PrPC-encoding plasmid (pcDNA 3.1 backbone) and PrPC-IRES-GFP were provided by D. A. Harris (Boston University School of Medicine, Boston, MA, USA) and PrPC-truncated form ΔF35 by A. Aguzzi (University Hospital Zürich, Institute for Neuropathology, Switzerland). To generate deletion constructs ΔCD, ΔCC, ΔHR and ΔCR, the PrPC-encoding plasmid was used as a template for inverse PCRs, and the inserts obtained were fused. Briefly, a primer set was designed for each construct in order to amplify the entire plasmid, except for the region of Prnp to be deleted, i.e. regions 95–133, 95–110, 112–133 and 105–125 for ΔCD, ΔCC, ΔHR and ΔCR, respectively. Primers (Ecogen) were as follows: CD (F: 5′-AGCAGGCCCATGATCCATTTTG-3′, R: 5′-ATGGGTACCCCCTCCTTGGC-3′); CC (F: 5′-GTGGCAGGGGCTGCGGCAG-3′, R: 5′-ATGGGTACCCCCTCCTTGGCC-3′); HR (F: 5′-AGCAGGCCCATGATCCATTTTG-3′, R: 5′-TGCCACATGCTTGAGGTTGG-3′); CR (F: 5′-TACATGCTGGGGAGCGCC-3′, R: 5′-TTTTGGTTTGCTGGGCTTGTTC-3′). After amplification (Accuprime Taq Polymerase™, Invitrogen), the blunt ends of the amplimers were phosphorylated using the T4 kinase reaction (Invitrogen) and then religated (Fast-Link Ligase™, Epicentre Biotech.). An aliquot of each ligation reaction was electroporated into Escherichia coli DH5α, and transformants were selected for ampicillin resistance. Twenty-five candidates were selected and screened with sequence analysis (Terminator Big Dye™ v3.1, Applied Biosystems).
Cell Culture and Transfection
HEK293 cells (ATCC CRL-1573™, American Type Culture Collection, MD, USA) were maintained in Dulbecco’s modified eagle medium (DMEM, Invitrogen-Life Technologies), 10% foetal bovine serum (FBS, Invitrogen-Life Technologies) and 1% penicillin/streptomycin (Invitrogen-Life Technologies) in 75 cm2 culture bottles in a 5% CO2 atmosphere at 37 °C. One day before transfection, cells were cultured in DMEM supplemented with 10% FBS and without antibiotics, on poly-D-lysine (Sigma) coated plates. Transfection was performed using Lipofectamine Plus (Invitrogen-Life Technologies), according to the manufacturer’s instructions as indicated [41].
Caspase-3 Activity
Twenty-four hours after transfection, cells were scraped and lysed for 20 min on ice in cold lysis buffer (50 mM Hepes pH 7.5, 150 mM NaCl, 1.5 mM MgCl2, 1 mM EGTA pH 8, 10% glycerol, 1% Triton X-100) containing 1x protease inhibitor cocktail and phosphatase inhibitors. Lysates were centrifuged at 12000g for 5 min at 4 °C and supernatants were collected. Protein concentration was determined using a BCA protein assay kit (Pierce). The caspase-3 activity assay, with Ac-Asp-Glu-Val-Asp-7-amino-4-trifluoromethylcoumarin (Ac-DEVD-AFC, Sigma) as a substrate, was performed as previously described [42].
Immunocytochemical Procedures
One day before transfection, counted HEK293 cells were seeded onto poly-D-lysine (0.01 μg/μl) coated glass coverslips (12 mm Ø). Three days post-transfection, mouse α-synuclein (1 μg/ml medium) was added to the culture media. Treatment with α-synuclein was maintained for 3 days. Cells were fixed in 4% buffered paraformaldehyde (Sigma) and then permeabilized with 0.1% Triton X-100 (Sigma) in 0.1 M PBS. A similar fixation procedure was used for microfluidic devices (see [43] for details). After fixation, and extensive rinsing with 0.1 M PBS, cultures were blocked with 10% FBS in 0.1 M PBS prior to incubation with primary antibodies. Neurons were identified using a class III β-tubulin antibody (1:3000 diluted; Biolegend). PrPC was detected using anti-mouse 6H4 (1:500, Prionics; Schlieren, Switzerland), which recognizes the sequence DYEDRYYRE of the prion protein (human PrPC: aa 144–152), α-synuclein (1:500 diluted; Cell Signalling) and p-α-synuclein (mouse and human) (p129S/81A; 1:400 diluted; Abcam). After incubation with primary antibodies, cells were incubated with the pertinent Alexa Fluor-tagged secondary antibodies (Alexa-488 goat anti-mouse or Alexa-568 goat anti-rabbit) (Invitrogen-Life Technologies). Finally, cells were stained with 0.1 μM DAPI (Sigma) diluted in 0.1 M PBS, mounted on Mowiol™ (Calbiochem, San Diego, CA, USA) and viewed using an Olympus BX61 fluorescence microscope.
Western Immunoblot
Samples were homogenized in 10% wt/vol of 50 mM Tris–HCl, pH 7.4/150 mM NaCl/0.5% Triton X-100/0.5% Nonidet P-40, and a mixture of protease inhibitor cocktail (Roche, Basel, Switzerland) and phosphatase inhibitors (10 mM tetra-sodium pyrophosphate, 200 μM sodium orthovanadate and 10 mM sodium fluoride). After this, samples were centrifuged at 15,000g for 20 min at 4 °C. The resulting supernatant was normalized for protein content using BCA kit (Thermo Scientific Pierce, Paisley, UK). Cell extracts were boiled at 100 °C for 10 min, followed by 6% SDS electrophoresis and were then electrotransferred to nitrocellulose membranes for 1 h at 4 °C. Membranes were then blocked with 5% fat milk in 0.1 M Tris-buffered saline (pH 7.4) for 1 h and incubated overnight in 0.5% blocking solution containing primary antibodies. After incubation with peroxidase-tagged secondary antibodies (1:2000 diluted, Sigma), membranes were revealed with an ECL-plus chemiluminescence western blot kit (Amershan-Pharmacia Biotech, Piscataway, NJ, USA). In some experiments, peroxidase activity was revealed using a high sensitivity ECL-chemiluminescence kit (QuantaRed™, Thermo Scientific). In our experiments, each nitrocellulose membrane was used to detect α-synuclein (1:1000; Cell Signalling), p-α-synuclein (1:1000, p129S/81A; Abcam), β-actin (1:20,000; Sigma), β-tubulin (1:10,000; Sigma) and class III β-tubulin antibody (1:5000; Biolegend).
Densitometry and Statistical Processing
For quantification, developed films were scanned at 2400 × 2400 dpi (i800 MICROTEK high quality film scanner), and the densitometric analysis was performed using the Quantity One Image Software Analysis (Biorad, Barcelona, Spain). Statistical analysis of the obtained data was performed with Bonferroni post hoc test (Multiple comparison test) using GraphPad Prism 6 (Mac OsX, Grahpad). Data are presented as mean ± SEM. Differences between groups were considered statistically significant at *P < 0.05.
