Abstract
Zinc (Zn) participates as a cofactor for many enzymes in the cellular metabolism, and its serum levels have been associated with different metabolic diseases, especially obesity (OB). Nevertheless, its associations are not clear in the children population. The objective of this study is to evaluate the association between serum Zn levels (SZn) with overweight/obesity status (OW/OB), as well as its cardiometabolic traits in a population of children in Mexico City. Anthropometrical data (body mass index z score (BMIz)), demographic variables (age and sex), and cardiometabolic traits (total cholesterol (TC), high-density lipoprotein cholesterol (HDLc), low-density lipoprotein cholesterol (LDLc), triglycerides (TG), fasting plasma glucose (FPG), and insulin) were analyzed in this cross-sectional study. SZn were measured by inductively coupled plasma mass spectrometry (ICP–MS). The population included 210 children from Mexico City (girls (n = 105) and boys (n = 105)) between ages 6 and 10 years. Normal-weight (NW) schoolchildren had higher SZn concentrations (66 µg/dL; IQR: 48 to 91) compared to OW or OB schoolchildren (61 µg/dL; IQR: 45 to 76). The data showed a significant negative association between SZn and BMIz without sex exclusion (r = − 0.181 and p = 0.009). The boy’s population did not show an association between the SZn and BMIz compared to the girl’s population which showed a significant negative association (r = − 0.277 and p = 0.004). In addition, other associations were found between SZn and TC (boys (r = 0.214 and p = 0.025), LDLc (boys (r = 0.213 and p = 0.029), and TG (girls (r = − 0.260 and p = 0.007)). Moreover, 38.6% of the total children in our population study had Zn deficiency (ZnD). NW schoolchildren had higher SZn concentrations compared to OW or OB schoolchildren. A diet low in Zn can be a factor to evaluate in the development of childhood OB in Mexico. However, further studies need to be performed on the children Mexican population to replicate and confirm our findings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The prevalence of overweight/obesity (OW/OB) in schoolchildren has increased consistently around the world; in recent years, this prevalence has been considered a pandemic in many populations, especially those with high incomes [1, 2]. However, today has been described that OW/OB are now on the rise in low- and middle-income populations [3].
OB is a multifactorial disease with genetic, environmental, behavioral, and sociocultural characteristics [4, 5]. In this context, many children with OB retain a high body mass index (BMI), which can be maintained or increased in adulthood, contributing to the development of cardiometabolic diseases [6], specifically type 2 diabetes, hypertension, and heart disease [7]. Moreover, OB has recently been associated with severity and mortality among the adult population with the COVID-19 [8, 9].
Mexico has shown a high prevalence of OW/OB in schoolchildren in the last 2 decades, and the National Health and Nutrition Survey found that three out of ten children have OW or OB [10]. The main factors of increases in OB have been the association of frequent intake of foods with high fat and sugar content and a more sedentary lifestyle. Nevertheless, Mexico has implemented new health policies focusing on food labeling as an alternative to prevent OB [11, 12], which are related to food education, lifestyle change, and time increases in daily exercise [13]. In addition, security food and traditional food programs have been carried out to decrease OB in the Mexican population. Some of these programs include the Strategic Project for Food Security between the Secretariat of Agriculture, Livestock, Rural Development, Fisheries and Food (SAGARPA) in collaboration with the FAO; the Sustainable Modernization of Traditional Agriculture program implemented by SAGARPA and the International Maize and Wheat Improvement Centre (CIMMYT) and Education, Health and Food Program (PROSPERA) by Education by the Secretary of Social Development that supports families to acquire and increase the variety and quantity of food [11, 14, 15].
Trace elements have an essential role in cellular metabolism, and a deficiency of these elements can lead to the incidence of OW and OB [16,17,18]. However, these findings do not show conclusive evidence. The main trace elements that have been studied and associated with OW/OB are zinc (Zn) and copper (Cu), followed by magnesium (Mg), chromium (Cr), and selenium (Se) [19,20,21,22,23]. In the case of Zn, this is an essential element present in several enzymes, and it participates in the mechanisms of energy metabolism by carbohydrates, proteins, and lipids [24, 25].
Serum Zn levels (SZn) are altered with OB due to oxidative stress and inflammatory processes [25,26,27,28], and Zn levels have been related to OB. However, the relationship between SZn and OW/OB is unclear in the children population. Recently, Fan et al. reported that Zn deficiency (ZnD) is an important cause of morbidity and mortality in the children population [19]. On the other hand, ZnD in children increases the risk of growth retardation [29,30,31,32,33], insulin resistance [34,35,36], and neurological disorders [37, 38] and increased susceptibility to infections [39, 40].
The aim of this study was to measure SZn and its association with OW/OB and cardiometabolic traits (total cholesterol (TC), high-density lipoprotein cholesterol (HDLc), low-density lipoprotein cholesterol (LDLc), triglycerides (TG), fasting plasma glucose (FPG), and insulin) in a population of schoolchildren from Mexico City.
Materials and Methods
Study Design
A cross-sectional study was carried out, and children from 6 to 10 years old were recruited from four elementary schools (two public and two private) selected by convenience in Mexico City and located in the same geographic area. Children with normal weight (NW), OW, or OB were included according to the BMIz [41]. Children with any disease or taking any medication that affected the metabolic profile were excluded.
Ethical Approval
The study was conducted according to the guidelines established in the Declaration of Helsinki and based on the Regulations of the General Health Law on Health Research in Mexico, based on articles 14 and 16. The research protocol was approved by Research, Ethics, and Biosecurity Committees from the Hospital Infantil de México Federico Gómez (approval register: HIM/2013/003) and by school authorities. Likewise, children and parents gave written assent and consent to participate in the study.
Measurements
Sociodemographic Characteristics
The parents answered a questionnaire that was sent to the home, and information was obtained on chronic diseases of the student and the level of education of the mother (secondary education or less, high school or technical school, and university or postgraduate studies). To evaluate the socioeconomic level of the families, information was obtained on the characteristics of the home and possession of goods such as refrigerators, washing machines, heaters, televisions, computers, ovens, internet, automobiles, and landline telephones. Principal component analysis was used, and considering the score obtained, the households were divided into categories of socioeconomic level in tertiles (low, medium, and high) based on the score obtained.
