Abstract
Purpose
Studies have found that erectile dysfunction (ED) may be a short-term or long-term complication in coronavirus disease 2019 (COVID-19) patients, but no relevant studies have completed a pooled analysis of this claim. The purpose of the review was to comprehensively search the relevant literature, summarize the prevalence of ED in COVID-19 patients, assess risk factors for its development, and explore the effect of the COVID-19 infection on erectile function.
Methods
Medline, Embase, and the Cochrane Library was performed from database inception until April 14, 2022. Heterogeneity was analyzed by χ2 tests and I2 was used as a quantitative test of heterogeneity. Subgroup analyses, meta-regression, and sensitivity analyses were used to analyze sources of heterogeneity.
Results
Our review included 8 studies, 4 of which functioned as a control group. There were 250,606 COVID-19 patients (mean age: 31–47.1 years, sample size: 23–246,990). The control group consisted of 10,844,200 individuals (mean age: 32.76–42.4 years, sample size 75–10,836,663). The prevalence of ED was 33% (95% CI 18–47%, I2 = 99.48%) in COVID-19 patients. The prevalence of ED based on the international coding of diseases (ICD-10) was 9% (95% CI 2–19%), which was significantly lower than the prevalence of ED diagnosed based on the International Index of Erectile Function (IIEF-5) (46%, 95% CI 22–71%, I2 = 96.72%). The pooling prevalence of ED was 50% (95% CI 34–67%, I2 = 81.54%) for articles published in 2021, significantly higher than that for articles published in 2022 (17%, 95% CI 7–30%, I2 = 99.55%). The relative risk of developing ED was 2.64 times in COVID-19 patients higher than in non-COVID-19 patients (RR: 2.64, 95% CI 1.01–6.88). The GRADE-pro score showed that the mean incidence of ED events in COVID-19 patients was 1,333/50,606 (2.6%) compared with 52,937/844,200 (0.4%) in controls; the absolute impact of COVID-19 on ED was 656/100,000 (ranging from 4/100,000 to 2352/100,000). Anxiety (OR: 1.13, 95% CI 1.03–1.26, I2 = 0.0%) in COVID-19 patients was a risk factor for ED.
Conclusion
COVID-19 patients have a high risk and prevalence of ED, mainly driven by anxiety. Attention should be paid to patient’s erectile functioning when treating COVID-19.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The coronavirus disease 2019 (COVID-19) broke out in countries around the world beginning in 2019 [1]. The COVID-19 outbreak was listed by the World Health Organization as a major global public health problem [2]. Current studies indicate that COVID-19 has multiple site mutations, and the epidemic has still not been completely controlled [3,4,5]. Epidemiological data show that a large portion of the population is susceptible to COVID-19, but disease incidence appears to be positively correlated with age and underlying diseases, (i.e., hypertension, diabetes, and cardiovascular disease) [6]. There were 500,186,525 confirmed COVID-19 cases worldwide and 6,190,349 deaths attributed to the disease as of April 15, 2022 [7].
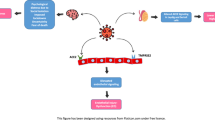
The American Urological Association (AUA) guidelines define erectile dysfunction (ED) as the persistent or repeated inability to achieve and/or maintain penile sexual needs, and ED is one of the most common manifestations of male sexual dysfunction [8]. It appears that psychological, vascular, endocrine, and neurological factors can lead to ED, which is most common in males [9, 10]. The prevalence of ED has been found to fluctuate between 0.48% and 75% in COVID-19 patients [11, 12]. Studies have reported that COVID-19 can invade host cells through the Spike-Angiotensin converting enzyme 2 (ACE2) binding pathway [13]. In Leydig cells, seminiferous tubules, and germ cells, ACE2 is highly expressed [14, 15]. COVID-19 could thus directly invade testicular tissue via these ACE2 receptors and cause ED [16]. Additionally, other studies have found that the virus persists in the penis long after the initial COVID-19, and have argued that widespread endothelial cell dysfunction caused by COVID-19 could lead to ED [17]. However, there is no current consensus on the effects of COVID-19 on ED. This review aimed to comprehensively search relevant literature and summarize the prevalence and risk factors of ED after COVID-19 infection.
Methods
The study followed by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) and was registered in PROSPERO (ID: CRD42022327263) [18].
