Abstract
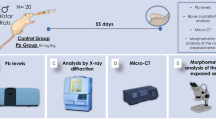
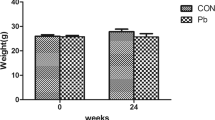
The alveolar bone is an important mineralized structure of the periodontal support apparatus, and information about the methylmercury (MeHg) effects on the structural integrity is scarce. Therefore, this study aimed to investigate whether systemic, chronic, and low-dose exposure to MeHg can change the alveolar bone microstructure of rats. Adult Wistar rats (n = 30) were exposed to 0.04 mg/kg/day of MeHg or vehicle through intragastric gavage. The animals were euthanized after 60 days, and blood samples were collected for trolox equivalent antioxidant capacity (TEAC), glutathione (GSH), lipid peroxidation (LPO), and comet assays. The mandible of each animal was collected and separated into hemimandibles that were used to determine the total Hg level in the bone and to analyze microstructural damage and alveolar bone loss in terms of trabecular number (Tb.N), trabecular thickness (Tb.Th), bone volume fraction (BV/TV), and exposed root area of the second molars. MeHg exposure triggered oxidative stress in blood represented by lower levels of GSH and TEAC and the increase in LPO and DNA damage of the blood cells. High total Hg levels were found in the alveolar bone, and the microstructural analyses showed a reduction in Tb.N, Tb.Th, and BV/TV, which resulted in an increase in the exposed root area and a decrease in bone height. Long-term MeHg exposure promotes a systemic redox imbalance associated with microstructural changes and alveolar bone loss and may indicate a potential risk indicator for periodontal diseases.







Similar content being viewed by others
References
Organization WH (2013) Mercury and health (fact sheet no. 361). Geneva
Hong Y-S, Kim Y-M, Lee K-E (2012) Methylmercury exposure and health effects. J Prev Med Public Health 45(6):353. https://doi.org/10.3961/jpmph.2012.45.6.353
Bernhoft RA (2012) Mercury toxicity and treatment: a review of the literature. J Environ Public Health 2012. https://doi.org/10.1155/2012/460508
Antunes A, Ferrer B, Marques Gonçalves F, Tsatsakis AM, Renieri EA, Skalny AV, Farina M, Rocha JB, Aschner M (2018) Oxidative stress in methylmercury-induced cell toxicity. J Toxics 6(3):47. https://doi.org/10.3390/toxics6030047
Bittencourt LO, Puty B, Charone S, Aragão WAB, Farias-Junior PM, Silva MCF, Crespo-Lopez ME, Leite AL, Buzalaf MAR, Lima RR (2017) Oxidative biochemistry disbalance and changes on proteomic profile in salivary glands of rats induced by chronic exposure to methylmercury. J Oxidative Med Cell Longev 2017:1–15. https://doi.org/10.1155/2017/5653291
Crespo-Lopez ME, Costa-Malaquias A, Oliveira EH, Miranda MS, Arrifano GP, Souza-Monteiro JR, Espirito-Santo Sagica F, Fontes-Junior EA, Maia CS, Macchi BM (2016) Is low non-lethal concentration of methylmercury really safe? A report on genotoxicity with delayed cell proliferation. PLoS One 11(9). https://doi.org/10.1371/journal.pone.0162822
Nogueira LS, Vasconcelos CP, Mitre GP, da Silva Kataoka MS, Lima MO, de Oliveira EH, Lima RR (2019) Oxidative damage in human periodontal ligament fibroblast (hPLF) after methylmercury exposure. J Oxidative Med Cell Longev 2019:1–7. https://doi.org/10.1155/2019/8470857
Arrifano GP, Martín-Doimeadios RCR, Jiménez-Moreno M, Ramírez-Mateos V, da Silva NF, Souza-Monteiro JR, Augusto-Oliveira M, Paraense RS, Macchi BM, do Nascimento JLM (2018) Large-scale projects in the amazon and human exposure to mercury: the case-study of the Tucuruí dam. J Ecotoxicol Environ Saf 147:299–305. https://doi.org/10.1016/j.ecoenv.2017.08.048
Crespo-López ME, Macêdo GL, Arrifano GP, Maria da Conceição NP, do Nascimento JLM, Herculano AM (2011) Genotoxicity of mercury: contributing for the analysis of Amazonian populations. J Environ Int 37(1):136–141. https://doi.org/10.1016/j.envint.2010.08.009
