Abstract
The optimal management of patients with low-grade glioma (LGG) is controversial. The controversy largely stems from the lack of well-designed clinical trials with adequate follow-up to account for the relatively long progression-free survival and overall survival of patients with LGG. Nonetheless, the literature increasingly suggests that expectant management is no longer optimal. Rather, there is mounting evidence supporting active management including consideration of surgical resection, radiotherapy, chemotherapy, molecular and histopathologic characterization, and use of modern imaging techniques for monitoring and prognostication. In particular, there is growing evidence favoring extensive surgical resection and increasing interest in the role of chemotherapy (especially temozolomide) in the management of these tumors. In this review, we critically analyze emerging trends in the literature with respect to management of LGG, with particular emphasis on reports published during the past year.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Despite their initially indolent nature, low-grade gliomas (LGGs) may cause considerable morbidity and inevitably lead to death. Whereas expectant management once was acceptable and the norm, current trends and mounting evidence now favor more active management, including consideration of surgical resection, radiotherapy, chemotherapy, molecular and histopathologic characterization, and use of modern imaging techniques for monitoring and prognostication. Some of these changes have gained significant momentum and support, whereas others remain investigational and controversial. In this review, we critically analyze emerging trends in the literature with respect to management of LGGs, with particular emphasis on reports published during the past year.
Definition and Epidemiology
The term LGG technically includes all World Health Organization (WHO) grade I and II gliomas. However, this broad grouping contains tumors that are clinically, histologically, and molecularly diverse. For example, the management of WHO grade I gliomas is dramatically different from that of WHO grade II gliomas, the former being amenable to surgical cure while the role of surgery for the latter is still being justified. Therefore, in the context of this review, LGG refers only to WHO grade II diffuse astrocytomas, oligodendrogliomas, and oligoastrocytomas, all of which have similar invasive and malignant potential. Approximately 2,000 to 3,000 LGGs are diagnosed in the United States every year, accounting for nearly 15% of all primary brain tumors. Peak incidence occurs in people between 35 and 44 years of age, and there is an increased prevalence among white people and men [1]. Despite a preponderance of astrocytomas, there has been an increasing diagnosis and/or incidence of pure oligodendrogliomas and mixed oligoastrocytomas in recent years [2]. Low-grade astrocytomas have a predilection for “secondary” functional areas, such as the supplementary motor area and the insular lobe, whereas oligodendrogliomas are seen most commonly along the convexity in subcortical areas, particularly in the frontal lobe [3].
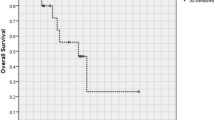
The patient’s presenting symptoms and imaging characteristics are critical guides for management. Seizure is the most common presenting symptom, occurring in up to 80% of patients [4]. Other less common modes of presentation include headache, lethargy, and personality changes. In still others, the slow-growing nature of the tumor may conceal the diagnosis for years. When patients present with symptoms related to mass effect or intracranial hypertension, surgical treatment often is necessary and undisputed. In contrast, patients who do not have evidence of radiographic tumor growth and whose symptoms are well controlled medically are the ones in whom management becomes difficult and controversial. This controversy largely stems from the lack of well-designed clinical trials with adequate follow-up to account for the relatively long progression-free survival (PFS, 36–95 months) and overall survival (OS, ≥7 years) some patients with LGG enjoy [4–6, 7•]
Prognostic Factors
The most important negative prognostic factors to emerge from the literature include increasing age, astrocytic histology, large tumor diameter (>4–6 cm), tumors crossing the midline, neurologic deficits, and poor performance status [2, 4–6, 7•, 8, 9]. In contrast, presentation with seizures, which generally occur in patients who are otherwise neurologically intact, often is identified as a positive prognostic factor [5, 8, 9]. (Schiff et al. [9] provide a more extensive review of prognostic factors for LGG.) In 2002, Pignatti et al. [4] described a simple scoring system to account for these important prognostic factors so that physicians could better counsel patients and stratify patients for subsequent trials (Table 1). Based on a multivariate analysis of data from one prospective European Organisation for Research and Treatment of Cancer (EORTC) trial and validated on the data from another, they assigned one point each for age ≥40 years, astrocytoma histology, maximal tumor diameter ≥6 cm, tumor crossing the midline, and presence of neurologic deficit before surgery. Low-risk patients (scores 0–2) had a median OS of 7.72 years, compared with 3.20 years for high-risk patients (scores 3–5) [4]. The University of California, San Francisco (UCSF) group recently introduced a new LGG scoring system that uses a four-point scoring system to predict OS and PFS, assigning one point each for age greater than 50 years, Karnofsky performance score (KPS) ≤80, maximum tumor diameter greater than 4 cm, and eloquent involvement of the tumor (Table 1) [7•]. When stratified according to low-risk (scores 0–1), medium-risk (score 2), and high-risk (scores 3–4) groups, 5-year OS was 97%, 81%, and 56%, respectively, and 5-year PFS was 76%, 49%, and 18%, respectively [7•]. This newer scoring system is unique in that it is the first such system to consider eloquence as a poor independent prognostic factor. The importance of eloquence may be attributable to being at higher risk of neurologic deficits but also may speak to the resectability of a tumor, as patients with noneloquent tumors are more likely to have more extensive resections.