Anthropometry
Anthropometric parameters were registered by two previously trained nutritionists using standardized international anthropometric procedures [42]. Weight was measured with a balance (SECA model-882, SECA Corp., Hamburg, Germany) to the nearest 0.1 kg, and height was measured on a stadiometer (SECA model-225, SECA Corp., Hamburg, Germany) with a precision of 0.1 cm. Waist circumference was measured with a nonelastic flexible measuring tape (Seca 200). The measurements were carried out without shoes and wearing light clothing, standing in the middle of the scale platform or stadiometer, arms resting freely by their sides, with their heads in the Frankfurt horizontal plane. BMIz was obtained using the children’s age, weight, height, and sex, which were classified as NW (z score ≥ –2 to <1), OW (z score ≥ 1 to < 2), and OB (z score ≥ 2), according to standards provided by the World Health Organization [43]. Waist circumference was used as a proxy to assess central visceral adiposity, and the waist circumference percentile was calculated considering age, sex, and height using the waist circumference tables of Mexican children [44].
Biochemical Determinations
Serum sample collection
A sample of 5 mL of peripheral blood was collected by venipuncture from each participant after a 12 h fast in a sterile vacutainer tube. Separation of serum was performed in the following steps: (a) total blood sample was allowed to stand for 20 min, (b) separation of serum by centrifugation in glass tubes at 3000 × g for 10 min to 4 °C, and (c) all serum samples were stored in Eppendorf tubes at − 80 °C.
Analysis of TC, HDLc, LDLc, TG, and FPG was performed by commercial kits, and measures were carried out at LAB 300, Instrumentation Laboratory, Barcelona, Spain. For LDLc, DeLong’s modified Friedwald formula was utilized [45]. Insulin was determined by chemiluminescence immunoassay (IMMULITE 2000, Euro, DPC, Llanberis, UK).
Analysis of Zn by ICP–MS
SZn quantification was performed with inductively coupled plasma mass spectrometry (ICP–MS iCAP Q, Thermo Scientific, Germany) following the protocol proposed by Rios Lugo et al. [46]. Samples were traced with indium (In; 10 μg L−1) and mineralized with a microwave system (MARS6 CEM, Matthews, North Carolina) before analysis of total Zn with ICP–MS. The mineralization process was realized with 8 mL HNO3 in two steps (ramp of temperature to 200 °C and holding for 15 min). Finally, samples were recovered and evaporated to dryness and diluted to 10 mL with 2% v/v HNO3. SZn quantification in samples was performed by an external calibration curve of Zn (10, 25, 50, 75, 100, 200, 500, and 1000 μg L−1). Moreover, contribution contamination in the analysis was considered by calculating SZn in samples (blank reagents), as well as the recovery of an internal standard (In), final volume (10 mL), and sample volume (0.1 mL). Concentrated high-purity HNO3 (Milestone Duopur system Milestonesrl, Italia) and high-purity water with 18 MΩ cm (Milli-Q® system Millipore, México) were used in the sample preparation. In addition, Zn standards were obtained from the High-Purity Standards (North Charleston, USA).
Data Analysis
Analysis was performed with SPSS® v20.0 (SPSS Inc., Chicago, Illinois). Measures of central tendency were used to describe the baseline characteristics of the study population. Weight and height measurements were adjusted for age and sex using multiple linear regression. For statistical analysis, the categories of OW and OB (OW/OB) were combined and compared to children with NW to balance the sample size and provide greater statistical stability. The normality of the continuous variables was evaluated using the Kolmogorov–Smirnov test, indicating a nonnormal distribution of the data. In this case, the medians and interquartile range (IQR) were obtained for continuous data without normal distribution and percentages for categorical variables. The Mann–Whitney U test was used to compare age, anthropometric measurements, SZn, and metabolic parameters according to nutritional status. To determine which variables were related to ZnD, the study population was divided into two groups based on SZn, one below the cutoff value (< 70 ug/dL) and one above the cutoff value (> 70 ug/dL) according to the International Zinc Nutrition Consultative Group (IZiNCG) [47]. For age, sex, BMI, waist circumference (WC), and biochemical status, Mann–Whitney U test was used, while socioeconomic variables were analyzed using the Pearson X2 test. In addition, Spearman linear correlation was carried out to evaluate the correlations between SZn and BMIz, WC, FPG, TC, TG, LDLc, HDLc, and insulin. P values < 0.05 were considered statistically significant for all analyses.
Results
General Characteristics of the Study Population
The general characteristics of the population are shown in Table 1. The median age of the children population was 8.0 ± 1.1 years. Statistically significant differences were found in the anthropometric variables (weight, height, BMIz, and WC) according to nutritional status (p < 0.05). In addition, school type in the children population showed a significant statistical difference (p = 0.025).
Biochemical Profile
The girls’ metabolic profile showed statistically significant differences between girls with normal weight and those with OW/OB (Table 2). Girls with OW/OB had higher concentrations of FPG (p = 0.043), TC (p = 0.001), TG (p < 0.001), LDLc (p < 0.001), and insulin (p < 0.001), while HDLc was higher in girls with NW (p = 0.004). Boys with OW or OB had higher concentrations of FPG (p = 0.001), TG (p < 0.001), and insulin (p < 0.001), while boys with NW also had higher concentrations of HDLc (p = 0.02) in comparison to boys with OW and OB.
Zn Levels According to Nutritional Status and Sex
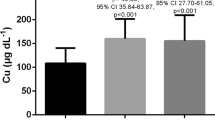
SZn levels in the children according to nutritional status and sex are shown in Fig. 1. SZn showed significant differences between the schoolchildren with NW and the schoolchildren with OW/OB (p = 0.033), where SZn values in OW/OB had a median of 61 µg/dL (IQR: 45 to 76) versus those in NW who showed a concentration of 66 µg/dL (IQR: 48 to 91). These results were independent of sex. In addition, our study did not find statistically significant differences in SZn according to sex (p = 0.813). In the case of ZnD, the results showed that 38.5% of the children were below the cutoff value established according to the IZiNCG.
Zn Cutoff Value and Anthropometric, Biochemical, and Socioeconomic Variables
We did not find a relationship between age or sex with SZn using the cutoff value, nor did we find statistically significant differences with BMIz. Notably, those children with higher WC were related to SZn levels below the cutoff value (p = 0.038). Regarding biochemical measures, we found that children with ZnD had lower LDLc and insulin levels compared to children without ZnD (p < 0.05). Moreover, the results obtained did not reveal statistically significant differences from the other biochemical parameters (Table 3). This last finding was reinforced when we evaluated the type of school, where the highest deficiency was found in children attending private schools. Finally, focusing only on the population below the cutoff value, we found a higher ZnD in children whose mothers had a higher level of education.
