Abstract
Background
Several reports showed that sexual function was affected during and after the COVID-19 pandemic.
Aims
The objective of the study was to demonstrate whether a realistic association exists between the COVID-19 pandemic and erectile dysfunction (ED) among a sampled Egyptian population in Damietta governorate.
Methods
This cross-sectional study consisted of 330 adult males diagnosed with COVID-19 infection. They were categorized in three age groups (18–29, 30–39, and 40–50 years, respectively). COVID-19-confirmed cases were assessed by the Arabic version of the International Index of Erectile Function questionnaire (IIEF) scores.
Results
The prevalence of ED according to the IIEF was 55.1%. The ED was categorized into mild ED which represents 25.8% of the patients, mild to moderate which represents 22.4% of the patients, moderate which represents 7% of the patients, and severe which represents 0% of the patients. We found a significant negative correlation between the age of the patients and the IIEF score. Also, we found an association between the severity of COVID-19 infection and the IIEF score.
Conclusion
An association of new-onset ED in men who suffered COVID-19 infection was established. This may be due to virus-induced endothelial cell dysfunction; however, an underlying mechanism and causation have not yet been clearly elucidated. While it appears that COVID-19 infection may be a risk factor for ED, additional research is needed to establish causality.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
An overwhelming health concern about cases suffering from acute respiratory distress was first discovered in Wuhan, Hubei Province, China, in December (2019). These cases turned out to be affected by coronavirus disease 2019 (COVID-19) with substantial casualties. The etiology of COVID-19 had been determined as a novel coronavirus, now known as severe acute respiratory syndrome coronavirus (SARS-CoV-2) [1].
Several reports showed that sexual function was affected among males and females during and after the pandemic [2,3,4,5,6,7]. Men’s complaints have included erectile dysfunction (ED) and decreased sexual satisfaction in comparison to a pre-COVID state [5]. Of note, many patients have reported a decrease in erectile function (EF), which was confirmed by a reduction of their International Index of Erectile Function (IIEF) assessment [8].
The high incidence of sexual dysfunction during the pandemic led to assumptions of biological underlying mechanisms such as hypogonadism, endothelial, and cardiopulmonary dysfunction were proposed [9].
End-organ damage seen with severe COVID-19 infections is thought to be a result of endothelial dysfunction, resulting both from direct infection and a systemic inflammatory response. Electron microscopy has demonstrated viral elements in the endothelial cells of affected organs including the penis [11].
Moreover; several other studies have shown that psychological disturbances, e.g., anxiety or depression, were the principal underlying etiology of sexual dysfunction during the pandemic [6,7,8].
The aim of the study was to demonstrate whether a realistic association exists between the COVID-19 pandemic and erectile dysfunction (ED) among a sampled Egyptian population in Damietta governorate.
Methods
This cross-sectional study consisted of 330 adult males diagnosed with COVID-19 infection. They were categorized into the following age groups 18–29, 30–39, and 40–50 years. This categorization was chosen as it was used by similar studies and seems to be the most suitable in covering the targeted population and in producing clear statistical results. Patients were recruited from the post-COVID follow-up outpatient clinic at Al-Azhar University Hospital, Damietta over a period of 6 months from March 2022 to August 2022. Our study followed the Helsinki Declaration principals. Ethical approval was obtained from the institutional review board of Damietta Faculty of Medicine (Al-Azhar University). Written informed consent was obtained from every patient at the recruitment. Inclusions included males aged 18–50 years of age who are sexually active and who were diagnosed with COVID-19 infection (only those who finished the management protocol and had been discharged at least 2 weeks prior to joining the study). Subjects with confirmed erectile dysfunction (ED) due to known causes were excluded. All patients who were receiving any medications that could cause ED including anti-anxiety agents, antidepressants, antipsychotics, or mood stabilizers were not recruited. Moreover; all subjects with endocrinal diseases, neurological diseases, prostatic diseases, pelvic trauma or spinal cord injury, Peyronie’s disease or curvature, alcoholics, metabolic syndrome, and chronic illnesses (diabetes mellitus, hypertension, liver disease, renal failure, and cardiovascular disease) were also excluded from the study.