The impact of increasing age on the LGG prognosis has received particular attention during the past year because older patients (ie, those ≥55–60 years of age) are increasingly being diagnosed with LGG. As might be expected, older patients with LGG have a poorer prognosis, with a 5-year OS of 30% to 40% [10, 11]. Moreover, each additional year of age has a negative impact on prognosis, suggesting that reports from investigators studying age as a binomial likely have understated the impact of increasing age on outcomes [10, 11]. Despite the poorer prognosis, however, patients who survive 2 years beyond the initial diagnosis may experience prolonged PFS [10].
Imaging
Besides the prognostic factors already reviewed, there is increasing interest in the role of imaging in the management of LGG. Several studies have been published touting the prognostic significance of various imaging findings, including contrast enhancement, tumor growth rates, choline and creatinine peaks on magnetic resonance (MR) spectroscopy, relative cerebral blood volume (rCBV), and absolute diffusion coefficients (ADCs) [12–15]. Unfortunately, studies directly comparing these various MRI-based imaging modalities are limited. In one comparative study, MR spectroscopy was shown to be superior to tumor growth rates and rCBV measurements for predicting anaplastic transformation [15]. On the other hand, in another study, tumor growth rate was superior to initial volume, rCBV, and ADC for predicting PFS and OS [14].
The relative importance of imaging findings compared with known prognostic factors is difficult to ascertain because studies rarely simultaneously account for known prognostic factors and imaging findings. The study by Chaichana et al. [16] of the prognostic significance of contrast enhancement is an exemplary exception. Before concluding that contrast enhancement portends decreased survival and increased recurrence, the authors demonstrated that the two groups studied (those with and without contrast enhancement) were well matched with respect to all known prognostic factors (eg, KPS and age) [16]. Further prospective studies incorporating clinically important prognostic factors and imaging findings will need to be conducted to understand the true importance of these novel imaging modalities.
Molecular Pathogenesis
Further advances in the management of LGG will be made only by developing a more thorough understanding of the pathogenesis of these tumors. Recent reports have dramatically altered our conceptual framework of LGG molecular genetics, suggesting that isocitrate dehydrogenase (IDH) mutations are an early event in LGG pathogenesis. IDH1, found in the cytoplasm and peroxisome, catalyzes the oxidative decarboxylation of isocitrate to α-ketoglutarate, reducing NADP+ to NADPH.
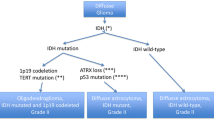
Previously, it was recognized that most LGGs harbored one of two mutually exclusive genetic changes: TP53 mutations in most low-grade astrocytomas and deletions of chromosomes 1p and 19q in most pure low-grade oligodendrogliomas (Table 2) [9]. Low-grade mixed gliomas tend to have either TP53 mutation or 1p/19q codeletion. Recent studies, however, have demonstrated IDH1 mutations in 59% to 90% of grade II astrocytomas, 68% to 85% of grade II oligodendrogliomas, and 50% to 83% of grade II oligoastrocytomas (Table 2) [17–19, 20•, 21]. The fact that IDH1 mutations are seen in similar frequencies in tumors with TP53 mutation and 1p/19q deletion suggests these mutations may precede other genetic alterations [17, 20•]. This is supported further by serial biopsies of LGGs showing that when IDH1 mutations occur, they always precede and never follow TP53 mutation or loss of heterozygosity of 1p/19q [19, 22]. Moreover, large-scale genetic sequencing of 105 glioblastomas identified IDH1 mutations in almost all secondary glioblastomas but in only 7% of primary (de novo) glioblastomas [23].
