Abstract
Purpose of Review
This review will focus on the most common co-inhibitory molecules, emphasizing the importance of these in relation to rheumatic disease.
Recent Findings
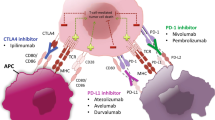
Checkpoint molecules are pivotal in determining the outcome of antigen activation. Checkpoint molecules consist of co-stimulatory and co-inhibitory molecules, where the first activates and the latter inhibits the antigen presentation process. Studies show that increased activity of co-inhibitory molecules is associated with a good prognosis in rheumatic diseases. Opposite, when cancer patients are treated with antibodies blocking the inhibitory pathways, autoimmune diseases, including arthritis, develop as immune-related adverse events (IrAE). This emphasizes the importance of these pathways in autoimmune disease.
Summary
Co-inhibitory molecules are becoming increasingly interesting as future treatment targets in rheumatic conditions. Treatments with antibodies blocking these pathways result in IrAE, often manifesting as autoimmune rheumatic diseases. Therefore, a need to get acquainted with these molecules is growing so we can cope with future challenges in rheumatic diseases.




Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Liang SC, Latchman YE, Buhlmann JE, Tomczak MF, Horwitz BH, Freeman GJ, et al. Regulation of PD-1, PD-L1, and PD-L2 expression during normal and autoimmune responses. Eur J Immunol. 2003;33:2706–16.
Mueller DL. Mechanisms maintaining peripheral tolerance. Nat Immunol. 2009;11:21–7.
Chen L, Flies DB. Molecular mechanisms of T cell co-stimulation and co-inhibition. Nat Rev Immunol. 2013;13:227–42.
Wherry EJ, Kurachi M. Molecular and cellular insights into T cell exhaustion. Nat Rev Immunol. 2015;15:486–99.
McKinney EF, Lee JC, Jayne DRW, Lyons PA, Smith KGC. T cell exhaustion, co-stimulation and clinical outcome in autoimmunity and infection. Nature. 2015;523:612–6.
Blank CU, Haining WN, Held W, et al. Defining “T cell exhaustion.”. Nat Rev Immunol. 2019;19:665–74 1–10. This paper provides a thorough discussion of the term “T cell exhaustion.”.
Yi JS, Cox MA, Zajac AJ. T cell exhaustion: characteristics, causes and conversion. Immunology. 2010;129:474–81.
Frasca D, Diaz A, Romero M, Blomberg BB. Human peripheral late/exhausted memory B cells express a senescent-associated secretory phenotype and preferentially utilize metabolic signaling pathways. EXG. 2017;87:113–20.
Salimzadeh L, Le Bert N, Dutertre C-A, et al. PD-1 blockade partially recovers dysfunctional virus–specific B cells in chronic hepatitis B infection. J Clin Invest. 2018;128:4573–87 This study provides a thorough description of PD-1’s role in B cell exhaustion.
Allahmoradi E, Taghiloo S, Tehrani M, Hossein-Nattaj H, Janbabaei G, Shekarriz R, et al. CD4+ T cells are exhausted and show functional defects in chronic lymphocytic leukemia. Iran J Immunol. 2017;14:257–69.
McKinney E, Lyons P, Lee J, Jayne D, Smith KGC. Making treatment personal: measurement of exhaustion to target treatment in autoimmunity, infection, and vaccination. Lancet. 2014;383:S12.
McKinney DEF, Lee J, Lyons PA, Rayner TF, Carr EJ, Hatton A, et al. Signatures of CD4 T cell help and CD8 exhaustion predict clinical outcome in autoimmunity, infection, and vaccination. Lancet. 2013;381:S74.
Zhang R, Li H, Bai L, Duan J. Association between T cell immunoglobulin and mucin domain 3 (TIM-3) genetic polymorphisms and susceptibility to autoimmune diseases. Immunol Investig. 2019;48:563–76.
Lin S-C, Kuo C-C, Chan C-H. Association of a BTLA gene polymorphism with the risk of rheumatoid arthritis. J Biomed Sci. 2006;13:853–60.
Oki M, Watanabe N, Owada T, Oya Y, Ikeda K, Saito Y, et al. A functional polymorphism in B and T lymphocyte attenuator is associated with susceptibility to rheumatoid arthritis. Clin Dev Immunol. 2011;2011:305656–8.