Results
α-Synuclein Transport in Prnp +/+, Prnp 0/0 and Tga20 Mice
Adult Prnp +/+, of recombinant endotoxin-free mouse α-synuclein (Fig. 1) in the postcommissural striatum, and the presence of phosphorylated α-synuclein (p-α-synuclein, p129S/81A–positive), were analysed 45 days later. Both sham- and non-operated mice presented the described pattern of p-α-synuclein in the adult mouse telencephalon (Supplementary Fig. 1, [44]). The antibody p129S/81A showed minor cross-reactivity with phosphorylated Neurofilament L. Indeed, several telencephalic regions showed background staining including the cingulate and parietal neocortex, hippocampus, striatum and some telencephalic axonal tracts (e.g. mamillothalamic tract) (Supplementary Fig. 1) [44]. However, aggregated forms of p-α-synuclein such as Lewy body-like (LBL) or Lewy neurite-like (LNL) forms were never observed after immunohistochemistry using the p129S/81A antibody in the telencephalon of non-operated and sham-operated mice, only appearing in the telecephalon after α-synuclein fibril injections (Supplementary Fig. 1). High magnification of LBL observed in the neocortex and amygdala 45 days after mouse α-synuclein striatal injections can be seen in Supplementary Fig. 1f, g. As observed, these aggregates were clearly identifiable over the background even using Ni-DAB development.
p-α-Synuclein pathology in the telencephalon of Prnp 0/0, Prnp +/+ and Tga20 mice injected with mouse α-synuclein fibrils in the postcommissural striatum. a-c Schemes illustrating the location of p-α-synuclein deposits (asterisks) shown in panels (d–o). d-o High power photomicrographs showing p-α-synuclein labelling in the striatum (d–f); neocortical layer V (g–i); amygdala (j–l) and S. nigra (m–o) of Prnp 0/0 (d, g, j, m), Prnp +/+ (e, h, k, n) and Tga20 (f, i, l, o) mice. Note the relevant accumulation of p-α-synuclein labelling in intracellular deposits of retrograde-labelled projecting neurons. Scale bar: d = 100 μm pertains to e–o
As indicated, the mice were processed after 45 days post-injection (Prnp +/+ (n = 6); Prnp 0/0 (n = 6) and Tga20 (n = 7)) in order to determine whether the regional distribution of p-α-synuclein was similar in the different Prnp genotypes (Figs. 1 and 2, Supplementary Fig. 1). Injection of mouse α-synuclein sonicated fibrils into postcommissural striatum induced p-α-synuclein pathology bilaterally throughout the brain, including striatum, amygdala, stria terminalis, substantia nigra and neocortex (Figs. 1 and 2, Supplementary Fig. 1). The anatomical and cellular distribution of p-α-synuclein aggregates was observed in Prnp +/+, Prnp 0/0 and Tga20 mice, as previously reported for wild-type mice in another study using similar α-synuclein fibrils and protocols [30]. At the cellular level, p-α-synuclein was mainly located in neurites and the neuronal perikaryon (as thick LBL or LNL aggregates) (Figs. 1 and 2, Supplementary Fig. 1e, f). At these post-inoculation times, p-α-synuclein labelling was observed bilaterally in the striatum, substantia nigra, amygdala, and entorhinal cortex and, ipsilaterally, in the motor cortex. However, although α-synuclein pathology was observed in the absence of Prnp, histological examination and quantitative analysis of genotypes determined increased p-α-synuclein staining as LBL in the ipsilateral motor cortex of Tga20 mice compared to Prnp 0/0 and Prnp +/+ (Prnp 0/0 = 11.86 ± 0.91; Prnp +/+ = 19.80 ± 2.25; Tga20 = 27.56 ± 2.19 (mean ± SEM). Prnp 0/0 vs Prnp +/+, mean diff −7.94, t = 2.669, 95% CI of diff = −15.63 to −0.2592. Prnp 0/0 vs Tga20, mean diff −15.70, t = 5.159, 95% CI of diff = −23.56 to −7.84. Prnp +/+ vs Tga20, mean diff −7.756, t = 2.795, 95% CI of diff = −14.92 to −0.59; ANOVA Bonferroni multiple comparison test) (Fig. 2). These data strongly suggest that although non-mandatory, Prnp overexpression enhances the regional transport of p-α-synuclein pathology in living mice.
Increased α-synuclein labelling as LBL aggregates in the neocortex in Tga20 mice. a–c Examples of p-α-synuclein aggregates in the motor cortex of Prnp 0/0, Prnp +/+ and Tga20 mice injected with mouse α-synuclein fibrils in the postcommissural striatum. Note the relevant accumulation of p-α-synuclein labelling in intracellular deposits of retrograde-labelled neurons in the cortical layer V of Tga20 mice. The LBL and LNL aggregates can be clearly seen over the pale background in the cortex. d Graph illustrating the quantification of the neuronal aggregates in the different genotypes. Each count represents one section. (Mice number Prnp +/+ (n = 5); Prnp 0/0 (n = 4) and Tga20 (n = 6)). In addition, the mean ± SEM is also plotted. *P < 0.05 and ***P < 0.01, ANOVA Bonferroni post hoc test. Scale bar: a = 100 μm pertains to b and c
Development of Microfluidic Devices to Monitor α-Synuclein Fibril Transport
α-Synuclein intracellular transport has been studied in vitro using commercial microfluidic devices (e.g. [45–48]). Our laboratory has developed two microfluidic designs based on previously published devices of our group (Fig. 3) [43]. Two different types of microgrooves (both 1 mm length) were generated for this study: 100 microgrooves of 3 μm (high) × 10 μm (wide) sections and 100 microgrooves of 10 (high) × 10 μm (wide) sections (Fig. 3a). Results in protein transport were similar for the two devices since microfluidic pressures were controlled to avoid non-specific non-neuronal transport (see below). As noted, α-synuclein transport in vitro can be done both anterogradely and retrogradely [45–47]. Thus, we cultured Prnp +/+ embryonic (E15.5) cortical neurons for 5–7 days in our devices to ensure crossing of axons between A and B. Under these conditions, around ≈85% of the devices showed large numbers of crossing axons after Fluo4-AM staining between reservoirs (Supplementary Fig. 2a, b). In addition, immunohistochemical analysis demonstrated that a large number of TUJ1-positive neurons with fewer astrocytes (glial fibrillary acidic protein (GFAP)-positive) and oligodendrocytes (olig2-positive) were observed in the devices (Fig. 3b, c). Recombinant (1 μg/ml) mouse (Fig. 3) or human (Supplementary Fig. 3) α-synuclein fibrils were added to one of the reservoirs (mainly in A; (A *) in Fig. 3) following the protocol of [46] with different volumes of medium between reservoirs (B > A; 100 μl), and their transport (A ⇒ B) were analysed 5 days later with immunocytochemistry (Fig. 3d–h, Supplementary Fig. 3) or western blot (Fig. 3i and Supplementary Figs. 2 and 4).