IDH mutations in gliomas have some remarkable features. First, every IDH1 mutation occurs in codon 132, which normally codes for an arginine in the enzyme’s active site. All produce amino acid substitutions, which in more than 90% is a histidine, resulting in decreased catalytic activity [17, 19, 20•]. IDH1 shares substantial homology with IDH2, a mitochondrial enzyme catalyzing the same reaction. Rare IDH2 mutations also were recognized recently in gliomas, especially oligodendrogliomas [18, 20•]. All IDH2 mutations are point mutations at codon 172 in the enzyme’s active site, a position representing the precise analogue of R132 in IDH1. IDH mutations are exceedingly rare in pediatric gliomas, nonglioma brain tumors, and other cancers [18].
The mechanisms by which IDH mutations predispose to gliomagenesis remain mysterious. Although the mutated protein is catalytically less active, consistent with a loss of function, these mutations are always heterozygous. Moreover, none of the mutations is a nonsense mutation, further suggesting the mutations may produce a dominant negative or gain of function [24]. Thus, IDH1 and IDH2 seem to function as tumor suppressor genes. Their inactivation has been shown to induce genes crucial to angiogenesis, although the relevance of this finding to LGGs that lack angiogenesis remains uncertain [24].
Investigation of the role of cancer-related cell signaling pathways continues in LGG. Recent reports highlight the importance of the MAPK pathway in pilocytic astrocytomas, with many of these tumors manifesting tandem duplication of 7q, resulting in a fusion gene incorporating the kinase domain of the BRAF oncogene with constitutive BRAF activity [25]. However, the 7q34 duplication is not seen in grade II astrocytomas [26]. Another important oncogenic signaling pathway is the PI3K-Akt-mTOR pathway, on which PTEN normally serves as a brake. Although PTEN sometimes is mutated in primary glioblastomas, PTEN mutations do not occur in LGG. However, most LGGs epigenetically silence PTEN via hypermethylation [27, 28]. Evidence of overactivation of the PI3K-Akt-mTOR pathway manifesting as phosphorylation of downstream proteins appeared to correlate inversely with survival, although numbers were small and this finding requires confirmation [28].
To what extent molecular markers such as 1p/19q codeletion status, IDH mutational status, and the presence or absence of MGMT promotor hypermethylation, which is a prognostic factor in glioblastoma outcome, predict responsiveness to specific therapies or overall prognosis remains uncertain. The presence of 1p/19q deletion seems to portend a better prognosis in LGG, although its favorable impact is weaker than in grade III gliomas. Small studies have suggested that MGMT methylation status may predict improved OS [29], but the small size of these studies and a potential confounding correlation between MGMT methylation and 1p/19q codeletion mandate larger studies. Similarly, in univariate analyses, IDH1 mutations conferred improved OS in low-grade and anaplastic gliomas as well as in glioblastomas, but it remains unclear whether mutational status retains prognostic significance when other prognostic markers are incorporated into multivariate models [19, 21].
