Abstract
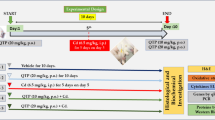
Cranial irradiation-induced inflammation plays a critical role in the initiation and progression of radiation-induced brain injury (RIBI). Anti-inflammation treatment may provide therapeutic benefits. Corilagin (beta-1-O-galloyl-3, 6-(R)-hexahydroxydiphenoyl-D-glucose, C27H22O18) was a novel member of the tannin family with anti-inflammatory properties and is isolated from some medicinal plants, such as Phyllanthus amarus and Caesalpinia coriaria. In this study, the effect of Corilagin on RIBI was investigated and the underlying mechanisms were explored. Spatial learning and memory ability of mice were investigated by the Morris water maze test. Evans blue leakage and electron microscopy were used to assess the integrity of blood-brain barrier (BBB). The mRNA and protein expressions of inflammatory cytokines, TNF-α and IL-1β, were measured by using real-time PCR and Western blotting. The activation of microglial cells and expression of TNF-α were examined by immunofluorescence staining. Phosphorylated signal transducers and activators of transcription 3 (p-STAT3) and IκBα, and the translocation of p65 from cytoplasm to nucleus were detected by using Western blotting. Morris water maze test showed that Corilagin ameliorated the neurocognitive deficits in RIBI mice. Evans blue leakage and electron microscopy exhibited that Corilagin partially protected the BBB integrity from cranial irradiation-caused damage; immunofluorescence staining showed that Corilagin could inhibit microglial activation and TNF-α expression. Real-time PCR and Western blotting revealed that Corilagin downregulated the expression of TNF-α and IL-1β and inhibited the irradiation-induced activation of NF-κB pathways by upregulating p-STAT3 expression. In conclusion, Corilagin could attenuate RIBI through inhibiting microglial activation and the expressions of inflammatory cytokines. Corilagin might inhibit the activation of NF-κB pathway in a STAT3-associated manner, thereby downregulating the inflammatory cytokine expressions.











Similar content being viewed by others
References
Khuntia D, Brown P, Li J, Mehta MP (2006) Whole-brain radiotherapy in the management of brain metastasis. J ClinOncol 24(8):1295–1304
Johannesen TB, Langmark F, Lote K (2003) Cause of death and long-term survival in patients with neuro-epithelial brain tumours: a population-based study. Eur J Cancer 39(16):2355–2363
Cole AM, Scherwath A, Ernst G, Lanfermann H, Bremer M, Steinmann D (2013) Self-reported cognitive outcomes in patients with brain metastases before and after radiation therapy. Int J Radiat Oncol Biol Phys 87(4):705–712
Beltran C, Naik M, Merchant TE (2010) Dosimetric effect of target expansion and setup uncertainty during radiation therapy in pediatric craniopharyngioma. Radiother Oncol 97(3):399–403
Li J, Bentzen SM, Li J, Renschler M, Mehta MP (2008) Relationship between neurocognitive function and quality of life after whole-brain radiotherapy in patients with brain metastasis. Int J Radiat Oncol Biol Phys 71(1):64–70
Schnegg CI, Kooshki M, Hsu FC, Sui G, Robbins ME (2012) PPARδ prevents radiation-induced proinflammatory responses in microglia via transrepression of NF-kappaB and inhibition of the PKCα/MEK1/2/ERK1/2/AP-1 pathway. Free RadicBiol Med 52(9):1734–1743
Liu JL, Tian DS, Li ZW, Qu WS, Zhan Y, Xie MJ, Yu ZY, Wang W et al (2010) Tamoxifen alleviates irradiation-induced brain injury by attenuating microglial inflammatory response in vitro and in vivo. Brain Res 1316:101–111
Zhao W, Robbins ME (2009) Inflammation and chronic oxidative stress in radiation-induced late normal tissue injury: therapeutic implications. Curr Med Chem 16(2):130–143