Associations Between Zn Levels and BMIz and Biochemical Profile
The results obtained for the correlations between SZn, BMIz, and cardiometabolic traits are shown in Table 4. Our study found a negative correlation between Zn levels and BMIz (r = − 0.181, p = 0.009). In addition, the BMIz showed positive correlations with WC, FPG, TC, TG, LDLc, and insulin without difference by sex, except for HDLc (r = − 0.396, p ≤ 0.001). The boys’ population showed a positive correlation between SZn and TC and LDLc. Moreover, negative correlations were found between SZn and BMIz (r = − 0.277, p ≤ 0.004), FPG (r = − 0.229, p ≤ 0.019), and TG (r = − 0.260, p ≤ 0.007) in the female population.
Discussion
Our work determined SZn levels in a population of children in Mexico City and showed that more than one-third of the study population had ZnD according to the cutoff established by IZiNCG [47, 48]. Our finding is consistent with other studies on the Mexican children, which have shown that the Mexican children have ZnD [49,50,51,52]. Likewise, other studies performed on the Latin American population showed similar results [53,54,55,56,57]. On the other hand, our results did not show significant differences in the age and sex distribution between the population studied with and without ZnD. Nevertheless, the study by Pullakhandam et al. mentioned that ZnD is higher in adolescents than in children because the requirements increase in the development stage [58].
Studies have shown evidence about the SZn and its relationship with OW and OB in humans [46, 59,60,61,62], but the data has not even been clear. Our study found a statistically significant difference between the population of children with OW/OB and NW (Fig. 1). These results are consistent with other performed studies on populations from Egypt, Korea, and India [63,64,65]. In contrast, Weisstaub et al. reported the absence of a relationship between SZn and OW/OB in a population of Chilean preschool children [66]. Likewise, Jaksic et al. found no association between SZn levels and BMIz in a population of Montenegro children [67].
No significant differences were found between BMIz and WC by sex in our children’s population. Our study found that a higher WC percentile had lower SZn despite having a normal BMIz. This indicates that BMIz and WC should be taken into account in the evaluation of trace element deficiency as has been reported by Zohal et al. [68] and Kim et al. [69]. These authors reported that low SZn levels and other trace elements are related to increases in WC and BMIz.
Childhood OB can cause metabolic and hormonal changes [70, 71]. In this way, the prevalence of OW/OB was > 50% in our population, where the prevalence was higher in girls. Our results exceeded the values reported by government institutions from Mexico [72, 73]. Nevertheless, these results differ from those reported by Del Monte et al. [74], where a higher prevalence of OW/OB was indicated in the child population. Moreover, our results showed significant differences between public and private schools for the values of BMIz and SZn.
Low socioeconomic status and low maternal education are associated with an increase in OW/OB in the child population [75,76,77]. However, the findings have been unclear because, in the Asian population, a relationship was reported between a high maternal education level and a higher prevalence of OW/OB in the child population [78,79,80]. In contrast, in the Western population, maternal education level was negatively associated with the prevalence of OW/OB [81, 82]. In this case, our study did not show significant differences between the maternal education level and the socioeconomic level.
Cardiometabolic traits have been linked to SZn in animal models [83, 84] and humans population with OW/OB [25, 85,86,87,88]. However, the available information is not yet conclusive. In our study, the female population showed significant differences in all cardiometabolic traits between NW and OW/OB. These results could have been due to the hormonal changes that have been reported by Arslan et al. [89] and Wisniewski and Chernausek [90]. In the case of the male population, significant differences were found between BMIz and cardiometabolic traits. In addition, we found statistically significant differences for LDLc and insulin with the cutoff established by IZiNCG. Our results agree with the study by Acosta García et al., which was performed on a Mexican children’s population [91].
Cardiometabolic parameters were found to be higher in the groups of schoolchildren OW or OB compared to children with NW, showing that from these ages, there are already clear differences that could remain or increase in adulthood, according to the criteria established by the Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents, and National Heart, Lung, and Blood Institute (NHLBI 2011) [92]. On the other hand, the dietary intake of Zn has been related to cardiometabolic traits in populations with OW/OB [86,87,88]. Costarelli et al. [93] mentioned that a lower dietary intake of Zn presents a deeper inflammatory state, an altered lipid profile, and higher production of insulin relative to OB individuals with a normal dietary intake of Zn. Additionally, El-Ashmony et al. reported that zinc supplementation could lower TC, LDLc, and TG and increase HDLc [94]. Moreover, other experimental studies have found a significant decrease in Zn in adipose tissue and a negative correlation with insulin, HOMA-IR, and TNF-α values in OB animals [95, 96] and humans [97].
The relationship between SZn and BMIz is not clear [27]. Our study demonstrated a negative association between SZn and BMIz regardless of sex, which was maintained in the female population (Table 4). The results found in our study were similar to those of other studies that reported this association [25, 27, 59, 62, 63, 65, 68]. However, the study by Sugawara et al. [98] contrasts with our results, as they reported a positive correlation between SZn and BMIz, while other studies have reported the absence of an association between Szn and BMIz [66, 99]. Likewise, the children population showed positive correlations of TC, TG, and LDLc with SZn (boys with TC and LDLc and girls with TG). These results are consistent with the study by Zavala G et al. [100]. However, the study of Azab et al. reported negative correlations between SZn and FPG and TG [63].
The relationship between the decrease in SZn with OW/OB has been evaluated through oxidative stress at the level of adipose tissue [97, 101, 102]. To date, the molecular mechanisms are not clear, but it has been shown that under these conditions of OW/OB, the increase in visceral fat due to OW and OB contributes to the secretion of cytokines such as IL-6, IL-8, and TNF-α, as well as an increase in the cortisol synthesis. This in turn induces the expression of metallothionein and Zip14 in adipose and hepatic tissue, contributing to the decrease in SZn levels [27, 100, 103].
Within the limitations of the study is that it is a sample of school children from elementary schools in Mexico City selected for convenience, so the findings found in this study cannot be generalized to all Mexican children. In addition, the Tanner stage of the schoolchildren was not measured; however, information was collected on the age of the schoolchildren, which is a proxy variable for said stage, and taking this into account when doing the analysis, no difference was found in the age between deficient and non-deficient school children of SZn. Finally, inflammation markers that could affect serum zinc levels were not obtained either, and studies are needed to complement these findings, since the studies are still inconsistent.