Surgical Resection
The lack of pathognomonic imaging for LGG and the need for molecular, chromosomal, and histopathologic characterization of tumors mandate tissue acquisition for accurate diagnosis, prognostication, and management. Needle biopsy specimens have been associated with a greater than 50% misdiagnosis rate [30, 31]. Surgical resection (vs biopsy alone) affords a better opportunity to characterize, grade, and study tumor tissue to ensure proper diagnosis, treatment, and prognostication. Despite the lack of a randomized controlled trial, the evidence for the benefits of extensive surgical resection is growing. In 2001, Keles et al. [32] reviewed the literature and concluded that a preponderance of the evidence favored more extensive resection for patients with LGG. Since then, several additional long-term institutional studies have been published favoring extensive surgical resection [8, 33, 34, 35•]. Smith et al. [35•] retrospectively analyzed outcomes in 216 patients who underwent surgical resection for LGG at UCSF between 1989 and 2005, from a total of more than 800 patients treated for LGG during that period. Patients who underwent biopsy were specifically excluded because such patients usually have complicating factors and inclusion might confound the interpretation of the results. On multivariate analysis, extent of resection (EOR) was significantly associated with improved OS but not PFS. Five-year survival in patients with at least 90% EOR was 97%, whereas it was 76% in those with less than 90% EOR [35•]. In 170 patients treated surgically at Johns Hopkins Hospital between 1996 and 2007, McGirt et al. [33] similarly found that gross total resection (GTR; based on independent radiologist interpretation) was independently associated with improved OS and PFS compared with subtotal resection (5-year OS: 95% vs 70%, P = 0.017; median time to progression: 7 vs 3.5 years, P = 0.043). Although these studies suggest GTR is desirable, not all tumors are amenable to GTR. Predictors of incomplete tumor resection include tumor involvement of the corticospinal tract, large tumor volume, and oligodendroglioma histopathologic type [36].
Some may argue that enthusiasm for these retrospective reports must be tempered by results from prospective trials and other retrospective series that failed to find a significant prognostic effect of EOR. For example, the prospective intergroup American trial comparing low- and high-dose radiation therapy found EOR to be a significant prognostic factor for both OS and PFS on univariate analysis but found it was not significant on multivariate analysis [2]. Similarly, Pignatti et al. [4], who retrospectively studied the prospectively collected data from EORTC trials 22844 and 22845, found that extensive surgery (ie, >90%) was associated with longer OS on univariate analysis but failed to show significance on multivariate analysis. Although prospective, these studies have significant shortcomings, including neurosurgeon assessment of EOR, inclusion of biopsied patients in the analyses, and the fact that the studies were not primarily designed or powered to assess the effect of EOR.
In addition to OS and PFS, cognitive and quality-of-life outcomes after surgical resection must be considered, especially because concerns regarding these outcomes have thwarted the enthusiasm for radiotherapy. Although surgery may transiently exacerbate baseline deficits, most patients return to baseline or improve upon preoperative cognitive function within 3 months [37]. Moreover, advances in intraoperative technology (eg, neuronavigation) and pre- and intraoperative brain mapping techniques (eg, functional MRI, magnetic source imaging, and cortical and subcortical stimulation mapping) now allow neurosurgeons to tailor resections to individual functional brain architecture, minimizing the risk of permanent deficit to less than 2% and ensuring that patients’ quality of life is preserved [38, 39]. Duffau et al. [39] found that LGG patients operated on with the assistance of cortical stimulation had a significantly lower permanent deficit rate, a higher GTR rate, and a survival advantage compared with patients who were operated on without intraoperative mapping. In fact, the authors found that mapping may be used to identify dynamic changes in individual patients’ functional brain architecture, allowing more extensive tumor resections using a multistaged surgical approach [40]. Besides making surgeries safer and more extensive, advances in brain mapping also have made surgery an option for more patients [39]. In particular, there has been significantly increased interest in the surgical management of insular gliomas, which are challenging from an anatomic and eloquence standpoint but can be resected with only a 6% risk of postoperative deficit [41].
Ideally, a multicenter, multinational, prospective trial should be conducted to address this issue, but such a trial is unlikely because of the difficulty in recruiting sufficient numbers to demonstrate differences, the long-term follow-up that would be necessary, and ethical concerns that sufficient data already exist supporting GTR.
Radiotherapy
Among all available treatment modalities, radiotherapy is the only intervention shown in a randomized controlled trial to provide some benefit to LGG patients [42]. Even so, the optimal role for radiotherapy in the management of patients with LGG remains unclear. EORTC 22845 reported longer PFS and increased rates of seizure control in patients receiving upfront radiotherapy (54 Gy) compared with patients who were treated at the time of progression (PFS: 5.3 vs 3.4 years, P < 0.0001; seizure control rates: 75% vs 59%, P = 0.0329). OS, however, was not significantly different between the two groups (7.4 vs 7.2 years) [42]. Despite its efficacy with respect to PFS and seizure control, the authors concluded that radiotherapy might still be deferred in patients with LGG who are “in a good condition.” The ambivalence is attributable, in part, to the fact that quality of life was not studied; therefore, it was unclear at what cost patients with LGG were realizing a benefit in PFS and seizure control without an OS advantage. Moreover, by delaying radiotherapy, 35% of patients in the latter group (with a median follow-up of 7.4 years) never required radiation therapy, sparing them the possible adverse effects of radiation [42].