Zou Y, Zhang Z, Liu Y, Liu D, Xu W. Are programmed cell death 1 gene polymorphisms correlated with susceptibility to rheumatoid arthritis? Medicine (Baltimore). 2017;96:e7805–7.
Walker EJ, Hirschfield GM, Xu C, Lu Y, Liu X, Lu Y, et al. CTLA4/ICOS gene variants and haplotypes are associated with rheumatoid arthritis and primary biliary cirrhosis in the Canadian population. Arthritis Rheum. 2009;60:931–7.
Kailashiya V, Sharma HB, Kailashiya J. Role of CTLA4 A49G polymorphism in systemic lupus erythematosus and its geographical distribution. J Clin Pathol. 2019;72:659–62.
Kubo S, Saito K, Hirata S, Fukuyo S, Yamaoka K, Sawamukai N, et al. Abatacept inhibits radiographic progression in patients with rheumatoid arthritis: a retrospective analysis of 6 months of abatacept treatment in routine clinical practice. The ALTAIR study. Mod Rheumatol. 2013;24:42–51.
Walunas TL, Lenschow DJ, Bakker CY, Linsley PS, Freeman GJ, Green JM, et al. CTLA-4 can function as a negative regulator of T cell activation. Immunity. 1994;1:405–13.
Krummel MF, Allison JP. Pillars article: CD28 and CTLA-4 have opposing effects on the response of T cells to stimulation. The journal of experimental medicine. 1995. 182: 459-465. J Immunol. 2011;187:3459–65.
Jago CB, Yates J, Olsen Saraiva Camara N, Ri L, Lombardi G. Differential expression of CTLA-4 among T cell subsets. Clin Exp Immunol. 2004;136:463–71.
Cao J, Zou L, Luo P, Chen P, Zhang L. Increased production of circulating soluble co-stimulatory molecules CTLA-4, CD28 and CD80 in patients with rheumatoid arthritis. Int Immunopharmacol. 2012;14:585–92.
Wong CK, Lit LCW, Tam LS, Li EK, Lam CWK. Aberrant production of soluble costimulatory molecules CTLA-4, CD28, CD80 and CD86 in patients with systemic lupus erythematosus. Rheumatology (Oxford). 2005;44:989–94.
Hebbar M, Jeannin P, Magistrelli G, Hatron PY, Hachulla E, Devulder B, et al. Detection of circulating soluble CD28 in patients with systemic lupus erythematosus, primary Sjogren’s syndrome and systemic sclerosis. Clin Exp Immunol. 2004;136:388–92.
Hashkes GG. Abatacept in the treatment of polyarticular JIA: development, clinical utility, and place in therapy. DDDT. 2011;5:61–70.
Noisette A, Hochberg M. Abatacept for the treatment of adults with psoriatic arthritis: patient selection and perspectives. PTT. 2018;8:31–9.
Khanna D, Spino C, Johnson S, et al. Abatacept in early diffuse cutaneous systemic sclerosis: results of a phase II investigator-initiated, multicenter, double-blind, randomized, placebo-controlled trial. Arthritis Rheum. 2019;72:125–36.
Pimentel-Quiroz VR, Ugarte-Gil MF, Alarcón GS. Abatacept for the treatment of systemic lupus erythematosus. Expert Opin Investig Drugs. 2016;25:493–9.
Yang JC, Hughes M, Kammula U, Royal R, Sherry RM, Topalian SL, et al. Ipilimumab (anti-CTLA4 antibody) causes regression of metastatic renal cell cancer associated with enteritis and hypophysitis. J Immunother. 2007;30:825–30.
Johnson DB, Sullivan RJ, Ott PA, Carlino MS, Khushalani NI, Ye F, et al. Ipilimumab therapy in patients with advanced melanoma and preexisting autoimmune disorders. JAMA Oncol. 2016;2:234–40.
Ramos-Casals M, Brahmer JR, Callahan MK, Chavez AF, Keegan N, Khamashta MA, et al. Immune-related adverse events of checkpoint inhibitors. Nat Rev Disease Primers. 2020;6:38 1–21.
Postow MA, Sidlow R, Hellmann MD. Immune-related adverse events associated with immune checkpoint blockade. N Engl J Med. 2018;378:158–68.