Lima LA, Bittencourt LO, Puty B, Fernandes RM, Nascimento PC, Silva MCF, Alves-Junior SM, Pinheiro JJV, Lima RR (2018) Methylmercury intoxication promotes metallothionein response and cell damage in salivary glands of rats. J Biol Trace Elem Res 185(1):135–142. https://doi.org/10.1007/s12011-017-1230-9
Farias-Junior PMA, Teixeira FB, Fagundes NCF, Miranda GHN, Bittencourt LO, de Oliveira Paraense RS, Silva MCF, Santo Sagica FE, de Oliveira EH, Crespo-López ME (2017) Chronic intoxication by methylmercury leads to oxidative damage and cell death in salivary glands of rats. Metallomics 9(12):1778–1785. https://doi.org/10.1039/c7mt00168a
Kim K-H, Kabir E, Jahan SA (2016) A review on the distribution of Hg in the environment and its human health impacts. J Hazard Mater 306:376–385. https://doi.org/10.1016/j.jhazmat.2015.11.031
Fernandes Azevedo B, Barros Furieri L, Peçanha FM, Wiggers GA, Frizera Vassallo P, Ronacher Simões M, Fiorim J, Rossi de Batista P, Fioresi M, Rossoni L (2012) Toxic effects of mercury on the cardiovascular and central nervous systems. J BioMed Res Int 2012. https://doi.org/10.1155/2012/949048
Schuurs A (1999) Reproductive toxicity of occupational mercury. A review of the literature. J Dent 27(4):249–256. https://doi.org/10.1016/s0300-5712(97)00039-0
Suzuki N, Yamamoto M, Watanabe K, Kambegawa A, Hattori A (2004) Both mercury and cadmium directly influence calcium homeostasis resulting from the suppression of scale bone cells: the scale is a good model for the evaluation of heavy metals in bone metabolism. J Bone Miner Metab 22(5):439–446. https://doi.org/10.1007/s00774-004-0505-3
Yachiguchi K, Sekiguchi T, Nakano M, Hattori A, Yamamoto M, K-i K, Maeda M, Tabuchi Y, Kondo T, Kamauchi H (2014) Effects of inorganic mercury and methylmercury on osteoclasts and osteoblasts in the scales of the marine teleost as a model system of bone. J Zool Sci 31(5):330–337. https://doi.org/10.2108/zs130265
Abd El-Aziz GS, El-Fark MM, Saleh HA (2012) The prenatal toxic effect of methylmercury on the development of the appendicular skeleton of rat fetuses and the protective role of vitamin E. Anat Rec (Hoboken) 295(6):939–949. https://doi.org/10.1002/ar.22485
Zhou S, Yang Y, Ha N, Zhang P, Ma X, Gong X, Hong Y, Yang X, Yang S, Dai Q (2018) The specific morphological features of alveolar bone. J Craniofacial Surg 29(5):1216–1219. https://doi.org/10.1097/scs.0000000000004395
Rawlinson S, Boyde A, Davis G, Howell P, Hughes F, Kingsmill VJ (2009) Ovariectomy vs. hypofunction: their effects on rat mandibular bone. 88(7):615–620
Passos-Soares JS, Vianna MIP, Gomes-Filho IS, Cruz SS, Barreto ML, Adan LF, Rösing CK, Trindade SC, Cerqueira EM, Scannapieco FA (2017) Association between osteoporosis treatment and severe periodontitis in postmenopausal women. 24(7):789–795
Fleischmannova J, Matalova E, Sharpe P, Misek I, Radlanski R (2010) Formation of the tooth-bone interface. J Dental Res 89(2):108–115. https://doi.org/10.1177/0022034509355440
Kong H-K, Wong M-H, Chan H-M, Lo SC-L (2013) Chronic exposure of adult rats to low doses of methylmercury induced a state of metabolic deficit in the somatosensory cortex. J Proteome Res 12(11):5233–5245. https://doi.org/10.1021/pr400356v
Ellman G (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82(1):70–77. https://doi.org/10.1016/0003-9861(59)90090-6
Rufino M, Alves R, Britoetal E (2007) Determination of the total antioxidant activity in fruits by the capture of free radical DPPH. J Press Release Embrapa 127:1–4
Re R, Pellegrini N, Proteggente A, Pannala A, Yang M, Rice-Evans C (1999) Antioxidant activity applying an improved ABTS radical cation decolorization assay. J Free Radic Biol Med 26(9–10):1231–1237. https://doi.org/10.1016/s0891-5849(98)00315-3
Kohn HI, Liversedge M (1944) On a new aerobic metabolite whose production by brain is inhibited by apomorphine, emetine, ergotamine, epinephrine, and menadione. J Pharmacol Exp Ther 82(3):292–300