Data collection
All patients were subjected to the following.
-
1.
Full history taking (medical and surgical), marital status, occupation, sexual activity, and ED
-
2.
COVID-19 confirmation by using the reverse transcription polymerase chain reaction (RT-PCR) test of pharyngeal and nasal swabs. The severity of COVID-19 was determined by following the guidelines stated by Zhu et al. [12].
-
3.
Clinical examination and evaluation of potency were done by the validated Arabic version of the International Index of Erectile Function (IIEF) [13]. The IIEF Questionnaire was developed to address the need for a self-report measure of both erectile function and sexual function that can be given under guidance of a clinician. The IIEF Questionnaire presents the quality of male sexual function in terms of five domain scores: erectile function, orgasmic function, sexual desire, intercourse satisfaction, and overall satisfaction. This questionnaire consists of only five questions, and each IIEF-5 item is scored on a five-point ordinal scale where lower values represent poorer sexual function [10]. Thus, a response of 0 for a question was considered the least functional, whereas a response of 5 was considered the most functional. The possible scores for the IIEF5 range from 1 to 25 (one question has scores of 1–5), and a score above 21 was considered as normal erectile function and at or below this cutoff, ED. According to this scale, ED is classified into four categories based on IIEF-5 scores: severe (1–7), moderate (8–11), mild to moderate (12–16), mild (17–21), and no ED (22–25) [14].
The data entry and statistical analyses were performed using SPSS (Statistical Package of Social Sciences) version 26 (SPSS Inc., Chicago, IL, USA). Continuous normally distributed data were expressed in mean and standard deviation. The quantitative data were examined by Kolmogorov–Smirnov test for normality of data. Kruskal–Wallis test was used for continuous not normally distributed data. Categorical data were described as numbers and percentages and were analyzed using the Chi-square test. Statistical significance was considered when probability (P) value is less than or equal to 0.05.
Results
This study included 330 patients diagnosed with COVID-19 infection. The mean age of the patients was 35.7 ± 7.34 years with a range of 25–49. According to the severity of infection, 54.2% of the patients were mild, 34.2% were moderate, 7.8% were severe, and 3.6% were critical. In terms of the duration between the infection and the occurrence of ED, the mean duration was 6.7 ± 3 months (Tables 1 and 2).
Erectile function of the patients was assessed by the IIEF score, which consisted of 5 questions. The mean IIEF score was 19.45 ± 4.36 with a range of 10–25. Based on this score, the patients were divided into mild ED (22.8%), mild to moderate ED (22.4%), and moderate ED (7%). Severe ED was not reported in our study (Tables 3, 4, and 5).
By comparing the different degrees of COVID-19 infection according to the IIEF score, the IIEF score was significantly lower in patients with moderate to severe and severe COVID-19 infection (P value = 0.001) (Table 6).
Correlation analysis revealed a statistically significant correlation between the IIEF score and the severity of infection, in which most of the patients with ED were mild and moderate COVID-19 infection (P = 0.001) (Table 7).
In the present study, most of the ED cases were in the age category of 40–50 years; however, most of the normal EF cases were in the age category of 30–39 years. Also, a statistically significant association was found between the degree of ED and the age category in which most of the mild to moderate and moderate ED were in the age category of 40–50 years (P value = 0.001) (Table 7 and Fig. 1).
Discussion
Previously, COVID-19 has been shown to have harmful effects on various organs throughout the body, including the heart, kidneys, and vascular system [15]. Our current understanding of COVID-19 and its effect on the penile tissue and subsequent erectile function remains unclear. The importance of identifying the virus’ short and long-term effects on male reproductive organs is potentiated by a recent study observing COVID-19 particles in penile tissue through transmission electron microscopy and hematoxylin and eosin (H&E) staining [11]. As COVID-19 causes widespread endothelial dysfunction, and erectile function is dependent on a functional endothelium and proper vascular flow, it is hypothesized that a COVID-19 infection may be associated with new onset erectile dysfunction [16].
