Abstract
Purpose of Review
Fibromyalgia Syndrome (FMS) is a complex chronic pain condition characterized by widespread musculoskeletal pain and numerous other debilitating symptoms. The purpose of this review is to provide a comprehensive overview, based on everyday clinical practice, of the drugs presently employed in the treatment of FMS.
Recent Findings
The treatment of FMS is based on a multimodal approach, with pharmacologic treatment being an essential pillar. The drugs used include tricyclic antidepressants, serotonin and noradrenaline reuptake inhibitors, other antidepressants, anticonvulsants, myorelaxants, and analgesics. The effectiveness of these medications varies, and the choice of drug often depends on the specific symptoms presented by the patient. Many drugs tend to either address only some domains of the complex FMS symptomatology or have a limited effect on pain.
Summary
Each treatment option comes with potential side effects and risks that necessitate careful consideration. It may be beneficial to divide patients into clinical subpopulations, such as FMS with comorbid depression, for more effective treatment. Despite the complexities and challenges, the pharmacological treatment remains a crucial part for the management of FMS. This review aims to guide clinicians in prescribing pharmacological treatment to individuals with FMS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
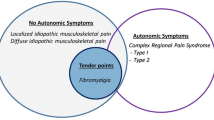
Fibromyalgia syndrome (FMS) is a complex chronic pain condition. It's characterized by widespread musculoskeletal pain, profound fatigue, sleep disturbances, and numerous other symptoms affecting various organs and systems. These include dysautonomias, regional pain syndromes, and mood disturbances [1]. The latest diagnostic criteria have placed increased emphasis on non-musculoskeletal symptoms [2, 3], which are almost always present among patients, varying in number and severity [4].
The treatment of FMS is based on a multimodal approach to better address the array of symptoms experienced by patients. Pharmacologic treatment forms a crucial part of this approach. While it's often insufficient alone to control the complex symptoms of this syndrome, it can provide satisfactory results for some patients [4]. Three drugs, pregabalin, duloxetine, and milnacipran, have been FDA-approved for FMS treatment. Currently, no drugs are EMA-approved for this condition, making any drug use for FMS off-label. This review offers an overview of the drugs used in FMS treatment. While many of these drugs primarily serve as analgesics, it's crucial for clinicians to always bear in mind the nociplastic origin of FMS pain when prescribing pharmacological treatment to individuals with fibromyalgia [5].
Pharmacological Treatment: General Aspects
FMS is a complex condition influenced by both peripheral and central factors [6]. Peripheral factors include an inflammatory environment and possibly autoantibodies against satellite glial cells [7]. Central factors involve altered neurotransmitter levels and brain activity in pain processing regions, highlighting central sensitivity's importance [8,9,10,11]. Effective FMS drugs mainly target the central nervous system (CNS), like antidepressants and anticonvulsants (Table 1). However, these treatments often fall short. Analgesics and non-steroidal anti-inflammatory drugs (NSAIDs) have proven ineffective, tricyclic antidepressants have limited effects, while duloxetine, milnacipran, and pregabalin have shown promise [12]. Data have not changed much since then, although there are some novelties.
Prescribing medication for FMS is complex, and should follow the principle of "start low and go slow." Patients should discern between disease symptoms and medication side effects. Using multiple medications can address FMS's complex nature, and using symptom assessment scales like the Fibromyalgia Assessment Status (FAS) can monitor symptom intensity [13]. Management typically requires a multimodal approach, extending beyond medication use alone.
The following sections analyze various medications studied and commonly used in clinical practice.
Antidepressants
The effectiveness of antidepressant drugs in treating chronic pain syndromes is now well-established. The type of chronic pain is important in this setting, since antidepressants are especially recommended for chronic primary pain syndromes [14, 15], the class to which FMS belongs to. However, no study reported high certainty evidence about the effects of antidepressants for pain, and for fibromyalgia just a moderate certainty exists, which has still to be interpreted with caution since many studies are tied to industries [16].
There are various types of antidepressant drugs each distinguished by their mechanism of action. A detailed description of each class would be useful.
Tricyclic Antidepressants
Tricyclic antidepressants (TCAs) work by inhibiting noradrenaline and serotonin reuptake in the CNS, with some, like amitriptyline, also blocking voltage-gated sodium channels. This dual action is key to their success in treating pain. Amitriptyline, at 25 mg, has been found more effective than alternatives such as pregabalin and duloxetine in reducing pain intensity in FMS patients [17]. Despite this, studies on amitriptyline are older and involve fewer participants. Systematic reviews suggest it's more effective in treating sleep disturbances, fatigue, and improving quality of life compared to duloxetine and pregabalin [18], but not with a reduction in depressive symptoms [19]. Daily dosages for FMS pain management are lower than for depression treatment, suggesting serotonin-norepinephrine reuptake inhibitors may be better for patients with both FMS and depression. However, evidence still lack in this regard and reviews regarding TCA use for FMS remain inconclusive [16].
Monoamine Oxidase Inhibitors
Monoamine oxidase (MAO) inhibitors, used in treating Parkinson's disease and depression, have been sparingly studied for FMS. Early studies showed that the second-generation MAO-A inhibitor, Moclobemide, didn't show significant analgesic activity in FMS compared to Amitriptyline or placebo [20, 21]. Another MAO-A inhibitor, Pirlindole, improved pain but didn't affect other symptoms, like asthenia or sleep quality [22]. Nonetheless, the evidence is still inconclusive.
Selective Serotonin Reuptake Inhibitors (SSRIs)
SSRIs have been used for FMS treatment, but studies and reviews show inconsistent results [23]. Some found SSRIs significantly improved pain, sleep, depression, and quality of life [18]. However, a Cochrane meta-analysis and another review suggested that SSRIs are not superior to a placebo for primary FMS symptoms [16, 24].
Overall, it should be considered that serotonin has a bivalent activity on pain, with an alternate predominance of pronociceptive or antinociceptive effects, according to often unpredictable conditions [25]. For this reason, SSRI should not be considered as first line drugs for the treatment of depression in FMS.
Serotonin and Noradrenaline Reuptake Inhibitors (SNRIs)
Currently, SNRIs are the most used drugs for FMS, with moderate efficacy evidence [16]. A meta-analysis showed 42% of SNRI-treated patients reported a 30% pain reduction, compared to 32% on a placebo [18]. However, nonresponders to SNRIs, particularly duloxetine, remain common. A study on 59 patients and 30 healthy controls found that nonresponders to SNRIs are characterized by less favorable metabolic parameters and comorbid depression and other psychiatric conditions [26]; however, it has been underlined by recent meta-analyses that duloxetine is most effective with FMS comorbid with depression [27].
Duloxetine, FDA-approved for FMS treatment, works by inhibiting serotonin and noradrenaline reuptake. Studies indicate a daily 120 mg dose improves pain and depression significantly [19]. Lower doses (30 mg) were less effective than pregabalin 450 mg and not superior to a placebo [17]. Higher doses (120 mg) are more effective but have more side effects, especially in cases with comorbid depression. Duloxetine's pain reduction effectiveness is independent of its mood effects and presence of major depressive disorders, but is more effective in FMS with depression [28]. Despite higher effective doses reported, we recommend starting with 30 mg daily, increasing dosage every two weeks.