Kostine M, Finckh A, Bingham CO 3rd, et al. EULAR points to consider for the diagnosis and management of rheumatic immune-related adverse events due to cancer immunotherapy with checkpoint inhibitors. Ann Rheum Dis. 2020;80(1):36–48 217139–13. This paper provides a thorough discussion of treating patients with immune-related adverse events.
Montastruc F, Renoux C, Dell’Aniello S, Simon TA, Azoulay L, Hudson M, et al. Abatacept initiation in rheumatoid arthritis and the risk of cancer: a population-based comparative cohort study. Rheumatology (Oxford). 2018;58:683–91.
Mercer LK, Askling J, Raaschou P, Dixon WG, Dreyer L, Hetland ML, et al. Risk of invasive melanoma in patients with rheumatoid arthritis treated with biologics: results from a collaborative project of 11 European biologic registers. Ann Rheum Dis. 2017;76:386–91.
Dougados M, Soubrier M, Antunez A, et al. Prevalence of comorbidities in rheumatoid arthritis and evaluation of their monitoring: results of an international, cross-sectional study (COMORA). Ann Rheum Dis. 2013;73:62–8.
Keir ME, Butte MJ, Freeman GJ, Sharpe AH. PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol. 2008;26:677–704.
Gato-Cañas M, Zuazo M, Arasanz H, et al. PDL1 signals through conserved sequence motifs to overcome interferon-mediated cytotoxicity. Cell Rep. 2017;20:1818–29.
Lecis D, Sangaletti S, Colombo MP, Chiodoni C. Immune checkpoint ligand reverse signaling: looking back to go forward in cancer therapy. Cancers. 2019;11:624–13.
You W, Shang B, Sun J, Liu X, Su L, Jiang S. Mechanistic insight of predictive biomarkers for antitumor PD-1/PD-L1 blockade: a paradigm shift towards immunome evaluation (review). Oncol Rep. 2020;44:424–37.
Xiao Y, Yu S, Zhu B, et al. RGMb is a novel binding partner for PD-L2 and its engagement with PD-L2 promotes respiratory tolerance. J Exp Med. 2014;3:81.
Greisen SR, Kragstrup TW, Thomsen JS, et al. Programmed death ligand 2 - a link between inflammation and bone loss in rheumatoid arthritis. J Transl Autoimmun. 2020;3:100028.
Sharpe AH, Pauken KE. The diverse functions of the PD1 inhibitory pathway. Nat Rev Immunol. 2018;18:153–67.
Peled M, Tocheva AS, Sandigursky S, Nayak S, Philips EA, Nichols KE, et al. Affinity purification mass spectrometry analysis of PD-1 uncovers SAP as a new checkpoint inhibitor. Proc Natl Acad Sci U S A. 2018;115:E468–77.
Jubel JM, Barbati ZR, Burger C, Wirtz DC, Schildberg FA. The role of PD-1 in acute and chronic infection. Front Immunol. 2020;11:79–15.
Zehn D, Wherry EJ. Immune memory and exhaustion: clinically relevant lessons from the LCMV model. In: Crossroads between innate and adaptive immunity V. Cham: Springer International Publishing; 2015. p. 137–52.
Dai S, Jia R, Zhang X, Fang Q, Huang L. Cellular immunology. Cell Immunol. 2014;290:72–9.
Francisco LM, Sage PT, Sharpe AH. The PD-1 pathway in tolerance and autoimmunity. Immunol Rev. 2010;236:219–42.
Greisen S, Rasmussen T, Stengaard-Pedersen K, Hetland M, Horslev-Petersen K, Hvid M, et al. Increased soluble programmed death-1 (sPD-1) is associated with disease activity and radiographic progression in early rheumatoid arthritis. Scand J Rehabil Med. 2013;43:101–8.
Yang L, Qiao G, Hassan Y, Li Z, Zhang X, Kong H, et al. Program death-1 suppresses autoimmune arthritis by inhibiting Th17 response. Arch Immunol Ther Exp. 2016;64:417–23.
Nielsen C, Ohm-Laursen L, Barington T, Husby S, Lillevang ST. Alternative splice variants of the human PD-1 gene. Cell Immunol. 2005;235:109–16.