Conclusions
Schoolchildren with NW had higher SZn concentrations compared to schoolchildren with OW or OB. ZnD is a public health problem that can be underestimated in OW and OB, especially during childhood and adolescence, where Zn plays important roles in development and growth as well as in lipid and carbohydrate metabolism. Therefore, this type of study helps to understand its relationship with other variables that alert an early metabolic risk using parameters such as BMIz and WC. Together with the lipid profile, these should be considered to evaluate in a more comprehensive way a population at risk such as children, and thus avoid complications in adulthood.
Data Availability
The data set of this study is available from the corresponding authors on reasonable request.
Abbreviations
- BMI:
-
Body mass index
- BMIz:
-
Body mass index z score
- TC:
-
Total cholesterol
- ENSANUT:
-
The National Health and Nutrition Survey
- FPG:
-
Fasting plasma glucose
- HDLc:
-
Cholesterol high-density lipoprotein
- ICP–MS:
-
Inductively coupled plasma mass spectrometry
- IZiNCG:
-
International Zinc Nutrition Consultative Group
- LDLc:
-
Cholesterol low-density lipoprotein
- NW:
-
Normal weight
- OB:
-
Obesity
- OW:
-
Overweight
- SZn:
-
Serum zinc levels
- TG:
-
Triglycerides
- WC:
-
Waist circumference
- Zn:
-
Zinc
References
NCD Risk Factor Collaboration (NCD‐RisC) (2017) Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: a pooled analysis of 2416 population-based measurement studies in 128·9 million children, adolescents, and adults. Lancet 390:2627–2642. https://doi.org/10.1016/S0140-6736(17)32129-3
Wang Y, Lim H (2012) The global childhood obesity epidemic and the association between socio-economic status and childhood obesity. Int Rev Psychiatry 24(3):176–188. https://doi.org/10.3109/09540261.2012.688195
Turnbull B, Gordon SF, Martínez-Andrade GO, González-Unzaga M (2019). Childhood obesity in Mexico: a critical analysis of the environmental factors, behaviours and discourses contributing to the epidemic. Health Psychol Open 6(1). https://doi.org/10.1177/2055102919849406
González-Muniesa P, Mártinez-González M-A, Hu FB, Després J-P, Matsuzawa Y, Loos RJF, Moreno LA, Bray GA, Martinez JA (2017) Obesity Nat Rev Dis Primers 3:17034. https://doi.org/10.1038/nrdp.2017.34
Rohde K, Keller M, la Cour PL, Blüher M, Kovacs P, Böttcher Y (2019) Genetics and epigenetics in obesity. Metab Clin Exp 92:37–50. https://doi.org/10.1016/j.metabol.2018.10.007
Gardner DSL, Hosking J, Metcalf BS, Jeffery AN, Voss LD, Wilkin TJ (2009) Contribution of early weight gain to childhood overweight and metabolic health: a longitudinal study (EarlyBird 36). Pediatrics 123(1):e67–e73. https://doi.org/10.1542/peds.2008-1292
Kelishadi R (2007) Childhood overweight, obesity, and the metabolic syndrome in developing countries. Epidemiol Rev 29(1):62–76. https://doi.org/10.1093/epirev/mxm003
Thakur B, Dubey P, Benitez J, Torres JP, Reddy S, Shokar N, Aung K, Mukherjee D, Dwivedi AK (2021) A systematic review and meta-analysis of geographic differences in comorbidities and associated severity and mortality among individuals with COVID-19. Sci Rep 11:8562. https://doi.org/10.1038/s41598-021-88130-w
Nogueira-de-Almeida CA, Del Ciampo LA, Ferraz IS, Del Ciampo IRL, Contini AA, Ued F (2020) COVID-19 and obesity in childhood and adolescence: a clinical review. J Pediatr 96(5):546–558. https://doi.org/10.1016/j.jped.2020.07.001
Shamah-Levy T, Campos-Nonato I, Cuevas-Nasu L, Hernández-Barrera L, del Carmen Morales-Rúan M, Rivera-Dommarco J, Barquera S (2020) Sobrepeso y obesidad en población mexicana en condición de vulnerabilidad. Resultados de la Ensanut 100k. Salud Publica Mex 61(6):852–865
Ibarrola-Rivas MJ, Galicia L (2017) Rethinking food security in Mexico: discussing the need for sustainable transversal policies linking food production and food consumption. Investig Geogr 94. https://doi.org/10.14350/rig.57538
White M, Barquera S (2020) Mexico adopts food warning labels, why now? Health Syst Reform 6(1):e1752063. https://doi.org/10.1080/23288604.2020.1752063
Vilchis-Gil J, Klünder-Klünder M, Flores-Huerta S (2008) Effect on the metabolic biomarkers in schoolchildren after a comprehensive intervention using electronic media and in-person sessions to change lifestyles: community trial. J Med Internet Res 20(2):e44. https://doi.org/10.2196/jmir.9052
Ordóñez-Barba GM, Silva-Hernández AL (2019) Progresa-Oportunidades-Prospera: avatares, alcances y resultados de un programa paradigmático contra la pobreza. Papeles Poblac 25(99):77–111. https://doi.org/10.22185/24487147.2019.99.04
Rizzoli-Córdoba A, Martell-Valdez L, Delgado-Ginebra I, Villasís-Keever MÁ, Reyes-Morales H, O’Shea-Cuevas G, Aceves-Villagrán D, Carrasco-Mendoza J, Villagrán-Muñoz VM, Halley-Castillo E, Vargas-López G, Muñoz-Hernández O (2015) Escrutinio poblacional del nivel de desarrollo infantil en menores de 5 años beneficiarios de PROSPERA en México. Bol Med Hosp Infant Mex 72(6):409–419. https://doi.org/10.1016/j.bmhimx.2015.10.003
Zohal M, Jam-Ashkezari S, Namiranian N, Moosavi A, Ghadiri-Anari A (2019) Association between selected trace elements and body mass index and waist circumference: a cross sectional study. Diabetes Metab Syndr: Clin Res Rev 13(2):1293–1297. https://doi.org/10.1016/j.dsx.2019.01.019
Fedele D, De Francesco A, Riso S, Collo A (2021) Obesity, malnutrition, and trace element deficiency in the coronavirus disease (COVID-19) pandemic: an overview. Nutrition 81:111016. https://doi.org/10.1016/j.nut.2020.111016