Milnacipran, an SNRI with greater selectivity for norepinephrine, FDA-approved for FMS, shows promising improvements in pain, well-being, physical function, and fatigue at 100 mg and 200 mg per day dosages [29]. It also improves well-being and pain in FMS, excluding sleep quality, regardless of depression [30]. However, recent research indicates limited effectiveness in alleviating FMS symptoms [31]. Recommended dosage is 100 mg daily, starting with 12.5 mg and gradually increasing.
Other Antidepressants
Trazodone is a Serotonin Antagonist and Reuptake Inhibitor (SARI) that acts as an antagonist of 5HT2a and 5HT2c serotonin receptors and inhibits serotonin reuptake [32]. At lower doses, it has hypnotic and anxiolytic effects [33], and has been used for FMS treatment. Trazodone (50-300 mg/day), alone or combined with pregabalin, notably improved sleep, reduced anxiety, depression, and Fibromyalgia Impact Questionnaire (FIQ) scores [34, 35]. However, 21.1% of patients reported tachycardia. In combination with pregabalin, it was better tolerated and improved FMS severity, depression, and pain.
Reboxetine, a Noradrenaline Reuptake Inhibitor (NRI), shows promise for chronic pain relief due to its selective noradrenaline activity. It has been reported to reduce musculoskeletal pain in patients with depression, independent of mood improvements [36]. Studies suggest that esreboxetine, reboxetine's active enantiomer, improves pain, fatigue, and FIQ scores at a 4 mg/day dosage [37]. A comparison study found no significant differences between reboxetine and amitriptyline in treating FMS symptoms [38].
Mirtazapine increases the release of serotonin and norepinephrine without inhibiting their reuptake. It has shown mixed results in FMS treatment. While some studies indicate improvements in pain, sleep disturbances, and quality of life [39,40,41], others suggest it's less effective than duloxetine [42]. A Cochrane review found mirtazapine may be useful for addressing FMS symptoms, but the evidence quality was low [43]. Adverse effects are common, and dosage adjustments may be needed to manage drowsiness.
Anticonvulsants: Pregabalin and Gabapentin
Anticonvulsants like pregabalin and gabapentin, known as α2δ ligands, can impact nociception by modulating neuronal excitability [44]. They regulate calcium channels and therefore neurotransmitter release, including glutamate, noradrenaline, serotonin, dopamine, and substance P [45]. They may benefit FMS patients with neuropathic pain and psychiatric symptoms.
Pregabalin has shown effectiveness for FMS treatment and is FDA-approved. Studies found that a 450 mg/day dosage significantly reduced pain and improved sleep quality and fatigue [46]. This dosage's benefits on pain have been consistently confirmed [17]. A recent analysis found pregabalin 600 mg to be more effective for sleep and depression, while 150 mg primarily addressed fatigue and sleep but had no effect on pain [19]. Some patients on very low dosages (50 or 75 mg) for years experience low efficacy and long-term side effects, especially in patients with retinal nerve fiber layer damage [47]. A study found duloxetine 30-60 mg more effective than pregabalin 75-150 mg for FMS patients with depression [48]. Another study showed pregabalin had modest efficacy in pain relief, overall assessment, and function at 450 mg/day, and improved sleep at all dose levels but didn't provide consistent benefit at 300 and 600 mg/day [49]. The side effects of pregabalin, which increase with dosage, include dizziness, drowsiness, weight gain, and peripheral edema. It is recommended to initiate pregabalin treatment with a small dose (25–75 mg) to increase weekly. A controlled-release (CR) formulation of pregabalin, which can be administered once a day, is also an option [50].
Gabapentin showed analgesic activity in conditions with chronic neuropathic pain but results for FMS are limited [51]. Two randomized controlled trials (RCTs) investigating the use of gabapentin in FMS have been conducted, as analyzed in a Cochrane review; the reduction in pain was significantly greater in the gabapentin group (1200–2400 mg daily) compared to the placebo group [52]. However, this is based on low-quality evidence from a single trial. An extended-release gabapentin formulation improved pain and sleep in a small study of FMS patients [53]. In clinical practice, patients should begin with a low single dose of gabapentin (100–300 mg) before bedtime, and additional doses at breakfast and lunch after one week, followed by a predominantly evening dose increment. Adverse events associated with gabapentin are similar to those of pregabalin and include drowsiness, dizziness, fatigue, and weight gain.
NMDR Antagonists
FMS is associated with increased N-methyl-D-aspartate receptor (NMDAR) activity, suggesting the potential of NMDAR modulation as a therapeutic intervention [54]. Ketamine, a non-competitive NMDAR antagonist administered intravenously, has been studied for its potential use in FMS treatment. In some studies, FMS patients receiving ketamine showed a progressive reduction in pain intensity during the infusion [55] and at 15 min post-infusion [56]. However, long-term analgesic effects of ketamine in FMS appear to be limited, potentially due to its pharmacokinetics [57]. Though single, low-dose, intravenous ketamine infusions provided only short-term reductions in self-reported pain intensity, higher doses and longer, more frequent infusions may offer better pain relief and more extended analgesia as suggested by two case studies [58, 59]. Despite the promise, it's crucial to monitor potential side effects including psychomimetic, gastrointestinal, and cardiovascular impacts. Further research is currently underway to understand the potential of ketamine in FMS treatment [60].
Myorelaxants
Cyclobenzaprine, a muscle relaxant structurally similar to amitriptyline, has shown moderate effectiveness in FMS, with improvements in symptoms, particularly sleep quality [61]. Studies also report enhancements in sleep, fatigue, pain, and mood with very low-dose cyclobenzaprine (1–4 mg) taken at bedtime [62]. A recent trial with a sublingual formulation (TNX-102 SL, 5.6 mg final dose) showed improvements in daily pain, sleep quality, and FIQR by week 14 [63]. Common side effects include oral hypoesthesia and oral paresthesia, but can also cause nausea, weakness, constipation, and neurovegetative symptoms. Due to these side effects, dosage titration is important.
Tizanidine is a muscle relaxant with sedative properties (centrally acting alpha-2-adrenergic agonist). Considering the presence of α2-adrenergic receptors on the spinal synapse, where their activation cause inhibition of glutamate release, it is likely that tizanidine also has analgesic properties. Its effectiveness in FMS has been scarcely studied, but a trial involving 30 patients showed its potential in improving tender points and fatigue [64]. It may benefit patients with significant myofascial pain [65].
Analgesics
Limited, low-quality evidence suggests NSAIDs are not effective for FMS treatment [66]. They may be used in mixed-type pain cases alongside traditional fibromyalgia medications.
Opioids
Opioids can help manage chronic pain but may lead to tolerance, dependency, and side effects like constipation and sedation. Studies show decreased μ-opioid receptor availability in FMS, less improvement in pain-related interference with daily life (compared to tramadol), likelihood of opioid-induced hyperalgesia, and risk of opioid use disorder [67,68,69, 70]. Long-term opioid use can cause endocrine changes [71] and higher 10-year all-cause mortality rates [72]. Despite guidelines are against opioid analgesic use, they are often prescribed for FMS due to a lack of alternative treatments [73]. Their use should be considered only when all other pharmacological and non-pharmacological therapies have failed, or in low doses in combination with medications having a different mechanism of action. Cannabinoids should be preferred to opioids (see below).
