Abstract
Purpose
Plexin C1 is a transmembrane receptor and plexin C1 overexpression might have role in carcinogenesis. Hepatocellular carcinoma (HCC) has poor prognosis because of its aggressive behavior and limited treatment options, especially in advanced stage. We recently documented that Plexin C1 was overexpressed in HCC. We aimed to evaluate the prognostic significance of Plexin C1 overexpression in HCC in the present study.
Methods
Plexin C1 overexpression was evaluated immunohistochemically on paraffin-embedded blocks of the HCC patients. Plexin C1 immunohistochemical staining was scored. Plexin C1 overexpression staining intensity and prevalence were used for plexin scale staining evaluation and plexin scores were estimated according this staining scale. Plexin C1 score and its association with survival and clinicopathological features was assessed.
Results
Sixty-seven HCC patients with adequate tissue for pathological evaluation were included. Median age was 63 years with male predominance (male to female ratio was 4.75 (n 57/12). Well-differentiated HCC (53.7%) patients had higher plexin C1 overexpression (p < 0.05). Median OS was 22.1 months. Patients with lower plexin C1 score (< 12) had shorter OS (17.5 vs 30.1 months, p = 0.036). Neutrophil count, GGT, and PNR (platelet/neutrophil ratio) had prognostic significance (p = 0.047, p = 0.018, and p = 0.045).
Conclusion
Plexin C1 overexpression is inversely correlated with grade in HCC. The patients with lower rate of Plexin C1 overexpression have worse survival outcome. It might be a prognostic factor in HCC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hepatocellular carcinoma (HCC) is high among the leading causes of cancer deaths [1]. Viral hepatitis (hepatitis B and C), alcoholic liver disease, chronic liver injury, and aflatoxin are well-known risk factors for HCC. Surgery and orthotopic liver transplantation are main treatment options for early-stage HCC [2]. Locoregional therapeutic interventions (i.e., chemoembolization) are other options for selected patients in locally advanced disease setting. Hepatocellular carcinoma has poor prognosis with a 5-year overall survival less than 20% in advanced stage [3]. It is an angiogenic tumor; therefore, tumor proliferation and angiogenesis are targeted in advanced stage HCC. Multikinase inhibitors such as sorafenib, regorafenib, cabozantinib, and lenvatinib have been shown to have efficacy in advanced stage HCC [4,5,6]. However, it is still incurable even with targeted therapies in advanced disease. So, clinical trials with agents focusing on novel targets are needed in this area.
Plexins (Plexin A1-4, B1-3, C1, and D1) are transmembrane receptors which are involved in cell adhesion and induction of intracellular signaling for tumor growth and axonal orientation [2, 7, 8]. Additionally, they have critical roles in organogenesis [2]. Plexin A and B predominantly bind to semaphorinsleading to promotion of astrocytic cell differentiation [7, 8]. Semaphorins might also contribute to angiogenesis and regulation of immune response [9]. Furthermore, plexins were also reported to have critical roles in other solid tumors besides gliomas [2, 10, 11]. Plexin B1 is the receptor for semaphorin 4D (Sema 4D) [12]. Loss or activation of plexin-B1 were reported to have prognostic significance in solid tumors, such as hormone receptor positive breast cancer or prostate cancer [10, 11]. The receptor for soluble viral semaphorin A39R originating from Vaccinia virus is plexin C1 (“Virus Encoded Semaphorin Protein receptor” (VESPR)) [13]. GPI-anchored semaphorin 7A (Sema 7A) is a human ligand for plexin C1 [2]. Plexin C1 has role in stimulation of monocyte cytokine production13. In addition, plexin C1 might have tumor suppressor effect in melanoma [14].
So, plexin C1 seems to differ from other plexin subtypes, in terms of molecular functional characteristics rather than axonal guidance. Recently, we documented the expression pattern of plexin C1 in liver and its overexpression in HCC [2].
In present study, we aimed to evaluate the diagnostic and prognostic significance of plexin C1 in HCC and its correlation with clinicopathological features.
Methods
Patients
The patients with advanced stage HCC were evaluated for their clinicopathological features and plexin C1 overexpression. This study included the patients that was diagnosed between 2010 and 2015 in eight cancer centers. Patient demographic characteristics and laboratory results (i.e., complete blood count, biochemical analysis) at diagnosis were recorded from hospital central database. Hematological ratios such as NLR (neutrophil-lymphocyte ratio) and PNR (platelet-neutrophil ratio) were calculated.
Immunohistochemistry
Formalin (%10) fixed and paraffin-embedded tissue sections (4 µm thick) were taken on positively charged slides and were held in EDTA buffer solution (pH 8.0) for antigen retrieval within an automatic immunohistochemistry staining device (Ventana, Benchmark GX) for 1 h. Then, slides were stained with primary antibody against Plexin (dilution 1/50) which is obtained from Gebze Technical University, Kocaeli for 32 min. Primary antibody binding was detected and visualized with Ultraview universal diaminobenzidine (DAB) detection kit. Staining was completed after counterstaining with haematoxylin (Ventana). After rinsing out under running tab water, slides were held in ethyl alcohol and in xylol, each for 2 min long. Then, slides were covered via entellan and immunohistochemical evaluation was made under light microscope (Olympus, BX43, Japan) by a pathologist closely interested in hepatopathology.