Hirahara S, Katsumata Y, Kawasumi H, Kawaguchi Y, Harigai M. Serum levels of soluble programmed cell death protein 1 and soluble programmed cell death protein ligand 2 are increased in systemic lupus erythematosus and associated with the disease activity. Lupus. 2020;56:096120332091651–11.
Liu C, Jiang J, Gao L, Wang X, Hu X, Wu M, et al. Soluble PD-1 aggravates progression of collagen-induced arthritis through Th1 and Th17 pathways. Arthritis Res Ther. 2015;17:340 1–13.
Jalali S, Price-Troska T, Paludo J, Villasboas J, Kim H-J, Yang Z-Z, et al. Soluble PD-1 ligands regulate T cell function in Waldenstrom macroglobulinemia. Blood Adv. 2018;2:1985–97.
Greisen SR, Yan Y, Hansen AS, Venø MT, Nyengaard JR, Moestrup SK, et al. Extracellular vesicles transfer the receptor programmed death-1 in rheumatoid arthritis. Front Immunol. 2017;8:e1694–14.
Pauken KE, Dougan M, Rose NR, Lichtman AH, Sharpe AH. Adverse events following cancer immunotherapy: obstacles and opportunities. Trends Immunol. 2019;40:511–23.
Liao W, Zheng H, Wu S, Zhang Y, Wang W, Zhang Z, et al. The systemic activation of programmed death 1-PD-L1 axis protects systemic lupus erythematosus model from nephritis. Am J Nephrol. 2017;46:371–9.
Stefanski AL, Wiedemann A, Reiter K, Hiepe F, Lino AC, Dörner T. Enhanced programmed death 1 and diminished programmed death ligand 1 up-regulation capacity of post-activated lupus B cells. Arthritis Rheum. 2019;71:1539–44.
Wilde B, Hua F, Dolff S, Jun C, Cai X, Specker C, et al. Aberrant expression of the negative costimulator PD-1 on T cells in granulomatosis with polyangiitis. Rheumatology. 2012;51:1188–97.
Paluch C, Santos AM, Anzilotti C, Cornall RJ, Davis SJ. Immune checkpoints as therapeutic targets in autoimmunity. Front Immunol. 2018;9:711.
Lui Y, Davis SJ. LAG-3: a very singular immune checkpoint. Nat Immunol. 2018;19:1278–9.
Casati C, Camisaschi C, Rini F, Arienti F, Rivoltini L, Triebel F, et al. Soluble human LAG-3 molecule amplifies the in vitro generation of type 1 tumor-specific immunity. Cancer Res. 2006;66:4450–60.
Andreae S, Buisson S, Triebel F. MHC class II signal transduction in human dendritic cells induced by a natural ligand, the LAG-3 protein (CD223). Blood. 2003;102:2130–7.
Li N, Jilisihan B, Wang W, Tang Y, Keyoumu S. Soluble LAG3 acts as a potential prognostic marker of gastric cancer and its positive correlation with CD8+T cell frequency and secretion of IL-12 and INF-γ in peripheral blood. CBM. 2018;23:341–51.
Fougeray S, Brignone C, Triebel F. A soluble LAG-3 protein as an immunopotentiator for therapeutic vaccines: preclinical evaluation of IMP321. Vaccine. 2006;24:5426–33.
Narayanan S, Ahl PJ, Bijin VA, Kaliaperumal N, Lim SG, Wang C-I, et al. LAG3 is a central regulator of NK cell cytokine production. bioRxiv. 2020;2020:2020013192800.
Cook KD, Whitmire JK. LAG-3 confers a competitive disadvantage upon antiviral CD8+ T cell responses. J Immunol. 2016;197:119–27.
Nakachi S, Sumitomo S, Tsuchida Y, Tsuchiya H, Kono M, Kato R, et al. Interleukin-10-producing LAG3+ regulatory T cells are associated with disease activity and abatacept treatment in rheumatoid arthritis. Arthritis Res Ther. 2017;19:97–108.
Chen S-Y, Hsu W-T, Chen Y-L, Chien C-H, Chiang B-L. Lymphocyte-activation gene 3+ (LAG3+) forkhead box protein 3- (FOXP3-) regulatory T cells induced by B cells alleviates joint inflammation in collagen-induced arthritis. J Autoimmun. 2016;68:75–85.