Tramadol, a weak opioid and norepinephrine and serotonin reuptake inhibitor, showed efficacy in four randomized controlled trials for fibromyalgia treatment. A study found that tramadol at a dosage of 37.5 mg in combination with paracetamol significantly improved pain scores and FIQ results in comparison to a placebo group [74]. A systematic review with meta-analysis confirmed its positive effect on pain and quality of life in fibromyalgia patients [75]. In addition, the addictive potential of tramadol appears limited [76]. However, the quality of evidence in these studies was "low", and no significant improvements in depression or sleep quality were observed. In summary, the benefit-to-risk profiles of tramadol appears favourable, making tramadol a valuable consideration for managing cases of FMS where there is a significant pain component interfering with quality of life, or as an emergency ("SOS") medication in such scenarios.
Tapentadol, a centrally acting analgesic with dual action as a μ-opioid receptor agonist and a noradrenaline reuptake inhibitor, has potential for treating fibromyalgia due to its unique properties [77]. It offers similar analgesic effects to conventional opioids but with fewer side effects, although it does have a higher abuse potential than tramadol [78]. There is limited literature reporting its use in FMS patients. A study showed that it enhances conditioned pain modulation in a subpopulation of fibromyalgia patients, indicating increased endogenous pain inhibition [79]. Ideal dosages range from 50 to 250 mg twice daily for severe chronic pain, particularly with a prevalent neuropathic pain component [77, 80].
GABAergic Drugs
GABA receptors, GABAa and GABAb, play a role in hyperpolarization and ion regulation [81]. GABAa receptors are ligand-gated ion channels selectively permeable to chloride ions, that entering inside the cell cause hyperpolarization. GABAb receptors are G-protein coupled receptors, with inhibitory effect on calcium current and activation of potassium current. GABAa are ligand-gated chloride channels, while GABAb are GTP-binding protein-coupled receptors and regulate K + and Ca2 + channels. Benzodiazepines, allosteric modulators of GABAa receptors, have been used for anxiety, sleep enhancement, and muscle relaxation. Although there is no conclusive evidence against these medications in the treatment of FMS due to lack of data [82, 83], recent clinical guidelines for FMS discourage their use due to their potentially harmful adverse effects [83], especially in combination with opioids [84]. As a result, their use is recommended just as add-on therapy. Short-acting benzodiazepines may help with initial insomnia. Non-benzodiazepine sedative-hypnotic medications, like zopiclone and zolpidem, can enhance sleep and alleviate fatigue. GABAb receptor is mostly concentrated in the spinal cord, and its agonists like baclofen and sodium oxybate have been used for motor neuron diseases and sleep disturbances. They showed effects on sleep, decreasing sleep onset latency and increasing slow wave sleep, in disorders like fibromyalgia [85].
Antipsychotic Medications
There is some evidence that antipsychotic medications could be useful for FMS. Quetiapine, an antagonist at serotonin 5-HT2a and Dopamine D2 receptors, functions as a hypnotic at low doses (50 mg), an antidepressant at intermediate doses (300 mg), and an antipsychotic at high doses [86]. Its metabolite, norquetiapine, inhibits norepinephrine transporters and antagonizes α2 and 5-HT7 receptors [87]. Quetiapine, given in 25–100 mg daily doses, reduced stiffness and fatigue but not pain in FMS patients in one study [88]. A randomized, placebo-controlled study found it improved sleep but not other symptoms [89]. When used for patients with both depression and FMS, it significantly improved depression, pain, and quality of life [90], but less effectively than amitriptyline [91]. It may alleviate pain, sleep problems, depression, and anxiety in FMS patients with depression, but side effects like weight gain should be considered [92]. Use is suggested for FMS patients with major depression or persistent symptoms from depression/anxiety.
There is some evidence suggesting antipsychotics like olanzapine may help alleviate FMS symptoms, particularly alongside depression, but their use is limited by side effects such as weight gain and somnolence, which led some patients to discontinue treatment [93]. However, these findings are from older studies and further research is needed to confirm their effectiveness and safety [94].
Cannabis and Cannabinoids
Cannabis sativa contains cannabinoids like THC and CBD that interact with specific receptors in the nervous and immune systems [95] and has been used to manage pain and other symptoms, like sleep [96]. Δ9-tetrahydrocannabinol (THC or Δ9-THC) has psychoactive effects [97] while cannabidiol (CBD) lacks psychoactive effects but demonstrated efficacy in addressing a wide range of conditions [98, 99], including chronic pain [100], Current research investigates both the whole plant and isolated cannabinoids (THC and CBD). Regarding isolated cannabinoids, [101], including two randomized controlled trials, concluded that there is no compelling, high-quality evidence to support the use of nabilone, a synthetic cannabinoid equivalent to THC, in treating FMS patients. Dronabinol, another form of synthetic THC, was evaluated in FMS patients with neuropathic pain [102]. Results showed a significant reduction in pain intensity and depression, leading to an improved quality of life, but only in patients able to tolerate the treatment (with an abandonment rate of about 25%) [102].
In terms of medical cannabis (MC), an observational study indicated reduced pain intensity from using cannabis preparations. An observational study, spanning six months and involving 367 FMS patients using MC preparations, revealed a reduction in the average pain intensity, while a small randomized placebo-controlled clinical study suggested THC-rich cannabis oil could help reduce symptoms and improve quality of life in FMS patients [103, 104]. In a recent publication, a prospective cohort study involving 30 women diagnosed with FMS demonstrated a significant improvement in various aspects of quality of life, including general quality of life, general health, physical health, and psychological well-being, after 30 days of cannabis treatment [105]. These findings suggest a potentially significant role for cannabis in the treatment of FMS, particularly in cases resistant to other treatments. Early cannabis treatment may lead to short-term benefits, improving quality of life by addressing pain, sleep, and physical and psychological well-being, although further studies are necessary to understand its potential and long-term impact. In particular, side effects include impacts on the central nervous system, psychological effects, vision, psychiatric issues, gastrointestinal problems, somnolence, diarrhea, psychological distress, and more [106]. Evidence supports avoidance of cannabis during adolescence and early adulthood, in people prone to or with mental health disorders, in pregnancy and before and while driving [106].
Discussion and Treatment Guidelines
In the realm of FMS treatment, it has become increasingly clear that a solely pharmacological approach is not sufficient. The best results are achieved with a multidisciplinary approach, considering the complex and multifaceted nature of FMS. Various non-pharmacological therapies have been researched and tested, including balneotherapy [107], hyperbaric oxygen [107], and acupuncture [108] among others. However, while these treatments can be beneficial, pharmacological therapy remains a crucial component in managing fibromyalgia and achieving satisfactory outcomes.
The treatment of FMS and associated symptoms demands a personalized approach (Table 1). It should prioritize the use of antidepressants and anticonvulsants while generally excluding strong opioids, with specific exceptions for weak opioids like tapentadol and tramadol. It is imperative that pharmacological therapy be integrated within a multidisciplinary framework, aligning with the bio-psychosocial model, and complemented by physical and psychological interventions. Table 2 summarizes the main drugs used for FMS treatment and their initial and final dosages.