We evaluated plexin C1 overexpression on liver tissue in HCC, viral hepatitis B without any fibrosis, viral hepatitis B and C with advanced fibrosis, steatohepatitis, and liver tissue with normal structure. Immunohistochemical staining results of plexin were scored and evaluated by using two separate scaling methods (Table 1). Total staining score was calculated by multipling staining intensity and staining prevalance of the tumor cells. More detailed scaling method (scale 2) is used for statistical analysis.
Statistical Analysis
Overall survival (OS) analysis was performed by using the Kaplan–Meier method, and statistical significance for OS was determined with log-rank test. The association between dichotomized factors (below vs. above the median value or upper limit of normal, ULN) was evaluated by chi-square test. Neutrophil-to-lymphocyte ratio (NLR) and platelet-to-lymphocyte ratio (PLR) calculations were based on a cutoff value derived from a receiver operating characteristic (ROC) curve analysis by using as classifier long versus short OS (> 22.1 vs. < 22.1 months, respectively). If we now the upper or lower limits of the laboratory tests, we used the values for dichotomizing. Although we know the limits of laboratory tests, we tried to test whether there are different cutoff values which show us a prediction for our cases. Many parameters were tested based on median, mean or ROC curve analysis to find new predictive cutoff values.
Results
Sixty-nine advanced stage HCC patients followed-up at 8 experienced cancer centers were evaluated; however, two patients were excluded because of inadequate tissue for immunohistochemical analysis on paraffin-embedded tissue samples. A total of 67 patients were included to this study for immunohistochemical evaluation. However, plexin C1 overexpression and scales could have been definitely evaluated in 46 patients because of technical issues. Thirty-four patients had both tumor and non-tumoral adjacent liver tissue on paraffin blocks while others had only tumor tissue on paraffin blocks. The clinicopathological characteristics and survival outcomes of the patients are summarized in Table 2. Male-to-female ratio was 4.75 with a median age of 63 (range = 40–89) years. Sixty-one percent (n = 42) had hepatitis B virus infection as a risk factor for HCC.
Tumor grade could have been definitely documented in 54 patients because of technical details. Twenty-nine (53.7%) patients had well-differentiated HCC whereas 19 (35.2%) had moderately differentiated HCC and 6 (11.1%) had poorly differentiated HCC. The patients with well-differentiated HCC had higher rate of plexin C1 overexpression. There was no association between plexin C1 overexpression and any clinical parameter. However, “grade” as a pathological feature was shown to correlate with plexin C1 overexpression. High grade (“poorly differentiated”) tumors had weak plexin C1 staining (55% vs 66.1%, p < 0.05). Interestingly, plexin C1 was also overexpressed in non-tumor adjacent liver tissue of HCC patients. Its overexpression was irrespective of tumor tissue. Tumor and background liver tissue plexin C1 scales according to tumor differentiation are shown in Table 3.
Median OS was 22.1 months for all patients. In this study, we found that plexin C1 score had an effect on overall survival. The patients with low plexin score (score < 12) had significantly shorter overall survival in comparison to the patients with plexin score of 12 (17.5 vs 30.1 months, p = 0.036) (Fig. 1). In addition, neutrophil count, GGT, and PNR were shown to have prognostic significance in univariate analysis (p = 0.047, p = 0.018, and p = 0.045, respectively). There was no association between survival and any other clinical features.
Discussion
This is the first study in the literature which showed that plexin C1 score had an effect on overall survival. Plexin C1 was overexpressed in well-differentiated HCC and non-tumor adjacent tissue of advanced stage HCC in our study. Additionally, plexin C1 is strongly stained in normal liver tissue without any fibrosis while it has incomplete weak staining in both steatohepatitis and advanced fibrosis2. Taking all of these points into account, we consider that the structural distortion in the liver might have led plexin C1 overexpression.
Plexin C1 overexpression was evaluated on liver tissue in HCC, viral hepatitis B without any fibrosis, viral hepatitis B and C with advanced fibrosis, steatohepatitis, and liver tissue with normal structure. However, all of these subgroups had smaller sample size. As expected, there was strong completely membranous plexin C1 staining in viral hepatitis without any fibrosis and normal liver tissue. Membranous staining was partially incomplete and weak in steatohepatitis whereas it was weak to intermediate, prominently incomplete in viral hepatitis with advanced fibrosis. Well-differentiated HCC tumor tissue had incompletely weak membranous staining; however, membranous staining was incomplete to intermediate complete on advanced fibrotic liver tissue that led to tumor grow up. So, we documented plexin C1 normal staining pattern (i.e., strong complete membranous staining) in both normal liver tissue and minimal chronic viral hepatitis without any fibrosis. We determined that membranous staining was weak and incomplete in liver tissue with prominent steatohepatitis and/or fibrosis. Interestingly, there was no membranous staining or partially incomplete weak staining in HCC liver tissue.