Analysis of α-synuclein transport using microfluidic devices. a 2D representation of the two PDMS devices used in the present study. b, c Double immunofluorescence photomicrographs illustrating TUJ1/GFAP (b) or TUJ1/olig2 (c) staining in primary cultured neurons in the devices. d Primary cortical cultures of the Prnp +/+ were maintained in the devices for 7 days. Then, mouse α-synuclein fibrils were added to A reservoir (asterisk), and their transport to B reservoir was analysed with immunocytochemistry (d–h) and western blot (i). d Examples of double-labelled neurons (TUJ1/α-synuclein) in B reservoir (indicated with camera icon) showing α-synuclein labelling (arrows). e, f Examples of p-α-synuclein-labelled neurons and neurites (arrows) in A reservoir (indicated with camera icon). g, h Examples of p-α-synuclein-labelled neurons and axons (arrows) in B reservoir (indicated with camera icon). i Western blot showing the presence of α-synuclein (17 kDa band) in both cellular extracts (A and B) and the absence in the culture medium of B in contrast to A reservoir, avoiding passive fluid transport. Membranes were reblotted with an antibody against β-tubulin or TUJ1 for standardization and characterization. Scale bar: b, d, e, g and h = 40 μm
First, we aimed to determine endogenous α-synuclein and p-α-synuclein labelling in our devices. At these stages, a very low α-synuclein immunostaining was observed in untreated devices in both A and B reservoirs. In addition, after using the p-α-synuclein (p129S/81A) antibody, no labelling was observed in the absence of α-synuclein fibril cultures. However, after α-synuclein fibril treatment in A (Fig. 3d), immunoreacted cultures showed the presence of relevant α-synuclein staining in the perikaryon, neurites and axons of cultured TUJ1-positive neurons in B (Fig. 3d). In addition, relevant p-α-synuclein labelling was observed in morphologically identified neurons located in both reservoirs (A and B) (Fig. 3e–h). More relevantly, p-α-synuclein aggregates (after mouse or human fibril treatment) were detected in identified axons and in the cytoplasm of cultured neurons in A as well in B (Fig. 3e–h, Supplementary Fig. 3b–g). In addition, to avoid the presence of passive transport of α-synuclein, we developed the detection of the protein in cell extracts and media of both reservoirs using the QuantaRed™-enhanced chemifluorescent HRP substrate (Thermo Fisher, cat. 15159) (Fig. 3i and Supplementary Figs. 2 and 4). After mouse α-synuclein fibril incubation in A, results revealed the presence of α-synuclein in both cellular extracts (A and B), with the absence in the culture media of B in contrast to the media of A reservoir, indicating the absence of passive fluidic flux between A ⇒ B (Fig. 3i and Supplementary Figs. 2 and 4) [43, 46]. In our devices, although different α-synuclein bands could be detected in A, the low molecular weight of α-synuclein (≈17 kDa) was mainly detected in B, as also recently reported by [47](Fig. 3, Supplementary Figs. 2 and 4). α-Synuclein transport was always observed in those devices showing large connectivity between A and B reservoirs (Fig. 3, Supplementary Figs. 3 and 4). However, in those displaying few axon numbers crossing between reservoirs (Supplementary Fig. 3), α-synuclein was almost absent in B (cell and media) and was only detected in the cellular and media extracts of A. This reinforced the notion of a specific axonal transport of α-synuclein fibrils between neurons displaying low endogenous levels of α-synuclein at these time points in culture (Supplementary Fig. 2). Thus, these devices are well suited to monitor cellular transport of mouse or human α-synuclein fibrils.
In Vitro Transport of α-Synuclein under Prnp Dosage
As indicated above, PrPC has been described as a receptor for β-amyloid [4, 49]. Although the participation of PrPC in the intercellular β-amyloid transport in microfluidic devices remains elusive, its expression seems to be needed to trigger β-amyloid-mediated effects in treated neurons (see the “ Introduction ” section for references). Primary cortical cultures from Prnp +/+, Prnp 0/0 and Tga20 embryos were treated with exogenous recombinant mouse α-synuclein fibrils, and both the binding in treated cells and their transport was analysed with western blot or immunocytochemistry (Fig. 4). First, we checked the percentage of devices without the α-synuclein transport. Results indicated that 14.28% (Prnp 0/0), 22.22% (Prnp +/+) and 16.66% (Tga20) of the cultures showed no α-synuclein transport in our microfluidic devices. In fact, these cultures displayed very few axons crossing between reservoirs as determined by Fluo4-AM staining (see example in Supplementary Fig. 2a). Second, we analysed the presence of exogenous α-synuclein in neurons in B reservoir after treatment in A. We were able to determine the presence of α-synuclein in neurons, irrespective of the Prnp genotype (Fig. 4a–d). Since neuronal presence of α-synuclein fibrils cannot be ascertained in a quantitative basis by simple fluorescence analysis, we processed parallel samples for western blot. Indeed, after protofibril treatment in A, western blots revealed increased α-synuclein/tubulin ratio in Tga20 than in WT and Prnp 0/0 cultured neurons in A suggesting a tendency of higher protofibril binding in presence of larger PrPC amounts (Prnp 0/0 = 0.344 ± 0.07; Prnp +/+ = 0.386 ± 0.08, Tga20 = 0.56 ± 0.14 (mean ± SEM)) (Fig. 4b). Next, western blot results corroborated that α-synuclein protofibrils could be transported to neurons from A to B irrespective of the Prnp genotype (Fig. 4). However, although not statistically significant (ANOVA Bonferroni post hoc test), values for transported α-synuclein were slightly higher in Tga20-derived primary neuronal cultures as compared to wild-type and Prnp 0/0 (Fig. 4c) (Prnp 0/0 = 0.467 ± 0.09; Prnp +/+ = 0.5561 ± 0.106, Tga20 = 0.7801 ± 0.206 (mean ± SEM)).