Furthermore, it's important to note that the efficacy of current FMS treatments is limited. To advance research in the field, there is a pressing need to develop new molecules and evaluate them in comprehensive, long-term comparative studies involving larger patient populations. While monotherapy would be the ideal therapeutic approach for FMS, it is often insufficient. Although combination therapies are commonly employed in clinical practice, there is a lack of substantial evidence supporting their actual benefit in FMS management. For instance, combinations involving drugs like pregabalin and antidepressants or amitriptyline have been studied in only a few trials. Given the limited effectiveness of monotherapy and the prevalent use of drug combinations, further well-designed prospective randomized clinical trials are necessary to explore the potential additive or synergistic effects of specific drug combinations tailored to individual patient needs (Table 1). This comprehensive, multidisciplinary approach is essential to addressing the complex nature of FMS.
High-quality evidence supports the effectiveness of several interventions in the management of fibromyalgia [27]. Cognitive-behavioral therapy demonstrates a short-term reduction in pain. Additionally, central nervous system depressants and antidepressants have shown benefits in pain management in the medium term. Similarly, antidepressants exhibit favorable results for improving the quality of life in the short term. However, it is worth noting that these improvements, while statistically significant, do not exceed the minimum clinically important change, which is 14 points on a 101-point scale for quality of life. Notably, evidence for long-term outcomes of these interventions is currently insufficient.
Further developments could arise from recognizing the heterogeneity of FMS as a factor limiting the effectiveness of pharmacological treatments. The existence of subgroups of FMS patients has been suggested by numerous studies, but most randomized controlled trials and studies on pathophysiology have not considered this variability factor, comparing the average results in the overall population of FMS patients. Analyzing the specific pathophysiological mechanisms of various patient subgroups could help identify drugs with a mechanism of action more targeted to the process that has led to the development of the disease. Help in this regard could come from recent studies on the polymorphism of genes for serotoninergic and dopaminergic system receptors, potentially useful for developing pharmacological strategies based on patient genotype.
The recognition that both biological (especially at the central nervous system level) and psychological and behavioral alterations are involved in the onset and maintenance of FMS suggests that, in addition to the use of symptomatic drugs, both cognitive-behavioral psychotherapy and appropriate physical exercise should be provided. The alliance between the patient and the doctor in identifying realistically achievable objectives with currently available therapeutic methods is a fundamental part of FMS treatment.
Conclusions
In conclusion, there are currently various pharmacological options for FMS, including antidepressants, anticonvulsants, NMDA antagonists, myorelaxants, opioids, tramadol, tapentadol, benzodiazepines, antipsychotics, and cannabis. While all these drugs have demonstrated some benefits, the extent of these benefits is often limited. Specifically, they tend to either address only some domains of the complex FMS symptomatology or have a limited effect on pain. Additionally, it may be beneficial to divide patients into clinical subpopulations, such as FMS with comorbid depression, for more effective treatment. Furthermore, each treatment option comes with potential side effects and risks that necessitate careful consideration. It's crucial for future research to establish their effectiveness and safety profiles more definitively.
The hope of finding a way to cure the pain and other symptoms of FMS is still a dream, and we currently accept the view that a combination of pharmacological and non-pharmacological treatments is the best way to manage FMS. Hence, future studies should focus on identifying the best combination of pharmacological and non-pharmacological treatments to best address the different subgroups of patients.
Data Availability
No datasets were generated or analysed during the current study.
References
Arnold LM, Bennett RM, Crofford LJ, Dean LE, Clauw DJ, Goldenberg DL, et al. AAPT diagnostic criteria for fibromyalgia. J Pain. 2019;20:611–28. Available from: https://doi.org/10.1016/j.jpain.2018.10.008.
Wolfe F, Clauw DJ, Fitzcharles MA, Goldenberg DL, Häuser W, Katz RS, et al. Fibromyalgia criteria and severity scales for clinical and epidemiological studies: a modification of the ACR preliminary diagnostic criteria for fibromyalgia. J Rheumatol. 2011;38:1113–22.
Wolfe F, Clauw DJ, Fitzcharles MA, Goldenberg DL, Häuser W, Katz RL, et al. Revisions to the 2010, 2011 fibromyalgia diagnostic criteria. Semin Arthritis Rheum. 2016;46:319–29. Available from: https://doi.org/10.1016/j.semarthrit.2016.08.012.
Sarzi-Puttini P, Giorgi V, Atzeni F, Gorla R, Kosek E, Choy EH, et al. Fibromyalgia position paper. Clin Exp Rheumatol. 2021 May-Jun;39 Suppl 130(3):186-193. https://doi.org/10.55563/clinexprheumatol/i19pig.
Sandström A, Ellerbrock I, Löfgren M, Altawil R, Bileviciute-Ljungar I, Lampa J, et al. Distinct aberrations in cerebral pain processing differentiating patients with fibromyalgia from patients with rheumatoid arthritis. Pain. 2022;163:538. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8832547/
Sarzi-puttini P, Giorgi V, Marotto D, Atzeni F. Fibromyalgia: an update on clinical characteristics, aetiopathogenesis and treatment. Nat Rev Rheumatol. 2020;16:645–660. Available from: https://doi.org/10.1038/s41584-020-00506-w.
Krock E, Morado-Urbina CE, Menezes J, Hunt MA, Sandström A, Kadetoff D, et al. Fibromyalgia patients with elevated levels of anti-satellite glia cell immunoglobulin G antibodies present with more severe symptoms. Pain. 2023;164:1828–40. Available from: https://pubmed.ncbi.nlm.nih.gov/36943275/. This article is important because it presents pioneering research indicating that a subset of fibromyalgia patients have elevated levels of anti-SGC antibodies, which could potentially pave the way for personalized treatment options targeting these autoantibodies.
Jensen KB, Loitoile R, Kosek E, Petzke F, Carville S, Fransson P, et al. Patients with fibromyalgia display less functional connectivity in the brain’s pain inhibitory network. Mol Pain. 2012;8:32. https://doi.org/10.1186/1744-8069-8-32.
Ellingsen DM, Beissner F, Moher Alsady T, Lazaridou A, Paschali M, Berry M, et al. A picture is worth a thousand words: linking fibromyalgia pain widespreadness from digital pain drawings with pain catastrophizing and brain cross-network connectivity. Pain. 2021;162:1352–63. Available from: https://pubmed.ncbi.nlm.nih.gov/33230008/.
Russell IJ, Orr MD, Littman B, Vipraio GA, Alboukrek D, Michalek JE, et al. Elevated cerebrospinal fluid levels of substance P in patients with the fibromyalgia syndrome. Arthritis Rheum. 1994;37:1593–601. Available from: http://www.ncbi.nlm.nih.gov/pubmed/7526868.
Amin OA, Abouzeid SM, Ali SA, Amin BA, Alswat KA. Clinical association of vitamin D and serotonin levels among patients with fibromyalgia syndrome. Neuropsychiatr Dis Treat. 2019;15:1421–6. Available from: https://www.tandfonline.com/action/journalInformation?journalCode=dndt20.
Häuser W, Walitt B, Fitzcharles MA, Sommer C. Review of pharmacological therapies in fibromyalgia syndrome. Arthritis Res Ther. 2014;16:1–10. Available from: https://arthritis-research.biomedcentral.com/articles/10.1186/ar4441.
Salaffi F, Di Carlo M, Farah S, Atzeni F, Buskila D, Ablin JN, et al. Diagnosis of fibromyalgia: comparison of the 2011/2016 ACR and AAPT criteria and validation of the modified fibromyalgia assessment status. Rheumatology (Oxford). 2020;59:3042–3049. Available from: http://www.ncbi.nlm.nih.gov/pubmed/32206792.
