Abstract
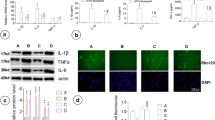
To explore the effect of dexmedetomidine (DEX) post-treatment on the inflammatory response of astrocyte induced by lipopolysaccharide (LPS). The astrocytes of neonatal mice were primarily cultured in vitro. After purification and identification, the cells were divided into five groups: group C: control group; group L: astrocytes were treated with 1 μg/ml LPS for 24 h; group D1, D2, and D3: astrocytes were pretreated with 1 μg/ml for 24 h LPS, and then cultured with low (0.1 μM), medium (1 μM), high (10 μM) concentration of DEX for 30 min, respectively. The cell survival rate was detected by cell counting kit. The expressions of inducible nitric oxide synthase (iNOS) mRNA, tumor necrosis gactor-α (TNF-α) mRNA, and interleukin-1β (IL-1β) mRNA were measured by RT-PCR in cell lysis solution of every group. The concentration of nitric oxide (NO) was detected by Griess method. The concentrations of IL-1β and TNF-α were measured, respectively, by enzyme-linked immuno sorbent assay. Compared with the group C, the expressions of iNOS mRNA, TNF-α mRNA, and IL-1βm RNA were significantly up-regulated, the release of NO, TNF-α, and IL-1β was significantly increased in group L (P < 0.05). Compared with group L, mRNA levels of inflammation-related factors and release of inflammatory factors were significantly down-regulated in group D2 and D3 (P < 0.05). There was no statistical difference between group D1 and group L. Pre-treatment with medium and high concentration of DEX can inhibit the LPS-induced inflammatory response of astrocyte.



Similar content being viewed by others
References
Choi, J. W., Gardell, S. E., Herr, D. R., et al. (2011). FTY720 (fingolimod) efficacy in an animal model of multiple sclerosis requires astrocyte sphingosine 1-phosphate receptor 1 (S1P1) modulation. Proceedings of the National Academy of Sciences, 108(2), 751–756.
Allen, N. J., Bennett, M. L., Foo, L. C., et al. (2012). Astrocyte glypicans 4 and 6 promote formation of excitatory synapses via GluA1 AMPA receptors. Nature, 486(7403), 410–414.
De Pablo, Y., Nilsson, M., Pekna, M., et al. (2013). Intermediate filaments are important for astrocyte response to oxidative stress induced by oxygen-glucose deprivation and reperfusion. Histochemistry and Cell Biology, 140(1), 81–91.
Fulmer, C. G., VonDran, M. W., Stillman, A. A., et al. (2014). Astrocyte-derived BDNF supports myelin protein synthesis after Cuprizone-induced demyelination. The Journal of Neuroscience, 34(24), 8186–8196.
Abbott, N. J., Rönnbäck, L., & Hansson, E. (2006). Astrocyte-endothelial interactions at the blood-brain barrier. Nature Reviews Neuroscience, 7(1), 41–53.
Haydon, P. G., & Carmignoto, G. (2006). Astrocyte control of synaptic transmission and neurovascular coupling. Physiological Reviews, 86(3), 1009–1031.
Seifert, G., Schilling, K., & Steinhäuser, C. (2006). Astrocyte dysfunction in neurological disorders: A molecular perspective. Nature Reviews Neuroscience, 7(3), 194–206.
Tan, J. A., & Ho, K. M. (2010). Use of dexmedetomidine as a sedative and analgesic agent in critically ill adult patients: A meta-analysis. Intensive Care Medicine, 36(6), 926–939.
Riker, R. R., Shehabi, Y., Bokesch, P. M., et al. (2009). Dexmedetomidine vs midazolam for sedation of critically ill patients: A randomized trial. JAMA, 301(5), 489–499.
Pandharipande, P. P., Pun, B. T., Herr, D. L., et al. (2007). Effect of sedation with dexmedetomidine vs lorazepam on acute brain dysfunction in mechanically ventilated patients: The MENDS randomized controlled trial. JAMA, 298(22), 2644–2653.
Yildiz, M., Tavlan, A., Tuncer, S., et al. (2006). Effect of dexmedetomidine on haemodynamic responses to laryngoscopy and intubation. Drugs in R & D, 7(1), 43–52.
Jakob, S. M., Ruokonen, E., Grounds, R. M., et al. (2012). Dexmedetomidine vs midazolam or propofol for sedation during prolonged mechanical ventilation: Two randomized controlled trials. JAMA, 307(11), 1151–1160.