Dong X, Luo M, Huang G, Zhang J, Tong F, Cheng Y, Cai Q, Dong J et al (2015) Relationship between irradiation-induced neuro-inflammatory environments and impaired cognitive function in the developing brain of mice. Int J Radiat Biol 91(3):224–239
Stoll G, Jander S (1999) The role of microglia and macrophages in the pathophysiology of the CNS. Prog Neurobiol 58(3):233–247
Gebicke-Haerter PJ (2001) Microglia in neurodegeneration: molecular aspects. Microsc Res Tech 54(1):47–58
Pocock JM, Liddle AC (2001) Microglial signalling cascades in neurodegenerative disease. Prog Brain Res 132:555–565
Luo XG, Chen SD (2012) The changing phenotype of microglia from homeostasis to disease. Transl Neurodegener 1(1):9
Xue J, Dong JH, Huang GD, Qu XF, Wu G, Dong XR (2014) NF-κB signaling modulates radiation-induced microglial activation. Oncol Rep 31(6):2555–60
Kyrkanides S, Moore AH, Olschowka JA, Daeschner JC, Williams JP, Hansen JT, Kerry OM (2002) Cyclooxygenase-2 modulates brain inflammation-related gene expression in central nervous system radiation injury. Brain Res Mol Brain Res 104(2):159–169
Hutchins AP, Poulain S, Miranda-Saavedra D (2012) Genome-wide analysis of STAT3 binding in vivo predicts effectors of the anti-inflammatory response in macrophages. Blood 119(13):e110–9
Zhang ZH, Yu LJ, Hui XC, Wu ZZ, Yin KL, Yang H, Xu Y (2014) Hydroxy-safflor yellow A attenuates Aβ1-42-induced inflammation by modulating the JAK2/STAT3/NF-KB pathway. Brain Res 1563:72–80
Shen ZQ, Dong ZJ, Peng H, Liu JK (2003) Modulation of PAI-1 and tPA activity and thrombolytic effects of corilagin. Planta Med 69(12):1109–1112
Duan W, Yu Y, Zhang L (2005) Antiatherogenic effects of phyllanthusemblica associated with corilagin and its analogue. YakugakuZasshi 125(7):587–591
Bharti S, Nidhi V, Juan PM (2014) Aparajita M (2014) An overview of important ethnomedicinal herbs of Phyllanthus species: present status and future prospects. Sci World J 2014:839172
Shibuya H, Kitagawa I (1996) Chemical study of Indonesian medicinal plants. J Pharm Soc Jpn 116(12):911–27
Kinoshita S, Inoue Y, Nakama S, Ichiba T, Aniya Y (2007) Antioxidant and hepatoprotective actions of medicinal herb Terminalia catappa L. from Okinawa Island and its tannin corilagin. Phytomedicine 14(11):755–762
Cheng JT, Lin TC, Hsu FL (1995) Antihypertensive effect of corilagin in the rat. Can J Physiol Pharmacol 73(10):1425–1429
Guo YJ, Luo T, Wu F, Liu H, Li HR, Mei YW, Zhang SL, Tao JY et al (2014) Corilagin protects against HSV1 encephalitis through inhibiting the TLR2 signaling pathways in vivo and in vitro. Mol Neurobiol. doi:10.1007/s12035-014-8947-7
Dong XR, Luo M, Fan L, Zhang T, Liu L, Dong JH, Wu G (2010) Corilagin inhibits the double strand break-triggered NF-kappaB pathway in irradiated microglial cells. Int J Mol Med 25(4):531–536
Schindler MK, Forbes ME, Robbins ME, Riddle DR (2008) Aging-dependent changes in the radiation response of the adult rat brain. Int J Radiat Oncol Biol Phys 70(3):826–834
Zhu L, Zhang L, Zhan L, Lu X, Peng J, Liang L, Liu Y, Zheng L et al (2014) The effects of Zibu Piyin Recipe components on scopolamine-induced learning and memory impairment in the mouse. J Ethnopharmacol 151(1):576–582
Cevik NG, Orhan N, Yilmaz CU, Arican N, Ahishali B, Kucuk M, Kaya M, Toklu AS (2013) The effects of hyperbaric air and hyperbaric oxygen on blood–brain barrier integrity in rats. Brain Res 1531:113–121
Overbergh L, Giulietti A, Valckx D, Decallonne R, Bouillon R, Mathieu C (2003) The use of real-time reverse transcriptase PCR for the quantification of cytokine gene expression. J Biomol Tech 14(1):33–43
Ivanov VN, Hei TK (2014) A role for TRAIL/TRAIL-R2 in radiation-induced apoptosis and radiation-induced bystander response of human neural stem cells. Apoptosis 19(3):399–413