Carville S, Constanti M, Kosky N, Stannard C, Wilkinson C. Chronic pain (primary and secondary) in over 16s: summary of NICE guidance. BMJ. 2021;373. Available from: https://www.bmj.com/content/373/bmj.n895.
Zis P, Daskalaki A, Bountouni I, Sykioti P, Varrassi G, Paladini A. Depression and chronic pain in the elderly: links and management challenges. Clin Interv Aging. 2017;12:709–20. Available from: https://www.dovepress.com/depression-and-chronic-pain-in-the-elderly-links-and-management-challe-peer-reviewed-fulltext-article-CIA.
Ferreira GE, Abdel-Shaheed C, Underwood M, Finnerup NB, Day RO, McLachlan A, et al. Efficacy, safety, and tolerability of antidepressants for pain in adults: overview of systematic reviews. BMJ. 2023;380. Available from: https://www.bmj.com/content/380/bmj-2022-072415.
Alberti FF, Becker MW, Blatt CR, Ziegelmann PK, da Silva Dal Pizzol T, Pilger D. Comparative efficacy of amitriptyline, duloxetine and pregabalin for treating fibromyalgia in adults: an overview with network meta-analysis. Clin Rheumatol. 2022;41:1965–78. Available from: https://pubmed.ncbi.nlm.nih.gov/35347488/. This article is significant as it provides a comprehensive evaluation of the efficacy of three different drugs in reducing pain intensity in fibromyalgia patients, offering critical insights for clinical decision-making and patient management.
Häuser W, Wolfe F, Tölle T, Uçeyler N, Sommer C. The role of antidepressants in the management of fibromyalgia syndrome: a systematic review and meta-analysis. CNS Drugs. 2012;26:297–307. Available from: http://link.springer.com/10.2165/11598970-000000000-00000.
Farag HM, Yunusa I, Goswami H, Sultan I, Doucette JA, Eguale T. Comparison of amitriptyline and US food and drug administration–approved treatments for fibromyalgia: a systematic review and network meta-analysis. JAMA Netw Open. 2022;5:e2212939–e2212939. Available from: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2792390.
Yavuzer G, Kapakdeveci A, Arasil T, Elhan A. Moclobemid treatment in primary fibromyalgia syndrome. Eur J Phys Med Rehabil. 1998. Available from: https://www.epistemonikos.org/fr/documents/968fb76a30214a96e7b822b212423f60eb17c8aa.
Hannonen P, Malminiemi K, Yli-Kerttula U, Isomeri R, Roponen P. A randomized, double-blind, placebo-controlled study of moclobemide and amitriptyline in the treatment of fibromyalgia in females without psychiatric disorder. Br J Rheumatol. 1998;37:1279–86. Available from: https://pubmed.ncbi.nlm.nih.gov/9973149/.
Ginsberg F, Joos E, Géczy J, Bruhwyler J, Vandekerckhove K, Famaey JP. A pilot randomized placebo-controlled study of pirlindole in the treatment of primary fibromyalgia. J Musculoskelet Pain. 1998;6:5–17. https://doi.org/10.2165/11595410-000000000-00000.
Calandre EP, Rico-Villademoros F, Slim M. An update on pharmacotherapy for the treatment of fibromyalgia. Expert Opin Pharmacother. 2015;16:1347–68.
Walitt B, Urrútia G, Nishishinya MB, Cantrell SE, Häuser W. Selective serotonin reuptake inhibitors for fibromyalgia syndrome. Cochrane Database Syst Rev. 2015;2015. Available from: https://pubmed.ncbi.nlm.nih.gov/26046493/.
Liu X, Wang G, Ai G, Xu X, Niu X, Zhang M. Selective ablation of descending serotonin from the rostral ventromedial medulla unmasks its pro-nociceptive role in chemotherapy-induced painful neuropathy. J Pain Res. 2020;13:3081–94. Available from: https://pubmed.ncbi.nlm.nih.gov/33262643/.
Krupa AJ, Korkosz M, Gorostowicz A, Nowakowski J, Kierzkowska I, Dudek D, et al. Predictors of treatment response to serotonin and noradrenaline reuptake inhibitors in fibromyalgia. Pol Arch Intern Med. 2023;133:16432–16432. Available from: https://europepmc.org/article/med/36799096. This article is important as it uncovers the associations between insulin resistance, psychiatric comorbidities, and treatment response to SNRIs in patients with fibromyalgia, providing essential insights for personalized patient treatment.
Mascarenhas RO, Souza MB, Oliveira MX, Lacerda AC, Mendonça VA, Henschke N, et al. Association of therapies with reduced pain and improved quality of life in patients with fibromyalgia: a systematic review and meta-analysis. JAMA Intern Med. 2021;181:104–12. Available from: https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2772354.
Arnold LM, Lu Y, Crofford LJ, Wohlreich M, Detke MJ, Iyengar S, et al. A double-blind, multicenter trial comparing duloxetine with placebo in the treatment of fibromyalgia patients with or without major depressive disorder. Arthritis Rheum. 2004;50:2974–84. Available from: http://doi.wiley.com/10.1002/art.20485.
Clauw DJ, Mease P, Palmer RH, Gendreau RM, Wang Y. Milnacipran for the treatment of fibromyalgia in adults: a 15-week, multicenter, randomized, double-blind, placebo-controlled, multiple-dose clinical trial. Clin Ther. 2008;30:1988–2004. Available from: https://pubmed.ncbi.nlm.nih.gov/19108787/.
Arnold LM, Palmer RH, Gendreau RM, Chen W. Relationships among pain, depressed mood, and global status in fibromyalgia patients: post hoc analyses of a randomized, placebo-controlled trial of milnacipran. Psychosomatics. 2012;53:371–9. Available from: https://pubmed.ncbi.nlm.nih.gov/22677218/.
Pickering G, Macian N, Delage N, Picard P, Cardot J-M, Sickout-Arondo S, et al. Milnacipran poorly modulates pain in patients suffering from fibromyalgia: a randomized double-blind controlled study. Drug Des Devel Ther. 2018;12:2485–96. Available from: https://www.dovepress.com/milnacipran-poorly-modulates-pain-in-patients-suffering-from-fibromyal-peer-reviewed-article-DDDT.
Stahl SM. Mechanism of action of trazodone: a multifunctional drug. CNS Spectr. 2009;14:536–46. Available from: https://www.cambridge.org/core/journals/cns-spectrums/article/abs/mechanism-of-action-of-trazodone-a-multifunctional-drug/336DB6B060471BA6C675337CC8AA637C.
Khouzam HR. A review of trazodone use in psychiatric and medical conditions. Postgrad Med. 2017;129:140–8. Available from: https://www.tandfonline.com/doi/abs/10.1080/00325481.2017.1249265.
Morillas-Arques P, Ma Rodriguez-Lopez C, Molina-Barea R, Rico-Villademoros F, Calandre EP. Trazodone for the treatment of fibromyalgia: An open-label, 12-week study. BMC Musculoskelet Disord. 2010;11:1–6. Available from: https://bmcmusculoskeletdisord.biomedcentral.com/articles/10.1186/1471-2474-11-204.
Calandre EP, Morillas-Arques P, Molina-Barea R, Rodriguez-Lopez CM, Rico-Villademoros F. Trazodone plus pregabalin combination in the treatment of fibromyalgia: a two-phase, 24-week, open-label uncontrolled study. BMC Musculoskelet Disord. 2011;12:95. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3112435/.