In this study, the association between males with COVID-19 infection and erectile dysfunction was investigated, and the prevalence of ED in COVID-19 patients was 55.1%, which is affirmative of another study that assessed the risk of ED in men with COVID-19 in the United States (US) and reported that COVID-19 diagnosis was significantly associated with ED [17].
Endothelial penile dysfunction in humans was reported following COVID-19 infection resulting in ED [18]. In addition to endothelial damage, there is a lack of clear understanding of the exact causes of ED among COVID-19-infected males; however, a systemic review found that stress, anxiety, and depression are among psychological factors that can be considered as possible causes of sexual dysfunction in COVID-19 patients [19]. Moreover, financial constraints and social restrictions experienced during the pandemic were among aggravating causes of sexual dysfunction among males [20,21,22,23,24].
Another important cause for sexual dysfunction is the fear and perception of contracting and/or spreading COVID-19 through sexual intercourse [25–27].
Moreover, it was reported that the men at highest risk of developing serious complications secondary to COVID‐19 also have a higher risk of ED. This group consisted of old-aged individuals, diabetics, subjects with cardiovascular disease, overweight/obese individuals, and those with multiple co-morbidities [28].
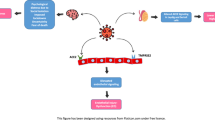
Studies investigating the pathogenesis of SARS‐CoV‐2 have revealed that the virus binds to the ACE2 receptor and enters the cell through the type 2 transmembrane serine protease 2 (TMPRSS2) enzyme found in the host cells [29]. ACE2 and TMPRSS2 are expressed in host target cells, particularly alveolar epithelial type II cells. They are also expressed in the digestive, cardiovascular and urinary systems, and testicular tissue [30].
In light of this information, Zhu et al. constructed a risk map of COVID‐19 using RNA sequencing datasets to evaluate the expression of the ACE2 receptor in various tissues and cells. According to this risk map, in addition to the respiratory system; cardiovascular, renal, gastrointestinal, and urogenital systems were also shown to be potentially vulnerable to the virus due to ACE2 expression [12].
Moreover, SARS-CoV-2 gonadal involvement was shown to increase serum prolactin levels and lowering testosterone levels via pituitary gland suppression, further adding to erectile function deterioration [31,32,33].
Kresch et al. examined patients who had symptomatic COVID‐19 infection and subsequently developed severe ED. The authors took tissue samples at the time of penile prosthesis implantation, and as a result of the histopathological examination, they stated that the systemic effect of COVID‐19 or widespread endothelial damage caused by the virus directly affecting the vascular endothelium could have a negative impact on penile vascular flow and lead to the deterioration of the erectile function [11].
In another study, Sivritepe et al. evaluated changes in the IIEF scores of 80 sexually active male patients hospitalized due to symptomatic COVID‐19 infection. According to the evaluations they performed during hospitalization and at the third month after discharge, there was a positive correlation between ED and the interleukin‐6 level. The authors attributed this correlation to the vascular consequences of possible interleukin‐6‐related inflammation [34].
In the present study, we found a significant negative correlation between the age of the patients and the IIEF score. This came in agreement with a cohort study that reported erectile dysfunction is strongly age-related with an approximately 2 to threefold increase in the prevalence of moderate-to-severe ED between the ages of 40 and 70 years [35]. A variety of medical, psychological, and hormonal statuses have been implicated in the etiology of ED. Testosterone is one of these factors. A relationship between aging and serum androgen levels was investigated in older men. The results are still controversial [36].
In the current study, we found an association between the severity of COVID-19 infection and the IIEF score. This is in agreement with Bary et al., who explained this correlation by a broad range of mechanisms including local direct and indirect effects on endothelial cells, secondary hypogonadism, and endocrine dysfunction as well as psychosocial factors [37].