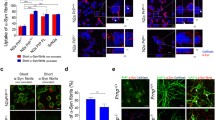
Determination of α-synuclein transport in neuronal cultures from mouse embryos carrying differing Prnp dosages. Recombinant mouse α-synuclein protofibrils were added to A reservoir (asterisk), and its binding to neurons in A reservoir as well as their transport towards B were analysed by western blot in cellular extracts. a–d Examples of double-labelled Prnp 0/0 (a, b) and Prnp +/+ (c, d) neurons (TUJ1/α-synuclein) in B reservoir showing discrete cytoplasmatic α-synuclein labelling (arrows). e Examples of western blot determination of one device for each Prnp genotype for α-synuclein. Anti-β-tubulin and anti-PrPC monoclonal antibodies were used for standardization and genotype characterization. Notice that PrPC was present in WT and Tga20 cells at the time of treatment. PrPC is downregulated shortly after plating neurons, and their levels increased over time in culture (see also [68] for details). f–g Densitometric analysis (see the “Material and Methods” section for details) were performed, and quantification was represented as the ratio between α-synuclein/β-tubulin detected in A reservoir after protofibril treatment (b) and ratio between α-synuclein/β-tubulin detected in B vs A reservoirs (c). Results for each device are represented by a single plot in the scatter plot. In addition, mean ± SEM is also plotted
Increased Binding of α-Synuclein in Prnp-Transfected Cells
Various possibilities have been proposed regarding α-synuclein interaction with plasma membrane [50–52, 48]. Thus, due to the in vitro and in vivo observations, we aimed to determine whether PrPC overexpression enhanced α-synuclein interaction with cells (Figs. 5 and 6 and Supplementary Fig. 5). We increased PrPC expression in a cellular system with very low PrPC expression, low endogenous α-synuclein binding properties [48] and lack of expression of other α-synuclein binding proteins (LAG3, neurexin 1β or APLP1) (HEK293 cells, Fig. 5) to analyse the binding of α-synuclein mouse protofibrils. First, HEK293 cells were transfected with PrPC-IRES-GFP, incubated with sonicated mouse α-synuclein protofibrils (1 μg/ml) and processed for α-synuclein immunolabelling (Fig. 5b). Results revealed that most GFP-positive HEK203 cells were labelled with the α-synuclein antibody (Fig. 5b). In a second set of experiments, HEK293 cells were transfected either with full-length Prnp (pcDNA-Prnp) or mock (pcDNA) plasmids and then incubated 24 h later with mouse α-synuclein fibrils; their cellular binding was analysed using western blot and immunocytochemistry for PrPC and α-synuclein (Fig. 5a, c–h). Blots indicated the presence of the 17 kDa α-synuclein band only in protein extracts of Prnp-transfected cells after α-synuclein treatment (Fig. 5a). This increased binding was also corroborated by immunocytochemistry in which α-synuclein labelling was prominent in identified double-labelled Prnp-expressing cells in contrast to non-expressing HEK293 cells (Fig. 5c–h). Fluorescence microscopy observation developed in 314 (PrPC-positive) identified cells from three different experiments demonstrated that 91.08% of the analysed cells with relevant α-synuclein labelling were also positive for PrPC (Fig. 5c, d). In contrast, a discrete puncta-like labelling of α-synuclein was observed randomly distributed over mock-transfected HEK293 cells with negligible levels of PrPC (Fig. 5e). At high magnification, although not exclusive, we determined a strong co-localization of the α-synuclein and PrPC labelling in discrete membrane regions of transfected cells, suggesting relevant cellular binding of protofibrils in regions with high PrPC presence (Fig. 5f–h).
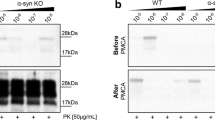
Increased binding of α-synuclein in Prnp-transfected HEK293 cells. a Western blot shows increased labelling of the 17 KDa α-synuclein band in HEK293 cells transfected with mouse Prnp-encoding plasmid in contrast to mock-transfected cells. Anti-β-tubulin monoclonal antibody was used for standardization, and anti-PrPC antibody was used to check PrPC overexpression after transfection. Notice that HEK293 cells showed a very low endogenous PrPC expression. The upper bands observed after protofibril treatment corresponded to non-monomeric forms of α-synuclein. b Examples of double-labelled GFP/α-synuclein HEK293 cells after transfection of PrPC-IRES-GFP. Note the presence of the relevant labelling in the two transfected cells in comparison to the disperse α-synuclein labelling in non-transfected cells (arrows). c–e Fluorescence photomicrographs showing examples of double-labelled cells PrPC (d) overexpressing cells and α-synuclein (c). HEK293 cells were transfected with Prnp-encoding plasmid (c, d) or mock-transfected cells (e). Arrows in c and d point to double-labelled cells, and the asterisk in d labels a PrPC-positive/α-synuclein-negative HEK293 cell. Arrows in e point to α-synuclein labelling in mock-transfected cells. f–h High magnification photomicrograph illustrating the distribution of α-synuclein (f) in PrPC-transfected HEK293 cells (g). Notice the relevant colocalization in several domains of the transfected cell including the plasma membrane (arrows in g and h). Scale bars: b, e = 25 μm. c, f = 25 μm belongs to d; g and h, respectively
a Scheme of the ΔCC, ΔHR maps and the full-length PrPC. b, c Fluorescence photomicrographs showing examples of double-labelled PrPC/α-synuclein cells (arrows). d, e Fluorescence photomicrographs showing examples of double-labelled cultures using the 6H4 PrPC and α-synuclein antibodies. Note the absence of double-labelled cells in these examples (arrows) and the background staining of α-synuclein labelling in non-transfected cells. h–k Fluorescence photomicrographs showing examples of double-labelled ΔHR/α-synuclein cells (arrows) after treatment over the labelling of non-transfected cells. Scale bar: b, d, f, h and j = 40 μm pertains to c and e, respectively
Involvement of the Charged Cluster Domain of PrPC in α-Synuclein Binding
It has been described how the residues of the CC of PrPC are involved in binding β-amyloid with PrPC [53]. Hence, we aimed to determine whether this domain also participates in α-synuclein binding (Fig. 6). After cloning, the expression of all PrPC variants in HEK293 cells were tested by western blotting (Supplementary Fig. 5). The endogenous level of Prnp expression in HEK293 was low (Fig. 5a), and all PrPC-modified proteins were detectable (Supplementary Fig. 5). However, expression of ΔF35 was markedly lower than that of the rest of the deleted forms, representing less than 50% of the expression of full-length PrPC (Supplementary Fig. 5). At this point, we considered the fact that some of these constructs are able to induce cell death when overexpressed in cell lines [54, 1]. Results indicate that only ΔF35 increased caspase 3 activity in transfected cells in contrast to other PrPC constructs (relative fluorescence units (RFU) ΔF35/pcDNA = 2.15 ± 0.38; ΔCC/pcDNA = 0.92 ± 0.27; ΔHR/pcDNA = 1.11 ± 0.21; PrPC/pcDNA = 1.14 ± 0.09; mean ± SEM) (Supplementary Fig. 5). After these results, we ignored ΔF35 in the next experiments and focused on the central domain (ΔCC and ΔHR) of PrPC (Figs. 5 and 6). In the experiments, we reduced the amount of the cDNA to half during cell transfection to ensure clear immunocytochemical detection of transfected cells. After transfection and immunocytochemistry, only 5.83% (22 of 377, n = 3) of the ΔCC-labelled cells were α-synuclein-positive (Fig. 6d–g) in contrast to ΔHR/α-synuclein (96.49% (110 of 114, n = 3)) (Fig. 6h–k) and PrPC/α-synuclein (91.08% (286 of 314 cells, n = 3) (Fig. 5c–h and Fig. 6b, c), indicating the participation of the CC domain of PrPC in α-synuclein binding to PrPC-transfected HEK293 cells.