Percário S (1994) Dosagem das LDLs modificadas através da peroxidação lipídica: correlação com o risco aterogênico. Anais Médicos dos Hospitais e da Faculdade de Ciências Médicas da Santa Casa de São Paulo 13(49–52):7–9
Singh N, Stephens R (1997) Microgel electrophoresis: sensitivity, mechanisms, and DNA electrostretching. J Mutat Res/DNA Repair 383(2):167–175. https://doi.org/10.1016/s0921-8777(96)00056-0
Suzuki T, Akagi H, Arimura K, Ando T, Sakamoto M, Satoh H, Nagamura A, Futatsuka M, Matsuyama A (2004) Mercury analysis manual. Ministry of the Environment, Japan
Hassumi JS, Mulinari-Santos G, Fabris ALS, Jacob RGM, Goncalves A, Rossi AC, Freire AR, Faverani LP, Okamoto R (2018) Alveolar bone healing in rats: micro-CT, immunohistochemical and molecular analysis. 26
Liberman DN, Pilau RM, Orlandini LF, Gaio EJ, Rösing CK (2011) Comparison of two methods for alveolar bone loss measurement in an experimental periodontal disease model in rats. J Braz Oral Res 25(1):80–84. https://doi.org/10.1590/S1806-83242011005000002
Bannach SV, Teixeira FB, Fernandes LMP, Ferreira RO, Santana LNS, Fontes-Júnior EA, Oliveira GB, Prediger RD, Maia CSF, Lima RR (2015) Alveolar bone loss induced by chronic ethanol consumption from adolescence to adulthood in Wistar rats. Indian J Exp Biol
Santana LNS, Bittencourt LO, Nascimento PC, Fernandes RM, Teixeira FB, Fernandes LMP, Silva MCF, Nogueira LS, Amado LL, Crespo-Lopez ME (2019) Low doses of methylmercury exposure during adulthood in rats display oxidative stress, neurodegeneration in the motor cortex and lead to impairment of motor skills. J Trace Elem Med Biol 51:19–27. https://doi.org/10.1016/j.jtemb.2018.09.004
Freire MAM, Santana LNS, Bittencourt LO, Nascimento PC, Fernandes RM, Leão LKR, Fernandes LMP, Silva MCF, Amado LL, Gomes-Leal W (2019) Methylmercury intoxication and cortical ischemia: pre-clinical study of their comorbidity. J Ecotoxicol Environ Saf 174:557–565. https://doi.org/10.1016/j.ecoenv.2019.03.009
Clarkson TW (2002) The three modern faces of mercury. J Environ Health Perspect 110(suppl 1):11–23. https://doi.org/10.1289/ehp.02110s111
Foulkes E (2000) Transport of toxic heavy metals across cell membranes (44486). J Proc Soc Exp Biol Med 223(3):234–240. https://doi.org/10.1177/153537020022300304
Ye B-J, Kim B-G, Jeon M-J, Kim S-Y, Kim H-C, Jang T-W, Chae H-J, Choi W-J, Ha M-N, Hong Y-S (2016) Evaluation of mercury exposure level, clinical diagnosis and treatment for mercury intoxication. J Ann Occup Environ Med 28(1). https://doi.org/10.1186/s40557-015-0086-8
Branco V, Caito S, Farina M, Teixeira da Rocha J, Aschner M, Carvalho C (2017) Biomarkers of mercury toxicity: past, present, and future trends. J Toxicol Environ Health, Part B 20(3):119–154. https://doi.org/10.1080/10937404.2017.1289834
Rasmussen KL, Boldsen JL, Kristensen HK, Skytte L, Hansen KL, Mølholm L, Grootes PM, Nadeau M-J, Eriksen KMF (2008) Mercury levels in Danish medieval human bones. J Archaeol Sci 35(8):2295–2306. https://doi.org/10.1016/j.jas.2008.03.003
Yamada M-o, Tohno S, Tohno Y, Minami T, Ichii M, Okazaki Y (1995) Accumulation of mercury in excavated bones of two natives in Japan. J Sci Total Environ 162(2–3):253–256. https://doi.org/10.1016/0048-9697(95)04435-4
Lindh U, Brune D, Nordberg G, Wester P-O (1980) Levels of antimony, arsenic, cadmium, copper, lead, mercury, selenium, silver, tin and zinc in bone tissue of industrially exposed workers. J Sci Total Environ 16(2):109–116. https://doi.org/10.1016/0048-9697(80)90018-2
Bittencourt LO, Dionizio A, Nascimento PC, Puty B, Leão LKR, Luz DA, Silva MCF, Amado LL, Leite A, Buzalaf MR (2019) Proteomic approach underlying the hippocampal neurodegeneration caused by low doses of methylmercury after long-term exposure in adult rats. J Metallomics 11(2):390–403. https://doi.org/10.1039/c8mt00297e