Data search
Embase, Medline, and the Cochrane Library were searched using Ovid SP until April 14, 2022. The search strategies are listed in Table S1. References of included studies were searched manually. There were no restrictions for the literature search. Two reviewers independently conducted the process of records search, study selection, quality assessment, and data extraction. Disagreements between the 2 reviewers were resolved by a third reviewer.
Inclusion and exclusion criteria
All types of studies that reported ED’s prevalence in COVID-19 were included. The diagnosis of COVID-19 was based on reverse transcription polymerase chain reaction (RT-PCR) or any measurement was provided in each study’s methodology. The assessment of ED according to any measurement [i.e., the international coding of diseases (ICD-10) or International Index of Erectile Function (IIEF-5)] was provided in each study’s methodology. The question that directed the review was “Does COVID-19 increase the risk of ED?”, and it followed a Patients, Interventions, Comparisons, Outcomes, and Study Design (PICOS).
P: COVID-19 patients.
I: diagnosis of ED.
C: healthy population.
O: prevalence and risk factors for ED.
S: all studies.
In addition, studies that provided odds ratios (ORs), relative risks (RRs), hazard ratios, and 95% confidence intervals (CIs) were included. Studies that did not examine the prevalence of or assessment methods related to ED, duplicate studies, studies using the same population, reviews, commentaries, letters, editorials, conference abstracts, case reports, studies with < 10 participants and animal studies were excluded.
Study selection
We started by removing duplicate studies. We then filtered all articles by title and abstract. Next, full-text studies were screened based on our criteria. Finally, studies included were reviewed and finalized.
Data extraction
Data were extracted from eligible studies using preformatted tables, reviewed, and finalized. The extracted data included the first author’s name, year of publication, the region, study design, sample size, age, diagnostic method of COVID-19, and the methods of assessing ED, determining ED’s prevalence, and determining risk factors of ED (ORs and 95% CI).
Quality and evidence assessment
The quality assessment of case–control/cohort studies and cross-sectional studies was assessed using the Newcastle–Ottawa Scale (NOS) [19] and the cross-sectional study quality methodology checklist [20], respectively. The evidence’s overall quality was ranked using the Grading of Recommendations Assessment, Development and Evaluation (GRADE) [21].
Outcomes
The outcomes of the review were (1) the prevalence of ED in included studies, (2) RR for developing ED in COVID-19 patients compared with non-COVID-19 patients, and (3) risk factors for ED’s development in COVID-19 patients.
Statistical analyses
A meta-analysis was used to calculate the weight of prevalence of ED and risk factors for ED in COVID-19 patients using STATA 12.0 (StataCorp, College Station, TX, USA). ORs and 95% CIs of risk factors were extracted from multivariate analyses. A p value < 0.05 was considered statistically significant. Heterogeneity was quantitatively assessed using I2, and heterogeneity was analyzed using chi-square tests [22]. If there was no statistical heterogeneity, a fixed-effects model was used for meta-analysis [23]. If there was statistical heterogeneity, a random-effects model was used, and subgroup analysis [24], meta-regression, and sensitivity analysis were used to further analyze heterogeneity. Funnel plots, Begg-Mazumdar Kendall’s tau tests [25], and Egger bias tests [26] were performed to evaluate publication bias, and, if there was any publication bias, the trim-and-fill approach was used [27].
Results
Literature Search
In total, 392 records were retrieved. After removing 66 duplicate articles, 326 articles were screened by read-through of abstracts and titles. Then, 11 studies were read in full text. After reading the full text, 3 articles were excluded, 1 article was because there was no data on the prevalence of ED, and 2 articles were for they were studies of sexual function in female patients. A total of 8 studies met our inclusion and exclusion criteria [11, 12, 28,29,30,31,32,33]. Figure 1 shows the specific screening process and results.
Study characteristics and quality assessment
A total of 250,606 COVID-19 patients were included, with an average age of 31–47.1 years and a sample size of 23–246,990. Four of the included studies had control groups, which, when combined, comprised 10,844,200 individuals, with mean ages ranging between 32.76 and 42.4 years and sample sizes ranging from 75 to 10,836,663 persons. The prevalence of ED ranged from 0.48 to 75.0%. The characteristics of the included studies are shown in Table 1. Three studies were retrospective, 2 were prospective studies, 2 were cross-sectional studies, and 1 was a case–control study. Two studies were from North America, 2 studies were from Europe, 2 studies were from Asia, and 2 studies were from Africa. The quality assessment of the studies included is listed in Table S2 and Table S3, with 3 studies rated as moderate and 5 studies rated as high quality. The GRADE-pro score showed that the mean incidence of ED in COVID-19 patients was 1,333/50,606 (2.6%) compared with 52,937/844,200 (0.4%) in controls, and the absolute impact of COVID-19 on ED was 656/100,000 (from 4/100,000 to 2352/100,000). The evidence’s overall quality was considered to be low (Table 2).