Recent studies therefore focused on quality-of-life measures after radiotherapy to better define its role in managing patients with LGG. Radiation leukoencephalopathy may ensue months to years after radiotherapy of the brain and may include progressive deterioration in personality, gait and balance, urinary continence, attention, memory, and executive function [43]. To reduce such risks, studies have been conducted demonstrating that total dose, fractional dose, and irradiation fields can be reduced without affecting the efficacy of treatment (see Baumert and Stupp [44] for more extensive reviews of this subject). Still, patients with LGG are at substantial risk of suffering from these complications because of their relatively long OS. Douw et al. [45] recently reported the most comprehensive and long-term analysis of cognitive and quality-of-life outcomes in 65 patients with LGG, half of whom had received radiotherapy. With a mean follow-up of 12 years, 27% of patients who had not been irradiated had significant cognitive deficits in at least 5 of 18 neuropsychological test parameters, whereas 53% of patients who received radiotherapy had significant cognitive deficits. Deficits were most pronounced in the domains of cognitive processing and attention, but nonsignificant differences also were observed in information processing speed, psychomotor functioning, and working memory [45]. These long-term sequelae of radiotherapy further challenge its upfront and systematic use considering radiotherapy and its complications can be delayed for more than a decade in some patients and the fact that advances in other treatment domains (eg, surgery and chemotherapy) may obviate the need for upfront radiation. Do patients who have had a GTR receive any additional benefit from radiotherapy? Likewise, does radiotherapy confer any advantage to patients who are treated with upfront temozolomide? As described in the “Chemotherapy” section, trials are currently under way to answer these types of questions.
Chemotherapy
With respect to chemotherapy, neuro-oncologists have focused their attention largely on temozolomide, which offers the advantages of an oral agent with a favorable toxicity profile compared with procarbazine, lomustine, and vincristine (PCV); crosses the blood–brain barrier well; and is more active against glioblastoma than PCV. Phase 2 clinical trials indicate that temozolomide, given on either a standard 5-day schedule or a dose-dense, metronomic schedule (3 weeks on, 1 week off or 7 weeks on, 4 weeks off), is active against both previously irradiated and unirradiated growing LGGs [29, 46, 47]. Moreover, temozolomide is associated with a favorable quality-of-life profile [48].
The two major questions relating to temozolomide use in LGG are whether temozolomide can substitute for radiation therapy and whether there is benefit from combining these two therapeutic modalities. Clinical trials addressing both these questions have been launched. European and Canadian investigators initiated a phase 3 clinical trial randomly assigning patients with LGG to receive either standard radiation or temozolomide. Patients are stratified based on chromosome 1p status. PFS is the primary end point, and the study incorporates neurocognitive and quality-of-life end points to assess the impacts of radiation and temozolomide in these regards.
Clinical trials are evaluating the combination of temozolomide with radiotherapy in high-risk LGGs previously untreated with radiation or chemotherapy. The Radiation Therapy Oncology Group (RTOG) recently completed accrual to a phase 2 clinical trial (RTOG 0424) of this combination; results are not expected before 2013. Under the aegis of the Eastern Cooperative Oncology Group (ECOG), the three major US brain tumor cooperative groups have launched a phase 3 effort (ECOG E3F05) randomly assigning LGG patients to receive standard radiation therapy combined with temozolomide and followed by a year of temozolomide or to receive radiation therapy alone. The trial design closely parallels the European trial of radiation versus temozolomide; in concert, these two trials should comprehensively address the role of temozolomide in the management of LGG.
The activity of chemotherapy in recurrent LGG post radiotherapy, as well as a growing appreciation for the chemosensitivity of tumors with an oligodendroglial component, led the RTOG to study the combination of PCV and radiation therapy. In this trial (RTOG 9802), patients with LGG deemed high risk because of age greater than 40 years or less than GTR were randomly assigned to receive standard radiation therapy with or without PCV. Although the cohort receiving chemoradiation had improved PFS, OS did not differ significantly between the two groups [49], suggesting that PCV was as active as salvage therapy as in combination with radiation.