Discussion
In this study, we determined that α-synuclein fibrils can be transported to different brain regions of wild-type mice after injection in the postcommissural striatum. Our results reinforce the notion that the spreading of p-α-synuclein pathology does not occur by diffusion or non-specific transport [45]. The transport observed in our experiments was similar to that reported in other studies using wild-type mice [29, 28], with relevant p-α-synuclein deposits in the striatum, substantia nigra, amygdala and neocortex. The anatomical connections between the striatum, substantia nigra, amygdala and neocortex are well described in the literature (e.g. [55]) and support the observed transport of α-synuclein. Although it has been reported to exist anterograde and retrograde transport of α-synuclein (see above), in our experiments, transported α-synuclein seemed to be more often transported retrogradely in the brain parenchyma, as suggested in other works [29, 28]. Our results also demonstrate for the first time that p-α-synuclein pathology after injection could spread to different brain regions in the absence of PrPC. Thus, Prnp expression is not mandatory for α-synuclein transport in the mouse brain, although increased levels of α-synuclein transport can be seen in wild-type and overexpressing mice. In fact, it has been reported that the absence of PrPC does not modify the appearance or temporal evolution of p-α-synuclein deposits in transgenic mice overexpressing human α-synuclein driven by a platelet-derived growth factor-β promoter [56]. Furthermore, changes on Prnp dosage do not alter α-synuclein expression in adult mice (not shown). Although data using additional models of synucleinopathies (e.g. A53T mice) have not been published, the present results are in line with these observations [56]. However, we also determined an increased number of motor pyramidal neurons displaying LBL aggregates in Prnp-overexpressing mice which suggest that, as also reported for β-amyloid, PrPC might participate in the cellular binding of α-synuclein and its expansion.
The interaction of several amyloids to PrPC is well characterized [14, 6, 4, 15–17]. We determined, using two different Prnp constructs, that their overexpression can enhance the binding of α-synuclein in HEK293 cells with low endogenous capability of α-synuclein binding (see also [48] for details). Several studies have reported the interaction of endogenous peptides of the amyloid family with the plasma membrane [57–61]. In fact, the interaction of Aβ, human or rat amylin, PrP(106–126) or α-synuclein fibrils with plasma membrane has been well described [57–60, 62], and several putative interactions with plasma membrane proteins have been described as well (e.g. APP [59] or GRP78 [51]). To this concern, a recent study of Mao and coworkers [48] reviewed in [63] points to the lymphocyte-activation gene 3 (LAG3/CD223) as the neuronal receptor of α-synuclein. LAG3 showed increased binding properties to α-synuclein protofibrils as compared to neurexin 1β, and APLP1 in SH-SY5Y-overexpressing cells [48]. mRNA levels of LAG3 do not change between Prnp genotypes (GEO database ref. GSE16223). However, and since a functional interaction between LAG3 with PrPC cannot be ruled out, we hypothesise that PrPC as well as other proteins (e.g. GRP78) may cooperate with LAG3 in neuronal α-synuclein transport. This is also relevant if considered that the absence of LAG3 does not fully impair α-synuclein protofibril transport in vitro and in vivo [48].
Although not described for other fibrillar peptides, PrPC has been reported as a receptor for Aβ (see above). The present study indicates that PrPC might contribute to enhanced binding of α-synuclein fibrils to the plasma membrane, in line with other studies, reporting an increased level of binding between Aβ and PrPC during ageing in several mouse models of Alzheimer’s disease [15]. In addition, our data suggest that the CC domain actively participates in α-synuclein binding. Residues located in the CC domain (aa 90–110 or aa 91–115) have been involved in binding with β-amyloid [64, 53] in cooperation with the N-terminal residues 23–58 [53]. As these PrPC domains have been revealed as putative pharmacological targets for Alzheimer’s disease [65–67], our data might also enhance the eligibility of PrPC as a putative target to modulate α-synuclein expansion.
Change history
05 May 2017
An erratum to this article has been published.
References
del Rio JA, Gavin R (2016) Functions of the cellular prion protein, the end of Moore’s law, and Ockham’s razor theory. Prion 10(1):25–40
Nicolas O, Gavin R, del Rio JA (2009) New insights into cellular prion protein (PrPc) functions: the “ying and yang” of a relevant protein. Brain Res Rev 61(2):170–184
Linden R, Martins VR, Prado MA, Cammarota M, Izquierdo I, Brentani RR (2008) Physiology of the prion protein. Physiol Rev 88(2):673–728
Lauren J, Gimbel DA, Nygaard HB, Gilbert JW, Strittmatter SM (2009) Cellular prion protein mediates impairment of synaptic plasticity by amyloid-beta oligomers. Nature 457(7233):1128–1132
Dohler F, Sepulveda-Falla D, Krasemann S, Altmeppen H, Schluter H, Hildebrand D, Zerr I, Matschke J et al (2014) High molecular mass assemblies of amyloid-beta oligomers bind prion protein in patients with Alzheimer’s disease. Brain 137(Pt 3):873–886
Freir DB, Nicoll AJ, Klyubin I, Panico S, Mc Donald JM, Risse E, Asante EA, Farrow MA et al (2011) Interaction between prion protein and toxic amyloid beta assemblies can be therapeutically targeted at multiple sites. Nat Commun 2:336
Zou WQ, Xiao X, Yuan J, Puoti G, Fujioka H, Wang X, Richardson S, Zhou X et al (2011) Amyloid-beta42 interacts mainly with insoluble prion protein in the Alzheimer brain. J Biol Chem 286(17):15095–15105
Ganzinger KA, Narayan P, Qamar SS, Weimann L, Ranasinghe RT, Aguzzi A, Dobson CM, McColl J et al (2014) Single-molecule imaging reveals that small amyloid-beta1-42 oligomers interact with the cellular prion protein (PrP(C)). Chembiochem 15(17):2515–2521