Prevalence of ED and subgroup analysis
After pooling, the prevalence of ED was 33% (95% CI 18–47%, I2 = 99.48%, Fig. 2) in COVID-19 patients. When the four studies with a control group were combined, the risk of developing ED was 2.64 times in COVID-19 patients that in patients without COVID-19 (RR: 2.64, 95% CI 1.01–6.88, Fig. 3). Subgroup analysis showed that the prevalence of ED diagnosed according to ICD-10 was 9% (95% CI 2–19%), which was significantly lower than the prevalence of ED diagnosed based on IIEF-5 (46%, 95% CI 22–71%, I2 = 96.72%, Figure S1). Further, this difference was statistically significant, with a p-value less than 0.05, indicating that ED diagnosis was a source of between-study heterogeneity. In addition, the pooling prevalence of ED was 50% (95% CI 34–67%, I2 = 81.54%) for articles published in 2021, significantly higher than that for articles published in 2022 (17%, 95% CI 7–30%, I2 = 99.55%, Figure S2), the difference was statistically significant (P < 0.05), suggesting that publication year may be one of the sources of inter-study heterogeneity. Such heterogeneity can be due to the larger sample size of more recent studies, or to different outcomes for different COVID-19 variants, or to the increasing rates of vaccination.
Meta-regression and sensitivity analysis
Sample size (regression coefficient: 1.507, 95% CI 1.157–1.965, p = 0.009) was one of the sources of between-study heterogeneity in meta-regression analyses (Figure S3). Sensitivity analyses indicated that the omission of any of the included studies did not significantly affect the prevalence of ED (Figure S4).
Risk factors for ED in COVID-19 patients
Four studies provided data on anxiety, suggesting that anxiety (OR: 1.13, 95% CI 1.03–1.26, I2 = 0.0%) was a risk factor for ED in COVID-19 patients. However, age (OR: 1.03, 95% CI 0.98–1.09, I2 = 68.3%, 4 studies), body mass index (BMI) (OR: 0.98, 95% CI 0.87–1.11, I2 = 44.3%, 3 2 studies) and depression (OR: 1.01, 95% CI 0.86–1.19, I2 = 64.0%, 3 studies) were not risk factors for ED in COVID-19 patients (Fig. 4). Other risk factors that could not be analyzed using meta-analysis are listed in Table S4. The study also found that COVID-19 was one of the risk factors for ED, and OR was higher with increasing severity of illness [32, 33].
Publication bias
The funnel plot of our study is asymmetric (Figure S5). Begg’s test showed p value is 0.71, and Egger’s test showed p value is 0.006, suggesting the existence of publication bias. The trim-and-fill method showed that five additional studies would be needed to eliminate publication bias in the future (Figure S6). The results of the five studies were similar to previous work [i.e., Harirugsakul et al. (2021) [28], Hu et al. (2021) [29], Rabie et al. (2021) [31], Sansone et al. (2021) [33] and Sivritepe et al. (2022) [12].
Discussion
This study pooled all studies on ED in COVID-19 patients, performed a meta-analysis of the prevalence and risk factors for ED, and explored whether COVID-19 increases the risk of ED. A meta-analysis of the 8 included articles showed that the prevalence of ED was 33% in patients with COVID-19, of which the prevalence of ED diagnosed by ICD-10 was 9%, and the prevalence of ED diagnosed by IIEF-5 was 46%. The diagnostic method used to determine ED has a great impact on its prevalence, which may be due to the high sensitivity of IIEF-5 for diagnosing ED (i.e., 0.98.) [34] and/or two studies (Chu et al. and Katz et al.) [11, 30] using ICD-10 to diagnose ED had significantly larger sample sizes than the other included studies. The pooling prevalence of ED for articles published in 2021 was 50%, higher than that for articles published in 2022 (17%). The effect of publication year on ED prevalence may be due to the larger sample size of articles published in 2022 than in 2021 (250,338 vs. 268) and/or possibly the effect of COVID-19 variants. In a meta-regression, the sample size was one of the reasons for the high heterogeneity of this study. The included studies’ sample was uneven and varied greatly, which might be due to differences in each study’s capabilities in obtaining COVID-19 patients’ case data. When pooling studies with a control group, we found that in COVID-19 patients the relative risk of developing ED was 2.64 times greater than in patients without COVID-19. The GRADE-pro score showed that the mean incidence of ED events in COVID-19 patients was 1,333/50,606 (2.6%), and the absolute impact of COVID-19 on ED was 656/100,000 (increased from 4/100,000 to 2352/100,000). Taken together, COVID-19 appears to increase the risk of ED.