Finally, reports suggest there may be a role for neoadjuvant therapy before surgical resection [50]. In both reported cases, although contralateral involvement via the corpus callosum originally prohibited GTR, chemotherapy shrunk the tumors to the extent that GTR was possible. The impact of timing of surgery can and will be appreciated only when a prospective trial is performed, such as was done for the timing of radiation therapy for the management of LGG [42].
Conclusions
The management of LGG is changing. New treatment strategies are being proposed that recognize the potential risks of a “wait-and-see” policy and radiotherapy as well as the potential benefits of extensive surgical resection and upfront chemotherapy. Considering the evidence currently available, the optimal treatment strategy likely includes offering extensive surgical resection when possible and delaying radiotherapy until the time of progression (Fig. 1). Several trials currently under way almost surely will revolutionize the treatment of these tumors further, defining the role of temozolomide in the management of these tumors and perhaps obviating the need for radiotherapy. Further multivariate investigations are necessary to define the prognostic significance of data from novel imaging techniques and molecular markers of pathogenesis.
Management of low-grade glioma (LGG). This flow diagram outlines a standard scheme for managing LGG, emphasizing the need to evaluate patients for surgical resection as one of the first steps in the comprehensive, multidisciplinary management of these tumors. This algorithm necessitates tissue acquisition for management in most cases, except for patients who are low risk and those who are asymptomatic. Once LGG has been confirmed, management varies depending on risk stratification of the patient, as described in Table 1. It is noteworthy that radiation therapy is delayed until the time of progression. aTemozolomide should be considered for treatment of high-risk patients when there is evidence of codeletion of 1p/19q or in the setting of a clinical trial
References
Papers of particular interest, published recently have been highlighted as: • Of importance
Central Brain Tumor Registry of the United States: Statistical Report: Primary Brain Tumors in the United States, 2000–2004. Available at http://www.cbtrus.org/reports//2007-2008/2007report.pdf. Accessed February 2010.
Shaw E, Arusell R, Scheithauer B, et al.: Prospective randomized trial of low- versus high-dose radiation therapy in adults with supratentorial low-grade glioma: initial report of a North Central Cancer Treatment Group/Radiation Therapy Oncology Group/Eastern Cooperative Oncology Group study. J Clin Oncol 2002, 20:2267–2276.
Duffau H, Capelle L: Preferential brain locations of low-grade gliomas. Cancer 2004, 100:2622–2626.
Pignatti F, van den Bent M, Curran D, et al.: Prognostic factors for survival in adult patients with cerebral low-grade glioma. J Clin Oncol 2002, 20:2076–2084.
Bauman G, Lote K, Larson D, et al.: Pretreatment factors predict overall survival for patients with low-grade glioma: a recursive partitioning analysis. Int J Radiat Oncol Biol Phys 1999, 45:923–929.
Claus EB, Black PM: Survival rates and patterns of care for patients diagnosed with supratentorial low-grade gliomas: data from the SEER program, 1973–2001. Cancer 2006, 106:1358–1363.
• Chang EF, Smith JS, Chang SM, et al.: Preoperative prognostic classification system for hemispheric low-grade gliomas in adults. J Neurosurg 2008, 109:817–824. This comprehensive study of LGG risk factors decribes the most recent LGG scoring system, which was validated in a subsequent multi-institutional study.
Bauman G, Fisher B, Watling C, et al.: Adult supratentorial low-grade glioma: long-term experience at a single institution. Int J Radiat Oncol Biol Phys 2009, 75:1401–1407.
Schiff D, Brown PD, Giannini C: Outcome in adult low-grade glioma: the impact of prognostic factors and treatment. Neurology 2007, 69:1366–1373.
Pouratian N, Mut M, Jagannathan J, et al.: Low-grade gliomas in older patients: a retrospective analysis of prognostic factors. J Neurooncol 2008, 90:341–350.
Schomas DA, Laack NN, Brown PD: Low-grade gliomas in older patients: long-term follow-up from Mayo Clinic. Cancer 2009, 115:3969–3978.
Hattingen E, Raab P, Franz K, et al.: Prognostic value of choline and creatine in WHO grade II gliomas. Neuroradiology 2008, 50:759–767.