This study has some limitations. The plexin expression was not performed in all patients due to small biopsy materials. But, we analyzed plexin score in all available liver tumor tissue samples. There were some missing data in the study group. We evaluated the relationship between and plexin C1 overexpression and clinicopathological parameters.
Grade was inversely correlated with plexin C1 expression, in parallel to our previous study [2]. Poorly differentiated tumors have higher grade. It is a well-known process that HCC is a hypervascularized neoplasm, and angiogenesis is more prominent in poorly differentiated HCC. Antiangiogenic agents including multikinase inhibitors are cornerstones of the treatment of advanced stage HCC. In our study, we showed that poorly differentiated/high-grade HCC had lower plexin 1 expression. So, plexin C1 might be used as a predictive marker for these antiangiogenic agents. We consider that it should be supported by randomized clinical trials with larger number of patients.
References
Global Burden of Disease Liver Cancer Collaboration, Akinyemiju T, Abera S, Ahmed M, Alam N, Alemayohu MA, Allen C, et al. The burden of primary liver cancer and underlying etiologies from 1990 to 2015 at the global, regional, and national level: results from the Global Burden of Disease Study 2015. JAMA Oncol. 2017;3:1683–1691.
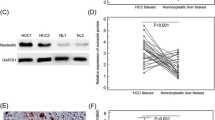
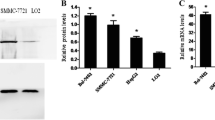
Odabas G, Cetin M, Turhal S, Baloglu H, Sayan AE, Yagci T. Plexin C1 marks liver cancer cells with epithelial phenotype and Is overexpressed in hepatocellular carcinoma. Can J Gastroenterol Hepatol (2018). 18 Sep19; 2018:4040787. https://doi.org/10.1155/2018/4040787. eCollection 2018
Chan SL, Wong AM, Lee K, Wong N, Chan AKC. Personalized therapy for hepatocellular carcinoma: where are we now? Cancer Treat Rev. 2016;45:77–86.
Kudo M, Finn RS, Qin S, Han KH, Ikeda K, Piscaglia F, et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: a randomised phase 3 non-inferiority trial. Lancet. 2018;391:1163–73.
Heo YA, Syed YY. Regorafenib: a review in hepatocellular carcinoma. Drugs. 2018;78:951–8.
Abou-Alfa GK, Meyer T, Cheng AL, El-Khoueiry AB, Rimassa L, Ryoo BY, et al. Cabozantinib in patients with advanced and progressing hepatocellular carcinoma. N Engl J Med. 2018;379:54–63.
Yu L, Zhou Y, Cheng S, Rao Y. Plexin a-semaphorin-1 are verse signaling regulates photoreceptor axon guidance in Drosophila. J Neurosci. 2010;30:12151–6.
Angelopoulou E, Piperi C. Emerging role of plexins signaling in glioma progression and therapy. Cancer Lett. 2018;414:81–7.
Neufeld G, Sabag AD, Rabinovicz N, Kessler O. Semaphorins in angiogenesis and tumor progression (2012). Cold Spring Harb Perspect Med 2: a006718.
Rody A, Karn T, Ruckhaberle E, Hanker L, Metzler D, Muller V, et al. Loss of Plexin B1 is highly prognostic in low proliferating ER positive breast cancers- results of a large scale microarray analysis. Eur J Cancer. 2009;45:405–13.
Wong OG, Nitkunan T, Oinuma I, Zhou C, Blanc V, Brown RS, et al. Plexin-B1 mutations in prostate cancer. Proc Natl Acad Sci USA. 2007;104:19040–5.
Stevens L, McClelland L, Fricke A, Williamson M, Kuo I, Scott G. Plexin B1 suppresses c-Met in melanoma: a role for plexin B1 as a tumor-suppressor protein through regulation of c-Met. J Invest Dermatol. 2010;130:1636–45.
M. R. Comeau, R. Johnson, R. F. DuBose, Petersen M, Gearing P, VandenBos T, Park L, et al. A pox virüs encoded semaphorin induces cytokine production from monocytes and binds to a novel cellular semaphorin receptor, VESPR. Immunity 1998;8:473–482.
Scott GA, McClelland LA, Fricke AF, Fender A. Plexin C1, a receptor for semaphorin7a, inactivates coflin and is a potential tumor suppressor for melanoma progression. J Investig Dermatol. 2009;129:954–63.
Author information
Authors and Affiliations
Contributions
Manuscript writing and editing: SNT, MD, MA. Pathological and immunhistochemical evaluation: GE, GA, TY. Statistical analysis: LK. All of the authors contributed to the other steps of manuscript including data collection.
Corresponding author
Ethics declarations
Ethics Approval
Our study had ethics approval from Marmara University Ethics Committee (protocol code: 9.2015.081/70,737,436–050.06.04, approval date: 08.05.2015).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
NazimTurhal, S., Dogan, M., Esendagli, G. et al. The Relationship Between Plexin C1 Overexpression and Survival in Hepatocellular Carcinoma: a Turkish Oncology Group (TOG) Study. J Gastrointest Canc 53, 356–362 (2022). https://doi.org/10.1007/s12029-021-00602-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-021-00602-4