We found that anxiety in patients with COVID-19 was a risk factor for ED, whereas age, BMI, and depression were not risk factors for ED. A large number of existing studies have found the negative impact of psychological factors on ED [29, 35,36,37,38]. However, studies have found that sexual activity has a protective effect against the quarantine-related plague of anxiety and mood disorders during the COVID-19 outbreak [39]. Given the bidirectional interaction between sexual activity and mental health [39, 40]. Excluding possible effects of anxiety and depression, Sansone et al. confirmed that the increased prevalence of ED was not only a result of the psychological burden, but was also clearly attributable to other truly organic factors, of which endothelial dysfunction was the most likely culprit. Moreover, the study was also highly suggestive of the role of infection in ED development and the possible clinical relevance of COVID-19 as an additional risk factor for ED development [33]. Additionally, due to the limited number of included studies, some studies which did determine statistically significant risk factors could not be meta-analyzed. Hu et al. [29] found that the Global Severity Index was the only independent risk factor for ED in newly diagnosed COVID‐19 patients (OR: 8.697, P = 0.015), suggesting an important role of ED on disease at the time of the first diagnosis. Saad et al. [32] showed that smoking, moderate COVID-19, baseline IIEF-5 scores, and severe COVID-19 in patients with COVID-19 were independent risk factors for ED. A logistic regression, adjusted for age and BMI (Sansone et al.), showed that COVID-19 infection [odds ratio: 5.27 (95% CI 1.49–20.09) was an independent risk factor for ED and that ED may be a short- and a long-term risk factor for complications in COVID-19 [33]. The possible mechanisms of ED caused by COVID-19 in the current study are as follows: (1) Endothelial dysfunction [41]: the nitric oxide synthase’s expression levels in the cavernous endothelium and the average level of endothelial progenitor cells in patients with COVID-19 were decreased [17]. (2) Direct testicular injury: novel coronaviruses have been found in COVID-19 patients semen and testes in acute and convalescent periods [42]. Autopsy reports have revealed that patients’ testes have edema, mild lymphocytic infiltration, marked leukopenia, and seminiferous tubule damage [43]. (3) Hypogonadism [41]: a large study found that COVID‐19 was related with decreased testosterone, with secondary hypogonadism in 85% of patients [44]. (4) Inflammatory cytokines: IL-1β, IL-6, and TNF-α were associated to the clinical progression of sexual dysfunction [44, 45]. In COVID-19 patients, IL-6 could be used as a marker for ED, and when it’s cut-off point was 14.2 ng/ml, the sensitivity for detecting ED risk was 0.78 and the specificity was 0.72 [12]. (5) Psychological dysfunction [41, 46]. (6) Impaired pulmonary hemodynamics [41]. (7) Anosmia and ageusia: it has been suggested that anosmia and ageusia may play an important role in the etiology of temporary ED associated with COVID-19 [47].
To our knowledge, the study was the first meta-analysis of the prevalence and risk factors for ED in COVID-19 patients. We summarized the current prevalence of ED in COVID-19 patients and found that studies’ number in this field was relatively small, and the related research was still needed, especially for the occurrence, development, and treatment of ED after recovery from COVID-19. However, we also provided data for future interventional studies. Furthermore, in COVID-19 patients, anxiety was a risk factor for ED’s development. ED might be the first symptom of an otherwise asymptomatic cardiovascular disease, and all patients with ED without an apparent cause should undergo a comprehensive cardiovascular examination [48, 49]. We recommend that special attention needs to be paid to the mental health of COVID-19 patients to reduce ED incidence, and comprehensive cardiovascular examinations should be conducted for patients with ED of unknown cause.