Caseiras GB, Chheang S, Babb J, et al.: Relative cerebral blood volume measurements of low-grade gliomas predict patient outcome in a multi-institution setting. Eur J Radiol 2010, 73:215–220.
Brasil Caseiras G, Ciccarelli O, Altmann DR, et al.: Low-grade gliomas: six-month tumor growth predicts patient outcome better than admission tumor volume, relative cerebral blood volume, and apparent diffusion coefficient. Radiology 2009, 253:505–512.
Hlaihel C, Guilloton L, Guyotat J, et al.: Predictive value of multimodality MRI using conventional, perfusion, and spectroscopy MR in anaplastic transformation of low-grade oligodendrogliomas. J Neurooncol 2009, 97:73–80.
Chaichana KL, McGirt MJ, Niranjan A, et al.: Prognostic significance of contrast-enhancing low-grade gliomas in adults and a review of the literature. Neurol Res 2009, 31:931–939.
Balss J, Meyer J, Mueller W, et al.: Analysis of the IDH1 codon 132 mutation in brain tumors. Acta Neuropathol 2008, 116:597–602.
Hartmann C, Meyer J, Balss J, et al.: Type and frequency of IDH1 and IDH2 mutations are related to astrocytic and oligodendroglial differentiation and age: a study of 1,010 diffuse gliomas. Acta Neuropathol 2009, 118:469–474.
Ichimura K, Pearson DM, Kocialkowski S, et al.: IDH1 mutations are present in the majority of common adult gliomas but rare in primary glioblastomas. Neuro Oncol 2009, 11:341–347.
• Yan H, Parsons DW, Jin G, et al.: IDH1 and IDH2 mutations in gliomas. N Engl J Med 2009, 360:765–773. This seminal article highlights the importance of IDH mutations in the pathogenesis of gliomas.
Sanson M, Marie Y, Paris S, et al.: Isocitrate dehydrogenase 1 codon 132 mutation is an important prognostic biomarker in gliomas. J Clin Oncol 2009, 27:4150–4154.
Watanabe T, Nobusawa S, Kleihues P, Ohgaki H: IDH1 mutations are early events in the development of astrocytomas and oligodendrogliomas. Am J Pathol 2009, 174:1149–1153.
Griffin CA, Burger P, Morsberger L, et al.: Identification of der(1;19)(q10;p10) in five oligodendrogliomas suggests mechanism of concurrent 1p and 19q loss. J Neuropathol Exp Neurol 2006, 65:988–994.
Zhao S, Lin Y, Xu W, et al.: Glioma-derived mutations in IDH1 dominantly inhibit IDH1 catalytic activity and induce HIF-1alpha. Science 2009, 324:261–265.
Sievert AJ, Jackson EM, Gai X, et al.: Duplication of 7q34 in pediatric low-grade astrocytomas detected by high-density single-nucleotide polymorphism-based genotype arrays results in a novel BRAF fusion gene. Brain Pathol 2009, 19:449–458.
Korshunov A, Meyer J, Capper D, et al.: Combined molecular analysis of BRAF and IDH1 distinguishes pilocytic astrocytoma from diffuse astrocytoma. Acta Neuropathol 2009, 118:401–405.
Wiencke JK, Zheng S, Jelluma N, et al.: Methylation of the PTEN promoter defines low-grade gliomas and secondary glioblastoma. Neuro Oncol 2007, 9:271–279.
McBride SM, Perez DA, Polley MY, et al.: Activation of PI3K/mTOR pathway occurs in most adult low-grade gliomas and predicts patient survival. J Neurooncol 2010, 97:33–40.
Kesari S, Schiff D, Drappatz J, et al.: Phase II study of protracted daily temozolomide for low-grade gliomas in adults. Clin Cancer Res 2009, 15:330–337.
Muragaki Y, Chernov M, Maruyama T, et al.: Low-grade glioma on stereotactic biopsy: how often is the diagnosis accurate? Minim Invasive Neurosurg 2008, 51:275–279.
Jackson RJ, Fuller GN, Abi-Said D, et al.: Limitations of stereotactic biopsy in the initial management of gliomas. Neuro Oncol 2001, 3:193–200.