In the current cohort, the deterioration in the erectile functions of moderate and severe patient groups had significantly lower IIEF score and higher prevalence of ED. In order to achieve a good erection, adequate blood flow to the penis must be provided. It is clear that this requires a well‐functioning cardiopulmonary system. COVID‐19 targets vital organs, such as the heart and lungs, it may take these systems up to 6 months to recover their functions after the disease, and there may sometimes be irreversible damage [38].
It is reported that the main cause of ED in lung patients is decreased functional capacity due to hypoxemia [38]. In a multicenter prospective study, Sonnweber et al. reported that a significant percentage of post‐COVID‐19 patients presented with radiological pulmonary abnormalities and pulmonary dysfunction 100 days after diagnosis. However, the authors also noted a significant improvement in symptoms and cardiopulmonary status over time [39].
In a study examining the possible mechanisms of the long‐term effects of COVID‐19 on sexual health, it is generally stated that the long‐term effects of the disease are proportional to the presence and severity of the accompanying non‐communicable diseases [40]. Since we examined the short‐term results of our patients, we consider that the deterioration in IIEF‐5 scores may have been related to impaired exercise capacity and cardiopulmonary function associated with COVID‐19. There is a need for further studies examining long‐term outcomes in order to validate this hypothesis.
Our sample size was considerable, and all participants were confirmed COVID-19 diagnosis. However, several limitations exist to the current work with the absence of comparison group and pre-existed erectile function status, the assumption of whether COVID-19 was the cause of ED could not be concluded and the confounding bias from social situations such as health policy during pandemic and change in sexual habit might affect the erectile function.
Conclusion
In conclusion, we reported an association of new-onset ED in men who had COVID-19 infection. This may be due to virus-induced endothelial cell dysfunction; however, an underlying mechanism and causation have not yet been clearly elucidated. While it appears that COVID-19 infection may be a risk factor for ED, additional research is needed to establish causality. The study reported the prevalence of ED to be higher in male patients older than 40 years old and that erectile function was significantly affected by the severity of COVID-19 infection. Future studies are needed to determine the predictive factor of ED in COVID-19 patients and appropriate early interventions.
Availability of data and material
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
- ED:
-
Erectile dysfunction
- IIEF:
-
International Index of Erectile Function
- ACE2:
-
Angiotensin-converting enzyme 2
- COVID-19:
-
Coronavirus disease 2019
- EF:
-
Erectile function
- MERS-CoV:
-
Middle East respiratory syndrome coronavirus
- SARS-CoV-2:
-
Severe acute respiratory syndrome coronavirus 2
References
Ahn DG, Shin HJ, Kim MH et al (2020) Current status of epidemiology, diagnosis, therapeutics, and vaccines for novel coronavirus disease 2019 (COVID-19). J Microbiol Biotechnol 30(3):313–324
Bulut EC, Ertaş K, Bulut D, Koparal MY, Çetin S (2021) The effect of COVID-19 epidemic on the sexual function of healthcare professionals. Andrologia 53(3):e13971. https://doi.org/10.1111/and.13971
Culha MG, Demir O, Sahin O, Altunrende F (2021) Sexual attitudes of healthcare professionals during the COVID-19 outbreak. Int J Impot Res 33(1):102–109. https://doi.org/10.1038/s41443-020-00381-9
de Rose AF, Chierigo F, Ambrosini F et al (2021) Sexuality during COVID lockdown: a cross-sectional Italian study among hospital workers and their relatives. Int J Impot Res 33(1):131–6. https://doi.org/10.1038/s41443-020-00393-5