This study had some limitations. First, the included studies were highly heterogeneous (I2 = 99.48%). Thus, we used subgroup analyses, meta-regression, and sensitivity analyses to determine potential heterogeneity, and found that methods of diagnosing ED and the size of the study sample were partially responsible for the high heterogeneity. Second, related to risk factors for ED, the number of studies on some variables was limited, and the application of the combined results was limited. Additionally, due to the small number of included studies, some risk factors could not be combined. Third, there was publication bias amongst the studies included in our review, and further attention should be paid to newer work that could supplement and update our findings. Fourth, as some original literatures did not provide relevant data, we could not explore the potential link between the time span from COVID-19 infection to the onset of ED and ED.
Conclusion
In conclusion, ED’s prevalence was higher in COVID-19 patients, and anxiety played a driving role in the development of ED. Thus, to reduce the occurrence of ED, it is very important to evaluate the psychological function of patients while treating COVID-19.
References
Atzrodt CL, Maknojia I, McCarthy RDP, Oldfield TM, Po J, Ta KTL et al (2020) A guide to COVID-19: a global pandemic caused by the novel coronavirus SARS-CoV-2. FEBS J 287:3633–3650. https://doi.org/10.1111/febs.15375
Organization WH. WHO Director-General's opening remarks at the media briefing on COVID-19 - 11 March 2020. https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020
Saito A, Irie T, Suzuki R, Maemura T, Nasser H, Uriu K et al (2022) Enhanced fusogenicity and pathogenicity of SARS-CoV-2 Delta P681R mutation. Nature 602:300–306. https://doi.org/10.1038/s41586-021-04266-9
Saxena SK, Kumar S, Ansari S, Paweska JT, Maurya VK, Tripathi AK et al (2022) Characterization of the novel SARS-CoV-2 Omicron (B.1.1.529) variant of concern and its global perspective. J Med Virol 94:1738–1744
Tian D, Sun Y, Xu H, Ye Q (2022) The emergence and epidemic characteristics of the highly mutated SARS-CoV-2 Omicron variant. J Med Virol 94:2376–2383. https://doi.org/10.1002/jmv.27643
Rahman A, Sarkar A (2019) Risk factors for fatal middle east respiratory syndrome coronavirus infections in Saudi Arabia: analysis of the WHO Line List, 2013–2018. Am J Public Health 109:1288–1293. https://doi.org/10.2105/ajph.2019.305186
Organization WH. https://www.who.int/emergencies/diseases/novel-coronavirus-2019
Montague DK, Barada JH, Belker AM, Levine LA, Nadig PW, Roehrborn CG et al (1996) Clinical guidelines panel on erectile dysfunction: summary report on the treatment of organic erectile dysfunction. The American Urological Association. J Urol 156:2007–2011. https://doi.org/10.1016/s0022-5347(01)65419-3
Besiroglu H, Otunctemur A, Ozbek E (2015) The relationship between metabolic syndrome, its components, and erectile dysfunction: a systematic review and a meta-analysis of observational studies. J Sex Med 12:1309–1318. https://doi.org/10.1111/jsm.12885
Gratzke C, Angulo J, Chitaley K, Dai YT, Kim NN, Paick JS et al (2010) Anatomy, physiology, and pathophysiology of erectile dysfunction. J Sex Med 7:445–475. https://doi.org/10.1111/j.1743-6109.2009.01624.x
Chu KY, Nackeeran S, Horodyski L, Masterson TA, Ramasamy R. COVID-19 Infection Is Associated With New Onset Erectile Dysfunction: Insights From a National Registry. Sexual Medicine. 2022;10(1) (no pagination):
Sivritepe R, Ucak Basat S, Baygul A, Kucuk EV (2022) The effect of interleukin-6 level at the time of hospitalisation on erectile functions in hospitalised patients with COVID-19. Andrologia. https://doi.org/10.1111/and.14285
Xu X, Chen P, Wang J, Feng J, Zhou H, Li X et al (2020) Evolution of the novel coronavirus from the ongoing Wuhan outbreak and modeling of its spike protein for risk of human transmission. Sci China Life Sci 63:457–460. https://doi.org/10.1007/s11427-020-1637-5