Gurbet, A., Basagan-Mogol, E., Turker, G., et al. (2006). Intraoperative infusion of dexmedetomidine reduces perioperative analgesic requirements. Canadian Journal of Anesthesia, 53(7), 646–652.
Arain, S. R., Ruehlow, R. M., Uhrich, T. D., et al. (2004). The efficacy of dexmedetomidine versus morphine for postoperative analgesia after major inpatient surgery. Anesthesia and Analgesia, 98(1), 153–158.
Shehabi, Y., Ruettimann, U., Adamson, H., et al. (2004). Dexmedetomidine infusion for more than 24 hours in critically ill patients: Sedative and cardiovascular effects. Intensive Care Medicine, 30(12), 2188–2196.
Hofer, R. E., Sprung, J., Sarr, M. G., et al. (2005). Anesthesia for a patient with morbid obesity using dexmedetomidine without narcotics. Canadian Journal of Anesthesia, 52(2), 176–180.
Can, M., Gul, S., Bektas, S., et al. (2009). Effects of dexmedetomidine or methylprednisolone on inflammatory responses in spinal cord injury. Acta Anaesthesiologica Scandinavica, 53(8), 1068–1072.
Memiş, D., Hekimoğlu, S., Vatan, I., et al. (2007). Effects of midazolam and dexmedetomidine on inflammatory responses and gastric intramucosal pH to sepsis, in critically ill patients. British Journal of Anaesthesia, 98(4), 550–552.
Paris, A., Mantz, J., Tonner, P. H., et al. (2006). The effects of dexmedetomidine on perinatal excitotoxic brain injury are mediated by the α2A-adrenoceptor subtype. Anesthesia and Analgesia, 102(2), 456–461.
Zhang, X., Wang, J., Qian, W., et al. (2014). Dexmedetomidine inhibits tumor necrosis factor-alpha and interleukin 6 in lipopolysaccharide-stimulated astrocytes by suppression of c-Jun N-terminal kinases. Inflammation, 37(3), 942–949.
Font-Nieves, M., et al. (2012). Induction of COX-2 enzyme and down-regulation of COX-1 expression by lipopolysaccharide (LPS) control prostaglandin E2 production in astrocytes. Journal of Biological Chemistry, 287(9), 6454–6468.
Gu, L., Hertz, L., & Peng, L. (2013). Dexmedetomidine causes neuroprotection via astrocytic α2-adrenergic receptor stimulation and HB-EGF release. Journal of Anesthesiology and Clinical Research, 2(1), 6–14.
Ayoglu, H., Gul, S., Hanci, V., et al. (2010). The effects of dexmedetomidine dosage on cerebral vasospasm in a rat subarachnoid haemorrhage model. Journal of Clinical Neuroscience, 17(6), 770–773.
Bélanger, M., Allaman, I., & Magistretti, P. J. (2011). Brain energy metabolism: focus on astrocyte-neuron metabolic cooperation. Cell Metabolism, 14(6), 724–738.
Chorney, S. R., Gooch, M. E., Oberdier, M. T., et al. (2012). The safety and efficacy of dexmedetomidine for postoperative sedation in the cardiac surgery intensive care unit. HSR proceedings in intensive care & cardiovascular anesthesia, 5(1), 17–24.
Roberson, D. B., & Riddle, J. D. (2013). The impact of intra-operative dexmedetomidine infusion on immediate postoperative pain: A systematic review protocol. The JBI Database of Systematic Reviews and Implementation Reports, 11(10), 42–54.
Huang, Y., Lu, Y., Zhang, L., et al. (2014). Perineural dexmedetomidine attenuates inflammation in rat sciatic nerve via the NF-κB pathway. International Journal of Molecular Sciences, 15(3), 4049–4059.
Xiang, H., Hu, B., Li, Z., et al. (2014). Dexmedetomidine controls systemic cytokine levels through the cholinergic anti-inflammatory pathway. Inflammation, 37(5), 1763–1770.
Yi, J. W., Lee, B. J., Choi, I. Y., et al. (2013). Dexmedetomidine alleviates short-term memory impairment through inhibiting apoptosis in the hippocampus following transient cerebral ischemia in gerbils: 7AP3-2. European Journal of Anaesthesiology (EJA), 30, 107.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xie, C., Wang, Z., Tang, J. et al. The Effect of Dexmedetomidine Post-treatment on the Inflammatory Response of Astrocyte Induced by Lipopolysaccharide. Cell Biochem Biophys 71, 407–412 (2015). https://doi.org/10.1007/s12013-014-0213-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-014-0213-0