Freeland-Graves JH, Sanjeevi N, Lee JJ (2015) Global perspectives on trace element requirements. J Trace Elem Med Biol 31:135–141. https://doi.org/10.1016/j.jtemb.2014.04.006
Fan Y, Zhang C, Bu J (2017) Relationship between selected serum metallic elements and obesity in children and adolescent in the U.S. Nutrients 9(2):104. https://doi.org/10.3390/nu9020104
Cao J, Gao Z, Yan J, Li M, Su J, Xu J, Yan CH (2016) Evaluation of trace elements and their relationship with growth and development of young children. Biol Trace Elem Res 171:270–274. https://doi.org/10.1007/s12011-015-0537-7
Yin Y, Li Y, Li Q, Jia N, Liu A, Tan Z, Wu Q, Fan Z, Li T, Wang L (2017) Evaluation of the relationship between height and zinc, copper, iron, calcium, and magnesium levels in healthy young children in Beijing, China. Biol Trace Elem Res 176:244–250. https://doi.org/10.1007/s12011-016-0830-0
Tascilar ME, Ozgen IT, Abaci A, Serdar M, Aykut O (2011) Trace elements in obese Turkish children. Biol Trace Elem Res 143:188–195. https://doi.org/10.1007/s12011-010-8878-8
Zhang H, Cai L (2020) Zinc homeostasis plays an important role in the prevention of obesity-induced cardiac inflammation, remodeling and dysfunction. J Trace Elem Med Biol 62:126615. https://doi.org/10.1016/j.jtemb.2020.126615
Ranasinghe P, Wathurapatha WS, Ishara MH, Jayawardana R, Galappatthy P, Katulanda P, Constantine GR (2015) Effects of Zinc supplementation on serum lipids : a systematic review and meta-analysis. Nutr Metab (Lond) 12:26. https://doi.org/10.1186/s12986-015-0023-4
Olechnowicz J, Tinkov A, Skalny A, Suliburska J (2017) Zinc status is associated with inflammation, oxidative stress, lipid, and glucose metabolism. J Physiol Sci 68:19–31. https://doi.org/10.1007/s12576-017-0571-7
Kelishadi R, Hashemipour M, Adeli K, Tavakoli N, Movahedian-Attar A, Shapouri J, Poursafa P, Rouzbahani A (2010) Effect of zinc supplementation on markers of insulin resistance, oxidative stress, and inflammation among prepubescent children with metabolic syndrome. Metab Syndr Relat Disord 8(6):505–510. https://doi.org/10.1089/met.2010.0020
Habib SA, Saad EA, Elsharkawy AA, Attia ZR (2015) Pro-inflammatory adipocytokines, oxidative stress, insulin, Zn and Cu: interrelations with obesity in Egyptian non-diabetic obese children and adolescents. Adv Med Sci 60(2):179–185. https://doi.org/10.1016/j.advms.2015.02.002
Marreiro DDN, Cruz KJC, Morais JBS, Beserra JB, Severo JS, De Oliveira ARS (2017) Zinc and oxidative stress: current mechanisms. Antioxidants 6(2):24. https://doi.org/10.3390/antiox6020024
Prasad AS (2014) Impact of the discovery of human zinc deficiency on health. J Trace Elem Med Biol 28(4):357–363. https://doi.org/10.1016/j.jtemb.2014.09.002
Mayo-Wilson E, Junior JA, Imdad A, Dean S, Chan XHS, Chan ES, Jaswal A, Bhutta ZA (2014) Zinc supplementation for preventing mortality, morbidity, and growth failure in children aged 6 months to 12 years of age. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD009384.pub2
Salgueiro MJ, Zubillaga MB, Lysionek AE, Caro RA, Weill R, Boccio JR (2002) The role of zinc in the growth and development of children. Nutrition 18(6):510–519. https://doi.org/10.1016/S0899-9007(01)00812-7
Farias PM, Marcelino G, Santana LF, de Almeida EB, Guimarães RDCA, Pott A, Hiane PA, Freitas KDC (2020) Minerals in pregnancy and their impact on child growth and development. Molecules 25(23):5630. https://doi.org/10.3390/molecules25235630
Krebs NF, Miller LV, Hambidge MK (2014) Zinc deficiency in infants and children: a review of its complex and synergistic interactions. Paediatr Int Child Health 34(4):279–288. https://doi.org/10.1179/2046905514Y.0000000151
Fukunaka A, Fujitani Y (2018) Molecular sciences role of zinc homeostasis in the pathogenesis of diabetes and obesity. Int J Mol Sci 19(2):476. https://doi.org/10.3390/ijms19020476
Salas-González MD, Rodríguez-Rodríguez E, Ortega AIJ, González-Rodríguez LG, López-Sobaler AM (2021) Zinc and its relation to insulin resistance in children. Nutr Hosp 38(Spec No2):68–70. https://doi.org/10.20960/nh.03802
Chabosseau P, Rutter GA (2016) Zinc and diabetes. Arch Biochem Biophys 611:79–85. https://doi.org/10.1016/j.abb.2016.05.022
Mezzaroba L, Alfieri DF, Simão ANC, Reiche EMV (2019) The role of zinc, copper, manganese and iron in neurodegenerative diseases. Neurotoxicology 74:230–241. https://doi.org/10.1016/j.neuro.2019.07.007
Cicero CE, Mostile G, Vasta R, Rapisarda V, Santo Signorelli S, Ferrante M, Nicoletti A (2017) Metals and neurodegenerative diseases. A systematic review. Environ Res 159:82–94. https://doi.org/10.1016/j.envres.2017.07.048
Haase H, Rink L (2014) Zinc signals and immune function. BioFactors 40(1):27–40. https://doi.org/10.1002/biof.1114
Maares M, Haase H (2016) Zinc and immunity: an essential interrelation. Arch Biochem Biophys 611:58–65. https://doi.org/10.1016/j.abb.2016.03.022
Onis MD, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J (2007) Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ 85(9):660–667. https://doi.org/10.2471/BLT.07.043497
World Health Organization (2020) Physical status: the use and interpretation of anthropometry: report of a WHO Expert Committee. Geneva; 1995. WHO technical report series, 854. Available from: https://apps.who.int/iris/handle/10665/37003. Accessed 21 Dec 2022
De Onis M, Habicht JP (1996) Anthropometric reference data for international use: recommendations from a World Health Organization Expert Committee. Am J Clin Nutr 64(4):650–658. https://doi.org/10.1093/ajcn/64.4.650