Li MY, Li L, Zhang Y, Wang XS (2020) Expression of the SARS-CoV-2 cell receptor gene ACE2 in a wide variety of human tissues. Infect Dis Poverty 9:45. https://doi.org/10.1186/s40249-020-00662-x
Groner MF, de Carvalho RC, Camillo J, Ferreira PRA, Fraietta R (2021) Effects of COVID-19 on male reproductive system. International braz j urol : official journal of the Brazilian Society of Urology 47:185–190. https://doi.org/10.1590/s1677-5538.ibju.2021.99.04
Guo J, Sheng K, Wu S, Chen H, Xu W (2021) An update on the relationship of SARS-CoV-2 and male reproduction. Front Endocrinol 12:788321. https://doi.org/10.3389/fendo.2021.788321
Kresch E, Achua J, Saltzman R, Khodamoradi K, Arora H, Ibrahim E et al (2021) COVID-19 Endothelial dysfunction can cause erectile dysfunction: histopathological, immunohistochemical, and ultrastructural study of the human penis. World J Mens Health 39:466–469. https://doi.org/10.5534/wjmh.210055
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605. https://doi.org/10.1007/s10654-010-9491-z
Whiting P, Rutjes AW, Reitsma JB, Bossuyt PM, Kleijnen J (2003) The development of QUADAS: a tool for the quality assessment of studies of diagnostic accuracy included in systematic reviews. BMC Med Res Methodol 3:25. https://doi.org/10.1186/1471-2288-3-25
Brozek JL, Akl EA, Alonso-Coello P, Lang D, Jaeschke R, Williams JW et al (2009) Grading quality of evidence and strength of recommendations in clinical practice guidelines. Part 1 of 3. An overview of the GRADE approach and grading quality of evidence about interventions. Allergy 64:669–677. https://doi.org/10.1111/j.1398-9995.2009.01973.x
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558. https://doi.org/10.1002/sim.1186
Leonard T, Duffy JC (2002) A Bayesian fixed effects analysis of the Mantel-Haenszel model applied to meta-analysis. Stat Med 21:2295–2312. https://doi.org/10.1002/sim.1048
DerSimonian R, Kacker R (2007) Random-effects model for meta-analysis of clinical trials: an update. Contemp Clin Trials 28:105–114. https://doi.org/10.1016/j.cct.2006.04.004
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50:1088–1101
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634. https://doi.org/10.1136/bmj.315.7109.629
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56:455–463. https://doi.org/10.1111/j.0006-341x.2000.00455.x
Harirugsakul K, Wainipitapong S, Phannajit J, Paitoonpong L, Tantiwongse K (2021) Erectile dysfunction among Thai patients with COVID-19 infection. Transl Androl Urol 10(12):4376–4383
Hu B, Ruan Y, Liu K, Wei X, Wu Y, Feng H et al (2021) A Mid-to-Long term comprehensive evaluation of psychological distress and erectile function in COVID-19 recovered patients. J Sex Med 18(11):1863–1871
Katz J, Yue S, Xue W, Gao H (2022) Increased odds ratio for erectile dysfunction in COVID-19 patients. J Endocrinol Invest 45(4):859–864
Rabie AM (2021) COVID-19 and sexual dysfunction in men: SARS-CoV-2 in the testes. Sexologies 30(4):e141–e148
Saad HM, GamalEl Din SF, Elbokl OM, Adel A (2022) Predictive factors of erectile dysfunction in Egyptian individuals after contracting COVID-19: a prospective case-control study. Andrologia. https://doi.org/10.1111/and.14308
Sansone A, Mollaioli D, Ciocca G, Colonnello E, Limoncin E, Balercia G et al (2021) “Mask up to keep it up”: preliminary evidence of the association between erectile dysfunction and COVID-19. Andrology 9(4):1053–1059
Neijenhuijs KI, Holtmaat K, Aaronson NK, Holzner B, Terwee CB, Cuijpers P et al (2019) The international index of erectile function (IIEF)-a systematic review of measurement properties. J Sex Med 16:1078–1091. https://doi.org/10.1016/j.jsxm.2019.04.010
Harirugsakul K, Wainipitapong S, Phannajit J, Paitoonpong L, Tantiwongse K (2021) Erectile dysfunction among Thai patients with COVID-19 infection. Transl Androl Urol 10:4376–4383. https://doi.org/10.21037/tau-21-807