Austyn JM, Gordon S (1981) F4/80, a monoclonal antibody directed specifically against the mouse macrophage. Eur J Immunol 11(10):805–15
Stone HB, Moulder JE, Coleman CN, Ang KK, Anscher MS, Barcellos-Hoff MH, Dynan WS, Fike JR et al (2004) Models for evaluating agents intended for the prophylaxis, mitigation and treatment of radiation injuries. Report of an NCI Workshop, December 3–4, 2003. Radiat Res 162(6):711–728
Moulder JE, Cohen EP (2007) Future strategies for mitigation and treatment of chronic radiation-induced normal tissue injury. Semin Radiat Oncol 17(2):141–8
Warrington JP, Csiszar A, Mitschelen M, Lee YW, Sonntag WE (2012) Whole brain radiation-induced impairments in learning and memory are time-sensitive and reversible by systemic hypoxia. PLoS One 7(1), e30444
Acharya MM, Christie LA, Lan ML, Donovan PJ, Cotman CW, Fike JR, Limoli CL (2009) Rescue of radiation-induced cognitive impairment through cranial transplantation of human embryonic stem cells. Proc Natl AcadSci USA 106(45):19150–19155
Diserbo M, Agin A, Lamproglou I, Mauris J, Staali F, Multon E, Amourette C (2002) Blood–brain barrier permeability after gamma whole-body irradiation: an in vivo microdialysis study. Can J Physiol Pharmacol 80(7):670–678
Nordal RA, Wong CS (2005) Molecular targets in radiation-induced blood–brain barrier disruption. Int J Radiat Oncol Biol Phys 62(1):279–287
Hong JH, Chiang CS, Campbell IL, Sun JR, Withers HR, McBride WH (1995) Induction of acute phase gene expression by brain irradiation. Int J Radiat Oncol. Biol Phys 33(3):619–626
Gaber MW, Sabek OM, Fukatsu K, Wilcox HG, Kiani MF, Merchant TE (2003) Differences in ICAM-1 and TNF-alpha expression between large single fraction and fractionated irradiation in mouse brain. Int J Radiat Biol 79(5):359–366
Lee WH, Sonntag WE, Mitschelen M, Yan H, Lee YW (2010) Irradiation induces regionally specific alterations in pro-inflammatory environments in rat brain. Int J Radiat Biol 86(2):132–144
Conner KR, Forbes ME, Lee WH, Lee YW, Riddle DR (2011) AT1 receptor antagonism does not influence early radiation-induced changes in microglial activation or neurogenesis in the normal rat brain. Radiat Res 176(1):71–83
Zhang J, Tong F, Cai Q, Chen L-j, Dong J-h, Wu G, Dong X-r (2015) Shenqi Fuzheng Injection attenuates irradiationinduced brain injury in mice via inhibition of the NF-κB signaling pathway and microglial activation. Acta Pharmacol Sin 36:1288–1299
Ross PJ, Ashley S, Norton A, Priest K, Waters JS, Eisen T, Smith IE, O’Brien MER (2004) Do patients with weight loss have a worse outcome when undergoing chemotherapy for lung cancers? Br J Cancer 90:1905–11
Langius JAE, Bakker S, Rietveld DHF, Kruizenga HM, Langendijk JA, Weijs PJM, Leemans CR (2013) Critical weight loss is a major prognostic indicator for disease-specific survival in patients with head and neck cancer receiving radiotherapy. Br J Cancer 109:1093–1099
Rola R, Raber J, Rizk A, Otsuka S, VandenBerg SR, Morhardt DR, Fike JR (2004) Radiation-induced impairment of hippocampal neurogenesis is associated with cognitive deficits in young mice. Exp Neurol 188(2):316–330
Baker DG, Krochak RJ (1989) The response of the microvascular system to radiation: a review. Cancer Invest 7(3):287–294
Rubin P, Gash DM, Hansen JT, Nelson DF, Williams JP (1994) Disruption of the blood–brain barrier as the primary effect of CNS irradiation. Radiother Oncol 31(1):51–60
Barichello T, Lemos JC, Generoso JS, Cipriano AL, Milioli GL, Marcelino DM, Vuolo F, Petronilho F et al (2011) Oxidative stress, cytokine/chemokine and disruption of blood–brain barrier in neonate rats after meningitis by Streptococcus agalactiae. Neurochem Res 36(10):1922–30