Klünder-Klünder M, Flores-Huerta S (2011) Waist circumference values according to height percentiles: a proposal to evaluate abdominal obesity in Mexican children and adolescents between 6 and 16 years of age. Arch Med Res 42(6):515–522. https://doi.org/10.1016/j.arcmed.2011.09.004
Delong DM, Delong ER, Wood PD, Lippel K, Rifkind BM (1986) A comparison of methods for the estimation of plasma low- and very low-density lipoprotein cholesterol: the lipid research clinics prevalence study. J Am Med Assoc 256(17):2372–2377. https://doi.org/10.1001/jama.1986.03380170088024
Rios-Lugo MJ, Madrigal-Arellano C, Gaytán-Hernández D, Hernández-Mendoza H, Romero-Guzmán ET (2020) Association of serum zinc levels in overweight and obesity. Biol Trace Elem Res 198(1):51–57. https://doi.org/10.1007/s12011-020-02060-8
De Benoist B, Darnton-Hill I, Davidsson L, Fontaine O, Hotz C (2007) Conclusions of the Joint WHO/UNICEF/IAEA/IZiNCG interagency meeting on zinc status indicators. Food Nutr Bull 28(3):S480–S484. https://doi.org/10.1177/15648265070283S306
Gibson RS, Hess SY, Hotz C, Brown KH (2008) Indicators of zinc status at the population level: a review of the evidence. Br J Nutr 99(S3):S14–S23. https://doi.org/10.1017/S0007114508006818
Morales-Ruán MC, Villalpando S, García-Guerra A, Shamah-Levy T, Robledo-Pérez R, Ávila-Arcos MA, Rivera JA (2012) Iron, zinc, copper and magnesium nutritional status in Mexican children aged 1 to 11 years. Salud Publica Mex 54(2):125–134. Available from: https://saludpublica.mx/index.php/spm/article/view/7121. Accessed 21 Dec 2022
Cruz-Góngora VDL, Martínez-Tapia B, Cuevas-Nasu L, Rangel-Baltazar E, Medina-Zacarías MC, García-Guerra A, Villalpando S, Rebollar R, Shamah-Levy T (2021) Anemia, deficiencias de zinc y hierro, consumo de suplementos y morbilidad en niños mexicanos de 1 a 4 años: resultados de la Ensanut 100k. Salud Publica Mex 61:821–832. https://doi.org/10.21149/10557
Cantoral A, Téllez-Rojo MM, Levy TS, Hernández-Ávila M, Schnaas L, Hu H, Peterson KE, Ettinger AS (2015) Differential association of lead on length by zinc status in two-year old Mexican children. Environ Health 14:95. https://doi.org/10.1186/s12940-015-0086-8
Shamah-Levy T, Villalpando S, Jáuregui A, Rivera JA (2012) Overview of the nutritional status of selected micronutrients in Mexican children in 2006. Salud Publica Mex 54(2):146–151. Available from: https://saludpublica.mx/index.php/spm/article/view/7123. Accessed 21 Dec 2022
Cediel G, Olivares M, Brito A, Cori H, López de Romaña D (2015) Zinc deficiency in Latin America and the Caribbean. Food Nutr Bull 36(2_suppl):S129–S138. https://doi.org/10.1177/037957211558578
Marín C, Oliveros H, Villamor E, Mora M (2021) Niveles de micronutrientes en niños escolares colombianos e inseguridad alimentaria. Biomedica 41(3):458–471. https://doi.org/10.7705/biomedica.5866
Palacios AM, Hurley KM, De-Ponce S, Alfonso V, Tilton N, Lambden KB, Reinhart GA, Freeland-Graves JH, Villanueva LM, Black MM (2020) Zinc deficiency associated with anaemia among young children in rural Guatemala. Matern Child Nutr 16(1):e12885. https://doi.org/10.1111/mcn.12885
Gupta S, Brazier AKM, Lowe NM (2020) Zinc deficiency in low-and middle-income countries: prevalence and approaches for mitigation. J Hum Nutr Diet 33(5):624–643. https://doi.org/10.1111/jhn.12791
Pinzón-Rondón ÁM, Hoyos-Martínez A, Parra-Correa D, Pesraza-Flechas AM, Ruiz-Sternberg ÁM (2019) Association of nutritional support programs with zinc deficiency in Colombian children: a cross-sectional study. BMC Nutr 5:42. https://doi.org/10.1186/s40795-019-0305-8
Pullakhandam R, Ghosh S, Kulkarni B, Reddy GB, Rajkumar H, Kapil U, Deb S, Kurpad AV, Sachdev HS (2022) Reference cut-offs to define low serum zinc concentrations in healthy 1–19 year old Indian children and adolescents. Eur J Clin Nutr 76:1150–1157. https://doi.org/10.1038/s41430-022-01088-4
Di Martino G, Matera MG, De Martino B, Vacca C, Di Martino S, Rossi F (1993) Relationship between zinc and obesity. J Med 24(2–3):177–183
Severo JS, Morais JBS, Beserra JB, Dos Santos LR, De Sousa MSR, De Sousa GS, De Matos Neto EM, Herique GS, Marreiro DDN (2020) Role of zinc in zinc-α2-glycoprotein metabolism in obesity: a review of literature. Biol Trace Elem Res 193:81–88. https://doi.org/10.1007/s12011-019-01702-w
Hernández-Mendoza H, Martínez-Navarro I, Hernández-Ochoa E, Espinoza-Ruiz M, Lugo-Trampe A, Trujillo-Murillo KDC, López-García MA, Rios-Lugo MJ, Chang-Rueda C (2022) Serum zinc levels are associated with obesity and low-density lipoprotein cholesterol in Mexican adults. Trace Elem Med Biol 73:127002. https://doi.org/10.1016/j.jtemb.2022.127002
Marreiro DDN, Fisberg M, Cozzolino SMF (2002) Zinc nutritional status in obese children and adolescents. Biol Trace Elem Res 86(2):107–122. https://doi.org/10.1385/BTER:86:2:107
Azab SF, Saleh SH, Elsaeed WF, Elshafie MA, Sherief LM, Esh AM (2014) Serum trace elements in obese Egyptian children: a case-control study. Ital J Pediatr 40:20. https://doi.org/10.1186/1824-7288-40-20
Gu K, Xiang W, Zhang Y, Sun K, Jiang X (2019) The association between serum zinc level and overweight/obesity: a meta-analysis. Eur J Nutr 58:2971–2982. https://doi.org/10.1007/s00394-018-1876-x
Malik VS, Dayal D, Khaiwal R, Bharti B, Bhalla A, Singh S, Kaur H, Attri S (2020) Low serum copper and zinc concentrations in North Indian children with overweight and obesity. Pediatr Endocrinol Diabetes Metab 26(2):79–83. https://doi.org/10.5114/pedm.2020.95627