Fang D, Peng J, Liao S, Tang Y, Cui W, Yuan Y et al (2021) An online questionnaire survey on the sexual life and sexual function of Chinese adult men during the coronavirus disease 2019 epidemic. Sex Med 9:100293. https://doi.org/10.1016/j.esxm.2020.100293
Bakr AM, El-Sakka AI (2022) Erectile dysfunction among patients and health care providers during COVID-19 pandemic: a systematic review. Int J Impot Res 34:145–151. https://doi.org/10.1038/s41443-021-00504-w
Chen T, Bhambhvani HP, Kasman AM, Eisenberg ML (2021) The association of the COVID-19 pandemic on male sexual function in the United States: a survey study of male cannabis users. Sex Med 9:100340. https://doi.org/10.1016/j.esxm.2021.100340
Mollaioli D, Sansone A, Ciocca G, Limoncin E, Colonnello E, Di Lorenzo G et al (2021) Benefits of sexual activity on psychological, relational, and sexual health during the COVID-19 breakout. J Sex Med 18:35–49. https://doi.org/10.1016/j.jsxm.2020.10.008
Brotto L, Atallah S, Johnson-Agbakwu C, Rosenbaum T, Abdo C, Byers ES et al (2016) Psychological and interpersonal dimensions of sexual function and dysfunction. J Sex Med 13:538–571. https://doi.org/10.1016/j.jsxm.2016.01.019
Sansone A, Mollaioli D, Ciocca G, Limoncin E, Colonnello E, Vena W et al (2021) Addressing male sexual and reproductive health in the wake of COVID-19 outbreak. J Endocrinol Invest 44:223–231. https://doi.org/10.1007/s40618-020-01350-1
Patel KP, Vunnam SR, Patel PA, Krill KL, Korbitz PM, Gallagher JP et al (2020) Transmission of SARS-CoV-2: an update of current literature. Eur J Clin Microbiol Infect Dis 39:2005–2011. https://doi.org/10.1007/s10096-020-03961-1
Yang M, Chen S, Huang B, Zhong JM, Su H, Chen YJ et al (2020) Pathological findings in the testes of COVID-19 patients: clinical implications. Eur Urol Focus 6:1124–1129. https://doi.org/10.1016/j.euf.2020.05.009
Salonia A, Pontillo M, Capogrosso P, Gregori S, Tassara M, Boeri L et al (2021) Severely low testosterone in males with COVID-19: a case-control study. Andrology 9:1043–1052. https://doi.org/10.1111/andr.12993
Maiorino MI, Bellastella G, Giugliano D, Esposito K (2018) From inflammation to sexual dysfunctions: a journey through diabetes, obesity, and metabolic syndrome. J Endocrinol Invest 41:1249–1258. https://doi.org/10.1007/s40618-018-0872-6
Kaynar M, Gomes ALQ, Sokolakis I, Gül M (2022) Tip of the iceberg: erectile dysfunction and COVID-19. Int J Impot Res 34:152–157. https://doi.org/10.1038/s41443-022-00540-0
Bertolo R, Cipriani C, Bove P (2021) Anosmia and ageusia: a piece of the puzzle in the etiology of COVID-19-related transitory erectile dysfunction. J Endocrinol Invest 44:1123–1124. https://doi.org/10.1007/s40618-021-01516-5
Inman BA, Sauver JL, Jacobson DJ, McGree ME, Nehra A, Lieber MM et al (2009) A population-based, longitudinal study of erectile dysfunction and future coronary artery disease. Mayo Clin Proc 84:108–113. https://doi.org/10.4065/84.2.108
Leiblum SR, Rosen RC (1991) Couples therapy for erectile disorders: conceptual and clinical considerations. J Sex Marital Ther 17:147–159. https://doi.org/10.1080/00926239108404956
Funding
This study was supported by the National Natural Science Foundation of China (No.82070560 and No. 81470826) and 1.3.5 Project for Disciplines of Excellence, West China Hospital, Sichuan University (No. ZYGD18023).
Author information
Authors and Affiliations
Contributions
Jinzhi Zhang and Wei Shi have contributed equally to this work. Design: Jinzhi Zhang, Wei Shi and Huatian Gan. Data search and selection: Jinzhi Zhang and Wei Shi. Data analysis and manuscript writing: All authors.
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflicts of interest to disclose.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, J., Shi, W., Zou, M. et al. Prevalence and risk factors of erectile dysfunction in COVID-19 patients: a systematic review and meta-analysis. J Endocrinol Invest 46, 795–804 (2023). https://doi.org/10.1007/s40618-022-01945-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-022-01945-w