Krell HV, Leuchter AF, Cook IA, Abrams M. Evaluation of reboxetine, a noradrenergic antidepressant, for the treatment of fibromyalgia and chronic low back pain. Psychosomatics. 2005;46:379–84.
Arnold LM, Hirsch I, Sanders P, Ellis A, Hughes B. Safety and efficacy of esreboxetine in patients with fibromyalgia: a fourteen-week, randomized, double-blind, placebo-controlled, multicenter clinical trial. Arthritis Rheum. 2012;64:2387–97. https://doi.org/10.1002/art.34390.
Konuk N, Ortancil O, Bostanci B, Kiran S, Sapmaz P. A comparison of reboxetine and amitryptilline in the treatment of fibromyalgia syndrome with co-morbid depressive symptoms: an open-label preliminary study. Klin Psikofarmakol Bülteni-Bull Clin Psychopharmacol. 2010;20:29–37. https://doi.org/10.1080/10177833.2010.11790631.
Yeephu S, Suthisisang C, Suttiruksa S, Prateepavanich P, Limampai P, Russell IJ. Efficacy and safety of mirtazapine in fibromyalgia syndrome patients: a randomized placebo-controlled pilot study. Ann Pharmacother. 2013 Jul-Aug;47(7-8):921-32. https://doi.org/10.1345/aph.1R725.
Miki K, Murakami M, Oka H, Onozawa K, Yoshida S, Osada K. Efficacy of mirtazapine for the treatment of fibromyalgia without concomitant depression: a randomized, double-blind, placebo-controlled phase IIa study in Japan. Pain. 2016;157:2089. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4988084/.
Suttiruksa S, Yeephu S, Prateepavanich P, Suthisisang C. Effects of mirtazapine on quality of life of Thai patients with fibromyalgia syndrome: a double-blind, randomized, placebo-controlled trial. Asian Biomed. 2016;10:435–45.
Mehta P, Basu A, Ahmed S. Effectiveness and adverse effects of the use of mirtazapine as compared to duloxetine for fibromyalgia: real-life data from a retrospective cohort. Rheumatol Int. 2022;42:1549–54. Available from: https://link.springer.com/article/10.1007/s00296-022-05135-y.
Welsch P, Bernardy K, Derry S, Moore RA, Häuser W. Mirtazapine for fibromyalgia in adults. Cochrane Database Syst Rev. 2018. https://doi.org/10.1002/14651858.CD012708.pub2.
Stahl SM, Porreca F, Taylor CP, Cheung R, Thorpe AJ, Clair A. The diverse therapeutic actions of pregabalin: is a single mechanism responsible for several pharmacological activities? Trends Pharmacol Sci. 2013;34:332–9. Available from: https://pubmed.ncbi.nlm.nih.gov/23642658/.
Malemud C. Focus on pain mechanisms and pharmacotherapy in the treatment of fibromyalgia syndrome. Clin Exp Rheumatol. 2009;27:S86–91.
Crofford LJ, Rowbotham MC, Mease PJ, Russell IJ, Dworkin RH, Corbin AE, et al. Pregabalin for the treatment of fibromyalgia syndrome: results of a randomized, double-blind, placebo-controlled trial. Arthritis Rheum. 2005;52:1264–73. https://doi.org/10.1002/art.20983.
Biçer GY, Zor KR, Biçer KE, Küçük E, Küçük EB. Can the long term using of pregabalin in fibromyalgia affect the choroid and retinal nerve fiber layer? Eye (Lond). 2022;36:2318–22. Available from: https://pubmed.ncbi.nlm.nih.gov/34857924/.
Bidari A, Moazen-Zadeh E, Ghavidel-Parsa B, Rahmani S, Hosseini S, Hassankhani A. Comparing duloxetine and pregabalin for treatment of pain and depression in women with fibromyalgia: an open-label randomized clinical trial. Daru. 2019;27:149–58. Available from: http://www.ncbi.nlm.nih.gov/pubmed/30877484.
Pauer L, Winkelmann A, Arsenault P, Jespersen A, Whelan L, Atkinson G, et al. An international, randomized, double-blind, placebo-controlled,phase III trial of pregabalin monotherapy in treatment of patients with fibromyalgia. J Rheumat. 2011;38:2643–52. Available from: https://pubmed.ncbi.nlm.nih.gov/21965636/.
Alciati A, Atzeni F, Masala IF, Cirillo M, Sciortino D, Perna G, et al. Controlled-release pregabalin in the treatment of fibromyalgia. Expert Rev Neurother. 2018;18:617–23. Available from: http://www.ncbi.nlm.nih.gov/pubmed/30092164.
Tong C, Zhengyao Z, Mei L, Dongpo S, Qian H, Fengqun M. Pregabalin and gabapentin in patients with spinal cord injury-related neuropathic pain: a network meta-analysis. Pain Ther. 2021;10:1497–509. Available from: https://link.springer.com/article/10.1007/s40122-021-00302-8.
Cooper TE, Derry S, Wiffen PJ, Moore RA. Gabapentin for fibromyalgia pain in adults. Cochrane Database of Systematic Reviews. John Wiley and Sons Ltd. 2017.
North JM, Hong K soo J, Rauck RL. The effect of a novel form of extended-release gabapentin on pain and sleep in fibromyalgia subjects: an open-label pilot study. Pain Pract. 2016;16:720–9. https://doi.org/10.1111/papr.12319.
Littlejohn G, Guymer E. Modulation of NMDA receptor activity in fibromyalgia. Biomedicines. 2017;5:15. Available from: https://www.mdpi.com/2227-9059/5/2/15/htm.
Graven-Nielsen T, Aspegren Kendall S, Henriksson KG, Bengtsson M, Sörensen J, Johnson A, et al. Ketamine reduces muscle pain, temporal summation, and referred pain in fibromyalgia patients. Pain. 2000;85:483–91.
Noppers I, Niesters M, Swartjes M, Bauer M, Aarts L, Geleijnse N, et al. Absence of long-term analgesic effect from a short-term S-ketamine infusion on fibromyalgia pain: a randomized, prospective, double blind, active placebo-controlled trial. Eur J Pain. 2011;15:942–9.
Pastrak M, Abd-Elsayed A, Ma F, Vrooman B, Visnjevac O. Systematic review of the use of intravenous ketamine for fibromyalgia. Ochsner J. 2021;21:387–94. Available from: https://www.ochsnerjournal.org/content/21/4/387.
Hanna AF, Smith AJ. Intravenous K-T relief in a patient with fibromyalgia. 2016. Available from: https://doi.org/10.4172/foa.1000104.
Sharma S, Gupta R. Outpatient ketamine infusions for the treatment of fibromyalgia and chronic pain syndrome: a case report. 2023.
Javorcikova Z, Dangoisse M, Nikis S, Lechat JP, Gillain A, Fils JF, et al. The place of S-ketamine in fibromyalgia treatment (ESKEFIB): study protocol for a prospective, single-center, double-blind, randomized, parallel-group, dose-escalation controlled trial. Trials. 2021;22:1–11. Available from: https://trialsjournal.biomedcentral.com/articles/10.1186/s13063-021-05814-4.