Kato R, Sumitomo S, Tsuchida Y, et al. CD4+CD25+LAG3+ T cells with a feature of Th17 cells associated with systemic lupus erythematosus disease activity. Front Immunol. 2019;10:716–0.
Puhr HC, Ilhan-Mutlu A. New emerging targets in cancer immunotherapy: the role of LAG3. ESMO Open. 2019;4:e000482–6.
Angin M, Brignone C, Triebel F. A LAG-3-specific agonist antibody for the treatment of T cell-induced autoimmune diseases. J Immunol. 2020;204:810–8 This paper shows the effects of LAG-3 agonistic in delayed-type hypersensitivity.
Zhu C, Anderson AC, Schubart A, Xiong H, Imitola J, Khoury SJ, et al. The Tim-3 ligand galectin-9 negatively regulates T helper type 1 immunity. Nat Immunol. 2005;6:1245–52.
Cao E, Zang X, Ramagopal UA, Mukhopadhaya A, Fedorov A, Fedorov E, et al. T cell immunoglobulin mucin-3 crystal structure reveals a galectin-9-independent ligand-binding surface. Immunity. 2007;26:311–21.
Chiba S, Baghdadi M, Akiba H, Yoshiyama H, Kinoshita I, Dosaka-Akita H, et al. Tumor-infiltrating DCs suppress nucleic acid–mediated innate immune responses through interactions between the receptor TIM-3 and the alarmin HMGB1. Nat Immunol. 2012;13:832–42.
Huang Y-H, Zhu C, Kondo Y, et al. CEACAM1 regulates TIM-3-mediated tolerance and exhaustion. Nature. 2014;517:386–90.
Banerjee H, Kane LP. Immune regulation by Tim-3. F1000Res. 2018;7:316–9.
Koohini Z, Hossein-Nataj H, Mobini M, Hosseinian-Amiri A, Rafiei A, Asgarian-Omran H. Analysis of PD-1 and Tim-3 expression on CD4+ T cells of patients with rheumatoid arthritis; negative association with DAS28. Clin Rheumatol. 2018;37(8):2063–71 1–9.
Li S, Peng D, He Y, Zhang H, Sun H, Shan S, et al. Expression of TIM-3 on CD4+ and CD8+ T cells in the peripheral blood and synovial fluid of rheumatoid arthritis. APMIS. 2014;122:899–904.
Song L, Wang Y, Sui Y, Sun J, Li D, Li G, et al. High interleukin-37 (IL-37) expression and increased mucin-domain containing-3 (TIM-3) on peripheral T cells in patients with rheumatoid arthritis. Med Sci Monit. 2018;24:5660–7.
Jiao Q, Qian Q, Zhao Z, Fang F, Hu X, An J, et al. Expression of human T cell immunoglobulin domain and mucin-3 (TIM-3) and TIM-3 ligands in peripheral blood from patients with systemic lupus erythematosus. Arch Dermatol Res. 2016;308:553–61.
Guo L, Yang X, Xia Q, Zhen J, Zhuang X, Peng T. Expression of human T cell immunoglobulin domain and mucin-3 (TIM-3) on kidney tissue from systemic lupus erythematosus (SLE) patients. Clin Exp Med. 2013;14:383–8.
Jin L, Bai R, Zhou J, Shi W, Xu L, Sheng J, et al. Association of serum T cell immunoglobulin domain and mucin-3 and interleukin-17 with systemic lupus erythematosus. Med Sci Monit Basic Res. 2018;24:168–76.
Martinet L, Smyth MJ. Balancing natural killer cell activation through paired receptors. Nat Rev Immunol. 2015;15:243–54.
Rotte A, Jin JY, Lemaire V. Mechanistic overview of immune checkpoints to support the rational design of their combinations in cancer immunotherapy. Ann Oncol. 2018;29:71–83.
Lupo KB, Matosevic S. CD155 immunoregulation as a target for natural killer cell immunotherapy in glioblastoma. J Hematol Oncol. 2020;13:76 1–10.
Zhao W, Dong Y, Wu C, Ma Y, Jin Y, Ji Y. TIGIT overexpression diminishes the function of CD4 T cells and ameliorates the severity of rheumatoid arthritis in mouse models. Exp Cell Res. 2016;340:132–8.