Weisstaub G, Hertrampf E, López de Romaña D, Salazar G, Bugueño C, Castillo-Duran C (2007) Plasma zinc concentration, body composition and physical activity in obese preschool children. Biol Trace Elem Res 118:167–174. https://doi.org/10.1007/s12011-007-0026-8
Jaksic M, Martinovic M, Gligorovic-Barhanovic N, Vujacic A, Djurovic D, Nedovic-Vukovic M (2019) Association between inflammation, oxidative stress, vitamin D, copper and zinc with pre-obesity and obesity in school children from the city of Podgorica. Montenegro J Pediatr Endocrinol Metab 32(9):951–957. https://doi.org/10.1515/jpem-2019-0086
Zohal M, Jam-Ashkezari S, Namiranian N, Moosavi A, Ghadiri-Anari A (2019) Association between selected trace elements and body mass index and waist circumference: a cross sectional study. Diabetes Metab Syndr: Clin Res Rev 13(2):1293–1297. https://doi.org/10.1016/j.dsx.2019.01.019
Kim H-N, Song S-W, Choi W-S (2016) Association between serum zinc level and body composition: the Korean National Health and Nutrition Examination Survey. Nutrition 32(3):332–337. https://doi.org/10.1016/j.nut.2015.09.006
Styne DM, Arslanian SA, Connor EL, Farooqi IS, Murad MH, Silverstein JH, Yanovski JA (2017) Pediatric obesity—assessment, treatment, and prevention: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 102(3):709–757. https://doi.org/10.1210/jc.2016-2573
Speiser PW, Rudolf MC, Anhalt H, Camacho-Hubner C, Chiarelli F, Eliakim A, Freemark M, Gruters A, Hershkovitz E, Krude H, Ltzer Y, Lustig RH, Pescovitz OH, Pinhas-Hamiel O, Rogol AD, Shalitin S, Sultan C, Stein D, Vardi P, Werther GA, Zadik Z, Zuckerman-Levin N, Hochberg Z (2005) Childhood obesity. J Clin Endocrinol Metab 90(3):1871–1887. https://doi.org/10.1210/jc.2004-1389
Instituto Nacional de Estadística y Geografía (2020) Estadísticas a propósito del día mundial contra la obesidad. Available from: https://www.inegi.org.mx/contenidos/saladeprensa/aproposito/2020/EAP_Obesidad20.pdf. Accessed 21 Dec 2022
Secretaría de Salud, Instituto Nacional de Salud Pública, Instituto Nacional de Estadística y Geografía (2018) Encuesta Nacional de Salud y Nutrición 2018. Available from: https://ensanut.insp.mx/encuestas/ensanut2018/doctos/informes/ensanut_2018_presentacion_resultados.pdf. Accessed 21 Dec 2022
Del Monte-Vega MY, Shamah-Levy T, Méndez-Gómez H, Ávila-Arcos MA, Galindo-Gómez C, Ávila-Curiel A (2021) Cambios en sobrepeso y obesidad en escolares mexicanos de primarias públicas entre 2015 y 2018. Salud Publica Mex 63(2):170–179. https://doi.org/10.21149/11280
Rodd C, Sharma AK (2017) Prevalence of overweight and obesity in Canadian children, 2004 to 2013: impact of socioeconomic determinants. Paediatr Child Health 22(3):153–158. https://doi.org/10.1093/pch/pxx057
Zulfiqar T, Strazdins L, Banwell C, Dinh H, D’Este C (2018) Growing up in Australia: paradox of overweight/obesity in children of immigrants from low-and-middle-income countries. Obes Sci Pract 4(2):178–187. https://doi.org/10.1002/osp4.160
Ogden CL, Carroll MD, Fakhouri TH, Hales CM, Fryar CD, Li X, Freedman DS (2018) Prevalence of obesity among youths by household income and education level of head of household - United States 2011–2014. MMWR Morb Mortal Wkly Rep 67(6):186–189. https://doi.org/10.15585/mmwr.mm6706a3
Feng Y, Ding L, Tang X, Wang Y, Zhou C (2011) Association between maternal education and school-age children weight status: a study from the China Health Nutrition Survey, 2011. Int J Environ Res Public Health 16(14):2543. https://doi.org/10.3390/ijerph16142543
Liu W, Liu W, Lin R, Li B, Pallan M, Cheng KK, Adab P (2016) Socioeconomic determinants of childhood obesity among primary school children in Guangzhou. China BMC Public Health 16:482. https://doi.org/10.1186/s12889-016-3171-1
He W, James SA, Merli MG, Zheng H (2014) An increasing socioeconomic gap in childhood overweight and obesity in China. Am J Public Health 104(1):e14–e22. https://doi.org/10.2105/AJPH.2013.301669
Lamerz A, Kuepper-Nybelen J, Wehle C, Bruning N, Trost-Brinkhues G, Brenner H, Hebebrand J, Herpertz-Dahlmann B (2005) Social class, parental education, and obesity prevalence in a study of six-year-old children in Germany. Int J Obes 29:373–380. https://doi.org/10.1038/sj.ijo.0802914
Brophy S, Cooksey R, Gravenor MB, Mistry R, Thomas N, Lyons RA et al (2009) Risk factors for childhood obesity at age 5: analysis of the millennium cohort study. BMC Public Health 9:467. https://doi.org/10.1186/1471-2458-9-467
Fan G, Qiao Y, Gao S, Guo J, Zhao R, Yang X (2017) Effects of zinc alpha2 glycoprotein on lipid metabolism of liver in high-fat diet-induced obese mice. Horm Metab Res 49(10):793–800. https://doi.org/10.1055/s-0043-118910
Russell ST, Tisdale MJ (2010) Antidiabetic properties of zinc-α2-glycoprotein in ob/ob mice. Endocrinology 151(3):948–957. https://doi.org/10.1210/en.2009-0827
Yeung DC, Lam KS, Wang Y, Tso AW, Xu A (2009) Serum zinc-α2-glycoprotein correlates with adiposity, triglycerides, and the key components of the metabolic syndrome in Chinese subjects. J Clin Endocrinol Metab 94(7):2531–2536. https://doi.org/10.1210/jc.2009-0058
Ho M, Baur LA, Cowell CT, Samman S, Garnett SP (2017) Zinc status, dietary zinc intake and metabolic risk in Australian children and adolescents; Nepean Longitudinal Study. Eur J Nutr 56:2407–2414. https://doi.org/10.1007/s00394-016-1280-3
Cruz KJC, Morais JBS, de Oliveira ARS, Severo JS, Marreiro DDN (2017) The effect of zinc supplementation on insulin resistance in obese subjects: a systematic review. Biol Trace Elem Res 176:239–243. https://doi.org/10.1007/s12011-016-0835-8
Güngör NK (2014) Overweight and obesity in children and adolescents. J Clin Res Pediatr Endocrinol 3:129–143. https://doi.org/10.4274/jcrpe.1471