Tofferi JK, Jackson JL, O’Malley PG. Treatment of fibromyalgia with cyclobenzaprine: a meta-analysis. Arthritis Rheum. 2004;51:9–13. Available from: http://doi.wiley.com/10.1002/art.20076.
Moldofsky H, Harris HW, Tad Archambault W, Kwong T, Lederman S. Effects of bedtime very low dose cyclobenzaprine on symptoms and sleep physiology in patients with fibromyalgia syndrome: a double-blind randomized placebo-controlled study. J Rheumat. 2011;38:2653–63. Available from: https://pubmed.ncbi.nlm.nih.gov/21885490/.
Lederman S, Arnold LM, Vaughn B, Kelley M, Sullivan GM. Efficacy and safety of sublingual cyclobenzaprine for the treatment of fibromyalgia: results from a randomized, double-blind, placebo-controlled trial. Arthritis Care Res (Hoboken). 2023. Available from: https://doi.org/10.1002/acr.25142.
McLain D. An Open label dose finding trial of tizanidine [ZanaflexTM] for treatment of fibromyalgia. J Musculoskelet Pain. 2002;10:7–18. https://doi.org/10.1300/J094v10n04_02.
Desai MJ, Saini V, Saini S. Myofascial pain syndrome: a treatment review. Pain Ther. 2013;2:21–36. Available from: https://link.springer.com/article/10.1007/s40122-013-0006-y.
Derry S, Wiffen PJ, Häuser W, Mücke M, Tölle TR, Bell RF, et al. Oral nonsteroidal anti-inflammatory drugs for fibromyalgia in adults. Cochrane Database Syst Rev. 2017;2017. Available from: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD012332.pub2/full.
Harris RE, Clauw DJ, Scott DJ, McLean SA, Gracely RH, Zubieta J-K. Decreased central mu-opioid receptor availability in fibromyalgia. J Neurosci. 2007;27:10000–6. https://doi.org/10.1523/JNEUROSCI.2849-07.2007.
Peng X, Robinson RL, Mease P, Kroenke K, Williams DA, Chen Y, et al. Long-term evaluation of opioid treatment in fibromyalgia. Clin J Pain. 2015;31:7–13. Available from: https://journals.lww.com/clinicalpain/fulltext/2015/01000/long_term_evaluation_of_opioid_treatment_in.2.aspx.
Jackson D, Singh S, Zhang-James Y, Faraone S, Johnson B. The effects of low dose naltrexone on opioid induced hyperalgesia and fibromyalgia. Front Psychiatry. 2021;12. Available from: https://pubmed.ncbi.nlm.nih.gov/33664680/.
Hall OT, Teater J, Entrup P, Deaner M, Bryan C, Harte SE, et al. Fibromyalgia predicts increased odds of pain-related addiction exacerbation among individuals with pain and opioid use disorder. Pain. 2023;164:1801–9. Available from: https://journals.lww.com/pain/fulltext/2023/08000/fibromyalgia_predicts_increased_odds_of.17.aspx. This article is important because it provides the first evidence of fibromyalgia as a risk factor for pain-related exacerbation of opioid use disorder, and introduces a new, promising scale for measuring pain-related opioid use disorder exacerbation.
Diasso PDK, Abou-Kassem D, Nielsen SD, Main KM, Sjøgren P, Kurita GP. Long-term opioid treatment and endocrine measures in chronic non-cancer pain patients. Eur J Pain. 2023;27:940–51. https://doi.org/10.1002/ejp.1797.
Song IA, Choi HR, Oh TK. Long-term opioid use and mortality in patients with chronic non-cancer pain: ten-year follow-up study in South Korea from 2010 through 2019. EClinicalMedicine. 2022;51. Available from: http://www.thelancet.com/article/S2589537022002887/fulltext.
Rivera J, Vallejo MA. Fibromyalgia is associated to receiving chronic medications beyond appropriateness: a cross-sectional study. Rheumatol Int. 2016;36:1691–9. Available from: https://link.springer.com/article/10.1007/s00296-016-3568-2.
Bennett RM, Kamin M, Karim R, Rosenthal N. Tramadol and acetaminophen combination tablets in the treatment of fibromyalgia pain: a double-blind, randomized, placebo-controlled study. Am J Med. 2003;114:537–45.
da Rocha AP, Mizzaci CC, Nunes Pinto ACP, da Silva Vieira AG, Civile V, Trevisani VFM. Tramadol for management of fibromyalgia pain and symptoms: systematic review. Int J Clin Pract. 2020;74:e13455. https://doi.org/10.1111/ijcp.13455.
Cagle S, Bay D, Herndon C. What is the addictive potential of tramadol? Evidence-Based Pract. 2020;23:29–30. Available from: https://journals.lww.com/ebp/fulltext/2020/02000/what_is_the_addictive_potential_of_tramadol_.23.aspx.
Coluzzi F, Fornasari D, Pergolizzi J, Romualdi P. From acute to chronic pain: tapentadol in the progressive stages of this disease entity. Eur Rev Med Pharmacol Sci. 2017;21:1672–83.
FS Alshehri. Tapentadol: a review of experimental pharmacology studies, clinical trials, and recent findings. Drug Des Devel Ther. 2023;17:851–61 Available from: https://doi.org/10.2147/DDDT.S402362.
van de Donk T, van Velzen M, Dahan A, Niesters M. Cornea nerve fibre state determines analgesic response to tapentadol in fibromyalgia patients without effective endogenous pain modulation. Eur J Pain. 2019;23:1586–95. Available from: http://www.ncbi.nlm.nih.gov/pubmed/31162787.
de Tommaso M, Vecchio E, Nolano M. The puzzle of fibromyalgia between central sensitization syndrome and small fiber neuropathy: a narrative review on neurophysiological and morphological evidence. Neurol Sci. 2022;43:1667–84. Available from: https://link-springer-com.pros1.lib.unimi.it/article/10.1007/s10072-021-05806-x.
Watanabe M, Maemura K, Kanbara K, Tamayama T, Hayasaki H. GABA and GABA Receptors in the central nervous system and other organs. Int Rev Cytol. 2002;213:1–47.
Corrigan R, Derry S, Wiffen PJ, Moore RA. Clonazepam for neuropathic pain and fibromyalgia in adults. Cochrane Database Syst Rev. 2012;2017. https://doi.org/10.1002/14651858.CD009486.pub2.
Macfarlane GJ, Kronisch C, Dean LE, Atzeni F, Häuser W, Fluß E, et al. EULAR revised recommendations for the management of fibromyalgia. Ann Rheum Dis. 2017;76:318–28.
Peirce GL, Smith MJ, Abate MA, Halverson J. Doctor and pharmacy shopping for controlled substances. Med Care. 2012;50:494–500. Available from: https://pubmed.ncbi.nlm.nih.gov/22410408/.
A. Brown M, Guilleminault C. A review of sodium oxybate and baclofen in the treatment of sleep disorders. Curr Pharm Des. 2011;17:1430–5. Available from: https://pubmed.ncbi.nlm.nih.gov/21476957/.
Zhornitsky S, Potvin S, Moteshafi H, Dubreucq S, Rompré PP, Stip E. Dose-response and comparative efficacy and tolerability of quetiapine across psychiatric disorders: a systematic review of the placebo-controlled monotherapy and add-on trials. Int Clin Psychopharmacol. 2011;26:183–92. Available from: https://journals.lww.com/intclinpsychopharm/fulltext/2011/07000/dose_response_and_comparative_efficacy_and.1.aspx.