Balducci C, Beeg M, Stravalaci M, Bastone A, Sclip A, Biasini E, Tapella L, Colombo L et al (2010) Synthetic amyloid-beta oligomers impair long-term memory independently of cellular prion protein. Proc Natl Acad Sci U S A 107(5):2295–2300
Nieznanski K, Surewicz K, Chen S, Nieznanska H, Surewicz WK (2014) Interaction between prion protein and Aβ amyloid fibrils revisited. ACS Chem Neurosci 5(5):340–345
Calella AM, Farinelli M, Nuvolone M, Mirante O, Moos R, Falsig J, Mansuy IM, Aguzzi A (2010) Prion protein and Aβ-related synaptic toxicity impairment. EMBO Mol Med 2(8):306–314
Cisse M, Sanchez PE, Kim DH, Ho K, Yu GQ, Mucke L (2011) Ablation of cellular prion protein does not ameliorate abnormal neural network activity or cognitive dysfunction in the J20 line of human amyloid precursor protein transgenic mice. J Neurosci 31(29):10427–10431
Kessels HW, Nguyen LN, Nabavi S, Malinow R (2010) The prion protein as a receptor for amyloid-beta. Nature 466(7308):E3–E4 discussion E4-5
Barry AE, Klyubin I, Mc Donald JM, Mably AJ, Farrell MA, Scott M, Walsh DM, Rowan MJ (2011) Alzheimer’s disease brain-derived amyloid-beta-mediated inhibition of LTP in vivo is prevented by immunotargeting cellular prion protein. J Neurosci 31(20):7259–7263
Kostylev MA, Kaufman AC, Nygaard HB, Patel P, Haas LT, Gunther EC, Vortmeyer A, Strittmatter SM (2015) Prion-protein-interacting amyloid-beta oligomers of high molecular weight are tightly correlated with memory impairment in multiple Alzheimer mouse models. J Biol Chem 290(28):17415–17438
Um JW, Strittmatter SM (2013) Amyloid-beta induced signaling by cellular prion protein and Fyn kinase in Alzheimer disease. Prion 7(1):37–41
Scott-McKean JJ, Surewicz K, Choi JK, Ruffin VA, Salameh AI, Nieznanski K, Costa AC, Surewicz WK (2016) Soluble prion protein and its N-terminal fragment prevent impairment of synaptic plasticity by Aβ oligomers: implications for novel therapeutic strategy in Alzheimer’s disease. Neurobiol Dis 91:124–131
Hall GF, Patuto BA (2012) Is tau ready for admission to the prion club? Prion 6(3):223–233
Dehay B, Fernagut PO (2016) Alpha-synuclein-based models of Parkinson's disease. Rev Neurol (Paris)
Hasegawa M (2016) Molecular mechanisms in the pathogenesis of Alzheimer’s disease and tauopathies-prion-like seeded aggregation and phosphorylation. Biomolecules 6(2)
Kraus A, Groveman BR, Caughey B (2013) Prions and the potential transmissibility of protein misfolding diseases. Annu Rev Microbiol 67:543–564
Lee S, Kim HJ (2015) Prion-like mechanism in amyotrophic lateral sclerosis: are protein aggregates the key? Exp Neurobiol 24(1):1–7
Wu JW, Hussaini SA, Bastille IM, Rodriguez GA, Mrejeru A, Rilett K, Sanders DW, Cook C, Fu H, Boonen RA, Herman M, Nahmani E, Emrani S, Figueroa YH, Diamond MI, Clelland CL, Wray S, Duff KE (2016) Neuronal activity enhances tau propagation and tau pathology in vivo. Nat Neurosci 19(8):1085–1092. doi:10.1038/nn.4328
Braak H, Del Tredici K (2008) Invited article: nervous system pathology in sporadic Parkinson disease. Neurology 70(20):1916–1925
Le NT, Narkiewicz J, Aulic S, Salzano G, Tran HT, Scaini D, Moda F, Giachin G et al (2015) Synthetic prions and other human neurodegenerative proteinopathies. Virus Res 207:25–37
Fernandez-Borges N, Erana H, Venegas V, Elezgarai SR, Harrathi C, Castilla J (2015) Animal models for prion-like diseases. Virus Res 207:5–24
Walker LC, Jucker M (2015) Neurodegenerative diseases: expanding the prion concept. Annu Rev Neurosci 38:87–103
Luk KC, Kehm V, Carroll J, Zhang B, O'Brien P, Trojanowski JQ, Lee VM (2012) Pathological alpha-synuclein transmission initiates Parkinson-like neurodegeneration in nontransgenic mice. Science 338(6109):949–953
Masuda-Suzukake M, Nonaka T, Hosokawa M, Oikawa T, Arai T, Akiyama H, Mann DM, Hasegawa M (2013) Prion-like spreading of pathological alpha-synuclein in brain. Brain 136(Pt 4):1128–1138
Masuda-Suzukake M, Nonaka T, Hosokawa M, Kubo M, Shimozawa A, Akiyama H, Hasegawa M (2014) Pathological alpha-synuclein propagates through neural networks. Acta Neuropathol Commun 2:88
Desplats P, Lee HJ, Bae EJ, Patrick C, Rockenstein E, Crews L, Spencer B, Masliah E et al (2009) Inclusion formation and neuronal cell death through neuron-to-neuron transmission of alpha-synuclein. Proc Natl Acad Sci U S A 106(31):13010–13015
Angot E, Brundin P (2009) Dissecting the potential molecular mechanisms underlying alpha-synuclein cell-to-cell transfer in Parkinson’s disease. Parkinsonism Relat Disord 15(Suppl 3):S143–S147
Emmanouilidou E, Vekrellis K (2016) Exocytosis and spreading of normal and aberrant alpha-synuclein. Brain Pathol 26(3):398–403
Bueler H, Fischer M, Lang Y, Bluethmann H, Lipp HP, DeArmond SJ, Prusiner SB, Aguet M et al (1992) Normal development and behaviour of mice lacking the neuronal cell-surface PrP protein. Nature 356(6370):577–582
Carulla P, Llorens F, Matamoros-Angles A, Aguilar-Calvo P, Espinosa JC, Gavin R, Ferrer I, Legname G et al (2015) Involvement of PrP(C) in kainate-induced excitotoxicity in several mouse strains. Sci Rep 5:11971
Rangel A, Madronal N, Gruart A, Gavin R, Llorens F, Sumoy L, Torres JM, Delgado-Garcia JM et al (2009) Regulation of GABA(A) and glutamate receptor expression, synaptic facilitation and long-term potentiation in the hippocampus of prion mutant mice. PLoS One 4(10):e7592
Fischer M, Rulicke T, Raeber A, Sailer A, Moser M, Oesch B, Brandner S, Aguzzi A et al (1996) Prion protein (PrP) with amino-proximal deletions restoring susceptibility of PrP knockout mice to scrapie. EMBO J 15(6):1255–1264
Steele AD, Emsley JG, Ozdinler PH, Lindquist S, Macklis JD (2006) Prion protein (PrPc) positively regulates neural precursor proliferation during developmental and adult mammalian neurogenesis. Proc Natl Acad Sci U S A 103(9):3416–3421
Kim C, Lv G, Lee JS, Jung BC, Masuda-Suzukake M, Hong CS, Valera E, Lee HJ et al (2016) Exposure to bacterial endotoxin generates a distinct strain of alpha-synuclein fibril. Scientific reports 6:30891
Taylor AM, Blurton-Jones M, Rhee SW, Cribbs DH, Cotman CW, Jeon NL (2005) A microfluidic culture platform for CNS axonal injury, regeneration and transport. Nat Methods 2(8):599–605