Arslan N, Erdur B, Aydin A (2010) Hormones and cytokines in childhood obesity. Indian Pediatr 47:829–839. https://doi.org/10.1007/s13312-010-0142-y
Wisniewski AB, Chernausek SD (2009) Gender in childhood obesity: family environment, hormones, and genes. Gender Med 6(Part 1):76–85. https://doi.org/10.1016/j.genm.2008.12.001
Acosta García E, Carías D, Páez Valery M, Naddaf G, Domínguez Z (2017) Zinc, copper and vitamins C, E and A in a pubertal overweight and insulin-resistant population. Acta Bioquim Clin Latinoam 51(2):203–212
Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents; National Heart, Lung, and Blood Institute. Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report (2011). Pediatrics. 128(Suppl 5):S213–S256. https://doi.org/10.1542/peds.2009-2107C
Costarelli L, Muti E, Malavolta M, Cipriano C, Giacconi R, Tesei S, Piacenza F, Pierpaoli S, Gasparini N, Faloia E, Tisabassi G, Boscaro M, Polito A, Mauro B, Maiani F, Raguzzini A, Marcellini F, Giuli C, Papa R, Emanuelli M, LattanzionF ME (2010) Distinctive modulation of inflammatory and metabolic parameters in relation to zinc nutritional status in adult overweight/obese subjects. J Nutr Biochem 21(5):432–437. https://doi.org/10.1016/j.jnutbio.2009.02.001
El-Ashmony SMA, Morsi HK, Abdelhafez AM (2012) Effect of zinc supplementation on glycemic control, lipid profile, and renal functions in patients with type ii diabetes: a single blinded, randomized, placebo-controlled, trial. J Biol Agric Healthc 2(6):33–41. Available from: https://core.ac.uk/outputs/234658440. Accessed 21 Dec 2022
Demirci Ş, Gün C (2022) Zinc supplementation improved neuropeptide Y, nesfatin-1, leptin, C-reactive protein, and HOMA-IR of diet-induced obese rats. Biol Trace Elem Res 200:3996–4006. https://doi.org/10.1007/s12011-021-02987-6
Abolghasemi J, Sharifi MH, Nasiri K, Akbari A (2020) Thyme oxymel by improving of inflammation, oxidative stress, dyslipidemia and homeostasis of some trace elements ameliorates obesity induced by high-fructose/fat diet in male rat. Biomed Pharmacother 126:110079. https://doi.org/10.1016/j.biopha.2020.110079
Banaszak M, Górna I, Przysławski J (2021) Zinc and the innovative zinc-α2-glycoprotein adipokine play an important role in lipid metabolism: a critical review. Nutrients 13(6):2023. https://doi.org/10.3390/nu13062023
Sugawara D, Makita E, Matsuura M, Ichihashi K (2022) The association between serum zinc levels and anthropometric measurements and nutritional indicators in children with idiopathic short stature. Cureus 14(5):e24906. https://doi.org/10.7759/cureus.24906
Obeid O, Elfakhani M, Hlais S, Iskandar M, Batal M, Mouneimne Y, Adra N, Hwalla N (2008) Plasma copper, zinc, and selenium levels and correlates with metabolic syndrome components of Lebanese adults. Biol Trace Elem Res 123:58–65. https://doi.org/10.1007/s12011-008-8112-0
Zavala G, Long KZ, García OP, Caamaño MDC, Aguilar T, Salgado LM, Rosado JL (2013) Specific micronutrient concentrations are associated with inflammatory cytokines in a rural population of Mexican women with a high prevalence of obesity. Br J Nutr 109(4):686–694. https://doi.org/10.1017/S0007114512001912
Morais JBS, Severo JS, Beserra JB, de Oiveira ARS, Cruz KJC, de Sousamelo SR, do Nascimient GVR, de Macedo GFS, do Nascimento Marreiro D (2019) Association between cortisol, insulin resistance and zinc in obesity: a mini-review. Biol Trace Elem Res 191:323–330. https://doi.org/10.1007/s12011-018-1629-y
Cunha TA, Vermeulen-Serpa KM, Grilo EC, Leite-Lais L, Brandão-Neto J, Vale SH (2022) Association between zinc and body composition: an integrative review. J Trace Elem Med Biol 71:126940. https://doi.org/10.1016/j.jtemb.2022.126940
Feitosa MCP, Lima VBDS, Neto MJM, Marreiro DDN (2013) Plasma concentration of IL-6 and TNF-α and its relationship with zincemia in obese women. Rev Assoc Med Bras 59(5):429–434. https://doi.org/10.1016/j.ramb.2013.03.003
Acknowledgements
We acknowledge to children, parents, principals, and elementary schools personnel for their participation in the study. My grateful thanks are also extended to Edduin Hernández-Ochoa for his technical support with sample processing. Special thanks are extended to Laboratorio del Agua y Monitoreo Ambiental, Universidad del Centro de México, for their valuable technical support on this project.
Funding
The present work was supported by Consejo Nacional de Ciencia y Tecnología (CONACYT) in the following projects: Laboratorio Nacional de Ciencia, Tecnología y Gestión Integrada del Agua (Project: 315880-CONACYT) and by Hospital Infantil de México Federico Gómez (Fondos Federales HIM/2013/003). We thank CONACYT for the doctoral scholarship awarded (2020–000026-02NACF-17180).
Author information
Authors and Affiliations
Contributions
I.M.N., M.J.R.L., H.H.M., J.V.G., and P.E.C.T. designed the study, perform the statistical analysis, wrote the manuscript, and designed tables and figures. I.M.N., H.H.M., M.K.K., and J.V.G. collect the data. I.M.N., M.J.R.L., and H.H.M. samples treatment and analysis by ICP–MS. E.L.E., O.G.C., I.M.N., M.J.R.L., H.H.M., M.K.K., J.V.G., and P.E.C.T. critically reviewed the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Martínez-Navarro, I., Vilchis-Gil, J., Cossío-Torres, P.E. et al. Relationship of Serum Zinc Levels with Cardiometabolic Traits in Overweight and Obese Schoolchildren from Mexico City. Biol Trace Elem Res 201, 4307–4319 (2023). https://doi.org/10.1007/s12011-022-03533-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-022-03533-8