Omar SS, Dawood W, Eid N et al (2021) Psychological and sexual health during the COVID-19 pandemic in Egypt: are women suffering more? Sex Med 9Omar SS, Dawood W, Eid N, Eldeeb D, Munir A, Arafat W. Psychological and Sexual Health During the COVID-19 Pandemic in Egypt: Are Women Suffering More? Sex Med 9(1):100295. https://doi.org/10.1016/j.esxm.2020.100295
Duran MB, Yildirim O, Kizilkan Y et al (2021) Variations in the number of patients presenting with andrological problems during the coronavirus disease 2019 pandemic and the possible reasons for these variations: a multicenter study. Sex Med 9(1):100292
Fuchs A, Matonóg A, Pilarska J, Sieradzka P, Szul M, Czuba B, Drosdzol-Cop A (2020) The Impact of COVID-19 on Female Sexual Health. Int J Environ Res Public Health 30;17(19):7152. https://doi.org/10.3390/ijerph17197152
Fang D, Peng J, Liao S et al (2021) An online questionnaire survey on the sexual life and sexual function of Chinese adult men during the coronavirus disease 2019 epidemic. Sex Med 9(1):100293
Sansone A, Mollaioli D, Ciocca G et al (2021) Addressing male sexual and reproductive health in the wake of COVID-19 outbreak. J Endocrinol Invest 44(2):223–231
Hamming I, Timens W, Bulthuis M et al (2004) Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J Pathol 203(2):631–7
Kresch E, Achua J, Saltzman R et al (2021) COVID-19 endothelial dysfunction can cause erectile dysfunction: histopathological, immunohistochemical, and ultrastructural study of the human penis. World J Mens Health 39(3):466
Zhu J, Zhong Z, Ji P et al (2020) Clinicopathological characteristics of 8697 patients with COVID-19 in China: a meta-analysis. Fam Med Community Healths 8(2):e000406
Shamloul R, Ghanem H, Abou-zeid A (2004) Validity of the Arabic version of the sexual health inventory for men among Egyptians. Int J Impot Res 16(5):452–455
Rhoden EL, Telöken C, Sogari PR, Vargas Souto CA (2002) The use of the simplified International Index of Erectile Function (IIEF-5) as a diagnostic tool to study the prevalence of erectile dysfunction. Int J Impot Res 14(4):245–250
Nägele MP, Haubner B, Tanner FC et al (2020) Endothelial dysfunction in COVID-19: current findings and therapeutic implications. Atherosclerosis 314(58):62
Vardi Y, Dayan L, Apple B (2009) Penile and systemic endothelial function in men with and without erectile dysfunction. Eur Urol 55(4):979–985
Chu KY, Nackeeran S, Horodyski L (2022) COVID-19 infection is associated with new onset erectile dysfunction: insights from a national registry. Sex Med 10(1):100478–100481
Saad HM, GamalEl Din SF, Elbokl OM, Adel A (2022) Predictive factors of erectile dysfunction in Egyptian individuals after contracting COVID-19: a prospective case–control study. Andrologia 13(54):58–1
Masoudi M, Maasoumi R, Bragazzi NL (2022) Effects of the COVID-19 pandemic on sexual functioning and activity: a systematic review and meta-analysis. BMC Public Health 22(1):189
Behzadifar M, Ghanbari MK, Bakhtiari A et al (2020) Ensuring adequate health financing to prevent and control the COVID-19 in Iran. Int J Equity Health 19(1):61
Wanberg CR, Csillag B, Douglass RP et al (2020) Socioeconomic status and well-being during COVID-19: a resource-based examination. J Appl Psychol 105(12):1382–1396
Carroll N, Sadowski A, Laila A et al (2020) The impact of COVID-19 on health behavior, stress, financial and food security among middle to high income Canadian families with young children. Nutrients 12(8):2352
Martin SA, Atlantis E, Lange K et al (2014) Predictors of sexual dysfunction incidence and remission in men. J Sex Med 11(5):1136–1147
Mahanty C, Kumar R, Mishra BK (2021) Analyses the effects of COVID-19 outbreak on human sexual behaviour using ordinary least-squares based multivariate logistic regression. Qual Quant 55(4):1239–1259
Lotfi M, Hamblin MR, Rezaei N (2020) COVID-19: transmission, prevention, and potential therapeutic opportunities. Clin Chim Acta 508:254–266