Takata F, Dohgu S, Matsumoto J, Takahashi H, Machida T, Wakigawa T, Harada E, Miyaji H et al (2011) Brain pericytes among cells constituting the blood–brain barrier are highly sensitive to tumor necrosis factor-α, releasing matrix metalloproteinase-9 and migrating in vitro. J Neuroinflammation 8:106
Liu T, Zhang T, Yu H, Shen H, Xia W (2014) Adjudin protects against cerebral ischemia reperfusion injury by inhibition of neuroinflammation and blood–brain barrier disruption. J Neuroinflammation 11:107
Li L, McBride DW, Doycheva D, Dixon BJ, Krafft PR, Zhang JH, Tang J (2015) G-CSF attenuates neuroinflammation and stabilizes the blood–brain barrier via the PI3K/Akt/GSK-3β signaling pathway following neonatal hypoxia-ischemia in rats. Exp Neurol pii: S0014–4886(15):00005–9
Lee YW, Hennig B, Toborek M (2003) Redox-regulated mechanisms of IL-4-induced MCP-1 expression in human vascular endothelial cells. Am J Physiol Heart Circ Physiol 284(1):H185–92
Greene-Schloesser D, Robbins ME (2012) Radiation-induced cognitive impairment from bench to bedside. Neuro Oncol 14(4):iv37–44
Rübe CE, Wilfert F, Palm J, König J, Burdak-Rothkamm S, Liu L, Schuck A, Willich N et al (2004) Irradiation induces a biphasic expression of pro-inflammatory cytokines in the lung. Strahlenther Onkol 180(7):442–8
Ardestani S, Deskins DL, Young PP (2013) Membrane TNF-alpha-activated programmed necrosis is mediated by Ceramide-induced reactive oxygen species. J Mol Signal 8(1):12–12
Rübe CE, Wilfert F, Uthe D, Schmid KW, Knoop R, Willich N, Schuck A, Rübe C (2001) Modulation of radiation-induced tumor necrosis factor (TNF-α) expression in the lung tissue by pentoxifylline. Radiother Oncol 64:177–87
Welte T, Zhang SS, Wang T, Zhang Z, Hesslein DG, Yin Z, Kano A, Iwamoto Y et al (2003) STAT3 deletion during hematopoiesis causes Crohn’s disease-like pathogenesis and lethality: a critical role of STAT3 in innate immunity. Proc Natl Acad Sci U S A 100(4):1879–1884
Gautron L, De Smedt-Peyrusse V, Layé S (2006) Characterization of STAT3-expressing cells in the postnatal rat brain. Brain Res 1098(1):26–32
Smith AM, Qualls JE, O’Brien K, Balouzian L, Johnson PF, Schultz-Cherry S, Smale ST, Murray PJ (2011) A distal enhancer in Il12b is the target of transcriptional repression by the STAT3 pathway and requires the basic leucine zipper (B-ZIP) protein NFIL3. J Biol Chem 286(26):23582–23590
Mandal P, Park PH, McMullen MR, Pratt BT, Nagy LE (2010) The anti-inflammatory effects of adiponectin are mediated via a heme oxygenase-1-dependent pathway in rat Kupffer cells. Hepatology 51(4):1420–1429
Yu Z, Zhang W, Kone BC (2002) Signal transducers and activators of transcription 3 (STAT3) inhibits transcription of the inducible nitric oxide synthase gene by interacting with nuclear factor kappaB. Biochem J 367(Pt 1):97–105
Fu XY (2006) STAT3 in immune responses and inflammatory bowel diseases. Cell Res 6(2):214–219
Chiba T, Yamada M, Sasabe J, Terashita K, Shimoda M, Matsuoka M, Aiso S (2009) Amyloid-beta causes memory impairment by disturbing the JAK2/STAT3 axis in hippocampal neurons. Mol Psychiatry 14(2):206–222
Acknowledgments
This study is sponsored by the National Nature Science Foundation of China (nos. 81172595 and 81573090), Post-doctoral Program foundation of China (no. 20100480905), and a grant from the Foundation of Special Post-doctoral Program of China (201104440).
Conflict of Interest
No potential conflicts of interest were disclosed.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Fan Tong and Jian Zhang are considered co-first authors.
Fan Tong and Jian Zhang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Tong, F., Zhang, J., Liu, L. et al. Corilagin Attenuates Radiation-Induced Brain Injury in Mice. Mol Neurobiol 53, 6982–6996 (2016). https://doi.org/10.1007/s12035-015-9591-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-015-9591-6