Bradley MA, Barst BD, Basu N (2017) A review of mercury bioavailability in humans and fish. Int J Environ Res Public Health 14(2):169. https://doi.org/10.3390/ijerph14020169
Ynalvez R, Gutierrez J, Gonzalez-Cantu H (2016) Mini-review: toxicity of mercury as a consequence of enzyme alteration. J Biometals 29(5):781–788. https://doi.org/10.1007/s10534-016-9967-8
Farina M, Aschner M (2019) Glutathione antioxidant system and methylmercury-induced neurotoxicity: an intriguing interplay. Biochim Biophys Acta, Gen Subj 1863(12):129285. https://doi.org/10.1016/j.bbagen.2019.01.007
Crespo-López ME, Macêdo GL, Pereira SI, Arrifano GP, Picanço-Diniz DL, do Nascimento JLM, Herculano AM (2009) Mercury and human genotoxicity: critical considerations and possible molecular mechanisms. J Pharmacol Res 60(4):212–220. https://doi.org/10.1016/j.phrs.2009.02.011
Liu W, Yang T, Xu Z, Xu B, Deng Y (2019) Methyl-mercury induces apoptosis through ROS-mediated endoplasmic reticulum stress and mitochondrial apoptosis pathways activation in rat cortical neurons. Free Radic Res 53(1):26–44. https://doi.org/10.1080/10715762.2018.1546852
Silva de Paula E, Carneiro MFH, Grotto D, Hernandes LC, Antunes LMG, Barbosa F Jr (2016) Protective effects of niacin against methylmercury-induced genotoxicity and alterations in antioxidant status in rats. J Toxicol Environ Health, Part A 79(4):174–183. https://doi.org/10.1080/15287394.2015.1137264
Grotto D, Barcelos GR, Valentini J, Antunes LM, Angeli JP, Garcia SC, Barbosa F Jr (2009) Low levels of methylmercury induce DNA damage in rats: protective effects of selenium. Arch Toxicol 83(3):249–254. https://doi.org/10.1007/s00204-008-0353-3
Kirkpatrick M, Benoit J, Everett W, Gibson J, Rist M, Fredette N (2015) The effects of methylmercury exposure on behavior and biomarkers of oxidative stress in adult mice. Neurotoxicology 50:170–178. https://doi.org/10.1016/j.neuro.2015.07.001
Barcelos GR, Angeli JP, Serpeloni JM, Grotto D, Rocha BA, Bastos JK, Knasmüller S, Júnior FB (2011) Quercetin protects human-derived liver cells against mercury-induced DNA-damage and alterations of the redox status. Mutat Res 726(2):109–115. https://doi.org/10.1016/j.mrgentox.2011.05.011
Chen N, Lin M, Liu N, Wang S, Xiao X (2019) Methylmercury-induced testis damage is associated with activation of oxidative stress and germ cell autophagy. J Inorg Biochem 190:67–74. https://doi.org/10.1016/j.jinorgbio.2018.10.007
Silva-Pereira LC, da Rocha CA, Cunha LR, da Costa ET, Guimarães AP, Pontes TB, Diniz DL, Leal MF, Moreira-Nunes CA, Burbano RR (2014) Protective effect of prolactin against methylmercury-induced mutagenicity and cytotoxicity on human lymphocytes. Int J Environ Res Public Health 11(9):9822–9834. https://doi.org/10.3390/ijerph110909822
Wang X, Yan M, Zhao L, Wu Q, Wu C, Chang X, Zhou Z (2016) Low-dose methylmercury-induced apoptosis and mitochondrial DNA mutation in human embryonic neural progenitor cells. Oxidative Med Cell Longev 2016:5137042–5137010. https://doi.org/10.1155/2016/5137042
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95(2):351–358. https://doi.org/10.1016/0003-2697(79)90738-3
Joshi D, Kumar MD, Kumar SA, Sangeeta S (2014) Reversal of methylmercury-induced oxidative stress, lipid peroxidation, and DNA damage by the treatment of N-acetyl cysteine: a protective approach. J Environ Pathol Toxicol Oncol 33(2). https://doi.org/10.1615/jenvironpatholtoxicoloncol.2014010291
Pal M, Ghosh M (2012) Prophylactic effect of alpha-linolenic acid and alpha-eleostearic acid against MeHg induced oxidative stress, DNA damage and structural changes in RBC membrane. Food Chem Toxicol 50(8):2811–2818. https://doi.org/10.1016/j.fct.2012.05.038