López-Muñoz F, Álamo C. Active metabolites as antidepressant drugs: the role of norquetiapine in the mechanism of action of quetiapine in the treatment of mood disorders. Front Psychiatry. 2013;4:48288. Available from: www.frontiersin.org.
Hidalgo J, Rico-Villademoros F, Calandre EP. An open-label study of quetiapine in the treatment of fibromyalgia. Prog Neuropsychopharmacol Biol Psychiatry. 2007;31:71–7.
Potvin S, Morin M, Cloutier C, Gendron A, Bissonnette A, Marchand S. Add-on treatment of quetiapine for fibromyalgia: a pilot, randomized, double-blind, placebo-controlled 12-week trial. J Clin Psychopharmacol. 2012;32:684–7. Available from: https://journals.lww.com/psychopharmacology/fulltext/2012/10000/add_on_treatment_of_quetiapine_for_fibromyalgia__a.16.aspx.
McIntyre A, Paisley D, Kouassi E, Gendron A. Quetiapine fumarate extended-release for the treatment of major depression with comorbid fibromyalgia syndrome: a double-blind, randomized, placebo-controlled study. Arthritis Rheumat. 2014;66:451–61. https://doi.org/10.1002/art.38228.
Calandre EP, Rico-Villademoros F, Galán J, Molina-Barea R, Vilchez JS, Rodriguez-Lopez CM, et al. Quetiapine extended-release (Seroquel-XR) versus amitriptyline monotherapy for treating patients with fibromyalgia: a 16-week, randomized, flexible-dose, open-label trial. Psychopharmacology (Berl). 2014;231:2525–31. Available from: https://pubmed.ncbi.nlm.nih.gov/24398824/.
Walitt B, Klose P, Üçeyler N, Phillips T, Häuser W. Antipsychotics for fibromyalgia in adults. Cochrane Database Syst Rev. John Wiley and Sons Ltd. 2016.
Freedenfeld RN, Murray M, Fuchs PN, Kiser RS. Decreased pain and improved quality of life in fibromyalgia patients treated with olanzapine, an atypical neuroleptic. Pain Pract. 2006;6:112–8. https://doi.org/10.1111/j.1533-2500.2006.00072.x.
Rico-Villademoros F, Hidalgo J, Dominguez I, García-Leiva JM, Calandre EP. Atypical antipsychotics in the treatment of fibromyalgia: a case series with olanzapine. Prog Neuropsychopharmacol Biol Psychiatry. 2005;29:161–4.
Grayson M. Cannabis. Nature. Outlook. 2015;525:2015.
Di Marzo V. New approaches and challenges to targeting the endocannabinoid system. Nat Rev Drug Discov. Nature Publishing Group; 2018. p. 623–39. Available from: https://pubmed.ncbi.nlm.nih.gov/30116049/.
Pertwee RG. The diverse CB 1 and CB 2 receptor pharmacology of three plant cannabinoids: Δ 9-tetrahydrocannabinol, cannabidiol and Δ 9-tetrahydrocannabivarin. Br J Pharmacol. 2008;153:199–215.
Irving PM, Iqbal T, Nwokolo C, Subramanian S, Bloom S, Prasad N, et al. A randomized, double-blind, placebo-controlled, parallel-group, pilot study of cannabidiol-rich botanical extract in the symptomatic treatment of ulcerative colitis. Inflamm Bowel Dis. 2018;24:714–24. Available from: https://pubmed.ncbi.nlm.nih.gov/29538683/.
Couch DG, Cook H, Ortori C, Barrett D, Lund JN, O’Sullivan SE. Palmitoylethanolamide and cannabidiol prevent inflammation-induced hyperpermeability of the human gut in vitro and in vivo-a randomized, placebo-controlled, double-blind controlled trial. Inflamm Bowel Dis. 2019;25:1006–18. Available from: https://pubmed.ncbi.nlm.nih.gov/31054246/.
Hohmann AG, Suplita RL. Endocannabinoid mechanisms of pain modulation. Drug Addict Basic Res Ther. 2008;8:737–64.
Walitt B, Klose P, Ma F, Phillips T, Häuser W. Cannabinoids for fibromyalgia (Review). Cochrane Database Syst Rev. 2016.
Weber J, Schley M, Casutt M, Gerber H, Schuepfer G, Rukwied R, et al. Tetrahydrocannabinol (Delta 9-THC) Treatment in chronic central neuropathic pain and fibromyalgia patients: results of a multicenter survey. Blanck TJJ, editor. Anesthesiol Res Pract. 2009;2009:827290. Available from: https://doi.org/10.1155/2009/827290.
Sagy I, Bar-Lev Schleider L, Abu-Shakra M, Novack V. Safety and efficacy of medical cannabis in fibromyalgia. J Clin Med. 2019;8:807.
Chaves C, Bittencourt PCT, Pelegrini A. Ingestion of a THC-rich cannabis oil in people with fibromyalgia: a randomized, double-blind, placebo-controlled clinical trial. Pain Med. 2020 [cited 2021 Jan 12];21:2212–8. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7593796/report=abstract.
Hershkovich O, Hayun Y, Oscar N, Shtein A, Lotan R. The role of cannabis in treatment-resistant fibromyalgia women. Pain Pract. 2023;23:180–4. Available from: https://pubmed.ncbi.nlm.nih.gov/36333278/.
Solmi M, De Toffol M, Kim JY, Choi MJ, Stubbs B, Thompson T, et al. Balancing risks and benefits of cannabis use: umbrella review of meta-analyses of randomised controlled trials and observational studies. BMJ. 2023;382:44. Available from: https://www.bmj.com/content/382/bmj-2022-072348.
Cao C, Li Q, Zhang X, Varrassi G, Wang H. Effectiveness of hyperbaric oxygen for fibromyalgia: a meta-analysis of randomized controlled trials. Clin Pract. 2023;13:583–95. Available from: https://pubmed.ncbi.nlm.nih.gov/37218804/.
Almutairi NM, Hilal FM, Bashawyah A, Al Dammas F, Yamak Altinpulluk E, Hou J De, et al. Efficacy of acupuncture, intravenous lidocaine, and diet in the management of patients with fibromyalgia: a systematic review and network meta-analysis. Healthcare (Basel). 2022;10. Available from: https://pubmed.ncbi.nlm.nih.gov/35885703/.
Funding
No funds, grants, or other support was received.
Author information
Authors and Affiliations
Contributions
V.G., P.S.P. wrote the introduction and manuscript text and prepared the table. G.P., S.S., and F.A. helped conducting the literature review. A.A., R.T., G.V. contributed to the discussion. G.V. helped with the construction of the table. G.V., D.F., S.C. and S.F.B. edited and reviewed the manuscript for important intellectual content. All authors reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
VG received funding from Dompè farmaceutici in the last 6 months. The other authors declare no competing interests.
Human and Animal Rights
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Giorgi, V., Sarzi-Puttini, P., Pellegrino, G. et al. Pharmacological Treatment of Fibromyalgia Syndrome: A Practice-Based Review. Curr Pain Headache Rep (2024). https://doi.org/10.1007/s11916-024-01277-9
Accepted:
Published:
DOI: https://doi.org/10.1007/s11916-024-01277-9