Luo Q, Deng Z, Xu C, Zeng L, Ye J, Li X, et al. Elevated Expression of immunoreceptor tyrosine-based inhibitory motif (TIGIT) on T lymphocytes is correlated with disease activity in rheumatoid arthritis. Med Sci Monit. 2017;23:1232–41.
Luo Q, Li X, Fu B, et al. Decreased expression of TIGIT in NK cells correlates negatively with disease activity in systemic lupus erythematosus. Int J Clin Exp Pathol. 2018;11:2408–18.
Mao L, Hou H, Wu S, Zhou Y, Wang J, Yu J, et al. TIGIT signalling pathway negatively regulates CD4 + T cell responses in systemic lupus erythematosus. Immunology. 2017;151:280–90.
Liu S, Sun L, Wang C, et al. Treatment of murine lupus with TIGIT-Ig. Clin Immunol. 2019;203:72–80 This paper shows the effects of TIGIT in an animal model for Lupus.
Schorer M, Rakebrandt N, Lambert K, Hunziker A, Pallmer K, Oxenius A, et al. TIGIT limits immune pathology during viral infections. Nat Commun. 2020;11:1288 1–14.
Cai G, Freeman GJ. The CD160, BTLA, LIGHT/HVEM pathway: a bidirectional switch regulating T cell activation. Immunol Rev. 2009;229:244–58.
Yang B, Huang Z, Feng W, Wei W, Zhang J, Liao Y, et al. The expression of BTLA was increased and the expression of HVEM and LIGHT were decreased in the T cells of patients with rheumatoid arthritis [corrected]. PLoS One. 2016;11:e0155345.
Shang Y-J, Cui Q-F, Li J-L, Guo G-N, Zhu W-Y. Expression of the costimulatory molecule BTLA in synovial tissues from rheumatoid arthritis patients. Xi Bao Yu Fen Zi Mian Yi Xue Za Zhi. 2012;28:643–6.
Shang Y, Guo G, Cui Q, Li J, Ruan Z, Chen Y. The expression and anatomical distribution of BTLA and its ligand HVEM in rheumatoid synovium. Inflammation. 2012;35:1102–12.
Oster C, Wilde B, Specker C, Sun M, Kribben A, Witzke O, et al. BTLA Expression on Th1, Th2 and Th17 effector T-cells of patients with systemic lupus erythematosus is associated with active disease. IJMS. 2019;20:4505.
Sawaf M, Fauny J-D, Felten R, Sagez F, Gottenberg J-E, Dumortier H, et al. Defective BTLA functionality is rescued by restoring lipid metabolism in lupus CD4+ T cells. JCI Insight. 2018;3:413.
Werner K, Dolff S, Dai Y, Ma X, Brinkhoff A, Korth J, et al. The co-inhibitor BTLA is functional in ANCA-associated vasculitis and suppresses Th17 cells. Front Immunol. 2019;10:2843.
Wang J, Wu G, Manick B, Hernandez V, Renelt M, Erickson C, et al. VSIG-3 as a ligand of VISTA inhibits human T cell function. Immunology. 2019;156:74–85.
Ceeraz S, Eszterhas SK, Sergent PA, Armstrong DA, Ashare A, Broughton T, et al. VISTA deficiency attenuates antibody-induced arthritis and alters macrophage gene expression in response to simulated immune complexes. Arthritis Res Ther. 2017;19:270–13.
Han X, Vesely MD, Yang W, et al. PD-1H (VISTA)-mediated suppression of autoimmunity in systemic and cutaneous lupus erythematosus. Sci Transl Med. 2019;11:eaax1159.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This article does not contain any studies with human or animal subjects performed by any of the authors.
Conflict of Interest
The authors declare no conflict of interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This Article is part of the Topical Collection on Pediatric Rheumatology
Rights and permissions
About this article
Cite this article
Greisen, S.R., Deleuran, B. Checkpoint Molecules in Rheumatology—or the Benefits of Being Exhausted. Curr Rheumatol Rep 23, 22 (2021). https://doi.org/10.1007/s11926-021-00991-2
Accepted:
Published:
DOI: https://doi.org/10.1007/s11926-021-00991-2