Pennanen-Iire C, Prereira-Lourenço M, Padoa A et al (2021) Sexual health implications of COVID-19 pandemic. Sex Med Rev 9(1):3–14
Hoffmann M, Kleine-Weber H, Schroeder S et al (2020) SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell 181(2):271–280
Sungnak W, Huang N, Bécavin C et al (2020) SARS-CoV-2 entry factors are highly expressed in nasal epithelial cells together with innate immune genes. Nat Med 26(5):681–687
Fan C, Lu W, Li K et al (2021) ACE2 expression in kidney and testis may cause kidney and testis infection in COVID-19 patients. Front Med (Lausanne) 13;7
Shen Q, Xiao X, Aierken A et al (2020) The ACE2 expression in Sertoli cells and germ cells may cause male reproductive disorder after SARS-CoV-2 infection. J Cell Mol Med 24(16):9472–9477
Ma L, Xie W, Li D et al (2021) Evaluation of sex-related hormones and semen characteristics in reproductive-aged male COVID-19 patients. J Med Virol 93(1):456–462
Brown RSE, Khant Aung Z, Phillipps HR et al (2019) Acute suppression of LH secretion by prolactin in female mice is mediated by kisspeptin neurons in the arcuate nucleus. Endocrinology 160(5):1323–1332
Salar R, Erbay G, Şanlı A et al (2023) Effect of COVID-19 infection on the erectile function. Andrology 11(1):10–16
Salar R, Erbay G, Şanlı A, Yavuz U, Kandemir E, Turel H, FeratÖncel H (2023) Effect of COVID-19 infection on the erectile function. Andrology 11(1):10–16. https://doi.org/10.1111/andr.13315
Feldman HA, Goldstein I, Hatzichristou DG et al (1994) Impotence and its medical and psychosocial correlates: results of the Massachusetts Male Aging Study. J Urol 151(1):54–61
Atan A, Basar MM, Tuncel A et al (2007) Is there a relationship among age, international index of erectile function, international prostate symptom score, and aging males’ symptoms score? Int Urol Nephrol 39(1):215–222
Feldman HA, Goldstein I, Hatzichristou DG, Krane RJ, McKinlay JB (1994) Impotence and its medical and psychosocial correlates: results of the Massachusetts Male Aging Study. J Urol 151(1):54–61. https://doi.org/10.1016/s0022-5347(17)34871-1
Huang C, Huang L, Wang Y et al (2021) RETRACTED: 6-month consequences of COVID-19 in patients discharged from hospital: a cohort study. Lancet 397(10270):220–232
Sonnweber T, Sahanic S, Pizzini A et al (2021) Cardiopulmonary recovery after COVID-19: an observational prospective multicentre trial. Eur Respir J 57(4):2003481
Köseoğlu N, Köseoğlu H, Ceylan E et al (2005) Erectile dysfunction prevalence and sexual function status in patients with chronic obstructive pulmonary disease. J Urol 174(1):249–252
Acknowledgements
The authors are grateful to all participants in the study.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB).
Author information
Authors and Affiliations
Contributions
MA, ZO, OH, AE, and ME designed and performed the research. MA, ZO, OH, AE, and ME performed the work. MA, ZO, OH, AE, and ME analyzed and wrote the paper. All authors have critically reviewed and approved the final draft and are responsible for the content and similarity index of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study protocol was reviewed and approved by ethics committee on human research by Al Azhar Faculty of Medicine IRB (00012367-22-04-001). All methods were performed in accordance with the relevant guidelines and regulations. Written informed consents were received from participants upon explanation of the study.
Consent for publication
Not applicable, the manuscript does not contain any individual personal data.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ahmed, M.A., Obaid, Z.M., Hashem, O. et al. Prevalence of new onset erectile dysfunction among Damietta governorate men after contracting COVID-19. Ir J Med Sci 193, 1581–1587 (2024). https://doi.org/10.1007/s11845-024-03610-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-024-03610-y