Lu TH, Hsieh SY, Yen CC, Wu HC, Chen KL, Hung DZ, Chen CH, Wu CC, Su YC, Chen YW, Liu SH, Huang CF (2011) Involvement of oxidative stress-mediated ERK1/2 and p38 activation regulated mitochondria-dependent apoptotic signals in methylmercury-induced neuronal cell injury. Toxicol Lett 204(1):71–80. https://doi.org/10.1016/j.toxlet.2011.04.013
Huang CF, Liu SH, Hsu CJ, Lin-Shiau SY (2011) Neurotoxicological effects of low-dose methylmercury and mercuric chloride in developing offspring mice. Toxicol Lett 201(3):196–204. https://doi.org/10.1016/j.toxlet.2010.12.016
Dickinson DA, Forman HJ (2002) Cellular glutathione and thiols metabolism. Biochem Pharmacol 64(5–6):1019–1026. https://doi.org/10.1016/s0006-2952(02)01172-3
Sarafian TA (1999) Methylmercury-induced generation of free radicals: biological implications. Met Ions Biol Syst 36:415–444
Berglund M, Åkesson A, Bjellerup P, Vahter M (2000) Metal–bone interactions. J Toxicol Lett 112:219–225. https://doi.org/10.1016/S0378-4274(99)00272-6
Nagashima K, Fujii Y, Tsukamoto T, Nukuzuma S, Satoh M, Fujita M, Fujioka Y, Akagi H (1995) Apoptotic process of cerebellar degeneration in experimental methylmercury intoxication of rats. J Acta Neuropathol 91(1):72–77. https://doi.org/10.1007/s004010050394
Ryter SW, Kim HP, Hoetzel A, Park JW, Nakahira K, Wang X, Choi AMJA, signaling r (2007) Mechanisms of cell death in oxidative stress. 9(1):49–89
Lopes Castro MM, Nascimento PC, Souza-Monteiro D, Santos SM, Arouck MB, Garcia VB, Araújo RF, de Araujo AA, Balbinot GS, Collares FM (2020) Blood oxidative stress modulates alveolar bone loss in chronically stressed rats. 21(10):3728
Argenta MA, Buriol TM, Hecke MB (2010) Metodologia para a obtenção de parâmetros físicos e geométricos do osso trabecular função de imagens de micro tomografia. In: XXXI Iberian-Latin-American Congress on Computational Methods in Engineering. pp. 15–18
Nanci A (1999) Content and distribution of noncollagenous matrix proteins in bone and cementum: relationship to speed of formation and collagen packing density. J Struct Biol 126(3):256–269. https://doi.org/10.1006/jsbi.1999.4137
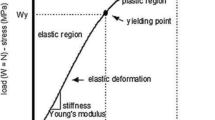
Silva A, Boyd S, Manske S, Alves J, de Carvalho J (2019) Assessment of the elastic properties of human vertebral trabecular bone using computational mechanical tests and x-ray microtomography—a subvolume analysis. J Biomed Phys Eng Express 5(4):045031. https://doi.org/10.1088/2057-1976/ab2c70
Sodek J, Mckee MD (2000) Molecular and cellular biology of alveolar bone. J Periodontol 24(1):99–126. https://doi.org/10.1034/j.1600-0757.2000.2240106.x
Fernandes MI, Gaio EJ, Oppermann RV, Rados PV, Rosing CK (2007) Comparison of histometric and morphometric analyses of bone height in ligature-induced periodontitis in rats. Braz Oral Res 21(3):216–221. https://doi.org/10.1590/S1806-83242007000300005
CHO MI, Garant PR (2000) Development and general structure of the periodontium. J Periodontol 24(1):9–27. https://doi.org/10.1034/j.1600-0757.2000.2240102.x
Funding
This work was supported by the Brazilian National Council for Scientific and Technological Development (CNPq), Fundação de Amparo a Pesquisa do Estado do Pará (FAPESPA), and Pró-Reitoria de Pesquisa e Pós-Graduação da UFPA (PROPESP, UFPA, Brazil).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures were previously approved by Ethics committee on animal experimentation by Federal University of Para (BIO 225-14-CEPAE-UFPA) following the guidelines suggested by NIH Guide to Care and Use of Laboratory Animals.
Competing Interest
The authors declare no conflicts of interest in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
de Oliveira Lopes, G., Aragão, W.A.B., Bittencourt, L.O. et al. Imaging Microstructural Damage and Alveolar Bone Loss in Rats Systemically Exposed to Methylmercury: First Experimental Evidence. Biol Trace Elem Res 199, 3707–3717 (2021). https://doi.org/10.1007/s12011-020-02492-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-020-02492-2