Llorens F, Carulla P, Villa A, Torres JM, Fortes P, Ferrer I, del Rio JA (2013) PrP(C) regulates epidermal growth factor receptor function and cell shape dynamics in Neuro2a cells. J Neurochem 127(1):124–138
Gurtu V, Kain SR, Zhang G (1997) Fluorometric and colorimetric detection of caspase activity associated with apoptosis. Anal Biochem 251(1):98–102
Reginensi D, Carulla P, Nocentini S, Seira O, Serra-Picamal X, Torres-Espin A, Matamoros-Angles A, Gavin R et al (2015) Increased migration of olfactory ensheathing cells secreting the Nogo receptor ectodomain over inhibitory substrates and lesioned spinal cord. Cell Mol Life Sci 72(14):2719–2737
Sacino AN, Brooks M, Thomas MA, McKinney AB, McGarvey NH, Rutherford NJ, Ceballos-Diaz C, Robertson J et al (2014) Amyloidogenic alpha-synuclein seeds do not invariably induce rapid, widespread pathology in mice. Acta Neuropathol 127(5):645–665
Volpicelli-Daley LA, Luk KC, Patel TP, Tanik SA, Riddle DM, Stieber A, Meaney DF, Trojanowski JQ et al (2011) Exogenous alpha-synuclein fibrils induce Lewy body pathology leading to synaptic dysfunction and neuron death. Neuron 72(1):57–71
Freundt EC, Maynard N, Clancy EK, Roy S, Bousset L, Sourigues Y, Covert M, Melki R et al (2012) Neuron-to-neuron transmission of alpha-synuclein fibrils through axonal transport. Ann Neurol 72(4):517–524
Brahic M, Bousset L, Bieri G, Melki R, Gitler AD (2016) Axonal transport and secretion of fibrillar forms of alpha-synuclein, Aβ42 peptide and HTTExon 1. Acta Neuropathol 131(4):539–548
Mao X, Ou MT, Karuppagounder SS, Kam TI, Yin X, Xiong Y, Ge P, Umanah GE, Brahmachari S, Shin JH, Kang HC, Zhang J, Xu J, Chen R, Park H, Andrabi SA, Kang SU, Goncalves RA, Liang Y, Zhang S, Qi C, Lam S, Keiler JA, Tyson J, Kim D, Panicker N, Yun SP, Workman CJ, Vignali DA, Dawson VL, Ko HS, Dawson TM (2016) Pathological α-synuclein transmission initiated by binding lymphocyte-activation gene 3. Science 353(6307). doi:10.1126/science.aah3374
Biasini E, Turnbaugh JA, Unterberger U, Harris DA (2012) Prion protein at the crossroads of physiology and disease. Trends Neurosci 35(2):92–103
Kumar P, Segers-Nolten IM, Schilderink N, Subramaniam V, Huber M (2015) Parkinson’s protein alpha-synuclein binds efficiently and with a novel conformation to two natural membrane mimics. PLoS One 10(11):e0142795
Bellani S, Mescola A, Ronzitti G, Tsushima H, Tilve S, Canale C, Valtorta F, Chieregatti E (2014) GRP78 clustering at the cell surface of neurons transduces the action of exogenous alpha-synuclein. Cell Death Differ 21(12):1971–1983
Zabrocki P, Bastiaens I, Delay C, Bammens T, Ghillebert R, Pellens K, De Virgilio C, Van Leuven F et al (2008) Phosphorylation, lipid raft interaction and traffic of alpha-synuclein in a yeast model for Parkinson. Biochim Biophys Acta 1783(10):1767–1780
Younan ND, Sarell CJ, Davies P, Brown DR, Viles JH (2013) The cellular prion protein traps Alzheimer’s Aβ in an oligomeric form and disassembles amyloid fibers. FASEB J 27(5):1847–1858
Vilches S, Vergara C, Nicolas O, Mata A, Del Rio JA, Gavin R (2016) Domain-specific activation of death-associated intracellular signalling cascades by the cellular prion protein in neuroblastoma cells. Mol Neurobiol 53(7):4438–4448
Smith AD, Bolam JP (1990) The neural network of the basal ganglia as revealed by the study of synaptic connections of identified neurones. Trends Neurosci 13(7):259–265
Steele AD, Zhou Z, Jackson WS, Zhu C, Auluck P, Moskowitz MA, Chesselet MF, Lindquist S (2009) Context dependent neuroprotective properties of prion protein (PrP). Prion 3(4):240–249
McHattie SJ, Brown DR, Bird MM (1999) Cellular uptake of the prion protein fragment PrP106-126 in vitro. J Neurocytol 28(2):149–159
Kawahara M, Kuroda Y, Arispe N, Rojas E (2000) Alzheimer’s beta-amyloid, human islet amylin, and prion protein fragment evoke intracellular free calcium elevations by a common mechanism in a hypothalamic GnRH neuronal cell line. J Biol Chem 275(19):14077–14083
White AR, Maher F, Brazier MW, Jobling MF, Thyer J, Stewart LR, Thompson A, Gibson R et al (2003) Diverse fibrillar peptides directly bind the Alzheimer’s amyloid precursor protein and amyloid precursor-like protein 2 resulting in cellular accumulation. Brain Res 966(2):231–244
Zheng W, Wang L, Hong Y, Sha Y (2009) PrP106-126 peptide disrupts lipid membranes: influence of C-terminal amidation. Biochem Biophys Res Commun 379(2):298–303
Grey M, Linse S, Nilsson H, Brundin P, Sparr E (2011) Membrane interaction of alpha-synuclein in different aggregation states. J Parkinsons Dis 1(4):359–371
Jo E, McLaurin J, Yip CM, St George-Hyslop P, Fraser PE (2000) Alpha-synuclein membrane interactions and lipid specificity. J Biol Chem 275(44):34328–34334
Wood H (2016) Parkinson disease: LAG3 facilitates cell-to-cell spread of alpha-synuclein pathology. Nat Rev Neurol 2(12):678. doi:10.1038/nrneurol.2016.164
Maciejewski A, Ostapchenko VG, Beraldo FH, Prado VF, Prado MA, Choy WY (2016) Domains of STIP1 responsible for regulating PrPC-dependent amyloid-beta oligomer toxicity. Biochem J 473(14):2119–2130
Risse E, Nicoll AJ, Taylor WA, Wright D, Badoni M, Yang X, Farrow MA, Collinge J (2015) Identification of a compound that disrupts binding of amyloid-beta to the prion protein using a novel fluorescence-based assay. J Biol Chem 290(27):17020–17028
Nieznanski K, Choi JK, Chen S, Surewicz K, Surewicz WK (2012) Soluble prion protein inhibits amyloid-beta (Aβ) fibrillization and toxicity. J Biol Chem 287(40):33104–33108
Lauren J (2014) Cellular prion protein as a therapeutic target in Alzheimer’s disease. J Alzheimers Dis 38(2):227–244
Mata A, Urrea L, Vilches S, Llorens F, Thune K, Espinosa JC, Andreoletti O, Sevillano AM, Torres JM, Requena JR, Zerr I, Ferrer I, Gavin R, Del Rio JA (2016) Reelin expression in Creutzfeldt-Jakob disease and experimental models of transmissible spongiform encephalopathies. Mol Neurobiol. doi:10.1007/s12035-016-0177-8
Acknowledgements