Keles GE, Lamborn KR, Berger MS: Low-grade hemispheric gliomas in adults: a critical review of extent of resection as a factor influencing outcome. J Neurosurg 2001, 95:735–745.
McGirt MJ, Chaichana KL, Attenello FJ, et al.: Extent of surgical resection is independently associated with survival in patients with hemispheric infiltrating low-grade gliomas. Neurosurgery 2008, 63:700–707; author reply 707–708.
Schomas DA, Laack NN, Rao RD, et al.: Intracranial low-grade gliomas in adults: 30-year experience with long-term follow-up at Mayo Clinic. Neuro Oncol 2009, 11:437–445.
• Smith JS, Chang EF, Lamborn KR, et al.: Role of extent of resection in the long-term outcome of low-grade hemispheric gliomas. J Clin Oncol 2008, 26:1338–1345. Although retrospective, this is one of the most convincing reports to date arguing that greater extent of resection results in improved outcomes.
Talos IF, Zou KH, Ohno-Machado L, et al.: Supratentorial low-grade glioma resectability: statistical predictive analysis based on anatomic MR features and tumor characteristics. Radiology 2006, 239:506–513.
Teixidor P, Gatignol P, Leroy M, et al.: Assessment of verbal working memory before and after surgery for low-grade glioma. J Neurooncol 2006, 81:305–313.
Duffau H: Surgery of low-grade gliomas: towards a ‘functional neurooncology.’ Curr Opin Oncol 2009, 21:543–549.
Duffau H, Lopes M, Arthuis F, et al.: Contribution of intraoperative electrical stimulations in surgery of low grade gliomas: a comparative study between two series without (1985–96) and with (1996–2003) functional mapping in the same institution. J Neurol Neurosurg Psychiatry 2005, 76:845–851.
Robles SG, Gatignol P, Lehericy S, Duffau H: Long-term brain plasticity allowing a multistage surgical approach to World Health Organization grade II gliomas in eloquent areas. J Neurosurg 2008, 109:615–624.
Sanai N, Polley MY, Berger MS: Insular glioma resection: assessment of patient morbidity, survival, and tumor progression. J Neurosurg 2010, 112:1–9.
van den Bent MJ, Afra D, de Witte O, et al.: Long-term efficacy of early versus delayed radiotherapy for low-grade astrocytoma and oligodendroglioma in adults: the EORTC 22845 randomised trial. Lancet 2005, 366:985–990.
Surma-aho O, Niemela M, Vilkki J, et al.: Adverse long-term effects of brain radiotherapy in adult low-grade glioma patients. Neurology 2001, 56:1285–1290.
Baumert BG, Stupp R: Low-grade glioma: a challenge in therapeutic options: the role of radiotherapy. Ann Oncol 2008, 19(Suppl 7):vii217–vii222.
Douw L, Klein M, Fagel SS, et al.: Cognitive and radiological effects of radiotherapy in patients with low-grade glioma: long-term follow-up. Lancet Neurol 2009, 8:810–818.
Kaloshi G, Benouaich-Amiel A, Diakite F, et al.: Temozolomide for low-grade gliomas: predictive impact of 1p/19q loss on response and outcome. Neurology 2007, 68:1831–1836.
Pouratian N, Gasco J, Sherman JH, et al.: Toxicity and efficacy of protracted low dose temozolomide for the treatment of low grade gliomas. J Neurooncol 2007, 82:281–288.
Liu R, Solheim K, Polley MY, et al.: Quality of life in low-grade glioma patients receiving temozolomide. Neuro Oncol 2009, 11:59–68.
Shaw EG, Berkey B, Coons SW, et al.: Initial report of Radiation Therapy Oncology Group (RTOG) 9802: prospective studies in adult low-grade glioma (LGG). J Clin Oncol 2006, 24:1500.
Duffau H, Taillandier L, Capelle L: Radical surgery after chemotherapy: a new therapeutic strategy to envision in grade II glioma. J Neurooncol 2006, 80:171–176.
Disclosure
No potential conflicts of interest relevant to this article were reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Pouratian, N., Schiff, D. Management of Low-Grade Glioma. Curr Neurol Neurosci Rep 10, 224–231 (2010). https://doi.org/10.1007/s11910-010-0105-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11910-010-0105-7