The authors thank Tom Yohannan for the editorial advice and the IBEC Nanotechnology Platform staff for their generous help. This research was supported by grants from the Spanish Ministry of Economy and Competitiveness through the project (BFU2015-67777-R) (MINECO/FEDER), the Spanish prion network (Prionet Spain, AGL2015-71764-REDT) (MINECO/FEDER), the Generalitat de Catalunya (SGR2014-1218), CIBERNED (PI2014/02-4 (Rapid dementias), PRY-14-114 and PRY2016-02, La Caixa Obra Social Foundation and La Marató de TV3) to J.A.D.R. J.M.G.A. was supported by the European Research Council (ERC) through the project ERC-2012-StG 306751 and the MINECO (DPI2015-64221-C2-1-R). M.V. was supported by Fondo de Investigación Sanitaria-Instituto de Salud Carlos III. E.T. was supported by MINECO/FEDER (BIO2015-63557-R). I.F. was supported by the Seventh Framework Programme of the European Commission, grant agreement 278486: DEVELAGE and Instituto de Salud Carlos III–Fondos FEDER, a way to build Europe FIS PIE14/00034 and PI14/00757. J.S. was supported by the Seventh Framework Programme of the European Commission, grant agreement 228685-2: BOND and Instituto de Salud Carlos III (PI10/01171); MINECO/FEDER (TEC2015-72718-EXP) and the Botín Foundation. M.S.-F was supported by CIBERNED, A.H was supported by La Caixa Obra Social Foundation and L.U. was supported by a fellowship from the Marató TV3 foundation. L.P. is grateful to the Generalitat de Catalunya for its financial support through the FI Programme (2015-FI-B-00817).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interests.
Additional information
The original version of this article was revised: The name of author should be José Manuel García-Aznar (García-Aznar, JM) from José Manuel García Aznar (Aznar, JMG). Two affiliations “Department of Electronics, University of Barcelona, Martí i Franquès 1, E-08028 Barcelona, Spain” and “Centro de Investigación Biomédica en Red en Bioingeniería, Biomateriales y Nanomedicina (CIBER-BBN), 28029 Madrid, Spain” were also added for Josep Samitier.
An erratum to this article is available at https://doi.org/10.1007/s12035-017-0553-z.
Electronic Supplementary Material
Supplementary Fig. 1.
a-b Electron microscopy photomicrograph illustrating recombinant mouse α-synuclein fibers in aggregated stage (a) and after sonication procedure (b). c Western blot of sonicated α-synuclein fibers. Note the appearance of the ≈ 17 kDa band as well as the ≈ 35 kDa band typical of non-monomeric α-synuclein. Similar band pattern was observed in the case of human α-synuclein fibrils d-e Low power photomicrographs illustrating p-α-synuclein staining in sham-operated (d) and mouse α-synuclein-operated (e) Prnp +/+ mice. p129S/81A p-α-synuclein labelling can be seen in parietal and cingular neocortex, hippocampus, mamillothalamic tract, fornix, globus pallidus, caudate putamen and white matter. However, after injection, p-α-synuclein deposits as LBL or LNL aggregates (arrows in e) can clearly be seen over the background using the p129S/81A antibody. f-g High power photomicrographs illustrating p-α-synuclein LBL after mouse fibril injection in neocortex (f) or amygdala (g). Abbreviations: A, amygdala; CP, caudate putamen; EC, entorhinal cortex; GP, globus pallidus; H, hippocampus; T, thalamus. Scale bar: d = 500 μm pertains to e; f = 25 μm pertains to g. (JPEG 8544 kb)
Supplementary Fig. 2.
Analysis of mouse α-synuclein transport using microfluidic devices. a-b Examples of Fluo4-AM labelling (FITC optics) of microfluidic devices after 7 DIV. Note the difference in the number of labelled axons between (a) and (b) in the microchannels. c Example of western blotting of α-synuclein in a device without relevant interconnection reservoirs (a case). Two different exposures (10 seg and 4 min) are shown in the panel. Note the presence of a very pale band of α-synuclein in the B cell extract (asterisk) only detectable after 4 min of exposure. In these cultures, no endogenous α-synuclein labelling was observed, demonstrating detected α-synuclein in B derived from interneuronal transport of exogenous α-synuclein protofibrils as also demonstrated in α-synuclein (Fig. 4a-d) p-α-synuclein staining (Fig. 3e-h, Supplementary Fig. 3). Anti-β-tubulin was used for protein characterization. Scale bar: a = 400 μm pertains to b. (JPEG 3042 kb)
Supplementary Fig. 3.
Analysis of human α-synuclein fibril transport using microfluidic devices. a 2D representation of the two PDMS devices used in the present study. b-g Primary cortical cultures of Prnp +/+ were maintained in the devices for 5-7 days. Then human recombinant α-synuclein was added to A reservoir (asterisk) (b,d,f), neuronal presence of p-α-synuclein in A was analysed (c), and their transport to B reservoir was analysed with p-α-synuclein immunocytochemistry (d-g). b-c Examples of double-labelled neurons (TUJ1/p-α-synuclein) in A reservoir (indicated with camera icon) showing p-α-synuclein labelling as LBL (arrows in b and c). d-g Examples of p-α-synuclein-labelled neurons and axons (TUJ1-positive, arrows) in B reservoir (indicated with camera icon). Scale bar: b and f = 40 μm pertains to c-e and g, respectively. (JPEG 8502 kb)
Supplementary Fig. 4.
Overexposed (15 min) uncropped films showing the absence of α–synuclein in cultured media of B in contrast to A reservoir, indicating the absence of fluidic flux between reservoirs illustrated in Fig. 3i. (JPEG 2392 kb)
Supplementary Fig. 5.
a Western blot illustrating the overexpression of the different PrPC constructs (ΔF35, ΔHR, ΔCC, and PrPC) in HEK293 cells. The cellular distribution of the constructs in the plasma membrane can be seen in [54] b Histogram illustrating the activation of caspase 3 by the different PrPC constructs (including ΔCD and ΔCR constructs). Data represent the mean ± S.E.M. of three different experiments. *** P < 0.01, ANOVA Bonferroni post hoc test. (JPEG 1479 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Urrea, L., Segura-Feliu, M., Masuda-Suzukake, M. et al. Involvement of Cellular Prion Protein in α-Synuclein Transport in Neurons. Mol Neurobiol 55, 1847–1860 (2018). https://doi.org/10.1007/s12035-017-0451-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-017-0451-4